Abstract
Retinal astrocytic hamartomas are rare, benign tumors of glial origin. These lesions are often associated with systemic syndromes, including tuberous sclerosis complex and neurofibromatosis type 1, but also may be encountered in otherwise healthy individuals as an acquired lesion. We present the following case to illustrate clinical and imaging characteristics typically seen in astrocytic hamartoma found as “optic nerve incidentaloma” in an otherwise healthy teenager.
Keywords
Introduction
Retinal astrocytic hamartomas (RAHs) are rare, benign tumors of glial origin. These lesions are often associated with systemic syndromes, including tuberous sclerosis complex (TSC) and neurofibromatosis type 1 (NF1), but may also be encountered in otherwise healthy individuals as an acquired lesion (1, 2). Due to the clinical diversity of these lesions, they present specific challenges in diagnosis and treatment. Although the lesions typically remain stable over time, potential for exudative retinopathy and detachment have been reported. The histopathology of these heterogeneous lesions typically reveals a proliferation of well-differentiated astrocytes with variable amounts of calcification. The advent of modern imaging modalities, such as spectral domain optimal coherence tomography (OCT), has recently expanded our understanding of these lesions.
Recently, astrocytic hamartomas have been classified into 4 distinct subtypes (3): type 1 lesions are typically flat and lie within the retinal nerve fiber layer; type 2 lesions have elevation and various degrees of retinal traction; type 3 lesions have internal moth-eaten optically empty spaces that represent intratumoral calcification; and type 4 lesions have optically empty intralesional cavities within the nerve fiber layer. These distinct and very unique subtypes make the proper diagnosis of astrocytic hamartomas a particular challenge when encountered in clinical practice. Correlation of the classification with systemic features revealed type 2 with a greater number of cutaneous plaques, type 3 with a higher incidence of subependymal giant cell astrocytoma, and type 4 with a higher incidence of pulmonary lymphangiomyomatosis. We present the following case to illustrate clinical and imaging characteristics typically seen in astrocytic hamartoma found as “optic nerve incidentaloma” in an otherwise healthy teenager.
Case report
This 16-year-old boy came to our attention for a routine ophthalmological examination. The family history was unremarkable. The visual acuity was 20/20 bilaterally. Pupillary function and color perception did not show any abnormality. Fundus examination showed a peripapillary whitish lesion (Fig. 1). We checked for isolated or multifocal retinal pigment epithelial (RPE) depigmented lesions, but we did not find them.
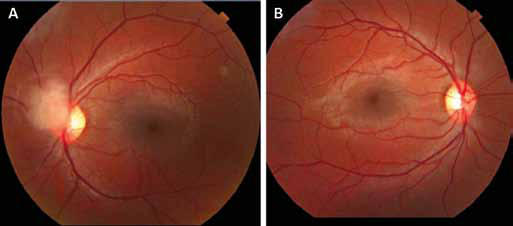
Color fundus photos showing a peripapillary whitish lesion in the left eye.
The patient underwent multimodal retinal imaging: a color fundus photograph evaluated by the Topcon fundus camera, retinal angiography by HRA II Heidelberg®, structural higher resolution spectral domain (SD)-OCT by Spectralis®, and Humphrey Visual Field (24-2 Swedish interactive threshold algorithm standard) (2).
The peripapillary preretinal lesion showed slow enhancement and peripheral vascularity by retinal angiography (Fig. 2). The periphery showed normal perfusion with nonproliferative telangiectatic vessels (Fig. 3).
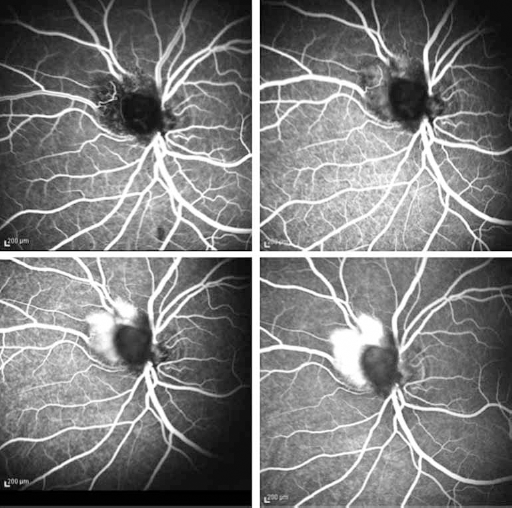
Fluorescein angiography features: the peripapillary preretinal lesion showed slow enhancement.
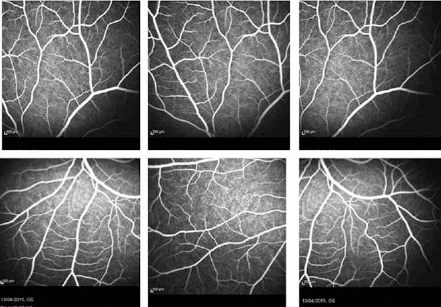
Fluorescein angiography features: in the mid-periphery it is possible to see nonproliferative telangiectatic vessels.
The OCT scans through the optic nerve enabled further detailed descriptions of RAH: abrupt elevation of a mass above the nerve fiber layer with some internal retinal disorganization, mild vitreoretinal adherence, and a continuous branching pattern with the hyaloid membrane (Fig. 4). The differential diagnoses are reported in Table I.
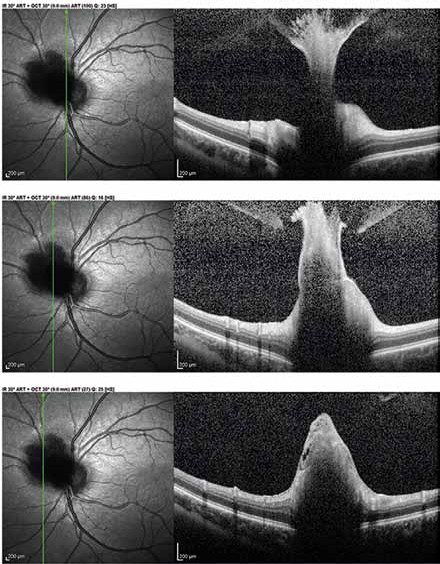
Structural optimal coherence tomography macular scans through the optic nerve show abrupt elevation of mass above the nerve fiber layer with some internal retinal disorganization, mild vitreoretinal adherence, and branching pattern continuos with the hyaloid membrane.
List of differential diagnoses
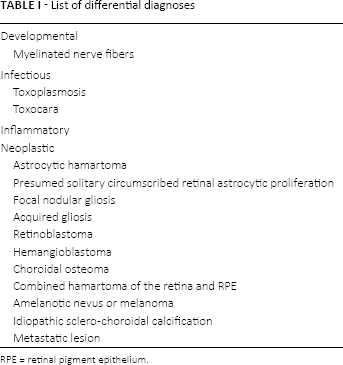

RPE = retinal pigment epithelium.
We inquired about tuberous sclerosis and/or neurofibromatosis. Dermatologists ruled out tuberous sclerosis and neurofribomatosis: the Wood's lamp examination did not show any subclinical pigmentary abnormality; the skin, fingers, and toes were normal.
Discussion
Overall, several retinal lesions may have a white appearance (1). Disc edema was excluded due to its typical appearance and vessel orientation as well as its acute onset. We ruled out a subtle compressive optic neuropathy: pupillary function and color perception were normal.
The developmental, infectious and inflammatory etiology of the lesion seemed to be questionable. Myelinated nerve fibers are usually radial. The lesion did not have the aspect of a ruptured cyst of a cysticercosis either.
We also mention both toxoplasmosis and toxocara. However, toxoplasmosis is usually flat and tends to have a more vitreous cell. Toxocara tends to be a subretinal granuloma with overlying retinal striae. Granulomatous lesions are expected to be associated with other signs of inflammation. The multimodal findings in their entirety do not support these diagnoses.
Solitary circumscribed retinal astrocytic proliferation is a recently described condition seen as a pearl-white nodule but appears in older patients (4).
Out of all the differential diagnoses of nonpigmented lesions, the noncalcified variant of astrocytic hamartoma seems to be the most likely, since it classically arises from the retinal nerve fiber layer: this mass was in the nerve fiber layer of our patient.
RPE depigmented lesions were described in TSC. Pinpoint RPE lesions appear as a single lesion or multifocal lesions, measuring approximately 200 μm. In our case, we did not find RPE “punched-out” depigmentation (5). OCT scans through the optic nerve fitted with the type 2 classification of RAHs. (1). We excluded retinoblastoma because usually they are more vascular and have more prominent vessels. This is not the rare medulla epithelioma that can be seen originally in the posterior fundus. (Only 2 cases are described in the literature, Lawrence Yannuzzi, personal communication.)
The confocal imaging acquisition may play a role in the dark aspect of the lesion. This is not axoplasmic debris. It could be myelin or astrocytic cells but the fan-shape or the discrete bordered morphology of those lesions were not evident here. If it progresses or becomes symptomatic, we would undertake a trial of steroids or a fine-needle aspiration biopsy.
It is unusual to have such a branching pattern continuous with the hyaloid membrane. Also, this did not have a “mulberry” appearance and it was nasal. Our final opinion is that this lesion seems to be a wide type 2 astrocytic hamartoma, based on OCT, angiographic appearance, and clinical course. The patient is a young man with an adherent hyaloid membrane, and we are not surprised that the big elevation is branching with the vitreous without detaching it. The nasal localization is not the most common of all, but it has been described (4).
Conclusion
This young boy came to our attention with an isolated peripapillary lesion – which did not determine a compressive optic neuropathy – with slow enhancement and peripheral vascularity revealed by retinal angiography. OCT scans showed an abrupt elevation of a mass above the nerve fiber layer with some internal retinal disorganization, mild vitreoretinal adherence, and a branching pattern continuous with the hyaloid membrane. Fundus examination excluded other lesions; the vitreous was clear, and no other signs of intraocular inflammation were clinically evident. For all these reasons, the patient was diagnosed with astrocytic hamartoma type 2. At the 12-month follow-up visit, the patient was stable; the VA was 20/20; and the VF showed a subtle enlargement of the blind spot (Fig. 5).
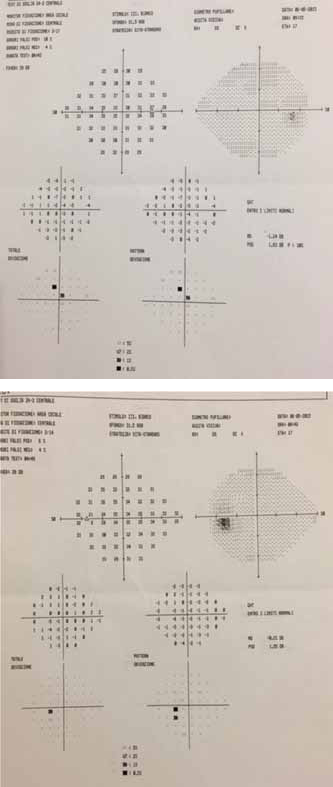
Visual field of both eyes 12 months since the first diagnosis: the comparison between the 2 eyes show a subtle blind spot enlargement in the left eye.
Footnotes
Acknowledgment
We thank Dr. Pichi for his valuable comments.
Financial support: No grants or funding have been received for this study.
Conflict of interest: None of the authors has financial interest related to this study to disclose.
