Abstract
Purpose
To describe a new technique to split rock-hard nuclei using an ultrasonic chopper (Ultrachopper) and a prechopper, in order to perform a modified small incision manual cataract extraction.
Methods
The Ultrachopper device, which is compatible with modern phacoemulsification systems, is used to facilitate the division of very hard nuclei in a straightforward manner using a manual prechopper, and the two fragments are extracted using Kansas forceps.
Results
In rock-hard nuclei, this technique is very effective to divide and extract the fragments. The risk of complications related to phacoemulsification on these very challenging cases is avoided.
Conclusions
This modified small incision manual cataract extraction technique, assisted with an ultrasonic chopper (Ultrachopper) and a prechopper, is a very good alternative in rock-hard nuclei.
Introduction
Phacoemulsification has progressively become the standard for cataract surgery worldwide, but in cases of rock-hard nuclei, the incidence of complications, like posterior capsule rupture and corneal edema are still higher than in standard cases (1-2-3-4). Modifications of the phacoemulsification original techniques have been proposed to overcome the challenge of dividing very hard nucleus. Akahoshi described in 1992 his phaco prechop technique, using a mechanical manual device to separate the nucleus before emulsifying the fragments. That author has shown in many scientific meetings that his technique can be performed in hard cataracts, and many cataract services use it (5-6-7-8-9). On the other hand, several authors have found that this technique is very difficult to master (9, 10).
Some studies and researchers have suggested in the last 20 years that other alternatives, like standard extracapsular extraction or small incision manual extraction, might be superior to phacoemulsification in those very advanced cases (11, 12).
A device consisting of a blade vibrating at ultrasonic speed (Ultrachopper, Alcon, Fort Worth, USA) has been described as an option to divide these rock-hard nuclei (9, 13, 14). This ultrasonic chopper is effective in cutting rock-hard cataracts. However, when performing phacoemulsification in such advanced cases, dividing the nucleus is not the only challenging step, because emulsifying the very dense nuclear fragments also poses additional risks to the corneal endothelium and posterior capsule. Therefore, we looked for an alternative, and herein we describe a technique that combines the cutting capabilities of Ultrachopper, completing the division of the nucleus with an Akahoshi prechopper, followed by a manual removal of the fragments, in order to perform a safer cataract extraction in very advanced cases.
Surgical technique
Using topical or peribulbar anesthesia, initially a 6.5 mm biplanar sclerocorneal tunnel is constructed, beginning around 1.5-2.0 mm posterior to the limbus and with a depth of around 70% of the scleral thickness, either superior or temporal without entering the anterior chamber. A corneal side-port incision, for a second instrument, is created. The anterior capsule is stained with trypan blue, usually under an air bubble. A 2,7-mm incision is performed with a keratome through the previously created scleral tunnel. A 5.5 to 6.0 mm capsulorhexis is performed. Hydrodissection is completed by carefully injecting fluid, not in an excessive amount, to diminish the possibility of sudden posterior capsule blowout. The Ultrachopper is then used to initiate the division of the nucleus into two halves, with the vacuum set at 100 mm Hg and the flow rate at 25 cc/min, using continuous torsional phaco at 100% power and longitudinal phaco at 50% power (Infinity, Alcon Laboratories, Inc. Fort Worth, USA). It is true that when using a peristaltic machine, the preset vacuum level is only reached when there is complete occlusion of the outflow line, typically at the phaco tip. In the case of the Ultrachopper the occlusion occurs at the lateral aspiration ports. However, it is also true that vacuum developed by the machine is proportional to the viscosity of the aspirate and a low level of vacuum is created when aspirating a mixture of cortex, small fragments of nuclear material, ophthalmic viscosurgical device (OVD) and balanced saline solution (BSS), as it occurs when the Ultrachopper is dividing the nucleus. It is advisable to first start the vacuum and not the ultrasonic energy (i.e., keep the foot pedal in position 2), so that the Ultrachopper tip removes cortex, along with the OVD, leaving only BSS in the proximity of the aspiration ports located in the superior portion that is proximal to the flattened segment, assuring that a constant flow of fluid will help to refrigerate the shaft (15). Then the ultrasonic energy is activated and the vibrating blade can make a deep thin groove into the nucleus without exerting significant stress on the capsular bag and zonules. The Ultrachopper does not pose a risk to the posterior capsule, because the length of the blade (2.5 mm) reaches around 40% to 50% of the nucleus thickness, even in the mid-periphery of these hard rock cataracts, which usually are very large and bulky (Figs. 1 and 2). The endpoint of using the Ultrachopper is reached when the depth of the cut performed, is deep enough to let the whole length of the curved portion of the blade, be inside the nuclear material, at an angle of around 30 degrees. It is not necessary to rotate the nucleus to complete the creation of the deep groove in the nucleus. During the step of using the Ultrachopper a second instrument through the side port may be used to hold the eye relatively steady. Moreover, in extremely hard nuclei a sustainer can be used to perform counter fixation in order to facilitate a controlled and gentle creation of the central deep cut. Typically, that step will take less than 1 minute, and usually around 15 seconds. When working with the Ultrachopper, the surgeon should be cautious to avoid injuring the iris. Subsequently, using the blades of an Akahoshi Combo prechopper, it is usually very easy to divide the nucleus without enlarging the incision (Fig. 3 and supplementary Video 1, available online at ophthalmology.pointofcarejournals.com); however, sometimes when a posterior leathery plate is present it could be necessary to use two additional instruments to completely separate the fragments, one through the main incision and the other through the side port incision. After finishing the nuclear division, the main incision is enlarged to 6.5 mm, through the previously constructed biplanar sclerocorneal tunnel. Then, a Drysdale nucleus manipulator is used to push the lower part of one heminuclei, still inside the capsular bag, making it to do a complete tumble. With that maneuver, it is very easy to prolapse the first heminucleus into the anterior chamber (Fig. 4 and supplementary Video 1). Then a Kansas forceps, which has two rows of teeth on jaws in order provide a firm purchase on the nuclear fragments, is used to remove it from the eye, through the 6.5 mm incision (Fig. 5 and supplementary Video 1). The second heminucleus is aligned in position and easily prolapsed to the anterior chamber with the Drysdale manipulator or any other instrument, and removed from the eye with the Kansas forceps. Cortical aspiration is performed in the standard fashion with an I/A probe.
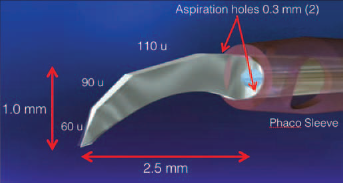
The Ultrachopper has a flattened and curved blade and two small aspiration ports. The device is assembled in a phacoemulsification hand-piece (Image provided by L. Escaf, Barranquilla, Colombia. Used with permission).
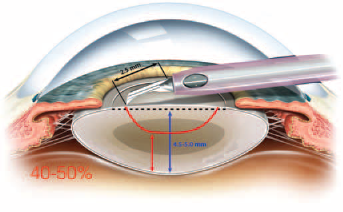
The Ultrachopper blade is 2,5 mm length, thus a “safety zone” of around 2,0 mm will stay untouched while using the device to cut a hard nucleus, which usually has more than 4,5 mm in thickness (Image provided by L. Escaf, Barranquilla, Colombia. Used with permission).
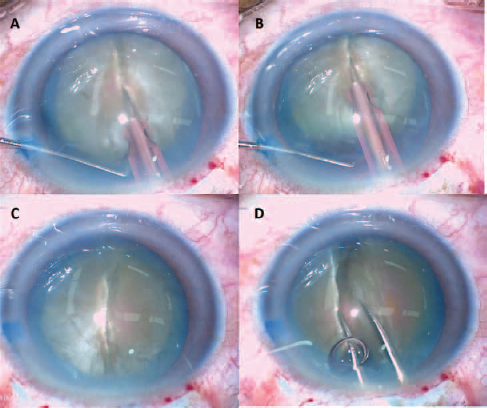
A hard nucleus is easily separated in halves using the combination of an Ultrachopper and a manual Akahoshi prechopper. (
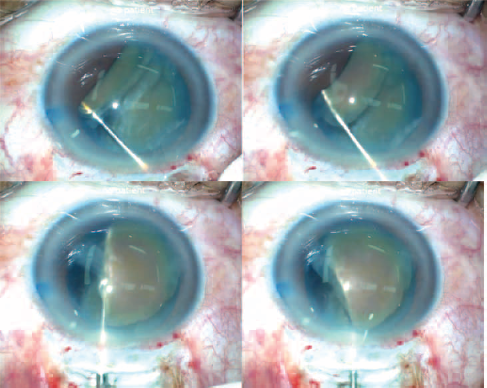
Using a Drysdale manipulator, or a similar instrument, some pressure is exerted on the inferior portion of the medial wall of one heminuclei, causing it to tumble and to prolapse out of the capsular bag.
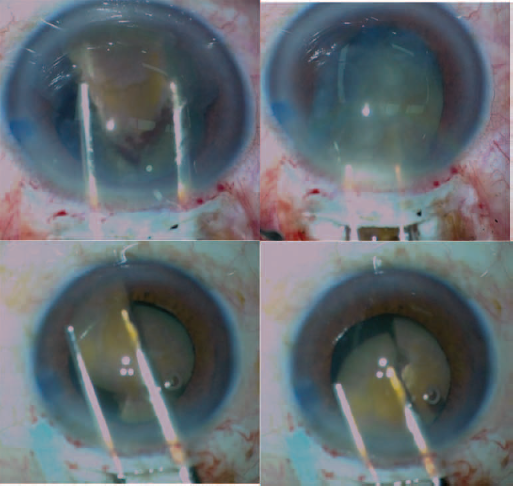
The two heminuclei are extracted from the anterior chamber using a Kansas forceps.
A rigid or foldable intraocular lens is implanted in the capsular bag.
Since the constructed tunnel is not so long (only 1.5 to 2.0 mm), in order to guarantee the stability of the wound and control induced astigmatism, suturing is part of our protocol. Two or three separated sutures are placed.
We use this technique when the nuclear color and opalescence is over 6.5 with the Lens Opacities Classification System III (LOCS III).
Our results in about 50 cases have been very good so far. We have not had any posterior capsule rupture or zonular dialysis. However, the selected cases for this technique did not have iridodonesis or phacodonesis, or evident zonular dialysis in the preoperative examination. In addition, although we did not evaluate the percentage of endothelial cell loss, since we did not have any case of persistent corneal edema, we think it could be comparable to manual extraction. Further studies are warranted to compare results of this alternative with other techniques in rock-hard cataracts.
Discussion
Phacoemulsification in rock-hard cataracts is challenging. In 2004, Bourne et al (1) published the results of a randomized controlled trial performed in two centers in the UK (Moorfields Eye Hospital, London, and the Oxford Eye Hospital, Oxford) between 1994 and 1998. Within the group of 45 patients with hard cataracts, eyes that underwent phacoemulsification had a significantly higher risk of severe cell loss (>15% loss by 1 year) than those that underwent extracapsular cataract extraction (ECCE) (52.6% vs. 23.1%). The authors concluded that phacoemulsification may not be the optimal procedure in rock-hard cataracts and that ECCE should be preferred (1). It is true that phacoemulsification techniques and equipment used around 20 years ago have significantly evolved, but some more recent results have also shown high endothelial cells loss in hard cataracts after phacoemulsification. In 2011, Kim et al reported endothelial cell loss in hard cataracts with phacoemulsification between 37.2 and 42.6% (2).
A validation of a scoring system for preoperative stratification of intraoperative risks of complications during cataract surgery was performed by Agrawal et al in a multi-centric study in India between 2005 and 2006. The hardness of the nucleus (classified as dense, total, brunescent, black and white cataract) was included as a significant risk factor for complications (3).
During the last 20 years, many techniques have been described to deal with phacoemulsification in very hard cataracts, suggesting that there is not yet one that is consistently effective in such cases (16-17-18-19-20-21).
In 1998, Akahoshi (5) described the two approaches of phaco prechop: Karate prechop for cataracts from soft-to-medium hardness (grade I-III), and Counter Prechop for hard cataracts (grade III-V) and complex cases like incomplete capsulorhexis, weak ciliary zonules, pseudoexfoliation syndrome, etc. In the first technique, the sharp edge of a specially designed cross-action forceps (Combo prechopper) is directly inserted into the center of the nucleus, and the blades are slowing opened while the instrument is gently pushed down, until the nuclear division is attained. Then the instrument is withdrawn and the round and dull portion of the blades are used to complete the separation of the heminuclei. Finally, the same maneuvers can be used to obtain four quadrants. In the second technique (Counter Prechop) a second instrument (Nucleus sustainer) is used to stabilize the nucleus. The sustainer is introduced up to the equator of the lens to hold the nucleus. With the blades closed, the Universal Prechopper, which has thinner and sharper blades than the Combo prechopper, is inserted directly into the nucleus while the sustainer applies counterforce. The tips of both instruments must be positioned deeply enough to surround the hardest central core of the nucleus, and in that moment they are advanced toward each other. When the tip of the prechopper reaches the center of the nucleus, the blades are opened in order to bisect the cataract. It may be necessary to relocate and reopen the blades several times, to obtain a complete division. Similar maneuvers are repeated to divide the nucleus in 4 to 8 fragments. In 1998, Akahoshi reported more than 9000 cases of successful procedures, including in rock hard nuclei, with only two cases of zonular rupture. Other groups of surgeons have also reported positive experiences using phaco prechop in hard cataracts (5-6-7-8-9). However, other surgeons have found this technique rather difficult (10, 13).
In addition, as it will be discussed below, obtaining the fragments is only the first difficulty to solve in these challenging cases. The subsequent phase of emulsifying those pieces of hard nuclei, is also very risky, both for the corneal endothelium and for the posterior capsule.
Some variations of the phaco prechopping instruments and/or techniques have been also described. In 2004, Viteri published the V-prechop technique, which included performing two oblique nucleus fractures with the prechopper, with the shape of a “V”, with the vertex pointing to the center of the corneal incision, before hydrodissection. This technique was described as an easier option than standard prechop, especially in soft and medium cataracts (13).
The Salvitti Akahoshi Prechopping Forceps is a cross-action instrument with wider blades to maximize surface area in contact with the nucleus, and sharper tip to facilitate insertion into the cataract material. It has been used in combination with a liquefaction device (AquaLase), but in hard nuclei it has been suggested that this alternative, which uses high-pressure streams of warm (about 60°C) balanced saline solution to fragment the cataract material, is not as efficient as ultrasonic energy (22).
On the other hand, manual small-incision cataract surgery (SICS) for decades has been another alternative in those advanced cases (4, 23). Some years ago, in a trial in India, 270 patients with mature white cataract were randomized to phacoemulsification or manual SICS. Uncorrected distance visual acuity (UDVA) was comparable in the 2 groups at 6 weeks. Yet, the manual SICS group had less corneal edema than the phacoemulsification group. They found that an additional advantage of manual SICS over phacoemulsification was that it proved to be a much faster and cost-effective surgical technique in those eyes with such advanced white cataracts (10). Other researchers have found manual small incision cataract surgery also more cost-effective than phacoemulsification (24).
However, in comparison to standard extracapsular cataract extraction, small-incision cataract surgery requires more nucleus maneuvers inside the anterior chamber during delivery, which increase the odds of corneal endothelial cells trauma (4, 25, 26). Standard manual extracapsular extraction is a time-proven technique and has been shown for several decades to be safe in hard cataracts. Recently Mohanty et al published their results in 207 patients with advanced cataracts (brunescent, black, total, white or dense) who underwent conventional extracapsular cataract extraction (12). They found that 2.9% of the cases had posterior capsule rupture (in contrast with 7.5% of similar cases performed with phacoemulsification in the study by Agrawal et al (3)). However, on the other hand, since the incision is larger (typically 9 to 12 mm), standard extracapsular extraction has more risk of high postoperative-induced astigmatism, and wound-related complications, like dehiscence.
The use of prechopping techniques in manual SICS has been also reported. In 2002 Wiriyaluppa and Kongsap (27) published their combined option, using Prechopping, as described by Akahoshi, to divide the nucleus before removing it manually through a 5-6 mm corneal incision. Following bisection of the nucleus, ophthalmic viscosurgical device was injected to prolapse the first fragment into the anterior chamber with the assistance of a spatula and then, using gentle pressure on the posterior lip of the wound, it was extracted from the eye with a 0.12 mm corneal forceps. In 2006 they described a modification of their technique using a nuclear chopper and a 23 G disposable needle or a Micro vitreoretinal blade, instead of a prechopper forceps (28).
Bhatti (29) in 2005 described another manual small incision cataract surgery technique including the use of the Akahoshi's phaco prechop. Nuclear division was performed by that author through a 5-6 mm corneal tunnel with a technique similar to Counter prechop, but, unlike Wiriyaluppa and Kongsap, the fracture was performed partially outside the capsular bag, after dislocating the proximal portion of the nucleus into the anterior chamber. The prechopper was inserted through the corneal tunnel into the posterior aspect of the nucleus while the anterior aspect of the nucleus was stabilized using counterpressure exerted through a sideport by a dialer, so that it was not pushed towards the endothelium by the prechopper. The fragments were then removed with a vectis under copious viscoelastic (29, 30).
Ultrachopper is an ultrasonic blade that was described in 2007 by Escaf et al, as a tool to perform nuclear fracture in a more effective way (14, 31, 32). The Ultrachopper is a modified phaco needle, with a thin, flat and curved tip. It has two aspiration ports located in the superior portion, proximal to the flattened segment. As mentioned, this ultrasonic blade may be used with any phaco system by connecting it to the hand-piece; it can quickly be interchanged with another phaco needle when necessary to go on with the emulsification of the fragments. Some systems have the option of an additional port for this device where an additional hand-piece can be connected independently (Infinity and Centurion from Alcon) to avoid the necessity of changing the tip of the hand-piece. It has been shown that this ultrasonic chopper is very efficient in dividing rock-hard nuclei (14, 31, 32). We found that mastering the Ultrachopper as the only tool used to divide a rock-hard nucleus is not so easy, while using it to construct an initial deep groove and then use a manual Akahoshi Combo prechopper makes the step of dividing these very hard nuclei very easy. On the other hand, using sole the manual Akahoshi prechopper in these very advanced cataracts is also difficult (9).
As mentioned before, in those challenging cases, nuclear fractis is only the first obstacle to overcome. To emulsify the very dense and bulky resulting fragments is also very demanding and poses risks to the corneal endothelium and posterior capsule.
We consider that there is still room for SICS in such cases because manually removing the fragments is safer and more predictable than using phacoemulsification. In addition, taking advantage of the capabilities of Ultrachopper for dividing those rock-hard cataracts, makes the technique easier than dividing the nucleus with manual approaches usually used in SICS or employing the prechoppers (26-27-28-29-30).
In conclusion, this Ultrachopper-assisted prechopping for small incision cataract extraction, is a very good alternative in rock-hard cataracts, and should be in the armamentarium of today's cataract surgeon.
