Abstract
Introduction
A meta-analysis was done to investigate the clinicopathological significance of the loss of p27kip1 expression in papillary thyroid carcinoma (PTC).
Methods
The meta-analysis involving 17 studies included 1,652 PTC and 328 benign cases. The rate of p27kip1 expression loss in PTC and benign lesions, and the correlations between p27kip1 expression loss and clinicopathological characteristics of PTC were determined.
Results
The estimated rate of p27kip1 expression loss was 0.557 (95% confidence interval [CI] 0.443-0.665) and 0.139 (95% CI 0.062-0.283) in PTC and benign lesions, respectively. In subgroup analysis, the rates of p27kip1 expression loss were 0.683, 0.393, and 0.414 in the classical variant, follicular variant, and papillary thyroid microcarcinoma, respectively. Loss of p27kip1 expression was significantly correlated with lymph node metastasis and distant metastasis (odds ratio 3.559, 95% CI 1.146-11.056 and 4.735, 95% CI 1.322-16.960, respectively). Extrathyroidal extension was correlated with loss of p27kip1 expression, but not in a statistically significant way (p = 0.051). There were no significant correlations between loss of p27kip1 expression and sex, tumor size, BRAFV600E mutation, and tumor multifocality.
Conclusions
Loss of p27kip1 expression is frequently found in PTC compared with benign lesions and normal thyroid tissue. When present in PTC, it is correlated with aggressive tumor behavior.
Introduction
Papillary thyroid carcinoma (PTC) is the most common endocrine organ malignancy. The majority of PTC cases have an indolent course compared to other malignant tumors (1). However, some PTCs have aggressive features, such as lymph node metastasis and distant metastasis, which are associated with tumor recurrence and poor survival rates (2). Various diagnostic and prognostic markers that have been identified include ki-67, p53, galectin-3, p27kip1, cytokeratin 19, and serum neopterin (1, 3–5). p27kip1 is a cyclin-dependent kinase inhibitor whose expression is reduced in many human cancers including thyroid cancer (4). However, the clinicopathological implications of the loss of p27kip1 expression have not been fully elucidated in PTC.
To clarify this issue, we performed a meta-analysis with the aim of determining the rate of 27kip1 expression loss in PTC and benign thyroid lesions. In addition, the clinicopathological implications of p27kip1 expression loss were evaluated.
Materials and Methods
Published study search and selection criteria
Relevant articles were obtained by searching the PubMed and MEDLINE databases through March 15, 2016. These databases were searched using the key words “thyroid” and “p27kip1 OR p27”. The titles and abstracts of all searched articles were screened for exclusion. Review articles were screened to find additional eligible studies. Articles were included if the study was performed in human PTC and if there was information about the clinicopathological characteristics of PTC. Articles were excluded if they were case reports or non-original articles, or if the article was not written in English.
Data extraction
Data from all eligible studies (3, 4, 6–20) were extracted by 2 independent authors. The extracted data included the first author's name, year of publication, study location, number of patients analyzed, antibody dilution ratio, evaluation criteria, and information for the correlation between loss of p27kip1 expression and clinicopathological characteristics.
Statistical analyses
To perform the meta-analysis, all data were analyzed using the Comprehensive Meta-Analysis software package (Biostat). We investigated the rates of loss of p27kip1 expression in PTC and benign lesions, and the correlations between p27kip1 expression loss and various clinicopathological characteristics of PTC. Heterogeneity between the studies was checked by the Q and I 2 statistics and expressed as p values. Additionally, sensitivity analysis was conducted to assess the heterogeneity of eligible studies and the impact of each study on the combined effect. Because the eligible studies used various diagnostic criteria and populations, the application of a random-effects model rather than a fixed-effects model was more suitable. For the assessment of publication bias, Begg's funnel plot and Egger's test were used. The results were considered statistically significant at p<0.05.
Results
Selection and characteristics of the studies
Two hundred thirty-two reports were identified in the database search. Among these, 215 were excluded because they involved other diseases (n = 91), used animals or cell lines (n = 75), contained insufficient/no information (n = 36), were non-original (n = 8), or were not in English (n = 5). Finally, 17 studies were included in this systematic review and meta-analysis (Fig. 1 and Tab. I). These studies included 1,652 PTC and 328 benign cases.
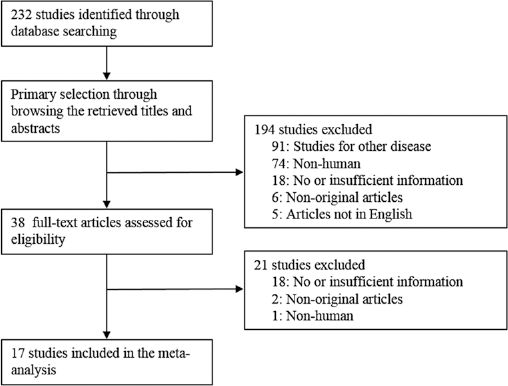
Flowchart of study search and selection methods.
Main characteristics of eligible studies
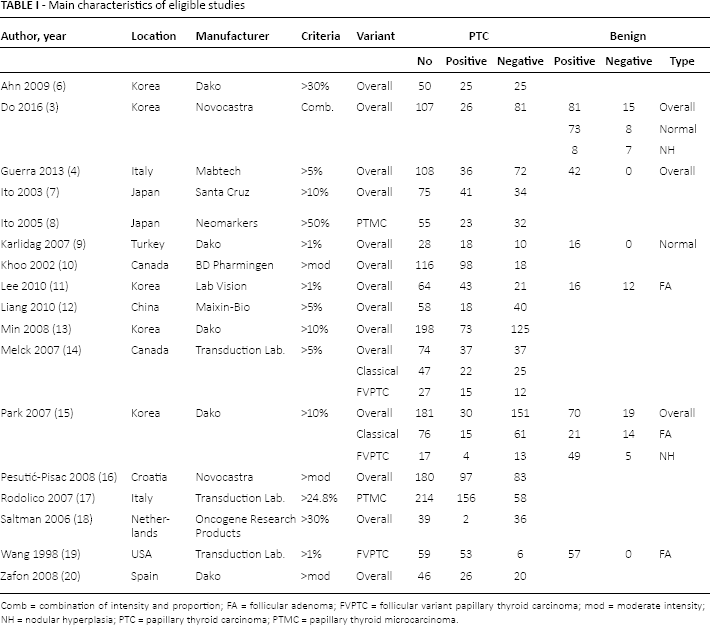
Comb = combination of intensity and proportion; FA = follicular adenoma; FVPTC = follicular variant papillary thyroid carcinoma; mod = moderate intensity; NH = nodular hyperplasia; PTC = papillary thyroid carcinoma; PTMC = papillary thyroid microcarcinoma.
Systematic review and meta-analysis
The rate of loss of p27kip1 expression in patients with PTC in the eligible studies varied from 10.2% to 92.3%, and the estimated rate of loss was 0.557 (95% CI 0.443-0.665) (Tab. II). The range of loss of p27kip1 expression of benign lesions was 0-46.7%, and the estimated rate of loss was 0.139 (95% CI 0.062-0.283). In subgroup analysis based on variants of PTC, the rate of loss of p27kip1 expression was 0.683 (95% CI 0.381-0.882), 0.393 (95% CI 0.097-0.795), and 0.414 (95% CI 0.162-0.720) in the classical variant, follicular variant, and papillary thyroid microcarcinoma, respectively. In benign lesions (follicular adenoma and nodular hyperplasia), loss of p27kip1 expression was 0.268 (95% CI 0.092-0.571) and 0.228 (95% CI 0.035-0.708), respectively. The rate of loss of p27kip1 expression of normal thyroid tissue was 0.092 (95% CI 0.047-0.170).
Correlations between loss of p27kip1 expression and clinicopathological parameters were evaluated. Loss of p27kip1 expression was significantly correlated with lymph node metastasis and distant metastasis (odds ratio [OR] 3.559, 95% CI 1.146-11.056 and OR 4.735, 95% CI 1.322-16.960, respectively). Extrathyroidal extension was correlated with loss of p27kip1 expression but this was not statistically significant (p = 0.051). There were no significant correlations between loss of p27kip1 expression and sex, tumor size, BRAFV600E mutation and tumor multifocality (Tab. III).
Meta-analysis for the rates of loss of p27kip1 expression in papillary thyroid carcinoma and benign lesions
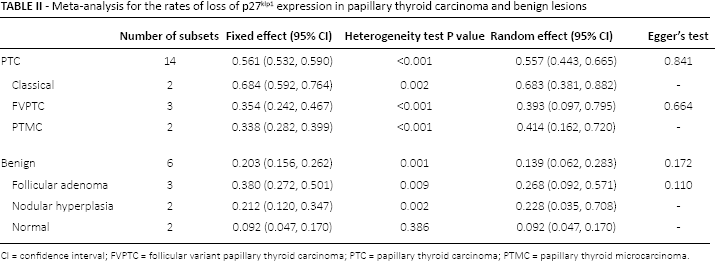
CI = confidence interval; FVPTC = follicular variant papillary thyroid carcinoma; PTC = papillary thyroid carcinoma; PTMC = papillary thyroid microcarcinoma.
Meta-analysis for odds ratio between loss of p27kip1 expression and clinicopathological parameters in papillary thyroid carcinoma
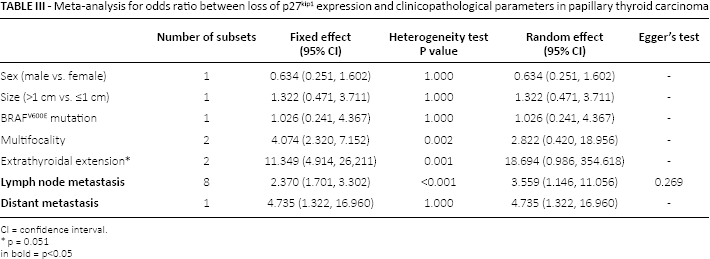
CI = confidence interval.
p = 0.051
in bold = p<0.05
Discussion
Although the majority of PTC cases have an indolent course, distant metastasis has been found in 2.2% of PTC (1, 3). Several studies for prognostic markers of PTC have been reported but the results were inconclusive. This study is the first meta-analysis of the rate of loss of p27kip1 expression and the correlation between p27kip1 expression loss and clinicopathological characteristics in PTC.
In many malignancies, loss of p27kip1 expression is significantly correlated with aggressive behavior and poor prognosis (4). In thyroid cancer cells, p27kip1 downregulation may be induced by the RET/PTC-1 oncogene and may be associated with human carcinogenesis (21). Therapy using the phosphoinositol-3-kinase (PI3K)/mTOR inhibitor has been tested in various cancers including thyroid cancer (22). The inhibitor induces G0/G1 cell cycle arrest and apoptosis (22). Various cyclins, cyclin-dependent kinases (CDKs) and CDK inhibitors, such as p27kip1, are involved in the transition of G0/G1 to S phase. Therefore, a better understanding of the role of p27kip1 expression may be important for the management of PTC using drugs associated with cell cycle arrest. In our meta-analysis, the rate of loss of p27kip1 expression was significantly higher in PTC than in benign lesions (0.557, 95% CI 0.443-0.65 vs. 0.139, 95% CI 0.062-0.283).
Numerous studies have reported on the correlation between p27kip1 expression and clinicopathological parameters (3, 4, 6–20). However, the results have been contentious due to discrepancies caused by various factors, including different populations and different evaluation criteria for p27kip1 expression. We felt that a meta-analysis examining the correlation between p27kip1 expression and clinicopathological parameters would be useful in obtaining more conclusive information. In the present meta-analysis, loss of p27kip1 expression was significantly correlated with lymph node metastasis and distant metastasis. However, no correlations were evident between p27kip1 expression and tumor size, BRAFV600E mutation and tumor multifocality. Low p27kip1 expression has been significantly correlated with extrathyroidal extension (3, 23). Because the heterogeneity for the correlation between p27kip1-positive cases and extrathyroidal extension was too large in 2 eligible studies (63.6% vs. 14.9%), there was not statistical significance in the meta-analysis (3, 23).
The prognostic role of loss of p27kip1 expression has not been fully elucidated. An unpublished finding of the present meta-analysis was that distant metastasis was present in 2.7% of PTC cases at diagnosis and was significantly associated with poor disease-free survival (hazard ratio 6.517, 95% CI 3.510-12.097). In another study, loss of p27kip1 expression was observed in 85.2% and 54.8% of patients with and without distant metastases, respectively (12), while Tallini et al (23) found that low p27kip1 expression was significantly correlated with a poor disease-free survival rate. However, in the present meta-analysis, the correlation between p27kip1 expression and survival rate could not be determined due to insufficient information from the eligible studies. Taken together, our data and those of previous reports suggest that loss of p27kip1 expression may be useful for predicting the prognosis of PTC.
There are some limitations to the present meta-analysis. First, with immunohistochemical staining, p27kip1 can be expressed in both the cytoplasm and the nucleus. In the process of the loss of p27kip1 expression, p27kip1 is first exported from the nucleus to the cytoplasm and sequentially sequestered in the cytoplasm. p27kip1 expression has been reported in the nucleus of normal thyroid follicular cells (24). By contrast, other authors reported that p27kip1 was almost entirely located in the cytoplasm of nonthyroid cancer cells and was relocalized to the nucleus by inhibition of the PI3K/Akt pathway (25). However, the significance of subcellular localization could not be clarified in our meta-analysis due to insufficient information in the eligible studies. Second, the eligible studies used various evaluation criteria for p27kip1 immunohistochemical expression. In subgroup analysis based on evaluation criteria, the rate of p27kip1 expression loss was 0.289 (95% CI 0.178-0.433) and 0.617 (95% CI 0.480-0.737) in lower (≤1%) and higher (>1%) criteria subgroups, respectively. In addition, to compensate for the heterogeneity due to the variable evaluation criteria between eligible studies, all analyses in the current study were performed using the random-effects model. More studies will be needed for confirmation of the evaluation criteria of p27kip1 immunohistochemical expression.
In conclusion, loss of p27kip1 expression was frequently found in PTC rather than in benign thyroid lesions or normal thyroid tissue. Loss of p27kip1 expression was significantly correlated with aggressive behavior such as lymph node metastasis and distant metastasis. These findings will be useful in predicting tumor behavior in PTC as well as differentiating PTC from benign lesions.
Footnotes
Financial support: This study was supported by research funds from Chosun University, 2016.
Conflict of interest: The authors declare that there is no conflict of interest.
