Abstract
Background:
The development and application of medical glue has been continuously expanding and advancing. However, there are few glues that combine low-cost with excellent biocompatibility.
Methods:
We have prepared a medical tissue glue using a gelatin (Gel), sericin (SS) and carboxymethyl chitosan (CMCS) blend solution, cross-linked with 1-ethyl-3-(3-dimethylaminopropyl)-carbodiimide (EDC). The combination’s characteristics and microstructure morphology were observed by Fourier transform infrared spectroscopy (FT-IR) and scanning electron microscope (SEM). Bond strength tests were used to measure the bond strength of the glue. To assay blood compatibility, a hemolytic test, dynamic coagulation test and platelet adherence test were also investigated. Further, the cellular behavior of L-929 and a systemic acute toxicity test on the Gel/SS/CMCS tissue glue were also investigated by MTT and H&E staining.
Results:
Characterization analysis showed that there was stable binding between raw materials, forming an amide bond with homogeneous holes. The bond strength of the tissue glue reached 2.50 ± 0.04 N in 10 minutes, slightly higher than the alpha-cyanoacrylate biological glue (2.25 ± 0.05 N). Blood compatibility tests revealed that the glue had outstanding blood compatibility. Further, cytotoxicity test and systemic acute toxicity test both showed that the glue was without cytotoxicity and not toxic to the body.
Conclusions:
The Gel/SS/CMCS tissue glue we prepared at low cost had excellent biocompatibility and structural characteristics. It could be a better candidate for tissue engineering in biomedical applications applied in clinical practice to promote skin wound healing and to further reduce the formation of skin wound scars.
Introduction
Tissue engineering is a hot research field in modern medicine, and has brought hope for the reconstruction of a variety of functional tissues and organs. The purpose of tissue engineering is to rebuild the original structure of the body itself. Therefore, the material should be biodegradable (1). Importantly, the material should also induce cell growth. At present, there are 3 kinds of biodegradable scaffold materials for tissue engineering: synthetic macromolecules, such as polylactic acid (2-4), polyglycolide acid (5, 6), etc.; and natural polymers, which are widely favored by scientists in the field of biomaterials because of their unique biocompatibility, such as sericin protein (7, 8), silk fibroin (9, 10), collagen (11), etc. The third is natural inorganic materials, such as coral reef (12), hydroxyapatite (13, 14), etc. From the point of view of degradation rate, mechanical properties, processing performance and price, synthetic polymers are far better than natural polymers, but importantly, their properties of cell affinity and biocompatibility are worse than those of natural polymer. On the other hand, natural polymer materials have poor processing performance, their rate of degradation cannot be controlled and they are expensive. Based on the above considerations, it is of great importance to find biomaterials that combine suitable degradation rates with good biocompatibility.
With the widespread application of biomedical materials in medical practice, the biomedical glue used to replace traditional sutures after surgery has been rapidly developed in recent decades and extensively studied. This comes into direct contacted with the blood and tissues of skin wound. Tissue glue, as part of tissue engineering, has to have a suitable pore structure to provide for cell adhesion and proliferation. The material should be gradually degraded in the wound repair process, so that the pore spaces are not completely blocked (which would lead to fibrosis hyperplasia (15, 16)), so any skin wound scar is reduced.
Sericin (SS), a kind of globular protein with excellent properties, accounting for 20%-30% of the content of silk, contains 18 kinds of amino acids which are essential to the human body and have good hydrophilicity (17). To address concerns about the generally poor mechanical properties of natural polymer materials, SS can be combined with polyvinyl alcohol (18) or other synthetic macromolecules (19) to enhance its mechanical properties. Rao et al (20) found that the addition of SS can increase the mechanical properties of porous SS/silk fibrin (SF) scaffold. In addition, the study found that the amino acids in SS in terms of content or types are similar to the natural moisturizing factor of skin (21). And SS (22, 23) and most other similar compounds, such as SF (24) or bacterial cellulose (25) treated with SS, can improve extracellular matrix production, and thus promote skin wound healing.
Gelatin (Gel), is a degraded product of collagen in the connective tissue of animal skin, bone, muscle membrane and tendon. It is a kind of high molecular weight protein, composed of 18 kinds of amino acids (26), and is widely used in glues (27, 28), hemostatic agents (29) and wound dressings (30).
Carboxymethyl chitosan (CMCS) has outstanding water solubility (31). In addition, CMCS has been confirmed to have an inhibitory effect on Staphylococcus aureus (32, 33). Furthermore, it can promote the adhesion, growth and reproduction of fibroblasts in vitro (34) and in vivo (35). It can also promote skin wound healing (36). Scaffolds based on Gel and CMCS for dermal tissue engineering have been studied (37). They are highly porous, and have a high water uptake and water retention capacity. The cells seeded on the scaffolds demonstrated expression of collagen type I, hypoxia-inducible factor-1α and vascular endothelial growth factor, providing a clue regarding their growth and proliferation along with their potential to support angiogenesis during skin wound healing.
The development and application of medical glue has been continuously expanding and advancing (38, 39). The need is for a glue for medical applications for skin injury that is (i) safe, nontoxic and nonirritating; (ii) biodegradable; (iii) fast-curing and with a high bond strength; and (iv) that promotes wound healing and repair. Since the 1970s, the clinical application of α-cyanoacrylate medical tissue glue has reached millions of patients (40). However, the heat of polymerization has been the greatest problem with it (41), and its drawbacks have limited it applicability – including its brittleness, local tissue toxicity (42) and price, which is too high for many patients to be able to afford. Therefore, it is of great importance to develop a medical tissue glue that acts on skin wounds, based on a wide range of raw materials and low price, and which is conducive to cell adhesion and growth. And what is more, regarding tissue engineering, it should reduce the formation of scars. Therefore, the purpose of this study was to develop a tissue glue composed of Gel, SS and CMCS, with the addition of cross-linked, water-soluble 1-ethyl-3-(3-dimethylaminopropyl)-carbodiimide (EDC), and then to evaluated its essential properties.
Materials and methods
Materials
Gel (type A from porcine skin) was purchased from DaMao (Tianjing, China). SS was made in the laboratory following a procedure described in the literature (43) (molecular weight: 66.2~130 kDa). CMCS (high viscosity >400 mPa•s) was purchased from XiYa (Shandong, China). EDC and dimethyl sulfoxide (DMSO) were purchased from Sigma Aldrich (St. Louis, MO, USA). Roswell Park Memorial Institute-1640 medium (RPMI-1640) and trypsin were purchased from Hyclone (St. Logan, UT, USA). Fetal bovine serum (FBS) was purchased from SiJiqing (Zhejiang, China). 3-[4,5-Dimethylthiazol-2-yl]-2,5-diphenyltetrazolium bromide (MTT) was purchased from Solarbio (Beijing, China). New Zealand white rabbit and Sprague Dawley (SD) rats were obtained from the Animal Experiment Center of DaPing Hospital (Chongqing, China). All chemicals and solvents were used without further purification.
Preparation of Gel/SS/CMCS tissue glue
A 30 wt% solution of Gel, a 5 wt% solution of SS and a 3 wt% solution of CMCS were all dissolved in deionized water. The Gel, SS and CMCS solution were stirred at 37°C -40°C at about 220-260 RPM and allowed to react for about 60 minutes. Then water-soluble carbodiimide (EDC) was added to cross-link for 20 minutes, and let it stand still for a few hours to obtain a tissue glue with transparent color and emulsion-like quality. The freeze-dried tissue glue was analyzed by Fourier transform infrared spectroscopy (FT-IR; Spectrum 100, Perkin Elmer) using KBr pellets, at a spectral range of 4,000-600 cm-1. It was found that there were slight deviations of 1,630 cm-1 (vC=O, amide I) and 1,542 cm-1 (vN-H, vC-N, amide II) compared with Gel and CMCS, which indicated that the combination of Gel and CMCS had formed amide bonds (Fig. 1). Different samples, each composed of different components, were prepared to evaluate their essential properties (Tab. I).
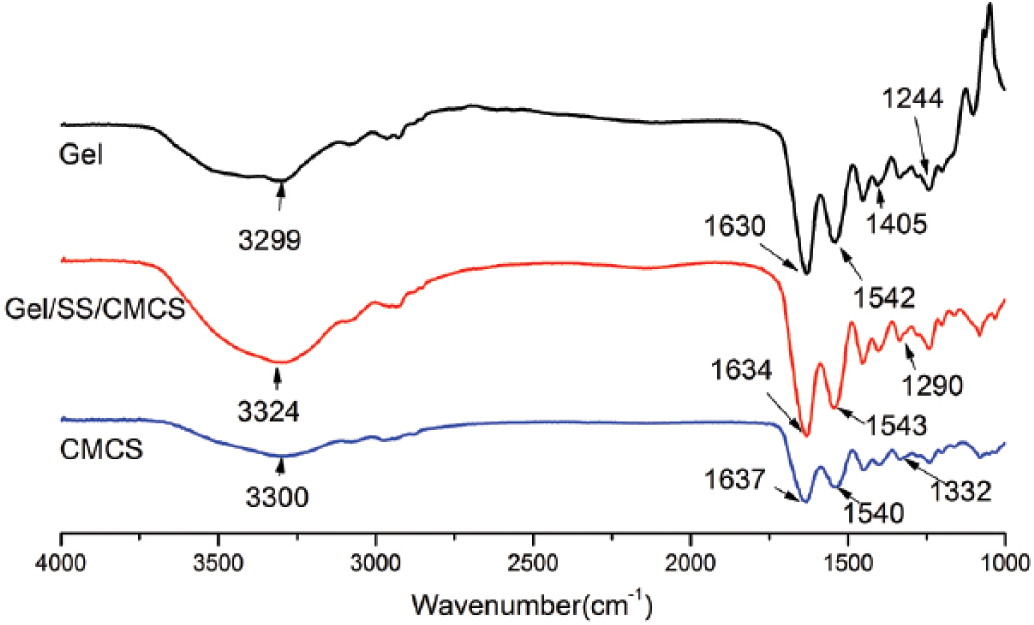
Infrared spectra of gelatin (Gel), Gel/SS/CMCS and CMCS. CMCS = carboxymethyl chitosan; SS = sericin.
Components in each sample
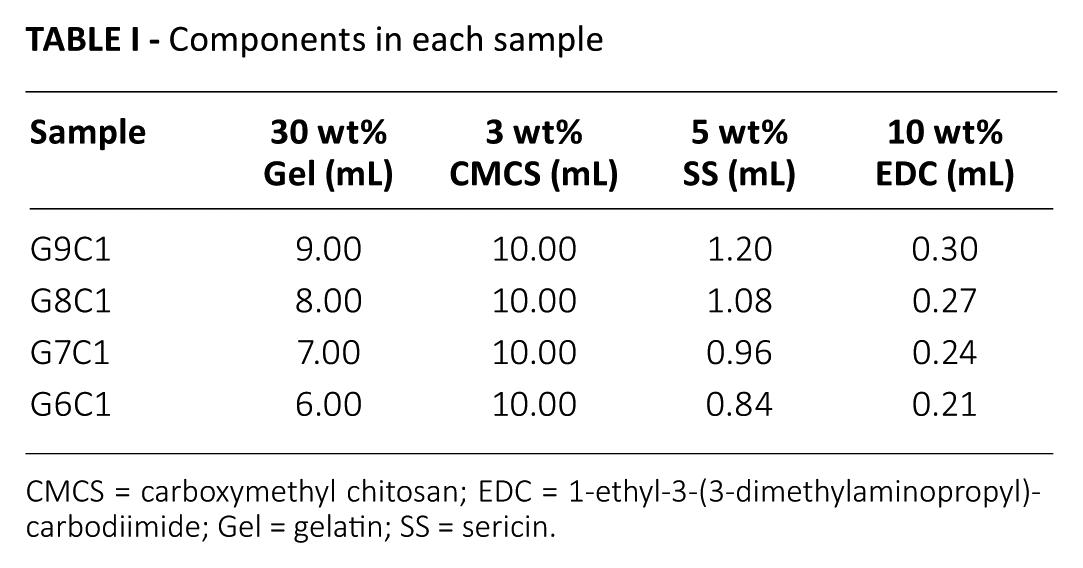
CMCS = carboxymethyl chitosan; EDC = 1-ethyl-3-(3-dimethylaminopropyl)-carbodiimide; Gel = gelatin; SS = sericin.
Characterization of Gel/SS/CMCS tissue glue
Scanning electron microscopy
The microstructure and surface morphology of freeze-dried tissue glues were observed by scanning electron microscope (SEM; LEO-supra35; ZEISS, Germany). Before observations, we sputtered the samples with an ultrathin layer of gold in a coating system.
Bond strength test
To simulate the structure and composition of the dermis and subcutaneous tissue of wounds, which are mainly composed of protein and polysaccharide, especially rich in collagen, a certain concentration of filtered thermal Gel solution was added to a glass sheet [S = 6 × 2 cm2, Length(L) × Width(W)], coated evenly and dried under natural conditions for 24 hours. A glass sheet with a thin film of Gel was thus obtained. The test area was the central region of the glass sheet with a thin film of Gel [(S = 2 × 2 cm2) (L × W)].
Tissue glue solution (50 µL) was added to the test area of one glass sheet, and 20 µL of EDC was added to another glass sheet. Weights (100 g) were then used to press the sheets for 5 or 10 minutes at 37°C to bond the test areas of the 2 glass sheets together.
The bond strength was the maximum force required to separate the 2 pieces of glass, which was tested by a computer-controlled biomechanical testing machine (DNS20, China CIMACH) (n = 5). The test device was attached to the 2 glass sheets with suckers. The hooks of the suckers were then connected to the mechanical sensor of the testing machine. The testing rate of the mechanical sensor was 10 mm/min.
Evaluation of blood compatibility
Hemolytic test
In brief, the ear edge vein blood of a New Zealand white rabbit was drawn and prepared in a fresh dilution with anticoagulant rabbit blood. Freeze-dried (-20°C for 2 hours, then -80°C for 12 hours) materials (50 ± 1 mg) (1 × 1 × 0.5 cm; L × W × T) of different proportions fixed with 10 mL of physiological saline (0.9 wt% NaCl) (experimental group), 10 mL of physiological saline (negative control group) and 10 mL of deionized water (positive control group) were keep at 37°C for 30 minutes. Diluted fresh anticoagulant (20 μL) was added to each group, then transferred to a constant temperature oscillator for 1 hour at 37°C, 120 RPM. This was then centrifuged for 5 minutes at 1,000 RPM, and 200 μL of supernatant was inserted into a 96-well plate. Absorbance was measured by a microplate reader (Multiskan GO; America Thermo) at 540 nm (n = 3). The hemolytic rate was then calculated as follows (44):
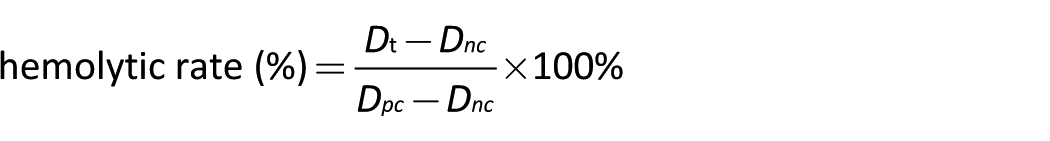
where Dt represents the absorbance of the experimental group, Dnc and Dpc represent the absorbance of the negative control group and the positive control group, respectively.
Dynamic coagulation test
Freeze-dried materials of different proportions (50 ± 1 mg) (experimental group) and those with no added material (blank control group) were left to stand for 5 minutes at 37°C. Fresh diluted anticoagulant (250 μL) and 20 μL of 0.2 mol/L CaCl2 were added to each group, shaken well and left to stand for 5 minutes at 37°C. Deionized water (100 mL) was added to each group, then shaken for 10 minutes at 37°C, let it stand still for a certain period of time until the solution was clear, then 200 μL of supernatant was added to a 96-well plate.
The steps above were repeated, with changes to time of shaking, from the initial 10 minutes, to 20, 30 and 50 minutes. Optical density (OD) values were determined by microplate reader at 540 nm (n = 3). Blood clotting index (BCI) was calculated as follows:

where IS represents the OD values of the experimental group and ID represents the OD values of the blank control group.
Platelet adherence test
Diluted fresh anticoagulant (1 mL) was added to material samples (50 ± 1 mg) (experimental group) or not added (blank control group), shaken for 1 hour at 37°C, then 19 mL of 0.109 mol/L trisodium citrate solution was added to each group, sealed and fully mixed, then let it stand still for 2 hours. Supernatant (10 μL) was added to the blood cell counting chamber and accurately counted by inverted microscope (n = 3). The platelet consumption rate (Pc) was determined as follows:

where Nt represents the number of platelets in the experimental group and No represents the number of platelets in the blank control group.
In vitro cytotoxicity test
Leaching solution of the experimental material (freeze-dried material samples immersed in Dulbecco’s modified Eagle’s medium [DMEM] with 10% FBS and 1% penicillin and streptomycin for 24 hours at 37°C) and cultured mouse fibroblast cells (L-929) were prepared, then 100 μL of cell suspension (2 × 104 cells/cm2) and 100 μL of leaching solution of the materials were each added to each well of a 96-well plate. The cultured cells were used as a control sample. The culture environment was maintained at 37°C in 5% CO2. At 24, 48, 72 and 96 hours, attached cells were stained with 20 μL of 5 mg/mLMTT for 4 hours at 37°C in 5% CO2. A formazan derivative was formed and then dissolved thoroughly with 150 μL of DMSO for 10 minutes. OD values were determined at 490 nm (n = 3).Relative growth rate (RGR) of L-929 was determined as follows:

where ODt represents the OD values of the experimental group and ODc represents the OD values of the control group.
Systemic acute toxicity test
The systemic acute toxicity of the material was assessed by intravenous injection of material into SD rats. The rats were anesthetized with pentobarbital sodium (45 mg/kg) intraperitoneally. Each group of rats was half male and half female. The experimental group A (n = 10) and experimental group B (n = 10) were intravenously injected with the material diluted solutions (G9C1 and G8C1, 200 mg/mL, respectively), and the control group (n = 10) was intravenously injected with physiological saline.
Following the standard GB/T16886.11-2011 (45), the injection amount was less than 0.04 mL/g (rat body weight), and the injection speed was less than 2 mL/min, to complete the sample injection dose within 24 hours one or more times. After 7 days, a pathology examination of all rats was carried out, and then heart, liver, spleen, lung and kidney were removed. The organ tissues were fixed in 10% formalin and then stained with hematoxylin and eosin (H&E). Pathological changes were observed under a microscope.
Statistical analysis
Statistical analysis of data was performed using 1-way analysis of variance (ANOVA). Results were expressed as means ± standard deviation (SD), with p values less than 0.05 indicating significance.
Results
Characterization of Gel/SS/CMCS tissue glue
SEM
The microstructure of material samples was investigated using SEM, as illustrated in Figure 2. As shown in the figure, the samples of P-G9C1 and P-G8C1 showed smooth holes which were uniform and interpenetrated each other. In contrast, P-Gel was rough, and the holes were uneven. Furthermore, it can be seen that S-Gel was also rough and uneven, while the surface of the glue materials was smooth. In addition, S-G8C1 was better than S-G9C1.

SEM photographs of microstructure of material samples. Cross-sections of microstructures of G9C1 (P-G9C1) (
Bond strength
Figure 3A and B shows the bond strength for different curing times, different compositions of Gel/CMCS (G/C) and different concentrations of EDC. It can be seen from the curves that tissue glues had optimal bond strength when the concentration of cross-linking agent was 10 wt%. The bond strength of the tissue glue increased with the increase of the proportion of Gel for the same curing time and same concentration of cross-linking agent. In addition, the bond strength of tissue glue at a curing time of 10 minutes was better than at 5 minutes. Based on the above results, when the curing time is 10 minutes and the concentration of EDC is 10 wt%, the best bond strength will be found with G9C1 (2.50 ± 0.04 N).
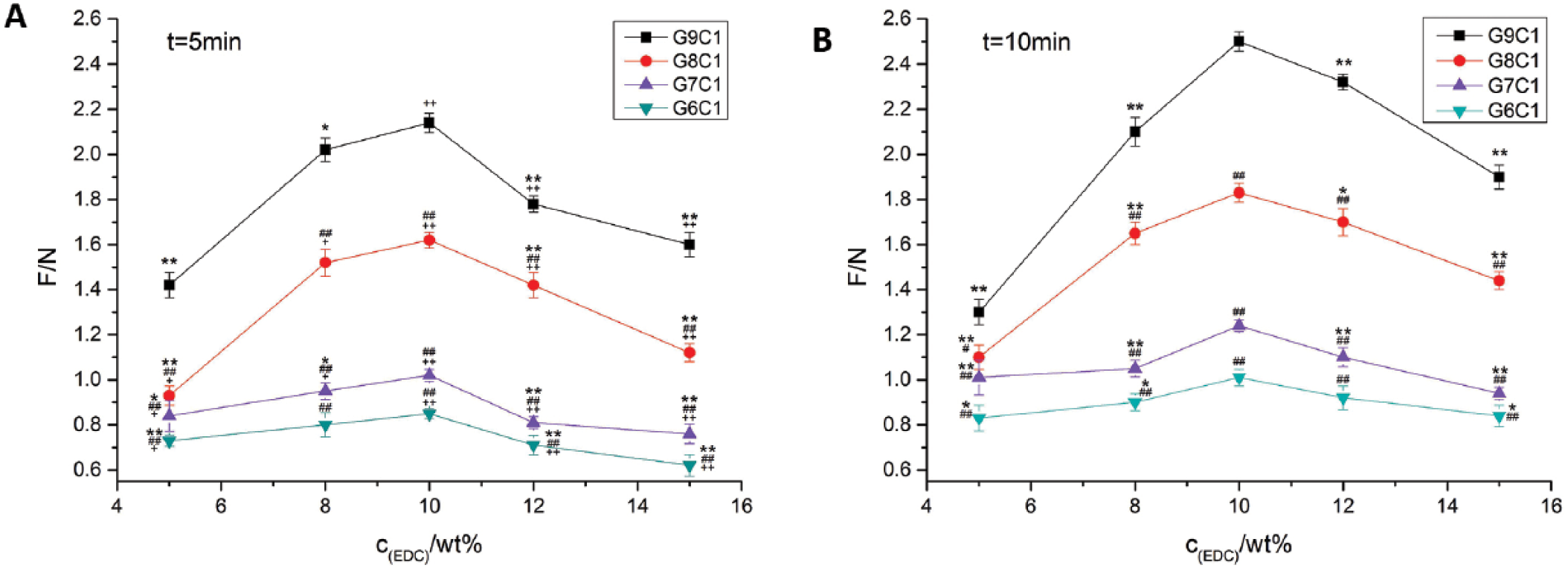
Bond strength curves of tissue glue for different samples and different concentrations of cross-linking agent: (
Evaluation of blood compatibility
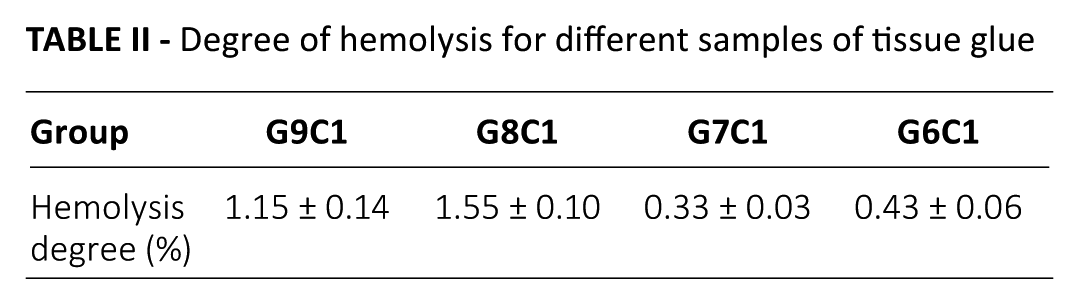
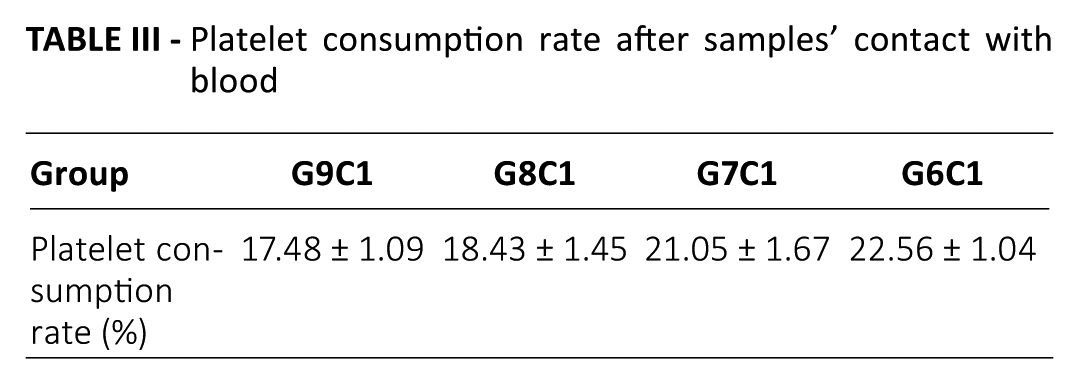
We could conclude that the maximum degree of hemolysis of different samples was 1.55% (Tab. II), which is far less than the 5% standard set by the International Organization for Standardization (ISO) (44). From Figure 4, we see that the BCI values of various proportions of materials showed a downward trend over time, and the BCI values of the biomedical glues were relatively low. Table III shows that the platelet consumption rate of each group was far below 40%, which is in accord with the safety evaluation of medical materials specified by the ISO (44).
Degree of hemolysis for different samples of tissue glue
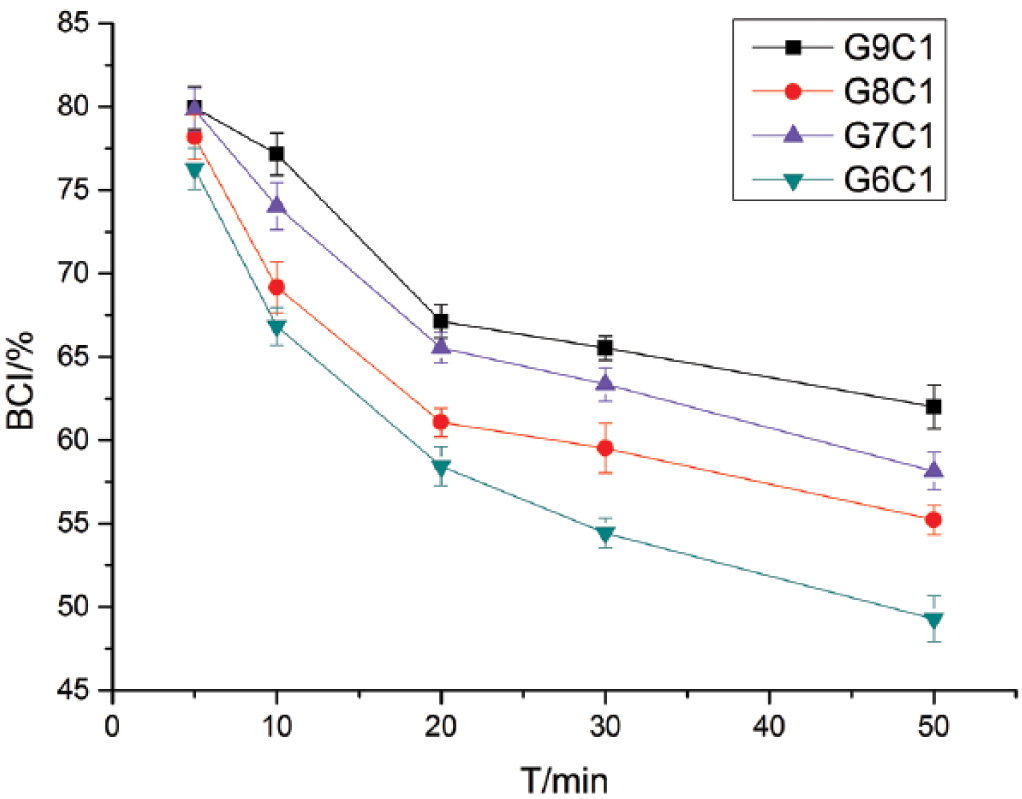
Blood clotting index (BCI) curves for Gel/SS/CMCS tissue glue at different times. CMCS = carboxymethyl chitosan; Gel = gelatin; SS = sericin; T = minutes is the unit of time.
Platelet consumption rate after samples’ contact with blood
Growth status of L-929 cells
The L-929 cells of the experimental groups were demonstrated good growth condition (Fig. 5). There was no large area of cell death or abnormalities. Rather, their morphology was similar to the morphology of normal cell. However, the growth condition of cells in commercially available biological glue was significantly worse, which can be seen from the graph (Fig. 5), showing high levels of cell death and deformation. Thus, it is suggested that the tissue glue had no obvious toxic effect on L-929 cells. Figure 6 shows the OD values for all groups at 490 nm. We can see that the cell growth status of all tissue glue groups was sometimes significantly lower than that of the blank control group, while that of the α-cyanoacrylate group was significantly lower than the control group at all times. Based on the scores for material toxicity (Tab. IV), although the RGR of cells in the experimental group was slightly lower than that in the blank control group, it was still higher than 75% (Tab. V) - within the range of a standard evaluation of cell cytotoxicity (46).
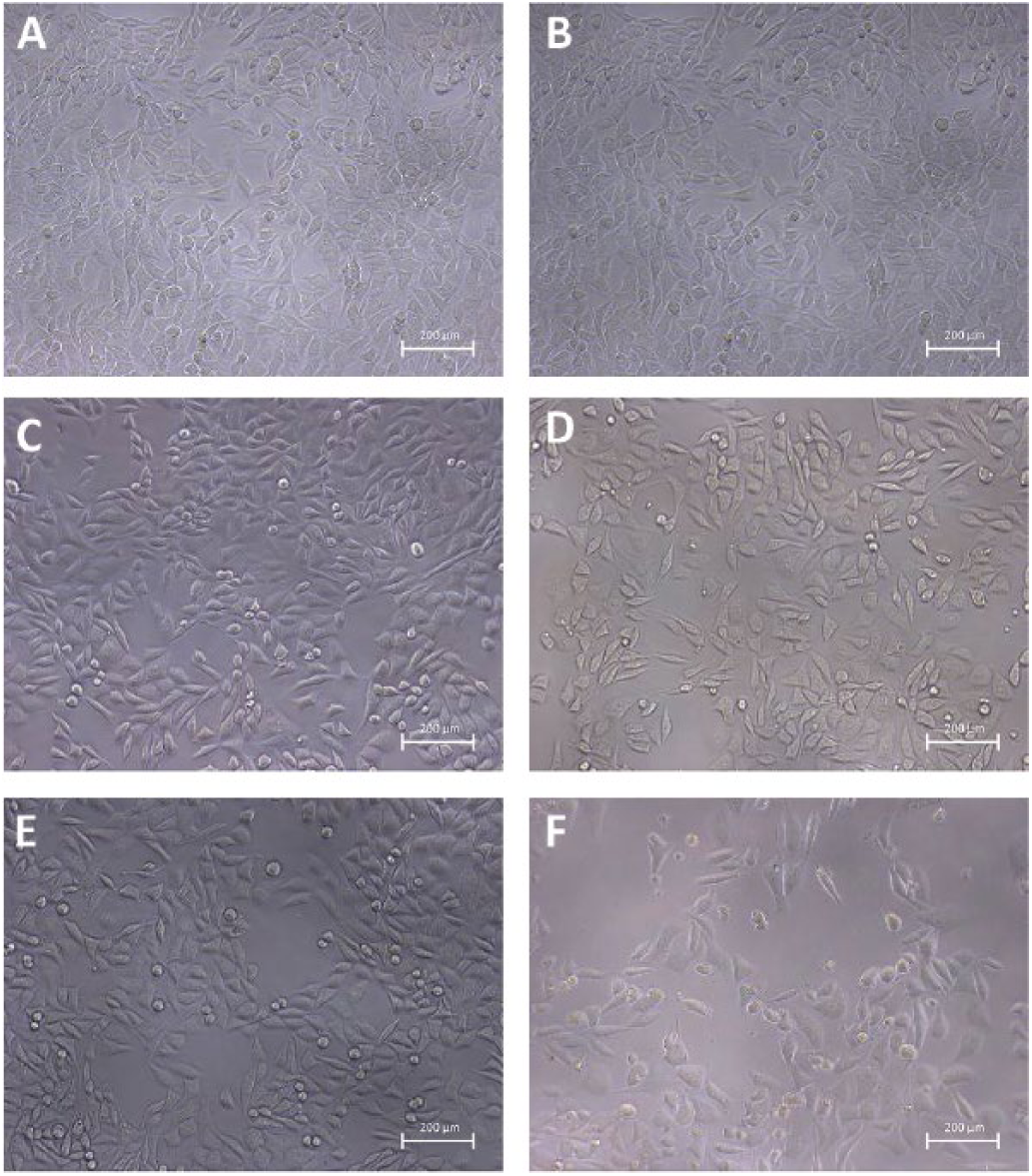
Inverted microscope photographs of L-929 growth morphology in samples after 4 days: (
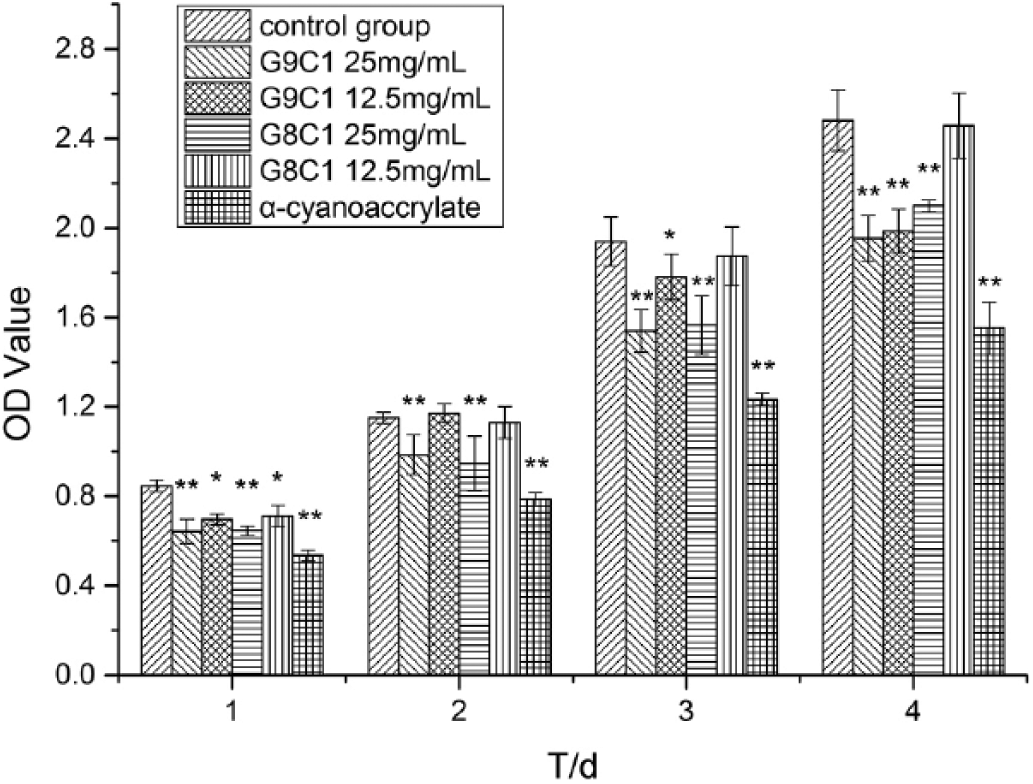
Optical density (OD) values showing growth levels for L-929 cells. All groups were compared with control group (*p<0.05, **p<0.01, vs. control). T = time; d = days.
RGR for different toxicity levels
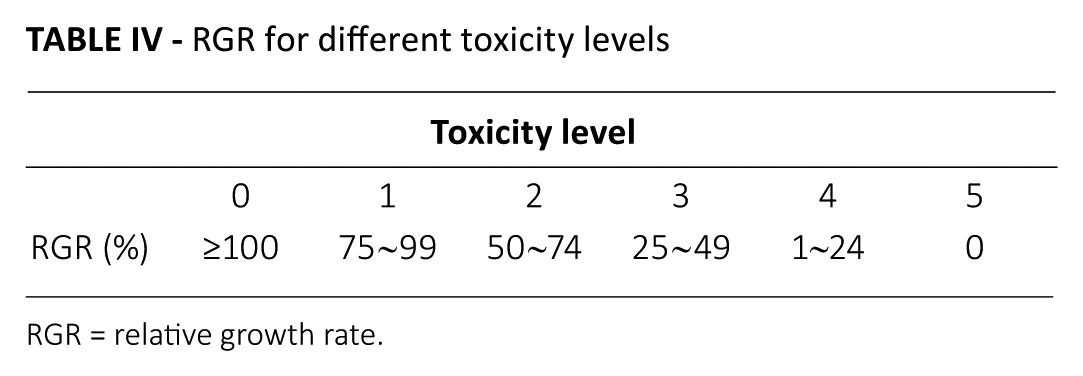
RGR = relative growth rate.
Relative increment rate and toxicity grading of material for L-929 cells
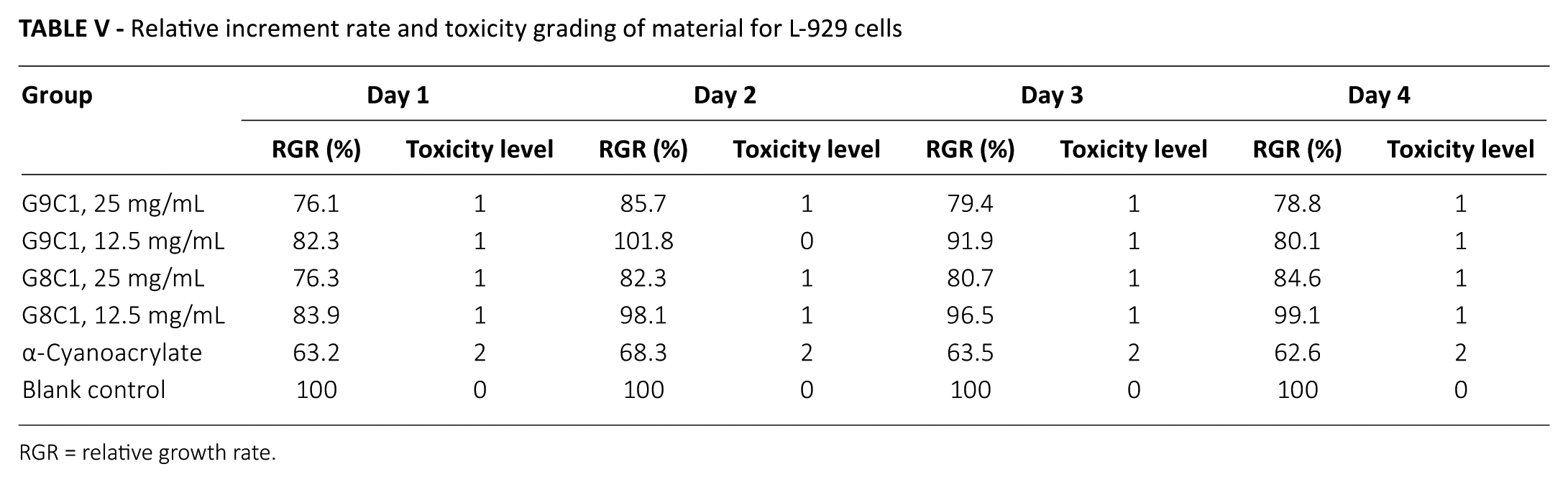
RGR = relative growth rate.
Histological examination
The pathology tissue sections of each organ are shown in Figure 7. With H&E staining, it can be seen that the Cardiomyocytes of experiment groups, like normal cells, are striated and short cylindrical. The nucleus is located in the central of cell, its cell membrane are embedded concave and convex. Intercellular differentiation into desmosomes to help the cells connected to each other. Besides, there were no cell swelling and cell lysis. Similarly, the nucleus of liver cells was normal, and no cells showing edema were found in the experimental groups. The enlargement of the spleen was the most obvious signal of pathological changes, while no tumefaction was found in solenocytes. In addition, lung cells of had clear bubbles, and there was no observed congestion or dark field. Moreover, there was no bleeding, swelling or congestion in glomeruli, which we pay close attention to…
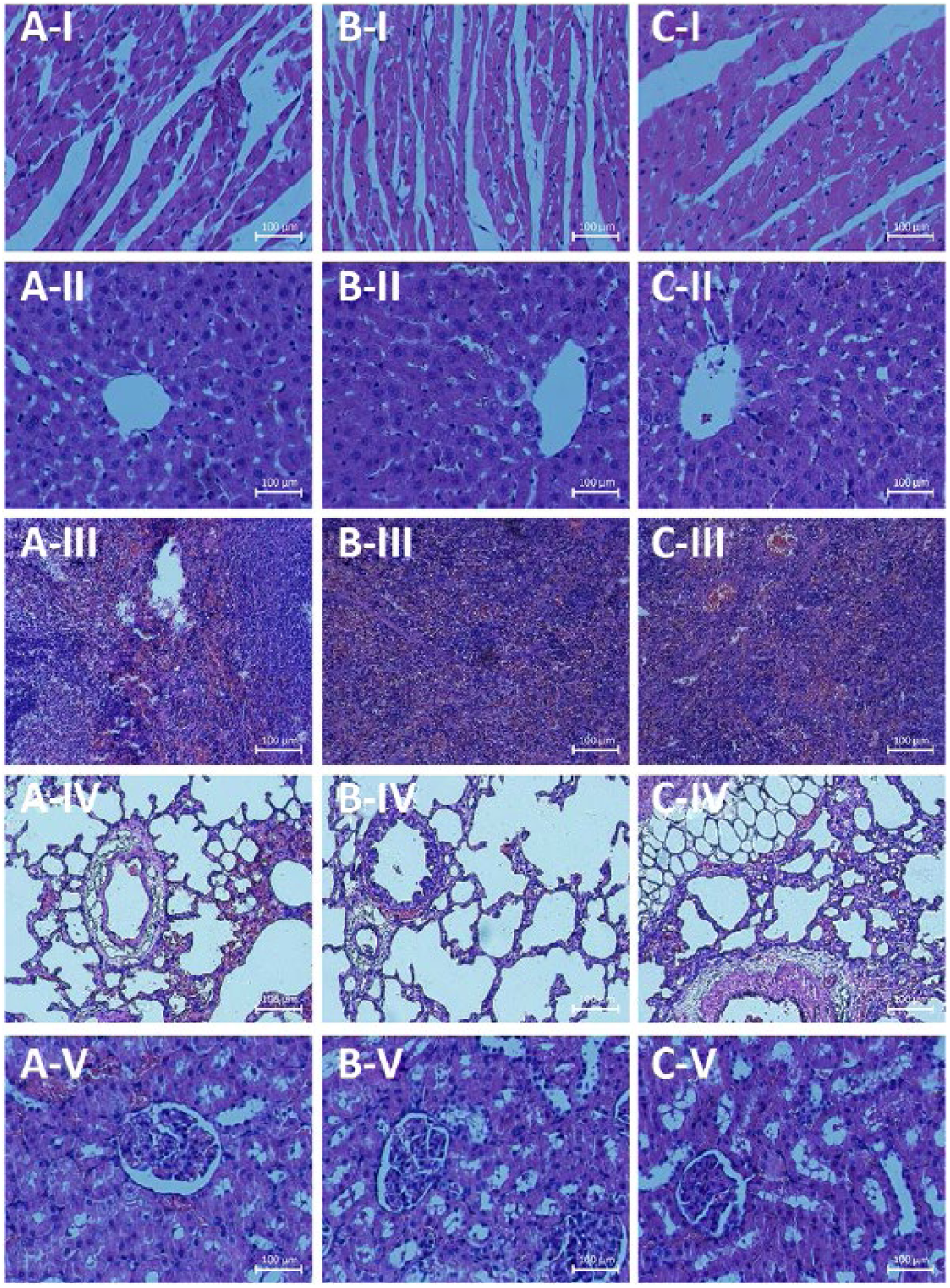
Important organ tissue sections: (
Discussion
Tissue glue is a kind of medical adhesives for inter-tissue adhesions. The tissue glue prepared for this study drew on the idea of tissue engineering, which is mainly used for skin wound adhesion after surgical procedures. It is expected to compensate for the shortcomings of the α-cyanoacrylate medical glue, which is an earlier version of medical adhesive. The aim was to develop a glue that would promote wound healing and repair; reduce complications such as postoperative infection, tissue hyperplasia and necrosis; and further reduce scar formation.
In the case of moderate conditions, the propadiene structure of EDC (R-NC=CN-R) can be used for the activation of -COOH (47). Under the action of EDC, the -COOH in Gel undergoes a condensation reaction to form carboxylic acid anhydride (48), and then combines with the -NH2 in SS and CMCS to form an amide bond. Thus it is cross-linked into a 3-dimensional network structure. The surface of materials we prepared had smooth holes that were uniform and which interpenetrated into each other, which can provide a suitable environment to promote the growth, proliferation and adhesion of cells around the skin wound. This is similar to the scaffold material in tissue engineering. Obviously, if the surface is rough and the holes uneven, it cannot promote cell growth. Thus, both from a section and surface view, the internal structure of the Gel/SS/CMCS mixture is more suitable for promoting growth of cells and providing a possibility for the application of glue to the wound.
Tissue glue requires excellent adhesive strength to tightly bond skin wounds, so the bond strength is one of the important indicators for evaluating its performance. Owing to the fact that Gel is a protein with good stickiness, containing many amino and carboxyl groups, the more Gel content is combined with the carboxymethyl groups of CMCS, the more stable the 3-dimensional network structure that forms will be, thus leading to stronger bond strength.
In addition, the cross-linking reaction of Gel with CMCS begins to occur when Gel is dissolved in an aqueous solution. EDC as an important cross-linking agent for the entire reaction: too high or too low concentration of EDC will affect the bonding strength of the adhesive itself. The present study found that the optimal concentration of EDC was 10 wt%.
At the same time, the curing time can also significantly affect the adhesive strength of the tissue glue. Increasing the curing time can significantly improve the bond strength. Based on the above results, we concluded that with a curing time of 10 minutes and an EDC concentration of 10 wt%, the bond strength of the G9C1 tissue glue would be optimal.
We also tested the bond strength of α-cyanoacrylate medical glue was 2.25 ± 0.05 N. No significant difference between Gel/SS/CMCS tissue glue and α-cyanoacrylate medical glue was found. It can be seen from the result of FT-IR, that the absorption at 3,324 cm-1 indicated the symmetric stretching bands of N-H and O-H (49). Due to the cross-linking between Gel and CMCS, intramolecular hydrogen bonding interactions were enhanced, then vN-H moved to high frequency compared with Gel and CMCS, which caused the excellent bond strength of Gel/SS/CMCS tissue glue.
To date, medical glue used in China has mostly been imported from abroad and is generally expensive, but Gel/SS/CMCS tissue glue could reduce that cost and achieve roughly the same bond strength as α-cyanoacrylate medical glue.
Because the Gel/SS/CMCS tissue glue in this study was mainly applied in the adhesion of skin wound tissue, contact with blood was involved. Therefore, the evaluation of blood compatibility is one of the important indexes in the safety evaluation of medical materials, which includes a hemolysis test, dynamic coagulation test and platelet adhesion test.
A hemolysis test was used to evaluate the influence of long-term contact with human tissue or direct implantation of medical materials and erythrocytes. In the contact with blood, blood stability changes, so it was important to evaluate the hemolysis properties of the materials in vitro by determining the degree of free hemoglobin and erythrocytolysis. When the materials contact with erythrocytes, the less erythrocytes will rupture, and the degree of hemolysis would be lower, which indicates that the impact of erythrocytes to materials is lower. Then the tissue glue is more suitable for wound adhesion. The BCI can be used to reflect the anticoagulant properties of the material directly. The anticoagulant properties and BCI are positively correlated. The BCI value of various proportions of materials showed a downward trend over time, which was related to the procoagulant effect of Ca2+. The BCI value of all groups of Gel/SS/CMCS glue was relatively low, demonstrating that the tissue glue had a good hemostatic effect during wound adhesion and proved that the tissue glue had good biosafety.
The formation of thrombus in blood has a direct relationship with platelet adhesion. A certain amount of platelet adhesion and aggregation occurs on the surface of the material when the blood is in contact with the material for a certain period. The Pc was the consumption rate of platelets by means of measuring the difference in the number of platelets before and after the material was in contact with blood. The higher the consumption rate of platelets, the more severe the platelet adherence to the material, and the greater the possibility of thrombosis occurs, so the material is not suitable for contact with blood.
Because the components in the Gel/SS/CMCS tissue glue are mostly natural proteins or polysaccharides, they can provide nutrition for the growth of L-929. At the same time, the results showed that the cells of the experimental groups emerged in a good growth condition, which is illustrated by the fact that the compound had no toxic or other side effects on the L-929 cells. However, the cells’ growth condition in contact with α-cyanoacrylate was significantly worse. It is possible that α-cyanoacrylate produces heat of polymerization when it contact with water, then some cells are killed by the high temperatures. In addition, it is also important to check the compatibility of the tissue glue with different cell phenotypes, and further studies are needed in this area.
We know that cell necrosis is a passive death due to pathological changes (50). A significant increase in membrane permeability of necrotic cells can lead to cell swelling, then organellar deformation or enlargement. In the early stage, the cell morphology did not change significantly, but later the cells would burst. In addition, necrotic cells will release inclusions when they undergo lysis, and this frequently causes inflammatory reactions.
When the body is subjected to a sudden acute injury or irritation and the structure of the cell is destroyed immediately, then a severe necrotic reaction occurs (51). The pathology sections of the 5 important organs of the experimental animals were examined to observe any cell necrosis in the experimental group, and then to evaluate the systemic acute toxicity of the Gel/SS/CMCS tissue glue. The pathology sections of the 5 organs from the experimental groups displayed normal conditions; they did not appeared swollen; with dark areas or ruptures; or with dissolution and errhysis of nuclear or other pathological lesions, which is similar to the morphology of normal tissue. These results showed that there were no tissue lesions in important organs of rats with the systemic acute action of Gel/SS/CMCS tissue glue, and that therefore the tissue glue was nontoxic and biosafe.
Conclusions
In the present study, we developed a low-cost medical tissue glue with good biocompatibility. From the characterization results, we know that there was generation of amide bonds, and that the surface of the tissue glue was smooth and had a porous structure in cross-section. The holes communicated with each other, which could be conducive to cell adhesion and growth. The sample of G8C1 was better than G9C1. There was no obvious difference in bond strength between the Gel/SS/CMCS and α-cyanoacrylate medical glues. The Gel/SS/CMCS glue had good structural characteristics and bond strength – also at a reduced the cost.
We evaluated the biological safety of medical tissue glue and examined its toxicity and biocompatibility. We demonstrated that the tissue glue had no significant toxicity in vitro, the pathology sections of each organ in contact with the glue were normal, and it demonstrated excellent biocompatibility with L-929 cells.
In summary, this new tissue glue is suitable for medical applications, with minimal toxicity and outstanding biocompatibility, has good bond strength and can reduce costs. Therefore, we expect that the tissue glue we prepared can be applied in clinical practice to reduce surgical skin scars, but other properties of the tissue glue such as compatibility with different cell phenotypes, effects on scar reduction in animal skin wound models and whether it can evoke a nonphysiological inflammatory responses need to be further characterized in further research to justify its clinical application.
Footnotes
Disclosures
Financial support: Chongqing Science & Technology Commission Project (cstc2016shmszx0635).
Conflict of interest: None of the authors has any financial interest related to this study to disclose.
