Abstract
Background
The aim of this study was to investigate the effects of storage medium and aging duration on Martens hardness (HM) and indentation modulus (EIT) of self-adhesive resin-based cements (SARCs).
Methods
A total of 416 discs were fabricated from 8 SARCs (n = 52 per SARC): (i) BeautyCem (BEA), (ii) Bifix SE (BIF), (iii) Clearfil SA Cement Automix (CLE), (iv) RelyX Unicem2 Automix (RXU), (v) SeT (SET), (vi) SmartCem 2 (SMC), (vii) SoloCem (SOC) and (viii) SpeedCEM (SPC). The specimens were ground and stored in (a) physiological saliva, (b) artificial saliva, (c) sodium chloride and (d) distilled water, at 37°C for 1, 7, 14, 28, 90 and 180 days. Non-aged specimens (3 hours after photo-initiation) of each SARC acted as control groups. HM and EIT were assessed using a universal hardness testing machine. Data were analyzed using Kolmogorov-Smirnov and Kruskal-Wallis tests and paired t-test, and 3-, 2- and 1-way ANOVA with post hoc Scheffé test (p<0.05).
Results
SARC materials exerted the highest influence on HM and EIT values (p<0.001, partial eta squared [ηP²] = 0.753 and 0.433, respectively), closely followed by aging duration (p<0.001, ηP² = 0.516 and 0.255) and storage medium (p<0.001, ηP² = 0.043 and 0.033). The interaction effect of the combinations of the 3 independent parameters was also significant (p<0.001, ηP² = 0.163 and 0.133). The lowest initial HM and EIT was presented by CLE, followed by SET and SPC; highest HM was for BIF, followed by RXU and SMC. SET gave a greater HM and EIT percentage decrease than SOC, SPC, BEA, SMC, RXU or CLE.
Conclusions
Aging duration is a major factor affecting the micromechanical properties of SARCs, while storage medium was shown to have a significant but minor role.
Keywords
Introduction
The longevity of an indirect restoration depends on the intrinsic stability of the restorative materials, the luting type and composite and the properties of the luting agent (1, 2). All parameters combine to form an entity and guarantee the reliability of the overall system. Ceramic restorations are nowadays increasingly used with adhesive systems (3). Data from in vitro studies provide evidence for good long-term bond strengths with self-adhesive resin-based cements (SARCs) when a correct pretreatment of the restoration and the hard tooth tissues is completed. The mechanical properties of these materials have already been investigated (4-5-6-7-8-9-10-11). The imitation of clinical aging, however, is still challenging. Therefore various aging methods have been used, imitating changes in temperature during food intake as well as specific environmental conditions (12, 13).
Generally, 99% of natural saliva is water, with additional organic and inorganic components. The organic components consist of more than 1,000 different types of proteins (e.g., enzymes such as lactoferrin, mucin or glycoproteins) and urea (14-15-16). Moreover, there are specific esterases (e.g., cholesterol esterase), which may negatively affect the mechanical properties of bisphenol-A-diglycidylether dimethacrylate (BisGMA)– and triethyleneglycol dimethacrylate (TEGDMA)–based resin composites (17-18-19). Therefore, natural saliva significantly differs in its composition compared with the most commonly used artificial saliva solutions (20). As a medium, natural saliva leads to higher solubility of polymers than artificial saliva, distilled water or sodium chloride (13). The solubility is also affected by the affinity of the material to absorb water. In general, SARCs do absorb water to some extent. This phenomenon depends on the chemical composition of the matrix, the type and proportion of filler particles, the degree of monomer conversion, the molecular architecture, any defects and the intraoral moisture level (21-22-23).
Conventional polymer matrices in resin composites are based on dimethacrylates such as BisGMA, urethane dimethacrylate (UDMA) and TEGDMA, and the SARC matrix is almost identical in structure with these. Besides conventional monomers, SARCs contain additional monomers with acidic groups, such as phosphoric acid esters or carboxylates. The role of acidic monomers is to form a chemical bond with the calcium ions of the hydroxyapatite (24, 25), resulting in a demineralization of the hard tooth tissues (26, 27). Moreover, the acidic groups of monomers chelate the calcium ions of the hydroxyapatite in the demineralized smear layer of the dentin or enamel surfaces (5). This reaction mechanism facilitates an improved bond to the tooth tissue, in contrast to the single micromechanical bond (24, 26).
The improved translucence of SARCs is a further benefit compared with traditional cements. SARCs therefore provide the option to fix restorations in the esthetic zone also in abutment teeth with reduced retention shape. Furthermore, the improved tolerance for humidity reduces the risk of postoperative sensitivity of the abutment teeth (28).
However, to date there is only a little information available regarding their long-term mechanical stability in relation to the storage medium. Therefore, the purpose of this study was to assess the effect of the aging medium (natural and artificial saliva, sodium chloride and distilled water) on 8 different SARCs, with regard to Martens hardness (HM) and elastic indentation modulus (EIT) for storage times up to 180 days.
The tested null hypotheses were:
All SARCs would demonstrate comparable values with respect to HM and EIT parameters over 180 days of storage in different media;
The storage time would have no effect on the HM and EIT parameters of the SARCs over 180 days of storage in different media;
The choice of storage medium would have no effect on the HM and EIT parameters of the SARCs over 180 days of storage in different media.
Materials and Methods
Specimen preparation and aging procedure
A total of 416 discs (diameter: 12 mm, thickness: 1.5 mm ± 0.05 mm) were fabricated out of 8 different SARC materials (n = 52 per SARC) as summarized in Table I. For fabrication, the SARCs were filled in a standardized silicone form (silicone: Heraform RS, type A and B, dark green and white; Heraeus Kulzer, Hanau, Germany) and overlapping light cured (Elipar S10; 3M) according to DIN EN ISO 4049:2010-03. The irradiance of the curing light was 2,066.4 (± 9.5) mW/cm2 (mean of 5 measurements on a spectrophotometer with a 4-mm diameter sensor; MARC resin Calibrator; BlueLight Analytics Inc., Halifax, Canada), while the exposure distance was 1.5 mm. Light curing was performed for 30 seconds in total 9 times in a circle, beginning in the middle of each specimen and continuing in 8 overlapping steps around the peripheral zones. All discs were ground and polished with a series of silicon carbide papers (SiC) up to P4000 at 150 rpm each paper for 10 seconds under constant water cooling (Abramin machine; Struers, Ballerup, Denmark). Between each step, specimens were stored in a black box and were randomly divided into 4 subgroups, according to the following storage medium (n = 13 per medium and per SARC):
Summary of products (in alphabetical order), abbreviations, manufacturers, lot numbers and material compositions
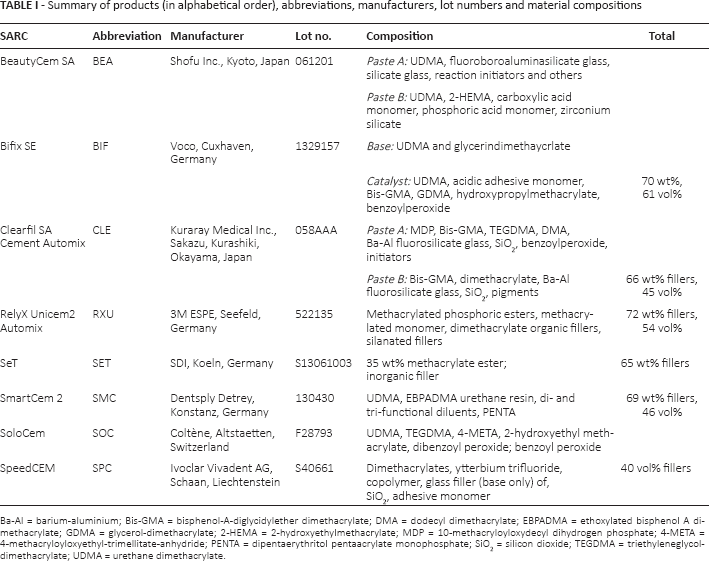
Ba-Al = barium-aluminium; Bis-GMA = bisphenol-A-diglycidylether dimethacrylate; DMA = dodecyl dimethacrylate; EBPADMA = ethoxylated bisphenol A dimethacrylate; GDMA = glycerol-dimethacrylate; 2-HEMA = 2-hydroxyethylmethacrylate; MDP = 10-methacryloyloxydecyl dihydrogen phosphate; 4-META = 4-methacryloyloxyethyl-trimellitate-anhydride; PENTA = dipentaerythritol pentaacrylate monophosphate; SiO2 = silicon dioxide; TEGDMA = triethyleneglycol-dimethacrylate; UDMA = urethane dimethacrylate.
Physiological saliva (pH 6.8): Naturally extracted saliva was collected from 10 healthy individuals with natural dentition having no active caries or periodontal damage. They abstained from food and beverage intake 2 hours prior to the saliva donation.
Artificial saliva (pH 4.7): Formulated from KCL 0.4 g/L, NaCl 0.4 g/L, CaCl2, 2H2O 0.906 g/L, NaH2PO4, 2H2O 0.690 g/L, Na2S, 9H2O 0.005 g/L and urea 1 g/L (29).
Sodium chloride (pH 5.7): NaCl; physiological salt solution 0.9%, (B. Braun, Melsungen, Germany).
Distilled water (pH 6.7): Aqua Bidest (Kerndl, Weissenfeld, Germany).
The storage in all 4 different media was performed at a constant temperature of 37°C, and the storage medium was changed every 14 days (HERA cell 150; Thermo Scientific, Heraeus, Hanau, Germany). On the day of testing, every specimen was gently wiped with dry filter paper on both sides and air-dried with oil-free air for 15 seconds before measurements. Further, scanning electron microscope images were made to characterize the filler particles.
Universal hardness measurements: HM and EIT
HM and EIT were measured with a universal hardness testing machine (Zwick/Roell ZHU 0.2/Z2.5; Zwick, Ulm, Germany) which analyzed both the elastic and the plastic deformation. Load/unload and penetration depth of the indenter were recorded during the dynamic measurement process (30). The specimens were measured at 3 hours post polymerization as well as after 1, 7, 14, 28, 90 and 180 days of aging. The diamond indenter pyramid (α = 136°) of the hardness testing machine was pressed vertically into the specimen with a load of 10 N for 20 seconds. The test force and the indentation depth (penetration depth maximum of 0.05 mm) were measured during the test procedure at increasing as well as decreasing force. The result of the test is the relation between test force and the relevant indentation depth. Three individual indentations were performed on each specimen. The HM (also known as universal hardness [HU]) is defined as the test force divided by the apparent area of indentation under the applied test force.
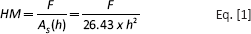
where HM is the Martens hardness (N/mm2), F is the test force (N) and AS(h) is the surface area of the indenter at distance h from the tip (mm2).
The indentation modulus was determined from the slope of the tangent adapted at the beginning (at maximum force) of the nonlinear indentation depth curve upon unloading (TestXpert V12.3 Master; Zwick) and calculated with the following equation (DIN EN ISO 14577) (31):
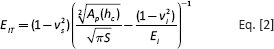
where EIT is the elastic indentation modulus of the indenter (Vickers pyramid) (kN/mm2), νs is Poisson's ratio of the specimen and νi is Poisson's ratio of the indenter.
The additional percentage decrease during the 180 days of storage was calculated according to the following equation:

where p is the percentage (%), W is the percentage value (HM and EIT values after 180 days of storage) and G is the basic value (initial HM and EIT value).
Statistical Analysis
For power analysis, 5 specimens of a SARC (Clearfil SA Cement; Kuraray Medical Inc., Sakazu, Japan) were fabricated, and their HM was measured before aging. To assess the effect of aging, the results from a prior study on composite resins were additionally used (nQuery Advisor, version 6.0; Statistical Solutions, Saugus, MA, USA) (32). The power analysis aimed to find a longitudinal impact of the storage level on HM. For a sample size of 10, a single group-paired t-test with a 0.05 2-sided significance level will have 99% power to detect HM = 80 N/mm² at 180 days, assuming that the standard deviation of HM is 31. In addition, the sample size was determined able to find cross-sectional differences between the tested storage media. A sample size of 10 was identified to have a power of 97% to detect a difference of 100 N/mm² in mean HM assuming that the common standard deviation of HM is 43. For this calculation, a 2-group t-test with a Bonferroni corrected 2-sided significance level equal to 0.008 was used. The measured data were analyzed using the Kolmogorov-Smirnov test, Kruskal-Wallis test, paired t-test and 3-, 2- and 1-way ANOVA, together with the post hoc Scheffé test. A high value of the partial eta-squared (ηP²) indicates an elevated amount of explained variance by a factor. The results of the statistical analyses with p values smaller than 0.05 were interpreted as statistically significant. Data were analyzed with SPSS version 22.0 (IBM, Armonk, NY, USA).
Results
Choice of SARC exerted the highest influence on HM and EIT values (p<0.001, ηP² = 0.753 and 0.433, respectively), closely followed by aging duration (p<0.001, ηP² = 0.516 and 0.255) and storage medium (p<0.001, ηP² = 0.043 and 0.033). The interaction effect of the combinations of the 3 independent parameters (SARC, storage medium and aging duration) was also significant (p<0.001, ηP² = 0.163 and 0.133).
Scanning electron microscope (SEM) images of the 8 different SARCs are presented in Figure 1. Differences in filler size and shape were detectable, independent of filler percentage. The largest maximum filler size was identified for SMC, followed by CLE, SOC, SPC, BIF, RXU, SET and BEA.

Scanning electron microscope (SEM) images of the 8 different self-adhesive resin-based cements (SARCs): BEA = BeautyCem; BIF = Bifix SE; CLE = Clearfil SA Cement Automix; RXU = RelyX Unicem2 Automix; SET = SeT; SMC = SmartCem 2; SOC = SoloCem; SPC = SpeedCEM.
Impact on HM and EIT of differences in non-aged SARCs
The detailed HM and EIT results for non-aged SARCs (all descriptive statistics and standard deviations) are presented in Table II. The significantly lowest HM was for CLE (p<0.001), followed by SET and SPC; the significantly highest HM was for BIF (p<0.001), followed by RXU and SMC. With respect to EIT for non-aged specimens, the significantly lowest values (p<0.001) were obtained for CLE, followed by SET, SPC, RXU, BEA, SMC and SOC.
Martens hardness (HM) and indentation modulus (EIT) values for the self-adhesive resin-based cements (SARCs), tested on non-aged specimens, shown in descending order
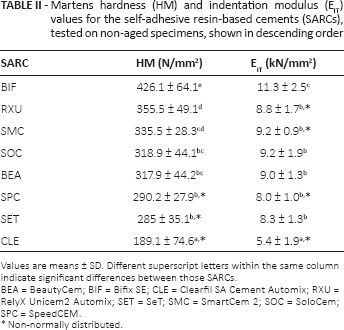
Values are means ± SD. Different superscript letters within the same column indicate significant differences between those SARCs.
BEA = BeautyCem; BIF = Bifix SE; CLE = Clearfil SA Cement Automix; RXU = RelyX Unicem2 Automix; SET = SeT; SMC = SmartCem 2; SOC = SoloCem; SPC = SpeedCEM.
Non-normally distributed.
Impact of aging duration on HM and EIT after 180 days of storage
For BIF, SOC and SPC, no impact of aging duration on HM (BIF: p = 0.579; SOC: p = 0.799; SPC: p = 0.188) or EIT (BIF: p = 0.233; SOC: p = 0.764; p = 0.068) was identified. For BEA, an impact of aging duration on HM (p = 0.001), but not on EIT (p = 0.057) was observed, as presented in the boxplots for all tested SARCs in Figure 2.
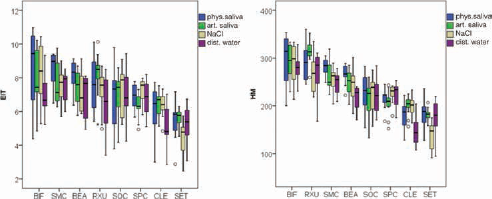
Boxplots of indentation modulus (EIT; kN/mm2) and Martens hardness (HM; N/mm2) values in descending order, for all 8 tested self-adhesive resin-based cements (SARCs) in the 4 different media: physiological saliva, dist. water, artificial saliva and sodium chloride, at a total storage time of 180 days. BEA = BeautyCem; BIF = Bifix SE; CLE = Clearfil SA Cement Automix; RXU = RelyX Unicem2 Automix; SET = SeT; SMC = SmartCem 2; SOC = SoloCem; SPC = SpeedCEM.
Impact of storage medium on HM and EIT after 180 days of storage
For CLE, RXU, SET and SMC, storage medium showed a significant impact on HM and EIT (p<0.021). Detailed HM and EIT results after 180 days of storage are shown in Figure 2: BEA and SMC specimens stored in distilled water showed significantly lower HM than those stored in physiological saliva (BEA: p<0.001; SMC: p<0.008). RXU presented significantly lower HM (p = 0.017) for storage in sodium chloride than in artificial saliva and significantly lower EIT (p = 0.031) for storage in distilled water than in artificial saliva. CLE showed significantly lower HM in distilled water than in artificial saliva (p<0.001), sodium chloride (p<0.001) or physiological saliva (p = 0.015), and significantly lower EIT values in distilled water than in artificial saliva (p = 0.004) and sodium chloride (p = 0.003). SET stored in sodium chloride presented significantly lower HM values than when stored in distilled water (p = 0.001), artificial saliva (p = 0.002) or physiological saliva (p = 0.009), and significantly lower EIT in sodium chloride than in physiological saliva (p = 0.047) or artificial saliva (p = 0.023).
Impact of 180 days of storage on HM and EIT(difference of 180 days – initial values)
BEA (p = 0.139), RXU (p = 0.314) and SMC (p = 0.769) stored in physiological saliva as well as CLE (p = 0.376) and SOC (p = 0.744) stored in sodium chloride showed no impact of storage. Figure 3 presents in detail all results for decreases in HM and EIT and therefore the impact for all tested SARCs in the 4 different media, as the difference between 180 days and the initial values.
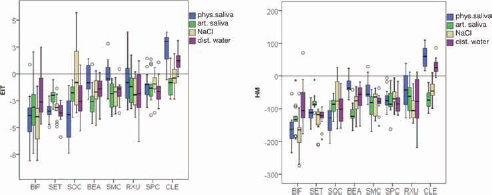
Boxplots of indentation modulus (EIT; kN/mm2) and Martens hardness (HM; N/mm2) values in ascending order, for the 8 tested self-adhesive resin-based cements (SARCs) in the 4 different media: physiological saliva, dist. water, artificial saliva, and sodium chloride, as the difference between the results at 180 days storage and the initial values. BEA = BeautyCem; BIF = Bifix SE; CLE = Clearfil SA Cement Automix; RXU = RelyX Unicem2 Automix; SET = SeT; SMC = SmartCem 2; SOC = SoloCem; SPC = SpeedCEM.
Percentage decrease among different SARCs
SET showed a significantly higher percentage decrease than did SOC, SPC, BEA, SMC, RXU or CLE, with respect to HM (p<0.042) and EIT(p<0.013). In addition, SOC presented a significantly higher percentage decrease compared with RXU and CLE (p<0.004), as well as RXU compared with CLE (p<0.001) for HM. SOC, BEA, SMC, SPC and RXU showed significantly higher percentage decreases than CLE with respect to EIT (p<0.001) (Fig. 4).
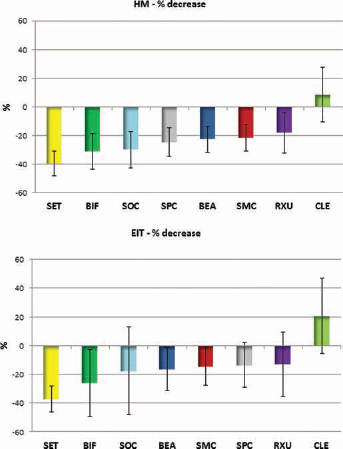
Martens hardness (HM) and indentation modulus (EIT) percentage decreases in ascending order, for all self-adhesive resin-based cements (SARCs), with results (with standard deviations) for each SARC, pooled for all media. BEA = BeautyCem; BIF = Bifix SE; CLE = Clearfil SA Cement Automix; RXU = RelyX Unicem2 Automix; SET = SeT; SMC = SmartCem 2; SOC = SoloCem; SPC = SpeedCEM.
Percentage decrease among different media
Storage in sodium chloride or artificial saliva showed a significantly higher percentage decrease than storage in distilled water or physiological saliva, and further, a significantly higher percentage decrease for distilled water compared with physiological saliva, with respect to HM (p<0.004). Storage in artificial saliva presented a significantly higher percentage decrease for EIT compared with storage in physiological saliva (p = 0.008). All detailed percentage decrease values for all SARCs in the different storage media are presented in Table III and Figure 5.
Martens hardness (HM) and indentation modulus (EIT) percentage decreases between 180 days storage and initial results, for self-adhesive resin-based cements (SARCs) in each storage medium
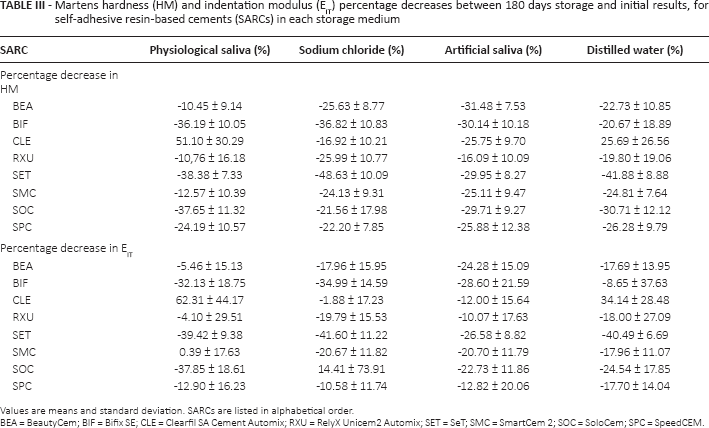
Values are means and standard deviation. SARCs are listed in alphabetical order.
BEA = BeautyCem; BIF = Bifix SE; CLE = Clearfil SA Cement Automix; RXU = RelyX Unicem2 Automix; SET = SeT; SMC = SmartCem 2; SOC = SoloCem; SPC = SpeedCEM.
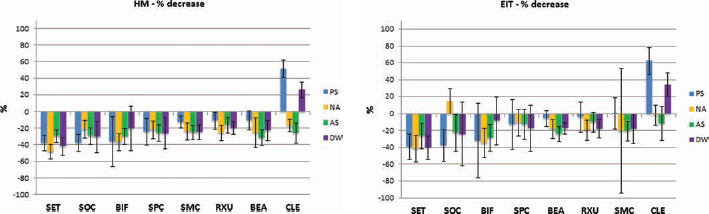
Martens hardness (HM) and indentation modulus (EIT) percentage decreases in ascending order, for all self-adhesive resin-based cements (SARCs), for each medium, with standard deviations (whiskers). PS = physiological saliva; NA = sodium chloride; AS = artificial saliva; DW = distilled water; BEA = BeautyCem; BIF = Bifix SE; CLE = Clearfil SA Cement Automix; RXU = RelyX Unicem2 Automix; SET = SeT; SMC = SmartCem 2; SOC = SoloCem; SPC = SpeedCEM.
Discussion
SARCs are becoming more and more popular for use in clinical practice due to the simple handling required and the improved bond strength to the hard tooth substance in comparison with conventional luting materials. In this technique, however, the restoration margins with the adhesive gap as well as the restoration materials are exposed to aging in the oral cavity, by food and natural saliva.
Among the materials analyzed, CLE presented the lowest initial HM and EIT values, whereas the highest initial values were observed with BIF. Therein, there was evidence of a direct correlation between the hardness parameters and filler content of the SARCs. The higher the percentage filler content (BIF: 61 vol%; RXU: 54 vol%), the higher the recorded initial hardness parameters. Thus, CLE (45 vol% filler), followed by SPC (40 vol% filler), exhibited the lowest hardness parameters and lowest filler content. The effect of filler size on mechanical properties is, however, difficult to assess with different inorganic filler amounts. SEM images identified larger maximum filler particle size in CLE (approx. 30 µm) than in BIF (approx. 15 µm) (Fig. 1).
In this study, a reduction of the HM and EIT values for the different SARCs was observed after 180 days of storage. The exception to this behavior was CLE, where an increase in mechanical properties with aging in physiological saliva or distilled water was observed, and generally the exception held when the results for storage in all media were pooled. The possible explanation for this behavior might be the composition of CLE, which has a lower filler percentage and with a larger filler size and therefore a higher matrix content. Consequently, the bonding surface interface of the filler and matrix is lower and might lead to this stability.
These specific matrix monomers are known for their hydrophilicity, and they may absorb liquid over the course of their storage (12, 33-34-35). The solvent absorption increases with a higher proportion of organic matrix and consequently a lower proportion of filler particles. In addition, the chemical composition of the monomers determines the solvent sorption, while increased hydroxyl groups or TEGDMA content in the matrix is related to an increased water sorption (12, 33-34-35). This could not be confirmed in this present study. An association of the hardness parameters and the filler particle and matrix compositions with respect to their long-term stability was not possible, due to a lack of information regarding the exact chemistry of some products. Differences have already been determined for RXU, SMC and CLE with respect to the micromechanical properties within the different SARCs with the same ranking (36), but the study methodology and aging was different. In summary, significant differences were observed between the SARCs. Therefore, the first null hypothesis must be rejected.
Confirming an earlier study with aging in distilled water, the most significant changes in mechanical properties were found during the first 30 days of immersion, in all media (37). At longer storage duration, the hardness parameters were preponderantly maintained. In this study, storage duration longer than 30 days affected only the mechanical properties of BEA. Regarding the filler particle sizes (Fig. 1), BEA exhibited the smallest filler particle sizes (approx. 6 µm). This implies a larger filler–matrix interface, which is more prone to degradation, as observed in a microhybrid and several nanohybrid composites (23, 38-39-40). It might be possible in future Martens hardness studies, based on the results achieved here, to reduce the aging time of 6 months in in vitro studies, due to the significant changes only within the first 30 days. However, it would be important to accurately validate this in further studies. The second null hypothesis could therefore be rejected, because the storage time showed a significant effect on the hardness parameters.
In general in this study, the hardness parameters of the SARCs were affected by the composition of the individual storage media. Apart from water, human saliva consists of diverse protein types (14-15-16, 41). It is known that specific proteins – e.g., esterases – lead to a deterioration of the hardness parameters of BisGMA- and TEGDMA-based composites (17-18-19, 42). In general, the chosen storage medium in the present study showed a significant effect on the HM and EIT values of all SARCs; however, due to the complexity of the results, it was difficult to identify a association between these parameters. It must be emphasized that lower HM parameters were observed after storage in distilled water than in the other 3 media, including natural saliva. Moreover, there was a larger reduction of both hardness parameters in sodium chloride and artificial saliva than in distilled water and natural saliva. The additional specific proteins in human saliva do not appear here to have had a significant negative effect on the surface hardness. CLE as the only SARC that showed even an increase in mechanical properties during storage in human saliva.
A main emphasis of this study was to assess the effects of storage in natural saliva, as an important step in approaching in vitro the conditions in the oral environment. A significant bacterial colonization and spore formation, as well as the development of an unpleasant odor, was observed in this test during the storage of the test samples. Severe bacterial contamination normally leads to an additional negative effect on the surface properties (18, 43). This could be reduced by a more frequent exchange of the media, which happens physiologically in the oral cavity with natural saliva. Moreover, human saliva is different in every individual and shows a strong variation even within a single day (14, 41). The natural saliva used in the present study was collected in the morning from participants in a fasting state. A different time of collection could have led to different study results. The SARCs were principally stored at a constant temperature of 37°C regardless of the storage medium. The intraoral temperature on food intake may be subject to significant variations; therefore, this point may be regarded as a limitation of the study and requires more detailed analysis in further studies. It was possible to reject the third hypothesis by confirming the effect of the storage medium.
The SARCs were polymerized for 30 seconds. Due to these ideal curing conditions and a sufficient exposure time based on the use of a calibrated high irradiance curing unit, the in vitro study conditions might have differed from those in a clinical situation, where a precise and close placement of the cutting unit is difficult intraorally, especially in approximal areas. Further, it must be emphasized that the first measurements were done at 3 hours post polymerization. Therefore, the post polymerization may have already been completed by the time of the first measurement, and it may have been possible that the measurements were not evident that would have explained why differences between the initial (3-hour) and the 24-hour measurements could not be analyzed, comparison with other studies (37, 39). Even though all test samples were stored in absolute darkness between the individual fabrication steps, the SARCs have dual hardening properties, where the polymerization occurs even without further light exposure. Reducing the elapsed time until performing the initial measurement or a change of the light exposure could thereby have affected the results. Therefore, further studies must be performed, which place more emphasis on the polymerization during the initial period.
The final data of the present study were used for a post hoc power analysis of the longitudinal impact of storage level on HM change. Therefore, when the sample size was 13, a single group paired t-test with 2-sided significance level of 0.05 will have a 99% power to detect an HM change of 80 at 180 days, assuming that the standard deviation of HM was 45. Further, the cross-sectional differences between the 4 tested storage media after 180 days were evaluated. A sample size of 13 in each group would have a 59% power to detect a difference in a HM mean of 50 (according to the observed data) assuming that the common standard deviation of HM is 41 using a 2-group t-test with a Bonferroni-corrected 2-sided significance level equal to 0.008.
Cross-sectional differences after 180 days between the 8 cements tested were also analyzed. A sample size of 13 in each group would have a 98% power to detect a difference in an HM mean of 100 (according to the observed data) assuming that the common standard deviation of HM is 41 using a 2-group paired t-test with a Bonferroni-corrected 2-sided significance level equal to 0.001. Our design of the present study was quite satisfactory, as the estimates for real data (observed standard deviations and observed effects) and the assumed ones were comparable. In general, the power analysis was calculated for HM values. Since smaller standard deviation estimates for EIT values were found, it can be assumed that the power analysis also applied to them.
Conclusions
Within the limitations of this in vitro study, it can be concluded that:
Natural saliva showed no significantly different effect on the surface hardness compared with other storage media.
Storage in natural saliva led to bacterial colonization and spore formation on the specimen surfaces.
Initial hardness parameters were related to the filler content of the SARC. The higher the filler content, the higher the HM and EIT.
A reduction of hardness parameters was identified in all SARCs within the 180-day storage time, with the exception of CLE.
Most of the significant changes of the hardness parameters were identified within the first 30 days of storage in all media.
Footnotes
Acknowledgements
The authors would like to thank Shofu, Voco, Kuraray, 3M ESPE, SDI, Dentsply Detrey, Coltène and Ivoclar Vivadent for their support in providing the materials.
Financial support: No grants or funding have been received for this study.
Conflict of interest: None of the authors has any financial interest related to this study to disclose.
