Abstract
Introduction
The need for human cornea tissues continues to grow as an alternative option to donor tissues. Silk protein has been successfully used as a substrate to engineer corneal epithelium and stroma in vitro. Herein, we investigated the in vivo response and the effect of silk crystalline structure (beta sheet) on degradation rate of silk films in rabbit multipocket corneal models.
Methods
Three different surgical techniques (peripheral-median P-M, central-superficial C-S, central-deep C-D) were used to assess the in vivo response as well as the degradation profile of silk films with low, medium and high beta sheet (crystalline) content at 2 and 3 months after surgery.
Results
Approach C-D showed signs of sample degradation without inflammation, with one single incision and a pocket created by flushing air two thirds deep in the corneal stroma. In comparison, approaches P-M and C-S with multiple incisions presented manually dissected surgical pockets resulted in inflammation and possible extrusion of the samples, respectively. Low beta sheet samples lost structural integrity at 2 months after surgery C-D, while medium and high beta sheet content films showed initial evidence of degradation.
Conclusions
The in vivo response to the silk films was dependent on the location of the implant and pocket depth. Crystallinity content in silk films played a significant role in the timing of material degradation, without signs of inflammation and vascularization or changes in stromal organization.
Introduction
The need for human cornea equivalent tissues continues to grow, with an estimated 10 million people worldwide suffering from corneal vision loss (1), and in the United States over 48,000 corneal transplants were performed in 2013 (2, 3). There remain few clinical options today to meet these growing needs, limited to allogenic and synthetic materials (4). In particular, allogenic materials originating from human donors are the gold standard in corneal graft replacement (2), but their disadvantages include limited availability of quality donor corneal grafts, corneal graft rejection and a progressively increasing failure rate (5–6–7). Alternatively, synthetic keratoprostheses based on polymethylmethacrylate still require corneal tissue carriers and have numerous complications including corneal melting, uveitis, endophthalmitis and retinal detachment, resulting in a high incidence of device failure (2, 8–9–10).
The need for alternative options to current cadaver human cornea sources will continue to grow in importance as a result of increasing concerns and costs of screening for transmissible diseases (e.g., human immunodeficiency virus) and laser-assisted in situ keratomileusis eye surgery, which significantly affects the mechanical performance of corneal stroma. Therefore, tissue engineered cornea strategies have been developed to partially or fully replace the full thickness of damaged/diseased corneas. A large variety of materials with different regenerative capabilities and functional properties have been explored (11, 12); the most clinically relevant are primarily based on natural polymers, such as crosslinked collagen, and in combination with synthetic polymer networks (i.e., poly(
The goal of the present study was to investigate the in vivo response and the effect of silk crystalline structure on the degradation rate of silk films in a multipocket corneal rabbit model for corneal regeneration. The rabbit corneal multipocket model was implemented to implant multiple samples per eye and to simultaneously study the effect of silk crystalline structure on film degradation rate, as well as the potential corneal stroma remodeling by collagen I and α smooth muscle actin (α-SMA) stainings. Furthermore, we elucidated the role of different surgical variables for the preparation of the corneal pocket, by varying mainly the location of the implant, stromal pocket depth, presence of suture, number of incisions, and secondarily pocket surgical technique and operating surgeons to underscore the underlying pitfalls associated with partial and full thickness lamellar keratoplasty.
Materials and Methods
Preparation of aqueous silk solution
Aqueous silk solution was prepared from
Preparation of polydimethylsiloxane substrates
Patterned polydimethylsiloxane (PDMS; Sylgard 184 Silicone Elastomer Kit; Dow Corning, Midland, MI, USA) substrates were prepared by casting on reflective diffraction grating with grooves of 3.5-μm width and 500-nm depth (Edmund Optics Inc., Barrington, NJ, USA), as used in our previous study (22). The PDMS substrates were washed in a 70% (v/v) ethanol solution and then rinsed in distilled water before casting the silk aqueous solution to generate the patterned silk films.
Preparation of sterile patterned porous silk film
A mixture of 1% (w/v) silk fibroin and 0.05% (w/v) polyethylene oxide (PEO; molecular weight [MW] ¼ 900,000; Sigma Aldrich, St. Louis, MO, USA) solution was prepared to induce pore formation within the silk films. A 1.5-mL aliquot of 1% (w/v) silk solution was cast on patterned PDMS substrates with areas of 45 × 45 mm2, resulting in films of approximately 4-μm thickness after drying. Postcasting, the films were water annealed in a vacuum oven (Isotemp Vacuum Oven Model 281A; Fisher Scientific, Pittsburgh, PA, USA) with a water tray at 25°C, 20 mm Hg vacuum, for 30 and 60 minutes to obtain silk films with low and medium beta sheet contents, respectively, and at 60°C, 20 mm Hg vacuum, for 60 minutes to achieve high beta sheet content (24). Silk films were then sterilized by ethylene oxide (EtO) cycle (12-hour exposure and 3-hour degassing) in accordance with the US Food and Drug Administration (FDA) Sterility Review Guidance K90-1. Subsequently, silk films were maintained in sterile distilled water under sterile conditions for 3 days to leach out the PEO phase, and then samples for animal implantation were prepared with a 2-mm biopsy punch and maintained in Hank's Balanced Salt Solution until surgery.
Silk film porosity assessment
Pore distribution within silk films was assessed by confocal microscopy. A Leica TCS SP2 AOBS confocal microscope (Leica Microsystems, Buffalo Grove, IL, USA) with a ×20 objective was used to take z-stacks of the 4-μm films in bright field. Depth profiles and z-stack images were obtained by rendering 2-dimensional images with a 500-nm interval over 6-μm depth, using Leica's software.
Fourier transform infrared spectroscopy analysis
To investigate the secondary structure and potential effect of EtO sterilization cycle on the beta sheet content of the silk films, Fourier transform infrared (FTIR) spectroscopy analysis was performed by multiple reflection, horizontal MIRacle attenuated total reflectance (ATR) (Pike Tech., Madison, WI, USA) with attached Jasco FT/IR-6200 spectrometer (JASCO, Tokyo, Japan). For each midinfrared spectrum (4,000-750 cm-1), 128 scans were collected in reflection mode at 4 cm-1 resolution. The amide I band (1,595-1,705 cm-1) was used to investigate conformational differences in silk fibroin structure. The beta sheet content of silk films depends on the relative absorbance of the multiple resonances that compose the amide I peak. In particular, the strong resonance band at 1,610-1,629 cm-1 is distinctive of beta sheet structure, while the resonance band at 1,640-1,650 cm-1 is an indication of random-coil structure (28). For each type of silk film, the conformational characterization was performed on samples before and after EtO sterilization. The fraction of beta sheet content was evaluated by Fourier self-deconvolution (FSD) of the infrared spectra covering the amide I region (1,595-1,705 cm−1), and curve fitting was performed with Opus 5.0 software (30, 31).
Animals
The study protocol for the peripheral-median (P-M) approach was approved by the Institutional Animal Care and Use Committee of Tufts University (Boston, MA, USA). The study protocol for the approach central-superficial (C-S) was approved by the Institutional Animal Care and Use Committee at Weill Cornell Medical College (New York, NY, USA). The study protocol for the approach central-deep (C-D) was approved by the Institutional Animal Care and Use Committee of the PLA Postgraduate Medical School (Beijing, China). All animal work was in accordance with the Association for Research in Vision and Ophthalmology (ARVO) Statement for the Use of Animals in Ophthalmic and Vision Research. The New Zealand White rabbits (Millbrook Labs, PO Box 513, Amherst, MA, USA; Charles River, Wilmington, MA, USA or the Animal Center, PLA 301 Hospital, Beijing, China) used in this study weighed between 4 and 5 kg, and were housed in separate cages under standard conditions (humidity- and temperature-controlled room, 12-hour light/12-hour dark cycle).
Silk film implantation
All surgeries were performed under sterile procedures. Three different surgical techniques depending on sample location were used in the preparation of the corneal multipocket model. The main differences, described in Table I, were in the location of the implant, stromal pocket depth, presence of suture, number of incisions and secondarily pocket surgical technique, as well as the operating surgeons (Fig. 1). Animals were anesthetized with an intramuscular injection of 35 mg/kg ketamine HCl (Ketaject; Phoenix Pharm, St. Joseph, MO, USA) and 10 mg/kg xylazine HCl (Tranuived; Vedco, St. Joseph, MO, USA) for approaches P-M and C-S, while for approach C-D they were anesthetized with equal volumes of 846-Mixture (0.2 mg/kg of xylidinothiazoline, dihydroetorphine hydrochloride and haloperidol; compounded by the Animal Center, PLA 301 Hospital, Beijing, China) and ketamine (0.2 mg/kg; DoubleCrane Pharm, Beijing, China). Proparacaine HCl ophthalmic solution 0.5% (Bausch & Lomb) was instilled into the conjunctival sac, and the operative area was disinfected with 5% povidone-iodine. Postoperative topical antibiotics were given as follows: approach P-M: polymyxin B/trimethoprim daily ×3 days; approach C-S: moxifloxacin 0.5% daily ×7 days; approach C-D: chlortetracycline daily ×7 days. For approach P-M animals (n = 3), 4 separate incisions of each right eye were performed parallel to the cornea limbus at 12:00, 3:00, 6:00 and 9:00 o'clock. The pockets were created with a crescent microsurgical knife half deep into the corneal stroma (Fig. 1). Low, medium and high beta sheet samples were implanted in the lamellar pocket in proximity to the limbus, and microsurgical forceps were used to position the samples flat. No sutures were used to close the wound. Animals were euthanized at 1, 2 and 3 months after surgery. For approach C-S animals (n = 3), the pocket was created with a crescent microsurgical knife, one third deep in the corneal stroma in the center of the eye. The low and high beta sheet samples were placed in proximity of the incisions, and the incisions closed with 10-0 nylon sutures, removed after 1 week postsurgery. Animals were euthanized at 3 months after surgery. In the case of approach C-D animals (n = 4), only 1 incision of each right eye was performed parallel to the corneal limbus, where the pocket was created by flushing air to separate the stromal layers at two-thirds deep in the corneal stroma (modified “bubble”) (32). Low, medium and high beta sheet samples were guided under a surgical microscope with a microkeratome and positioned in proximity to the center of the eye. Animals were euthanized at 2 months after surgery. All animals received pentobarbital (150 mg/kg) for euthanasia, and eyes were harvested by enucleation.
Surgical variables investigated in the preparation of rabbit corneal multipocket surgical model
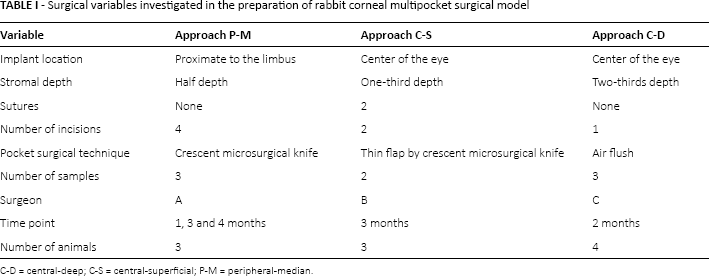
C-D = central-deep; C-S = central-superficial; P-M = peripheral-median.
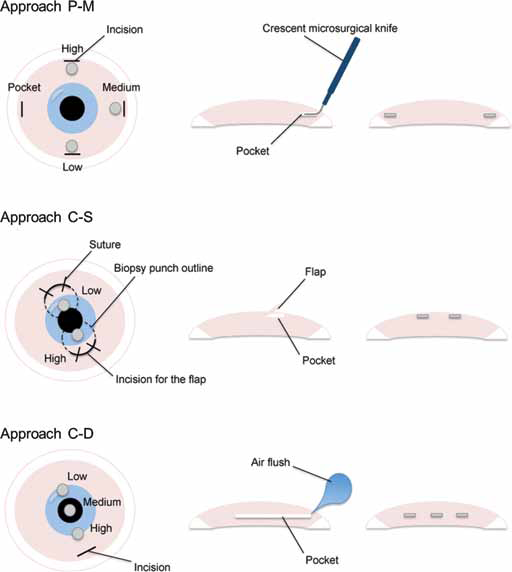
Schematic of rabbit corneal multipocket surgical approaches. The surgical variables investigated in the preparation of the corneal multipocket model were mainly the location of the implant, stromal pocket depth, presence of suture, number of incisions, secondary pocket surgical technique and operating surgeons. Approach peripheral-median
Histological and immunohistochemical analyses
To assess the in vivo response and degradation profile of silk films in relation to their beta sheet content, ocular globe integrity was maintained, and the specimens were fixed in 10% neutral buffered formalin (Protocol; Fisher Scientific, Pittsburgh, PA, USA) for 48 hours. Specimens were then processed, embedded in paraffin and cut in transverse sections of 5-µm thickness. Control samples were obtained from the rabbit control eye, which was not surgically treated, and the cornea was harvested and treated analogously to the operated eye. Histological sections were then deparaffinized with xylene, rehydrated through a series of graded ethanol and stained with hematoxylin and eosin (H&E). Brown-Hopps staining (Newcomer Supply, Middleton, WI, USA) was used to assess for the presence of gram-positive and gram-negative bacteria, following the manufacturer's instructions. Selected slides were deparaffinized and hydrated in distilled water, then stained with crystal violet solution (1% [w/v] aqueous) for 2 minutes. Between rinsing, slides were sequentially stained in Gram's iodine for 5 minutes and Gallego's solution for 5 minutes.
To characterize the collagen organization, remodeling and neovascularization within the corneal stroma, histological sections were stained for collagen I, α-SMA) and CD31 an bodies. Histological sections were deparaffinized, rehydrated through a series of graded ethanol, incubated in retrieval solution (10 mM citrate buffer, pH 6, for 20 minutes in vegetable steamer), and then incubated overnight with the anti-collagen I (1:500; Abcam, Cambridge, MA, USA) primary antibody. After washing in phosphate-buffered saline (PBS), sections were incubated for 1 hour in the polyclonal secondary antibody to mouse IgG (1:500; Abcam, Cambridge, MA, USA). Histological sections were analyzed with a light microscope (Leica DM500) using ×4, ×10 and ×20 objectives.
Statistical analysis
Data are expressed as means ± standard deviation (SD). Data were analyzed for statistical significance by 2-way ANOVA with a significance level of p<0.05 and Tukey-Kramer and Holm-Bonferroni posttest methods for means comparison (Origin Pro v. 8 software; OriginLab, USA).
Results
Morphological and structural characterization of silk film
After silk film preparation, the constructs were sterilized with EtO, and PEO was leached out under sterile conditions. As prepared, silk films with different beta sheet content were sectioned and stained with H&E to assess pores and thickness of the constructs. High, medium and low beta sheet content film thickness measured 358.57 ± 16 μm, 192.50 ± 20 μm and 151.25 ± 20 μm, respectively (Fig. 2A). A significant decrease in construct thickness was observed as beta sheet content decreased (p<0.05). Confocal scanning microscopy analysis revealed 5-μm pore distribution going through the entire thickness of the film, regardless of the beta sheet content, as shown from the image profile in Figure 2B. ATR-FTIR analysis of the samples post–EtO sterilization showed the maintenance of crystallinity degree in silk films fabricated at low, medium and high beta sheet content by the water annealing process (Fig. 2C) (28). In particular, samples with a low beta sheet content were characterized by an amide I absorbance split into 2 peaks centered at 1,643 and 1,621 cm-1 – an indication of the presence of silk with amorphous and beta sheeted structures, respectively (dotted line, see inset in Fig. 2C). By increasing the crystallinity degree through longer exposure to water annealing, silk films with a medium beta sheet content (medium beta sheet samples) were obtained, where the relative contribution of the crystalline silk present in the film increased (inset in Fig. 2C, dashed line), but the amorphous resonance band at 1,643 cm-1 was still visible. Exposure of silk films to water vapor at high temperature (i.e., 60°C) resulted in the formation of films where the amorphous resonance at 1,638 cm-1 was just a shoulder, and the amide I had a main peak at 1,621 cm-1 (dotted line, see inset in Fig. 2C) – an indication of a predominant beta sheet content. Low, medium and high beta sheet content was quantified by deconvoluting the amide I spectra, as 23% ± 3%, 35% ± 3% and 46% ± 2%, respectively.
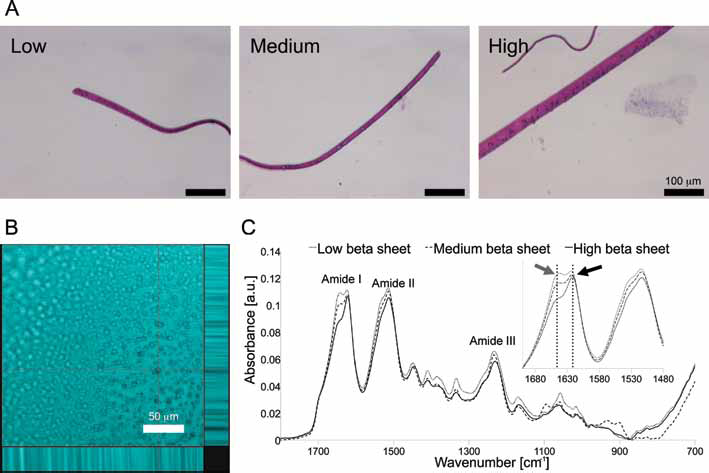
Porous silk film morphological and structural characterization. (
Macroscopic characterization of silk film implant site
Clinical observations of the implant site were made throughout the observation period, while slit lamp biomicroscopy and photography are shown for the day of surgical implantation and immediately prior to animal euthanasia (Fig. 3). In the case of approach P-M, blood was initially present where the samples were implanted. By the end of the experiment, the sites of implant showed signs of extensive collagen remodeling, infiltration and opacification. In comparison, approach C-S was clear from the blood due to the incision, and sutures were observed in proximity to the stromal pockets. At termination day, the samples were not clearly identifiable by optical images. For approach C-D, all the 3 samples were observed after implantation, while the cornea tissue did not show any particular indication of trauma or injury. Upon experiment termination, most of the samples were still visible with good structural integrity, and very rare signs of inflammation or corneal stromal remodeling were observed.
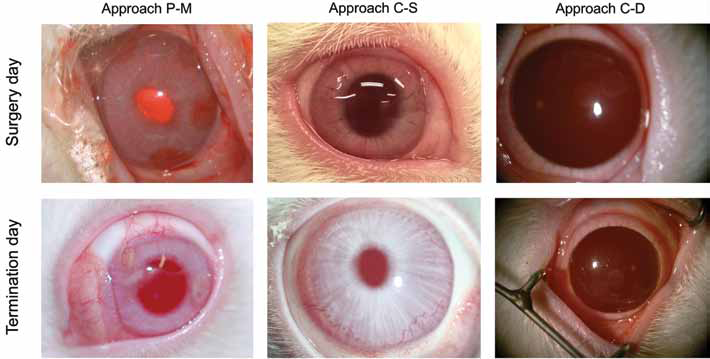
Macroscopic assessment of the surgical site. Representative rabbit eyes were photographed immediately after surgical implantation and at the experimental endpoint. Approach peripheral-median
Assessment of in vivo silk film degradation
Low, medium and high beta sheet samples implanted in a rabbit corneal pocket were analyzed after H&E staining for approaches, at 3, 3 and 2 months after surgery, respectively (Fig. 4). For approach P-M, each sample appeared folded and surrounded by a fibrotic capsule, rich in dense inflammatory tissue and multinucleated cells. None of the samples showed evidence of degradation during the corneal implant. Furthermore, anterior collagen layers lost their orderly arrangement, and signs of corneal stroma remodeling as well as increased stromal cell proliferation were observed. Brown-Hopps staining was used to assess the presence of gram-positive and gram-negative bacteria where the inflammation was present. None of the samples showed positive staining for bacteria. There were signs of degraded blood products (Suppl Fig. 1, available online as supplementary material at www.jab-fm.com). In the case of approach C-S, low and high beta sheet samples were not present anymore in the surgical pocket. The corneal tissue obtained that corresponded to the implanted samples showed proliferation of the epithelium layer in correspondence to the low beta sheet sample. In comparison, the corneal tissue in proximity to the high beta sheet film displayed disruption of the anterior collagen layers. For approach C-D, all of the samples appeared flat within the corneal pocket, and the surrounding collagen layers were aligned in an orderly fashion, while the corneal tissue appeared similar to the control sample (Suppl Fig. 2A, available online as supplementary material at www.jab-fm.com). The low beta sheet sample did not preserve its structural integrity after 2 months in a corneal pocket, while silk material debris were still present; inflammatory cells were not reported. For both medium and high beta sheet conditions, the silk films showed evidence of initial material degradation, where homogenous discontinuity within the samples was observed, as resulting from the enzymatic degradation of the silk protein. The measure of the silk film thickness relative to the prepared samples (Fig. 5) showed that only the low beta sheet sample implanted in the approach C-D displayed a significant reduction (p<0.05) in the film thickness as a result of the enzymatic degradation of the material. In particular, the low beta sheet silk film thickness was 50% thinner than the initial sample.
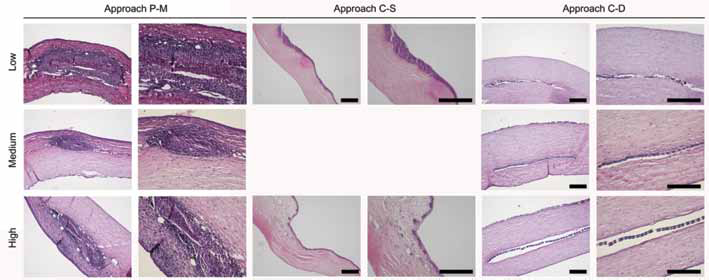
Histological assessment of silk film degradation. H&E staining of histological slides from low, medium and high beta sheet samples (arrows) implanted in a rabbit corneal stromal pocket model with 3 different surgical approaches: peripheral-median
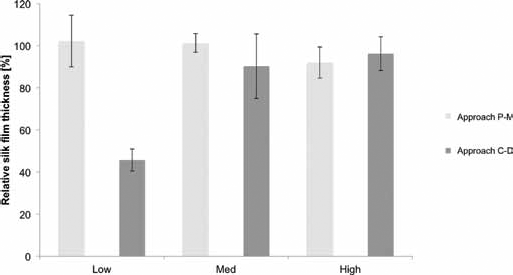
Quantification of silk film degradation. Measure of the silk film thickness relative to the prepared samples. Only the low beta sheet sample implanted in the approach central-deep (C-D) displayed a significant reduction (p<0.05) in the film thickness as a result of the enzymatic degradation of the material. P-M = peripheral-median.
Assessment of collagen structure, remodeling and neovascularization
Immunofluorescence staining against collagen I was performed to assess the structure of the corneal collagen following silk film implantation (Fig. 6). Following the surgical approach P-M, the orderly aligned and evenly distributed type I collagen fiber organization was not maintained at 3 months postsurgery. In particular, collagen expression in proximity to the low beta sheet sample was significantly increased, while for the medium and high beta sheet sample collagen fibers were misaligned. For approach C-S, the fluorescence signal from the collagen I positive staining displayed a lack of physiological organization and had increased protein expression, as shown by tissue remodeling in all of the samples after 3 months. In the case of approach C-D, collagen I was evenly distributed and physiologically aligned within the stroma, similar to the control rabbit cornea (Suppl Fig. 2B, available online as supplementary material at www.jab-fm.com). In particular, the collagen I fluorescence signal showed a homogenous distribution of collagen along the silk film implants, where the fibers were neatly organized at 2 months after surgery.
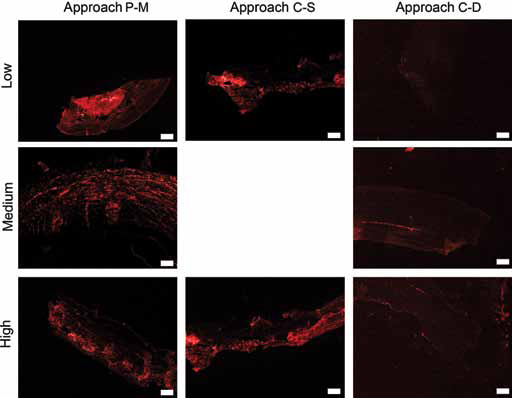
Assessment of collagen organization. Immunofluorescent staining of type I collagen of corneal tissue where low, medium and high beta sheet samples were implanted in a rabbit corneal stromal pocket model with 3 different surgical approaches – peripheral-median
Corneal stroma remodeling within the corneal pocket was characterized by immunofluorescence staining against α-SMA, as reported in Figure 7. Positive expression of α-SMA was mainly present in animals operated on with the surgical approach P-M. The majority of remodeling was observed around the samples and in the anterior part of the cornea toward the epithelium. In comparison, for the approaches C-S and C-D, the staining against α-SMA was negligible and comparable to the cornea control sample (Suppl Fig. 2C, available online as supplementary material at www.jab-fm.com).
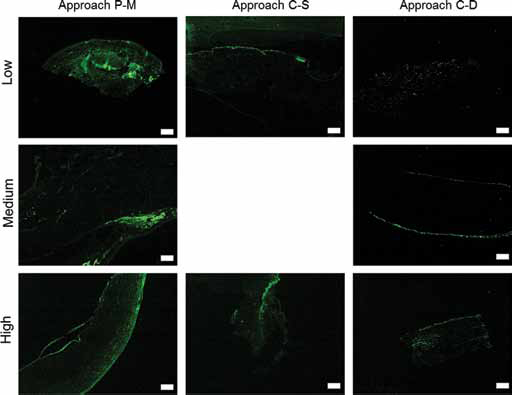
Assessment of corneal stromal remodeling. Immunofluorescent staining of α-SMA of corneal tissue where low, medium and high beta sheet samples were implanted in a rabbit corneal stromal pocket model with 3 different surgical approaches – peripheral-median
Phenomena of neovascularization were characterized by CD31 immunostaining. None of the samples showed positivity for the neovessel formation marker (Suppl Fig. 3, available online as supplementary material at www.jab-fm.com).
Discussion
The time frame of silk-based biomaterial degradation can span weeks to years depending on the processing of the material (33, 34), by controlling the content of beta sheet (crystalline domains). Silk is composed of fibroin chains, MW ∼390 kDa, with a block copolymer structure that self-assembles into beta sheets via hydrophobic hydration mechanisms (35–36–37). The rate of degradation relates directly to beta sheet dimension, which leads to more rapid proteolytic degradation (27), where specifically, the physical temperature-controlled water vapor annealing process allows the achievement of low crystalline content for a fast degrading profile. This physical treatment can be used to control structural properties and thus mechanical properties, thermal stability, enzymatic degradation and cell interactions (28). The enzymatic degradation of antiparallel beta pleated sheets in silk structures results in fibrils and then nanofilaments, which are nucleators of the crystalline regions. In vitro cytotoxicity studies of silk degradation have shown that silk is fully degradable and that the degradation products are not cytotoxic (38). The in vivo degradability of silk scaffolds has been studied in a number of surgical sites, including muscle, bladder and adipose tissue (39–40–41). Previous studies of silk films implanted in the rabbit corneal stroma showed no degradation of the constructs, as the crystallinity content of the protein was high due to the sterilization treatment (autoclave) (26). In the present work, we investigated the degradation profile in a rabbit corneal stroma space of silk films with optimized porosity and surface topography for stromal cell growth and interactions (22, 25). The beta sheet content in the low, medium and high samples was finely controlled by water annealing and maintained unaltered by using EtO sterilization, as demonstrated by the characterization of the protein secondary structure with FTIR. Previous in vitro degradation studies have already shown the increase in material degradation rate by reducing the beta sheet content for the same silk film format (24). A significant extent of material degradation was observed only for samples implanted with the surgical approach C-D, which did not induce significant injury or inflammation. In particular, the low beta sheet sample lost structural integrity and thickness was significantly reduced over time in the cornea pocket. In comparison, silk films with medium and high beta sheet content started to show the effect of proteolytic degradation.
The role of the surgical technique for corneal pocket creation is crucial in assessing the proper material response in such an environment (42). In particular, the degradation of biomaterials in this specific site has not been extensively investigated. Herein, we aimed to investigate in a rabbit multipocket corneal model the role of different surgical variables for the preparation of the pocket, mainly by varying the location of the implant, stromal pocket depth and presence of suture, as well as number of incisions. In fact, we demonstrated that the in vivo response to implantation was highly dependent on the surgical technique, easily confounding interpretation of material-specific host responses. In particular, a central, deeper location of the corneal pocket together with a lack of sutures limits injury and inflammatory responses, as in approach C-D. The samples implanted in approach C-S were potentially extruded from the ocular surface, due to the lack of depth in the pocket preparation. Furthermore, approach C-D demonstrated superiority for the use of an air flush in creating the corneal pocket instead of using a surgical blade. The flushing air creates a dissection plane that more easily allows for the deeper blade dissection and deeper placement of the films. We attribute these responses directly to the surgical procedures, as the materials were the same as those used in approach C-D, where no inflammation was observed and degradation and integration was found. Therefore, the use of flushing air to create the corneal pocket, and the central deep position of the sample, as well as a lack of sutures, are paramount in a successful multipocket surgical technique.
The corneal stroma makes up approximately 90% of the overall cornea thickness and consists of layers of aligned collagen fibrils referred to as lamellae (43). Approximately 200 to 250 lamellae extend from limbus to limbus, with collagen fibril orientation offset between adjoining layers. The lamellar collagen fibrils are mainly of type I and V collagen, and a high concentration of small leucine-rich proteoglycans, including decorin, lumican and keratocan, decorated with dermatan sulfate and keratan sulfate, is present and is credited with maintaining the interfibrillar spacing required for transparency and mechanical tension (44, 45). Reduction in collagen organization and composition can result in cornea deterioration and opacity (46).
Therefore, understanding the effects of the material degradation, as well as the surgical technique, on the native collagen structure and organization is critical to assessing the functionality of the corneal tissue (47). The staining against collagen type I showed the lack of fiber organization in the corneal pockets for the surgery approaches P-M and C-S, while positive staining against α-SMA demonstrated extensive corneal stromal remodeling only for the approach P-M, which had the most severe reaction regardless of the beta sheet content of the sample implanted. With regard to neovessel formation, none of the samples showed positivity for CD31 staining, suggesting a lack of any neovascularization for any of the surgical approaches.
Footnotes
Acknowledgement
The authors thank the NIH (R01 EY020856 and R01 EY016415) for their support for these studies.
Financial support: Funding was received from the US National Institutes of Health (R01 EY020856 and R01 EY016415) to support these studies.
Conflict of interest: None of the authors has any financial interest related to this study to disclose.
