Abstract
Purpose
Different results have been reported on the internal colonization of Cone Morse connections under in vitro dynamic loading. The aim of the present in vitro study was to evaluate the bacterial leakage in Cone Morse implant-abutment connections, both under loaded and unloaded conditions.
Methods
A total of 20 implants with a Cone Morse taper internal connection were used in this study. Ten were loaded under a special testing equipment (Test Group), while 10 were left unloaded (Control Group). The inner part of all implants was inoculated with 0.1 μl of a viable
Results
In the unloaded assemblies, bacterial contamination was found in 2 out of 10 implant-abutment junctions, on the 12th and 13th days. In the loaded implant-abutment connections, bacterial contamination was found in 2 out of 10 implant-abutment assemblies, on the 13th and on the 14th days.
Conclusions
The resistance of the Cone Morse implant-abutment junction reported in the literature and confirmed in the present study, where no differences in the percentages of microbial leakage were found in assemblies unloaded and in those subjected to a dynamic loading procedure, could help to explain the histological results in man of a lack of peri-crestal bone resorption in Cone Morse implants, placed below the level of the alveolar crest.
Keywords
Introduction
The presence of an implant-abutment junction (IAJ) has been correlated with the presence of microorganisms (1). These bacteria may harbor inside the microgaps that can be found in the assemblies and they have been reported to be the cause of the inflammation of the soft tissues (abutment Infiltrated Connective Tissue or ICT) facing the IAJ, potentially producing a bone resorption of the surrounding pericrestal bone (2-3-4-5). Bacterial migration has been correlated with tightening torque forces, micromovements of the different components during the masticatory cycles and the accuracy of the fit between implant and abutment (1). Even if the Cone Morse implant-abutment connection is considered to be the most stable and the most capable to resist penetration of microorganisms when compared with flat-to-flat or tube-in-tube connections, their possible bacterial colonization is not yet well understood (6, 7). In all implant-abutment different connections the size of the IAJ microgaps can be increased during the loading of the assemblies (2, 8, 9), introducing a so-called pumping effect (10). Higher quantities of microorganisms have been reported for loaded than unloaded external hexagon and internal hexagon implants (9). On the other hand, a minimal contamination has been reported for Cone Morse connections (2, 11). Different results have been reported on the internal colonization of Cone Morse connections under in vitro dynamic loading. do Nascimento et al (9) found no significant differences in the amount of bacteria, comparing unloaded and loaded groups, while, on the contrary, Koutouzis et al (10) found that the bacterial penetration was influenced by the loading conditions. One of 20 assemblies was found to be colonized by
Methods and materials
A total of 20 implants with a Cone Morse taper internal connection (Universal II CM, Implacil, De Bortoli, Sao Paulo, Brasil) were used in this in vitro study. Ten were loaded under a special testing equipment (Test Group), while 10 were left unloaded (Control Group). To simulate cyclic loading and to mimic intraoral conditions, the Test implants were embedded in autopolymerizing acrilic resin with a custom-made stainless steel ring form. The implants were positioned using a parallelometer to ensure uniform alignment of all specimens. The implants were positioned so that the cyclic fatigue load was applied to the long axis of the implants. All embedded implants were sterilized by autoclave for 15 minutes at 121°C. After several trials, 0.1 μl was determined to be the ideal quantity of bacterial suspension for inoculation in the implant systems.

Abutment connected to the implant at 30 N cm.

Implant/abutment immersed in nutrient solution, drawn by sterile syringe and analyzed by culture method.
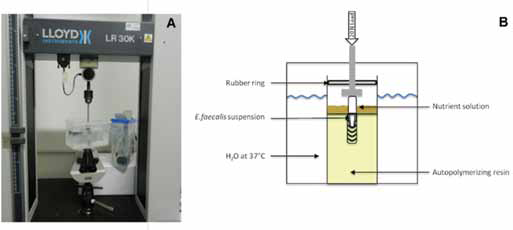
(
Results
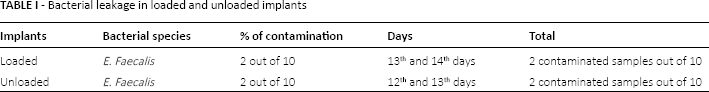
The frequencies of contamination in both tested groups were shown in Table I. In the unloaded assemblies, bacterial contamination was found in 2 out of 10 IAJ, on the 12th and 13th days. In the loaded implant-abutment connections, bacterial contamination was found in 2 out of 10 implant-abutment assemblies, on the 13th and on the 14th days. No assemblies showed contamination of the outer portions. The positive controls remained positive. The negative controls remained negative.
Bacterial leakage in loaded and unloaded implants

Discussion
A gap of 1-5 microns has been reported to be present, in retrieved human implants, between the implant and the healing screw, and this space was found to be filled by bacteria and calculus (12). Bacteria were also present inside the most apical portion of the hollow part of the implant (12). In another histological study on retrieved human implants, it has been reported that bacteria were often present between the implant and the abutment and in the internal portion of the implants (13). These results, with the finding of hollow spaces, in screw-retained abutments, between the implant and abutment components with the presence of fluids and bacteria inside the internal hollow cavities of the implants, serve to validate, in man, the results obtained from in vitro studies or animal experiments (12). Moreover, in retrieved human implants, an inflammatory infiltrate was present below the implant-abutment microgap (12), and, in an experimental study in monkeys, many inflammatory cells were found below the implant-abutment microgap (5). There is evidence that with cyclic loading the microgap can increase in size, especially in external hexagon implants, facilitating the flow of fluids and bacteria (6, 9, 13-14-15). The results of the present study did not agree with the statement that overall loaded implants showed higher bacterial counts than unloaded implants (9). The present data may reflect the possible differences in the precision fit, in the degrees of taper and in the internal connection features of the implant components in the different implant systems (10, 14, 16). The reported average misfits between implant components vary greatly, from 1 to 100 microns (9). The occlusal loading of the implants produces bending forces and/or micromovements within the implant systems (9) increasing the microgap and promoting a higher fluid and bacteria infiltration (15), especially if imprecise machining of implant components or improper male-female adaptation exist (17). Cone Morse connections have been proposed to get a better stability, with reduced micromovements, of the components, providing a better bacterial seal (18). The bacterial microleakage can, probably, be reduced by obtaining an optimal component fit, a reducing or absence of micromovements, and a minimal prosthetic misfit (19-20-21-22-23-24-25-26-27-28). The length of the IAJ in Cone Morse implant-abutment assemblies could be a reason for the reported differences in the bacterial leakage (14). Implants that use mechanical frictional abutments seem to present precise adaptation in the deeper inner portions of the system, resulting in reduced micromovements (9).
Conclusion
The resistance of the Cone Morse IAJ reported in the literature and confirmed in the present study, where no differences in the percentages of microbial leakage were found in assemblies unloaded and in those subjected to a dynamic loading procedure, could help to explain the histological results in man of a lack of peri-crestal bone resorption in Cone Morse implants, placed below the level of the alveolar crest.
Footnotes
Acknowledgment
The Authors gratefully acknowledge the help of Donato Di Iorio, D.D.S., Ph.D., for the specimens preparation.
Financial support: This work was partially supported by the Ministry of Education, University, and Research (M.I.U.R.), Rome, Italy.
Conflict of interest: The authors state they have no conflict of interest.
