Abstract
Purpose
The purpose of this in vitro study was to evaluate and compare the fracture strengths of post and core systems produced with different fabrication techniques and materials.
Methods
Forty extracted human single-root premolars were used in this study. After root canal treatment, the teeth were randomly divided into 4 groups of 10 each as follows: group C: metallic 1-piece posts and cores fabricated by casting, and serving as the control; group CM: metallic posts and cores fabricated with the copy milled technique; group LS: 1-piece posts and cores fabricated with the laser sintering technique; and group ZR: 1-piece zirconia posts and cores fabricated with computer-aided design and computer-aided manufacturing (CAD-CAM). The posts and cores were cemented to the teeth with adhesive resin cement; then, the specimens were mounted to acrylic resin blocks, attached to an Instron Universal Testing Machine, and loaded with a crosshead speed of 1 mm/min, until fracture. Data were statistically analyzed using 1-way analysis of variance (ANOVA), followed by the post hoc Tukey test (α = 0.05).
Results
The highest fracture results were found in group ZR (315.4 ± 53.4 N), which showed significant differences from all other groups (p<0.05). The lowest test values were found in group C (230.2 ± 29.8 N). Group LS (250.9 ± 29.0 N), group CM (253.0 ± 22.4 N) and group C did not show any significant differences (p>0.05).
Conclusions
Custom-made zirconia 1-piece posts and cores, fabricated using the CAD-CAM procedure, can be an alternative treatment method when compared with other techniques.
Introduction
The restoration of severely damaged endodontically treated teeth is still a topic of discussion in dentistry today (1). Endodontically treated teeth exhibit different responses to mechanical loads from intact teeth. The removal of pulp and root dentin reduces the stress–strain capacity of the teeth; however, it compromises the root fracture resistance (2). The choice of an appropriate restoration for endodontically treated teeth is guided by strength and esthetics (3), and one common method for restoring endodontically treated teeth is the use of the post and core (4).
Posts are needed for restorating teeth with insufficient coronal tooth structure to retain a core for definitive restoration (Fig. 1). Post material plays a crucial role in the biomechanical performance of endodontically treated teeth. Numerous experimental and computational studies have shown the relevance of post designs, including length, diameter and material, on the strength of restored teeth (5). Endodontic posts can be preformed or custom made, metallic or nonmetallic, stiff or flexible and esthetically or non-esthetically pleasing (6). Custom-made metal posts and cores are widely used in clinical practice because of their superior physical properties (3), but they do have disadvantages, such as a high modulus of elasticity, increasing the possibility of irrecoverable fractures of the remaining tooth structure (7). Additionally, cast posts may produce a gray discoloration of translucent all-ceramic crowns and the surrounding gingiva (8). Although there are disadvantages, metal posts are still widely used in dental practice.
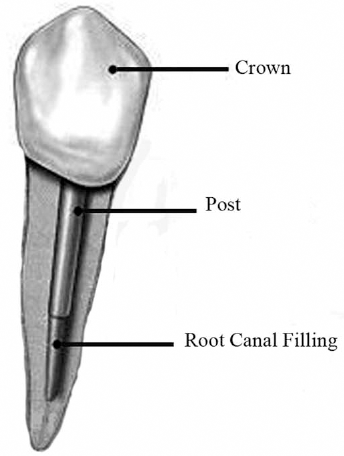
Schematic view of post and core restoration.
Increased esthetic expectations, as well as possible problems resulting from the corrosion of posts made from non-noble alloys, have encouraged the development of tooth-colored post systems (9). Due to favorable optical and mechanical properties, endodontic posts made of partially stabilized zirconia ceramic have also been described as being promising alternatives to those made of metal (10).
To date, alternative methods for producing posts and cores have been developed, and the use of copy-milling systems for high-strength ceramics allows for the fabrication of cores to be combined with prefabricated posts; additionally, completely milled posts and cores have been described in the literature (9, 11, 12). The technique for milling a 1-piece zirconia post and core has been described by Awad and Marghalani (13) and Streacker and Geissberger (12). The authors used computer-aided design and computer-aided manufacturing (CAD-CAM) technology to fabricate yttrium-tetragonal zirconium polycrystal ceramic posts.
Also for fabricating metallic post and cores, CAD-CAM machining and laser sintering of metal alloys are alternative fabrication methods (14). Laser sintering allows the efficient and direct production of customized metal parts from different types of metal alloys, including titanium, without any additional cost-incurring preprocessing and postprocessing (15). The laser sintering and metal milling procedures can also be used for fabricating cobalt-chromium restorations (15, 16).
There are many studies that evaluate the mechanical properties of prefabricated post and core systems (17-18-19). However, data on the mechanical properties of custom-made 1-piece posts and cores produced with CAD-CAM and laser sintering techniques are rare (11, 20). The purpose of this in vitro study was to evaluate and compare the fracture resistance of custom 1-piece post and core systems produced with different fabricating techniques and materials. The null hypothesis was that different fabricating techniques and materials would not affect the fracture resistance of the post and core systems.
Materials and methods
Forty freshly extracted human single root premolars were collect from patients receiving orthodontic treatment. The teeth were stored in a 0.1% thymol solution immediately after extraction, during the course of the study, and examined under a stereomicroscope. Teeth with cracks, caries and restorations were discarded. After the selection procedure, the teeth were transversally sectioned at their cervical portion, using a double-faced diamond disk fitted to a low-speed handpiece, and cooled with an air/water spray, so that the length of the roots was standardized at 13 ± 1.0 mm as determined by using a digital caliper.
The working length was measured by deducting 1 mm from the length recorded when the tips of #15 K-files were visible at the apical foramina. The specimens were instrumented with Mtwo NiTi rotary files up to size 40/0.04 at working length. All of the files were used to the full length of the root canal, as per the single-length technique. After each instrument was used, the root canals were irrigated with 5 mL of 2.5% NaOCl using a 30-gauge needle; then, the root canals were dried with absorbent paper points. All root canals were obturated with the lateral condensation technique using size 40 gutta-percha as a master cone. In all groups, an epoxy resin-based sealer was used as a root canal sealer.
Each specimen was embedded in autopolymerizing acrylic resin perpendicular to the long access of the root, and the post space was determined at a constant length of 10 mm and a diameter of 1.25 ± 0.5 mm for all teeth. The length was obtained by initially removing the gutta-percha with a Gates Glidden drill (Mani Inc., Tochigi-Ken, Japan) up to size 3 (Fig. 2).
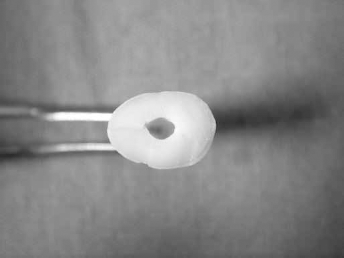
Prepared post space.
For fabricating the 1-piece posts and cores, the teeth were randomly divided into 4 groups, consisting of 10 teeth each. The 1-piece post and core patterns were fabricated with acrylic resin (Pattern Resin; GC America Inc.) on each of the prepared specimens. A syringe with a tip was used to inject the acrylic resin inside the previously lubricated post space. Once the post patterns were prepared to the predetermined length and width, the core pattern was fabricated by adding additional autopolymerizing acrylic resin with a brush. These patterns were used in the fabricating process of groups C, CM and LS.
The sample groups were divided as follows:
Group C: Cast post and core; the post and core were cast using a lost-wax technique from a Co-Cr alloy.
Group CM: Metal milled post and core; the post and core restorations were milled from a prefabricated Co-Cr block. The milling procedure was conducted according to the manufacturer's recommendations using a CAD-CAM procedure.
Group LS: Laser sintered post and core; the post and core restorations were made using laser sintering of a Co-Cr alloy powder, using the PM 100 system and a machined pattern resin post core of the same dimensions. The laser sintering procedure followed the recommendations of the manufacturer (EOSINT; EOS, Germany).
Group ZR: Zirconium oxide post–core; a milled zirconia post and core that was produced using the CAD-CAM procedure (CEREC 3; Sirona, Germany). The prepared post holes were covered with titanium oxide powder and scanned with the optic camera from the CEREC 3 system. The post and core restorations were designed with the CEREC 3 software program, and when the design procedure was finished, the milling unit milled the post and core restorations.
After the fabrication process, the completed specimens were cemented to the teeth with adhesive resin cement, and all of the specimens were stored in distilled water at 37°C for 3 days after the cementation process (Fig. 3). A special fixture was prepared to mount the tooth (along the long axis) at an angle of 130° to the point of the application of the force. Acrylic resin blocks were mounted to the stainless steel fixture on an Instron Universal Testing Machine (Fig. 4A), and the specimens were loaded with a crosshead speed of 1 mm/min, until fracture occurred (Fig. 4B).
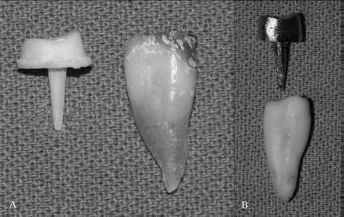
Prepared post and cores before cementation.
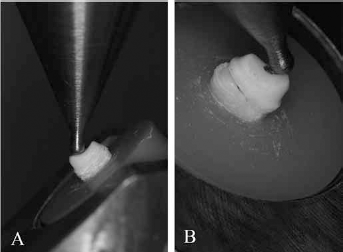
Views of the test specimen in the Instron machine, before
The data were statistically analyzed using the SPSS ver. 21 software program, and the Kolmogorov-Smirnov test showed that the data was of a normal distribution (p>0.05). The means and standard deviations of the fracture strengths were calculated, and the mean values were compared by 1-way analysis of variance (ANOVA), followed by the post hoc Tukey multiple comparisons test (α = 0.05).
Results
One-way ANOVA results revealed that fracture strength of 1-piece post and core restorations were affected by different post and core materials and fabrication techniques (p<0.05). The mean test values and their standard deviations are listed in Table I. The highest results were found in group ZR, which showed significant differences from all of the other groups (p<0.05). The lowest test values were found in group C. Group C, group CM and group LS did not show significant differences (p>0.05).
Mean fracture strength values of the test groups (N)
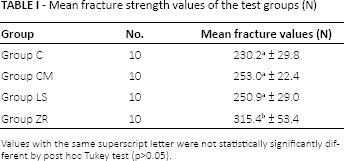
Values with the same superscript letter were not statistically significantly different by post hoc Tukey test (p>0.05).
Discussion
The results of this in vitro study support a rejection of the null hypothesis that different fabricating techniques and materials would not affect the fracture resistance of post and core systems. The fracture strength values of the 1-piece posts and cores were affected by the material and fabrication technique selected.
In the anterior region, because of the esthetic problems, prefabricated esthetic post systems such as fiber, ceramic, and zirconia are generally preferred. The clinical success of these materials depends on the severity of the clinical factors, but fracture resistance is a critical issue. However, as the bending resistance of a post depends on its diameter and physical properties, it is essential to have a basic knowledge concerning the mechanical properties of the individually selected post (21).
In wide, noncircular or extremely tapered canals, post systems that rely on the use of a cylindrical prefabricated post may not achieve the intimate adaptability of the post to the canal, possibly compromising the retention of the post (13). When these factors are evaluated, a custom made 1-piece cast and 1-piece milled posts and cores would be an alternative treatment option in some clinical cases.
Butz et al (22) reported that the survival rates and fracture strengths for prefabricated zirconia posts with composite cores are significantly lower, so this combination cannot be recommended for clinical use. Bittner et al (20) reported an advantage that 1-piece post and core systems avoid potential core delamination by eliminating interfaces between the post and the core. Additionally, one previous research study reported that the core construction technique was a decisive factor in the survival rate of a zirconia post (23).
Bittner et al state that the clinical performance of restorations machined by CAD-CAM provides a post and core with greater durability, maximum adaptability to the canal and adequate esthetics (20). A popular CAD-CAM system used in dental practice is the CEREC system (24). Streacker and Geissberger (12) and Bittner et al (20) used the CEREC InLab technique for fabricating a 1-piece zirconia post and core. In these studies, the researchers fabricated acrylic resin patterns that simulated the 1-piece post and cores, and these patterns were scanned for milling. Dayalan et al (18) reported a 3.59% error in the copy milling of the posts. This could be an error in machining or an error due to the inability of the scanner to record the finer details of the scanned patterns. In the present study, when the test specimens were examined, fabricating errors were not observed, which can be explained by the difference in the scanning procedure. In the CEREC system for scanning teeth, direct and indirect techniques can be used. In the indirect technique, after making the impression, a physical model (die) was prepared and scanned by laser in the laboratory for acquiring and transmitting information. However, the direct technique eliminates these steps, and the teeth are scanned directly using the intraoral camera of the system. In the present in vitro research, the post holes were scanned directly with the intraoral camera of the system, so that possible mistakes or deformations were eliminated during the fabricating process of the acrylic resin patterns. To date, there have been no reports that have used the direct technique in the scanning process for fabricating a custom-made post and core.
Strub et al (25) found mean fracture strength values for zirconia ceramic posts combined with prefabricated glass ceramic crowns of 1,494.5 ± 333.5 N, and 463.3 ± 46.2 N for zirconia ceramic posts with overpressed ceramic cores. In another report from the same group, mean fracture loads of 503 N for zirconia ceramic posts with composite resin cores, and 521 N for zirconia ceramic posts with ceramic cores were reported (26). When the previous studies were evaluated, because of core delamination, it was expected that the custom-made 1-piece zirconia post and core would show higher fracture strength values. In the present research, 1-piece zirconia posts and cores demonstrated the best fracture resistance values when compared with other test groups (315.4 ± 53.4 N). One possible explanation for the different fracture strength values obtained in these studies might be seen in the different study designs. Strub et al (25) and Heydecke et al (26) used completely restored teeth and tested the prefabricated zirconia posts and cores, while Friedel and Kern (11) reported that the fracture values were changed when the posts and cores were restored with crowns.
Beck et al (27) reported that the superior performance of prefabricated zirconia posts, as used in the present study, may be explained by the fact that these posts were industrially machined from wrought material consisting of hot isostatically pressed zirconia. Similarly, in this study, custom-made zirconia 1-piece posts and cores were first milled with a milling unit from prefabricated presintered zirconia blocks. After this procedure, the completed test specimens were sintered in a dental laboratory. This can be a critical factor in the mechanical properties of the material; therefore, the expected decreased fracture strength values of the test specimens were drawn.
In this in vitro research, when the failure type was evaluated, the majority of the fractures occurred in the cervical half of the root, and it was unrepairable. As previously mentioned in the study by Heydecke et al (26), this can be attributed to the fact that zirconia posts had the highest modulus of elasticity among the post types tested. This high elasticity modulus of the zirconia posts and the difference from the tooth can create catastrophic failure, which could be a limitation for this treatment method.
Metal post and core restorations are the gold standard for the treatment process in dental practice. However, different techniques can be used for fabricating the metal restorations, such as casting, milling, and laser sintering. Laser sintering is the newest technology in metal manufacturing, which allows for an efficient and direct proportion of customized metal parts from different types of metal alloys (28). In this research, the post and core restorations fabricated with metal milling and the laser sintering technique showed higher test results when compared with the posts and cores produced with the conventional lost-wax technique. This can be attributed to the casting defects and homogeneity of the Co-Cr alloy. In the metal milling and laser sintering procedure, standard prefabricated metal blocks were used, so higher physical properties of these test specimens were expected.
In this in vitro study, zirconia metal posts and cores were compared with metal posts and cores because, as previously indicated, the metal post and core systems are still widely used in dental practice and considered to be acceptable. Therefore, the aim of this in vitro study was to evaluate whether zirconia esthetic posts can be an alternative treatment option as opposed to the metal posts and cores. Further studies are required to compare the physical properties of other esthetic post systems, such as fiber, glass and ceramic post and core restorations, with zirconia posts and cores.
One limitation of this study was that the intraoral camera of the CEREC system cannot scan lengths that are deeper than 10 mm of the post hole. An increase in the success rate of endodontically treated teeth has been noted when the post length is equal to two thirds of the root length, or when this cannot be achieved, the post should have at least the same length as the crown (29). Braga et al (30) and Giovani et al (31) observed that when the post length was equal to half of the root length, the root behavior was similar to that of the roots that were prepared up to two thirds of their length. Jindal et al (32) reported that 10-mm post lengths showed the highest fracture strength values of the posts and cores when compared to the posts and cores with a 5-mm length. Cecchin et al (29) indicated that no statistically significant differences were found for the fracture resistances between the 12-mm and 8-mm post lengths. In this study, to achieve standardization, a 10-mm post length was selected.
The cementing process is a critical point in the clinical success of the posts and cores, as previously mentioned in the literature. Friedel and Kern (11) reported that when the phosphate monomer containing the resin composite Panavia 21 was used for bonding to zirconium oxide ceramic posts, a higher bond strength was achieved than when using conventional resin composites. Therefore, in this in vitro research, the posts were cemented with adhesive resin cement (Panavia 21).
Another limitation of this research was cyclic loading, which was not used for this study, and which may affect the results, because dental materials may behave differently with cyclic loads in comparing increasing loads to failure. Additionally, as with any in vitro study, a final limitation was the fact that it could not completely simulate in vivo conditions.
Conclusions
Within the limitations of this in vitro research, the following results were determined:
The zirconia posts and cores showed the highest fracture resistance values. Custom-made 1-piece posts and cores fabricated with the CEREC system and a chairside scanning technique can be an alternative to the custom-made 1-piece post and core fabricating technique, when compared with other techniques.
In the metallic posts and cores, the test specimens produced with laser sintering and metal milling procedures showed higher test values than the test specimens that were produced with conventional casting methods.
Footnotes
Acknowledgement
The authors wish to thank Benlioğlu Dental and Sirona the Dental Company for their experimental support.
Financial support: None received.
Conflict of interest: The authors declare they have no conflict of interest.
Meeting presentation: This study was presented as a poster at the 11th international congress of the Turkish Endodontic Society (27-28 April 2012).
