Abstract
Background
This study examined the effect of interfacial sliding and test material properties on the fixation strength and insertional properties of self-tapping bone screws. Various substitute materials (polyacetal [POM], poly(methyl methacrylate) [PMMA] and E-glass-filled Epoxy [Sawbones®]) for human bone were evaluated, and the results were compared with the findings for cadaver bone.
Methods
Initial coefficient of friction (CoF) of the screw material stainless steel AISI316 was tested using a pin-on-disk apparatus, and the screws were exposed to pullout tests after insertion torque tests. The effect of a smooth diamond-like carbon (DLC) coating was studied by applying the coating on both CoF test balls and bone screws.
Results
Mechanical properties of test blocks strongly correlated to both pullout strength and insertion torque of the screws: for noncoated 2.7-mm screws, tensile strength correlated to pullout strength and insertion torque, with Pearson correlation coefficients r=0.977 and r=0.738, respectively. In contrast, CoF correlated strongly to screw insertion torque but not to pullout strength in bone substitute materials (for noncoated 2.7-mm screws, r=0.652 and r=0.248, respectively). There were no significant differences in CoF using noncoated and DLC-coated screw materials against bone substitutes.
Conclusions
Proper materials for in vitro testing help in evaluating the biomechanics of the implants in advance. However, choosing the material needs attention, as their ability to model human bone depends on test type.
Introduction
Tribology and interfacial chemistry play major roles in implant–tissue interaction, biomechanical behavior and survival of implants in the human body. Insufficient screw anchorage is a serious problem in bone that has become mechanically weak e.g., due to osteoporosis. Implant materials and design, various coatings and surface patterning have been developed to improve bone–implant interfacial behavior.
Cortical bone screws are commonly used implants for fracture fixation and also for plate fixation. Nowadays, locking plate and compression plate systems are used to secure fracture fixation stability. Compression plate fixation relies on friction between the screw head and the plate, generated by tensional forces due to tightening of the screw in bone. In the locking plate system, the screw is mechanically attached to the plate by the threads in both the screw and the plate. In both cases, the screw is not supposed to take significant bending loads, to avoid shear failure. Pullout testing of screws in the axial direction is derived from their principal mode of operation in compression plate fixation; the screws are axially preloaded to generate compression between bone and plate. This compression should result in sufficient friction to transfer loads that act orthogonal to the screw axis. In addition to pullout tests (1-4), also screw pushout tests have been performed (5). In both cases, the ultimate holding power of the fixation system is determined. However, only a little effort has been devoted to the measurement and reporting of insertional torque (6-8), although those are relevant parameters as well.
Experimental setups are often used to evaluate fixation strength and to develop the function of the fixation devices. For several reasons, bone substitutes are typically used in in vitro experiments instead of cadaver bones. These reasons include, for example, biomechanical, ethical and practical considerations. Most critical concerns are related to the preservation of the specimens and variation in the mechanical properties of the cadaver bones. Thus, in many cases, synthetic materials or other natural materials (1, 2, 8-14) have been used in biomechanical research.
The improvement of the interface between bone and orthopedic or dental implants is still an unresolved problem. For different applications in orthopedics, metallic, ceramic or biological coatings have been widely investigated. One trend is to improve implant osseointegration. Of all of the factors investigated, the surface structure, biomechanical factors and biological response have been demonstrated to have the greatest influence on implant osseointegration (5). For this purpose, typical methods for surface modification include sandblasting, plasma-spraying and acid-etching, which all alter topography and increase active surface area. On the other hand, coatings can prevent bacterial adhesion, decrease friction or minimize wear on sliding surfaces (15, 16). To meet these demands, coatings need to be hard, inert and smooth. Coatings with the required properties can be applied on implant materials e.g., by physical vapor deposition methods.
Diamond-like carbon (DLC) has outstanding tribological properties and is, in addition, tolerated well by the body. Thus, a lot of effort has been put into research of DLC coatings in biomedical applications. The main reason for the success of DLC coatings in different applications is their low coefficient of friction (CoF) in combination with a high wear resistance (16). DLC has been shown to also have excellent hemocompatibility, wear resistance and hardness (17). Thus DLC coatings have good potential also in orthopedics, such as in reducing the insertion torque of fracture fixation screws (11, 18). However, several interfacial factors affect both in vivo and in vitro findings, and there are still some unclear factors regarding fixation stability.
The aim of this study was to see whether selected substitute materials could generally model human bone in fixation strength studies in vitro. Secondly, the effect of DLC coating on fixation strength and frictional properties of screws in different types of substitute materials was studied, and the results were compared with the findings in cadaver bone.
Materials and Methods
Synthetic bone blocks of various materials were used to find a more consistent model compared with cadaveric bone. In contrast to cadaveric bones, synthetic test specimens have low variance in mechanical properties and are readily available with well-specified properties. Furthermore, there is no risk of contamination or decomposition with the synthetic materials. The use of human bone samples in the present study received the permission of the Finnish National Authority for Medicolegal Affairs (TEO, 1781/32/200/01).
Screw insertion and pullout tests
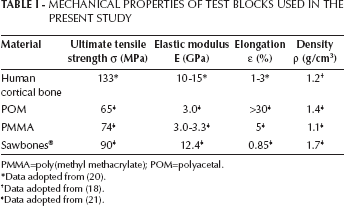
Three synthetic test materials were used: poly(methyl methacrylate) (PMMA), polyacetal (POM) and E-glassfilled epoxy (Sawbones®; Pacific Research Laboratories Inc., Vashon, WA, USA). These materials were used to mimic the compact bone and have been used in previous studies (13, 19). See the detailed list of material properties in Table I, comparing synthetic materials with human bone. Human cadaver bone was used only in insertion torque tests, the detailed results of which were reported earlier (18). Bone mineral density (BMD) is reported to significantly affect screw fixation strength (22, 23). Therefore, BMD was previously determined for the cadaver bones used in this study with high-resolution peripheral quantitative computed tomography (18).
Commercial cortical bone screws (stainless steel AISI 316L; Zimmer Inc., Warsaw, USA) with an outer diameter of 2.7 mm (inner 2.0 mm) and 3.5 mm (inner 2.5 mm) were inserted and pulled out from the test blocks. Each of the test blocks was of 75-80 mm length, 25-30 mm width and 4 mm thickness, and 3 screws were inserted in each block (see Fig. 1). The total number of experiments in each material/coating combination was 6-9. Pilot holes were drilled in the test blocks following manufacturer-specified size recommendations. A constant speed of 5 rpm for the insertion was achieved by an electric motor attached to the servohydraulic test equipment (Instron 8874; Instron, Norwood, MA, USA) maintaining a constant axial load (20 N) on the screws during the insertion. A 10 Nm load cell with an accuracy ± 1% of reading was used to measure insertion and removal torque. Screw insertion was carried out in diluted bovine serum with a total protein content of 24 mg/mL, using standard additives to prevent microbial activity. The additives included penicillin-streptomycin solution (EuroClone S.p.A., Siziano, Italy) and ethylenediaminetetraacetic acid (EDTA)-disodium salt (Merck KGaA, Darmstadt, Germany).

Test setup for inserting the screws and for torque measurements.
After insertion, the screws were pulled out from the test block with a constant displacement speed of 5 mm/min. Servohydraulic test equipment (model 8874; Instron Co, Norwood, MA, USA) with a 1 kN load cell (accuracy ± 1% of reading) and a custom-made pullout clamp was used in the testing.
Interfacial sliding tests
Friction between test blocks and stainless steel or DLC-coated stainless steel was tested by using a pin-on-disk apparatus described in standard ASTM G99-95 (24). For the pin, AISI 316 stainless steel balls 6 mm in diameter (density: 7.96 g/cm3, Brinell hardness: 160-190) were used mimicking the screw material (Goodfellow Cambridge Ltd., Huntingdon, UK).
In the tests, the sample was placed on a rotated holder while the ball was attached to a lever with a dead weight (load). The digital force signal from a strain gauge was recorded, and the CoF was determined.
The diameter of the sliding track was 4.5 mm, and a sliding speed of 3.5 mm/s with an applied load of 9.8-79.0 g was used. A relatively slow sliding speed was used to simulate in vitro testing conditions for torque measurements as per standard ASTM F543-07, and only friction during the initial 50 revolutions (sliding distance 71 cm) was determined for each axial load. Tests were carried out in diluted bovine serum with standard additives as described above.
DLC coating was applied on screws and balls for interfacial sliding tests by ultrashort pulsed laser ablation techniques (Coldab™) developed by Picodeon Ltd. (Helsinki, Finland). High-quality DLC coatings have a high fraction of sp3 bonding, with up to 85% achieved using several deposition techniques (25). Coating thickness in this application was about 400 nm as estimated by interference techniques.
Statistical analysis
One-way ANOVA was used to evaluate differences in insertion torque and pullout
strength for different materials. Student's
Results
Screw insertion and pullout
For both screw sizes, the highest insertion torque values were recorded for Sawbones® and the lowest for human cadaver bone (see Figs. 2 and 3). Insertion torque was significantly higher (P<0.05, 1-way ANOVA) for PMMA and Sawbones® than for cadaver bone.
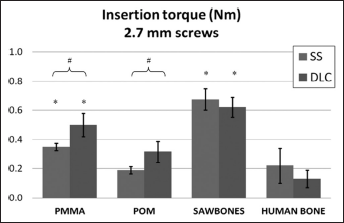
Insertion torque in test blocks for noncoated and diamond-like carbon (DLC)-coated stainless steel (SS) screws with diameter 2.7 mm. *P<0.05, vs. human bone (1-way ANOVA); #P<0.05, SS vs. DLC (t-test).
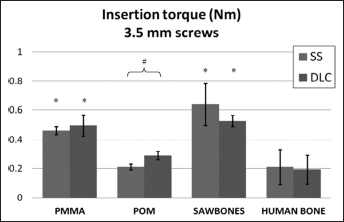
Insertion torque in test blocks for noncoated and diamond-like carbon (DLC)-coated stainless steel (SS) screws with diameter 3.5 mm. *P<0.05, vs. human bone (1-way ANOVA); #P<0.05, SS vs. DLC (t-test).
In the case of pullout strength, Sawbones® had the highest values and PMMA the lowest (see Figs. 4 and 5). Pullout strength for PMMA was significantly lower (P<0.05, 1-way ANOVA) than for Sawbones®. Pullout strength was not tested for cadaver bone due to histological sectioning of the samples required in our previous study (26).
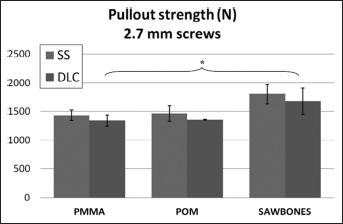
Pullout strength in bone substitute test blocks for non-coated and diamond-like carbon (DLC)-coated stainless steel (SS) screws with diameter 2.7 mm. *P<0.05, PMMA vs. Sawbones® (1-way ANOVA). No significant differences were found between SS and DLC.
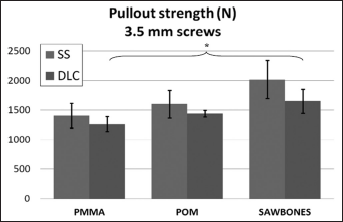
Pullout strength in bone substitute test blocks for non-coated and diamond-like carbon (DLC)-coated stainless steel (SS) screws with diameter 3.5 mm. *P<0.05, PMMA vs. Sawbones® (1-way ANOVA). No significant differences were found between SS and DLC.
Screw insertion torque and pullout strength were greatly affected by mechanical properties of bone substitute test blocks. Table II summarizes the correlations between screw insertion torque, pullout strength and material mechanical properties for synthetic test blocks. Interestingly, pullout strength was highly correlated to elastic modulus of the test blocks, whereas insertion torque was highly correlated to tensile strength of the test block. However, mechanical properties and fixation strength parameters of cadaver bone did not correlate as well as in the case of synthetic materials.
CORRELATION COEFFICIENTS (PEARSON, 2-TAILED) BETWEEN MECHANICAL PARAMETERS OF SYNTHETIC MATERIALS AND FIXATION STRENGTH PARAMETERS FOR EACH OF SCREW TYPES TESTED IN STUDY
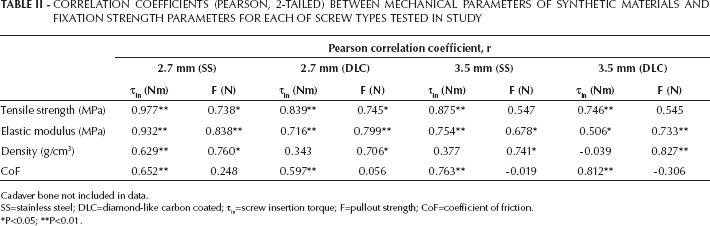
Cadaver bone not included in data.
SS=stainless steel; DLC=diamond-like carbon coated; τin=screw insertion torque; F=pullout strength; CoF=coefficient of friction.
P<0.05;
P<0.01.
Interfacial sliding between test blocks and screw materials
The CoF was determined for human cadaver bone and 3 bone substitute materials against stainless steel (SS) and DLC-coated SS (see Fig. 6). For SS, CoF was significantly (P<0.05, ANOVA) lower in bone than in the substitute materials (μ=0.09±0.04, 0.19±0.01, 0.31±0.01 and 0.29±0.03 for bone, POM, PMMA and Sawbones®, respectively). Also for DLC, CoF was significantly lower in bone than in substitute materials (μ=0.09±0.04, 0.20±0.03, 0.38±0.06 and 0.31±0.03 for bone, POM, PMMA and Sawbones®, respectively). However, no significant difference in these short-term tests of CoF was achieved by DLC coatings. In the tests for initial friction, CoF was not significantly affected by the axial loading in any of the materials.
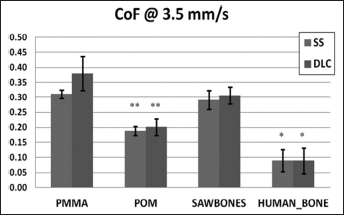
Coefficient of friction (CoF) between diamond-like carbon (DLC)-coated and noncoated stainless steel (SS) and tested materials. *P<0.05, vs. all other materials; **P<0.05, vs. PMMA and Sawbones® (1- way ANOVA). PMMA=poly(methyl methacrylate); POM=polyacetal.
CoF correlated strongly to screw insertion torque. For SS screws, correlation coefficients were r=0.652 and r=0.763 for 2.7-mm and 3.5-mm screws, respectively (Pearson 2-tailed). Similarly for DLC-coated screws, correlation values of r=0.597 and r=0.812 were determined for 2.7-mm and 3.5-mm screws, respectively.
However, pullout strength of bone substitute materials did not strongly correlate to CoF. For SS screws, correlation coefficients r=0.304 and r=0.061, and for DLC-coated screws, r=-0.112 and r=-0.307, were determined (for 2.7-mm and 3.5-mm screws, respectively; Pearson 2-tailed).
Discussion
This study examined the effect of interfacial sliding and test material properties on the fixation strength and insertional properties of self-tapping bone screws. Comparison was made also between human bone and substitute materials to find a homogenous/isotropic material modeling human bone in these modes of in vitro mechanical tests. Generally, the study showed that the mechanical properties of test blocks and the CoF have a significant influence on screw fixation strength and screw insertion torque.
Cadaveric bone specimens would be the most biomechanically appropriate model for simulating clinical cases. However, the bones have a number of associated difficulties, such as decomposition and variability in mechanical properties. Studies in the literature have demonstrated a variability in geometric and material properties within and between different cadaver subjects, which is not optimal for biomechanical testing. Thus, the use of bone substitute materials have been justified and recommended for in vitro tests by many researchers (9, 13, 19). The findings of this study also illustrate the difficulty in choosing a material resembling human bone for biomechanical testing. Each substitute material has pros and cons with respect to the type of mechanical testing.
The present study showed that the pullout strength in bone substitute materials was highly correlated with elastic modulus, tensile strength and density of test block. The pullout strength for POM was statistically similar to PMMA and Sawbones® with both screw sizes. In pullout, there were no significant differences with respect to surface modification. The results from the pullout tests are regarded primarily as a measure of bone (material) quality around the fixture. This is due to screw thread design transferring stresses to the surrounding material (27). Thus, the reduction in modulus of elasticity, tensile modulus or tensile strength would clearly impact the fixation strength, stiffness and durability of orthopedic implants also in clinical use (13).
According to our results, screw insertion torque was highly correlated to elastic modulus, tensile strength and CoF. The insertion torque for POM was statistically similar to that of cadaver bone with both screw sizes. Nevertheless, the mechanical properties of POM differ from those of human bone. Yet, insertion torque is reported to be mostly affected by screw design and geometry, such as core diameter and thread pitch (8). In general, our results were fully comparable to previous studies with similar materials and screws (8, 13, 19). Insertion torque, however, did not show a good correlation to human bone's mechanical properties. One would suspect from the mechanical parameters (Tab. I) that strong and stiff bone shows high insertion torque while the mechanical testing reveals conflicting findings (Figs. 2 and 3). This results from the inhomogeneous structure of bone, as well as from biological elements (lipids, proteins) in bone, which beneficially affect the sliding properties of the screws.
DLC coating has the potential to adjust the CoF, as shown in earlier studies (15, 16, 28). This suggests that DLC coatings could also be used to reduce insertion torque (or removal torque) and to increase fixation stability in orthopedics via reducing wear and corrosion with long-term exposure in the severe body environment. In this study, CoF was not affected by a smooth DLC coating in the bovine serum–lubricated setup. The tribological properties (both dynamic and static) of DLC films have been thoroughly investigated in the past, showing that their CoF greatly depends on experimental conditions (15, 16, 29). Thus we consider that the use of bovine serum in testing of CoF simulates well the clinical environment. Interestingly, significantly lower CoF values were recorded for human bone than for substitute materials against either SS or DLC. This finding needs better attention in further studies to understand sliding at the bone–implant interface and the role of bone components. Thus, a proper model for human bone was not found with respect to interfacial sliding properties.
Further, the DLC coating had a controversial effect on screw fixation properties in this study. Interestingly, insertion torque was lower for DLC-coated screws with Sawbones® and human bone. These materials have the highest tensile strength and elastic modulus. Thus, a DLC coating seems to perform better with stronger materials. Insertion torque seems to increase with DLC-coated screws in standard materials with lower strength. This may be due to carbon–carbon interactions between polymer (i.e., PMMA and POM) and DLC. In composite materials (i.e., Sawbones® or human bone), this interaction will not occur. Furthermore, pullout strength tends to decrease with DLC, but not significantly.
In vitro fatigue testing of fracture fixation is typically performed for biodegradable materials in an environment simulating human body conditions (30). However, fatigue tests can also reveal the long-term interfacial behavior of metallic implants like bone screws and fixation plates with novel surfaces and coatings, and thus, they should be considered.
Conclusion
Further development of novel coatings may produce coatings with exceptional interfacial properties (such as hardness, smoothness and inertness) improving either bone–implant interaction or tribology, depending on the application. Thus, interfacial factors should be taken into account in the development process for biomedical implants. In vivo tests are required to approve the behavior of DLC coatings in long-term physiological use, and the bone–implant interaction is the most crucial factor to be investigated. However, in vitro testing is also needed for initial testing of hypotheses, but one should also consider proper testing material for each application. In the case of bone screws, testing of fixation strength is fundamental. The CoF in this study was significantly lower in human bone than in the substitute materials. This finding needs to be studied further.
Footnotes
Acknowledgements
Ms. Anna-Maria Tikkanen is acknowledged with great appreciation for her help with the CoF experiments.
Financial support: The authors wish to acknowledge the financial support from the National Graduate School of Musculoskeletal Disorders and Biomaterials, Scandinavia-Japan Sasakawa Foundation, Finnish Cultural Foundation, North Savo Regional Fund and Emil Aaltonen foundation.
Conflicts of interest: None.