Abstract
Purpose
This paper provides a review of the evidence regarding the economic evaluation of family therapy and family-based therapies when delivered to children and adolescents.
Methods
Eight databases were searched for published studies and grey literature. We included studies where both costs and effectiveness were evaluated. Due to the substantial differences in interventions, setting, disease area, and sample, we conducted a narrative summary.
Results
Sixteen studies were included in the review. Most studies undertook a cost-effectiveness analysis (CEA; n = 14) and among those, 1 study additionally carried out a cost-utility analysis. Four studies evaluated the cost-benefit analysis (CBA) of family based intervention, two studies only carried out a CBA while the 2 other studies included both CBA and CEA. The review showed the broad types of family-based interventions and the range of psychological disorders and addictions for which they can be used. Family-based interventions focusing on children and adolescents’ health disorders were found to be cost beneficial for all the studies that used CBA, and to be cost effective in two-thirds of the studies that used CEA.
Conclusions
Recommendations resulting from the review are that future research should include health care costs beyond costs to the health care sector related to delivering the therapy and the spillover effects to the rest of the family, and should consider cost and effectiveness over a longer time horizon.
Introduction
Economic evaluation is a key component of health care decision making in the appraisal of new interventions, services, and technologies. It is particularly relevant in England where the National Institute for Health and Care Excellence (NICE) recommends which drugs and treatments the National Health Service (NHS) should fund. They base their guidelines on a methodological “reference case” that favors one type of economic evaluation, namely cost-utility analysis (CUA) with fully incremental analysis (1). This paper reviews the evidence on the economic evaluation of family-based therapy as an intervention for children and adolescents. There are various forms of family-based therapy; it commonly focuses on relationships within a family and is not solely delivered to the children and adolescents but it also involves their family members. Family-based therapy aims at maximizing cohesion, attachment, adaptability, support, and warmth while reducing maltreatment and scapegoating, and moderating parental control (2). Family-based therapy is manual based and delivered by trained therapists. Several studies have already shown the effectiveness of family therapy and family-based therapy against other types of psychological support or treatment for young people or children for various mental health conditions, including reducing overweight, obesity, self-harm, and suicidal behavior (3–6). A number of other studies have investigated the cost of delivering family therapy using administrative records within a large health care organization, insurance claims, or the Medicaid system, and found it less expensive, which led to fewer repeated episodes of care (7–11). However, the joint evidence of the cost and the effectiveness of family therapies appears to be modest despite the high relevance for policy to establish the value for money that family-based therapies and – more generally – any psychotherapeutic intervention could represent.
Reviews on economic evaluation with a larger scope, including any types of mental health interventions or services for children and adolescents, have already been undertaken (12–16). The first contribution to the area was made by Knapp (12), who identified a handful of literature references and made a compelling argument for increasing the use of economic evaluation in children and adolescents’ mental health decisions. He demonstrated how commissioners, clinicians, and researchers relied on economic analysis to obtain the best value from resources allocated to the planning and provision of services for children and adolescents with mental health problems. The general conclusion of the reviews of the past 20 years is that the number of studies where both costs and health outcomes of mental health interventions and services for children and adolescents are assessed has increased, but still remains limited, particularly compared to mental health interventions in the adult population.
Our review differs from previous reviews in 2 ways: it focuses on 1 type of intervention: family therapy or family-based therapy for children and adolescents, and it is not limited to a specific type of mental health or health condition.
We describe the methods we used for the identification of relevant studies, present the results of the literature review, and then discuss these results. We conclude with an exploration of further avenues of research.
Methods
Search strategy
The literature search aimed to identify studies on economic evaluations of family-based intervention therapy for children and adolescents. We searched the following databases in February 2015 from their inception dates to the present: CINAHL (EBSCO), Cost Effectiveness Analysis Registry (CEVR, Tufts Medical Centre), Embase Classic, Embase (Ovid), IDEAS (RePEc), NHS Economic Evaluation Database, Ovid MEDLINE (R), and PsycINFO (Ovid).
The searches were designed to identify studies on the cost and the effectiveness of family-based intervention for young persons by combining the search concept “children” or “adolescent,” and “family therapy” or “family intervention,” with the concepts “economic evaluation” or “cost effectiveness.” A full detail of the search strategy for Medline database is presented in Appendix A (available online at www.grhta.com) and full search strategies for all databases are available from the authors upon request. Bibliographies of included studies were also searched for relevant studies.
Inclusion criteria
To be eligible for inclusion, the studies had to evaluate both costs and effectiveness. We used the economic evaluation CHEERS checklist developed by Husereau et al (17) as a guide for best practice when conducting economic evaluations, and we only selected studies for full review where the 2 components of an economic evaluation were measured: costs and health-related effectiveness. Evaluations of family-based interventions focusing on cost only or on outcomes only were excluded. In addition, we excluded studies that reported qualitative data and literature reviews; studies that lacked quantitative data; studies in developing countries; and studies in which the language was not English. Also, studies that evaluated family-based intervention for adults, or studies where the impact of parenting interventions was measured on parents only were excluded, as the main focus of the review was to analyze the impact on children or young people. We did not apply any specific criteria for the family-based therapy and included any therapy where the family was involved. Similarly, we did not specify inclusion criteria for the disease areas, assuming that family-based therapies were likely to focus on mental health and behavioral disorders. Finally, we did not set any publication date limit, and studies were searched spanning almost 70 years (1946-2015).
Data collection and analysis
To select studies for the review, titles and abstracts were screened by 1 researcher using the above inclusion criteria; this process was managed using Endnote Software. When the decision to include or exclude a study was not straightforward, a second reviewer was consulted to resolve uncertainty. The detailed process of article selection was presented in a PRISMA chart (18). Once the included studies were identified, data were extracted using a form developed for this purpose. For each study, we extracted the following: cost perspective, type of economic evaluation, study population, country, outcome measures and length of follow-up, type of family based intervention, and sensitivity analysis. Due to the substantial differences in interventions, settings, disease areas, and samples, a meta-analysis was not conducted. Instead, a narrative summary of the included studies is presented below.
Results
The literature search yielded 1,322 potentially relevant studies. After the removal of duplicates, 920 references were identified for screening. In addition, 3 studies were identified scanning from a related review. In total, 923 titles and abstracts were screened of which 886 studies were excluded and 37 possibly relevant studies were retrieved for full-text assessment. After full-text review, 16 studies were included in the analysis and 21 studies were excluded. Studies were excluded because: 6 only focused on outcomes; 9 evaluated a parenting program; 4 were a family-based intervention for adults; 1 did not include family therapy as an intervention; and 1 was not a cost-effectiveness analysis (CEA). A PRISMA chart describing the inclusion and exclusion process is shown in Figure 1.
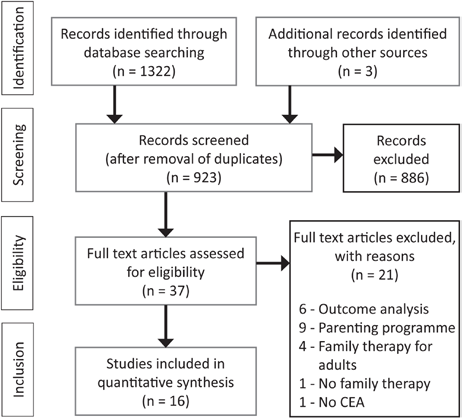
Flow diagram of excluded and included studies.
Description of included studies
Of the 16 studies included in the review, 9 were from the USA, 3 from the UK, and 1 each from the Netherlands, Canada, Sweden, and Finland (Tab. I). The majority of the studies were published during the last 10 years (9 studies from 2007 to 2014), 4 in the first half of 2000, and 3 before 2000 (1988, 1989, 1999).
Methodology of included studies
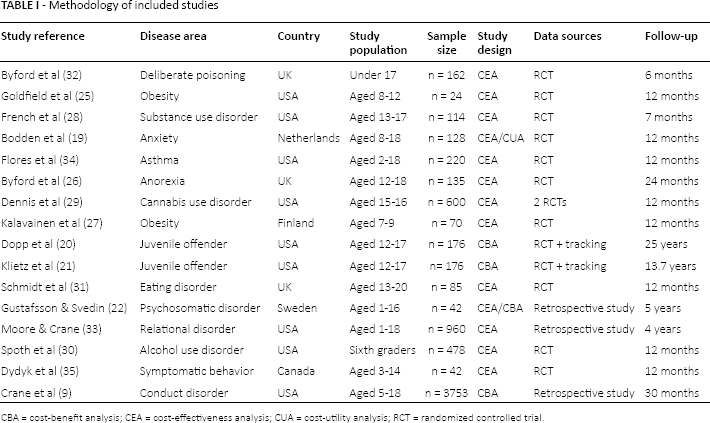
CBA = cost-benefit analysis; CEA = cost-effectiveness analysis; CUA = cost-utility analysis; RCT = randomized controlled trial.
The studied populations comprised children and/or adolescents aged between 1 and 20 years old. Family-based interventions were assessed in four main disease areas; (i) eating disorders, such as obesity or anorexia (n = 4); (ii) mental health or psychosomatic disorders, including anxiety, deliberate poisoning, or asthma (n = 5); (iii) substance use disorders (alcohol, cannabis) (n = 3); and (iv) conduct disorders, including juvenile offenders (n = 4). Most of the analyses (n = 11) used data from randomized control trials. They included, on average, 187 (standard deviation [SD]: 184.4) participants, and the follow-up period ranged from 6 months to 24 months with most trial studies using a 12-month follow-up (n = 8/11). Three studies were based on retrospective cohort studies and included a larger number of participants (on average 1,585 [SD: 1932]) that were followed between 30 months and 5 years. Finally, the 2 juvenile offender studies relied on a sample of participants from a trial, which were then followed on a longer term for a cost-benefit analysis (CBA). They each included 176 participants and the duration for the follow-up was 13.7 years and 25 years, respectively.
Most studies undertook a CEA (n = 14) and among those, 1 study additionally carried out a CUA (19). Four studies evaluated the CBA of family-based intervention, 2 studies only carried out a CBA (20, 21), while the 2 other studies included both CBA and CEA (9, 22).
Design of interventions
The studies included in the review showed a variety of designs of family-based interventions including family therapy (n = 5), multi-systemic therapy (n = 2), functional family therapy, multidimensional family therapy, intensive family therapy, joint family therapy and cognitive behavioral therapy (CBT), family CBT, and other family-based programs (Tab. II). There were 3 main characteristics that appeared to distinguish between family therapies in general. First, therapies could be delivered either in group (several families in a session with 1 therapist) or in individual sessions (1 family with 1 therapist) (23). Second, the intervention could be based at home (therapist's visits), at the hospital, or in a community practice. Finally, sessions could be delivered to the whole family (parent + child) or in separate session (parent only, or child only). Separate session for parents or caregivers usually took the form of parental counselling with a therapist (24).
Design of the family-based therapy
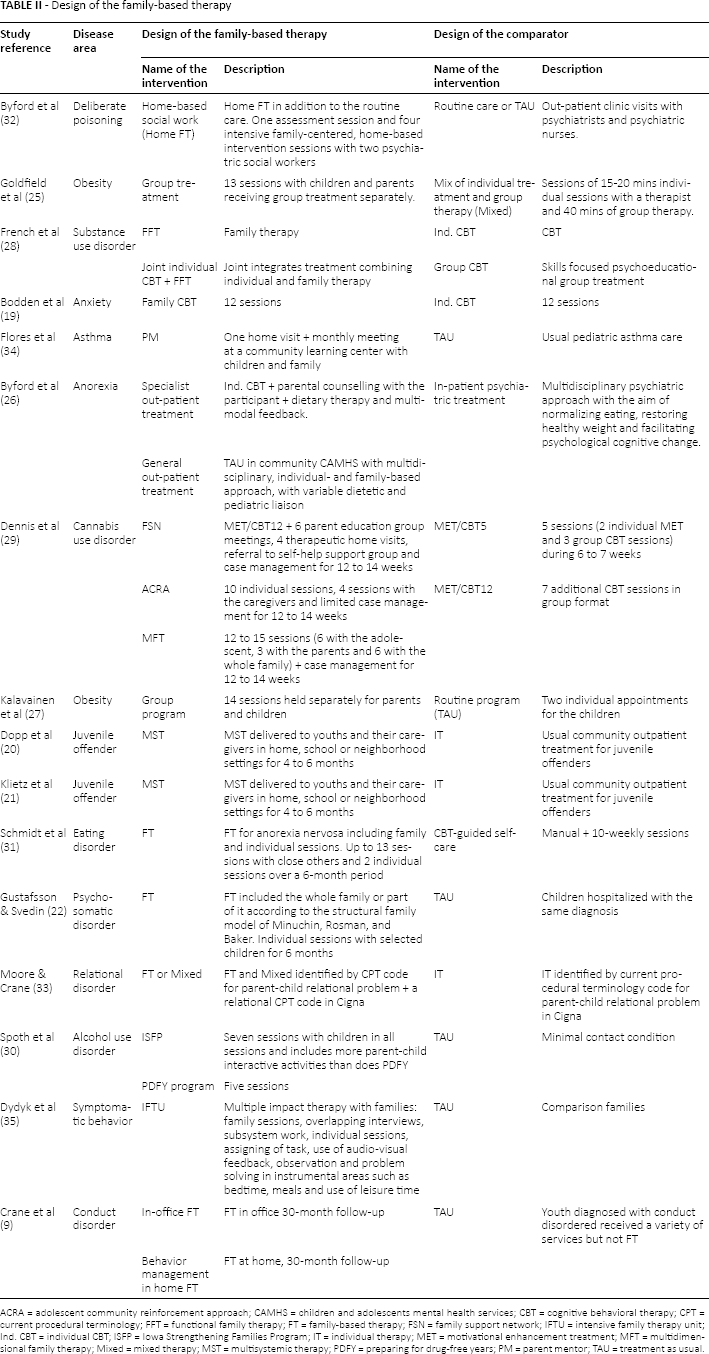
ACRA = adolescent community reinforcement approach; CAMHS = children and adolescents mental health services; CBT = cognitive behavioral therapy; CPT = current procedural terminology; FFT = functional family therapy; FT = family-based therapy; FSN = family support network; IFTU = intensive family therapy unit; Ind. CBT = individual CBT; ISFP = Iowa Strengthening Families Program; IT = individual therapy; MET = motivational enhancement treatment; MFT = multidimensional family therapy; Mixed = mixed therapy; MST = multisystemic therapy; PDFY = preparing for drug-free years; PM = parent mentor; TAU = treatment as usual.
In more than half of the studies, family-based interventions combined treatment sessions with the whole family, sessions with only 1 parent or caregiver, and additional sessions with the treated child only. Group sessions, where parents and children were seen separately, were most often used in the treatment of eating disorders (25–27). On the other hand, family therapies designed to treat mental health disorders or substance use disorders usually comprised family sessions with a therapist.
Comparison groups for the study included treatment as usual (n = 7), individual therapy (n = 5), individual CBT (n = 3), group CBT (n = 1), and a mix of both individual and group therapy. Several studies evaluated more than 1 family-based intervention and presented a study design with more than 2 treatment arms (9, 26, 28–30).
Outcome measures
Figure 2 presents the frequency of the outcomes and the cost measurements used across the 16 studies, and Table I in Appendix B (available online at www.grhta.com) provides an extended description of those. In the majority (13 out of 16) of the included studies, effectiveness was measured using health outcome measures. More specifically, the effectiveness of family interventions in eating disorder conditions was assessed using weight loss, such as the reduction in body mass index units (25, 27) and a change in the Morgan–Russell Average Outcome Scale (MRAOS) for patients with anorexia (26), or the abstinence rate from bingeing or vomiting at the end of the follow-up period (31). In the area of substance use disorders, the effectiveness of family-based interventions was evaluated as a change in the number of days of abstinence from cannabis use (29), the abstinence from marijuana use (28), or the number of case of alcohol use disorder prevented (30). For mental health disorders, health outcomes were measured as a change in the suicidal ideation scale and hopelessness (32), the number of anxiety-free days (19), or the return rate to therapy (33). Finally, the study on asthma used the reduction in asthma symptoms as a health outcome (34). Some studies used health care use and the reduction in hospital length of stay as measures of effectiveness (22, 35).
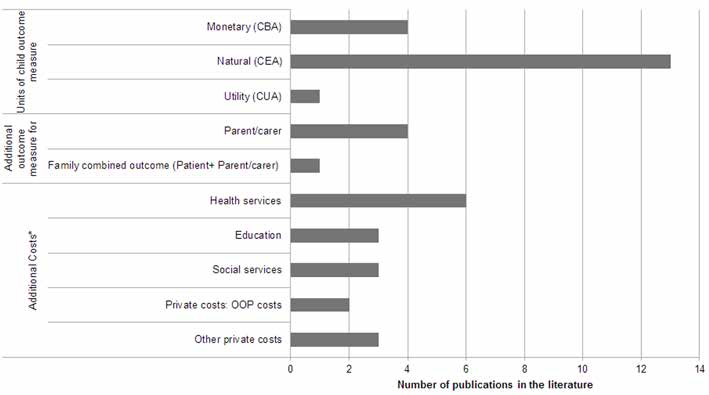
Types of outcomes and costs studied in the literature.
CBA measured the effectiveness in monetary value and was used in 4 out of 16 studies. In 2 studies, it represented avoidance of crime victim expenses related to family interventions for juvenile offenders and savings to the taxpayer (20, 21). The 2 other studies combining both CEA and CBA considered effectiveness as an overall reduction in health care expenses induced by family therapy for children with conduct disorders (9, 22).
Utility values were measured in 1 study only (19); quality-adjusted life years (QALYs) were generated from the generic health-related quality of life instrument EQ-5D (36) to evaluate the effectiveness of family therapy compared to individual therapy in the treatment of anxiety, in addition to the proportion of anxiety-free days.
As family therapy involves parents, care givers, brothers, sisters, or other close relatives and friends, 4 papers had interestingly looked at the impact of the treatment on relatives participating in the therapy in addition to the impact of the therapy on the adolescent/child patient. In 1 study (32), parents completed the General Health Questionnaire along with a treatment satisfaction questionnaire. They found that parents randomized in the family-based intervention were more satisfied than parents of the controls for children with deliberate self-poisoning at 2 months follow-up. Another study (25) looked at the impact of family therapy on the weight loss of parents along with the reduction of weight of children. Similarly, the asthma study (34) investigated the effectiveness of the interventions on the quality of life of care givers using the Pediatric Asthma Caregiver's Quality of Life Questionnaire (PACQLQ). Finally, only 1 study assessed the effectiveness of the intervention on the whole family. Bodden et al (19) collected EQ-5D scores of parents and children, and calculated family-based QALYs to evaluate the effectiveness of the intervention for clinically anxious children.
Cost measures
Economic evaluation studies require that cost components are specified precisely and presented in a disaggregated form. All 16 studies included the direct cost related to the delivery of the intervention; however, only 6 studies included additional costs.
One study (9) adopted a health-sector-cost perspective, including all Medicaid billed costs for pharmacy, hospital, and professional services for 30 months. Two studies adopted a broad service-providers’ perspective, and included costs related to any use of health, social, and educational services within the public perspective. More specifically, Byford et al (32) considered the costs of using health and social services, including hospital services, primary care, social worker and community care, foster and residential care, counselling by practice nurses, clinical psychologists or school counsellors, as well as the costs of educational welfare officers, psychologists, school doctors, and school nurses over the 6-month study period. Similarly, Byford et al (26) considered costs related to health, social services, education, and the voluntary and private sectors, including hospital contacts, private-sector inpatient stays, community health and social services, schooling, and medications at the 1- and 2-year follow-up points in the study.
The 3 other studies additionally considered costs to the family and adopted a societal perspective on costs (19, 31, 34). Bodden et al (19) included direct health care costs (e.g., contact with the GP, psychologist, psychiatrist, and the medication), direct non-health-care costs (e.g., paid housekeeper, day nursery, informal care), indirect costs (paid work, unpaid work, loss of leisure time, household work, school absence) and out-of-pocket costs related to health care use. The cost diaries used in the study recorded the resources used by all family members (child, sibling, mother, or father) as well as the reason for the resource use at the 3- and 6-month follow-up points; their analysis then only included family resource use related to the child's anxiety. Flores et al (34) estimated the total cost of the intervention including the program costs (personnel involved, payments to parents mentors, training sessions, monthly meetings, bus fares), direct medical costs (charges to emergency department visits and hospitalizations), and indirect income costs of missed work days for the employed caregivers. Finally, Schmidt et al (31) included adolescents’ public sector costs, such as education (e.g., home tuition, individual help in class, contact with the school nurse, educational psychologist, educational welfare officer, meeting with tutors, any educational support), health and social care service costs for the child (e.g., hospital care, primary care, A&E care; specialist services, e.g., dietician, psychiatrist, and child development center, social worker), and costs for family members (GP, outpatient appointments, and psychiatrist or psychologist). In addition, they included costs to the family and the patient as a consequence of bulimia nervosa, such as the cost of lost employment and families’ and patients’ out-of-pocket expenses. The costs were collected at baseline, and at 6- and 12-month assessments.
Is family therapy cost effective?
The results of the economic evaluation for each study are summarized in Table III. At the end of the follow-up period, of the 16 included studies, 11 concluded that family-based therapy was clearly cost beneficial and cost effective compared with the different comparators, and for various types of health outcomes, while another 2 studies found it cost effective under specific conditions. Byford et al (32) found no difference in cost or in effectiveness on the whole sample, but found that family therapy improved suicidal ideation for a subgroup of patients with major depression. Similarly the paper by Byford et al (26) showed no significant difference in the cost-effectiveness of family therapy compared to routine care in hospital, but the family-based outpatient treatment had the highest probability of being cost effective when uncertainty was taken into account. Family-based therapy was found to be cost beneficial for studies on juvenile offenders (20, 21) and cost effective for conduct disorders (9). It was also found to be cost effective for most of the studies on mental health, psychosomatic, and relational disorders. We note that family therapy was found both cheaper and more effective than treatment as usual for patients with asthma (34) and patient with psychosomatic disorders (22), and it was found cheaper and with equal effectiveness than the comparator for adolescents with symptomatic behaviours (35) and relational disorders (33). An exception to the cost effectiveness of family-based therapy for mental health disorders is the study on clinically anxious children (19), which showed that family CBT compared with individual CBT was of equal cost and effectiveness, but concluded that individual CBT had the highest probability of being cost effective in both cost per anxiety-free child and cost per QALY when modelling the CEA.
Is the family-based therapy cost effective?
Cost effectiveness result at the end of the last follow-up period.
ACRA = adolescent community reinforcement approach; BMI = body mass index; BMI-SDS = BMI standard deviation score; CBT = cognitive behavioral therapy; FFT = functional family therapy; FSNM = family support network meetings; FT = family-based therapy; Ind. CBT = individual CBT; ISFP = Iowa Strengthening Families Program; MDFT = multidimensional family therapy; MRAOS = Morgan–Russell Average Outcome Scale; PDFY = preparing for drug-free years; TAU = treatment as usual; PM = parent mentor; QALY = quality-adjusted life year.
While family-based therapy is found to be cost effective for children with obesity (25, 27) and anorexia (26), it was found to be more expensive and equally effective as self-guided CBT for adolescents with bulimia nervosa (31). Schmidt et al (31) concluded that family therapy is more costly and equally effective than individual self-guided CBT in the treatment of eating disorders. Most of the studies on substance use – except the study on alcohol – did not give evidence that family-based therapies were cost beneficial or cost effective when compared to another intervention, and this was mainly due to family-based therapies being more expensive than the comparator, and of equal or lower effectiveness. Dennis et al (29) found that the Family Support Network was more costly and less effective in the treatment of a cannabis use disorder. French et al (28) found no difference in effectiveness between treatments including family-based, individual, and group cognitive behavioral approaches. However, individual group-based therapy are the least costly compared to functional family therapy.
Discussion
The results from the literature review show diversity of 2 kinds. First, there is diversity in the types of family-based intervention being evaluated as previously stated by Pote et al (37). Second, family-based intervention is used to treat a broad range of psychological disorders and addictions among children and adolescents. Based on the included studies, we found that family-based interventions focusing on children and adolescents’ health disorders are cost beneficial for the 3 studies that used CBA, and are cost effective in two-thirds of the studies that used CEA. If we focus on the best practice guidelines for conducting economic evaluations (1, 38), this review shows that the quality of economic evaluations of family-based interventions for young people and children is limited. We develop this further in this section.
In the majority of the papers, the cost analysis only included the cost to the health care sector to deliver the intervention. Few papers included health resource use consecutive to the intervention (e.g., medications, GP visits, etc.) over a key time horizon that is long enough to reflect all the important differences in costs between the treatments being compared. Only 3 papers considered the costs from other public sectors, such as education, justice, or social services, despite 1 study underlying that family-based interventions have an impact on the resource use of children and adolescents in several public sectors, which are important to take into account in economic evaluations (32).
Regarding consequences and, more generally, effectiveness measurement, the NICE reference case recommends the use of a health outcome that not only is reliable for the comparison between competitive interventions, but also is appropriate for measuring the marginal impact of the health care decisions the policy maker will make for a broad range of treatments within the same budget. In this context, health effects should be expressed in terms of QALYs, which is currentlyconsidered to be the most appropriate generic measure of health benefit that reflects both mortality and health-related quality of life (1). While NICE states that EQ-5D is the preferred measure of health-related quality of life in adults, there is no consensus on the best health-related quality of life instrument to use in children and young people (39). Recent reviews of literature have identified several preference-based instruments being used to assess children's utility, including the young people modified EQ-5D, the Child Health Utility 9 dimensions (CHU-9D), the Health Utility Index II (HUI II) or the proxy-respondent EQ-5D (40, 41). In our review, only 1 study undertook a CUA using QALYs as the outcome and found individual CBT to be more cost effective than family CBT therapy (19). The paucity of utility data in economic evaluation of children interventions has already been highlighted (40) and this raises an important issue to inform resource allocation decisions across different treatments and health conditions.
With family-based therapies, there is potential to account for additional health benefits for relatives and carers in the economic evaluation. Several studies in the review collected parents or carers’ outcomes and used them as additional outcomes of interest in a cost-effectiveness analysis (25, 32, 34), and 1 study combined both children's and parents’ outcomes (19). The combination of benefits beyond the patient is not specifically stated in the NICE reference case, and relies on the strong assumption that QALYs can be aggregated across individuals as a simple additive aggregation. Whilst this has been done in prior studies on child health (42), and would be consistent with other health economic research showing benefits to other family members (43), such considerations require a theoretical justification and a discussion on the interdependence between the utility functions of children and adolescents and of the parents, as well as a consensus on how best to measure utility in children.
In an economic evaluation, the costs and benefits require an optimal length of follow-up or a time horizon that is long enough to reflect substantial differences in costs or consequences between the treatments being compared. If the analysis is undertaken within a trial follow-up, then the economic evaluation will be restricted to that horizon. However, one could easily imagine that therapies, such as family therapies, can process beyond the sessions that are attended with teenagers in the longer term, reflecting on the therapy; therefore such interventions are likely to keep on giving and improving the individual's wellbeing beyond the trial follow-up. Decision analysis modelling is the preferred method in this context; it consists of extrapolating the costs and consequences using probabilities and assumptions based on the data collected in a trial and data extracted from the literature. None of the papers in the review evaluated the long-term economic evaluation of family-based therapies using a decision analysis model. This probably comes from the fact that children and adolescents face such a large number of events over their life, and such a decision analysis model would carry a high level of uncertainty, especially if a lifetime horizon is considered. A mitigating strategy could be to consider a shorter time horizon, such as reaching the age of 25, which is considered to be the age when the adolescent brain is fully developed.
The strengths of this review include conducting a comprehensive search to identify all published and unpublished studiesestimating the economic evaluation of family-based therapies for children and adolescents in developed countries. To the best of our knowledge, this is the first review in that area. While we tried to minimize biases during the review, we found that due to the high heterogeneity and diversity of the comparison groups in studies, it was not appropriate to conduct a meta-analysis. In addition, due to limited capacity, we were unable to include non English-language studies. While every effort was made to identify all relevant articles, it is also possible that we may have missed some unpublished grey literature. The aim of this review was to find studies that undertook an economic evaluation of family-based interventions in children and adolescents and it discussed a number of limitations that are specific to the children and adolescents’ health context. Therefore, the findings of this review are unlikely to be generalizable to the economic evaluation of family-based therapy in an adult population.
Conclusion
While a number of studies in North America and Europe have simultaneously considered the cost effectiveness, clinical effectiveness, or health benefits of family-based therapies to treat young people and children with various conditions, few have conducted an economic evaluation considering costs beyond the delivery of the therapy. As family interventions have been found effective, particularly with children and adolescents (44–46), we suggest that future economic evaluations of family-therapies should include costs related to consecutive health care use over a longer time horizon. Methodological and theoretical concepts currently under development in health economics regarding the best way to account for potential spillover health benefits on families, and to validate utility measurements for the children and adolescent population, will also be key to guide the economic evaluations of family interventions for children and adolescents.
Footnotes
Acknowledgments
This review research was undertaken as part of the National Institute for Health Research Health Technology Assessment Programme (project number: 07/33). The views expressed in this publication are those of the authors and do not necessarily reflect those of the HTA programme, NIHR, NHS, or the Department of Health. The final revisions of the article have been conducted when Sophie Guthmuller took service at the European Commission, Joint Research Centre. The scientific output expressed does not imply a policy position of the European Commission. Neither the European Commission nor any person acting on behalf of the Commission is responsible for the use which might be made of this publication. The authors would like to thank Judy Wright and Kirstine McDermid for literature searches; and Joachim Marti and two anonymous reviewers for comments on an earlier version of the manuscript.
Financial support: None.
Conflict of interest: None of the authors has financial interest related to this study to disclose.
