Abstract
Drug-resistant forms of tuberculosis (TB), particularly multi- and extensively drug-resistant TB, represent an important obstacle to global control of the disease. Recently, new drugs, repurposed drugs, and new drug combinations have been evaluated, with a number showing promise for the treatment of drug-resistant TB. Additionally, a range of methods for accelerating mycobacterial culture, identification, and drug susceptibility testing have been developed, and several in-house and commercial genotyping methods for speeding drug resistance detection have become available. Despite these significant achievements in drug development and diagnostics, drug-resistant TB continues to be difficult to diagnose and treat. Significant international efforts are still needed, especially in the field of clinical and operational research, to translate these encouraging developments into effective patient cure and make them readily available to resource-constrained settings, where they are most needed.
Keywords
Introduction
Tuberculosis (TB) continues to cause more deaths worldwide than any other infectious disease. The World Health Organization (WHO) estimated that in 2011, there was 8.7 million cases of TB, with nearly 1 million deaths among HIV-negative cases and 0.43 million deaths associated with HIV infection. 1 More than 99% of deaths and 95% of new TB cases occur in middle- and low-income countries. 2 Together with the AIDS pandemic, the emergence of multidrug-resistant (MDR) TB contributed substantially to the resurgence of TB towards the end of the 20th-century, just when the disease was thought to be on the verge of elimination. MDR-TB poses a serious problem worldwide because its definition implies simultaneous resistance to the two most effective drugs available for treating TB, including isoniazid (INH) and rifampicin (RIF). The last reported data on global TB drug resistance shows the highest MDR-TB rates ever observed. 3
Shortly after the advent of TB chemotherapy in the late 1940s, drug-resistant strains of the causative agent, Mycobacterium tuberculosis, were noted to emerge upon mono-therapy, a finding that promoted the early design and administration of combined drug schemes. Today, drug-resistant TB is difficult to diagnose and treat. It poses a challenge not only to the clinical management of individual patients but also to the success of rational public health interventions designed to control the disease. One such intervention, and a primary one, is the directly observed therapy, short course (DOTS) strategy, which includes universal administration of standardized therapeutic schemes containing first line anti-TB drugs, including INH, RIF, pyrazinamide, and ethambutol. The global implementation of DOTS has contributed to reduce global TB rates but is insufficient to curb TB when implemented alone in settings with high levels of drug-resistant TB.4,5
Drug-resistant TB is a form of disease caused by tubercle bacilli with resistance to any anti-TB drug and can be classified in mono-, poly-, multi-, and extensively drug-resistant TB (see Box 1). MDR-TB is a major cause of treatment failure and its quantification is regarded as a reliable measure of the drug resistance problem in a given setting. Standard six-month schemes with first-line drugs are ineffective in MDR-TB cases, which require at least two-year treatments with less powerful, more harmful, and more costly second-line drugs. It should be emphasized, however, that all forms of drug-resistant TB are dangerous since administering a standard therapeutic scheme to an undetected case of mono-drug resistance to INH or RIF can easily lead to amplification of drug resistance. 6 For this reason, international organizations led by WHO currently recommend that the programmatic management of drug-resistant TB should address all its forms as a whole, from mono-drug-resistant TB to extensively drug-resistant TB (XDR-TB). 7
Classification of drug-resistant tuberculosis.
Globally, 3.7% of new TB cases and 20% of previously treated TB cases were estimated to be MDR-TB cases in 2011. There were an estimated 310,000 (range 220,000–400,000) MDR-TB cases among notified TB patients with pulmonary TB. Nearly 60% of these cases were reported in India, China, and the Russian Federation (Fig. 1). Extensively drug-resistant TB (XDR-TB) has been identified in the 84 countries where it was investigated (Fig. 2). The average proportion of MDR-TB cases with XDR-TB is 9.0% (6.7%–11.2%). 1
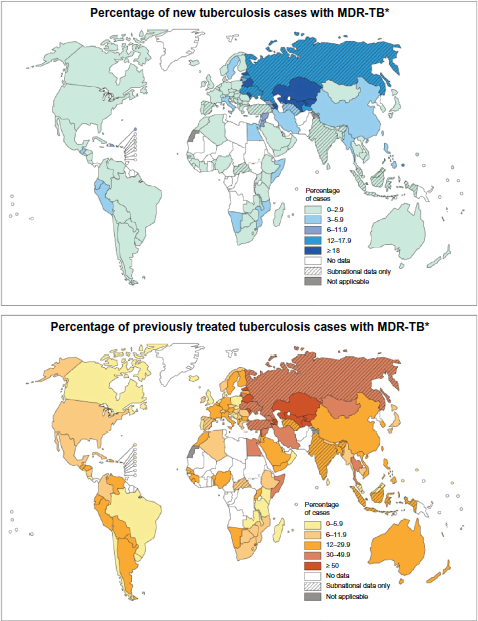
New (above) and previously treated (below) cases of tuberculosis with multidrug-resistant tuberculosis in the world.a
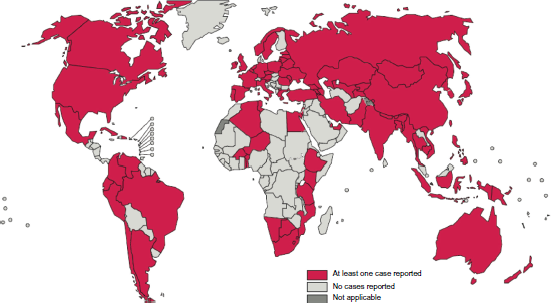
Countries reporting at least one case of extensively-drug-resistant tuberculosis by the end of 2011.
The clinical management of drug-resistant TB cannot be addressed as an independent entity because it is closely dependent upon laboratory diagnosis, programmatic guidelines/interventions, and epidemiological setting. Within this broad scope, the present review depicts the global situation of MDR-TB, describes the problems associated with the clinical management of drug-resistant TB in resource constrained settings, and analyzes the availability of efficient, easy to implement, and affordable diagnostic tools and therapeutic approaches.
Global Distribution of High Burden Countries for MDR-TB
High burden countries for MDR-TB are defined as those with 4,000 or more incident MDR-TB cases per year, and/or at least 10% of MDR-TB among newly registered TB cases. The 27 countries with high MDR-TB burden account for 86% of all MDR-TB cases worldwide. Only 4 are found in Africa, despite the fact that this continent contributes to the TB pandemic with 9 of the 22 high TB burden countries. The other high burden countries for MDR-TB are located in Asia and the former Soviet Union. These countries likely had wider access than African countries in administering anti-TB drugs under poor-quality management, thus promoting the development of bacillary drug resistance. The widespread presence of M. tuberculosis strains of the Beijing genotype family in Eastern European and Asian countries seems to be another factor favoring the emergence of MDR-TB there. Reputedly, Beijing strains have selective advantages over other strains for disseminating in the community and developing drug resistance. 8
TB is unquestionably associated with poor resource settings. The World Bank ranks countries according to their annual gross national income per capita in low, lower-middle, upper-middle, and high income economies. 9 Understandably, most countries with high TB burden are in the low income group. This is not the case for high burden MDR-TB, for which 70% of the countries are classified as middle income economies, and there is even other which has reached the high-income economy group (Box 2). Only 7 countries with a high burden for MDR-TB are classified in the low income group, which is encouraging in regards to the financial costs of efforts needed to alleviate the global MDR-TB situation. Indeed, diagnosis and treatment of MDR-TB are much more expensive and require more infrastructure and higher qualified human resources than standard strategies for controlling TB in low-resource countries, which are mainly based on sputum microscopic examination and first-line drug regimens. The fact that most countries with high MDR-TB burden have better economies contributes, but is not sufficient, to alleviate the complex MDR-TB problem in large areas of the world. Along with economic constraints, there are technical, human resource, administrative, and sociocultural issues that hinder the implementation of sound strategies for controlling MDR-TB in middle income countries. In addition, these countries seldom qualify for significant financial support from international aid organizations. Even when they receive support to launch or reinforce a given management strategy, sustainability based on their own resources is often jeopardized by bureaucracy, political mismanagement, or other domestic constraints.
The 27 high burden MDR-TB countries classified according to their economies. 9
Bangladesh, DR Congo, Ethiopia, Kyrgyzstan, Myanmar, Nigeria, Tajikistan
Armenia, Georgia, India, Indonesia, Pakistan, Philippines, Republic of Moldova, Ukraine, Uzbekistan, Viet Nam
Azerbaijan, Belarus, Bulgaria, China, Kazakhstan, Latvia, Lithuania, Russian Federation, South Africa
Estonia
Treatment Regimens for Drug-Resistant TB
The current treatment of drug-resistant TB is based on either standardized regimens or individualized schemes designed according to results of drug susceptibility testing. Management options depend on financial resources as well as on strengths and weaknesses of the TB program in each setting. Limiting issues are largely related to health administration efficiency, human resource competence, laboratory infrastructure, equipment maintenance, and sustainability of supply importation, among others.
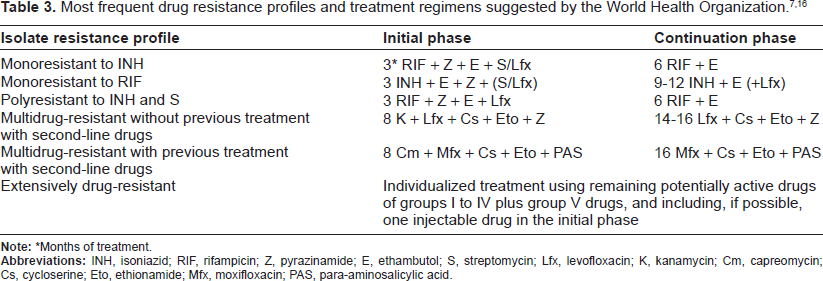
Pharmacological characteristics of first- and second-line drugs currently used for treating drug-resistant TB are shown in Tables 1 and 2. The most frequent drug resistance profiles and treatment regimens suggested by the WHO are summarized in Table 3.7,16 Mono-resistant and poly-resistant TB are, by definition, easier to manage than MDR-TB because at least one of two potent drugs, ie, INH or RIF, is still available for inclusion in the therapeutic scheme. MDR-TB cases with additional resistance to only one of the XDR-defining drugs (ie fluoroquinolones and injectable second-line drugs) show worse outcomes than other forms of MDR-TB; thus, these cases are regarded as pre-XDR-TB. 10 Understandably, XDR-TB is the most difficult form to treat because the most active groups of second-line anti-TB drugs are ineffective in these cases. The emergence of TB cases with resistance extended beyond the definition of XDR-TB has been recently documented and allegedly classified as a new form of drug-resistant TB. However, drug susceptibility testing for many second-line drugs is still difficult to standardize and there is not sufficient evidence relating in vitro resistance to such drugs with clinical outcome. For these reasons, WHO experts do not endorse the coining of terms such as “totally drug-resistant TB” to define those extremely severe cases of TB. 11
First-line drugs used in the treatment of drug-resistant TB.
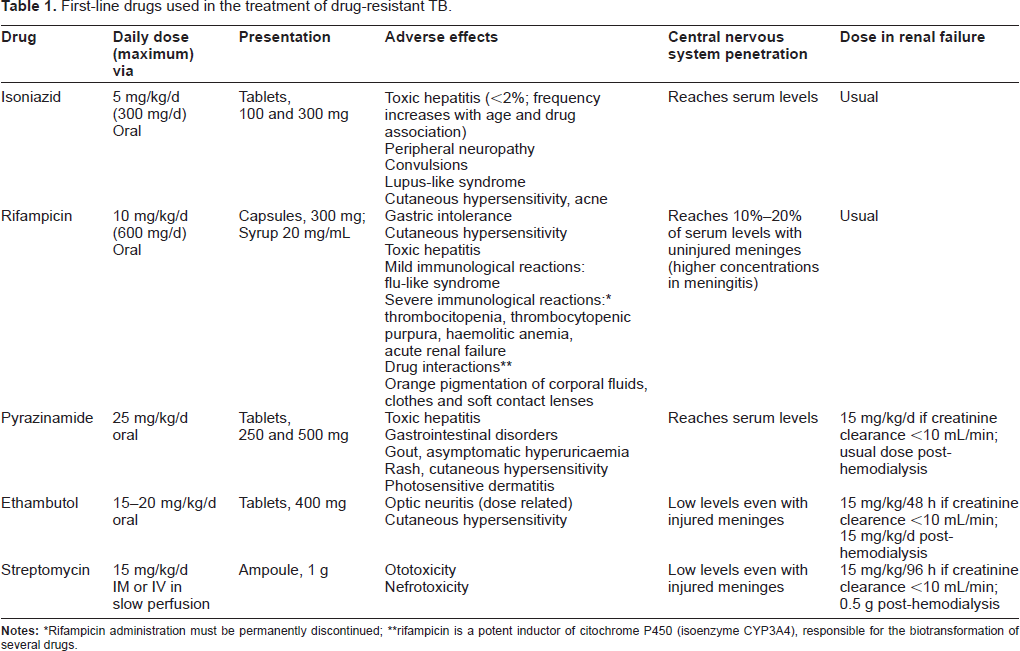
Rifampicin administration must be permanently discontinued;
rifampicin is a potent inductor of citochrome P450 (isoenzyme CYP3A4), responsible for the biotransformation of several drugs.
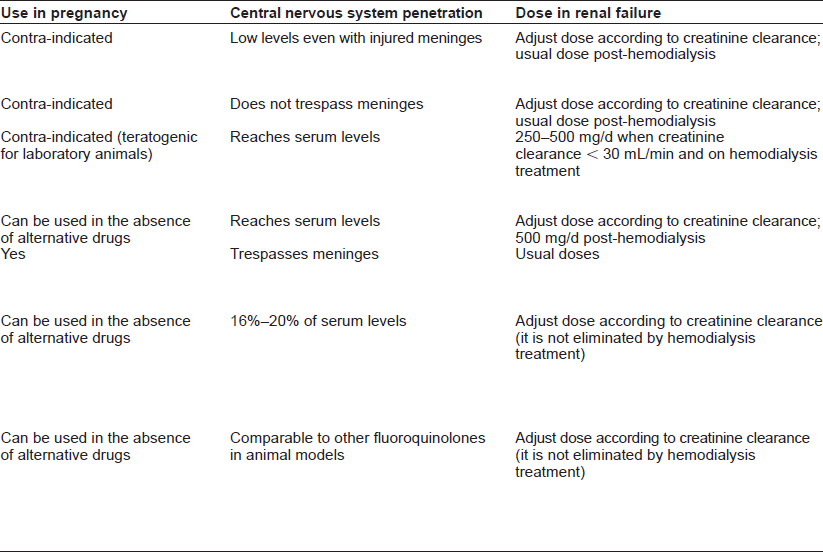
Second-line anti-TB drugs used in the treatment of drug-resistant TB.
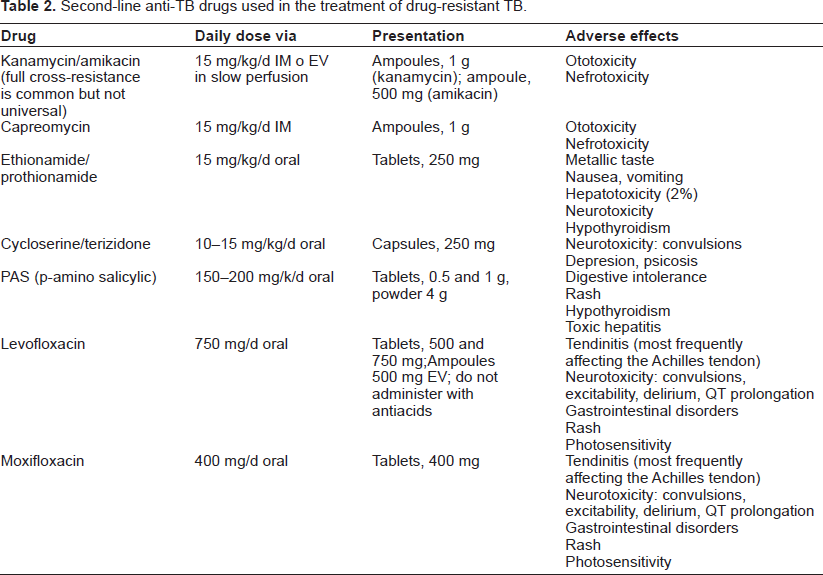
Months of treatment.
Treatment of mono- and poly-drug resistant TB
The most common forms of mono-resistant TB are INH and streptomycin resistance. The latter resistance reflects the widespread use of streptomycin in the past and does not represent a main threat to TB management since this drug is currently not included in standardized regimens. RIF mono-resistance is less frequent but much more dangerous because it is a strong predictor of MDR-TB and, even as monodrug-resistance, it predicts treatment failure. 12
In countries with limited resources, systematic drug susceptibility testing is not typically performed, drug resistance remains largely undetected, and cases of treatment failure and relapse are empirically treated. Hence, there is little evidence-based data regarding treatment outcomes of mono-drug resistant TB. An early review on clinical trials performed in Sub-Saharan and East Asian countries showed very low rates of treatment failure for INH-resistant TB when treated with 6-month regimens containing RIF, similar to the 2% failure observed under a highly proficient TB program in San Francisco, USA.13,14 In contrast, a recent meta-analysis found much higher failure rates for retreatment of INH-resistant TB (18%–44% in six cohort studies). 15
TB patients with previously undetected INH-resistance who undergo standard anti-TB treatment regimens are at risk of drug resistance amplification at the beginning of the second phase, which consists of INH and RIF only. If bacteriological conversion does not occur one month later, ie, by the fourth month after the onset of treatment, drug susceptibility testing is imperative. Drug regimens recommended by the WHO for INH-resistant TB last 9 months. They consist in an initial 3-month phase which includes RIF, pyrazinamide, and ethambutol, with/without streptomycin or a fluoroquinolone, followed by a 6-month continuation phase which typically includes RIF and ethambutol. 16 However, the level of evidence for any INH-resistant disease treatment is relatively weak and practices vary globally.
Standardized treatments for mono-RIF resistant TB extend longer, for 12–18 months, depending on the clinical presentation and the clinical/radiological/ bacteriological evolution. Close medical follow-up is mandatory to avoid drug resistance amplification. Drug schemes typically include a 3-month initiation phase with INH, ethambutol, pyrazinamide, one fluoroquinolone, and streptomycin. 16
Among poly-resistant TB, the most frequent combination is simultaneous resistance to INH plus streptomycin, which is managed using the same therapeutic schemes as used for INH-monoresistant TB. Other combinations are rare, can be detected only in settings where drug susceptibility testing is available, and no recommendation on standardized treatment based on evidence is available for these cases.
Treatment of MDR-TB
Several years ago, the WHO defined the five groups of anti-TB drugs potentially useful for MDR-TB. 16 This classification, which has been the basis for subsequent updated guidelines, is currently under revision.7,17 A slightly modified list is shown in Box 3.
Antituberculosis drugs with potential activity against MDR-TB.
The basis of current MDR-TB treatment consists of a combination of one injectable agent (kanamycin/ amikacin or capreomycin) and one fluoroquinolone (levofloxacin or moxifloxacin) associated with at least three potentially active drugs according to the patient's previous drug scheme and, if available, the results of drug susceptibility testing. A typical standardized regimen for MDR-TB consists of an 8-month initial phase of cycloserine, ethionamide, and pyrazinamide or PAS (in addition to a fluoroquinolone plus a second line injectable drug), and a continuation phase with oral agents for approximately 14–16 months (Box 4).
Standardized regimen for MDR-TB.
If the patient already received second-line drugs, there is an enhanced risk of amplifying the resistance to these drugs and eventually of generating XDR-TB. PAS should be used rather than pyrazinamide, and capreomycin instead of injectable aminoglycosides, until results of susceptibility tests to second-line drugs are available. There is little flexibility for personalized treatments beyond these schemes since they must be restricted within the frame of drug classification. Truly personalized treatments are those administered to patients with pre-XDR- and XDR-TB.5,16,18
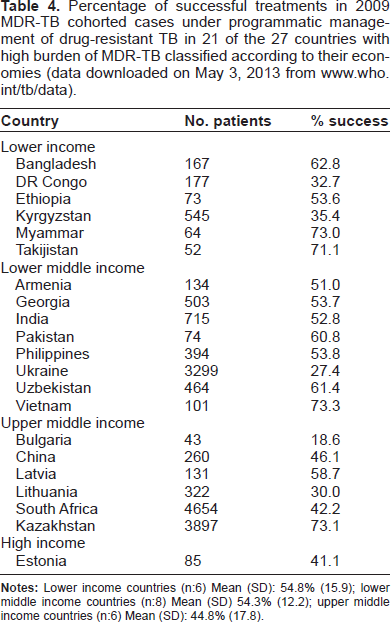
The prognosis of MDR-TB does not necessarily differ between high and low income countries when patient management is performed under strict programmatic conditions. 19 By 2011, approximately half of countries globally reported outcomes of at least one MDR-TB case under programmatic management of drug-resistant TB. The average success rate (cured patients plus finished treatment) according to the WHO oscillated between 48%–54%. 1 Specifically, 21 of the 27 countries with a high MDR-TB burden reported outcomes for 2009 cohorts. The proportion of successful treatments varied considerably among the 21 countries, independently of their income. When classified according to low, lower-middle, upper-middle, and high income economies, no significant differences were observed between categories regarding average success rates (Table 4).
Percentage of successful treatments in 2009 MDR-TB cohorted cases under programmatic management of drug-resistant TB in 21 of the 27 countries with high burden of MDR-TB classified according to their economies (data downloaded on May 3, 2013 from www.who.int/tb/data).
Treatment of XDR-TB
The treatment of XDR-TB depends on bacteriological results and the history of previous treatments for TB, which typically include second-line drugs. The results of susceptibility testing to second-line drugs are not as reliable as the results of susceptibility to RIF and INH. Although there are no standardized schemes, treatment generally includes an injectable drug (imipenem, meropenem-clavulanate), moxifloxacin (considered to be the most effective fluoroquinolone), linezolid, clofazimine, and the drugs in groups 1–4 considered as possibly still effective. Some new drugs are available for patients enrolled in compassionate treatment programs. 20 It should be stressed, however, that the use of these drugs is limited to a small number of patients who must be hospitalized under isolated conditions and under strict medical control. In any case, the prognosis of these severe forms of TB is somber and cure rates are below 50%.
The Bangladesh regimen
A alternative regimen for MDR-TB, which is cheaper and much shorter than current standard MDR-TB treatments, is currently being applied in Bangladesh. 21 Drugs used throughout the entire Bangladesh regimen include clofazimine, ethambutol, pyrazinamide, and high-dose gatifloxacin. Kanamycin, prothionamide, and high-dose isoniazid are used only during the intensive phase. This initial phase extends for at least 4 months or until sputum smear conversion. The continuation phase lasts only 5 months. The original study showed a cure rate over 80% in 206 patients treated with this regimen. To date, the scheme has been applied to more than 400 patients with follow-ups of 6–24 months after completion of therapy and 87% cure rates (Van Deun A, personal communication, February 2013). Overall drug-resistance rates in Bangladesh are low and patients previously treated with second-line drugs are excluded from this regimen. Thus, before a wide recommendation of this very convenient regimen is made, more evidence should be gathered, particularly from areas with higher background drug-resistance than Bangladesh.
A difficult issue: management of adverse drug reactions
Adverse drug reactions frequently occur in patients treated with second-line anti-TB drugs. The management of these situations requires expertise and availability of ancillary drugs. The problem became evident as a programmatic challenge as soon as the DOTS plus projects was launched. 22 In many developing countries, second-line drugs for treating drug-resistant TB are provided free of cost by the Public Health System, while ancillary drugs are not. Thus, adverse drug reactions result in a lack of adherence for patients who cannot afford expensive medicines such as corticosteroids. In addition, therapeutic drug monitoring, which plays an important role in the management of adverse drug reactions, is virtually unavailable in developing countries.
Treatment costs
According to a recent review, the main factors influencing treatment costs are the choice of second-line drugs included in the treatment regimen and the model of care chosen (hospitalization versus ambulatory care). The outpatient model of care is more cost-effective than the inpatient model. Again, it should be stressed that ambulatory treatment, a convenient choice for managing MDR-TB, is far from ideal for treating XDR-TB, where drug combinations must be meticulously handled and monitored to avoid further resistance amplification to the few drugs that remain potentially active in these cases. 23
Quality-assured medicines for treating drug-resistant TB are expensive. The cost of a 24-month drug regimen that includes capreomycin, moxifloxacin, cycloserine, ethionamide, and pyrazinamide ranges between 3,950 and 5,250 USD, depending on the manufacturer. According to WHO guidelines, the cost of the cheapest 24-month regimen, which includes kanamycin and levofloxacin, amounts to 2,268 USD.
Medicines with lower prices, but that are not quality-assured, are available on the market and have become a tempting option for low and medium income countries. Unfortunately, these less expensive medicines are often low-standard or even adulterated. This type of drug may not reach therapeutic levels, and in this way promote amplification of the resistance pattern of the patient's infecting strain. In fact, the widespread use of these drugs in low-resource settings is one of the factors putting the success of global efforts to control resistant TB at risk.24–26
Russia, India, China, and South Africa, four of the five newly developed BRICS economies, account for more than 60% of drug-resistant TB cases worldwide. Market expansion of TB medicines and the expected subsequent lowering of prices depend on the commitment of these countries to produce and/or acquire quality-assured drugs. In particular, China and India are important producers of second-line drugs, but only part of their production is quality-assured. These countries are making considerable efforts to fully adjust their pharmacological industries to the international quality standards according to the WHO. 27
Through the Global Drug Facility, the WHO mediates the acquisition of quality-assured second-line TB drugs using a pooled procurement mechanism to make lower prices available in the global market. Currently, many national TB control programs benefit, at least partially, from this international effort to facilitate access to quality-assured drugs. Several international donors, such as the Gates Foundation, UNITAIDS, and PEPFAR, play a crucial role as external sources of funding for countries with the lowest income economies. As described above, many countries with a high burden of MDR-TB have better economic profiles than countries with a high TB burden. Thus, most should be able to afford, at least partially, the purchase of quality-assured second-line TB drugs. 28
New anti-TB agents
The search for new anti-TB agents has been neglected for decades on the assumption that the disease was close to elimination. The emergence of MDR-TB in the 1990s and of XDR-TB in the 2000s fostered research on anti-TB drug development. New drugs, drug combinations, and re-purposed drugs potentially useful for treating MDR/XDR-TB have been recently proposed and are currently under evaluation.29,30 Some can be prescribed to a limited number of patients in resource-constrained settings within the frame of compassionate use programs supported by international aid organizations.
The discovery of ofloxacin inaugurated a new generation of anti-TB drugs. The use of this compound in patients with intractable TB was first described in 1985. 31 Ofloxacin belongs to a group of fluorated quinolones with strong anti-TB activity, which inhibit microbial DNA replication and transcription by interfering with DNA gyrase. Newer generation fluoroquinolones with demonstrably higher anti-TB activity, including levofloxacin and moxifloxacin, are already incorporated into standard regimens for drug-resistant TB.
Linezolid was approved in 2000 for human use as an antimicrobial agent and is especially active against Gram-positive bacteria. Like cycloserine, it belongs to the oxazolidinone group of compounds that act by inhibiting microbial protein synthesis. Linezolid has been successfully included in the therapeutic schemes of patients failing MDR-TB treatment. Two major disadvantages, including toxicity upon prolonged use and high cost, preclude its generalized prescription in resource-constrained settings, where it is mainly reserved for treatment of XDR-TB. 32 Allegedly, costs and toxicity can effectively be reduced by lowering doses to a quarter of the usual dose. 33 Additionally, an inexpensive generic version of the compound has been released in India with good therapeutic results. 34 Linezolid analogs with higher anti-TB activity and lacking adverse effects, such as PNU-100480 (sutezolid), are currently under evaluation in human volunteers.35–37
Clofazimine is an example of repositioned drug. 30 Described in 1957 as an anti-TB drug, this lipophilic riminophenazine was used with success in treating leprosy and included in standard regimens for this disease. The recent emergence of MDR/XDR-TB has renewed interest in its anti-TB activity, and the drug has been evaluated in therapeutic combinations for these forms of TB. Overall, variable success and no severe side effects were reported.38,39 Clofazimine has also been included in the successful Bangladesh scheme described above. 21
Other drugs repurposed for anti-TB treatment are the broad spectrum beta-lactam antibiotics. In particular, two carbapenems, imipenem, and meropenem, showed moderate efficacy in an experimental model of M. tuberculosis infection as well as in combination treatment of MDR- or XDR-TB.40–44
Nitroimidazopyrans are novel small molecules derived from metronidazole. They are active against TB by inhibiting the synthesis of mycolic acids. OPC-6783 (delamanid) and PA-824 are already in advanced clinical trials.45–47 Delamanid is expected to be approved by the US Food and Drug Administration. 28 Another new compound interfering with bacilli cell wall synthesis is SQ109. 48 Although this molecule is derived from ethambutol, it shows no cross resistance with it. Interestingly, synergy has been demonstrated between SQ109 and the linezolid analogue PNU-100480, which shows promise for the combined use of these novel drugs. 49 SQ109 is currently under evaluation in clinical trials. 50
The diarylquinoline R207910 was first described in 2005. It is derived from the structure of the anti-malarial quinolines but has specific anti-mycobacterial activity by inhibiting the proton pump of mycobacterial ATP synthase. 51 R207910 is also known as ™C207, the ‘J’ compound, and more recently, bedaquiline. At the end of 2012, it was licensed in the United States for use in MDR-TB with the warning of cardiac arrhythmias associated with a prolonged QT interval. It has a potent anti-TB activity but interferes with RIF; therefore, these drugs should not be combined for treating pansusceptible TB. 52 Regimens including bedaquiline showed higher efficacy but also higher toxicity than standard regimens for MDR-TB.53,54
One approach to anti-TB therapeutic development consists of using mouse models of infection to compare assorted combinations of new and old drugs, aimed at achieving an enhanced bactericidal activity and shortening treatment duration. 55 The most promising schemes are then applied in clinical trials as candidates for standardized drug-resistant TB regimens. 56 The synergy between the ethambutol-like SQ109 and the linezolid-derived PNU-100480 is a successful outcome of this approach. 49
The so-called early bactericidal activity is currently being assessed as a measure of the efficacy of new drugs, or drug combinations, when administered for a brief period to volunteer patients with pulmonary TB before starting conventional anti-TB treatment. It consists of comparing the decrease in counts of viable M. tuberculosis bacilli (expressed as colony-forming units) observed in sequential sputum specimens from patients with different experimental drug schemes. 57 In a paradigmatic study, the combination of pyrazinamide plus moxifloxacin plus PA824 achieved maximum early bactericidal activity. 55 Provided that results like this are further validated, they may approach the goal of a single standard regimen for treating pansusceptible TB as well as drug-resistant TB. This kind of regime would be the most useful in resource-constrained settings where drug susceptibility testing is not available. 55 The widespread emergence of drug resistance, however, is a predictable outcome of the standardized application of this type of scheme in the absence of proper laboratory monitoring.
Briefly, a wide spectrum of new and repurposed drugs has proven useful for treating drug-resistant TB in recent years. Much effort is still needed, particularly in the field of clinical research, to translate these promising achievements into effective patient cures and make them readily available in resource-constrained settings. Certain limitations still need to be addressed, especially those inherent to the TB drug market, that discourage pharmaceutical companies, including patent protection, unfavorable investment-return relation, and exiguous profit opportunity. 28
Role of the Laboratory in the Management of Drug-Resistant TB
The clinical management of drug-resistant TB primarily aimed at treating and curing individual patients, is closely dependent on programmatic interventions designed to control the disease in the community. Indeed, administration of effective treatment implies the fulfillment of several requisites, particularly laboratory support. The laboratory plays a key role not only in the detection of individual drug-resistant TB cases but also in the monitoring of treatment and in the surveillance of drug resistance levels in the community. Thus, for appropriate management of drug-resistant TB, both at the clinical and the programmatic level, there is an urgent need to strengthen laboratory capacity, proficiency, and safety in resource-constrained settings, and most importantly, to attain political will to ensure sustainability of these improvements. 7
In many low resource countries, current laboratory diagnosis of TB relies largely upon direct microscopic observation of stained sputum smear. Mycobacterial culture and drug susceptibility testing of the isolated M. tuberculosis bacilli, which are the basis of drug-resistant TB diagnosis and surveillance, require highly qualified human resources and biosafety level 3 laboratory facilities. Typically, in many low, and even in medium, resource countries, these conditions are fulfilled only in reference laboratories. 2
Phenotypic drug susceptibility testing
The proportion method for M. tuberculosis drug susceptibility testing allows the calculation of the proportion of resistant bacilli grown on solid medium in the presence of a drug at a given concentration. 58 As this 50-year-old test is accurate and relatively inexpensive compared with modern culture systems, it is still applied as the gold standard in many countries, particularly in those with medium and low income.
Drug susceptibility testing on solid medium is labor intensive, requires expertise, and takes 6–8 weeks to produce results. Semi-automated culture systems on liquid media were developed in the 1980s, which shortened turn-around-times to 2–3 weeks. Among these, the BACTEC TB-460 radiometric system proved to be highly reliable and for two decades was considered the gold standard for M. tuberculosis culture and drug susceptibility testing in high income countries.59,60
Due to radioactive waste contamination, BACTEC TB-460 was withdrawn from the market and a new generation of liquid culture systems based on fluorescent technology was developed, first in a manual version, the Mycobacterial Growth Indicator Tube (MGIT). 61 The BACTEC MGIT-960 system is based on the same technology but the tubes are incubated and automatically monitored every hour for fluorescent emission within an apparatus. Although other non-radiometric systems have been released, BACTEC MGIT-960 is the most commonly used worldwide for M. tuberculosis culture and drug resistance detection.62–64 Complementary to liquid culture systems are novel disposable lateral flow immunochromatographic devices for rapid (15 minutes) M. tuberculosis complex identification. 65 The use of liquid culture systems combined with rapid species identification has been recently endorsed by the WHO. 66
Automated liquid culture systems are still highly labor-intensive, expensive, and dependent upon highly sophisticated equipment. Simpler and cheaper in-house assays for rapid culture and drug susceptibility testing have been proposed for use in low resource settings. Two of these methods are based on the microscopic observation of early mycobacterial growth either in solid (thin layer agar method, TLA) or liquid enriched culture medium (microscopic observation broth drug susceptibility assay, MODS).67–69 Typical M. tuberculosis growth can be detected as early as 7–9 days post-inoculation using conventional light microscopy for TLA or an inverted microscope for MODS. This specific colony morphology also allows preliminary species identification. Both methods have comparable performances. 70 MODS has been recently endorsed by the WHO for use in patients at risk of drug resistance in resource-constrained settings. 71
Other non-commercial rapid culture approaches applied to drug susceptibility testing are based on colorimetric detection of bacterial metabolic activity using redox indicators. Tetrazolium salts and resazurin are most frequently applied in a microtiter plate format using enriched liquid medium. The Griess reagent is used in solid medium for revealing M. tuberculosis nitrate reductase activity. There is abundant literature on the adequate performance of these tests for rapidly detecting drug resistance.72–75 Colorimetric redox methods and the nitrate reduction assay have been endorsed by the WHO for drug resistance detection.76,77
The nitrate reduction assay is the most attractive non-commercial test for ready implementation in medium and low resource settings where conventional culture on solid medium is already being performed. It is inexpensive, requires minimal training, integrates easily into the laboratory workflow, does not introduce biohazards associated with handling of liquid culture, and does not require special equipment such as the inverted microscope used in MODS.
Genotypic drug resistance detection
Mycobacterium tuberculosis develops resistance to different drugs through spontaneous mutations in target genes. These chromosomal mutations occur at different rates for different drug targets and are selected under environmental pressure. Genotypic methods for detecting M. tuberculosis resistance are based on the identification of the gene mutations best known to confer drug resistance.78,79 For instance, most RIF-conferring mutations are concentrated in the core region of the rpoB gene of M. tuberculosis, making this small chromosomal segment an ideal target for genotypic detection of RIF-resistance. This is not the case for INH, where resistance is related to two (or more) genes and as many as one every four INH-resistant isolates may not carry any known associated mutation. High levels of isoniazid resistance are generally conferred by mutations in the katG gene, whereas low resistance levels are associated with mutations in the promoter region of the inhA gene. Fluoroquinolone resistance is strongly associated with mutations in a small segment of the gyrA gene, and thus this segment is a suitable target for genotypic detection of quinolone resistance. Similarly, amikacin- and capreomycin-resistant isolates generally carry mutations in the rrs gene. In general, frequencies of drug-associated mutations fluctuate between geographic regions.
A widely used solid phase format is the line probe assay or solid-phase hybridization assay. The method is based on PCR amplification of mycobacterial DNA from a sample or culture followed by reverse hybridization to specific probes previously immobilized on nitrocellulose or plastic strips. A color detection system allows visualization of the hybridized DNA as a band on the strip.
The INNO-LiPA Rif TB Assay (Innogenetics, Ghent, Belgium), the first commercial test of this kind, has been on the market for some time. It detects RIF-resistant M. tuberculosis either isolated in culture or directly from clinical samples and can deliver results within one working day.80,81 The strips contain ten oligonucleotide probes immobilized on its surface, of which one is specific for M. tuberculosis and the other nine represent either wild or mutated segments of the core rpoB region. The fact that RIF resistance is considered to be a reliable surrogate marker for MDR-TB in most regions of the world makes this test a valuable tool for rapidly identifying MDR-TB suspects. Evidence of its overall excellent performance is presented in a systematic review and meta-analysis. 82
A more recent option with a similar format and performance is the GenoType MTBDR (Hain Life-sciences, Nehren, Germany) series of assays for the rapid identification of M. tuberculosis and resistance to RIF and INH. Successive generations of the assay have been released to improve accuracy mainly by enhancing the spectrum of gene targets included as probes. Performance of the newer generation GenoType MTBDRplus for detecting RIF resistance is comparable to that of INNO-LiPA Rif TB.83,84 Results can be obtained in 1–2 days directly from smear positive sputum samples. Adequate performance for detection of INH resistance and screening of MDR-TB was documented when the test was evaluated in a high-volume public health laboratory. 85
The ultimate generation GenoType MTBDRsl (Hain Life Sciences), which is complementary of the previous test, has been designed to detect resistance to ethambutol and, most importantly, to XDR-TB defining second-line drugs. The assay includes probes that target the gyrA gene (for detection of fluoroquinolone resistance-associated mutations), the rrs gene (for detection of mutations associated with resistance to the injectable drugs capreomycin and amikacin), and the embB gene (for detection of mutations associated with ethambutol resistance).86,87 In a recent meta-analysis, this test showed adequate accuracy for detecting resistance to fluoroquinolones, amikacin, and capreomycin, but was insufficiently accurate for detecting resistance to kanamycin and ethambutol. Lack of data precluded evaluation of assay performance on clinical specimens. 88
Line probe assays for rapid screening of patients at risk of MDR-TB have been endorsed by the WHO. 89 For the Genotype MTBDRsl assay, however, WHO experts stated that the assay may be used as rule in testing for XDR-TB. However, they did not find it suitable to replace conventional phenotypic drug susceptibility testing, identify individual drugs as candidates for treatment, or defining XDR-TB cases for surveillance purposes. 90
The uneven performance of genotyping assays for detecting resistance to different drugs is not related to test format but to substantial gaps in scientific knowledge on mechanisms leading to the development of drug resistance. These gaps cannot be filled by using next-generation sequencing technologies, which are evolving quickly and show promise for rapid and affordable diagnostic solutions in clinical diagnosis. The issue will remain open, and genotypic detection assays will be imperfect until genetic mechanisms of drug resistance are more thoroughly understood.2,79
Commercial genotyping assays are very expensive and their use is out of reach for most low and medium income settings. Non-commercial methods have been proposed for detection of MDR-TB and show promising results, including line probe assays and those based on multiplex allele-specific PCR. These in-house methods are relatively simple to perform and affordable in medium-resource settings.91,92 However, some proficiency in molecular biology is required as well as separate room facilities for conducting the different steps of the PCR reaction. In particular, care should be taken to avoid amplicon contamination, especially when DNA is amplified directly from clinical specimens. As it occurs with any PCR-based detection test, the sensitivity is highly dependent upon the DNA extraction method chosen, the DNA content, and the presence of inhibitors in the sample.
Recently, real-time PCR technology was shown to have enormous potential for application in the field of clinical diagnosis. Among other assays based on this technology, an outstanding development was recently released: the Cepheid GeneXpert System (Sunnyvale, CA, USA), which aims to change the paradigms of TB care and particularly of drug-resistant TB care. 93 In its present format, the assay detects TB and RIF resistance. The principle consists of a hemi-nested real-time PCR which amplifies a M. tuberculosis-specific segment of the rpoB gene and molecular beacons which detect wild-type or mutated sequences. The entire assay is automatically performed inside a disposable cartridge and therefore does not require stringent biosafety precautions or skilled personnel. Decontamination and liquefaction of the clinical sample and its transference into the disposable cartridge are the only manual procedures. These steps take about 15 minutes and require only minimal training and similar precautions as those in vigor for the preparation of a sputum sample for direct smear examination. The overall time to results is 2 hours. As the entire amplification occurs inside a hermetically sealed cartridge, the risk of amplicon contamination is virtually nothing. The Xpert MTB/RIF may become a point-of-care tool for TB diagnosis in areas with high prevalence of drug resistance to first-line drugs. Optimal performance has been widely demonstrated in pulmonary, extrapulmonary, and pediatric TB.93–95 This procedure has been validated in low resource settings and endorsed by the WHO.96,97
However, if technologies such as the Xpert MTB/ RIF are to be widely implemented in low resource settings, safe and standardized MDR-TB regimes should be designed and monitored and administered only in areas where resistance to second-line drugs is low. Culture and phenotypic drug susceptibility testing would be still required for specimens yielding RIF-resistant results and for monitoring treatment. In fact, specific algorithms should be developed for application of this powerful tool in each particular setting, taking into account the predominant profiles of drug resistance to second-line drugs. Apparatus and cartridges are being distributed by international sponsors at subsidized prices in low resource countries. However, some issues should be carefully considered if the assay is to be widely applied in low resource settings. These issues include sustainable cartridge provision, apparatus annual calibration, reliable electric power supply and functioning room air conditioning, assuredly sustained availability of medicines (especially second line drugs), ready guidance by qualified medical personnel with expertise in managing drug-resistant TB, and quality-assured laboratory support for monitoring second line drug treatment, among others.
The availability of ready detection of drug-resistant TB where it is most needed is a huge step forward. However, the increasing numbers of available tests for detecting M. tuberculosis drug resistance to second-line drugs further complicates the management of drug-resistant TB cases. No international consensus has been reached on standardized susceptibility tests methods for second-line anti-TB drugs, even on issues such as critical concentrations and criteria for interpreting results. International experts are periodically updating recommendations, but have not yet identified a test fulfilling ideal requirements on accuracy, reproducibility, ease of use, affordability, and turnaround time. 77 To date, molecular drug resistance detection methods speed detection but do not replace phenotypic drug susceptibility testing. Both approaches are complementary and should be interpreted while taking into account a patient's medical history. 98
Role of Care Delivery and Medical Information Systems
Recently, Mauch et al 99 gathered evidence on TB care quality in countries from three continents, including the ‘inverse care law’. This law enounces that ‘the availability of good medical care tends to vary inversely with the need for the population served’. They concluded that diagnosis and treatment, even when provided for free, do not grant a cure to all patients. Elemental barriers remain in the most poverty-stricken patients within each country such as costs related transportation, accommodation, and nutrition. Common sense interventions, including close follow-up or support for transport and food, are highly effective. 100 Services should be decentralized and social security schemes should be made available to TB patients to amend long-dated social inequities related to TB care. 101 These simple measures will help to prevent treatment default, drug resistance amplification, further suffering, death, and disease transmission.
A role for community-based management of drug-resistant TB has been proposed in areas where increasing MDR-TB burden exceeds the capacity of specialized hospitals. 102 In terms of the need for care decentralization in certain settings, education on measures for community infection control must be provided, focusing on family protection (particularly to children and immunocompromised persons), ventilation, and use of separate rooms, among others.103,104 There are gaps between sound interventions recommended by the WHO and drug-resistant TB management in the real world; creative thinking is needed to fill these gaps. 105 The use of mobile phones for medication intake reminders and community-based networks/education, among others, are interesting initiatives in this sense.106–108
Electronic medical information systems are becoming increasingly accessible, even in remote rural areas of lower resource countries. Cell phone networks are increasingly supporting data services that allow internet access. These types of approaches would be most useful for: (i) tracking patients from diagnosis to therapy initiation, (ii) alerting patients who have been prescribed inadequate medicines, (iii) recalling patients who defaulted on treatment or were lost to follow-up, (iv) receiving laboratory results in real-time, (v) preventing duplicate records or misidentification by the use of unique patient identification numbers, and (vi) tracking drug adverse effects and advising distant health professionals on the management of drug-resistant TB. 109
Conclusions
The recent emergence of drug-resistant TB in large areas of the world has fostered the development of newer, more powerful tools for TB diagnosis and drug resistance detection. New devices close to point of care are generating a new demand for specific algorithms of integral TB care, which should be individually adapted to particular settings with particular facilities, capabilities, drawbacks, and drug resistance prevalence rates.
The clinical management of drug-resistant TB remains an unresolved issue. New drugs and ingenious new drug combinations are becoming increasingly available, which show great promise for the successful treatment of drug-resistant TB. These achievements, which are the outcome of intense, lengthy, and costly research efforts, can be swiftly spoiled by misuse of such medications. International organizations and national health systems should strengthen the control of interventions, with emphasis on monitoring the rational administration of new and old drugs to avoid misuse and early generation of drug resistance. 95
At the programmatic level, drug resistance surveillance should take advantage of new diagnostic tools to cover the substantial number of drug-resistant TB cases that are estimated to remain undetected globally “for whom diagnostics and drugs are not purchased, budgeted, manufactured, or even projected. These invisible patients will continue to transmit TB (and MDR-TB) to their families and communities until their disease resolves spontaneously or they die”. 110
Author Contributions
Conceived and designed the concept: DP, VR. Analyzed the data: DP, VR. Wrote the first draft of the manuscript: DP, VR. Contributed to the writing of the manuscript: DP, VR. Agree with manuscript results and conclusions: DP, VR. Jointly developed the structure and arguments for the paper: DP, VR. Made critical revisions and approved final version: DP, VR. All authors reviewed and approved of the final manuscript.
Funding
Author(s) disclose no funding sources.
Competing Interests
Author(s) disclose no potential conflicts of interest.
Disclosures and Ethics
As a requirement of publication the authors have provided signed confirmation of their compliance with ethical and legal obligations including but not limited to compliance with ICMJE authorship and competing interests guidelines, that the article is neither under consideration for publication nor published elsewhere, of their compliance with legal and ethical guidelines concerning human and animal research participants (if applicable), and that permission has been obtained for reproduction of any copyrighted material. This article was subject to blind, independent, expert peer review. The reviewers reported no competing interests. Provenance: the authors were invited to submit this paper.