Abstract
To assess some simple blood parameters at birth that can be used as a basis to suspect α-thalassemia minor (ATM), a prospective study involving 202 consecutive neonates with MCV of less than 95 fl or less were checked for Hb Barts by HPLC. The group was divided into two, one with an MCV of 90-95 (89 cases) and the other with an MCV below 90 (113 cases). For control, 104 consecutive neonates with an MCV ≥ 95 fl were similarly checked. It has been confirmed that an MCV that is below 90 fl, especially with and MCH of ≤30 pg is a strong indicator of the presence of ATM (109/113). On the other hand, MCV of 90 or more, especially with an MCH of 30 or more is a strong negative indicator for ATM (70/89). Firm diagnosis of ATM at birth can thus be secured in majority of neonates.
Introduction
ATM (α1 and α2) rarely gives appreciable drop in hemoglobin (Hb) or causes hemolysis.14,15 However, it usually gives microcytosis and erythrocytosis1,15 after the age of 6 months. To diagnose ATM, traditionally one of various techniques for Hb separation is used. Low Hb A2 is considered as a finding confirming the diagnosis in routine laboratories. 15 However, in our experience only a minority of ATM cases actually gives low Hb A2. The rest give normal Hb A2 level. Suspected cases can be checked by DNA studies, which are not widely available, and may also fail to find the abnormality due to the wide range of possible deletions/mutations involved.2,11
Finding Hb Barts at birth is a definitive proof of the presence of ATM or intermedia (that presents as Hb H disease later on).12,14 However, it is not practical to perform Hb electrophoresis (HBEL) for every neonate. Routine blood counts (CBC) are easy to do. Finding some parameters in CBC that are reproducible and specific for ATM would serve to reduces the HBEL tests to be done.
This study addressed the issue from this angle.
Patients and Methods
TEST GROUP: All neonates had CBC done in our Hospital. Of those having an MCV of 95 fl or less 202 consecutive cases, during the first 6 months of 2004, were prospectively taken for study as test population. Nothing was known about the parents of the babies from thalassemia point of view. There was no selection in the inclusion of cases in the study, except on MCV basis. This population was divided arbitrarily into two subpopulations, depending on their MCV. The first (TEST I) included those with an MCV below 90 fl. There were 113 such babies. We did not record the prematurity incidence in this group. The second (TEST II) included those with an MCV of 90-95 fl. There were 89 cases here. In these, 4 were born premature. This information was collected after the Hb separation results were available.
For control, 104 neonates with an MCV above 95 were taken, during the same period.
CBC's were performed using Coulter machine LH750. Since the policy in the Hospital was to perform CBC on cord bloods of neonates majority of specimens were of cord blood (97%). The rest were venous blood or heel prick specimens.
Hb separation was done by HPLC, using Biorad Variant v3.0 machine and β thalassemia short program. Band with retention time at 0.15-0.2 was considered as Hb Barts, as per manufacturer's information manual. Because in this program Hb Barts percentage is not measured we used manual calculation with ∓ 5% error.
Patients’ families were requested to bring back the babies 6 months after birth for follow up of their blood counts, as well as Hb separation.
Results
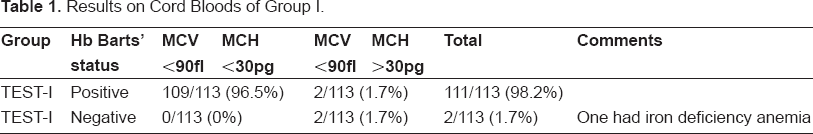
In patients of the first subgroup (113) with an MCV below 90 fl. 109 had Hb Barts (96.5%) if their MCH was also below 30 pg. Two additional patients had Hb Barts while their MCH was 30 or above. Total positive cases were 111 (98.2%). Only 2 patients had MCV ≤ 90 and MCH ≥ 30 were negative for Hb Barts. One of the two had iron deficiency anemia due to bleeding and his Hb was 12.1 g/dl at birth. See Table 1.
Results on Cord Bloods of Group I.
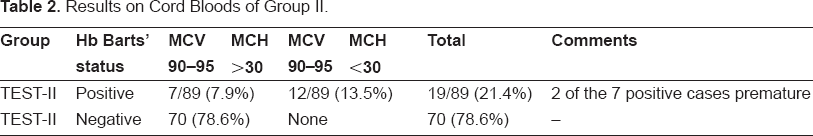
In the second subgroup, who had an MCV of 90-95 (89 patients) 70 were negative for Hb Barts (78.6%). 19 (21.4%) were positive. However, of these, 12 (13.9% of the group) had an MCH below 30. Seven (7.8%) of the 19 babies had an MCH ≥ 30 with the MCV of 90-95. Two of these were premature; hence their MCV was high. See Table 2.
Results on Cord Bloods of Group II.
Control group (104 babies). All had an MCV above 95 fl. In this group, only 3 cases showed Hb Barts. Two of them were premature. 101 cases were negative (97%, p ≤ 0.005).
Follow up results for test group was planned after they reached the age of 6 months. Only 71 (35.1%) showed up for the test. Of these, 48 were of subgroup I of the test population (42.5%), and 23 (25.8%) of subgroup II. Mean MCV for subgroup I was 60.4 fl, and for subgroup II 67.7 (p ≤ 0.05). Hb A2 levels in this second check ranged from 1.2 to 3.3% in the first group (mean 2.36%). Cases with sickle trait combined with α thalassemia trait were excluded from this range. In the second group mean HbA2 was 2.4% (p = 0.9). β thalassemia trait cases were not counted. Only 6 of the 48 cases (12.5%) with positive Hb Barts at birth had HbA2 level below the lower normal limit. However, red cell indices were suggestive of thalassemia in all. In group II, 3 cases were diagnosed as β thalassemia minor, because their Hb A2 was above 4% (mean 6.1%). See Table 3.
Results of follow-up at 6 months of age for TEST I & II subgroups.

In babies who had sickle trait as well.
Beta thalassemia and sickle cases excluded.
In group I there were 12 patients who also had Hb S at birth. In these cases mean HbS after the age of 6 months was 27.7%. In group II there were 5 patients with sickle trait and mean HbS level in them was 33.0% (p = 0.07). However, in all the 12 patients who had Hb Barts at birth Hb S was below 30% at six months.
Discussion
It is the experience of hematologists and hematopathologists in parts of the world which are endemic with α thalassemia, that routine Hb separation and HbA2 assay by column give the expected low levels in a minority of patients that otherwise have red cell indices suggestive of thalassemia trait.5,6,11 One has to rely on molecular genetic studies in these cases to confirm the suspected diagnosis. Not only such tests are not available everywhere as a routine, but also the known deletions and mutations are so numerous that it is difficult to obtain all primers needed to prove all cases.8,11
The basis for choosing the cut off MCV value of 90 fl is simply from authors’ experience in an area with high incidence of thalassemia.
People have tried predictive simple tests for diagnosis of ATM in order to overcome the difficulty of lack of low HbA2 level in the majority. One-tube osmotic fragilty was claimed to have high predictive value. 10 A group from the Central Middlesex Hospital in UK checked cord bloods, but aim was to check for haemoglobinopathies in general and they found cases with MCV ≤ 85 to have Hb Barts (9 out of 9), while there were 8 cases with Hb Barts out of 67 having an MCV between 85 and 92. 4 The issue was not taken any further and not brought in discussion.
It would be very useful and indeed convenient to restrict the highly suspicious cases at birth by certain simple parameters, so that one performs Hb separation techniques to look for Hb Barts, which is of prime importance in diagnosis of α-thalassemia minor at birth.7,9,16, Thus, diagnosis would be firmly established and molecular genetic studies, if available, can be performed at any time later to define the exact deletion or mutation. To our knowledge, there has not been a study which identifies α-thalassemia in patients who did not have Hb Barts at birth.
This study proved several points.
High validity of performing CBC on cord blood of all neonates in parts of the world where α-thalassemia is common.
High predictive value of having MCV ≤ 90 and MCH ≤ 30 at birth towards the presence of Hb Barts, indicating that such low red cell indices might be reliable predictors for diagnosis of α-thalassemia trait. If baby is immature by a couple of weeks then MCV up to 95 will be considered suspicious. For more premature babies (35 weeks or less) MCV up to 100 fl will be the cut-off. Such policy is now established in the center where the study was done, and other centers are adopting the policy as well.
There seems to be no probability of β-thalassemia trait causing those MCV and MCH levels.
There is a strong indication for performing Hb separation in cases with such MCV and MCH levels, to confirm presence of Hb Barts, and thus indicate the high probability of α-thalassemia trait diagnosis.
Very low probability of having low HbA2 level in proven α-thalassemia trait cases when checked after 6 months of age. Literature does not clearly state percentage of patients who give low HbA2.5,6
Consistently low HbS (usually less than 30%) in heterozygous sicklers who have α-thalassemia trait as well. This point confirms reports in the literature. 1
A smaller percentage of full term babies with MCV between 90 and 95 may have β-thalassemia trait (13%). These will obviously not be confirmed by neonatal Hb separation and have to wait till after the age of 6 months to be proven to have high HbA2.
These practical points are very useful in areas where thalassemia genes are common, like in the Arab Peninsula, 3 Middle East in general 7 and the Far east. 13 They will save time and obviate the need for more difficult and expensive tests in most cases. DNA and RNA testing may not be available in many parts anyway. World Health Organization can make use of this simple strategy for testing in these countries.
Disclosure
The authors report no conflicts of interest.
Footnotes
Acknowledgment
This work was reported in the XXXth Congress of the International Society of Haematology held in Istanbul, Turkey in October 2005.
