Abstract
An off-the-shelf Raman Spectrometer (RS) was used to noninvasively determine the presence of monosodium urate (MSU) crystals on the metatarsophalangeal joint (MTPJ) of a single gout sufferer. The spectrum sourced from the clinically diagnosed gout sufferer was compared to that sourced from an age-matched healthy subject scanned using the same protocol. Minimal signal processing was conducted on both spectra. Peaks characteristic of MSU crystals were evident on the spectrum sourced from the gout sufferer and not on the spectrum from the healthy control.
Introduction
Gout is the most common form of inflammatory arthritis, affecting around 3% of the population in both Europe and North America. 1 It is the result of hyperuricemia, which can cause deposition of monosodium urate (MSU) crystals in joints and other organs. When a critical level of crystal buildup is reached, the patient suffers acute arthritic attacks. Gout has related comorbidities of atherosclerosis, hypertension, obesity, and organ failure. 2 However, prognosis is excellent if diagnosed early and properly treated. 3
The gold standard diagnostic technique for gout is needle aspiration of the synovial fluid (SF) from the affected joint and identification of MSU crystals in the SF by compensated polarized light microscopy.4,5 This is an invasive, painful, and operator-dependent technique,6–9 explaining why it is only used in 10% of cases.
2
Physicians more often make a diagnosis by a combination of clinical appearance of the joint and blood uric acid levels.
10
X-ray analysis (XRA), dual-energy computed tomography (DECT), and high-resolution ultrasound (HRUS) have also been used for gout diagnosis, and magnetic resonance imaging (MRI) has been evaluated as a diagnostic for research purposes.11–21 Each of these techniques have their own inherent problems. XRA has poor prediction rates and is insensitive to early deposition.11,12 MRI is superior to XRA at detecting gout,13,14 but the appearance of gout on MRI is nonspecific
15
and contrast agents may be required.
13
Often DECT is unable to detect MSU in cartilage
16
and is less sensitive than aspiration.
17
In addition, DECT has significant cost implications, exposes the patient to radiation, and is available only to a few clinical units.
18
HRUS detects crystals
Raman Spectroscopy (RS) may offer a noninvasive alternative to these techniques as a point-of-care gout diagnostic. RS is a technique whereby incident light can be absorbed or scattered by a material when the energy of an incident photon excites a molecule in the material being irradiated. A small portion of the scattered light is shifted in energy with respect to the source beam. Plotting light scattered against frequency results in a Raman spectrum, effectively a “fingerprint” of the material's molecular structure. 22 RS has clinical applicability for diagnosing cancer, 23 diabetes,3,24 and Alzheimer's disease.4,25 It has previously been reported that RS can detect MSU crystals in aspirated SF 26 but this process requires needle aspiration and subsequent enzyme digestion and microfiltration rendering it impractical for clinical purposes as it is more time consuming and no less invasive than the gold standard.
In this paper, we detail how RS can identify MSU crystals, noninvasively, around the first metatarsophalangeal joint (MTPJ) of a clinically diagnosed gout sufferer.
Materials and Methods
Device
The RS device used was a Sierra (Snowy Range Instruments). The Sierra has a 785 nm wavelength laser with a maximum power of 100 mW. This results in high spectral resolution of 4 cm–1 and a spectral range of 200–2000 cm–1. The software used to interpret the Raman spectra was the inbuilt Snowy Range
Patients
Four clinically diagnosed gout sufferers were recruited through a trial conducted at St. Michael's Hospital (Toronto, Canada). All these patients were treated for gout, although only one patient was classed as having gout deposits. An age and gender matched healthy subject was selected and subjected to the same test protocol. The subject with gout is referred to as
Figure 1 shows how the Sierra was aligned to the first MTPJ of the subject.
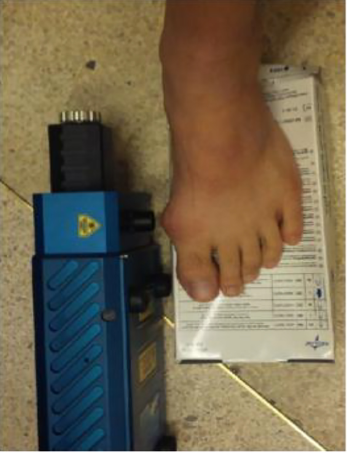
Snowy Range Sierra RS underside lens port aligned against the patient's MTP joint.
Laser Testing Protocol
The tests were conducted in a dark room to reduce interference from fluorescent lights. For both subjects, the RS was set to illuminate with an integration time of ten seconds, repeated automatically five times per selected point on the patients’ body. This collected five Raman traces, each with an exposure time of ten seconds, with the average of these five traces per irradiated spot being calculated and stored as the final Raman spectrum seen in Figure 2. The exposure time was segmented into these ten-second blocks giving the skin a rest time. This segmentation also allowed flexibility, by removing completely or averaging, if any patient movement occurred during the ten-second burst. A number of spots around the MTPJ were also examined with the same procedure to ensure the detection of MSU deposits. This method of breaking up the exposure time was utilized to increase the chances of detecting MSU while keeping the laser exposure to the skin to a minimum.

Trace from
Signal Analysis and Peak Identification
Subjects were scanned without the RS reference signal being removed in real-time, meaning that the Raman signal contains contributions from both the RS device itself and the subject in question. This was intentional and assured that any contribution to spectra from MSU peaks were not removed by signal processing. However, background fluorescence was removed using the built-in

A square over the peak indicates the presence of a peak on both the
A star indicates the presence of a peak on both the
An arrow indicates that there is no overlap between peaks of both spectra, ie, peaks present in the
Results
Figure 2 compares the Raman spectra of the
Initially, without comparing to the
Seven peaks (identified by the stars) have comparators at the same wave number in the
Discussion
These results indicate that MSU crystal deposits can be detected in clinically diagnosed gout sufferers by RS. Out of the 18 total MSU peaks identified by Kodati et al.
27
, 16 were present in the Raman spectrum of the clinically diagnosed gout patient. MSU peaks 386 and 1600 cm–1 were not present in either the
The majority of the other peaks that identify MSU (Fig. 3) is present in both the
Conclusion
The Sierra RS may have the ability to noninvasively identify MSU deposits at MTP joints. This preliminary study has shown that four Raman peaks (arrows) because of the MSU can be detected through the skin with no counterpart peaks associated with the
Experimental Concerns
The subjects were scanned without removing contributions from the RS background signal, ie, the portions of the spectrum that come from the internal optics of the RS. Incorporating an algorithm that can remove this needless contribution during real-time subject scanning should remove some of the noise from the spectra.
Ergonomics of the machine influence analysis. The Sierra does not have an adjustable focal point meaning that the subjects had to be physically manipulated until the laser shone directly onto the MTPJ. This could be addressed by the incorporation of a focus wheel on the device, which would enable the operator to refocus the apparatus until they were confident that they were hitting the MTPJ. Additionally, most MSU deposits collect on the top of the MTPJ, not the side. However, the Sierra weighs 9 kg and so placing this device on the top of the MTPJ was not possible.
Author Contributions
Conceived and designed the experiments: DC, MT. Analyzed the data: DC, MT. Wrote the first draft of the manuscript: DC. Contributed to the writing of the manuscript: DC, MT, LR. Agree with manuscript results and conclusions: DC, MT, LR. Jointly developed the structure and arguments for the paper: DC, MT. Made critical revisions and approved final version: DC, MT, LR. All authors reviewed and approved of the final manuscript.
