Abstract
Purpose
Improve risk management of patients undergoing investigations of the gastrointestinal (GI) tract, in regard to underlying diseases and choice of premedication. According to a nationwide survey in Japan, 74% of the deaths associated with premedication were patients aged 60 years or over.
Methods
Subjects were 418 patients undergoing investigations of the GI tract (367 endoscopy, 51 barium contrast radiography) between October 2001 and January 2004. Age distribution peaked in the 65-69 years group, and 40% of subjects were aged 65 years and over. Using a questionnaire, each subject was interviewed prior to the investigation to determine contraindications for anticholinergic agents or glucagon preparations. To confirm the risk associated with antispasmodic agents in elderly subjects, the group was subdivided into those aged under 65 years and those aged 65 and over, and compared.
Results
Anticholinergic agents were contraindicated in more than 50% of subjects aged 65 years and over, and glucagon was contraindicated in 11% of subjects aged 65 years and over. The proportion of elderly subjects in whom antispasmodic agents, including anticholinergics and glucagon, were contraindicated was significantly greater than for subjects aged under 65 years.
Conclusions
Using a written questionnaire at the time of obtaining informed consent facilitates the identification of underlying diseases and selection of appropriate premedication.
Keywords
Introduction
Generally, anticholinergic agents or glucagon preparations are administered prior to GI investigations in order to suppress peristalsis and secretions for easier observation of the target area. The parasympatholytic actions of anticholinergic agents contraindicate their use in patients with glaucoma, prostatic hypertrophy and cardiovascular conditions such as arrhythmia and heart disease. Glucagon, a peptide hormone secreted by the pancreas, is contraindicated in patients with phaeochromocytoma, although serious adverse reactions are considered uncommon, other than in patients with marked hyperglycemia.
The importance of clinical risk management (i.e. detecting and reducing the risk associated with medical procedures) has increased in current medical practice. In endoscopy in particular, recent advances and wider application have led to increased use in high-risk cases and according to a nationwide survey in Japan, 74% of deaths associated with endoscopic premedication were in patients aged 60 years or over. 1 We present the risk management initiatives we have introduced to overcome this problem.
We surveyed patients undergoing investigations of the gastrointestinal (GI) tract from the viewpoint of the influence of the underlying disease on selection of antispasmodic agent. We also investigated associations with age, in order to identify the high-risk group and assist in risk management. For the purpose of this study, elderly subjects were defined as those aged 65 years or over, as per the Japanese Welfare Law for the Elderly.
Methods
Patients
The subjects were 418 patients who attended the Second Department of Surgery of the Tokyo Women's Medical University School of Medicine for investigations of the GI tract (367 upper GI endoscopy, 51 barium contrast radiography) between October 2001 and January 2004. The peak of the subjects’ age distribution was 65-69 years, and 40% of subjects were aged 65 years and over (Fig. 1).
Distribution of the subjects’ ages.
Pre-investigation questionnaire
Using a pre-investigation questionnaire (Fig. 2), a nurse or doctor interviewed each subject prior to the investigation. Subjects for whom anticholinergic agents were contraindicated were defined in accordance with the ‘Guidelines for Endoscopy in Elderly Patients’ issued by the Japan Gastroenterological Endoscopy Society, namely, those with ‘hypertension, arrhythmia, ischaemic heart disease, glaucoma, or benign prostatic hypertrophy’, and glucagon preparations were contraindicated in subjects with ‘diabetes mellitus’.
Pre-investigation patient questionnaire.
Results
Numbers and proportions of the underlying diseases.

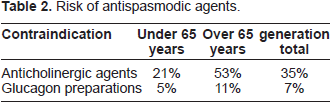
We also collated the proportion of subjects in whom antispasmodic agents (anticholinergic agents/ glucagon preparations) were contraindicated because of underlying diseases (Fig. 3). Of the younger subjects, aged less than 40 years of age, 10-20% has a risk associated with anticholinergic agents. The prevalence of risk-associated underlying diseases increased with age, with anticholinergic agents contraindicated in 53% of subjects aged 65 years and over. Glucagon preparations were contraindicated in 4-15% of subjects aged 40 years and over. To confirm the risk associated with antispasmodic agents in elderly subjects, we divided all patients into two group, aged under 65 years or 65 years and over, and compared the risk between groups (Table 2). Anticholinergic agents were contraindicated in 53% of subjects aged 65 years and over, significantly higher than the 21% of subjects aged under 65 years (χ
2
test, P = 0.0014). Glucagon was contraindicated in 11% of subjects aged 65 years and over, significantly higher than the 5% of subjects aged under 65 years (χ
2
test, P = 0.033).
Contraindication ratio of antispasmodic agents according to underlying disease. Risk of antispasmodic agents.
Discussion
The number of investigations of the GI tract performed in Japan has risen markedly in recent years, with expansion of the system of regular health checks and with increasing consumer demand for early detection and treatment. At the same time the ageing of Japanese society has increased the proportion of patients considered as high risk, in particular elderly patients with unrelated underlying diseases. The Accident Prevention Committee of the Japan Gastroenterological Endoscopy Society has conducted, and published in detail, nationwide surveys of investigation-related accidents at 5-yearly intervals since 1983.2–4 The third survey comprised 1,200,000 investigations, yielding 2600 accidents for an incidence of 0.22%. Patients aged 60 years or more accounted for 74% of deaths associated with premedication, and 82% of all investigation-related deaths, emphasising the need for risk management in elderly patients undergoing GI investigations.
Harada et al. examined the hemodynamic effects of anticholinergic agents and glucagon preparations administered as premedication for upper GI tract endoscopy, finding that the heart rate and pressure product rose significantly more with anticholinergic agents than with glucagon.5–16 In other words, the cardiac load is greater following the administration of anticholinergic agents than of glucagon.
The risk of hypoglycaemia should be worried also in non-diabetic patients following glucagon administration, in particular after 90-120 min, we give glucose tablets to the patients after endoscopy.
Collation of the present survey results revealed that anticholinergic agents were contraindicated in 35% of all subjects and that proportion rose with age. In particular, anticholinergic agents should be avoided in more than 50% of subjects aged 65 years and over. On the other hand, glucagon preparations were contraindicated in 7% of all subjects, and 11% of subjects aged 65 years and over, suggesting that, when choosing an antispasmodic agent for an elderly patient, from the viewpoint of preventing adverse events it is better to opt for glucagon rather than an anticholinergic agent.
In conjunction with the conducting of this study, we changed from our previous method of oral interview to using a patient questionnaire to assist with the choice of antispasmodic agent. As a result, in 2001 there was a change in the proportions of the different antispasmodic agents administered prior to endoscopy or barium contrast radiography of the GI tract, from 87% anticholinergics and 11% glucagon prior to introduction of the questionnaire to 79% and 21%, respectively, after its introduction. We considered the questionnaire useful in accurately identifying underlying diseases in the respondents, and assisting in the selection of the appropriate antispasmodic agent. In conducting this study, we were also reminded of the unavoidable fact that unpredictable adverse events will occur in a certain proportion of investigations, and that it is important from the risk management aspect to take a careful history and obtain informed consent in advance of the procedure.
Conclusions
The most prevalent underlying diseases requiring consideration in the selection of premedication for GI investigations are cardiovascular diseases, prostatic hypertrophy and diabetes mellitus. Anti-cholinergic agents were contraindicated in more than 50% of subjects aged 65 years and over, which was a significantly greater proportion than for subjects aged under 65 years. Using a written questionnaire facilitates the identification of underlying diseases and selection of the appropriate premedication. Overall, risk analysis has enabled better identification of factors that are useful in the fields of informed consent and risk management.
Key Points
The prevalence of risk-associated underlying diseases increased with age, with anticholinergic agents contraindicated in approximately 50% of subjects aged 65 years and over. Anticholinergic agents were contraindicated in 53% of subjects aged 65 years and over, significantly higher than the 21% of subjects aged under 65 years. Glucagon was contraindicated in 11% of subjects aged 65 years and over, significantly higher than the 5% of subjects aged under 65 years. We changed from our previous method of oral interview to using a patient questionnaire to assist with the choice of antispasmodic agent. We considered the questionnaire useful in accurately identifying underlying diseases in the respondents, and assisting in the selection of the appropriate antispasmodic agent.
