Abstract
Aims
To evaluate the safety, effectiveness, success rate and complications of needle knife precut papillotomy for inaccessible bile duct after failed pancreatic ducts access.
Methods
Selective common bile duct cannulation was required for 582 patients from November 2004 to May 2008. Precut sphincterotomy was performed in 28 patients (16 male, 12 female; mean age 71). When standard bile duct cannulation was unsuccessful after more than 20 minutes, the bile duct was considered inaccessible. Group A consisted of patients where pancreatic duct access was possible and transpancreatic papillary septotomy was performed (20 patients). If pancreatic duct cannulation also failed, needle knife precut method was performed and these patients belonged to group B (8 patients). The success and complication rates of the two groups were compared using the Chi-square test.
Results
The success rates were 85% and 87.5% respectively. Of the 28 patients in group A, 6 had mild to moderate pancreatitis and one patient had mild bleeding. The complication rates were 35% and 0% respectively and the differences were not significant.
Conclusion
Needle knife precut papillotomy is useful and acceptable in patients after failed pancreatic duct access.
Introduction
Endoscopic precut papillotomy is an established method for dealing with inaccessible bile duct. Several approaches have been reported, including the needle knife method,1–3 the Erlangen type papillotome method4,5 (including the short nose papillotome method), 6 and the transpancreatic papillary septotomy method using a standard papillotomy knife.7–9 The last technique has been reported to have a significantly higher rate of bile duct cannulation and a lower complication rate than the standard needle knife sphincterotomy. 8 If it is possible to access the pancreatic duct, the transpancreatic papillary septotomy method using a standard papillotomy knife may be considered to be the first choice for dealing with an inaccessible bile duct. If pancreatic duct is inaccessible, the needle knife method or the transhepatic approach is required. A needle knife papillotomy should be possible for patients in whom both, the pancreatic duct and the transhepatic route are inaccessible. However, no published reports have evaluated the results of precut papillotomy in patients in whom both, the bile duct and the pancreatic duct were inaccessible and in those, in whom the pancreatic duct was accessible. It is not known if there is a low success rate as well as a high risk of post-ERCP pancreatitis and perforation associated with endoscopic precut papillotomy, in the instance of failed pancreatic duct cannulation to perform transpancreatic papillary septotomy. Therefore, the results of patients in whom both ducts were inaccessible and were treated with needle knife precut papillotomy were evaluated in order to confirm the safety and effectiveness of this approach.
Patients and Methods
From November 2004 to May 2008, 1030 endoscopic retrograde pancreatocholangiography (ERCP) examinations were performed. A total of 582 patients had a native papilla (no previous endoscopic sphincterotomy, balloon dilatation and stenting) and required selective common bile duct cannulation; of the 582 patients, 28 (16 male, 12 female; mean age 71 years, range 13 years) had one of two types (transpancreatic papillary septotomy or needle knife precut papillotomy) of precut sphincterotomy.
The indications for precut sphincterotomy were: choledocholithiasis in 12 patients (42.8%); suspected cholangiocarcinoma in 7 patients (25.0%); pancreatic carcinoma with obstructive jaundice in 4 patients (14.3%); sphincter of Oddi dysfunction (SOD) in 3 patients (10.7%); and miscellaneous indications in 2 patients (postoperative bile leakage and choledochocele). The diagnostic criteria for SOD were based on clinical findings (recurrent biliary type abdominal pain) and increased serum liver enzymes without biliary stone and other biliary diseases.
Demographic data and indications for precut papillotomy.

Transpancreatic papillary septotomy was performed by using the standard sphincterotome which was guided over the guidewire inserted into the main pancreatic duct. Needle knife precut papillotomy was performed by placing the needle at the papillary orifice and cutting toward 11 o'clock.
Complications were defined according to the criteria of Cotton et al. 10
The success and complication rates were compared between the two groups using the chi-square test. P < 0.05 was considered statistically significant.
Results
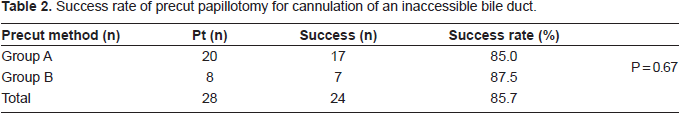
Success rate of precut papillotomy for cannulation of an inaccessible bile duct.
Complications of precut papillotomy for cannulation of an inaccessible bile duct.

Discussion
Endoscopic precut papillotomy is useful in patients with an inaccessible bile duct. If the transpapillary approach fails in patients in whom the bile duct is inaccessible endoscopically, it takes more time and resources to approach the duct using other methods (transhepatic or operative). In patients with ascites or an undilated hepatic duct, the transhepatic approach should be avoided. Although the precut method is infrequently required, it is an important technique for the treatment of biliary disease.
Recently, the precut method has been regarded as the standard method; it has a high success rate when done by expert endoscopists.11,12 However, the needle knife precut technique is by no means easy and safe, as there is a risk of pancreatitis and perforation.2,11 Thus, only expert pancreaticobiliary endoscopists should use this method. 13 Later, a precut sphincterotomy through the septum after selective cannulation of the pancreatic duct has been reported to be safe and effective. 8 The merit of this method is that the standard pull-type papillotomy knife can be used safely like the usual procedure of sphincterotomy. Therefore, this method is considered easier than the standard needle knife method and can be done by nonexpert pancreaticobiliary endoscopists as well. We adopted transpancreatic septotomy in the first place because of procedural ease and simplicity when the standard bile duct cannulation failed. The disadvantage of this method lies in the difficulty in cutting the suprapapillary region of the papilla. Therefore, duodenal papilla with a long oral protrusion is not suitable for this method, since sufficient separation of the pancreatobiliary orifice cannot be obtained.
Needle knife precut methods using a pancreatic stent have been reported to decrease the incidence of post-ERCP pancreatitis and to be safe because of the presence of pancreatic drainage and the ability to guide the cutting direction.8,14,15 However, this method requires selective pancreatic cannulation before the precut is done, and it is more complicated than pancreatic septotomy. A previously inserted pancreatic stent may interrupt the treatment procedure for the bile duct lesion, for example, stone removal. A pancreatic stent is not always necessary in all precut cases. Moreover this method is more expensive than other precut methods because of the cost of pancreatic stent.
A needle knife precut papillotomy at the suprapapillary region has been reported as a novel method with a high success rate of bile duct cannulation and a low incidence of post-ERCP pancreatitis.15,16 In this method, the cutting starts from the suprapapillary lesion (papillary roof) to avoid the orifice, whereas the standard needle knife method cuts the suprapapillary lesion, including the orifice. Post-ERCP pancreatitis may be prevented by avoiding papillary edema. However, it is questionable whether patients with a small papilla that has a small roof can be effectively cut while avoiding the orifice without developing complications. 17 It may be that only certain expert endoscopists can perform this procedure for any type of papilla.
If selective pancreatic duct cannulation is achieved, any type of precut method can be used. However, if selective cannulation of the pancreatic duct is impossible, the needle knife precut papillotomy is the only method that can be used. There have been no reports of patients with an inaccessible bile duct in whom pancreatic cannulation could not be done and a needle knife precut was done. Such patients are rare. In fact, only 8 cases have been treated this way in 3.5 years.
Although the success rates of needle knife method was similar to that of transpancreatic papillary septotomy, complication rate of needle knife method was lower than transpancreatic papillary septotomy with no significant difference. In transpancreatic papillary septotomy, post-ERCP pancreatitis may be caused by contrast injection and guidewire insertion into the pancreatic duct and electrocautery injury of the pancreatic duct orifice. Previous prospective study showed the effectiveness of pancreatic stenting on post-ERCP pancreatitis in high-risk patients undergoing standard biliary sphincterotomy. 18 There are several reports from various studies on risk factors for post-ERCP pancreatitis.19,20 SOD and precut papillotomy were regarded as high risk factors for post-ERCP pancreatitis. Pancreatic stenting may prevent pancreatitis for endoscopic pancreaticobiliary intervention in these high risk patients.21,22 However, in this study, 2 of the 3 SOD patients in group A developed post-ERCP pancreatitis despite pancreatic stenting. Pancreatic stenting for SOD patients may have prevented severe and fatal pancreatitis. Whenever possible pancreatic stenting should be performed for transpancreatic papillary septotomy, since there is no evidence currently that pancreatic stenting aggravates pancreatitis.
The time limits allowed for standard cannulation range from 10-30 minutes.8,17,23 Injury of the papilla may be more severe in patients in whom a long duration for cannulation is allowed before the precut papillotomy. Biliary cannulation was successfully performed in 95% of native papilla cases, although a long time period was allowed for standard cannulation before the precut papillotomy. However, precut papillotomy should be performed quickly in patients who require a papillotomy for choledocholithiasis and drainage for obstructive jaundice, 5 particularly in patients who have already had pancreatic cannulation.
This report is a single center study with relatively small number of cases. More data on the needle knife precut papillotomy after failed pancreatic duct access are required to confirm the safety and certainty. We should validate the evidence by more studies done in different centers.
Cases of inaccessible pancreatic duct at ERCP are rare. In many cases, selective biliary cannulation can be easily performed by transpancreatic papillary septotomy. However, in a few cases, both ducts are inaccessible. Needle knife precut papillotomy in patients with an inaccessible bile duct is a useful and acceptable method even when pancreatic duct cannulation fails.
Footnotes
The authors report no conflicts of interest.
