Abstract
Fanconi anemia is an extremely rare genetic disease characterized by chromosomal instability that induces congenital alterations in individuals. It causes defective hemopoiesis ultimately leading to bone marrow failure. Patients are susceptible to recurrent infections and increased risk of hemorrhage, as well as delayed and poor wound healing. Herein, we report a case of Fanconi anemia in which various classical signs of the disease were present. The patient has been on regular follow-up since three and a half years for management of dental problems. The different aspects of this rare disorder are discussed with emphasis on oral manifestations and their influence on the general health of affected patients. Due to an increased susceptibility to developing cancers in this specific population, it is imperative for pediatric dentists to know about the common oral manifestations and potentially cancerous lesions, in order to make an early diagnosis and provide comprehensive care and maintenance of oral health in affected individuals.
Keywords
Introduction
Blood disorders include a spectrum of diseases such as anemias, hemophilias, cancers, and immunodeficiencies. The common inherited anemias include sickle cell anemia, thalassemias, Diamond–Blackfan anemia, and Fanconi anemia (FA). Sickle cell anemia and thalassemia can arise from mutations in genes that are important for the structure of one of the two globin chains of adult hemoglobin (alpha and beta globins) and for its production in sufficient amount. FA results from a mutation in one of the 15 genes involved in the DNA repair pathway that is essential for the proper development of white blood cells, red blood cells, and platelets. FA is a genetically determined, DNA instability disease characterized by progressive bone marrow failure, multiple congenital abnormalities, and predisposition to cancer. It is named after the Swiss pediatrician, Guido Fanconi, who first described this disorder in 1927. 1 It is an extremely rare disease with a prevalence of 1:350,000 births. The mean age for diagnosis is 7 years, and the life expectancy is 25 years, and may attain between 30 and 40 years of age. 2 Majority of the patients develop cancer, usually acute myelogenous leukemia, and 90% of patients develop bone marrow failure by the age of 40 years. As many as 60%–75% of patients have congenital defects such as (1) short stature; (2) microcephaly; (3) endocrine problems; (4) skin pigmentation in the form of café au lait spots; (5) petechiae and bruises; (6) infections; (7) developmental disabilities; and (8) abnormalities of the skin, arms, head, eyes, kidneys, and ears. The hematological complications include progressively higher pancytopenia, anemia, thrombocytopenia, leukopenia, macrocytosis, and fetal-like erythropoiesis (D'Andrea 1997). The oral manifestations may be the presence of missing teeth, supernumerary teeth, small teeth, abnormal root shapes, malpositioned teeth, dental caries, gingivitis/periodontal disease, oral mucosallesions, salivary gland dysfunction, and propensity to develop oral cancers such as squamous cell carcinoma (SCC). Despite a multitude of problems, oral and dental findings of FA have rarely been reported in literature. 3 5 In this article, we report a case of FA along with a discussion on the main oral manifestations and their involvement in the health of patients with FA. The importance of providing multidisciplinary care and prevention of oral alterations in affected patients have further been highlighted. The patient's mother has given written consent for publication of this case report.
Case Report
A five-year-old male patient was brought by his parents to the Department of Pedodontics and Preventive Dentistry, Maulana Azad Institute of Dental Sciences, for routine dental examination. The child had been diagnosed with FA. The diagnosis of FA was made by a cytogenetic test, which revealed chromosomal breakage upon administering mitomycin C. The family history was significant as the patient's parents had a consanguineous marriage and were carriers for FA.
The patient was the only child of his parents and had no siblings. The parents’ dental condition was normal. The prenatal, natal, and past medical histories were significant. The patient's mother was given amnioinfusion in her seventh month of pregnancy, and the child was born through a cesarean operation after 36 weeks of pregnancy. The patient was small for the gestational age (1600 g body weight at birth) and was operated for patent ductus arteriosus within 20 days of birth. The patient had recurrent episodes of severe pneumonia after birth. There was a ventricular septal defect, which closed naturally, and the patient was operated for hernia at two years of age. The bone marrow of the patient was not working properly, and he was found to be thrombocytopenic with low hemoglobin (6 g%).
The patient was conscious and fully cooperative with well-developed cognition during general physical examination. The patient's height and weight were less than normal for his chronological age. The patient's left hand's thumb had been removed surgically since it was bifid and causing problems in routine life. The skin was pigmented on the palmar surface of his hands (Fig. 1).

Absence of left hand's thumb.
On intraoral examination, multiple carious lesions were seen. There was mesiodens present between the mandibular central incisors, which is an extremely rare occurrence (Fig. 2). There were retained deciduous mandibular incisors and delayed eruption of permanent mandibular incisors. White patches were also seen on the dorsal surface of the tongue (Fig. 3). The patient repeatedly used to develop cheek and tongue bite lesions with delayed healing (Fig. 3). When the patient turned eight and a half years old, he presented with sudden onset of painful bluish fluid-filled intraoral swelling in left maxillary first primary molar 64, which on diagnosis was found to be an eruption cyst (Fig. 4). The cyst later underwent remission and had uncomplicated healing. There were multiple restorations done for the patient symptomatically throughout his course of dental visits. Radiographs were required but could not be taken as radiation exposure increases the risk of tumor production in FA patients. The patient was behaviorally hyperactive and was not stable on a dental chair. Oral hygiene maintenance was poor, leading to recurrent lesions and infections in the oral cavity. Due to these reasons, rendering dental treatment was extremely challenging. The patient has been kept on regular six-monthly follow-up visits since five years of age until today, when he is eight and a half years old.

Presence of multiple carious lesions and mesiodens in relation to mandibular central incisors.

Cheek and tongue bite lesions along with white patches on tongue.
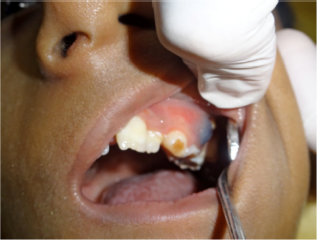
Eruption cyst in relation to left maxillary deciduous first molar.
Discussion
FA is a rare hereditary disorder characterized by congenital malformations, cellular hypersensitivity to DNA cross-linking agents, predisposition to acute myelogenous leukemia, and other malignancies. 6 FA shows genetic heterogeneity, although the proteins encoded by FA-related genes are considered to work together in a common pathway that regulates cellular resistance to DNA cross-linking agents. 7 At least 15 genes have been identified that are responsible for FA complementation groups, as follows: FANCA, FANCB, FANCC, BRCA2 (FANCD1), FANCD2, FANCE, FANCF, FANCG (XRCC9), FANCI, BRIP1 (FANCJ or BACH1), FANCL, FANCM, PALB2 (FANCN), RAD51C (FANCO), and SLX4 (FANCP). 8 Abnormalities of FA genes are inherited in an autosomal recessive manner, except for FANCB mutations, which are inherited in an X-linked recessive manner, seen in only 2% of cases. Mutation in the Fanconi pathway genes results in failure to produce blood cells and bone marrow failure over time and also predisposes individuals to development of various cancers.
Clinically, patients can have a wide array of abnormalities such as bifid thumbs, malformations of hands and arms, pigmented skin, gastrointestinal disorders, and genital anomalies. These were seen in the present case also, as there was a bifid left thumb that had been surgically removed and the presence of palmar pigmentation. The patient had also been operated for inguinal hernia. Developmental disorders such as microcephaly and growth deficiency may also occur. Short stature and growth hormone deficiency were also present in the case being reported. The skeletal age was found to be less than the chronological age. The short stature of these patients is related to deficiency of growth hormone, which affects ∼81% of FA individuals, including the one in the present case. 9 Low birth weight is common and was also seen in the present case. Less common abnormalities in FA include gastrointestinal defects such as esophageal atresia, imperforate anus, and tracheoesophageal fistula; cardiac defects such as patent ductus arteriosus, ventricular septal defect, pulmonary stenosis, and aortic stenosis; and central nervous system defects. Patent ductus arteriosus and ventricular septal defect were present in the patient being reported. Hematological abnormalities due to depressed bone marrow activity are the most serious clinical presentation. Because of the failure of hematologic components to develop white blood cells, red blood cells, and platelets, resistance against infection, oxygen-carrying capacity of cells, and hemostasis are all diminished. In the present case, white blood cell count was normal, but platelets and red blood cells were markedly diminished. Consequently, the affected FA patient may present with bleeding, pallor, and/or recurring infections. The present case had a history of repeated pneumonia, indicating a recurring infection tendency. Besides these, patients suffer from diminished appetite, nausea, abdominal pain, and vomiting. These problems can interfere with everyday life and create hurdles to normal growth and development.
In affected patients who survive into early adulthood, there is a greatly increased risk of solid tumors, such as hepatic tumors, which may be related to androgen use, and SCCs of the esophagus, oropharynx, and vulva. 10 Kaplan et al suggested that there are two defects determining the development of cancer in FA patients: defective chromosomal stability and immunodeficiency. 11 Patients who have undergone bone marrow transplantation (BMT) have a greater incidence of development of malignancies. In these patients, there are four additional factors, including pretransplant total body irradiation, cyclophosphamide treatment, chronic graft-versus-host disease (GVHD), and prolonged immunosuppressive treatment after transplantation.4,12,13
Oral manifestations
There are various oral manifestations seen in affected patients, which are described as follows.
Gingivitis and periodontitis
These are the most cited oral manifestations in individuals with FA. 14 Severe gingivitis was present in the case reported here. This is due to poor oral hygiene and thrombocytopenia, which exacerbates gingival bleeding. Aggressive periodontitis is seen with accentuated horizontal loss of alveolar bone. This is associated with deficiency of leukocytes and presence of pathogenic microorganisms such as Aggregatibacter actinomycetemcomitans. FA patients receiving BMT are given immunosuppressant agents, such as corticosteroids, which may further reduce the immunological defense leading to higher risk for periodontal disease. 15
Dental caries
Few studies have cited the prevalence of dental caries in this population. Tekcicek et al and Acikgoz et al reported that 35%–66% of FA patients develop dental caries and gingival problems.16,17 Caries is associated with poor oral hygiene and accumulation of plaque. This may be explained by the attention being focused on systemic alterations and not on the oral condition, such as maintaining optimum oral hygiene. Hyposalivation is frequently seen in FA patients due to endocrine alterations, which greatly predisposes them to dental caries. Dental caries involving multiple teeth along with xerostomia was seen in the present case, requiring frequent dental intervention.
Dental anomalies
Dental anomalies such as microdontia, supernumerary teeth, tooth agenesis, discolored teeth, abnormal tooth shape, rotation, transposition, delayed eruption and shedding of teeth, and micrognathia have been observed. The tooth with the highest prevalence of agenesis is the maxillary central incisor. The permanent canine is the tooth with the highest prevalence of transposition. Alterations in calcium metabolism during odontogenesis related to vitamin D-resistant rickets explain some of the dental alterations in individuals with FA, such as agenesia and presence of supernumerary teeth. 18 The other alterations may be justified by craniofacial anomalies such as microcephaly and micrognathia. 19 In the present case, mandibular mesiodens was seen, which is an extremely rare occurrence with an incidence of 0.01%. 20 Delayed eruption and shedding of teeth were also present.
Soft tissue lesions
Recurrent aphthous ulcers and eruption cysts are extremely common lesions in oral soft tissues in individuals with FA. This was one of the main reasons of frequent dental visits of the patient being reported. Otan et al associated recurrent aphthous ulcers with the hematological condition, particularly neutropenia and anemia, because there is an improvement in the condition of recurrent ulcers in the weeks after blood transfusions. 5 Another reason is that leukocyte deficiency, reducing the immunity of these individuals, leads to the development of ulcerated lesions. 21 Traumatic nonulcerated lesions and petechiae are common in these individuals and are normally related to low platelet counts.
Oral cancer and tongue lesions
In patients with FA, there is a high risk for development of head and neck squamous cell carcinoma. Immunosuppressive drugs administered for prophylaxis or treatment of GVHD are also associated with an increased risk of malignancies. Two-thirds of the head and neck squamous cell carcinoma in FA patients are located within the oral cavity, most frequently at the tongue margins and gingival areas. 22 Jansisyanont et al reported that the most common localizations of SCC in FA patients in descending order are the tongue, anogenital region, pharynx, larynx, oral mucosa, mandible, and skin. 4 OksÜzoğlu and YalÇın found that 14 of 40 FA cases with SCC had lesions on the tongue. 23 There are many alterations in the tongue of individuals with FA. The most frequently described are papillary atrophy, saburral tongue, macroglossia, and melanic pigmentation. Melanic pigmentation may extend up to the floor of the mouth and gingiva. A recent study found Mycoplasma salivarium to be a dominant microorganism in the oral cavity tumor sites of FA patients. 24 Genetic alterations in FA patients have been cited as one of the etiological factors of SCC of the tongue. When a BMT is performed, chromosomal instability is increased due to ionizing radiations, GVHD, immunosuppressant treatment, and post-BMT control therapy. All these factors together elevate the risk for the development of SCC by 4.4 times in individuals with FA.25,26 External factors such as solar irradiation, smoking, alcoholism, and human papillomavirus (HPV) confer an even greater risk for the development of malignant neoplasias.27,28 Kutler et al suggested that carcinogenesis induced by HPV in individuals with FA is associated with the inactivation of p53 by HPV, and not by direct mutagenesis. 29 In the case reported here, there were whitish patches on the dorsum of the tongue, which may be due to early dysplastic changes.
The treatment for SCC of the tongue is radical surgical removal of the tumor, associated with either radiotherapy or chemotherapy. The main preoperative problem in FA patients is the associated bone marrow failure, requiring hematologic consultations. The possibility of blood and platelet transfusions before surgery must be considered. A further concern for the surgeon is the development of postoperative complications, including wound infections and hematoma. Because SCC in FA patients is difficult to treat once advanced, it is necessary to diagnose malignancies at an early stage. Kutler et al suggested a biannual screening of the oral cavity and oropharynx that should start between the age of 15 and 20 years. 30 However, in patients with FA with a history of leukoplakia or recurrent oral lesions, head and neck examinations are recommended every six or eight weeks. 31 Efforts should be made to ensure optimum oral hygiene since poor oral hygiene has been linked to an increased risk of esophageal carcinoma. 32
Dental treatment should be specific and limited to infection control. Delivering oral health care is challenging for multiple reasons. Radiographs are not advisable in FA patients due to induction of tumors, making proper diagnosis of oral diseases difficult. This problem was encountered in the present case. Additionally, due to hemostatic alterations, even simple tooth extraction can precipitate crisis if adequate precautions are not taken. Noninvasive dental procedures do not require prophylactic platelet transfusions. For invasive procedures, desmopressin and antifibrinolytic drugs are used in mild cases and platelet transfusion in severe cases. Planning for complete treatment over a single sitting with platelet transfusion in a hospital setting is more desirable than planning for it over multiple sessions. 33 It helps save the trauma of multiple transfusions to the patient and has the advantage of being fully equipped in case of medical crisis.
The diagnosis of FA on the basis of clinical features is challenging due to the heterogeneous nature of the condition. The three types of investigations that are commonly used in the diagnosis of FA are chromosome breakage tests, mutation analyses, and bone marrow chromosome analyses. Chromosome breakage test is the first test to diagnose a patient with FA. Adding DNA cross-linking agents such as mitomycin C and diepoxybutane increases the number of chromosome breaks with distinct ranges for normal and FA cells, providing the basis for a diagnostic test. 34
The goal of FA treatment is to increase the survival rate of individuals and establish a better quality of life. The aim is to control physical alterations, reestablish the hematological condition, and treat the malignant alterations that develop in this population. The first line of therapy is androgens and hematopoietic growth factors, but only 50%–75% of patients respond. BMT is a definitive treatment but increases the risk of GVHD and SCC later on. Patients with FA need a close follow-up with an interdisciplinary team, which should include a hematologist for the control of anemia; a pediatrician for managing systemic problems of children; an endocrinologist for the assessment and treatment of developmental disorders; an ENT specialist for the examination of nasopharynx, oropharynx, and larynx; a cardiologist for heart diseases; and an oncologist for the management of tumors. A pediatric dentist should also be a part of the multidisciplinary team. Referral of patients to the pediatric dentist by a general dentist is necessary for the overall management of the patient and for the family's counseling. A highly planned preventive phase is important to prevent future radical treatment, which can be provided by a pediatric dentist. Treatment of acute dental infections should be carried out immediately and oral sources of infection should be eliminated, making sure that there are no foci of infection in order to ensure the overall health of the patient. Genetic testing should be done in all cases of suspected FA, siblings, parents, and close blood relatives. This will help in appropriate treatment planning and also in selecting a suitable donor for hematopoietic stem cell transplantation and to plan for genetic counseling.
Conclusion
Pediatric dentists are in a unique position to identify early changes or lesions associated with FA in the oral cavity. They must collaborate with the child's hematologist before any invasive procedure is undertaken. Knowledge of the various oral manifestations and their treatment is vital to ensure good oral health of these individuals. Given the chromosomal instability involved, hematological and endocrinal aberrations advocate differentiated and meticulous care for the affected patients. Providing an oral cancer screening with careful examination of mucosal tissues at every visit will help in early detection and treatment with subsequently more chances of survival. Pediatric dentists are an important part of the multidisciplinary team involved in the treatment and must be aware of the pathophysiology of the diverse oral diseases seen in FA. Regular follow-ups should be conducted to motivate the patients to maintain good periodontal health, help reduce the incidence of caries, and monitor the oral health of these individuals.
Author Contributions
Conceived the concepts: Mridula Goswami. Analyzed the data: Mridula Goswami, Urvashi Bhushan, Manoj Goswami. Wrote the first draft of the manuscript: Urvashi Bhushan. Contributed to the writing of the manuscript: Mridula Goswami, Urvashi Bhushan. Agree with manuscript results and conclusions: Mridula Goswami, Urvashi Bhushan, Manoj Goswami. Jointly developed the structure and arguments for the paper: Mridula Goswami, Urvashi Bhushan, Manoj Goswami. Made critical revisions and approved final version: Mridula Goswami. All authors reviewed and approved of the final manuscript.
