Abstract
Shifting from the historical TNM paradigm to the determination of molecular and genetic subtypes of tumors has been a major improvement to better picture cancerous diseases. The sharper the picture is, the better will be the possibility to develop subsequent strategies, thus achieving higher efficacy and prolonged survival eventually. Recent studies suggest that urokinase-type plasminogen activator (uPA), uPA receptor (uPAR), and plasminogen activator inhibitor-1 (PAI-1) may play a critical role in cancer invasion and metastasis. Consistent with their role in cancer dissemination, high levels of uPA, PAI-1, and uPAR in multiple cancer types correlate with dismal prognosis. In this respect, upfront determination of uPA and PAI-1 as invasion markers has further opened up the possibilities for individualized therapy of breast cancer. Indeed, uPA and PAI-1 could help to classify patients on their risk for metastatic spreading and subsequent relapse, thus helping clinicians in their decision-making process to propose, or not propose, adjuvant therapy. This review covers the implications for cancer diagnosis, prognosis, and therapy of uPA and PAI-1, and therefore how they could be major actors in the development of a precision medicine in breast cancer.
Introduction
Breast cancer (BC) is one of the most frequent cancers that occur in women. Worldwide, each year, the incidence and mortality have increased to over 1,050,000 newly diagnosed cases and 400,000 deaths. The progress made in terms of screening, treatment, and care support has contributed to improved relative survival (over 85% of BC five-year survivors after diagnosis).1,2 A significant improvement in survival correlates with early diagnosis and use of adjuvant therapy. A major step toward optimal care had been to define BC diversity and to accurately categorize patient sub-populations on a genomic and molecular basis, beyond standard histopathological TNM classifications.3,4 Biomarkers can be combined with clinicopathological characteristics to estimate recurrence risk (ie, prognostic value) and to predict therapy efficacy (ie, predictive value). Identifying patients with high risk for recurrence and administering optimal therapies while avoiding over-treating low-risk patients are major issues in BC management, because of the number of patients newly diagnosed each year. In addition, resistance to therapy and containment of metastatic spreading need to be effectively addressed for prolonging the survival. 5
In this context, two major compounds of the plasminogen activator system, urokinase-type plasminogen activator (uPA) and plasminogen activator inhibitor-1 (PAI-1), have been found to play possibly a key role in individualizing breast cancer treatment. The predictive value of the combinational use of these two biological markers for discriminating the risk group in both nodes positive and notably node-negative breast cancer patients has been subsequently established and validated.
Moreover, the combined ability of uPA/PAI-1 to predict both outcome and response/resistance to specific therapies should further lead to individualized management of patients with breast cancer, thus helping clinicians to predict treatment efficacy. 6 With the rise in personalized medicine, studying uPA/PAI-1 could be key to refine the therapeutic strategies in breast cancer. This review presents the biology, roles, and the putative role that uPA/PAI-1 could play in precision medicine in oncology.
Biology of the uPA System
The uPA system is a conversion system from plasminogen into plasmin, which plays important physiological roles. It also plays a key role in cancer invasion and metastasis dissemination by allowing malignant cells to invade the tumor site locally and spread to distant sites.7,8 This system includes the serine protease, uPA, membrane-linked receptor uPAR, and two serpin inhibitors, PAI-1 and PAI-2.
uPA is a 53-kDa serine protease initially synthesized as a catalytically inactive single chain polypeptide. pro-uPA whose proteolytic cleavage – mediated by different proteases including plasmin, cathepsin B, cathepsin L, and human kallikrein type 2 – gives the mature form that is a two-chain protein linked by a single disulfide bond. uPA can be structurally divided into three domains, an amino-terminal domain, which contains the binding site for uPAR, a carboxy terminal sequence containing the catalytic site, and a kringle domain of a yet unknown function.7,8
Unlike most serine proteases, uPA has two notable particularities. First, in contrast to many other proteases, uPA restricts substrate specificity, since it only converts inactive plasminogen to the enzymatically active form, plasmin, which is also a serine protease but has broad substrate specificity. Plasmin can particularly degrade several extracellular matrix (ECM) components such as laminin, fibronectin, and osteopontin.9,10 By cleaving these proteins, plasmin can activate growth factors and liberate them from ECM sequestration. The binding of these activated growth factors to their cognate receptors can cause increased proliferation, migration, invasion, and metastasis eventually. In addition, plasmin is able to activate precursor forms of a number of specific matrix metalloproteases, inter alia the precursor form of uPA, prouPA. These activated metalloproteases can then degrade the diverse forms of collagens, kallikrein-related peptidases, and other proteins in the ECM. 11
Thus, plasmin can play a critical role during multiple steps of cancer invasion and metastasis, by inducing the degradation of a number of ECM proteins and activating certain growth factors leading to aggressive cancers.12,13 The second characteristic of uPA is that both the proenzyme form (prouPA) and the active form of uPA bind with high affinity to their specific receptor. 14 uPAR is formed by a three-domain glycoprotein and because of lack of a transmembrane domain, uPAR will be linked to the cell membrane via a glycosyl phosphatidylinositol anchor. 15
To initiate signaling, uPAR must interact with molecules such as epidermal growth factor receptor, platelet-derived growth factor receptor, specific integrins, or low-density lipoprotein receptor-related (LDLR) proteins16–19 (Fig. 1). Then, the active complex uPA–uPAR initiates different signaling pathways, that is, the MAPK, Jak-Stat, and focal adhesion kinase systems. 20 All these signaling systems stimulate cell proliferation, enhance cell migration, and modulate cell adhesion.8,21 Thus, uPA may trigger cell signaling and trafficking by two distinct ways: directly by binding to its receptor uPAR and indirectly by the activation of plasmin (Fig. 3).

Urokinase plasminogen activation system: content and functions.
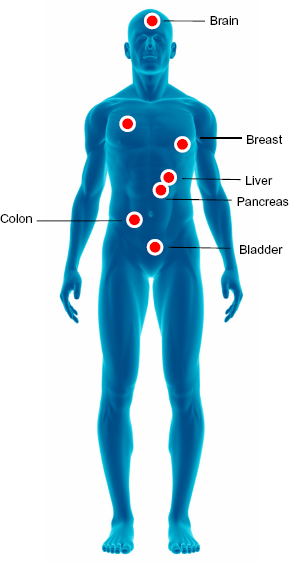
Solid tumors overexpressing uPA and uPAR.

t-PA, u-PA and their inhibitors.
In order to limit its proteolytic action, uPA can be inhibited by two protease inhibitors PAI-1 and PAI-2. PAI-1 is the primary physiological inhibitor of uPA, formed by a singlechain glycoprotein of 43 kDa. It reacts with UPA to form a stable complex.7,8 PAI-1 is also able to induce the internalization and degradation of uPAR-bound uPA; then, uPAR is itself endocytosed and recycled back to the cell surface. 22
There are 2 forms of PAI-2; a 47-kDa intracellular non-glycosylated form and a 60-kDa extracellular glycosylated form. 23 PAI-2 reacts in the same way but more slowly than PAI-1, and it has been shown that its overexpression inhibits apoptosis and therefore fosters cancer development. 24 Numerous studies indicate that the uPA system is involved in cancer.7,25,26 uPAR and uPA are overexpressed with remarkable consistency in a variety of human tumors, including leukemia and breast, lung, bladder, colon, liver, pleura, pancreas, and brain cancers.27–37 (Fig. 2).
Role of the uPA System in Breast Cancer
The results of experiments conducted on model systems have shown that uPA plays a major role in cancer invasion and metastasis. 38 Indeed, first reports have shown that there are correlations between the concentrations of uPA and the metastatic potential of various cell lines, and that using antagonist antibodies or small interfering RNA (SiRNA) against uPA tends to prevent or reduce metastases.8,39 Another confirmation of the role of uPA in metastatic spreading was obtained with uPA or plasminogen-deficient mice. Several studies reported that a deficiency in plasminogen in breast cancer mouse models reduced the formation of lung and lymph node metastasis without affecting main tumor growth. 40
It was originally believed that uPA promoted the spread of cancer simply by degrading the ECM, thus allowing invasion and metastasis. It is now widely acknowledged that there are additional activities supporting its role in the proliferation and spreading of cancer.6,41
During cancer invasion and metastasis, malignant cells must penetrate and remodel the ECM on several occasions. uPA has a limited specificity toward the ECM components and to date, it has only been shown to directly degrade fibronectin. 41 However, plasmin can digest most of the noncollagenous proteins including fibrin, laminin, fibronectin, and perlecan (a heparan sulfate proteoglycan).6,41–43 Plasmin can also contribute to the dissolution of the ECM by activating the precursor forms of certain MMPs. MMPs shown to be activated by plasmin include MMP-3, MMP-9, MMP-12, and MMP-13. 12 Clearly, therefore, regulated and focused proteolysis is necessary for promoting invasion. For uPA, degradation is likely to be achieved by binding to its receptor, while excessive proteolysis can be modulated by the endogenous inhibitors, that is, PAI-I and PAI-2. 8
In vitro studies have provided direct evidence that the uPA system is capable of stimulating mitogenesis. In some cell types, such as epidermal tumor lines (CCL.20.2) and melanoma cells,44,45 the mitogenic activity of uPA required both binding to uPAR and catalytic activity. On the other hand, with the human ovarian cancer cell line OV-MZ-6, only binding to the receptor was necessary for induction of proliferation. 46 Activation or release of a positive growth stimulation factor could also lead to a higher mitogenesis. Specific growth factors that are activated by plasmin and that stimulate cellular proliferation include FGF2, VEGF, IGF-1, and HGF.47,48
FGF2 and VEGF are well-known growth promoters of endothelial cells and therefore play a major role in angiogenesis, while IGF-1 and HGF stimulate the growth of epithelial cells.49–51 Angiogenesis is required for tumor growth, invasion, and metastasis. uPA acting through its receptor plays a key role in the multi-step mode. This role is likely to include both the ECM remodeling, allowing endothelial cells to invade the tumor stroma and the activation/release of pro-angiogenic factors such as FGF2, TGFb, and VEGF 13 (Fig. 4).

The role of uPA-R and other effectors in the growth of epithelial cells.
Because uPA promotes angiogenesis, we can assume that PAI-1 inhibits the process. Indeed, the different effects of PAI-1 on angiogenesis seem to be related to its concentration. Remarkably, in a recent study, PAI-1 was found to be proangiogenic at nanomolar concentrations corresponding to normal concentrations in the mouse plasma, but anti-angiogenic at micromolar concentrations. 52
To generate metastasis, malignant cells must migrate from their primary site to a distant location. Using both MCF-7 breast cancer cells and HT1080 fibrosarcoma, it was shown that uPA-enhanced cell migration required co-operation between the Ras-Erk and Rho-Rho kinase pathways. 53 It is therefore not surprising that in addition to enhancing cell migration, uPA may also stimulate cell adhesion. Attaching uPA modifies uPAR conformation receptor, which increases its affinity for vitronectin. These events, however, occur only when uPA is present in excess as compared with PAI-1. 54 Few studies have attempted to study the epigenetics of the uPA/PAI-1 system and it was demonstrated that uPA is hypomethylated and methylation of PAI-1 gene has been suggested as one of the molecular mechanisms involved in breast cancer associated with the downregulation of the expression of PAI-1.55,56
Recently, uPA was also shown to be able to prevent apoptosis. The inhibition of apoptosis could thus increase the survival potential of malignant cells during the metastatic process, therefore increasing the possibility for the establishment of secondary lesions. In addition, it could help tumor cells to acquire resistant phenotype in stress conditions, that is, after treatment. The ability for uPA to signal through uPAR will maintain an elevated basal level of activated ERK while inhibiting apoptosis, thus representing a novel mechanism by which the uPA–uPAR system may affect breast cancer progression in vivo. 57 This multifunctional capacity can explain why the uPA system is a powerful mediator of cancer spreading, and it has been identified as both a predictive and prognostic marker in breast cancer.
Predictive Value of uPA System as a Response Marker
Several studies have tried to establish whether uPA status could be associated with antitumor efficacy of several regimens, especially cytotoxic chemotherapy.
The predictive value of uPA/PAI-1 to forecast response to CMF regimen (ie, cyclophosphamide, methotrexate, and fluorouracil) has shown an intermediate level of evidence (ie, LOE II) and therefore remains to be confirmed in further randomized studies. 58 In high-risk patients (ie, high levels of uPA and/or PAI-1), a better response was achieved, especially in grade 2 patients, thus suggesting that chemotherapy was beneficial eventually. The CMF protocol is nevertheless the therapeutic standard, irrespective of the uPA PAI-1status. The results of the European trial NNBC-3 (“Node Negative Breast Cancer 3-Europe”), using uPA/PAI-1 as a discriminating factor to predict response to anthracyclines and taxanes in patients with no lymph node metastasis, has shown a high risk of relapse in patients with high uPA and PAI-1 values compared to clinical-pathological factors. 59 In addition to the trial by Janicke et al (2004), by using uPA and PAI-1 it has been shown that it is possible to classify about half of the patients with negative lymph node breast cancer as low risk, for whom chemotherapy in adjuvant conditions can be avoided, and half as high risk, who appear to benefit from adjuvant chemotherapy. 60
In the multicentric prospective study conducted by the AGO group including patients without lymph node metastasis, high uPA and PAI-1 patients (ie, 182/315) were further randomized between chemotherapy (CMF: n = 88) or observation (n = 94). 60
Among the 241 patients in the low-risk group, relapse-free survival at three years was 93.3% (P = 0.006) and the relapse rate was 6.7%. Before any treatment, in patients with high values of uPA and/or PAI-1 (n = 315), disease-free survival at three years was 85.3% and the relapse rate was 14.7%. These data confirm the previous findings in the literature as reviewed by Prechtl et al (2000) and led the Ethics Committee to validate this test, allowing better individualization of adjuvant treatment for patients with high levels of uPA and/or PAI-1. 61 In pN0 patients, uPA/PAI-1 reached the highest level of evidence (LOE I) for the prognostic value of disease-free survival at 10 years. For Oncotype DXTM and MammaPrint®, as on date, the prognostic and predictive values have not reached the level of evidence LOE I, which clearly shows the interest of uPA/PAI-1 in predicting the response to neoadjuvant chemotherapy. 62
Complementary analyses showed that adjuvant chemotherapy reduced the risk of relapse to 43.8% but over a short follow-up period only (three years). 63 Similarly, when the global population (ie, with or without lymph node metastasis) was studied, response to chemotherapy was higher in patients with elevated levels of uPA/PAI-1.64,65
The clinical application of these findings would be to provide additional information that could facilitate the selection for chemotherapy. However, for definitive conclusions about the predictive value of uPA/PAI-1 as a response marker with systemic therapies in various different molecular subtypes of breast cancer, large prospective trials are warranted.
Implementing uPA/PAI-1 Determination as Part of Precision Medicine in Breast Cancer
Modern oncology has entered the era of precision medicine, a generic term that encapsulates all the effort to shift from standard to customized treatment. Individualized medicine is mostly based on huge resources to identify markers that are likely to predict the level of aggressiveness of a newly diagnosed cancer, and next to search for predictive markers of response to a given therapy. Such preliminary information can be used subsequently to help clinicians to select the best strategies (ie, administrating systemic adjuvant therapy or not) and the best drug or drugs combination to be given, should they be given.66,67 Avoiding unnecessary treatments is now a critical issue in oncology, both because of the cost of the drugs (ie, with targeted therapies) and the possible treatment-related severe toxicities (ie, with cytotoxics), thereby negatively impacting the quality of life and efficacy–toxicity balance eventually. In this respect, using reliable markers that are likely to predict a risk for relapse or metastatic spreading is a promising strategy to implement precision medicine at the bedside. Several studies have tried to develop dedicated mathematical models as in silico tools for such a purpose.68,69
From a bioguided-medicine standpoint, as a follow-up to studies performed on patients with primary breast cancer, the Receptor and Biomarker Group of the European Organization for Research and Treatment of Cancer (EORTC) has validated the prognostic role that uPA and PAI-1 could play for this kind of cancer. 70 According to uPA/PAI-1 levels, therapeutic management has therefore changed.71,72 In particular, uPA and PAI-1 are critical in lymph node–negative patients because it can reduce significantly the over-treatment rate in patients with little risk of metastatic relapse. 73
In accordance with the St. Gallen Consensus guidelines, 73 more than 90% of node-negative patients today receive adjuvant systemic therapy, even though only 30% of these patients will eventually relapse. The low-risk group identified by uPA/PAI-1, representing about 50% of node-negative breast cancer patients, has a low risk for disease recurrence and usually excellent prognosis. This group has 10 years of disease-free survival (DFS) and overall survival (OS) of 87% and 90%, respectively, without any adjuvant systemic therapy.74,75 With today's standards of endocrine therapy, these patients would have a 10-year OS over 90%, with much milder treatment-related toxicities as compared with chemotherapy. Such encouraging results can, therefore, be used to support individualized therapy decisions. 76
Recent observations suggest that only patients considered high risk based on their values of uPA/PAI-1 shall benefit from adjuvant chemotherapy.71,72 Consequently, associating chemotherapy to novel targeted agents is justified with respect to the uPA/uPA-R-values. 77 Indeed, along with canonical nodal status, uPA and PAI-1 seem to be strong predictive factors for both DFS and OS.
Conclusions and Perspectives
Refining treatment modalities is now a major trend in clinical oncology. Bioguided medicine is largely implemented in several settings (lungs, digestive, melanoma), mostly as part of the upfront determination of biomarkers predictive of response to targeted therapies. Breast cancer has pioneered the field of personalized medicine through molecular and genomic determination of cancer sub-types, supplanting historical TNM classification. uPA/PAI-1 could be an emerging, new powerful marker to further refine the picture of the disease. In addition to selecting the best treatments and strategies to be undertaken in breast cancer patients, avoiding unnecessary adjuvant therapy is now a critical issue indeed. Along with other approaches, using upfront uPA/PAI-1status determination as a marker of risk for metastatic relapse could help to better select BC patients requiring a systemic therapy. In addition, uPA/PAI-1 could help as well to forecast treatment efficacy, thus potentially being part of a bioguided therapy.
Author Contributions
Conceived and designed the review: AG, KE, SB. Analyzed the data: AG, KE, AD. Wrote the first draft of the manuscript: AG, AD, KE, NL, AA. Contributed to the writing of the manuscript: JC, MC, GM. Agree with manuscript results and conclusions: AG, GM, JC, MC. Jointly developed the structure and arguments for the paper: AG, KE. Made critical revisions and approved final version: AG, KE, GM. All authors reviewed and approved of the final manuscript.
