Abstract
The biomarker potential of using various lipids fractions for predicting risk of acute myocardial infarction (AMI) is controversial. We therefore compared the lipid profiles, including serum total cholesterol (TC), low-density lipoprotein cholesterol (LDL), high-density lipoprotein cholesterol (HDL) and triglycerides (TG), in 67 AMI patients. Patients included 28 STEMI (ST-elevated myocardial infarction) patients, 39 NSTEMI (non-ST-elevated myocardial infarction) patients and 25 patients with chest pain. Control group included 54 age- and gender-matched normal subjects. We also studied the correlation between lipid profile and systemic inflammation in these subjects. There were significant decreases in TC, LDL and HDL levels in both STEMI and NSTEMI patients as compared to normal subjects; however, patients with chest pain did not show any significant change in these lipids. Serum TG levels did not differ significantly among the study groups. There were significant increases in serum high-sensitive C-reactive protein (hs-CRP) levels in STEMI and NSTEMI patients, as compared to control group. Serum hs-CRP showed significant inverse correlation with HDL; however, hs-CRP was not correlated with TC, LDL, and TG. In conclusion, our findings suggest that reduction in serum TC does not prevent the risk of AMI, whereas a decrease in serum HDL and increase in hs-CRP strongly predisposes the risky individuals to an AMI event. We emphasize the importance of HDL and CRP measurements for the assessment of a combined lipid-inflammation risk factor that could be a useful predictor of high risk individuals, as well as a prognostic marker in AMI patients.
Introduction
The pathogenesis of acute myocardial infarction (AMI) is multifactorial; however, several studies have implicated impaired lipid metabolism as one of the crucial factors in the development of this disease. Kumar et al 1 observed significantly higher total cholesterol (TC) and triglyceride (TG) levels and lower high-density lipoprotein cholesterol (HDL) levels in AMI patients. In a series of 50 male AMI patients, serum low-density lipoprotein cholesterol (LDL) levels and the ratio of LDL to HDL were not significantly different among the two groups; however, serum HDL levels were significantly decreased in AMI group. 2 The risk of AMI was associated with an increase in LDL and a decrease in HDL, in both Asians and non-Asians. 3 Lower concentrations of serum HDL and higher serum TG were found to be independent risk factors, while serum LDL was not associated with AMI. 4 Woo et al 5 observed higher mean TC, LDL, and TG, as well as lower mean HDL in AMI patients; high HDL was among the protective factors. Lehto et al 6 did not find any difference in mean serum TC levels between the AMI patients and controls, whereas mean HDL was significantly lower in the AMI group. The cardiac marker, troponin T, has been positively correlated with TC, LDL, and TG and negatively correlated with HDL. 7
The management of dyslipidemia after myocardial infarction is an important aspect of post-myocardial infarction care. 8 Using the bivariate and multivariate Cox proportional hazards analysis to identify independent predictors of subsequent major adverse coronary events (hospitalization for AMI or acute coronary syndrome), it was found that HDL predicted major adverse coronary events, which in turn provided support for interventions targeting HDL for cardiovascular risk reduction. 9 Another Cox proportional hazards model has revealed that plasma HDL—but not LDL—predicts the risk of recurrent cardiovascular events over the ensuing 16 weeks. Even LDL reduction does not account for the clinical risk reduction with atorvastatin treatment after acute coronary syndrome (ACS). 10 Li et al 11 have shown that the cases with low HDL level had rates of AMI events and CHD mortality similar to those of the entire group, including hyperlipidemia. However, AMI attacks and deaths decreased significantly at the normal and high HDL levels, indicating that protective effect of HDL against coronary artery disease is more prominent in people with low lipid level.
The above literature clearly indicates an important role of lipids metabolism in AMI. However, the biomarker value of various components of lipids profile is not clear due to conflicting findings in various studies. We therefore compared the lipid profiles of AMI and chest pain patients with respect to normal subjects. In addition, we also studied the role of inflammation in AMI and evaluated its correlation with lipid profiles.
Patients and Methods
This prospective study was conducted on 67 AMI patients and 25 patients with chest pain admitted to Prince Sultan Cardiac Center and King Khalid University Hospital, Riyadh, Saudi Arabia. The AMI patients were classified into STEMI (ST-elevated myocardial infarction, N = 28) and NSTEMI (non-ST-elevated myocardial infarction, N = 39). Mean ages of STEMI, NSTEMI, and chest pain patients were 56.21 ± 12.65 years, 61.98 ± 10.83 years, and 53.83 ± 13.75 years, respectively (Table 1). We also included 54 age- and gender-matched controls for comparison.
Characteristics of subjects.

The diagnosis of myocardial infarction required the presence at least two of the following criteria: (i) history of characteristic prolonged (≥30 minutes) pain or discomfort, (ii) creatine kinase (CK) levels exceeding twice the upper limit of normal (or CK—MB ≥ 50% of total CK); (iii) presence of new Q waves or new abnormal ST—T features. 12 Patients with STEMI were classified on the basis of the following criteria: (i) continuous chest pain upon presentation, refractory to nitrates, and lasting ≥ 30 minutes; (ii) ST-segment elevation of ≥0.2 mV in ≥2 contiguous precordial leads, or ≥0.1 mV in ≥2 contiguous limb leads, or new left bundle branch block on admission electrocardiogram; (iii) presentation within the first 12 hours from index pain. Patients with NSTEMI were required to have angina-like chest pain at rest in the last 24 hours lasting ≥ 5 minutes, with associated ST segment depression of ≥0.1 mV in ≥2 contiguous leads upon presentation. 13 The patient exclusion criteria included recent surgery, active infection, chronic inflammatory diseases, significant hepatic, or renal dysfunction and malignancy. The protocol of this study was approved by our Institutional Review Board (IRB) for human studies and all the patients signed informed consent.
Venous blood was collected after overnight fasting from all the subjects in serum separator Vaccutainer tubes. The levels of serum total cholesterol, lipoproteins, triglycerides, and hs-CRP were analyzed using an Autoanalyzer (Roche, Germany). The data were evaluated by one-way analysis of variance (ANOVA) followed by Dunnett's multiple comparison test using SPSS statistical package version 17. Pearson's and Spearman's tests were used for correlation analysis of continuous and categorical variables respectively.
Results
The characteristics of patients and controls are summarized in Table 1. The family history of associated diseases was noted for hypertension (3/28 STEMI, 1/39 NSTEMI and 5/25 chest pain) and CAD and hypertension (1 STEMI, 2 NSTEMI and 2 chest pain). There were significant decreases in TC (ANOVA F = 13.848,
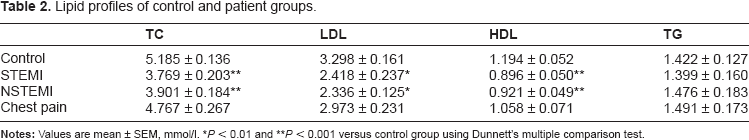
Lipid profiles of control and patient groups.

Box plots showing lipid profile (TC, LDL, HDL and TG) in normal subjects and patients with AMI (STEMI and NSTEMI) and chest pain.

Ratios of TC, LDL and TG to HDL in controls and different patient groups.
There were significant increases in serum hs-CRP levels in STEMI and NSTEMI patients as compared to control group (ANOVA F = 3.213,

Serum hs-CRP in different groups.
Age was significantly and inversely correlated with TC (R = −0.144,
Correlations between subjects' characteristics and biochemical parameters.

Statistically significant.
Discussion
Our results showed significant decreases in TC, LDL, and HDL levels in AMI patients (Table 2). Gorecki et al 14 observed higher levels of TC and LDL in patients with complicated versus those with uncomplicated clinical course of infarction, suggesting higher levels of these biomarkers during the first 24 hours of AMI have a strong negative prognostic value.
Akosah et al 15 reported acceptable or optimal LDL levels in a series of 183 young adults experiencing AMI. Gaziano et al 8 found that the mean TC and LDL levels were significantly lower while in-hospital than levels 2 to 3 months later; however, from a clinical perspective, in-hospital levels can be used to guide decisions regarding lipid-lowering therapy, which can begin in the immediate post-MI setting. In a series of 34 AMI patients, on the first day after admission there were significant decreases in TC (14.1%) and LDL (14.4%), as well as insignificant decreases in HDL (9.3%) and TG (19.5%). 16 On the basis of lipid profile data of 97 patients with NSTEMI and unstable angina, it has been concluded that HDL level (as opposed to LDL and TG) adds prognostic value to the prediction of in-hospital recurrent events during non-ST-elevation acute coronary syndromes. 17 Rosoklija et al 18 have followed-up the HDL cholesterol levels in STEMI patients from 24 hours to 3 months and concluded that the optimal times for determining the HDL level are the first 24 hours of the actual event; this is due to the fact that in the first 24 hours there is a relevant decrease of the HDL cholesterol level in the blood. The cause of reduced serum lipids in AMI patients in our study is not clear. It could be related to dietary modifications or due to metabolic changes during acute crisis. Nevertheless, the lipids data negate the general conception that dietary lipids restrictions may prevent the risk of AMI.
High serum levels of HDL are associated with reduced risk for the development of atherosclerotic disease. HDL particles are believed to be antiatherogenic, secondary to their capacity to drive reverse cholesterol transport and antagonize pathways of inflammation, thrombosis, and oxidation. The majority of patients in both the primary and secondary prevention settings continue to experience significant residual risk for acute cardiovascular events, even when their LDL cholesterol is lowered aggressively via a combination of lifestyle modification and pharmacologic intervention. 19 Al Aqeel et al 20 have observed that HDL appears to be the main lipid risk factor in patients presenting with AMI in Kuwaiti patients, suggesting that primary prevention strategies should focus on treatment modalities that increase HDL. In an in-vivo mouse model of myocardial ischemia/reperfusion, it has been observed that HDL and its sphingolipid component, sphingosine-1-phosphate, dramatically attenuated the infarct size, suggesting a rapid therapeutic elevation of plasma HDL levels may be beneficial in patients at high risk of acute myocardial ischemia. 21 There is an increased focus on targeting and treating low serum levels of HDL in an effort to further reduce risk for cardiovascular events, including myocardial infarction. 19
In our study, none of the lipids ratios were found to be informative in prediction of AMI (Fig. 2). On the contrary, LDL/HDL ratio has been suggested to be an independent predictor for AMI in the Japanese rural population. 22 Goswami et al 23 have suggested that the apo-B/apo-AI ratio is a better discriminator of CAD risk in the atherosclerosis-prone population than any of the conventional lipid ratios such as TC/HDL or LDL/HDL. Karthikeyan et al 3 have also found the strongest association occurs between ApoB/ApoA1 and the risk of AMI. McQueen et al 24 have observed the highest population-attributable risk (PAR) with the ratio of ApoB/ApoA1 (54%) compared to the PAR associated with the ratios of LDL/HDL (37%) and TC/HDL (32%).
We observed significant increase in hs-CRP levels in AMI patients (Fig. 3), which is in agreement with earlier reports.25–27 hs-CRP is a sensitive marker of inflammation and a potential independent predictor of cardiovascular disease as it may play a role in the development of atherosclerosis; additionally, it also adversely affects mortality 28 Suzuki et al 29 have found nearly equivalent systemic and coronary levels of hs-CRP in AMI patients. They also observed a positive correlation between systemic hs-CRP and coronary plaque area, suggesting an important link between systemic and coronary levels of inflammation. Their observations are also associated with vulnerable coronary morphology in the development of acute coronary syndromes. 29 Higher baseline hs-CRP level showed significant association with 12-month all-cause mortality, independent of other prognostic markers, in overweight or obese AMI patients. 30 The findings of a cross sectional study of 188 patients with STEMI suggested that plasma hs-CRP could be useful for prediction of development of heart failure in AMI patients. 31 Elevated serum hs-CRP levels in patients with AMI < 6 hours may portend vulnerable plaque rupture. 32 The patients with persistent, severe, treatment-unresponsive unstable angina (UA) had significantly higher CRP levels and a higher incidence of clinical events than patients with treatment-responsive UA, suggesting an important prognostic value of plasma CRP. 33 However, there was no correlation between plasma CRP and TC or HDL in UA patients. 33 A significant inverse correlation between hs-CRP and HDL (but not with other lipid fractions), as observed in our study, indicates the co-existence of inflammation and impaired lipid metabolism in AMI patients. The correlation data showed that serum HDL was not affected by age, gender, BMI, smoking, and blood pressure (Table 3). Although the levels of hs-CRP were directly correlated with age, hs-CRP was not influenced by gender, BMI, smoking, and blood pressure (Table 3).
Conclusion
Our findings suggest that reduction in serum cholesterol does not prevent the risk of AMI. There was a significant increase in systemic inflammation in AMI patients, inversely correlated with HDL levels, suggesting an important role of inflammatory mediators in AMI. Thus, a decrease in serum HDL and increase in hs-CRP strongly predispose the risky individuals to the event of AMI. We emphasize the importance of HDL and hs-CRP measurements in the assessment of a combined lipido-inflammatory risk factor for the screening of high risk individuals and the prognosis of AMI.
Author Contributions
Conceived and designed the experiments: HAK, ASA, SHS. Analyzed the data: HAK. Wrote the first draft of the manuscript: HAK. Contributed to the writing of the manuscript: HAK, ASA, SHS. Agree with manuscript results and conclusions: HAK, ASA, SHS. Jointly developed the structure and arguments for the paper: HAK, ASA, SHS. Made critical revisions and approved final version: HAK, ASA, SHS. All authors reviewed and approved of the final manuscript.
Funding
A grant from National Plan for Science and Technology (NPST) Program by King Saud University Project Number 08-BIO571–02.
Competing Interests
Author(s) disclose no potential conflicts of interest.
Disclosures and Ethics
As a requirement of publication author(s) have provided to the publisher signed confirmation of compliance with legal and ethical obligations including but not limited to the following: authorship and contributorship, conflicts of interest, privacy and confidentiality and (where applicable) protection of human and animal research subjects. The authors have read and confirmed their agreement with the ICMJE authorship and conflict of interest criteria. The authors have also confirmed that this article is unique and not under consideration or published in any other publication, and that they have permission from rights holders to reproduce any copyrighted material. Any disclosures are made in this section. The external blind peer reviewers report no conflicts of interest.
Footnotes
Acknowledgments
This study was supported by the National Plan for Science and Technology (NPST) Program by King Saud University Project Number 08-BIO571-02. We are thankful to Dr. Shahid Habib and Dr. Abdulrahman Al Moghairy for their clinical observations. We would also like to acknowledge the technical assistance of Adnan Ali Khan and the nursing staff of the King Khalid University Hospital and the Prince Sultan Cardiac Center (Riyadh) for sample collection and patient care.
