Abstract
PTP1B is involved in the oncogenesis of breast cancer. In addition, neoadjuvant therapy has been widely used in breast cancer; thus, a measurement to assess survival improvement could be pathological complete response (pCR). Our objective was to associate PTP1B overexpression with outcomes of breast cancer patients who underwent neoadjuvant chemotherapy. Forty-six specimens were included. Diagnostic biopsies were immunostained using anti-PTP1B antibody. Expression was categorized as negative (<5%) and overexpression (≥5%). Patients' responses were graded according to the Miller-Payne system. Sixty-three percent of patients overexpressed PTP1B. There was no significant association between PTP1B overexpression and pCR
Introduction
Breast cancer is one of the most common cancers in women around the world, with a higher incidence in developing countries.1,2 Breast cancer treatment is multimodal, and although it has been demonstrated that there is no difference in outcomes when comparing adjuvant and neoadjuvant therapies,3–5 the latter is currently the standard treatment for large and locally advanced tumors, allowing conservative surgeries without compromising the results in overall survival (OS). In addition, prognostic and treatment options can be influenced by clinical and pathological characteristics of breast cancer given the heterogeneity of this condition.6,7 Breast cancer molecular subtypes were originally defined by their genetic profile8,9 but can be assessed using immunohistochemistry for estrogen receptor (ER), progesterone receptor, Ki67, and erbB-2 receptor protein-tyrosine kinase (PTK; human epidermal growth factor receptor 2 (HER2)).10,11 These subtypes are known for their different epidemiologic risk factors and response to treatment. 10 On the other hand, pathological complete response (pCR) is a surrogate marker for outcomes in breast cancer. According to Cortazar et al, 12 a pCR of 18% was achieved in all subtypes, with a higher response in luminal B (HER2+) (30%), triple-negative (34%), and no luminal HER2+ (50%) subtypes, showing a pCR <10% in luminal A subtype.
In 1981, the World Health Organization (WHO) first published tumor response criteria, mainly for use in trials where tumor response was the primary endpoint. The WHO criteria introduced the concept of an overall assessment of tumor burden by summing the products of dimensional lesion measurements and determined response to therapy by evaluation of change from baseline while on treatment. 13 However, in the decades that followed their publication, cooperative groups and pharmaceutical companies that used these criteria often made some modifications, which led to confusion in the interpretation of trial results, 14 and the application of varying response criteria led to very different conclusions about the efficacy of the same regimen. 15 In response to these problems, an International Working Party was formed in the mid-1990s to standardize and simplify response criteria. The Response Evaluation Criteria in Solid Tumors (RECIST) was introduced in 2000 by an International Working Party to standardize and simplify tumor response criteria. 16 RECIST has subsequently been widely accepted as a standardized measure of tumor response, particularly in oncology clinical trials in which the primary endpoints are objective response or time to progression. 17 pCR after chemotherapy in primary breast cancer tumors has been an important prognostic factor for survival. 18 Despite a high specificity using imaging methods, sensitivity remains low, since not all patients with clinical response achieve a pCR, making it necessary to evaluate other measurement methods based on predicting factors. 19
Furthermore, when patients do not achieve a pCR to chemotherapy, the response has to be classified according to a grading system. There is no reference definition for pathological response. Miller and Payne grading system can predict OS and disease-free interval in patients with large and locally advanced breast cancers, assessing the histological response to primary chemotherapy. They reported a significant correlation between pathological response using this new grading system and OS (
Protein phosphorylation on tyrosine residues is an important event in post-transduction signaling of cells in order to regulate diverse responses. The regulation during these processes is crucial to maintain several biological effects, such as cellular proliferation, differentiation, migration, and apoptosis. PTP1B, a non-transmembrane member of this family, has long been studied as a negative regulator of insulin and leptin signaling, but has recently received renewed attention as a factor in oncogenesis.21,22 Supporting a possible oncogenic role of PTP1B in breast cancer is the finding that overexpression of PTP1B in the mouse mammary gland leads to spontaneous mammary tumor development, suggesting that this tyrosine phosphatase can act as an oncogene on its own. 23 In human beings, overexpression of PTP1B in breast epithelial cells distorts the normal acinar morphology and causes uninhibited proliferation and loss of polarity. 24 PTP1B has been potentially associated with the HER2 and its modulation of signaling. Wiener et al 25 reported that 21 out of 29 human breast cancers stained strongly for PTP1B when compared to normal breast tissue. This strong association between PTP1B and HER2 expression suggests that PTP1B and HER2 may cooperate in the pathogenesis of this subtype of breast cancers. More recently, Soysal et al 26 reported that PTP1B expression in breast cancer is associated with significantly improved clinical outcome.
To further explore the role of PTP1B in human breast cancer, we conducted an immunohistochemical study using 46 formalin-fixed breast cancer tissues of patients who underwent neoadjuvant chemotherapy, with clinical information and outcome data. The aim of our study was to investigate the association between PTP1B overexpression and pCR to study the impact of PTP1B on prognosis.
Materials and Methods
Breast cancer patients treated with neoadjuvant therapy, identified in a national health institute in Mexico City, Mexico (Instituto Nacional de Ciencias Médicas y Nutrición Salvador Zubirán), from 2003 to 2015, with available paraffin-embedded initial diagnostic biopsy and surgical specimens (mastectomy/conservative surgery) were included. This protocol was approved by the institutional research and ethics committees under the register HEM-1501.
Data Collection
All the information was collected from the hospital archives. Electronic records, including imaging and pathology, were also revised.
Immunohistochemistry
Immunohistochemical study was performed on formalin-fixed, paraffin-embedded breast cancer tissue using a polyclonal anti-PTP1B antibody (H-135: SC-14021, Santa Cruz Biotechnology) in a dilution of 1:200. Spleen was used as positive control tissue. No negative control was used. Tissues were sectioned at 5 μm and floated on distilled water at 45°C. Sections were mounted on chemically charged glass slides followed by drying at room temperature and incubated overnight at 57°C. The sections were deparaffinized according to established guidelines and quenched with 3% hydrogen peroxide for five minutes. They were rinsed in distilled water followed by Tris-buffered saline. Afterward, heat-induced antigen retrieval with citrate buffer at pH 6 was performed for 30 minutes followed by 15-minute cool-down period. Standard Dako EnVision + System-labeled Polymer Anti-rabbit + Liquid DAB + Substrate Chromogen System (DAB) technique was performed. Slides were developed, rinsed with distilled water, and counterstained with hematoxylin solution. Slides were mounted using aqueous solution, and the percentage of cells with a distinctive strong cytoplasmic staining was estimated by a light microscope.
Evaluation of Biopsies
The percentage of cells with a strong PTP1B cytoplasmic staining was estimated by two independent pathologists. All cases with a cytoplasmic PTP1B expression of <5% were considered negative (Fig. 1A), and ≥5% were considered positive (overexpression). Posteriorly, pathologic response to neoadjuvant chemotherapy was evaluated in specimens from the surgical procedure by two independent pathologists, which was graded according to Miller and Payne grading system (Tables 1 and 2). pCR was defined as absence of residual tumor in breast and axillary lymph nodes. Also, breast cancer subtypes were reanalyzed in the available immunostained biopsies.
Miller and Payne grading system for evaluation of breast tissue. 20

Miller and Payne grading system for evaluation of lymph nodes. 20


Cytoplasmic expression of PTP1B: (
Statistical Analysis
Patients' clinical and histological characteristics between PTP1B-positive and PTP1B-negative tumors were compared using chi-square test, Wilcoxon rank-sum test, or two-sample
Results
The final analysis included 46 breast cancer patients treated with neoadjuvant therapy based on the sequence of paclitaxel and doxorubicin plus cyclophosphamide.
The mean age at diagnosis was 55.4 years (range 32–80 years). Fifty-two percent of patients were diagnosed and treated after 2011. The mean tumor size at diagnosis was 3.5 cm (range 0.5–20 cm). Twenty-one patients (46%) presented positive lymph nodes demonstrated by imaging or physical examination, and 50% of patients had tumors of stage IIA. The most common breast cancer histological subtype was invasive ductal carcinoma (85%), followed by invasive lobular carcinoma (9%) and ductal carcinoma in situ (4%; Table 3).
Patients' demographic data.

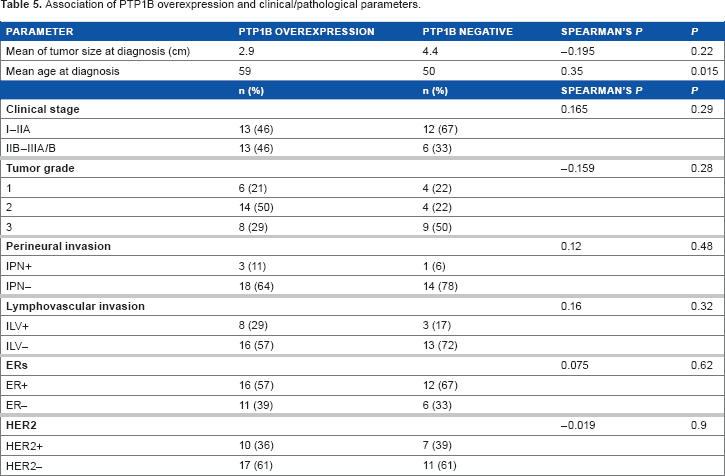
Consistent with the known cytoplasmic localization of PTP1B, breast cancers expressing this phosphatase showed strong PTP1B staining (≥5% and >50%, as shown in Fig. 1B and C). Twenty-nine patients (63%) overexpressed PTP1B (Table 4). PTP1B expression was not associated with tumor size, lymph node status, tumor grade, and pathological or clinical stages (Table 5). However, statistical significance was found when comparing age in PTP1B overexpression and PTP1B negative groups (59 vs 50 years, respectively,
PTP1B cytoplasmic expression.

Association of PTP1B overexpression and clinical/pathological parameters.
Moreover, PTP1B overexpression was associated with the subtypes of breast cancer, according to those defined at St. Gallen. PTP1B overexpression was higher in HER2-enriched subtypes (90%,
Association of PTP1B overexpression and molecular subtypes of breast cancer.

Breast pathological response was as follows: G1 9% (
Pathological response (Miller and Payne grading system).

Association between PTP1B expression and pathological response in breast and axillary lymph nodes.
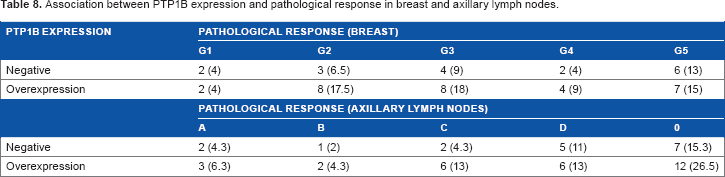

PTP1B overexpression (≥5%) and pCR (G5 + A or D) were associated, showing that 50% of patients who overexpressed PTP1B had no pCR compared to 28% of the PTP1B negative group (
Association of overexpression of PTP1B and pCR (

The median follow-up was 41 months (range 5–116 months). Neither nine-year OS curve (92 vs 91%, respectively,

Nine-year OS depending on PTP1B overexpression (dotted line: PTP1B overexpression and solid line: negative PTP1B expression;
Discussion
PTP1B is a widely expressed non-receptor PTP that is localized on intracellular membranes via a hydrophobic C-terminal targeting sequence. A role for PTP1B in the regulation of many cellular functions has been suggested. 27 Clinically, PTP1B is a critical node of insulin signaling due to its ability to dephosphorylate and inactivate the insulin receptor, thereby switching off this pathway.28,29 In fact, PTP1B-deficient mice are a unique model of insulin hypersensitivity due to enhanced insulin action.30–32 PTP1B is also involved in the control of immune cell signaling.33,34
PTP1B expression and its activity have been associated with the oncogenesis of diverse types of cancers such as esophagus, ovarian, colon, and breast cancers.25,35–38 In 1994, an association of the overexpression of PTP1B was first reported in a small cohort of patients with breast cancer.
25
However, the exact biological mechanism by which PTP1B facilitates breast cancer progression remains unknown. Previous studies in murine models have shown that the absence of PTP1B in mammary tumors (NDL2/PTP1B–/–) confers a delay in tumor development and a decreased frequency of lung metastases.
22
In breast cancer cells, a poor clinical outcome is associated with the amplification or expression of some PTK factors. It has been suggested that PTP1B is necessary for implantation and progression of mammary tumors.
39
PTP1B overexpression has also been associated with HER2+ and with a more aggressive breast cancer phenotype.
40
In human beings, there is no evidence of PTP1B as a prognostic factor. The existent data report the amplification of chromosome 20q13, where PTP1B gene is located, and it is demonstrated that the amplification of this region is associated with a poor prognosis in breast cancer.41–43 More recently, Soysal et al
26
published that 49% of patients with breast cancer express PTP1B and this was associated with a significant improvement in OS; however, we could not confirm this finding in our cohort (
Our study shows that PTP1B is overexpressed in 63% of breast cancer, which is consistent with previous reports (49–72.4%).25,26 Furthermore, our results did not show an association between PTP1B overexpression and tumor size at diagnosis, tumor grade, clinical stage, lymphovascular or perineural invasion, HER2, or ER. Interestingly, the difference between age at diagnosis was statistically significant when comparing patients overexpressing PTP1B and negative patients (59 vs 50 years, respectively,
The association between PTP1B expression in breast cancer and treatment based on two taxanes, paclitaxel and docetaxel, has been studied in vitro. The expression of this phosphatase correlated with the opposite sensitivity to these drug agents. 44 However, the molecular mechanism of this effect is not yet known. Both taxanes act by disrupting the function of microtubules. 45 Microtubule instability is necessary for cellular functions and is regulated by microtubule-associated proteins (MAPs), which in their dephosphorylating state bind to microtubules stabilizing them45–48 and act as a coupling site for some kinases and phosphatases.48,49 MAPs/microtubule affinity-regulating kinases (MARKs), which regulate phosphorylation state of MAPs, are regulated by two phosphatases: phosphatase 2A and PTP1B. 46 It is possible that an increase in PTP1B levels conditions a major dynamic instability due to MARK dephosphorylation and, at the same time, a chemoresistance to paclitaxel.45,50
Our study could not associate PTP1B overexpression and pCR in breast cancer patients treated with neoadjuvant chemotherapy (
Finally, recent in vitro studies are investigating the role of PTP1B and its interaction with other proteins51–53 involved in breast cancer oncogenesis,54,55 which eventually could help establish correlations between non-clinical and clinical settings.
Importantly, we emphasize that, at present, evaluation of pathological response is not yet standardized, making it important to continue evaluating prognostic and predictive markers in breast cancer, especially because pCR associates with better OS in some subtypes treated with neoadjuvant chemotherapy.56,57
Conclusion
Given our results and the results of other two previously reported studies,25,26 PTP1B is overexpressed in >50% of breast cancer patients; hence, it seems that this phosphatase plays an important role in breast cancer. It is necessary to have more studies, preferably in a large cohort, evaluating its role in different aspects of breast cancer, including chemosensitization.
Author Contributions
Conceived and designed the experiments: BMB. Contributed to the biostatistical analysis: AAA. Analyzed the data: MMRF. Wrote the first draft of the manuscript: MMRF. Contributed to the writing of the manuscript: ELR. Agreed with manuscript results and conclusions: MMRF, ELR, BMB, LGVR, MdlLSG, AAA. Jointly developed the structure and arguments for the article: MMRF. Made critical revisions and approved the final version: ELR. All authors reviewed and approved the final manuscript.
Footnotes
Acknowledgments
We thank the Oncology Department for acquiring the PTP1B Antibody essential for conducting our research.
