Abstract
A 63-year-old female with a well-vascularized pulmonary metastasis of an endometrial stromal sarcoma (ESS) of 6×6 cm received selective embolization with 150–250 μm polyvinyl alcohol (Contour; Boston Scientific, Natick, MA, USA) via a bronchial artery. Post-interventional loss of perfusion was qualitatively estimated to be >80%. The lesion was located in direct proximity to the pulmonary hilar vessels. Owing to recurrent and sudden hemoptyses, an interdisciplinary tumor board assessed the risk of life-threatening blood loss to be greater than that of angiography with particle embolization and agreed on an endovascular approach. Hemoptysis did not recur in a follow-up period of six months. Initial clinical symptoms were noted 25 years ago. However, establishing a definite diagnosis has, for a long time, remained a histopathological challenge.
Keywords
Introduction
Endometrial stromal sarcomas (ESS) are rare and account for only 0.2% of all malignant uterine tumors. 1 Apart from typical local recurrences in the pelvic area, metastases of the lung are common. Reported incidences range from 7–28%. 2 Metastases of ESS (especially to the lung) may occur decades after resection of the primary tumor.1,3 In general, methods like image-guided embolization4–6 and radiofrequency ablation 7 are employed increasingly and refined 8 in managing pulmonary tumors. To our knowledge, the response of pulmonary metastases of ESS to embolization has not yet been described. A review of the existing literature provided neither a description of how to proceed, should pulmonary metastasis of an ESS induce hemoptysis, nor whether selective polyvinyl alcohol embolization may be an effective and feasible approach.
Case Report
Twenty-five years ago, our patient had undergone a hysterectomy because of an uterine leiomyoma, followed by an atypical lung resection in 1993 owing to metastases of an unknown primary. The primary was suspected to be a schwannoma, which then progressed to become a neurosarcoma. Hormone therapy with tamoxifen was discontinued in 1994. In 1998, the patient was diagnosed with multiple diffuse pulmonary lesions, most likely secondary to leiomyomatosis. In 2008, a surgical resection of the left inferior lobe of the lung was performed because of a progressive cavernous lesion. Tuberculosis was ruled out beforehand and, computerized tomography (CT)-morphologically, the lesion was enhanced after contrast medium application, indicating an intense vascular supply. The lesion was further histo-morphologically peculiar, as it was found to be an estrogen and progesterone receptor-positive spindle cell neoplasm with recent and older hemorrhagic components. Even after discussion with several universities’ pathology departments’ advisory boards, the diagnosis remained indefinite; however, a metastasis of an ESS was favored. Given the morphology, the existence of pulmonary metastases, 9 and the immune-expression profile, the differential diagnosis of a hemangioperycytoma was also considered. Yet, in a published study describing eight cases, 10 all hemangioperycytomas were estrogen receptor negative. A bilateral salpingovarectomy in 2008 revealed no signs of malignancy.
The 63-year-old female presented with recurrent, infrequent, and sudden hemoptysis of about 200 mL. A CT scan of the thorax, abdomen, and pelvis in 2009 revealed progressive metastases of up to 6×6 cm in the left lung, directly adjacent to the heart and pulmonary hilar vessels (Figure 1), as well as of up to 20 mm in diameter in the paratracheal lymph nodes in the vicinity of the pulmonary vasculature. Moreover, a lesion of 6×4 cm was detected in the sacral bone with cortical destruction and infiltration of the spinal canal (Figure 2). The CT scan depicted no hemorrhagic effusion. Given the recurrent and sudden hemoptyses and the progressive expansive character of the well-vascularized pulmonary lesion, an interdisciplinary tumor board assessed the risk of life-threatening blood loss to be greater than that of angiography with particle embolization and agreed on an endovascular approach. By then blood loss was estimated to amount to ca. 300 mL per assault and occurred about twice weekly.

A computerized tomography scan slice of the thorax illustrating a progressive metastasis in the left lung, directly adjacent to the heart and pulmonary hilar vessels (arrow).
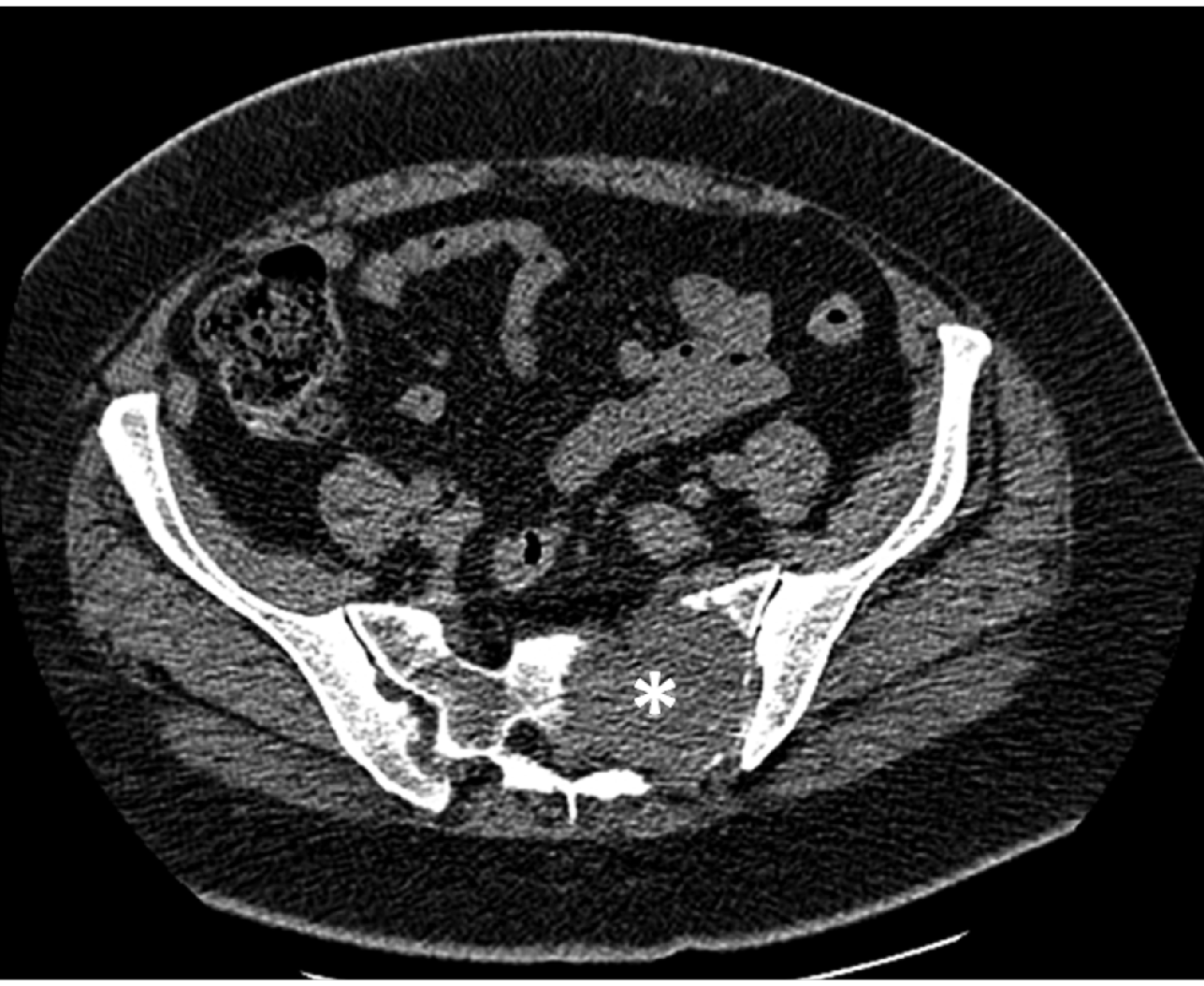
A computerized tomography scan slice of the pelvis demonstrating a lesion in the sacral bone (asterisk) with cortical destruction and infiltration of the spinal canal.
The angiography before embolization depicted a moderately hypertrophied left bronchial artery supplying the pulmonary lesion. Its branches tapered as they approached the metastasis (Figure 3A and B). They then appeared to fill a collection of abnormally dilated vessels, especially adjacent to the superior aspect of the mass. The corresponding CT (Figure 1) depicted a heterogeneous lesion of irregular vascularization, indicating distortion of the supplying pulmonary artery branches. Imaging revealed no evidence of focal aneurysm formation owing to tumor infiltration. The embolization was performed via selective placement of a 5 F SPECIAL angiographic catheter (Cordis Europe, Roden, NL). Bronchial arterial particle embolization was performed with injection of 150–250 μm polyvinyl alcohol (Contour; Boston Scientific, Natick, MA, USA). Post-interventional controls confirmed the loss of lesion perfusion to be >80% (Figure 3C and D). A super-selective microcatheter was not necessary, as the pulmonary target lesion was sufficiently targeted with the 5 F angiographic catheter. Clinical follow-up six months later revealed no recurrence of hemoptysis as well as tumor size reduction in CT scans and conventional X-rays from 6×6 cm to 4×4 cm after polyvinyl alcohol embolization (Figure 4 A and B).

(A and B) Angiograms before embolization depicting a moderately hypertrophied left bronchial artery supplying the pulmonary lesion, with tapering branches approaching the metastasis. (C and D) The post-bronchial arterial particle embolization angiograms confirm the loss of lesion perfusion.

(A and B) Conventional X-rays showing tumor size reduction after polyvinyl alcohol embolization within a six month period.
Discussion
The tumor entity of ESS is not well understood, especially concerning its development and growth. Because estrogen receptors seem to be commonly expressed, hormonal growth pathways appear to play a key role in the tumor's progression. 11 ESS can be traditionally classified into high- and low-grade, depending primarily on cytological differentiation and morphological features; and not – as often stated – on the mitotic index. 12 The 2003 WHO classification differentiates between stromal sarcomas of the endometrium, corresponding with low malignant stromal sarcomas, and undifferentiated sarcomas of the endometrium, which covers a group of highly malignant polymorph cells. 13 About 50% of all patients with low-grade ESS seem to develop recurrences, typically in the form of pulmonary and pelvic metastases. Only very few cases with skeletal involvement have been reported.1,14 Cases with the primary diagnosis of ESS in extra-uterine locations such as the vulva, vagina, ovaries, abdominal cavity, and retroperitoneal space are very rare. 15 ESS is often associated with endometriosis and/or hyperestrogenism. Endogenous hyperestrogenism may be induced either locally by endometriotic tissue, or systemically by pregnancy or polycystic ovarian syndrome. Exogenous hyperestrogenism can occur as a side-effect of ovulation-stimulating drugs. Endometriosis has been proposed as a precursor of low-grade ESS, thus offering an explanation for extra-uterine primary or secondary tumors.15,16
Multiple well-demarcated lesions with entrapped air surrounded by non-neoplastic respiratory epithelium are characteristic of the most common morphological pattern of pulmonary ESS metastases. 2 Several unusual morphological patterns exist including solitary lesions with infiltrative margins, lymphangitic, cystic, or even micronodular 17 morphology. These aspects may impede a correct diagnosis, sometimes mimicking lymphangioleiomyomatosis, for example. In our case, the pathology department was able to exclude lymphangioleiomyomatosis as a possible differential diagnosis. Furthermore, the pathologists excluded a pulmonary origin of the assessed lung lesions.
Owing to an arboreal vasculature and an undifferentiated appearance of the tumor cells, endometrial stromal sarcomas are easily mistaken for several other soft-tissue neoplasms. 10 Unfortunately, misdiagnosis as a benign uterine tumor is not uncommon in patients with ESS. 3 However, compared to other possible differential diagnoses with “cannonball” pulmonary metastasis, a patient with ESS may have a more favorable prognosis. 18
Conclusions
In a well-vascularized pulmonary metastasis of an ESS, selective embolization with polyvinyl alcohol via a bronchial artery is an effective and feasible approach to reduce perfusion of the lesion and thus the risk of critical blood loss. To date (six months after embolization), neither has there been a recurrence of hemoptysis nor has a further embolization, including percutaneous radiofrequency ablation and/or radiation after embolization, been necessary in our patient.
