Abstract
For islet transplantation, maintaining organ viability after pancreas procurement is critically important for optimal graft function and survival. We recently reported that islet yield was significantly higher in the modified ET-Kyoto (MK) solution, which includes a trypsin inhibitor (ulinastatin), compared with the UW solution, and that the advantages of MK solution are trypsin inhibition and less collagenase inhibition. In this study, we compared ulinastatin with other trypsin inhibitors, gabexate mesilate, and nafamostat mesilate, in preservation solution for islet isolation. Ulinastatin was easily dissolved in ET-Kyoto solution, while ET-Kyoto with gabexate mesilate and nafamostat mesilate became cloudy immediately after addition. Although there were no significant differences in islet yield among the three groups, viability was significantly higher for the MK group than for the GK group or the NK group. The stimulation index was significantly higher for the MK group than for the GK group. In summary, there are no other trypsin inhibitors that are more effective than ulinastatin. Based on these data, we now use ET-Kyoto solution with ulinastatin for clinical islet transplantation.
Keywords
Introduction
The solution for organ preservation is critically important for maintaining its function, reducing ischemia-reperfusion injury, and, therefore, increasing transplant efficiency. For islet transplantation, the storage conditions of the donor pancreas may influence the deleterious consequences of isolated islets during transplantation, which remains a major source of current issues in clinical practice. Donor pancreata for islet transplantation are usually preserved with University of Wisconsin (UW) solution. However, UW solution has several disadvantages: it is chemically unstable, it must be cold stored until use, and its short shelf life makes it expensive. It is also highly viscous, which may complicate the initial organ flush (30). Extracellular-type trehalose-containing Kyoto (ET-Kyoto) solution was recently developed for organ preservation solution and its effectiveness in cold lung storage has been demonstrated in clinical lung transplantation (4,23). It also is effective for skin flap storage and its clinical application is beginning in this field (31).
We previously showed that pancreas preservation with modified ET-Kyoto (MK) solution significantly improved islet yields, compared with UW preservation (21). Although high potassium in UW solution causes insulin release from pancreatic β-cells (6), ET-Kyoto solution has a high sodium/low potassium composition. Moreover, UW solution inhibits the activity of collagenase, an enzyme blend for pancreatic digestion (5,27), but MK solution inhibits collagenase to a lesser extent (21). MK solution includes a trypsin inhibitor (ulinastatin), which is one of the advantages of this solution. Indeed, pancreas preservation using MK solution was superior to that using ET-Kyoto solution without the trypsin inhibitor in a rat model (21).
In this study, we compared ulinastatin with other trypsin inhibitors (gabexate mesilate, and nafamostat mesilate) in preservation solution for islet isolation.
Materials and Methods
Preservation Solution
We used ET-Kyoto solution (4,23) with ulinastatin (Miraclid®, Mochida Pharmaceutical, Tokyo, Japan; named MK solution), gabexate mesilate (FOY®, Ono Pharmaceutical, Osaka, Japan; named GK solution), and nafamostat mesilate (FUTHAN®, Torii Pharmaceutical, Tokyo, Japan; named NK solution). The components of the solutions are shown in Table 1.
Composition Preservation Solutions

Measurement of Trypsin Inhibition Ability of Solutions
In order to assess the trypsin inhibition of MK, GK, and NK solutions and ET-Kyoto solution without trypsin inhibitors (control), 3 ml of 0.3 mM N-benzoyl-l-arginine ethylester reagent (BAEE; Sigma, Tokyo, Japan) was incubated for 5 min at 25°C and then 5 μl of 1 mg/ml trypsin and 45 μl of each solution were added. Trypsin activity was measured by absorption spectrophotometry (λ253 nm) using BAEE for the trypsin substrate, according to a previous report (12). Absorbance was measured at every minute up to 6 min. A BAEE unit was defined as a change in optical density of 0.001/min.
Porcine Islet Isolation
Porcine pancreata were obtained at a local slaughterhouse. About 10 min after the cessation of heart beating, the operation was started. After removing the pancreas, we immediately inserted a cannula into the main pancreatic duct, infused each preservation solution for ductal protection (9,20), and put the pancreas into each two-layer [preservation solution/perfluorochemical (PFC)] preservation container. Operation time was defined as the time elapsed between the start of operation and removal of the pancreas. Warm ischemic time (WIT) was defined as the time elapsed between cessation of heart beating and placement of the pancreas into the preservation solution. Cold ischemic time (CIT) was defined as the time elapsed between placement of the pancreas into the preservation solution and the start of islet isolation.
Islet isolation was conducted as previously described (9,10,15,22) in the standard Ricordi technique (26) with modifications introduced in the Edmonton protocol (11,24,28). In brief, after decontamination of the pancreas, the ducts were perfused in a controlled fashion with a cold enzyme blend of Liberase HI (1.4 mg/ml; Roche Molecular Biochemicals, Indianapolis, IN). The distended pancreas was then cut into 7–9 pieces, placed in a Ricordi chamber, and shaken gently. While the pancreas was being digested by recirculating the enzyme solution through the Ricordi chamber at 37°C, we monitored the extent of digestion with dithizone staining by taking small samples from the system. Once digestion was confirmed to be complete, RPMI-1640 medium (Gibco, Carlsbad, CA) was introduced into the system. Then the system was cooled to stop further digestive activity. The digested tissue was collected and washed with fresh medium to remove the enzyme. The phase I period was defined as the time between placement of the pancreas in the Ricordi chamber and the start of collecting the digested pancreas. The phase II period was defined as the time between the start and end of collection.
Islets were purified with a continuous density gradient with iodixanol (Optiprep®, Sigma-Aldrich, St. Louis, MO)-Kyoto (IK) solution in an apheresis system (COBE 2991 Cell Processor, Gambro Laboratories, Denver, CO). Since iodixanol has low viscosity, it needs less force during centrifugation, compared with Ficoll. For the solution, low-density (density 1.077) and high-density (density 1.100–1.125) IK solutions were produced by changing the volumetric ratio of iodixanol and Kyoto solution (9,14,15).
Islet Evaluation
The crude number of islets in each diameter class was determined by counting islets after dithizone staining (3 mg/ml, final concentration) (Sigma Chemical Co., St. Louis, MO) using an optical graticule. The crude number of islets was then converted to the standard number of islet equivalents (IEQ; diameter standardizing to 150 μm) (25). Gross morphology was qualitatively assessed by two independent investigators scoring the islets for shape (flat vs. spherical), border (irregular vs. well-rounded), integrity (fragmented vs. solid/compact), uniformity of staining (not uniform vs. perfectly uniform), and diameter (least desirable: all cells <100 μm/most desirable: more than 10% of the cells >200 μm) (11,25). Each parameter was graded from zero to 2 with zero equaling the worst and 2 the best score, so that the worst islet preparations were given a cumulative score of zero and the best a score of 10. Spherical, well-rounded, solid/compact, uniformly stained, and large islets were characterized as the best islets.
Islet viability after purification was assessed using acridine orange (10 μmol/L) and propidium iodide (15 μmol/L) (AO/PI) staining to visualize living and dead islet cells simultaneously (3,11,25). Fifty islets were inspected and their individual viability was determined visually, followed by calculation of their average viability (11).
In Vitro Assessment of Islet Function
Islet function was assessed by monitoring the insulin secretory response of the purified islets during glucose stimulation according to a procedure described by Shapiro and colleagues (28). Briefly, 1,200 IEQ were incubated with either 2.8 or 25 mM glucose in RPMI-1640 for 2 h at 37°C and 5% CO2. The supernatant was collected and insulin levels were determined using a commercially available enzyme-linked immunosorbent assay (ELISA) kit (ALPCO Insulin ELISA kit; ALPCO Diagnostics, Windham, NH). The stimulation index was calculated by determining the ratio of insulin released from islets in high glucose concentration to the insulin released in a low concentration. The data were normalized by total proteins from the cell lysate. All assessments were made in triplicate and the data (mean ± SE) were expressed as a percentage of the control values in each experiment to eliminate variables caused by differences among donor pancreata.
Recently, Goto et al. showed that the measurement of the adenosine diphosphate/adenosine triphosphate (ADP/ATP) ratio correlated with transplantation outcome (7). The ADP/ATP ratio was measured to evaluate the energy status of cultured islets, using the ApoGlow™ kit (Cambrex Bio Science Nottingham Ltd., Nottingham, UK). In brief, 80 IEQ of islets were washed in PBS and then mixed with 100 μl of nucleotide releasing reagent for 10 min at room temperature. Thereafter, 20 μl of nucleotide monitoring reagent was added to the solution, and the ATP levels were measured using a luminometer (FB 12 Luminometer, Berthold Detection Systems GmbH, Pforzheim, Germany) and expressed as the number of relative light units (RLU). After 10 min, the ADP in the solution was converted to ATP by adding 20 μl ADP converting reagent and then measured as the number of RLU. Subsequently, the ADP/ATP ratio of the islets was calculated.
In Vivo Assessment of Islet Function
Severe combined immunodeficient mice (SCID; CLEA Japan, Inc., Meguro, Tokyo) were used for the experiments. The recipients were rendered diabetic by a single injection of streptozotocin (STZ) at a dose of 220 mg/kg. Hyperglycemia was defined as a glucose level of >350 mg/dl detected twice consecutively after STZ injection. The 2,000 IEQ pig islets obtained from each group were transplanted into the renal subcapsular space of the left kidney of a diabetic SCID mice as previously described (16,17,20). During the 30-day posttransplantation period, the nonfasting blood glucose levels were monitored three times per week. Normoglycemia was defined when two consecutive blood glucose level measurements showed less than 200 mg/dl. No statistical differences in either pretransplantation blood glucose levels or pretransplantation body weight were observed among the three groups of mice. Mouse studies were approved by the Institutional Animal Research Committees of Kyoto University and Fujita Health University.
Statistics
The differences between each group were considered significant if the value was p < 0.05 using an unpaired Student's t-test with Bonferroni correction or the Kaplan-Meier log-rank test.
Results
Dissolution of Trypsin Inhibitors in ET-Kyoto Solution
Ulinastatin, gabexate mesilate, and nafamostat mesilate were used in this study. When these trypsin inhibitors were added in ET-Kyoto solution, ulinastatin was easily dissolved in ET-Kyoto solution, while ET-Kyoto with gabexate mesilate and nafamostat mesilate became cloudy immediately after addition (Fig. 1A). After 30 min, gabexate mesilate and nafamostat mesilate were dissolved in ET-Kyoto solution.

Dissolution of trypsin inhibitors in ET-Kyoto solution. (A) Extracellular-type trehalose-containing Kyoto (ET-Kyoto) with gabexate mesilate (GK) and nafamostat mesilate (NK) became cloudy immediately after addition. (B) Impact of MK (Kyoto with ulinastatin), GK, or NK solution on trypsin activity. N-benzoyl-l-arginine ethylester reagent (BAEE) was incubated for 5 min at 25°C and then trypsin along with MK solution (n = 5), GK solution (n = 5), NK solution (n = 5), or ET-Kyoto (control; n = 5) was added. Trypsin activity was measured by absorption spectrophotometry (λ253 nm) using BAEE reagent. Absorbance was measured every minute for 6 min. A BAEE unit was defined as a change in optical density of 0.001/min. Data are expressed as the mean ± SE. PFC, perfluorochemical.
Inhibition of Trypsin Activity
Previous reports show that trypsin inhibition with TLM preservation improves islet yields (12,21). We examined whether MK, GK, and NK solutions inhibited trypsin activity. All three solutions significantly inhibited trypsin activity (Fig. 1B), compared with ET-Kyoto (control). These observations suggest that these solutions could reduce trypsin activity during pancreas preservation.
Porcine Islet Isolation Characteristics
The characteristics of porcine islet isolation protocols are shown in Table 2. There were no significant differences in pancreas size, operation time, WIT, or CIT among the three groups. Phase I and phase II periods were also similar for the three groups.
Pig Islet Isolation Characteristics

Data are expressed as mean ± SE. PFC, perfluorochemical.
Islet recovery (%) = IEQ after purification/IEQ before purification × 100.
Viability was higher for the MK/PFC group than for the GK/PFC group or the NK/PFC group (p < 0.01).
Stimulation index was higher for the MK/PFC group than for the GK/PFC group (p < 0.025).
Islet yield before purification was higher, but not significantly so, in the MK group (n = 9), compared with the GK group (n = 3) or NK group (n = 3) (MK: 9063 ± 640 IEQ/g, GK: 8378 ± 642 IEQ/g, NK: 6058 ± 2116 IEQ/g) (Fig. 2A). Islet yield after purification was higher, but not significantly so, in the MK group, compared with the NK group. There were no significant differences between the MK group and the GK group (MK: 6864 ± 727 IEQ/g, GK: 6967 ± 439 IEQ/g, NK: 5645 ± 2268 IEQ/g) (Fig. 2B). Other porcine islet characteristics are shown in Table 2. Viability was significantly higher for the MK group than for the GK group or the NK group (p < 0.01). The stimulation index was significantly higher for the MK group than for the GK group (p < 0.025). There were no other significantly different characteristics among each group.

Islet yield before purification (A) and after purification (B). Data are expressed as the mean ± SE. IE, islet equivalents.
Assessment of Islet Function In Vitro and In Vivo
To assess the islet graft function of each group in vitro, the ADP/ATP ratio was measured. There was no significant difference in ADP/ATP ratio between each group (data not shown). To assess the islet graft function of each group in vivo, 2,000 IEQ islets of each group were then transplanted below the kidney capsule of STZ-induced diabetic SCID mice. The blood glucose levels of 8 of the 10 mice (80.0%) receiving islets of the MK group, 7 of the 9 mice (77.8%) of the GK group, and 7 of the 10 mice (70.0%) of the NK group decreased gradually and reached normoglycemia. There was no significant difference between the groups with respect to the attainability of posttransplantation normoglycemia (Fig. 3). Morphologic studies showed the presence of islets under the kidney capsule of all SCID mice 30 days after transplantation. The islet grafts of each group in the normoglycemic mice showed intense insulin staining (data not shown).
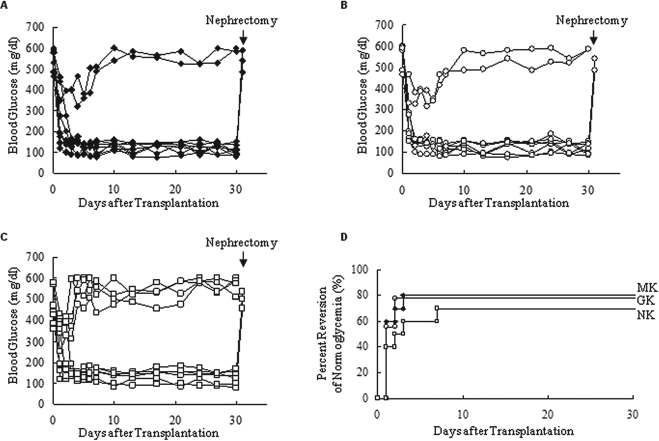
Evaluation of islet quality of each group in vivo. 2,000 IEQ islets of each group were then transplanted below the kidney capsule of streptozotocin (STZ)-induced diabetic severe combined immunodeficient (SCID) mice. (A–C) Nonfasting blood glucose levels of mice that were transplanted with islets of MK group (A), of GK group (B), or NK group (C). (D) Percentage of normoglycemia of STZ-induced diabetic mice after islet transplantation. Normoglycemia was defined as two consecutive posttransplant blood glucose levels showing less than 200 mg/dl. MK, n = 10; GK, n = 9; NK, n = 10.
In summary, there are no other trypsin inhibitors more effective than ulinastatin.
Discussion
In this study, we showed that MK solution was superior to GK or NK solutions, although the trypsin inhibition is greater in GK and NK than in MK. It may be due to differences of inhibitory effects of cytokines. Ulinastatin has been shown to inhibit not only trypsin activity but also the release of neutrophil elastase. It also down-regulates transcription of TNF mRNA, the activation of endothelial cells, and the expression of ICAM-1 induced by endotoxin in vitro (1,2,13). It has been shown that administration of ulinastatin decreased the ischemia-reperfusion injury (29) or attenuated the elevation in the concentrations of inflammatory cytokines and C-reactive protein, a marker of inflammation (32) in transplanted small intestine. The superiority of ulinastatin may also be due to less collagenase inhibition than other trypsin inhibitors. We previously reported that MK solution was superior to modified Celsior solution (Celsior solution with hydroxyethyl starch and nafamostat mesilate; HNC). HNC solution including nafamostat mesilate inhibited collagenase activity (18). Although different preservation solutions were used in the report, it seems that collagenase inhibition by nafamostat mesilate is higher than ulinasatatin.
Previously, we demonstrated that MK preservation including ulinastatin eliminated trypsin activity during pancreas preservation and ET-Kyoto preservation without ulinastatin resulted in lower islet yields (21). We also reported that ET-Kyoto with ulinastatin was the better combination for pancreas preservation than ET-Kyoto with Pefabloc (19). Other studies have shown that trypsin inhibition during human pancreas digestion improves islet yield (8,12). Since trypsin from pancreatic acinar cells destroys islets and ductal cells, trypsin inhibition could reduce degradation of the ductules and secure the delivery of collagenase solution to the immediate vicinity of the islets.
In conclusion, we showed that ET-Kyoto with ulinastatin was the best combination for pancreas preservation. Based on these data, we now use the ET-Kyoto solution with ulinastatin for clinical islet transplantation from brain-dead donor pancreata in US and non-heart-beating donor pancreata in Japan. MK preservation makes it feasible to use marginal donors for efficient islet transplantation into type 1 diabetes patients.
Footnotes
Acknowledgments
The authors wish to thank Mr. Yusuke Nakai (Kyoto University) and Ms. Yoshiko Tamura and Mr. Greg Olsen (Baylor Research Institute) for technical advice, Dr. Carson Harrod for his careful reading and editing of this manuscript, and Ms. Maki Watanabe (Fujita Health University) for assistance. This work was supported in part by the Juvenile Diabetes Research Foundation International (JDRFI); Otsuka Pharmaceutical Factory, Inc.; and the All Saints Health Foundation. The authors declare no conflict of interest.
