Abstract
Virtual reality (VR) is an innovative technology with the potential to enhance treatment for children with chronic pain and functional symptoms. Currently, little is known about patients’ experiences of VR in the setting of intensive interdisciplinary pain treatment (IIPT). This study aimed to better understand how patients engage with and benefit from VR. This case report focuses on a 12-year-old female with amplified musculoskeletal pain syndrome and comorbid functional neurological disorder receiving treatment in inpatient IIPT. VR was incorporated into physical/occupational and recreational therapy sessions. A semi-structured interview was completed one-month post-discharge. Qualitative analysis revealed three major themes: Process of Change (VR was unique/immersive, reduced pain focus, challenged skepticism, and changed pain perception), Efficacy (VR increased movement, supported transitioning from a wheelchair to walking independently, and increased confidence, excitement, and surprise), and Engagement (VR aided in acknowledging progress, increased camaraderie, was fun, and challenged patient to extend treatment goals made in VR to real life). Therapist observations of the benefits and barriers to using VR in treatment are described. Overall, this report indicates that VR may be a helpful tool to use with existing IIPT interventions to enhance patient engagement in treatment and improve functionaloutcomes.
Keywords
Introduction
Adequate management of pediatric pain remains highly challenging, poorly understood, and significantly undertreated [1]. Inadequate management of pain is associated with poor quality of life, economic burden, and a high risk of persistent pain and opioid misuse in adulthood [2–4]. Additionally, a growing number of pediatric patients with chronic pain have comorbid functional neurological disorder (FND) 1 , further complicating treatment and leading to poor outcomes [5].
The treatment of pediatric chronic pain has evolved significantly over the last 30 years, shifting from a focus on pharmacologic to non-pharmacologic and non-opioid therapy as first-line treatments [4, 6]. Similarly, the understanding of FND has shifted from being regarded as a diagnosis of exclusion without many treatment options to a diagnosis with positive symptoms and emerging behavioral treatments [7]. In particular, the last several years have seen an emergence in the use of non-pharmacologic digital health tools, particularly in managing chronic pain and functional symptoms [8, 9].
Virtual reality (VR) is one such technology that has the potential to enhance management of pediatric pain and functional symptoms [8–10]. VR provides an immersive, multisensory, three-dimensional environment that allows participants to have a modified experience of reality by creating a sense of “presence” in which the patient feels that they are physically in the virtual world [11]. Research has found VR modulates pain-signaling through distraction, helping patients to shift focus and build skills while enhancing their sense of control [12]. Mechanistically, VR is thought to compete with pain signaling pathways and aid in reorganizing neural networks, resulting in improved functioning [13, 14]. However, a full understanding of the mechanism for the efficacy of VR is not yet completely elucidated. Nevertheless, the use of VR in pediatric patients with chronic pain and functional symptoms may be particularly beneficial, as children and adolescents typically have experience using this technology and are open to participating in engaging and imaginative experiences [15].
While VR is an innovative technology with the potential to enhance treatment for pediatric patients with chronic pain and functional symptoms, little is known about patients’ actual experiences using VR in intensive interdisciplinary pain treatment (IIPT). These programs aim to normalize patients’ activity to premorbid levels of function while increasing self-management through coordinated and concurrent treatment from specialists in pain and rehabilitation medicine, behavioral psychology, and physical therapy (PT), recreational therapy (RT), and occupational therapy (OT). IIPT programs treat patients with the highest levels of pain and disability who have failed treatment at other levels of care (e.g., inpatient, outpatient); innovative and engaging treatment tools are especially needed to restore function for those with such severe impairment. The current study utilized qualitative analysis of a case report to identify themes related to the experience of using VR as a first step to better understand how pediatric patients can engage with and benefit from VR during IIPT.
Methods
Patient description
A 12-year-old female with a long history of amplified musculoskeletal pain syndrome and comorbid FND presented with pain in her left shoulder, elbow, wrist, and right knee. The pain began when she was five years old and was exacerbated by a shoulder and knee injury in the past year, resulting in increased pain as well as functional limb paralysis and weakness. As a result, she became functionally debilitated and required a wheelchair for mobility. She described her pain as constant and made worse by even the slightest movement of her extremities. Her pain and disability were in the severe range (e.g., ratings of average pain of 6.8 on a 0–10 visual analog scale; ratings of >30 on the Functional Disability Inventory [FDI] indicating severe disability; Figure 1A and 1B), impacting functional ability, activities of daily living, school attendance, physical functioning, social interaction, and emotional adaptation. Physical and occupational therapists observed impairments in the following areas: mobility, strength, balance, range of motion, gross motor skills, fine motor coordination, activity demand tolerance, gait deviation, abnormal positioning, stair negotiation, and activity tolerance. Her pain (average intensity of 3 out of 10; Figure 1A) and disability (FDI score of 10; Figure 1B) demonstrated significant reductions at discharge and two follow-up periods (six and 12 months).
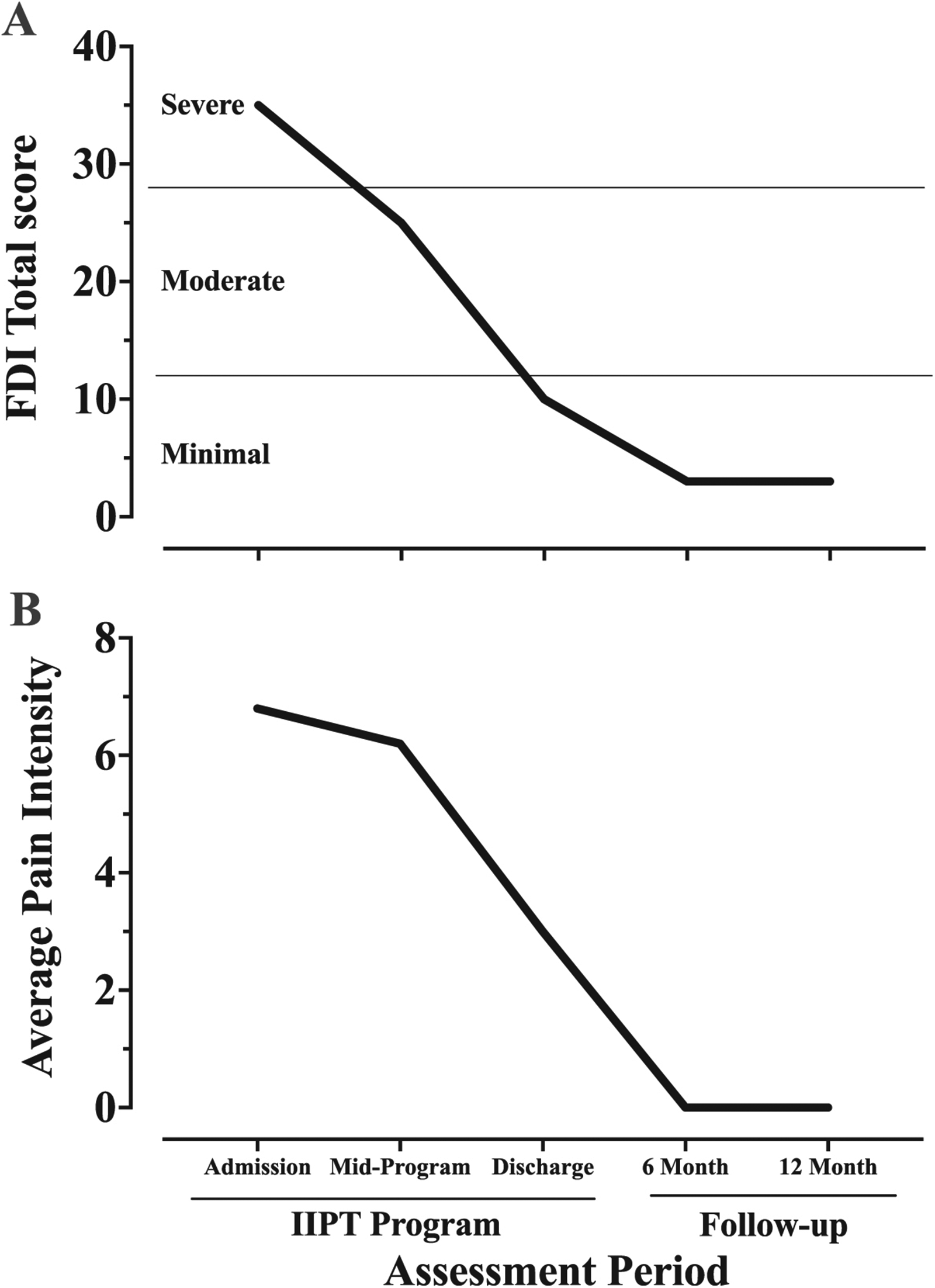
Reporting of (A) disability on the Functional Disability Inventory (FDI) and (B) average pain intensity during and following inpatient intensive interdisciplinary pain treatment.
The patient was admitted to an inpatient IIPT program for six weeks [16]. Briefly, she received three hours of individual OT and PT daily and two hours of group-based RT weekly among other program treatments (see Williams et al. [16] for a detailed program description and outcomes).
Integration of VR into clinical care
VR was incorporated into OT/PT once a week during a 45-minunte individual session and once a week during a one-hour group session in RT, for a total of five PT/OT sessions and five RT sessions. Off-the-shelf games, including Tilt Brush (Google), Beat Saber (Beat Games), and Fruit Ninja (Halfbrick Studios), were delivered by an HTC Vive Pro HMD. The use of VR was tailored to the goals of the individual therapy sessions.
OT: VR was used to help the patient achieve OT-related goals, including activity tolerance/functional endurance, grip strengthening, active reaching and range of motion, dynamic balance, activity in stance, functional mobility, and desensitization. Specific games used to work toward those goals included Tilt Brush (reaching, grip, coping, changing positions), Beat Saber (coordination, mobility, balance, speed), and Fruit Ninja (standing, endurance, coordination).
PT: VR was used as an enhancement to traditional PT treatment options, both as an incentive and for skill building. Specifically, VR games provided a highly engaging distraction during bilateral lower extremity weight bearing in stance/sitting or range of motion activities. Functional positions and movements were practiced in the unique VR environments to improve acceptance of these in everyday life. The patient also enjoyed playing VR games as a reward after accomplishing specific goals as a fun/enjoyable treatment option.
RT: The patient used VR during a therapist-facilitated one-hour group session with one to two other IIPT program patients. While one patient used the VR headset, the others watched their performance on the screen. Patients either worked on a collaborative art project (Tilt Brush) that engaged them physically and creatively or competed against each other in games (Beat Saber, Fruit Ninja).
Data collection and analysis
A doctoral-level psychologist (KLK), who was not involved in the patient’s care, completed a semi-structured interview around a series of prompts with the patient one month after discharge from the program; this was the only time point when she was interviewed about her VR experience (see Table 1). The interview was transcribed and checked against the audio recording for accuracy. The transcript of the interview was coded to identify themes related to the patient’s experience with VR. Two doctoral psychologists (SLC, KJH) separately coded the interview and then met to discuss discrepancies, identify code labels, and collapse codes as warranted. In total, 144 patient sentences/phrases were coded into 14 categories. Code mapping using multidimensional scaling was conducted with MAXQDA 2022 (VERBI Software, 2021) to identify overarching themes based on how the codes clustered (Figure 2). Occupational, physical, and recreational therapists (NDS, ETD, KS) also provided their observations of the clinical benefits and potential barriers to using VR in their respective treatment. This study was approved by the Institutional Review Board; the patient provided verbal assent, and her parents provided written informed consent.
Interview prompts for VR case study in IIPT.

Interview prompts for VR case study in IIPT.

VR: virtual reality; IIPT: intensive interdisciplinary pain treatment; OT: occupational therapy; PT: physical therapy; Rec: recreational.
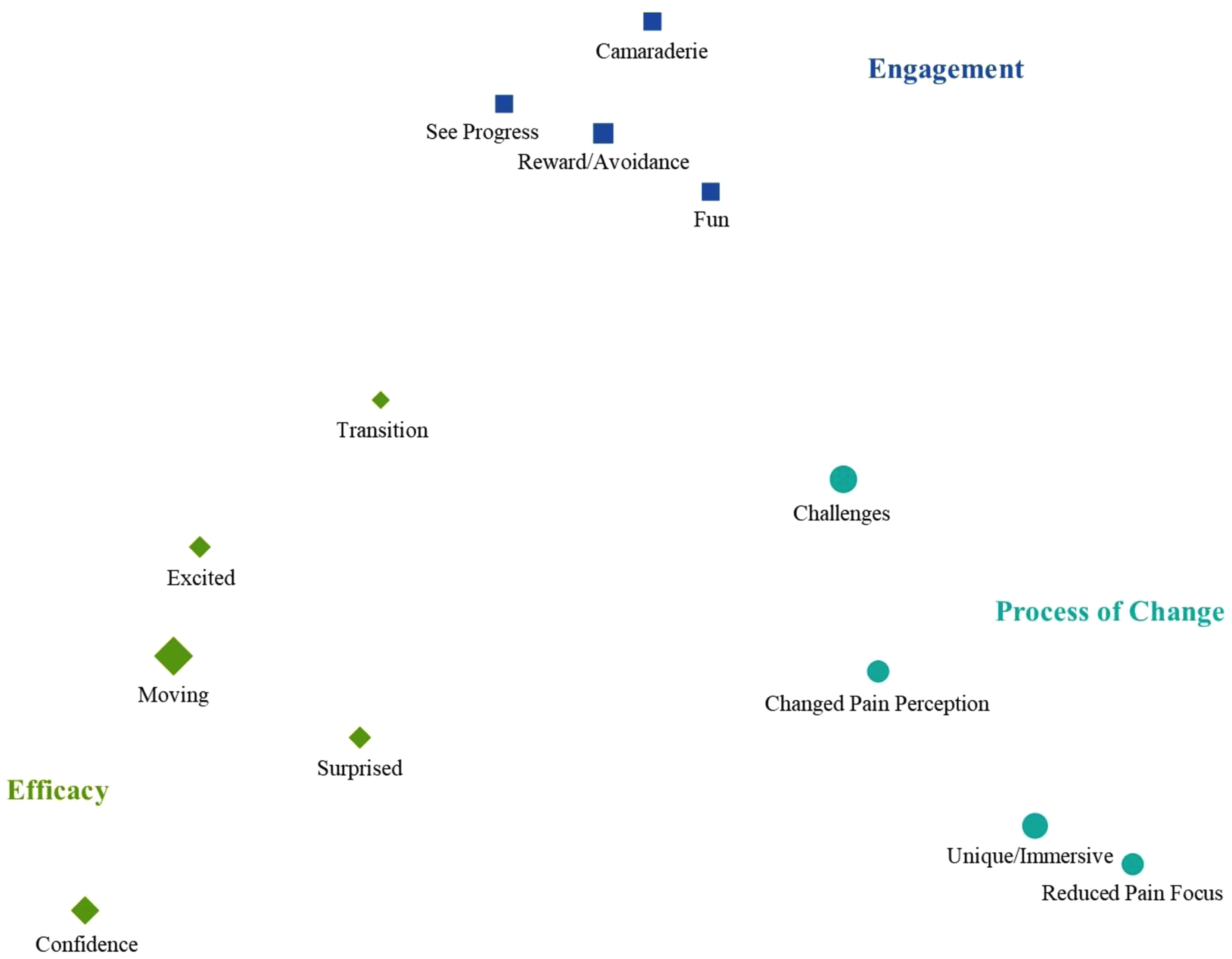
Code mapping using multidimensional scaling was conducted with MAXQDA 2022 (VERBI Software, 2021) to identify overarching themes based on how the codes clustered.
Patient’s experience
Three overarching themes were identified: Process of Change, Efficacy, and Engagement, along with the stand-alone code Safe.
Process of Change included four codes. Unique/Immersive captured the patient’s experience of engaging in VR. Reduced Pain Focus included descriptions of being distracted and highly engaged. Challenges captured the patient’s report of being skeptical of VR and feeling like the coping strategies she tried in the past “didn’t work” for her as well as VR worked during IIPT. Changed Pain Perception included statements about how thinking about pain changed during VR. Taken together, these codes capture the presumed mechanism of change for the patient –an immersive experience that helped to redirect attention away from pain and ultimately led to changed pain perception with an increase in functioning, including her unique challenges along the way.
Efficacy included five codes. Moving was the largest code category and focused on the patient’s report of beginning to move, increasing her movement, and meeting program and personal goals. The Transition code captured her progress in movement, increasingly requiring fewer supports and walking independently. The codes of Confidence, Surprised, and Excited, captured the patient’s experience of being surprised by the VR experience and that it “worked,” along with her increased feelings of confidence and success associated with this excitement.
Finally, Engagement included four codes: See Progress, Camaraderie, Fun, and Reward/Avoidance. The first three code titles are self-explanatory and included the patient’s ability to see progress throughout VR activities, social interaction with other patients, and enjoyment of VR, respectively. The Reward/Avoidance code captured the patient’s dilemma with the fact that, while VR helped her to walk for the first time in a year, it now meant that she would be expected to walk in settings outside of VR as well.
The code Safe did not share relationships with any other codes. It captured that the patient felt safe taking risks during VR sessions and was supported by the intervention team.
A summary of codes and themes with representative quotes is presented in Table 2. The visual spacing of the codes is presented in Figure 2. Overall, the patient described the VR intervention as a very positive, helpful tool that facilitated her recovery from a high level of impairment to complete functional restoration over the course of her IIPT program. As she noted at the end of the interview: “If I do ever end up having to go back to the FIRST program, I’m gonna be like ‘VR right now’ it fixed me the last time…I feel like it’s a really good and valuable tool.”
Themes, codes, and representative quotes from the qualitative analysis.
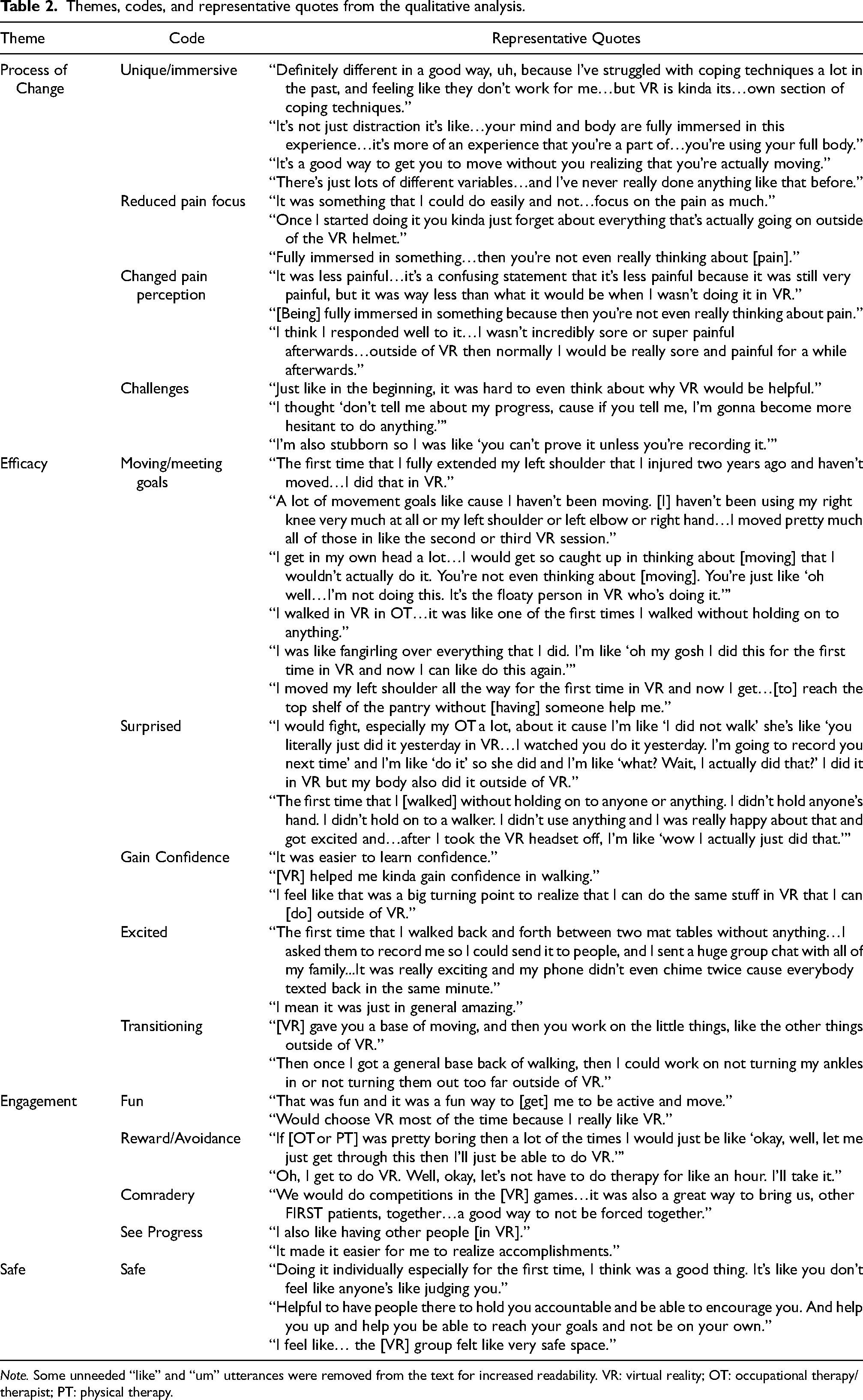
Themes, codes, and representative quotes from the qualitative analysis.

Note. Some unneeded “like” and “um” utterances were removed from the text for increased readability. VR: virtual reality; OT: occupational therapy/therapist; PT: physical therapy.
The RT, OT, and PT therapists agreed that incorporating VR facilitated significant functional improvements for this patient (see Table 3). Specifically, therapists noted that she progressed in active range of motion in bilateral upper extremities, stood for longer periods, initiated steps without walker support, improved grasp, and exhibited decreased pain behaviors more successfully during activities in VR compared to non-VR sessions. Table 4 presents a summary of the clinical lessons (challenges and solutions) learned from the therapy team regarding incorporating VR into treatment for this individual patient.
Clinical observations regarding use of VR in rehabilitation.

Clinical observations regarding use of VR in rehabilitation.

VR: virtual reality; IIPT: intensive interdisciplinary pain treatment.
Lessons learned about challenges and solutions to incorporating VR into a pain rehabilitation treatment.
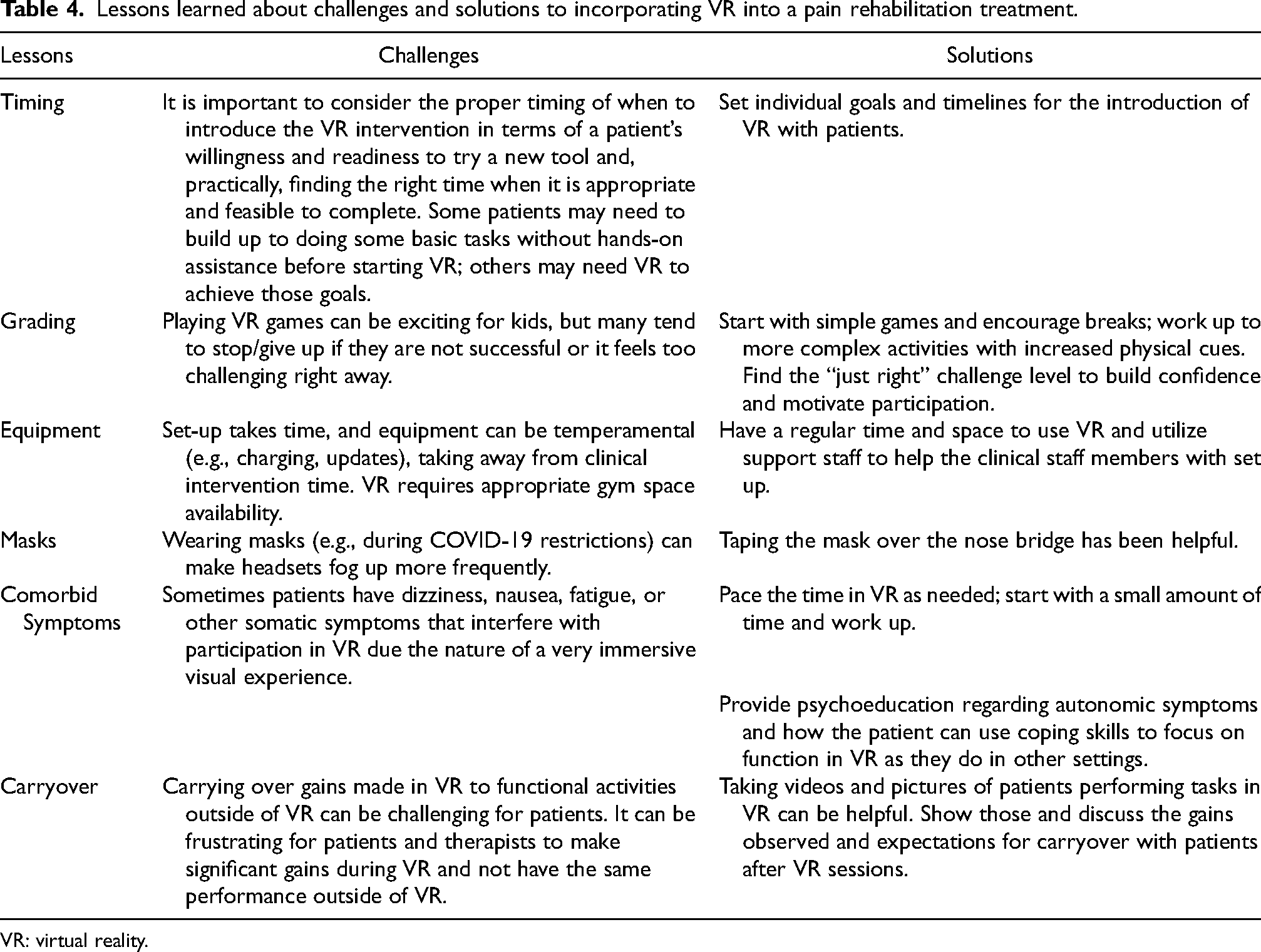
VR: virtual reality.
This qualitative analysis of a case report demonstrated the positive benefits of incorporating VR into the treatment of a pediatric patient with chronic pain and comorbid FND, complementing previous studies using VR in pediatric pain patients [9, 10]. Specifically, three major themes were identified, including the unique impact of VR on the process of change to decrease attention to pain and improve function, how VR helped the treatment itself be more effective, and the high degree of engagement she experienced using VR. Similar themes were observed by Griffin and colleagues [9], who reported positive experiences (e.g., enjoyment), distraction from pain, decreases in pain, and increased function with VR by patients. Furthermore, patients reported not initially enjoying or believing that VR would be helpful (similar to Challenges in the theme Process of Change), but they were willing to give VR a try. In addition, therapists agreed that including VR was a successful and fun way to enhance traditional therapies and facilitate significant physical and psychosocial improvement for this patient. These responses were comparable to clinician interviews by Griffin and colleagues [9], suggesting that VR helped patients achieve their rehabilitation goals, reduced pain, and increased function while overcoming psychological barriers to rehabilitation.
Although VR appeared to play a strong role in assisting with this patient’s functional recovery, it is important to appreciate other factors that may have influenced her improvement. It is possible that this patient’s positive experience was impacted by the treatment setting in which she received VR intervention. Two cornerstones of IIPT are the coordinated team approach and intensity of therapies, both of which likely contribute to the observed faster responses to IIPT vs. outpatient treatment among highly impaired patients with chronic pain [17]. In this case report, both the patient and therapists noted times when team communication and carryover to the next session was critical, particularly when a new movement first happened in VR. This team’s communication and interdisciplinary environment likely contributed to the rapid improvement observed for this patient. While it is likely that similar successful outcomes could be achieved by incorporating VR into pain treatment conducted in other settings (e.g., outpatient), it is possible that the number of sessions or timeline of recovery could similarly vary. Additionally, the lessons learned by the clinical staff (as mentioned in Table 4) may be used for consideration when working with other patients and may provide a launch point for future researchers, although they may not be applicable with every patient or in every situation. Finally, in terms of limitations with the current case study, no information (e.g., open-ended questions, immersiveness) was collected after each VR session that could have provided insight into the progression of these themes (e.g., themes may become more positive with more exposure) or factors contributing to the positive impact of VR (e.g., more positive with more immersiveness). Measurement of pain, immersiveness (e.g., Child Presence Questionnaire [18]), and post-VR session interviews of patients and providers should be considered.
In summary, this case report highlights the versatility of VR as a tool that providers from various disciplines can successfully incorporate into treatment. Notably, each discipline used the same tool differently to improve function and target different goals across individual and group sessions. Future studies incorporating VR into pain treatment would benefit from a greater focus on the clinical decision-making surrounding the choice of when to use VR, patient characteristics that impact outcomes, and utilization in other treatment settings. More rigorous trials are needed, especially trials integrating insights from both patients and clinicians during the design of VR-based interventions for pain rehabilitation. These trials will allow for the evaluation of the added value of VR in pain treatment while providing an understanding of the mechanisms underlying how VR effectively reduces pain and enhances function (see review by Logan and colleagues on VR-based school simulation [10]). For example, one potential trial would randomize patients to receive VR content in a graded, goal-based manner (e.g., starting with simple physical challenges in VR and gradually adjusting difficulty, as outlined in Table 3). Alternatively, patients might receive external feedback through three-dimensional movement capture during the VR session (e.g., see an avatar or representation of themselves moving in sync with their actual movements). To conclude, further investigation is warranted to determine the optimal approach for integrating these strategies into effective pain rehabilitation using virtual reality.
Footnotes
Acknowledgments
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors. The FIRST program received funding from the Junior Co-operative Society of Cincinnati Children’s Hospital Medical Center for the purchase of the VR equipment.
Declaration of interest
Authors have no financial relationships relevant to this article to disclose and no potential conflicts of interest.
