Abstract
PURPOSE:
This article provides an update to the 2018 Spina Bifida Association’s Transition to Adult Care Guidelines.
METHODS:
A workgroup of topic experts was convened including authors from the initial guideline workgroup. The workgroup reviewed and updated the primary, secondary, and tertiary outcome goals, clinical questions, and guideline recommendations based on a literature review.
RESULTS:
Twenty-two additional articles were identified from the literature search. Updated references included observational studies describing transition to adult care outcomes, transition care model initiatives, and a validated self-management assessment tool.
CONCLUSION:
Structured transition initiatives increase the likelihood of establishing with adult care, decrease acute care use for young adults with spina bifida, and have the potential to improve quality of life and optimize chronic condition management. However, there is still a need to implement structure transition practices more broadly for this population using these recommended guidelines.
Introduction
The primary goal of health care transition (henceforth referred to as transition) is to maximize lifelong functioning through the provision of high quality, developmentally appropriate health care that continues uninterrupted as the individual moves from adolescence to adulthood [1]. Collaboration and coordination between the individual, family, pediatric and adult health care providers, allied health services, and school systems are essential to navigate the complexities of transition to adult care and life [2–4]. Fostering the gradual, developmentally appropriate acquisition of independent skills through goal setting and coaching enables adolescents and young adults with spina bifida (SB) to optimize their independence and participation in adult roles and activities throughout transition [5–8].
While transition focuses on adolescent and young adult age groups, the trajectory to maximize adult function and independence is fostered throughout the lifespan by setting expectations early for adult independence and the eventual transition of care [3, 9]. Transition to adulthood and health care planning with the individual and their family is a lifelong process that begins at birth. However, the essential steps of the health care transition (i.e., preparation, hand-off, and completion) primarily take place in adolescent and young adult age groups. Transition preparation should begin between the ages of 12–14 [6, 10] and involves supporting the adolescent in the gradual, developmentally appropriate assumption of increased independence and responsibility for self-care and condition management through coaching in home, school, and clinic settings [5]. Transition hand-off involves transferring care plans and responsibilities from pediatric to adult providers as the individual establishes care in the adult setting. Secondary to the structure of contemporary health care systems, transfer usually occurs between the ages of 18–21, but timing can be variable based on care needs and health care settings [6, 11]. Transition completion refers to the establishment of the individual in the adult healthcare setting, with adult care providers, and with needed community supports to optimize their adult life [10].
Survival to adulthood for individuals with SB now exceeds 85%, but the degree of adult independence in the population varies [12]. In general, individuals with higher lesions (i.e., above the L2 sensory level) and hydrocephalus are more dependent on others for bowel and bladder management, mobility, self-care, transfers, and activities of daily living [13, 14]. Additionally, adolescents with SB may experience a two- to five-year delay in developing autonomy skills compared with their typically-developing peers and may overestimate their abilities [15–17]. By age 30, approximately one-third of individuals with SB report independence, one-third need supervision and occasional help, and one-third routinely require assistance for daily care needs [18]. Also concerning, young adults with SB are less likely to achieve emerging adult milestones such as leaving home, attending college, finding employment, developing romantic relationships, and having multiple friendships compared to their peers without SB [19, 20]. Executive function, socioeconomic status, intrinsic motivation, parental fostering of independence, and bowel continence are significant predictors of successful transition to adult participation [20–22]. Young adults with SB also may experience increased health risks during transition. Many young adults with SB have increased hospitalizations for chronic condition exacerbations, such as urinary tract infections, shunt complications, and skin ulcers, and more difficulty accessing health care services than their age-matched peers [23, 24]. Thus, lifelong assessment and gradual, iterative interventions to maximize chronic condition management, family function, socialization, cognitive function and school performance, mental health, and self-management/self-care are foundational to their optimal participation, function, and quality of life in adulthood [3, 25–28].
Guideline goals and outcomes
Primary
– Maximize health and participation in emerging adult milestones throughout the transition process for individuals with SB.
Secondary
– Provide person-centered, comprehensive transition care that includes transition planning and care coordination beginning by age 14; self-management coaching; decision-making support; education and employment resources; and independent-living support.
Tertiary
– Promote access to uninterrupted, developmentally appropriate SB condition management and preventative care throughout transition – specifically, ages 14–21.
Methods
This manuscript provides an update to the 2018 Spina Bifida Health Care Transition Guidelines [29]. These updates include more recent publication references, assessment tools, and resources to inform spina bifida health care transition clinical practice. The scientific methodology for guideline development has been described by Dicianno et al [30]. To update the previous guidelines, a workgroup of topic experts was convened including authors from the initial workgroup. Table 1 includes the clinical question framing these guidelines.
Clinical questions that informed the transition to adult care guidelines
Clinical questions that informed the transition to adult care guidelines
The following updated key term list was developed by the authoring group: “myelomeningocele”, “lipomyelomeningocele”, “meningocele”, “neural tube defects”, “spinal dysraphism”, “spina bifida” AND “young adult”, “transition of care”, “functional independence”, “autonomy,” “adult healthcare”, “transition to adult care”, “adolescent”, and “self-care”. Medline, PubMed, Web of Science, Cochrane Library, PsycInfo and CINAHL databases were searched for peer-reviewed articles published between January 1, 2016, and November 1, 2020. Additional articles were identified by the authoring group. When applicable, the evidence from the literature search was used to develop these guidelines and, where it was limited, general health care transition guidelines were provided with additional expert clinical recommendations for SB. Each article was reviewed by at least two authors for applicability to the identified outcome goals and to determine needed updates to the recommendations and/or citations for each of the original aged-basedguidelines.
Twenty-two additional articles were identified with the updated search. Of these, eight were cross-sectional studies [6, 31–37], one was a cohort study [38], one was an assessment tool validation study [39], three were qualitative [8, 40], five were literature reviews [41–45], and four were descriptive articles summarizing SB transition clinic models [2, 46].
Of the cross-sectional studies, four were single center studies. Regarding transition preparation, Hopson et al. described common individualized transition plan goals amongst 32 adolescents with SB including completing career interest surveys or exploration opportunities, working on bowel continence, and documenting medical history [6]. Three single-center, cross-sectional studies evaluated transfer and integration to adult care. Shepard et al. found that children engaged in a multidisciplinary SB clinic had more outpatient clinic use than transitioned adults and that adults who did not successfully transition had more emergency care and inpatient utilization than those who did establish with an adult provider [31]. Hettel et al. found that provider preference and communication were the most cited barriers to establishing adult care amongst 27 surveyed adults with SB [34]. Finally, Aguilera et al. surveyed ten young adults with SB established with an adolescent and young adult transition clinic, finding that all had routine primary care follow up, only two had emergency care visits in the last year, and seven reported good to excellent quality of life [36].
The other four cross-sectional studies involved multiple SB clinics. One international study found that amongst young adults who had transitioned to adult care from Brazil, Germany, and the United States, 76.5% of those requiring bladder catheterization were independent in intermittent catheterization, and there was no difference in self-catheterization amongst the nationalities [32]. Three studies focused on transition preparation. Wood et al. tested the predictive validity of the Transition Readiness Assessment Questionnaire-SB (TRAQ-SB) in 90 youth with SB, determining that higher TRAQ-SB scores were associated with urinary continence but not bowel continence or skin breakdown [37]. Wajchendler et al. surveyed 28 Canadian pediatric urologists regarding their SB transition practices and found that 78% did not provide ongoing care after 18 years but only 14% assessed transition readiness [35]. Similarly, Kelly et al. surveyed 34 pediatric SB clinics finding that most discussed the concept of transition but did not routinely evaluate their transition process or discuss insurance changes, and only 30% communicated with adult providers [33].
The cohort study focused on transfer success, revealing only 40% of young adults successfully transferred from a pediatric multidisciplinary clinic to an adult urology clinic. There were no identified predictors of successful transfer, potentially due to low study size [38]. The validity study assessed the TRAQ-SB, finding good internal reliability and strong age correlation for scores [39].
Qualitative studies addressed transition preparation and support topics in single centers. Betz et al. explored understanding of Individualized Education Plans (IEPs) among youth with SB. They found several IEP knowledge gaps and that self-management skills were not included on IEPs [8]. Lindsay et al. interviewed clinicians and young adults with SB regarding the implementation of a single center transition program in Canada, finding that the program facilitated care coordination but accessibility to adult care services and difficulties with adult clinic communication remained barriers [40]. Finally, Stromfors et al. interviewed eight adolescents from Sweden, finding that adolescents overestimated their independence and needed support for independence development as well as social and emotional health [17].
Reviews summarized SB adult care needs as well as SB transition preparation needs. Mukherjee and Pasulka summarized the health and psychosocial needs of adults and the need for primary care access and routine follow-up, structured transition, and strategies to address potentially preventable complications that lead to hospitalization (e.g., sepsis, skin ulcers, infective arthritis, and urinary tract infections) [41]. Similarly, Patel et al. summarized the lifelong multi-organ system SB-related conditions affecting adolescents and adults with SB that need to be addressed during transition [45]. De Kort summarized the literature addressing urological SB transition and recognized the need for dedicated transition staff, addressing readiness, and discussing sexuality and relationship health [44]. A Cochrane Review by Campbell et al. evaluating the effectiveness of transition interventions for youth with chronic conditions found only four randomized controlled trials, including one study that compared adolescents with SB who did and did not attend a two-day transition workshop [42]. The three non-SB studies showed improved patient knowledge and self-efficacy, but the SB-specific study did not find significant results. Finally in a mixed-methods review, Choi et al. cited eight studies addressing SB transition programs and found that quantitative studies reported positive outcomes regarding independence and satisfaction whereas qualitative studies reported negative experiences such as barriers to communication with providers [43].
Descriptive articles summarized various strategies to address structured transition for SB. Betz described perspectives on fostering comprehensive self-management competencies as part of transition, particularly regarding navigating relationships, the community, and adult health care [46]. Seeley and Lindeke described a quality improvement pediatric nurse care coordination intervention that improved TRAQ scores [2]. Fremion et al. described a comprehensive SB transition preparation clinic model that partners with a pediatric multidisciplinary SB clinic and an adult medical home clinic to address transition planning and chronic condition management [7]. Finally, Hopson et al. described the implementation of a lifetime model to provide comprehensive care to individuals with SB using a pediatric and adult hospital system partnership [3].
Using these articles, the authors updated the SB Transition Guidelines as listed in Table 2 with previous references from the 2018 guidelines also included [47–84]. Recognizing the challenge of initiating a comprehensive health care transition process, the workgroup also developed a stepwise strategy for implementing these guidelines into clinical practice based upon expert opinion (Fig. 1).
Summary of transition to adult care guidelines
IEP: individualized education plan. SB: spina bifida. TRAQ-SB: Transition Readiness Assessment Questionnaire Spina Bifida.
Summary of transition to adult care guidelines
IEP: individualized education plan. SB: spina bifida. TRAQ-SB: Transition Readiness Assessment Questionnaire Spina Bifida.
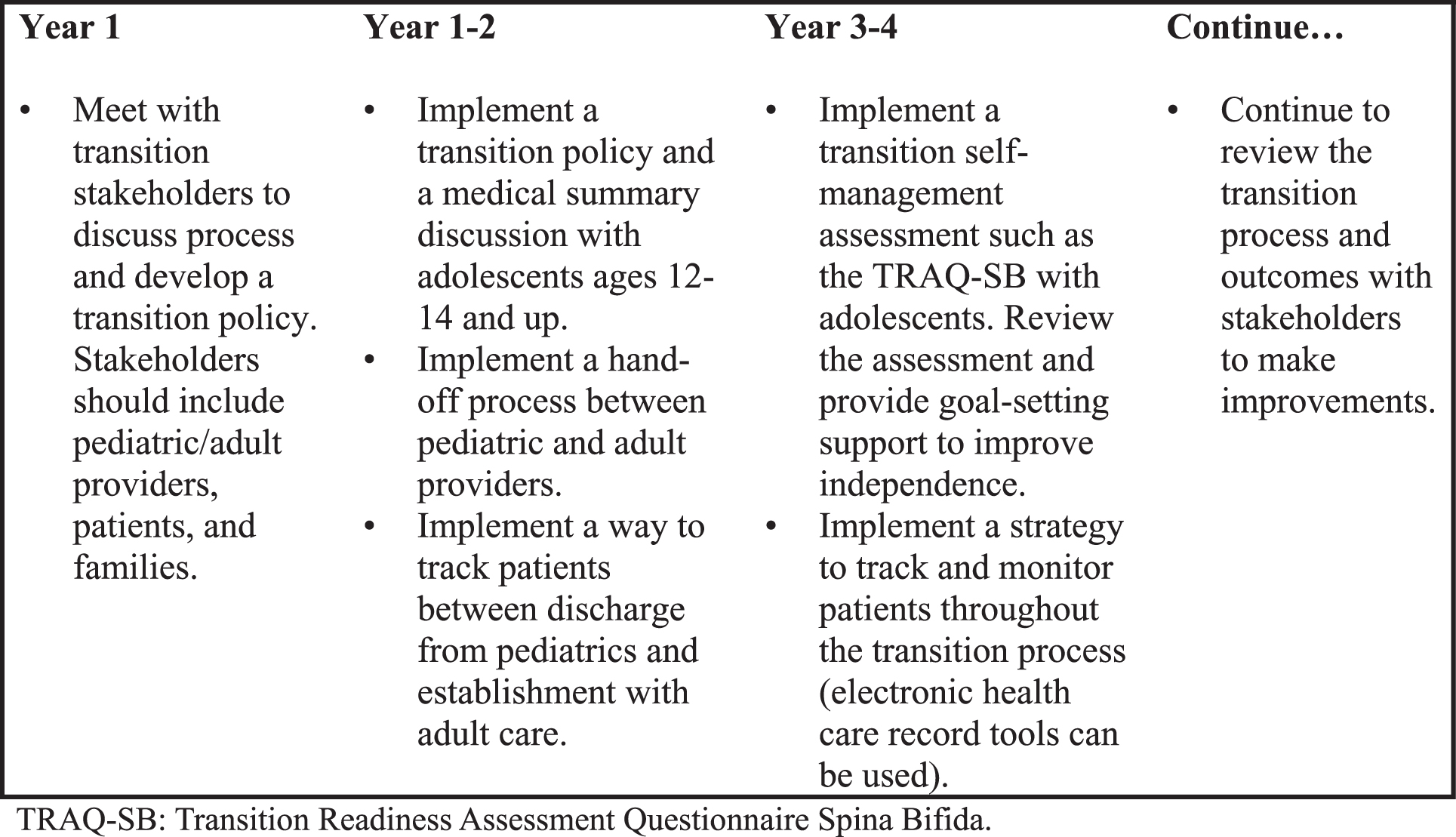
Suggested timeline for implementing a structured transition to adult care clinical process.
These updated guidelines provide additional references for the recommended SB Health Care Transition practices throughout the lifespan. Notably, they include a reference for the TRAQ-SB, a validated measure for transition readiness including specific questions regarding independence SB-care topics that can be used to direct self-management goal setting and measure intervention success during transition preparation [2, 39].
The updated literature search found additional studies addressing the three topics of health care transition: transition preparation, transfer, and completion/integration into adult care for adolescents and young adults with SB. Most studies were single center and descriptive. Studies addressing transition preparation described the need to support self-management independence and adolescent health including mental health and reproductive health [8, 46]. While several publications described single center, clinic-based transition initiatives to improve care coordination and transition readiness skills [2, 40], there is still a need to implement structured transition practices more broadly in pediatric clinics in partnership with adult care clinics [35, 82]. Publications addressing transfer to adult care identified gaps in establishing adult care, particularly around communication with providers and the need to ensure care transfer as well as the benefits of assuring access to adult primary care including decreased acute care utilization [31, 40]. Lastly, publications regarding transition completion and integration into adult care consisted of one study evaluating adult catheterization independence and two literature reviews of adult care needs [9, 45]. As evidence shows that time spent facilitating a successful transition can have significant health impact in the future, transition planning and care coordination are health care priorities for individuals with SB.
Limitations
Overall, there is limited literature evaluating outcomes of transition intervention at each stage: preparation, transfer, and completion. Most studies are single center with small sample sizes. These limitations highlight the need to further evaluate transition preparation and hand-off implementation strategies and patient outcomes as well as adult SB care models that support integration into the adult healthcare system and ongoing comprehensive care.
Conclusions
In summary, general transition to adult care guidelines as well as limited SB-specific studies support the recommendation that transition discussions should begin at birth. Early childhood transition planning should focus on developing long-term goals and expectations to promote optimal health and independence, lifelong care access, and financial planning. During the adolescent years, transition preparation should include developing a care plan (i.e., medical summary, financial plan, care team hand-off plan, decision-making supports, and care supports needed), supporting self-management development, addressing adolescent health topics, and care coordination. Transfer to adult care is an opportunity for proactive care coordination to ensure that individuals establish with adult providers and that adult providers receive a care summary. Finally, adults with SB establishing with adult health care need ongoing, comprehensive, coordinated care to address their SB-related conditions, mental health, general preventive care needs, and self-management supports needs. Further studies are needed to evaluate transition interventions to inform best practices and future guideline updates.
Footnotes
Acknowledgments
Timothy J. Brei, MD, Spina Bifida Association Medical Director; Developmental Pediatrician, Professor, Seattle Children’s Hospital.
Sara Struwe, MPA, Spina Bifida Association President & Chief Executive Officer.
Patricia Beierwaltes, DPN, CPNP, Guideline Steering Committee Co-Chair; Assistant Professor, Nursing, Minnesota State University, Mankato.
Brad E. Dicianno, MD, Guideline Steering Committee Co-Chair; Associate Medical Director and Chair of Spina Bifida Association’s Professional Advisory Council; Associate Professor, Department of Physical Medicine and Rehabilitation, University of Pittsburgh School of Medicine.
Nienke Dosa MD, MPH, Guideline Steering Committee Co-Chair; Upstate Foundation Professor of Child Health Policy; SUNY Upstate Medical University.
Lisa Raman, RN, MScANP, MEd, former Spina Bifida Association Director, Patient and Clinical Services.
Jerome B. Chelliah, MD, MPH, Johns Hopkins Bloomberg School of Public Health.
Julie Bolen, PhD, MPH, Lead Health Scientist, Rare Disorders Health Outcomes Team, National Center on Birth Defects and Developmental Disabilities, Centers for Disease Control and Prevention.
Adrienne Herron, PhD Behavioral Scientist, Intervention Research Team, National Center for HIV/AIDS, Viral Hepatitis, STD, and TB Prevention, Centers for Disease Control and Prevention.
Judy Thibadeau, RN, MN, Spina Bifida Association Director, Research and Services; former Health Scientist, National Spina Bifida Program, National Center on Birth Defects and Developmental Disabilities, Centers for Disease Control and Prevention.
Conflict of interest
Ellen Fremion and Kathrine Smith are unpaid board members and provider advisory committee members of the Spina Bifida Association.
Funding
The development of these Guidelines was supported in part by Cooperative Agreement UO1DD001077, funded by the Centers for Disease Control and Prevention. Its contents are solely the responsibility of the authors and do not necessarily represent the official view of the Centers for Disease Control and Prevention or the Department of Health and Human Services.
