Abstract
PURPOSE:
The purpose of this study was to examine the reliability and discriminant validity of the Quantitative Timed up and Go (QTUG) in typically developing (TD) children and children with cerebral palsy (CP).
METHODS:
Twenty-eight TD children and 8 with CP (GMFCS I-II) completed 3 TUG trials while wearing QTUG sensors. Test-retest reliability and discriminative ability were examined for the 57 constituent parameters of the TUG. Relationships between age and these parameters were also examined.
RESULTS:
Forty-four of the parameters demonstrated moderate to excellent test-retest reliability, with measures of angular velocity being the most reliable. Twenty-six parameters were different between TD children and those with CP, and twenty-eight gait parameters demonstrated correlations with age, further supporting its discriminative ability.
CONCLUSION:
The QTUG is a clinically feasible tool that is capable of both reliably measuring and discriminating many of the movement parameters with the TUG mobility task in TD children and those with CP GMFCS I-II. The results of the present study provide preliminary evidence that the QTUG can discriminate between children on several of the gait parameters within the TUG.
Introduction
Cerebral palsy is the leading cause of neuromotor impairments occurring in 1–4 per 1000 live births each year [1]. The deficits in motor performance and functional mobility observed in these children are associated with activity restrictions and lower levels of participation across multiple life domains [2]. Specifically, gait disorders are among the leading limitations with a negative impact on participation and self-perception in individuals with CP [3]. A surveillance study of more than 9,000 children with CP found that at 5 years of age, 54% of them with CP ambulate unaided (without assistive or mobility devices), 16% use an assistive device, and 30% are unable to ambulate [4]. The limitations and deviations in balance and gait with cerebral palsy are extensive and well documented [5–7]. Given the changes in functional balance and gait that occur along with the multitude of approaches utilized to target gait efficacy in children with CP, accurate longitudinal measurement of functional balance and gait in these children is warranted.
The Timed Up and Go test (TUG) is a widely used measure of balance and functional mobility that involves observing and timing the participant while they rise from an armchair, walk three meters, turn, walk back and sit down [8]. The TUG test has been evaluated in children with CP who are ambulatory to assess balance, anticipatory postural control, and functional mobility (9 [GMFCS I-II], 10 [GMFCS I-III]). The TUG is both responsive and reliable in children with cerebral palsy [10]. Furthermore, the correlation between TUG scores and GMFM-88 scores in children with CP reported by Chrysagis et al. supports the TUG’s validity in this population [11]. The TUG’s ability to differentiate the performance between children of differing GMFCS levels further supports its use as a meaningful clinical measure of balance and functional mobility in this population because TUG scores appear to coincide with the varying functional levels [9, 10]. However, the method of measurement used in the TUG (time taken to complete) does not stratify the test into its constituent components. A targeted assessment of these individual components could provide valuable clinical, predictive, and discriminative information. In fact, aspects of the TUG such as the sit-to-stand transition, several of the turn parameters, and variability of spatial and temporal parameters in gait have been found to be associated with fall risk in older adults [12–14]. These findings suggest that accurate quantitative information on the components of the TUG task could enhance the quality of the clinical examination and assessment, facilitating the clinician’s ability to better target meaningful deficits to address through intervention.
While the gold standard for accurate kinematic assessment has been laboratory-based, the use of inertial sensors has been explored in the literature as a more clinically feasible method for the quantification of gait parameters [14–18]. The Kinesis Quantified Timed Up and Go (QTUG) utilizes inertial sensors placed on the proximal tibia to quantify spatial, temporal, turn, and angular velocity parameters during the TUG test. The QTUG has been validated in elderly adults and those with neurologic disorders such as Parkinson’s disease and Multiple Sclerosis [14, 18]. While preliminary evidence supports the utility of using body-worn inertial sensors in children, [12, 19], the clinimetrics of the QTUG in children with CP have not been examined. Therefore, the aim of this study was to determine the discriminant validity and reliability of the QTUG for the quantification of spatial, temporal, turn, and angular velocity gait parameters in children with CP.
Methods
Participants
The sample size calculation using 3 trials, an α level of 0.05, β level of 0.20 (statistical power of 80%) with an expected ICC of 0.9×0.1, and a 10% dropout rate identified an appropriate sample size of 10–12 participants consistent with the methods described by Bonnet [20]. This study was approved by the Shenandoah University Institutional Review Board (#657). The parents and/or legal guardians, along with the participants (when able), provided informed consent.
Thirty-six participants were recruited in this study via convenience and snowball sampling. Eight children with CP and twenty-eight typically developing (TD) children were recruited. TD children were recruited via email, and inclusion criteria were 1) being between 5 and 17 years old, 2) having no orthopedic surgeries or injuries in the last 6 months, 3) having no history of neurologic injuries, and 4) not having an individualized education program (IEP). All interested participants who met the TD inclusion criteria completed data collection. For the recruitment of children with CP, an email was sent to parents of children with CP (GMFCS levels I-II) known to the researchers and to local pediatric physical therapy clinics. Inclusion criteria were 1) having a diagnosis of cerebral palsy classified as GMFCS level I or II and 2) being between 3–17 years of age. Researchers expanded the age range for children with CP based on the limited number of eligible participants within the community. Exclusion criteria were 1) inability to follow simple commands, 2) having a CP diagnosis of GMFCS level III–V, 3) having recent orthopedic surgeries or orthopedic injuries in the last 6 months, or 4) having botox injections within the last 4 weeks. Participant demographics can be found in Table 1.
Subject demographics
Subject demographics
The researchers originally reached out to nineteen families for participation, in which eleven guardians of participants agreed to volunteer for the study. The data collected on one participant was not used due to researcher error during data collection, and the participant was not able to return for a second trial. The data from two participants were excluded due to inability to follow commands. The data collection took place in a local physical therapy clinic as well as the university building of the researchers. The researchers accommodated some participants by collecting the data during their physical therapy treatment sessions if they were unable to make it to the prioritized location. Based on the structure and purpose of this study, there was no required follow-up.
All measurements were taken by second-year entry-level DPT students who were provided with the instruction booklet and time to practice with the QTUG prior to data collection. Data were collected over a three-year period with 14 students involved. No formal training was provided. Participants were seated on an adjustable bench with their feet flat on the floor and their hips and knees positioned at 90/90. A cone was placed on the floor 3 meters away from each child. Kinesis QTUGTM sensors were placed on each participant’s proximal tibia bilaterally, 1 inch distal to the inferior pole of the patella, with the sensor lights against the skin (Fig. 1). Each sensor was held in place with a self-adhesive bandage wrap. All participants wore shoes during the trials, and orthotics were also worn by all children who regularly wore them. Each participant was given the same instruction: “When I say go, stand up, walk around the cone, walk back, and sit down. Go as fast as you can, but do not run. 1, 2, 3, go!”. Each participant performed the QTUG a total of 3 times and took rest as needed in between trials. The same student recorded the data for all three trials. Participants were asked to repeat trials if they became significantly distracted and/or veered off task.
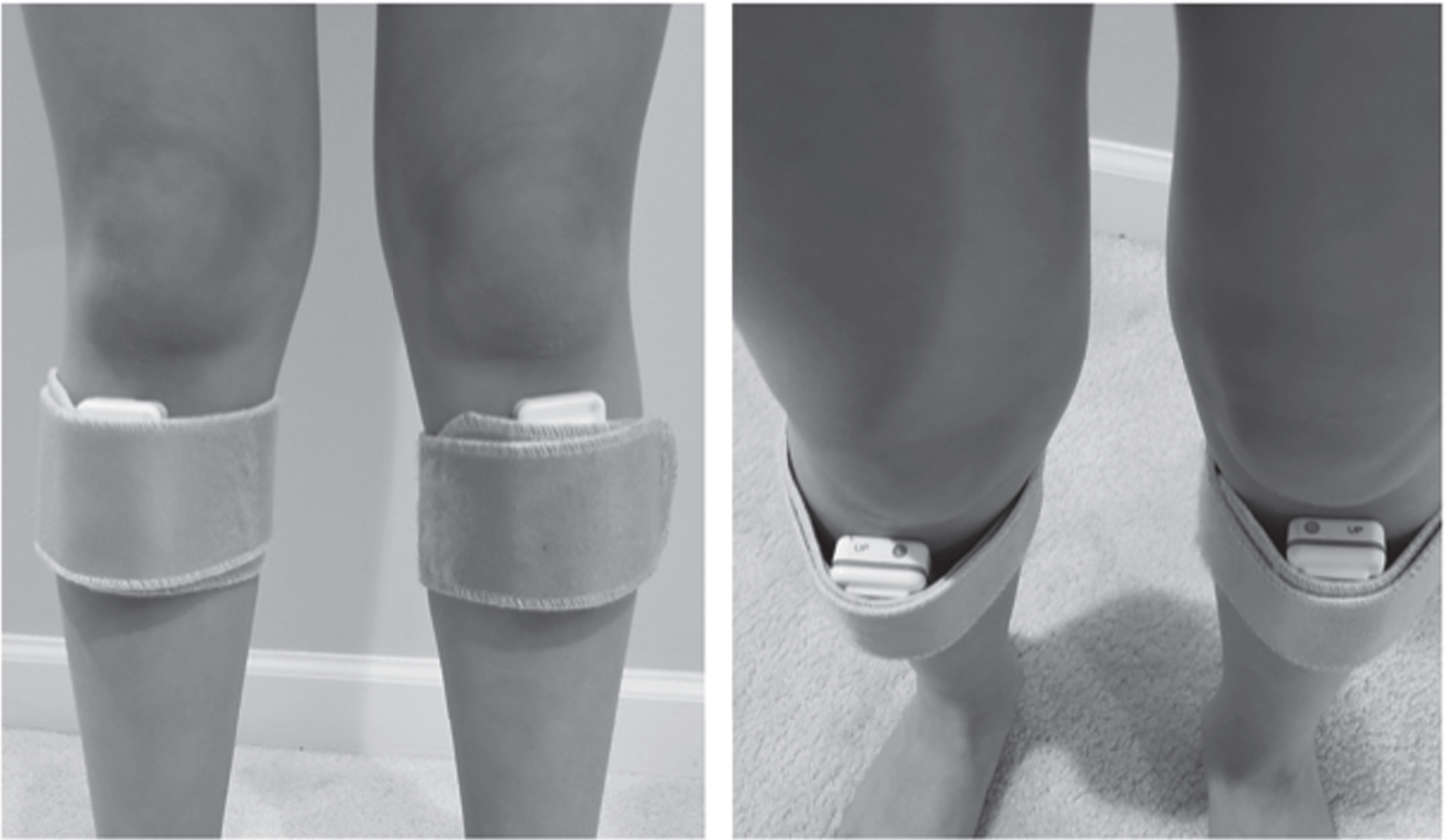
Anterior to posterior (left) and cranial to caudal view (right) view of child wearing QTUG sensors with self-adhesive bandage wrap on bilateral proximal tibias.
The 57 parameters recorded with the QTUG can be grouped into the following five categories: spatial gait parameters, temporal gait parameters, turn parameters, angular velocity parameters, and angular velocity×height parameters [21].
Statistical analysis
Kinesis QTUGTM data were downloaded directly into Excel (version 16.42 Microsoft Office Redmond, WA) and transferred to SPSS (version 27.0 IBM Chicago, IL). The data collected for all 57 parameters were analyzed for normality using the Shapiro-Wilk test for both the children with CP GMFCS I-II and the TD children. Data were then analyzed with an α level of 0.05 to determine statistical significance. The fifty-seven QTUG parameters were analyzed for test-retest reliability, discriminant validity, and correlation with age. As there are no generally accepted ICC cut off points, we used the cut off values described by Smith et al. [18]. Specifically, ICC >7 is considered excellent, 0.4–0.7 is considered fair to good, and <0.4 is considered poor [18, 22].
Results
Fifty-one of the 57 (89.5%) parameters were normally distributed in the children with CP GMFCS I-II, while 49 of the 57 (85.9%) parameters were normally distributed in the TD children (Shapiro-Wilk test, p > 0.05). Intraclass correlation coefficients were calculated with a 95% confidence interval to determine test-retest reliability for each of the 57 parameters recorded. ICC’s ranged from –0.225 to 0.955. Within the parameters, 13 of the 15 angular velocity parameters (87%), 6 of the 9 angular velocity×height parameters (66%), 2 of the 6 turn parameters (33%), 2 of the 4 spatial gait parameters (50%), and 10 of the 23 temporal gait parameters (43%) demonstrated excellent reliability (ICC >0.7). Of the fifty-seven parameters analyzed, twenty-six differed between children with CP GMFCS I-II and TD children, supporting their discriminant validity (Mann Whitney U test, p < 0.05). Within the parameters, 7 of the 15 angular velocity parameters (47%), 5 of the 9 angular velocity×height parameters (56%), 4 of the 6 turn parameters (67%), 3 of the 4 spatial gait parameters (75%), and 6 of the 23 temporal gait parameters (26%) discriminated between children with CP GMFCS I-II and TD children. Twenty-eight parameters were found to be correlated with age (Spearman rank order correlation, p < 0.05). Within the parameters, 12 of the 15 angular velocity parameters (75%), 4 of the 9 angular velocity×height parameters (44%), 3 of the 6 turn parameters (50%), 1 of the 4 spatial gait parameters (25%), and 8 of the 23 temporal gait parameters (35%) were correlated with age for all of the children combined. Within the subset of the CP GMFCS I-II children, 2 of the 15 angular velocity parameters (13%), 3 of the 6 turn parameters (50%), and 6 of the 23 temporal gait parameters (26%) were correlated with age. Within the TD group, 12 of the 15 angular velocity parameters (75%), 2 of the 9 angular velocity×height parameters (22%), 2 of the 4 spatial gait parameters (50%), and 9 of the 23 temporal gait parameters (39%) were correlated with age.
Reliability of parameters
QTUG parameters with excellent reliability
Test-retest reliability was excellent (ICCs >0.7) for thirty-three of the recorded parameters (Table 2), and seventeen of them discriminated between the children with CP GMFCS I-II and the TD children (Mann Whitney U test, p < 0.05). For the subset of children with CP GMFCS I-II, twenty parameters demonstrated excellent test-retest reliability (Table 2), while twenty-five parameters demonstrated excellent test-retest reliability in TD children (Table 2).
Parameters with excellent test-retest reliability
Parameters with excellent test-retest reliability
*p < 0.05 (Mann Whitney U test) between TD (typically developing) and CP; SG, Spatial Gait; TG, Temporal Gait; T, Turn; AV, Angular velocity; AVH, Angular velocity×Height.
Test-retest reliability was fair to good (ICC 0.4–0.7) in eleven of the parameters, with six of those able to discriminate between the children with CP GMFCS I-II and the TD children (Table 3; Mann Whitney U test, p < 0.05). For the subset of children with CP GMFCS I-II, nineteen parameters demonstrated fair to good test-retest reliability, and seventeen demonstrated fair to good test-retest reliability for TD children (Table 3).
Parameters with fair-good test-retest reliability
Parameters with fair-good test-retest reliability
*p < 0.05 (Mann Whitney U test) between TD (typically developing) and CP; SG, Spatial Gait; TG, Temporal Gait; T, Turn; AV, Angular velocity; AVH, Angular velocity×Height.
Test-retest reliability was poor (ICC <0.4) in thirteen of the parameters. 3 discriminated between the TD children and children with CP GMFCS I-II (Table 4; Mann Whitney U test, p < 0.05). Of the parameters that were poorly reliable for all participants, one demonstrated excellent reliability (ICC ≥0.7) for children with CP GMFCS I-II, and one demonstrated excellent reliability (ICC ≥0.7) in the TD children. For the subset of children with CP GMFCS I-II, eighteen parameters demonstrated poor test-retest reliability, while fifteen for TD children demonstrated poor reliability (Table 4).
Parameters with poor test-retest reliability
Parameters with poor test-retest reliability
*p < 0.05 (Mann Whitney U test) between TD (typically developing) and CP; SG, Spatial Gait; TG, Temporal Gait; T, Turn; AV, Angular velocity; AVH, Angular velocity×Height.
Out of the fifty-seven parameters, twenty-eight were correlated with age (Spearman rank order correlation, p < 0.05). One (average forward rotation speed) was strongly correlated with age (r≥0.7), twelve moderately correlated (r = 0.5–0.69) (Table 5), and fifteen poorly correlated (r = <0.5) with age (Table 6). In the subset of children with CP GMFCS I-II, eleven parameters were correlated with age, and all of these were strong correlations (r≥0.7, p < 0.05, Spearman rank order correlation). In TD children, 21 parameters were correlated with age (p < 0.05 Spearman rank order correlation). Of these, seven parameters were strongly correlated (r≥0.7), ten were moderately correlated (r = 0.5–0.69,) and 4 were poorly correlated (r = <0.5) (Table 6).
Parameters strongly and moderately correlated with age
Parameters strongly and moderately correlated with age
*p < 0.05 Spearman Rank-Order Correlation for the Combined (all), CP only or TD only subsets of children.
Parameters poorly correlated with age
*p < 0.05 Spearman Rank-Order Correlation for the Combined (all), CP only or TD only subsets of children.
The current study provides novel findings of the test-retest reliability and discriminant validity for a wide range of movement parameters during the TUG test using clinically feasible inertial sensors using the QTUG in TD children and children with CP GMFCS I-II. While test-retest reliability varied among the parameters, ranging from excellent to poor, forty-four showed fair to excellent reliability, and twenty-six could discriminate between children with CP GMFCS I-II and TD children. Furthermore, twenty-eight were correlated with age, further supporting their discriminative ability.
In addition to confirming the discriminative ability of the TUG itself, the majority of the parameters within the TUG test examined with the QTUG demonstrated at least fair reliability in both the children with CP GMFCS I-II and TD children. Consistent with the literature, the overall TUG times of the children with CP GMFCS I-II were longer than those in the TD children [23]. While it is unknown whether TUG time is associated with fall risk in children, the time taken to complete the TUG test can predict fall risk in a number of adult populations supporting its clinical relevance [24, 30]. Given that several of the constituent components contribute to the longer times taken to complete the TUG and could contribute to the higher falls risk, [12, 14] the ability to accurately measure these components is meaningful. Overall, the angular velocity parameters demonstrated the strongest reliability, while the temporal gait parameters, particularly those assessing asymmetry, demonstrated the weakest reliability, speaking to the clinical utility of the angular velocity measures over the asymmetry measures. In the present study, children with CP GMFCS I-II had faster angular velocities than TD children, which is consistent with the higher postural sway velocities reported in children with CP [26]. Variability of movement trajectories such as stride length is thought to be the result of errors or deficits in motor control. Such variability is considered to be a key contributor to dynamic instability during walking [27–29]. The reported correlation between varying stride rates and increased angular velocity in children with CP [25] therefore supports the clinical importance of the QTUG’s ability to measure angular velocity parameters.
Gait velocity (walk time), number of steps, and number of gait cycles were found to be reliable when TD and children were combined and in the subset of TD children but not reliable in the subset of children with CP GMFCS I-II. The limited inter-participant variability in these parameters amongst the children with CP GMFCS I-II, along with the smaller number of children with CP in the current study, may have contributed to the lower ICC compared to that of the larger, more heterogeneous sample that included TD and children with CP. The lower ICC, along with limited inter-participant variability, is consistent with what has been reported with the 10-meter walk test [31]. Furthermore, children with CP GMFCS I-II had slower walk times, more gait cycles, and a higher number of steps than TD children in the present study. The discriminative ability of these parameters identified in the current study further suggests that the lower reliability calculations may not accurately reflect their clinical utility. Chakraborty et al. have hypothesized that, in response to having a more variable step length, children with CP may take more steps to maintain balance and properly dissipate disturbances encountered when walking [32], which is consistent with the reported associations between fall risk and both number of steps and number of gait cycles [33].
The QTUG quantifies several parameters within the turning component of the TUG task, which could allow the clinician to accurately measure the turning ability in children with CP. The present study found that turn time and the number of steps per turn measured with the QTUG were greater in children with CP GMFCS I-II. These findings are consistent with those measured with the Step and Quick Turn Test (SQT) on a NeuroCom Balance Master [34]. Both the longer duration and increased steps to turn are associated with higher fall risk. Thus, it has been postulated both may be the result of the child adopting a careful turn strategy with a wider base of support to make up for their lack of dynamic stability [5]. However, similar to reports in adult populations, the present study found low test-retest reliability in these parameters. Therefore, caution must be taken with these measures when interpreting these measures clinically.
Decreased energy efficiency during gait has been widely reported in the literature, but quantification of this is difficult in most clinical settings [35, 36]. While the QTUG does not directly measure energy efficiency, a slower post-turn time compared to pre-turn time has been hypothesized to indicate impaired endurance [21]. The current study, however, found that pre-to-post-turn time had poor reliability and that only post-turn time was able to discriminate between the TD children and children with CP GMFCS I-II, suggesting that its ability to accurately and reliably measure gait endurance is limited. The distance ambulated during this task might simply be too short to assess endurance in such high-functioning children. Thus, clinical measures such as the two-minute walk test (2MWT) or the six-minute walk test (6MWT) may therefore be more appropriate for the assessment of endurance in ambulatory children with cerebral palsy [35–37].
The results of the present study provide preliminary evidence that the QTUG can discriminate between children on several of the gait parameters within the TUG. It is conceivable that the results of the present study actually underestimate the number of parameters that are discriminatory between TD children and children with CP given the small sample size examined. For example, while cadence and average stance time were not able to discriminate between children with CP GMFCS I-II and TD children, children with CP GMFCS I-II had a slower cadence and longer average stance time than TD children, which is consistent with previous literature [30, 38]. Given the strong reliability of many of these measures, further investigation of their discriminative ability is warranted. In addition to the ability to discriminate between TD children and children with CP GMFCS I-II on several parameters, the present study identified moderate to strong correlations between age and thirteen of the fifty-seven QTUG parameters. The documented correlations between age and TUG time [39, 40], along with the changes in gait parameters that occur as children age [41, 42], suggest that the present study provides preliminary evidence for the discriminative ability of the QTUG for these parameters. While laboratory-based measurement of gait and movement parameters are considered the gold standard for kinematic analyses, these methods are extremely costly and require a large workspace with extensive setup, including calibration and training [15]. The QTUG is much less costly, easily portable, and requires minimal training. The present study provides strong initial evidence to support the utility of the clinically feasible QTUG for the quantification of several components of the TUG task. A better understanding of these parameters, including the ability of the QTUG to reliably quantify these measures, could assist the clinician with accurate measurement of the specific impairments of their patients within the global TUG task and, therefore, aid in the development of more targeted interventions to address their limitations.
There are limitations to the present study that should be considered. First, while the power analysis supported the sample size in it, the number of children with CP was small. Furthermore, given the inherent variability of children with CP, this analysis might be an underestimate of the appropriate sample size, and this small sample is likely not representative of the larger population of children with CP. A larger sample size would not only enhance the validity of the findings but would also allow additional analyses, including the determination of age-based norms. Furthermore, the raters in this study were students (as opposed to clinicians with more experience), and they did not receive formal training prior to data collection. It can be hypothesized that with additional training and experience, the reliability of the data would increase. While this lack of training and experience may be considered a limitation, the majority of parameters had at least fair reliability supporting the clinical utility of the measurements without extensive training. The increased number of trials for children with CP when they veered off task and had to be discarded might also be considered a limitation due to increased levels of fatigue and, therefore, more variability in performance. This potential variability due to fatigue would suggest that the reliability for children with CP is stronger than that reported in this study, further supporting the utility of the QTUG in this population. Further investigation to determine age-matched norms, as well as the concurrent validity of the QTUG parameters with a laboratory-based kinematic analysis, is also warranted.
Conclusion
The QTUG is a clinically feasible tool that is capable of both reliably measuring and discriminating many of the movement parameters with the TUG mobility task in TD children and those with CP GMFCS I-II. Angular velocity measures, which may reflect postural sway velocities and variability of movement trajectories, are the most reliable measures in this population while also being discriminative. Turning parameters and measures of asymmetry were less reliable, but the turning parameters were found to be different between TD children and children with CP with CP GMFCS I-II suggesting discriminative ability. Knowledge of these findings can help to guide the clinician in a more comprehensive and accurate examination of the many components within the TUG task in children with CP with CP GMFCS I-II.
Footnotes
Acknowledgments
The authors would like to thank Kevin Anderson, SPT and Breanna Spain, SPT for their participation in the gathering and analyzing of data.
Conflict of interest
The authors have no conflicts of interest to report.
