Abstract
PURPOSE:
The aim of this study is to determine the factors influencing the decrease of the vaccination rate among children with nonprogressive neurodevelopmental disorders in Bosnia and Herzegovina.
METHODS:
This study included 149 parents of children with nonprogressive neurodevelopmental disorders. The children were rehabilitated at the University Clinical Hospital Mostar, from October 2017 to February 2019.
RESULTS:
The vaccination rate of children with nonprogressive neurodevelopmental disorders was 34.9% (
CONCLUSION:
Overall, this study showed that the majority of children with nonprogressive neurodevelopmental disorders were unvaccinated. The majority of the parents trusted the physicians’ opinion on vaccination. Neuropediatricians and neurophysiatrists most often postponed the regular vaccination of children.
Keywords
Introduction
Routine vaccination with a coverage higher than 95% resulted in global eradication of smallpox. Additionally, other infectious diseases such as polio and diphtheria have not been recorded among former Yugoslavian countries for more than 30 years [1].
Despite the convincing evidence on the positive role of vaccination in disease prevention, vaccine hesitancy has become a growing problem in public health. The resurgence of diseases is mostly caused by the postponing or refusal of vaccination, which can result in epidemics with possibly fatal outcomes [2, 3]. According to the World Health Organization (WHO) data from 2019, the average vaccination rate in Bosnia and Herzegovina (B&H) for vaccine-preventable diseases among children in the general population varies from 62% to 100% depending on type of vaccine. Due to missed vaccinations in B&H, three major epidemics of measles have occurred. The first in B&H was between 1997 and 1999, with 6,748 measles cases registered in B&H. The second one was between 2014 and 2015, with 5,084 cases registered, and the third one was in 2019, with 1,330 cases registered [4].
Anti-vaccination campaigns have had a huge impact on the growing hesitancy towards vaccination, resulting in lower vaccine coverage in recent decades, despite the fact that false assumptions have been rejected by the WHO and the United States Centers for Disease Control and Prevention (CDC) [5]. One of the most important events that influenced antivaccination propaganda was the study by Andrew Wakefield from 1998, which presented the relationship between the measles, mumps, and rubella vaccine and the onset of neurodevelopmental disorders such as autism. Moreover, other numerous unverified theories on the association of vaccines and neurodevelopmental delay disorders, diabetes mellitus, and Guillain-Barré syndrome have been proposed [5–7].
Most of the reasons for nonvaccination are medically unjustified [8], showing that the knowledge, experience, and personal attitudes of parents and healthcare professionals, as well as the healthcare environment, have a major impact on vaccination decision-making.
Vaccine hesitancy is a major issue for healthcare systems worldwide and should be addressed effectively. By dealing with it, negative consequences that could lead to extreme pandemics can be prevented. Therefore, the aim of this study is to determine the factors influencing the decrease in the vaccination rate of children with nonprogressive neurodevelopmental disorders in B&H. Special attention is paid to the role of healthcare professionals in vaccination decision-making and their contribution to the decrease of the vaccination rate.
Methods
Study design
This prospective study included 149 parents of children who were diagnosed with nonprogressive neurodevelopmental disorders and have been rehabilitated at the Department for Physical Medicine and Rehabilitation of University Clinical Hospital Mostar (UCHM), B&H, from October 2017 to February 2019. The exclusion criteria are as follows: parents of children hospitalized at the Department for Physical Medicine and Rehabilitation, parents of children who were not diagnosed with neurodevelopmental disorders, and parents of children with progressive neurological conditions. Data were collected through a survey questionnaire answered by parents. This study included children with nonprogressive neurodevelopmental disorders such as children with hypertonic, dystonic, or hypotonic syndrome; different kinds of paresis; and torticollis.
The detailed questionnaire consisted of one-choice or multiple-choice questions regarding the following: (1) child’s date of birth; (2) diagnosis; (3) place of residence; (4) relation of the person answering the questionnaire with child; (5) parents’ education level; (6) parents’ employment status; (7) number of children in the family; (8) number of vaccinated children in the family; (9) vaccination according to the schedule; (10) reasons for not having a child vaccinated according to the vaccination schedule; (11) type of healthcare professional who advised nonvaccination; (12) opinions of parents about the vaccination process; (13) knowledge of the parents on the safety and side effects of vaccines; (14) sources of vaccine-related information for parents; (15) parent satisfaction with the information received from the physician; (16) influence of the physician on the parents’ decision to have their children vaccinated; and (17) parents’ views on how the mandatory vaccination program in B&H could be improved. Questions 11–14 and 17 were multiple-choice questions.
Statistical analysis
Results were analyzed using SPSS version 23.0 (SPSS, Chicago, IL) and Microsoft Excel (Microsoft Office 365). Results are presented as absolute numbers (N) and percentages (%). Statistical significance was assessed using the chi-squared test (χ2 test) and Fisher’s exact test in the absence of expected frequencies. Binary logistic regression models were also used to assess different variables in multiple response questions where conditions were satisfied. Expected frequencies were checked in accordance with Field’s (2009) recommendation. Less than 20% of expected frequencies can be smaller than 5, but none of them can be smaller than 1. The significance level was set at
Results
The study involved 149 respondents, among which 122 (81.9%) were mothers, 19 (12.8%) were fathers and the rest were in another relationship with the child. The vaccination rate of children with nonprogressive neurodevelopmental disorders was 34.9% (χ2 = 13.59; s.s. = 1;
Review of respondents’ characteristics
Review of respondents’ characteristics
Out of the total respondents, 91 (61.1%) reported which sources of information on vaccination they used. The most common source of information about vaccines and the vaccination process were physicians, followed by the media, including the internet, television, and newspapers (Table 2). Different sources of information were assessed using binary logistic regression model. Moreover, the model did not predict a statistical significance regarding the parent’s decision on vaccination, thereby, none of the predictors was statistically significant (Table 3).
Information sources about vaccines and the vaccination process among parents of children with nonprogressive neurodevelopmental disorders
*Multiple-choice question. ** χ2 test used for every answer individually.
Statistical analysis of advice from pediatrician and neuropediatrician/neurophysiatrist for not vaccinating children using binary logistic regression
R2 = 0.24 (Cox i Snell); 0.33 (Nagelkerke).
A considerably higher percentage of the parents (58.4%) reported that they trusted their pediatrician and made decisions regarding the health of their children according to the physician’s recommendations, compared to the percentage of those who did not fully trust their pediatrician’s advice (χ2 = 4.19; s.s. = 1;
The majority of the parents (87.6%) reported that the vaccination of their children was postponed as per their physician’s recommendation (χ2 = 203.49; s.s. = 3;
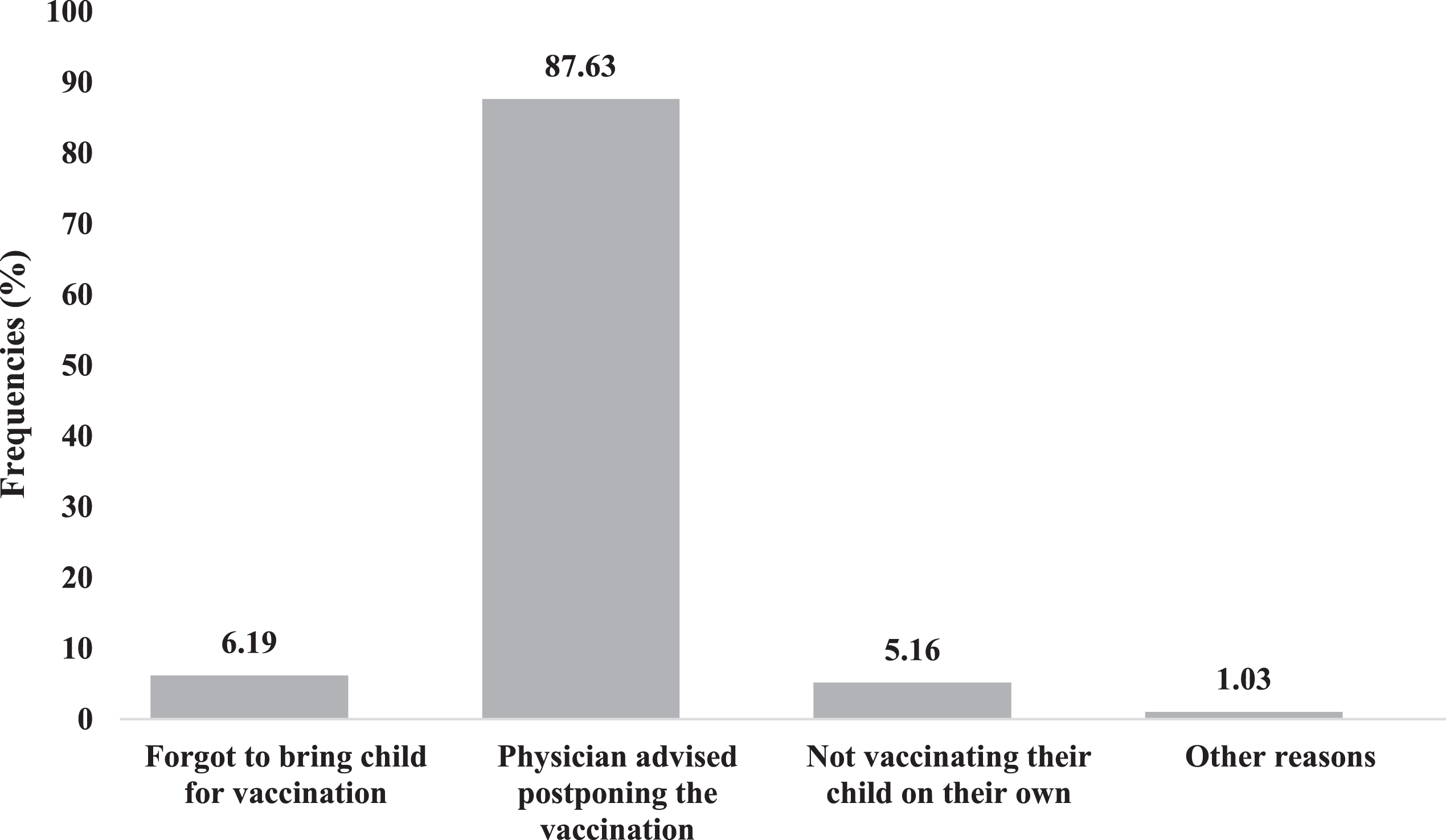
Reasons for vaccination refusal among parents of children with neurodevelopmental disorders. Physicians had the biggest influence on vaccination refusal (χ2 = 203.49; s.s. = 3;
Different medical specialties were also analyzed using binary logistic regression models based on the parents’ answers about the advice on the nonvaccination of their child. Only two predictors fulfilled the conditions to be put in the model, while others had expected frequencies less than one. In most cases, the nonvaccination of children was advised by a neuropediatrician or neurophysiatrist (44.2%) and a pediatrician (32.2%). It was a significant predictor of children actually remaining unvaccinated (Table 4). Omnibus tests show a significance level at 1%. The model explains between 24% and 33% of the nonvaccination of children.
Types of healthcare professionals who advised parents of children with nonprogressive neurodevelopmental disorders not to vaccinate their child
*Multiple-choice question. ** χ2 test was used for every answer individually.
Regarding the parents’ attitudes toward vaccination, 30.9% of the parents doubted the source of vaccines and their composition (χ2 = 21.80; s.s. = 1;
The parents’ personal beliefs about their decision on vaccination was examined using binary logistic regression. Only three predictors satisfied the conditions to be put in the model. The results of the omnibus tests showed a significance level of 5%, so the model predicted significantly higher probability for children to be unvaccinated compared to the model with constant alone. The model described a variance of nonvaccination between 5% and 8%. The predictor “I think that’s too much vaccine for my child” showed a statistical significance. The odds of parents not vaccinating their children were 6.1 times greater in those who answered this question (Table 5).
Assessing parents’ personal beliefs about their decision not to vaccinate their child using binary logistic regression
R2 = 0.05 (Cox i Snell); 0.08 (Nagelkerke).
The majority of the children (65.9%) were not regularly vaccinated in the group of parents who were informed about the vaccines and vaccination process (χ2 = 8.17; s.s. = 2;
The majority of the parents suggested that the mandatory vaccination program in B&H could be improved by sending a formal notice to parents via e-mail in the first place (27.5%, χ2 = 30.12; s.s. = 1;
Possible ways of improving the mandatory vaccination system in B&H according to the respondents
*Multiple-choice question. ** χ2 test was used for every answer individually.
Children with nonprogressive neurodevelopmental disorders should not be different in terms of vaccination from children who do not have this diagnosis and should be vaccinated according to the regular vaccination schedule [9]. Despite that, vaccination rate of children with nonprogressive neurodevelopmental disorders in this study was 34.9%, which is considerably lower than the recommended vaccination rate of more than 90% [10]. However, the vaccination rate in the study is less than half the vaccination rate of the children from the general population in B&H [11]. According to the results presented here, O’Neill as well as colleagues summarized the results from multiple studies in their review regarding this topic, which undoubtedly showed a similar negative trend in the vaccination rate of children with neurodevelopmental disorders in different countries [12].
The observed low vaccination rate is very concerning considering the increase in the rate of vaccination hesitancy in B&H, which may lead to vaccine-preventable disease outbreaks [13]. As a result, a large measles epidemic in B&H was reported between 2014 and 2015, with 5,083 cases registered, and the last measles epidemic in 2019, with more than 90% of cases wherein children were not vaccinated against measles [4].
The ESCULAPIO project conducted by the Italian Ministry of Health showed that physicians were the most common source of information on vaccines and the vaccination process, followed by the media [14]. In this study, the parents answered similarly to those in the ESCULAPIO project, where parents were twice as likely to be informed from physicians than from the media.
In general, the poor awareness about the efficacy of vaccines and the vaccination process among parents is often associated with the delay or refusal of vaccination, consequently showing a negative vaccination trend that was observed based on the results of the current study [15], with one third of the respondents not being sufficiently informed about the source of vaccines.
In the current study, the majority of the parents reported that they fully trusted their pediatrician and made decisions regarding the health of their children entirely on the recommendation of healthcare professionals. Schmitt et al. showed that one of the main predictors of vaccine acceptance is the recommendation that comes from healthcare professionals at the vaccination center [16]. Similar results were found in a study conducted in the U.S.A, wherein most of the parents who changed their minds about delaying or not accepting vaccination for their children listed “information or assurances from a healthcare provider” as the main reason [17]. In a qualitative study on vaccine hesitancy among healthcare workers in Europe, suggestions of medical personnel were most common reason for nonvaccination of children. Physicians unnecessarily used current child diagnosis as an excuse for omitting the vaccine which, either actively or passively, firmly influenced parents’ decision on vaccinating their child [16]. Although healthcare workers in Croatia, France, Greece, and Romania reported high levels of trust and confidence in the benefits of vaccination, they also showed some concerns about vaccines and the vaccination process. Moreover, physicians who practiced homeopathy or were entirely against vaccination did not recommend vaccination to their patients at all [18]. Furthermore, vaccination hesitancy among healthcare professionals regarding their recommended influenza vaccination may influence the opinion of parents and the general population about vaccination [19]. As revealed by previous studies in which parents were advised against vaccination, the medical staff was not convincing enough when explaining the vaccine benefits or the physicians made a negative impression on parents, which negatively influenced their decision to vaccinate their children [20, 21]. Thus, a negative attitude of healthcare professionals toward vaccination was not uncommon. Zimmerman et al. found that from a physicians’ perspective, the most common reasons for advising against vaccination were concerns about the vaccine side effects and potential vaccine litigation [22]. These examples represent an unnecessary delay of vaccination based on wrong assumptions.
In this study, neuropediatricians or neurophysiatrists along with pediatricians most commonly advised parents not to vaccinate their children. Moreover, more than one third of the parents received the same advice from pediatricians. Unlike these results, La Vela et al. and Livni et al. showed that healthcare professionals with a higher level of education are more likely to recommend vaccination than those who are less educated [23, 24]. Despite the education level and the availability of medical literature, healthcare professionals with pediatric subspecialties have doubts about the vaccination process. The European Centre for Disease Prevention and Control (ECDC) reported that, in some cases, healthcare workers along with their patients shared similar doubts about vaccination. In other cases, vaccine-hesitant patients influenced the beliefs of healthcare workers [18]. All of the above suggests that despite education level and the availability of medical literature, healthcare professionals, especially those with pediatric subspecialties, have doubts about the vaccination process.
Parents in the study had mixed opinions regarding vaccine safety. The number of those who doubted the source of vaccines along with their composition was almost equally proportional to those who believed that vaccines in B&H are safe and effective. While some studies have showed that parents decided to have their children vaccinated because they believed in the efficacy of vaccines and their ability to prevent the onset of the disease [25], previous studies have confirmed that the lack of confidence in the safety and efficacy of vaccines and the vaccination process were reasons for the nonvaccination of children [17].
In this study, around one third of the parents believed that delaying or missing the vaccination of their children has a medically justified reason. A study performed by Maayan-Metzger et al. reported that parents claimed that their physicians vaccinated their children without any prior screening [26]. This could be one of the reasons for the increasing number of vaccine refusals. Moreover, parents often refuse getting their children vaccinated because they think they are allergic to the vaccine [27]. However, without any real evidence of allergy, their suspicion is questionable.
Similar to the findings of Wolff’s study [28], the parents in this study had doubts on the safety of the vaccines because they knew someone who had an adverse reaction to them. While this claim is a completely unjustified reason for nonvaccination, the high number of individuals who support it is still a big concern for the vaccination process.
The present study found that the mandatory vaccination schedule in B&H could be better by improving the quality of communication between parents and healthcare professionals, i.e., sending a formal notice to parents by e-mailing or notifying them by phone about the dates of the vaccination. In previous studies, some parents missed the vaccination of their children because they forgot their appointment date [29, 30]. Parents believe that balanced information presented in a simple form, which includes both the advantages and disadvantages of vaccines, should be available. The current study shares a similar opinion to other papers that the lack of information on vaccination being often the main cause of their concern about vaccination [12].
In the light of the COVID-19 pandemic, there should be more effort to solve this problem. By having a good awareness of the efficacy of vaccines, hesitancy about them can be eliminated, namely to stop the spread of vaccine-preventable diseases. There is a rapid development of new COVID-19 vaccines that could stop its spread, but getting the vaccine itself is not enough to stop the pandemic. The cooperation of the population is also important so that the majority actually get vaccinated. Moreover, educating the parents of children with nonprogressive neurodevelopmental disorders about vaccination through a multidisciplinary approach, can improve the vaccination rate among this vulnerable group of children.
One of the limitations of this study is the small sample size due to the fact that only a limited number of children with neurodevelopmental disorders gravitate toward this medical center. Another is parents not participating in this type of study. Parents’ hesitation to participate in the study resulted in inadequately completed questionnaires in some cases, which should certainly be taken into account when interpreting the results. Another weakness in the study is the generalization problem, which arises from the fact that data were collected from a single medical center in B&H. Furthermore, it is necessary to expand the study to other medical centers in B&H to get a more representative sample.
Conclusions
The most common sources for parents of information on vaccination were physicians and the media. However, the majority of children with nonprogressive neurodevelopmental disorders in B&H remained unvaccinated. Parents mostly relied on the physician’s opinion on the vaccination of their children. Therefore, perhaps educating physicians on this topic could indirectly improve the vaccination coverage of this population of children. Among medical experts, neuropediatricians, neurophysiatrists, and pediatricians most commonly delayed the regular vaccination of children. Vaccination delay was not medically justified in most cases. According to parents, the mandatory vaccination system in B&H could be improved by sending a formal notice to parents and improving the communication between parents and healthcare professionals.
Footnotes
Acknowledgments
We thank the physicians and nurses at the Department for Physical Medicine and Rehabilitation of UCHM for their help during data collection.
Conflict of interest
None declared.
Ethical considerations
All procedures followed were in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki and its later amendments. As this was a descriptive study, every patient was informed and gave consent for data collection, and any potentially-identifying patient information was omitted.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial or profit sectors.
