Abstract
Muscle contraction requires specialized membrane structures with precise geometry and relies on the concerted interplay of electrical stimulation and Ca2+ release, known as excitation-contraction coupling (ECC). The membrane structure hosting ECC is called triad in skeletal muscle and dyad in cardiac muscle, and structural or functional defects of triads and dyads have been observed in a variety of myopathies and cardiomyopathies. Based on their function, the proteins localized at the triad/dyad can be classified into three molecular pathways: the Ca2+ release complex (CRC), store-operated Ca2+ entry (SOCE), and membrane remodeling. All three are mechanistically linked, and consequently, aberrations in any of these pathways cause similar disease entities. This review provides an overview of the clinical and genetic spectrum of triad and dyad defects with a main focus of attention on the underlying pathomechanisms.
Keywords
INTRODUCTION
Muscle contraction relies on the conversion of an electrical stimulus into mechanical work. In skeletal muscle, the sequence of events begins with the excitation of a motor neuron and the subsequent release of the neurotransmitter acetylcholine (ACh) into the neuromuscular junction. Binding of ACh to ACh receptors in the motor endplate triggers Na+ influx, generating a local depolarization of the membrane [1]. In cardiac muscle, membrane depolarization is not initiated by nervous activity, but by sinoatrial node (SAN) cells in the right atrium, spontaneously generating 60–100 action potentials per minute [2]. The action potential then spreads along the skeletal and cardiac muscle cells and deep into membrane invaginations known as T (transverse)-tubules [3]. Together with the terminal cisternae of the sarcoplasmic reticulum (SR), T-tubules form a specialized complex known as triad in skeletal muscle and dyad in cardiac muscle, hosting the excitation-contraction machinery (ECC, Fig. 1) [4]. In detail, ECC is driven by the multiprotein Ca2+ release complex (CRC), composed of the voltage-gated L-type Ca2+ channel dihydropyridine receptor (DHPR) on the T-tubule, and ryanodine receptor (RyR), triadin, calsequestrin, and junctin, all residing in the SR. In skeletal muscle, membrane depolarization at the T-tubules causes the conformational change of the α1 subunit of DHPR, encoded by CACNA1S, enabling its physical interaction with the Ca2+ channel RyR1 across the membrane gap between the T-Tubule and the SR [5]. This is different to cardiac muscle, where membrane depolarization triggers influx of extracellular Ca2+ through the cardiac α1 subunit of DHPR (CACNA1C), and the increased local Ca2+ levels then activate RyR2 via a mechanism known as Ca2+-induced Ca2+ release (CICR) [6]. Skeletal muscle and cardiac ryanodine receptors are homotetrameric Ca2+ channels, and the amount of released Ca2+ is regulated by a quaternary complex with junctin, calsequestrin and triadin [7]. Ca2+ release finally triggers shortening of the contractile unit, the sarcomere, composed of myosin and actin filaments and various structural and regulatory elements. The myosin head thereby binds to actin and performs a power stroke under ATP hydrolysis, resulting in a relative movement of the filaments and the generation of force [8]. Muscle relaxation occurs when Ca2+ is removed from the contractile unit through the combined action of Ca2+ pumps and Na+/Ca2+ exchangers [9]. Repeated contractions require the maintenance of high Ca2+ gradients and the strict regulation of luminal and cytosolic Ca2+ balance. Store-operated Ca2+ entry (SOCE) is a major mechanism regulating Ca2+ homeostasis, and essentially depends on the interaction of the reticular Ca2+ sensor STIM1 and the plasma membrane Ca2+ channel ORAI1. Upon Ca2+ depletion, STIM1 undergoes a conformational change and activates ORAI1 to induce extracellular Ca2+ influx, and Ca2+ store refill is then ensured by the reticular SERCA Ca2+ pumps [10–14].
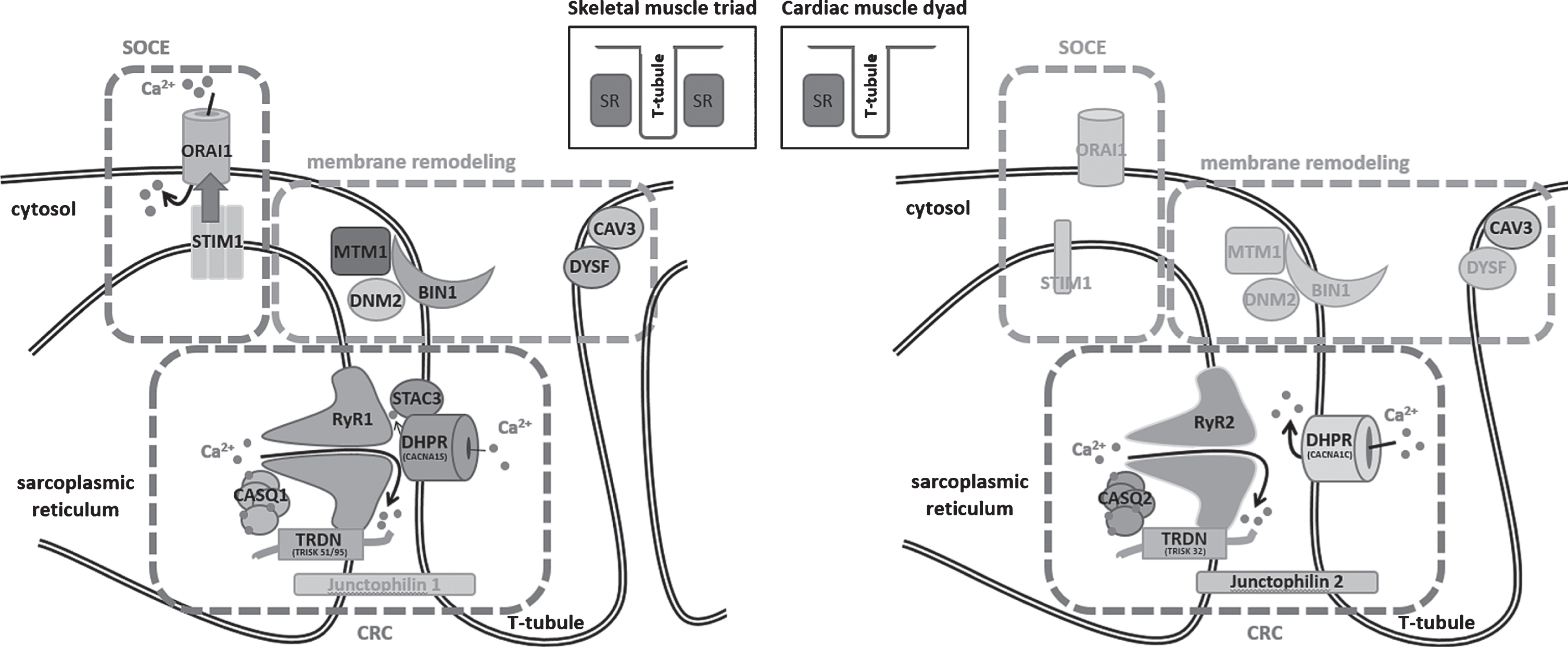
Schematic representation of the skeletal muscle triad and the cardiac muscle dyad and illustration of the fundamental key pathways. SOCE (store-operated Ca2+ entry) controls Ca2+ homeostasis through the combined activity of STIM1 and ORAI1, membrane remodeling depends on myotubularin (MTM1), amphiphysin 2 (BIN1), dynamin 2 (DNM2), caveolin-3 (CAV3), and dysferlin (DYSF), and the CRC (Ca2+ release complex) involves DHPR and the complex composed of ryanodine receptor (RyR), calsequestrin (CASQ), and triadin (TRDN), while junctophilin ties the sarcoplasmic reticulum with the T-tubule. Proteins marked in gray have not yet been associated with skeletal muscle or heart disorders.
Disturbances of Ca2+ homeostasis can severely impact on muscle physiology, and structural or functional triad or dyad defects give rise to various myopathies and cardiac disorders (summarized in Table 1). This review aims to provide a gene-by-gene overview of the mutations leading to defects of the Ca2+ release complex (CRC), store-operated Ca2+ entry (SOCE), or membrane remodeling. The mutations thereby often affect paralogue genes with tissue-specific expression in skeletal muscle and heart, emphasizing the parallelism of myopathies and cardiomyopathies. We mainly focus on myopathies, and we draw an analogy between the pathomechanisms underlying skeletal muscle and heart dysfunction.
Overview on the skeletal and cardiac muscle disorders, causative genes, and pathomechanisms associated with structural or functional triad and dyad defects
AD = autosomal dominant; AR = autosomal recessive; XL = X-linked; GOF = gain-of-function; LOF = loss-of-function.
CA2+ RELEASE COMPLEX (CRC) DISORDERS
Mutations in CACNA1S and CACNA1C
The dihydropyridine receptor (DHPR) is composed of the five equimolar α1, α2, β, δ, and γ subunits [15]. The voltage sensor and pore-forming subunit α1, encoded by CACNA1S in skeletal muscle and by CACNA1C in heart, contains four transmembrane domains (I–IV), and the cytoplasmic loop between domains II and III mediates the activation of the ryanodine receptor in skeletal muscle [16, 17]. CACNA1S mutations have been associated with different disorders such as malignant hyperthermia (MH, OMIM #601887) [18], hypokalemic periodic paralysis (HOKPP, OMIM #170400) [19], and recently also with a new congenital myopathy entity [20], while CACNA1C mutations have been reported in Brugada syndrome (BrS, OMIM #611875) [21] and in Timothy syndrome (TS, OMIM #601005) [22].
Malignant hyperthermia (MH) is triggered by volatile anesthetics, and major symptoms are uncontrolled contractures, muscle rigidity, hyperthermia, cardiac arrhythmia, hyperkalemia, and hypermetabolism [23, 24]. MH is potentially fatal if not rapidly treated with the muscle relaxant dantrolene. CACNA1S mutations account for less than 10 % of the MH cases, and to date only three different heterozygous missense mutations have been reported [18, 26]. It has been shown that these mutations increase the sensitivity of RyR1 to activation, leading to elevated resting Ca2+ levels in the cytosol [27, 28]. Muscle biopsies from MH patients were largely unremarkable and showed only minor alterations of the mitochondrial shape and also manifested mitochondrial breakdown, both potentially resulting from aberrant Ca2+ homeostasis in the muscle fibers [29]. Hypokalemic periodic paralysis is characterized by episodic and recurrent muscle weakness leading to paraparesis or tetraparesis lasting several hours to several days. The paralytic attacks are accompanied by hypokalemia, and treatment with the potassium channel opener acetazolamide has been shown to be beneficial [30]. A subset of HOKPP patients develop adult-onset myopathy, and the causative CACNA1S missense mutations affect a highly conserved arginine residue in the α1 voltage sensor domain [31]. Functional studies in the mouse model demonstrated that the loss of the positive charge impacts on the gating properties of the channel by causing an anomalous voltage-dependent inward current [32]. CACNA1S mutations were also associated with an unusual congenital myopathy with both dominant and recessive disease inheritance [20]. All patients had a comparable clinical presentation of generalized muscle weakness at birth, and the muscle biopsies exhibited cores, central nuclei, dilated triads, as well as a particular alveolar aspect of the intermyofibrillar network. DHPR stimulation resulted in significantly reduced reticular Ca2+ release in patient myotubes, suggesting an uncoupling of DHPR and RyR1 [20].
CACNA1C mutations have been found in patients with Brugada syndrome and Timothy syndrome. Brugada syndrome is a rare arrhythmia condition that can cause fast polymorphic ventricular tachycardia or ventricular fibrillation preceding sudden death [21]. The ECG pattern typically shows a persistent ST segment elevation with a right bundle branch block [21]. Heterozygous CACNA1C missense mutations only account for a subset of Brugada syndrome cases, and it has been shown that these mutations lead to decreased Ca2+ channel activity [21]. Timothy syndrome is a multi-systemic disorder combining a congenital heart disease - including patent ductus arteriosus, patent foramen ovale, ventricular septal defects, and tetralogy of Fallot - with immune deficiency, syndactyly, and cognitive abnormalities [22]. ECG typically reveals prolongation of the QT interval, leading to life-threatening arrhythmias. In contrast to Brugada syndrome, the Timothy syndrome mutations involve a gain-of-function and lead to sustained depolarizing L-type Ca2+ currents resulting from reduced channel inactivation [22].
Mutations in RYR1 and RYR2
The sarcoplasmic reticulum in skeletal and cardiac muscle is composed of structurally and functionally distinct domains, the junctional and the longitudinal SR. The junctional SR is primarily involved in Ca2+ release and hosts the ryanodine receptor (RyR). Each polypeptide of this homotetrameric protein is composed of more than 5000 amino acids forming six transmembrane domains. The C-terminal end of the RyR protein constitutes the Ca2+ channel, and the N-terminal cytoplasmic protrusion spans the narrow gap separating the junctional SR from the T-tubule [33–37]. Heterozygous missense mutations in RYR1 which account for the majority of molecularly diagnosed MH cases, render the channel hypersensitive to triggering agents, and lead to excessive Ca2+ release from the SR [38, 39]. Mutations in RYR1 have also been found to cause King-Denborough syndrome (OMIM #145600) [40], central core disease (CCD, OMIM #117000) [41, 42], multi-minicore disease (MmD, OMIM #255320) [43], centronuclear myopathy (CNM), congenital fiber type disproportion (CFTD), and the Samaritan myopathy [44], underlining the phenotypic variability arising from mutations in RYR1. RYR2 mutations have been described in the allelic diseases catecholaminergic polymorphic ventricular tachycardia (CPVT, OMIM #604772) [45] and arrhythmogenic right ventricular dysplasia 2 (ARVD2, OMIM # 600996) [46].
King-Denborough syndrome is a congenital myopathy associated with skeletal abnormalities, dysmorphic features, and susceptibility to malignant hyperthermia [47]. Muscle biopsies show a variety of myopathic features including atrophy, internalized nuclei, or cores [48]. It is not understood how the identified RYR1 mutations cause King-Denborough syndrome, but they reside in the same regions as MH mutations, indicating that both disorders might share a common pathomechanism [48].
Central core disease has been named after the central areas with reduced oxidative activity and a variable degree of sarcomeric disorganization running along the longitudinal muscle fiber axis. Clinically, CCD can be stable over long periods and typically presents with childhood-onset hypotonia, proximal muscle weakness, mild facial weakness, joint hypermobility, and scoliosis [49]. CCD is mainly caused by heterozygous missense mutations affecting amino acids in the C-terminal pore-forming domain of RyR1, and more severe cases with a fetal akinesia syndrome involving arthrogryposis and skeletal deformities have been described with recessive disease inheritance [50]. A subset of RYR1 mutations were found to generate a leaky channel leading to Ca2+ store depletion, others alter the interaction with DHPR and thereby uncouple excitation from contraction. In both cases, the amount of released Ca2+ upon depolarization is reduced [51–53].
Multi-minicore disease results from recessive RYR1 mutations dispersed over the entire gene, and is usually associated with an earlier disease onset and more severe clinical features with additional extraocular muscle involvement compared to CCD [43]. Biopsies from MmD patients display multiple areas of reduced mitochondrial activity and sarcomeric organization, and these minicores only span a limited zone on the longitudinal axis of the muscle fiber. Most MmD cases arise from missense mutations, but nonsense and splice site mutations have also been described. Patients with a clinicopathologic diagnosis of centronuclear myopathy (CNM) were found to carry recessive RYR1 missense or truncating mutations as well [54]. The affected individuals had an antenatal disease onset and were severely hypotonic at birth. Similarly to MmD, the patients had delayed motor milestones and showed facial weakness with extraocular muscle involvement. The muscle biopsies displayed cores as well as centralized nuclei, demonstrating a phenotypic overlap of RYR1-related MmD and CNM. Another muscle disorder associated with recessive missense and truncating RYR1 mutations is congenital fiber type disproportion (CFTD) [55]. The clinical presentation of the CFTD patients is comparable to RYR1-related MmD and CNM, and the muscle biopsies showed significantly smaller type I fibers as the main histological hallmark, whereas cores and centralized nuclei were not observed. The Samaritan myopathy is a unique form of multi-minicore disease, as it is characterized by an “inverse” course of disease: affected individuals present with a severe muscle phenotype at birth, but hypotonia and muscle weakness gradually improve and adults are only mildly affected [56]. This disease is caused by a single homozygous missense mutation in RYR1 and has only been described in the Samaritans, considering themselves as descendants of one of the twelve tribes forming the ancient kingdom of Israel in the 8th century BCE. In both multi-minicore disease and Samaritan myopathy, the RyR1 protein level was found to be strongly reduced in muscle extracts from affected individuals [44, 57], and siRNA-mediated downregulation of RYR1 in myotubes led to reduced CACNA1S expression and a disruption of the spatial organization of the EC coupling machinery, while IP3R was upregulated [58]. These findings illustrate that RyR1 deficiency alters the expression pattern of genes involved in Ca2+ homeostasis, and indicate that the upregulation of the alternative Ca2+ regulating IP3R system might be a compensatory mechanism.
Catecholaminergic polymorphic ventricular tachycardia is an arrhythmogenic disorder caused by heterozygous RYR2 mutations in more than 50% of the cases [45]. CPVT patients have a structurally normal heart and a normal resting ECG. Physical activity or stress can induce an increase of monomorphic and then polymorphic premature ventricular contractions (PVCs), followed by polymorphic ventricular tachycardia and ventricular fibrillation, possibly leading to syncope or sudden death [59]. It was shown that the RYR2 mutations alter the sensitivity of the channel, which tends to spontaneous Ca2+ release under conditions of reticular Ca2+ overload (SOICR, store-overload-induced Ca2+ release) [60, 61]. The mutations thereby do not appear to impact on ECC, as arrhythmias are not observed in unstimulated conditions. Dantrolene was shown to rescue arrhythmogenic RyR2 defects in cellular CPVT models, indicating a common pathomechanism for CPVT and malignant hyperthermia [62, 63]. Another heart disease caused by dominant RYR2 mutations is arrhythmogenic right ventricular dysplasia 2 (ARVD2), characterized by fibrous fatty replacements of the myocardium and in particular in the subepicardial layer of the right ventricle [46]. Physical effort can induce polymorphic ventricular tachycardia, representing a risk of sudden death. The ARVD2 mutations were shown to alter the RyR2 response to caffeine, resulting in an abnormal Ca2+ release [64]. The missense mutations causing either CPVT or ARVD2 are conjointly clustered in distinct N-terminal, central, and C-terminal regions of RyR2.
Mutations in STAC3
STAC3 is a recently discovered component of the excitation-contraction machinery, and mutations in STAC3 have been associated with the debilitating Native American myopathy (NAM, OMIM #255995) [65]. This autosomal recessive disorder was first reported in the Lumbee Indian tribe in North Carolina and is characterized by neonatal muscle weakness and arthrogryposis, dysmorphic facial features, and susceptibility to malignant hyperthermia with high mortality rate in childhood and adolescence [66]. Muscle biopsies from affected individuals revealed a non-specific myopathic pattern [65]. STAC3 possesses a functional interaction site for both the skeletal muscle and cardiac α1 subunit of DHPR, and promotes the localization of DHPR at the triad membrane [67, 68], demonstrating the importance of STAC3 in the regulation of excitation-contraction coupling. Indeed, the NAM STAC3 missense mutation was shown to reduce ECC [67], and the same observation was also made in myotubes from Stac3 knockout mice and morpholino-induced knockdown of stack3 in zebrafish embryos [65, 67].
Mutations in JPH2
The junctophilins are components of the junctional membrane complex (JMC), which physically and functionally connects the T-tubule with the SR to maintain the triad and dyad architecture [69]. The cardiac paralogue junctophilin 2 is encoded by JPH2, and mutations in this gene have been associated with hypertrophic cardiomyopathy (CMH17, OMIM #613873), one of the most common causes for sudden cardiac death in young athletes [70]. The JPH2 mutations were found to cause junctophilin 2 mislocalization, impaired Ca2+ handling, and cardiomyocyte hypertrophy in the cellular model. A murine model manifested pacing-induced spontaneous Ca2+ sparks followed by atrial fibrillations, indicating that junctophilin 2 also has a regulatory role on RyR2 [71].
Mutations in the ryanodine receptor effectors TRDN, CASQ1, and CASQ2
Triadin physically links the ryanodine receptor with calsequestrin [7], and recessive TRDN mutations cause catecholaminergic polymorphic ventricular tachycardia (CPVT, OMIM #615441) [72], a major cause of sudden death. All CPVT mutations were found in exons present in both the skeletal muscle and the cardiac isoform, and resulted in triadin protein loss. Accordingly, a subset of TRDN patients manifested an additional skeletal muscle disorder [73], and ablation of triadin in murine knockout models resulted in cardiac and skeletal muscle phenotypes [74, 75]. The hearts of the mice displayed lower expression levels of RYR2, CASQ2, and ASPH (junctin), abnormal contact sites between the T-tubules and the SR, as well as reticular Ca2+ overload resulting in spontaneous Ca2+ release (SOICR) and cardiac arrhythmias [74]. This emphasizes the importance of triadin in the structural and functional integrity of the cardiac Ca2+ release units. Physiological studies on skeletal muscle revealed an important reduction in muscle strength, and ultrastructural investigations uncovered abnormally oriented T-tubules, strongly suggesting that ECC is impaired [75].
Calsequestrin is the major Ca2+ storage protein in the sarcoplasmic reticulum. It binds Ca2+ with moderate affinity (Kd ∼ 103 M–1) and high capacity (40–50 ions/protein), and forms higher-order polymers with increasing Ca2+-binding capacities [76]. Calsequestrin also actively participates in the Ca2+ release process by providing a large Ca2+ pool in close proximity to the RyR release channel [77]. Heterozygous CASQ1 missense mutations were found in vacuolar myopathy (OMIM #616231) [78] and in tubular aggregate myopathy (TAM) [79, 80], both involving mild muscle weakness, but differing at the histopathological level. Vacuolar myopathy biopsies show vacuoles containing diverse SR proteins and enlargement of the terminal SR cisternae [78], while TAM muscle fibers typically accumulate densely packed membrane tubules [81]. Both disorders arise from adverse mutational effects: the TAM-related CASQ1 mutations were shown to significantly impair calsequestrin polymerization, resulting in reduced Ca2+ storage abilities of the SR, while the vacuolar myopathy mutation promoted the formation of high molecular mass polymers [78–80]. Noteworthy, Casq1 null mice exhibit a susceptibility to heat- and anesthetics-induced sudden death resembling malignant hyperthermia [82]. Recessive mutations in the cardiac paralogue CASQ2 have been associated with catecholamine-induced polymorphic ventricular tachycardia (CPVT, OMIM #114251) [83]. Whilst dominant RYR2 mutations are found in about half of the CPVT patients, recessive mutations in CASQ2 and TRDN are more seldom and account for less than 5% of the cases. Patients with CASQ2 mutations exhibit a childhood-onset relative resting bradychardia and a mild prolongation of the QTc segment, with Holter monitoring showing polymorphic ventricular tachycardia during exercise [83, 84]. In line with the functional impact of CASQ1 mutations, it was shown that the CASQ2 missense mutations alter the polymerization dynamics of calsequestrin, resulting in reduced Ca2+ binding capacities [85]. It has been proposed that the reduced Ca2+ buffering leads to a higher level of unbound Ca2+ in the SR with an increased risk for SOICR [86]. Indeed, mouse models harboring human CASQ2 mutations displayed stress-induced spontaneous Ca2+ release leading to ventricular tachycardia [87].
STORE-OPERATED CA2+ ENTRY (SOCE) DISORDERS
Upon stimulation of the ryanodine receptor, Ca2+ is released to the cytoplasm to trigger muscle contraction and to regulate various signaling pathways. The Ca2+ stores are refilled through store-operated Ca2+ entry (SOCE), an essential mechanism for prolonged tetanic stimulation that limits the effects of fatigue. The key players of SOCE are the reticular Ca2+ sensor STIM1 and the plasma membrane Ca2+ channel ORAI1. STIM1 contains an intraluminal region with Ca2+-sensing EF-hands, and a cytosolic part able to interact with ORAI1 [13, 88]. Ca2+ store depletion initiates STIM1 unfolding, oligomerization, and accumulation of the oligomers at the SR/plasma membrane junctions, where they bind and activate ORAI1 and thereby induce Ca2+ entry [11, 89–92]. Ca2+ reuptake to the SR is ensured by the ATP-dependent SERCA pumps.
Mutations in STIM1
Heterozygous missense mutations in STIM1 were found in patients with tubular aggregate myopathy (TAM, OMIM #160565), a rare muscle disorder involving weakness, cramps, and myalgia, which is characterized by the presence of densely packed membrane tubules on biopsies [93]. TAM clinically and genetically overlaps with Stormorken syndrome (STRMK, OMIM #185070), a multi-systemic disorder associating TAM with miosis, thrombocytopenia, ichthyosis, asplenia, dyslexia, and short stature [94, 95]. Although TAM and STRMK form a clinical continuum, the Ca2+-binding EF-hand domains appear to be a mutation hotspot in TAM patients [93, 96–100], while the full clinical picture of Stormorken sydrome essentially arises from a substitution of a single amino acid in the cytosolic domain of STIM1 [101–103]. Nevertheless, TAM and STRMK mutations were both shown to induce constitutive STIM1 oligomerization and ORAI1 activation without SR Ca2+ depletion in the cellular model, and accordingly, TAM and STRMK myoblasts featured increased basal Ca2+ levels in the cytosol [93, 100–103]. The multi-systemic phenotype of Stormorken syndrome might result from a different mutational impact on Ca2+-dependent inactivation (CDI) of the ORAI1 Ca2+ channel. Electrophysiological studies on transfected cells demonstrated that the STRMK mutation especially suppresses CDI, suggesting a prolonged Ca2+ influx compared to TAM [103]. SOCE is not restricted to skeletal or cardiac muscle, but instead regulates Ca2+ homeostasis in various tissues, explaining the broad phenotypical presentation of Stormorken syndrome. A recently generated mouse models harboring the STRMK mutation recapitulated the main clinical features of the human disorder [104]. The mice were smaller than the control littermates, and displayed muscle weakness, thrombocytopenia, spleen dysplasia, skin irritations, and abnormal Ca2+ homeostasis in the myotubes.
Mutations in ORAI1
ORAI1 is a highly Ca2+-specific plasma membrane channel composed of hexamers forming three concentric rings around the central pore, and each ORAI1 subunit contains 4 alpha-helical transmembrane domains [105, 106]. Channel opening is mediated through the interaction of STIM1 with the cytoplasmic N- and C-termini of the ORAI1 subunits [107]. Similarly to STIM1, heterozygous missense mutations in ORAI1 cause TAM with additional signs of Stormorken syndrome (OMIM #615883). All mutations affect highly conserved amino acids in the transmembrane domains [103, 108–110]. Exogenous expression of mutant ORAI1 resulted in elevated basal Ca2+ levels and significant Ca2+ influx in the absence of Ca2+ store depletion [108–110], and similar results were also obtained in patient myotubes [109, 110]. Mutations in the first transmembrane domain were especially shown to cause a long-lasting Ca2+ influx, correlating with a more severe disease phenotype [108].
MEMBRANE REMODELING DISORDERS
Remodeling of membranes is essential for normal muscle function [111]. The skeletal muscle triad and the cardiac dyad are specialized membrane structures with precise geometry, and the mechanical stress exerted by steady contractions require efficient membrane repair mechanisms. Consequently, defects in proteins acting in membrane trafficking and remodeling result in muscle disorders. The triad and dyad formation and maintenance are coordinated by the concerted action of various proteins including myotubularin, amphiphysin 2, dynamin 2, caveolin, and dysferlin, and mutations in any of the respective coding genes lead to structural T-tubule defects in animal models and humans [112].
Mutations in MTM1
Myotubularin, encoded by MTM1, is a 3-phosphatase dephosphorylating the phosphoinositides PtdIns3P and PtdIns(3,5)P2 [113], which confer a local signature to the membrane and play a key role in the recruitment of proteins, in endocytosis, and in membrane trafficking [114, 115]. MTM1 mutations cause X-linked myotubular (or centronuclear) myopathy (XLMTM, OMIM #310400), a severe and generalized neonatal muscle disorder predominantly affecting boys and involving atrophic muscle fibers, type I fiber predominance, centralized nuclei, and sometimes basophilic rings known as necklace fibers on muscle biopsies [116, 117]. Women can also be affected, especially in case of skewed X-inactivation, but the clinical presentation is often milder [118]. More than 280 different causative XLMTM mutations have been reported, and most are nonsense mutations, splice-site mutations, or deletions, and result in a strong reduction of the myotubularin protein level and the dysregulation of the phosphoinositide metabolism [119, 120]. Mice, dogs, or zebrafish devoid of myotubularin exhibited a disorganization of the triad structure, reduced levels of RyR1 and DHPR, and defects in excitation-contraction coupling [121–123].
Mutations in BIN1
Amphiphysin 2, encoded by BIN1, is able to sense and induce membrane curvature in endocytosis and recycling. It interacts with dynamin 2, and connects the actin and microtubule cytoskeleton to the nuclear envelope LINC (linker of nucleoskeleton and cytoskeleton) complex [124–126]. The skeletal muscle-specific isoform of amphiphysin 2 contains a phosphoinositide-binding domain and plays a role in T-tubule biogenesis [127]. BIN1 mutations cause either dominant (ADCNM) [128] or recessive (ARCNM, OMIM #255200) [129] centronuclear myopathy, and both disorders presumably involve a different pathomechanism. ARCNM occurs as a severe childhood-onset disorder predominantly affecting the proximal muscles, and the biopsies display atrophy, type I fiber predominance, and nuclear centralization and clustering [129, 130]. ADCNM is clinically milder, has been described with adulthood-onset muscle weakness, and the biopsies of affected individuals exhibit nuclear centralization and clustering as well as ultrastructural triad abnormalities [128]. Comparative functional studies have shown that both dominant and recessive BIN1 mutations prevent membrane tubulation and interfere with protein-protein interactions, and that only the defects caused by the recessive mutations can be rescued by wild type amphiphysin 2 [128]. This is in accordance with the observation that heterozygous carriers of recessive BIN1 mutations are healthy.
Mutations in DNM2
Dynamin 2 is a mechanochemical enzyme involved in membrane fission and acting as a key player for vesicle formation and membrane trafficking at the plasma membrane and the trans-Golgi network [131, 132]. It binds PtdIns(4,5)P2, interacts with amphiphysin 2, and is able to self-assemble into rings [132–135]. Heterozygous missense mutations restricted to hotspots in the MID (middle), PH (phospholipid binding), and GED (GTPase effector) domains have been found in patients with autosomal dominant centronuclear myopathy (ADCNM, OMIM #160150) [136, 137]. The clinical presentation thereby correlates with the position of the mutation, and ranges from severe neonatal hypotonia and respiratory insufficiency to adult-onset distal muscle weakness and mild eye movement defects [138]. Histological findings on muscle biopsies include myofiber atrophy, central nuclei, type I fiber predominance, as well as prominent fiber size variability and radial arrangements of sarcoplasmic strands [130, 138]. Biochemical studies indicated that the DNM2 mutations increase dynamin 2 oligomer stability and GTPase activity [139, 140], and in vivo investigations suggested that dynamin 2 is negatively regulated by myotubularin and amphiphysin 2 [141, 142]. Knock-in mice harbouring the most common human mutation R465W manifested a mild myopathy with a structural disorganization of the muscle fibers, abnormal contractile properties, and elevated basal Ca2+ concentrations in the cytosol [143, 144]. AAV-mediated expression of the same mutation resulted in abnormal T-tubule structures and a swollen sarcoplasmic reticulum [145], and expression of the severe S619L mutation in zebrafish revealed defective excitation-contraction coupling [146].
Mutations in CAV3
Caveolin-3 is the principal protein component of caveolae in muscle. Caveolae are cholesterol and sphingolipid-rich invaginations of the plasma membrane playing an important role in signal transduction and vesicular transport [147]. Caveolin-3 belongs to the dystrophin-glycoprotein complex conferring stability to the sarcolemma [148], and also localizes to the developing T-tubules during muscle differentiation [149]. Mutations in CAV3 give rise to various skeletal and cardiac muscle disorders including rippling muscle disease 2 (RMD2, also known as limb-girdle muscular dystrophy 1C, OMIM #606072) [150, 151], Tateyama distal myopathy (OMIM #614321) [152], long QT syndrome 9 (LQT9, OMIM #611818) [153], and familial hypertrophic cardiomyopathy (CMH, OMIM #192600) [154]. RMD2 is a childhood-onset muscle disorder characterized by mild to moderate proximal muscle weakness, cramps, myalgia, visible ripples moving over the muscle following mechanical stimulation, and elevated CK levels, and muscle biopsies from affected individuals display dystrophic changes and almost complete loss of caveolin-3 expression [150, 155]. Tateyama distal myopathy mainly affects the small muscles of the hands and feet, and the very same CAV3 mutation can cause RMD2 or Tateyama myopathy, suggesting that both disorders are part of a clinical continuum [151, 152]. Long QT syndrome 9 is characterized by a prolonged QT interval and polymorphic ventricular arrhythmias potentially causing syncope, seizure, or sudden death, and the causative CAV3 mutations were shown to induce an increased late sodium current [153]. Hereditary ventricular hypertrophy is an idiopathic cardiomyopathy that manifests with diastolic dysfunction of the cardiac ventricles, and can entail arrhythmia, congestive heart failure, and sudden death. As for the skeletal muscle disorders, the CMH-related CAV3 mutation resulted in a strongly reduced cell surface expression of caveolin-3 [154]. Mice lacking caveolin-3 showed a RMD2-like mild myopathy, and investigations of the skeletal muscle revealed disorganized T-tubule [156], highlighting the importance of caveolin-3 in T-tubule biogenesis.
Mutations in DYSF
Dysferlin plays a crucial role in the process of membrane repair, and co-localizes with caveolin-3 at the site of the injury [157, 158]. It is also found in the cytoplasm, and localizes with DHPR in the developing T-tubule system [159]. Mutations in DYSF have been associated with Miyoshi muscular dystrophy (MMD, OMIM #254130) [160], limb-girdle muscular dystrophy 2B (LGMDR2, formerly LGMD2D, OMIM #253601) [160], and distal myopathy with anterior tibial onset (OMIM #606768) [160]. Miyoshi muscular dystrophy is an early-adult-onset disorder involving distal muscle weakness of the upper and lower limbs with sparing of the intrinsic hand muscles [161]. Serum creatine kinase levels are increased, and biopsies show a dystrophic pattern with necrosis. LGMDR2 patients generally present with a less distal muscle involvement, and distal myopathy with anterior tibial onset has been described in a single consanguineous family with a rapidly progressive course [160]. However, Miyoshi, LGMDR2, and distal myopathy biopsies are similar, and all three disorders can arise from identical DYSF mutations resulting in strong reduction of dysferlin [160]. They are therefore often conjointly referred to as dysferlinopathies. Dysferlin-deficient mice developed a progressive muscular dystrophy closely resembling the human disease, and histological and ultrastructural analyses of muscle samples revealed T-tubule anomalies similar to what has been seen in Cav3 null mice [157].
LINK BETWEEN CRC, SOCE AND MEMBRANE REMODELING
CRC, SOCE and membrane remodeling are mechanistically interconnected, as CRC and SOCE concur and require the formation and maintenance of specialized membrane structures. This explains why defects in these key pathways cause similar disease entities. It was proposed that amphiphysin 2 is essential for the microtubule-dependent transport of DHPR to the T-tubules in heart [162], and accordingly, Bin1 knockdown in murine cardiomyocytes resulted in decreased surface DHPR, leading to impaired Ca2+ transients [163]. Mtm1-deficient mice displayed a reduction in protein levels and an abnormal localization of RyR1 and the α1 subunit of DHPR, most probably contributing to the altered triad structure and the defective Ca2+ transients observed in the animals [121, 164]. DHPR also interacts with dysferlin and caveolin-3, and it has been suggested that the formation of this oligomeric complex plays a role in the fusion of caveolin-3-containing vesicles with T-tubules [159].
Phosphoinositides are critical for triad and dyad structure, excitation-contraction coupling, as well as SOCE. The membrane repair capacities of dysferlin largely depend on its Ca2+-dependent binding of PtdIns4P and PtdIns(4,5)P2 [165], and the latter is also crucial for the recruitment of amphiphysin 2 and dynamin 2 to the membrane [133, 166]. PtdIns(3,5)P2 modulates skeletal muscle and heart contractibility through activation of RyR1 and RyR2 [167–169], and increased levels of PtdIns(3,5)P2 were shown to induce chronic Ca2+ leakage from the sarcoplasmic reticulum, and promoted the degradation of DHPR [167, 170]. Other studies highlighted the importance of phosphoinositides in SOCE: STIM1 interacts with PtdIns(4,5)P2 through its polybasic C-terminus, and inhibition of phosphatidylinositol 4-kinase prevents the formation of STIM1 oligomers at the plasma membrane [171]. The inhibition of phosphatidylinositol 4-kinases but not isolated PtdIns(4,5)P2 depletion also significantly reduced store-operated Ca2+ entry, indicating that PtdIns4P is a determinant for SOCE activation [172]. STIM1 was also found to bind the α1 subunit of DHPR in cardiac cells and to suppress the depolarization-induced channel opening [173]. In turn, STIM1 is negatively regulated by low polymeric forms of calsequestrin, which interfere with STIM1-ORAI1 interactions [174], demonstrating a reciprocal regulation of CRC and SOCE and the importance of the membrane structures these pathways rely on.
CONCLUSIONS
Cardiac and skeletal muscle contraction rely on similar membrane structures and the coordinated action of identical or evolutionary related proteins. Although a variety of cardiac and skeletal muscle disorders arise from structural or functional dyad or triad defects, only mutations affecting the Ca2+ release complex were found in malignant hyperthermia and in both cardiopathies and congenital myopathies. Mutations in CACNA1C, RYR2, and CASQ2 cause life-threatening arrhythmias primarily resulting from spontaneous SR Ca2+ release following exercise, and mutations in the skeletal muscle paralogues CACNA1S, RYR1, and CASQ1 cause muscle weakness resulting from reduced Ca2+ release upon ECC activation. With CAV3 as the only exception, mutations in genes implicated in membrane remodeling or SOCE were found in patients with congenital myopathies, but weren’t associated with hyperthermia or heart diseases. Noteworthy, mutations in the SOCE genes STIM1 and ORAI1, as well as in the membrane remodeling genes BIN1 and DNM2 mostly involve amino acid substitutions, and do not result in total protein loss [93, 137]. Knockout animal models for these genes exist, and some of them displayed cardiac defects. Cardiomyocyte-restricted knockout of Stim1 in mice resulted in a progressive decline of left ventricular function and the development of a dilated cardiomyopathy [175], and inactivation of the zebrafish orthologue of ORAI1 entailed reduced ventricular systolic function, bradycardia, and heart failure [176]. A critical role of STIM1 and ORAI1 has also been suggested in the pathogenesis of cardiac hypertrophy in humans [177]. Mice with heart-specific Bin1 deletion exhibited decreased T-tubule folding at the dyad and were susceptible to ventricular arrhythmias resulting from prolonged action potential duration [178]. In zebrafish hearts, bin1 knockdown significantly reduced Ca2+ transients and led to severe ventricular contractile dysfunction [163], and in humans, BIN1 expression was shown to be significantly decreased in failing cardiomyocytes [163]. Lastly, mice with dysferlin deficiency developed a mild cardiomyopathy that was exacerbated by stress exercise [179]. These examples demonstrate that SOCE and membrane remodeling are critical for normal skeletal and cardiac muscle function, and that mutations in the genes encoding key proteins of these pathways might account for molecularly yet uncharacterized heart diseases [121, 162–174].
Footnotes
ACKNOWLEDGMENTS
We thank Valérie Biancalana for her comments and suggestions. This work was supported by Inserm and Association Française contre les Myopathies (AFM 21267).
