Abstract
Collagen is a fibrillar protein that conforms the conjunctive and connective tissues in the human body, essentially skin, joints, and bones. It is one of the most abundant molecule in many of the living organisms due to its connective role in biological structure. It is a highly versatile material, extensively used in the medical, dental, and pharmacological fields. Collagen is capable of being prepared into cross-linked compacted solids or into lattice-like gels. The collagen family consists of at least 30 different genes, which produce 19 known types of collagen. All collagens contain greater or lesser stretches of triple helix. Some of the superior properties of collagen-based biomaterials, such as biocompatibility, biodegradability, mechanical properties, and cell activities, are pinpointed. These properties make collagen applicable in biomedicine, such as wound healing, tissue engineering, surface coating of medical devices, and skin supplementation.
The purpose of this article is to review the available literature on collagen with special emphasis on its role in development and maintenance of oral tissues. Also it reviews the types of collagen, it’s structure, sources, role in maintaining periodontal tissues and uses in dentistry.
Introduction
Collagen is a superabundant fibrous protein that constitutes most of the extracellular matrix (ECM) in all animals [1, 2]. The semantic origin of the term “collagen” is originated from the Greek term “Kolla,” which means glue [3]. This biological polymer is the main component of connective tissues, corresponding to more than 30% by weight of the total proteins in the animal body, and acts as an intracellular glue by inhibiting tissues from stretching or damaging. Overall, collagen guarantees tissues and organs’ structural integrity, including skin, blood vessels, tendons, cartilage, and bones [4, 5].
Although several review papers have been published about biomedical applications of collagen, this manuscript presented a more comprehensive one that covers the types of collagen, it’s structure, sources, role in maintaining periodontal tissues and uses in dentistry.
Definition and structure of collagen
According to Protein Data Bank, Collagen is the most abundant structural protein in the human body that gives support to various tissues such as tendons, skin, and teeth (collagen joined to mineral crystals). All proteins that have a structure based on three helix polypeptidic chains [6] (Fig. 1) belong to the collagen family, being identified 26 types until now [7].
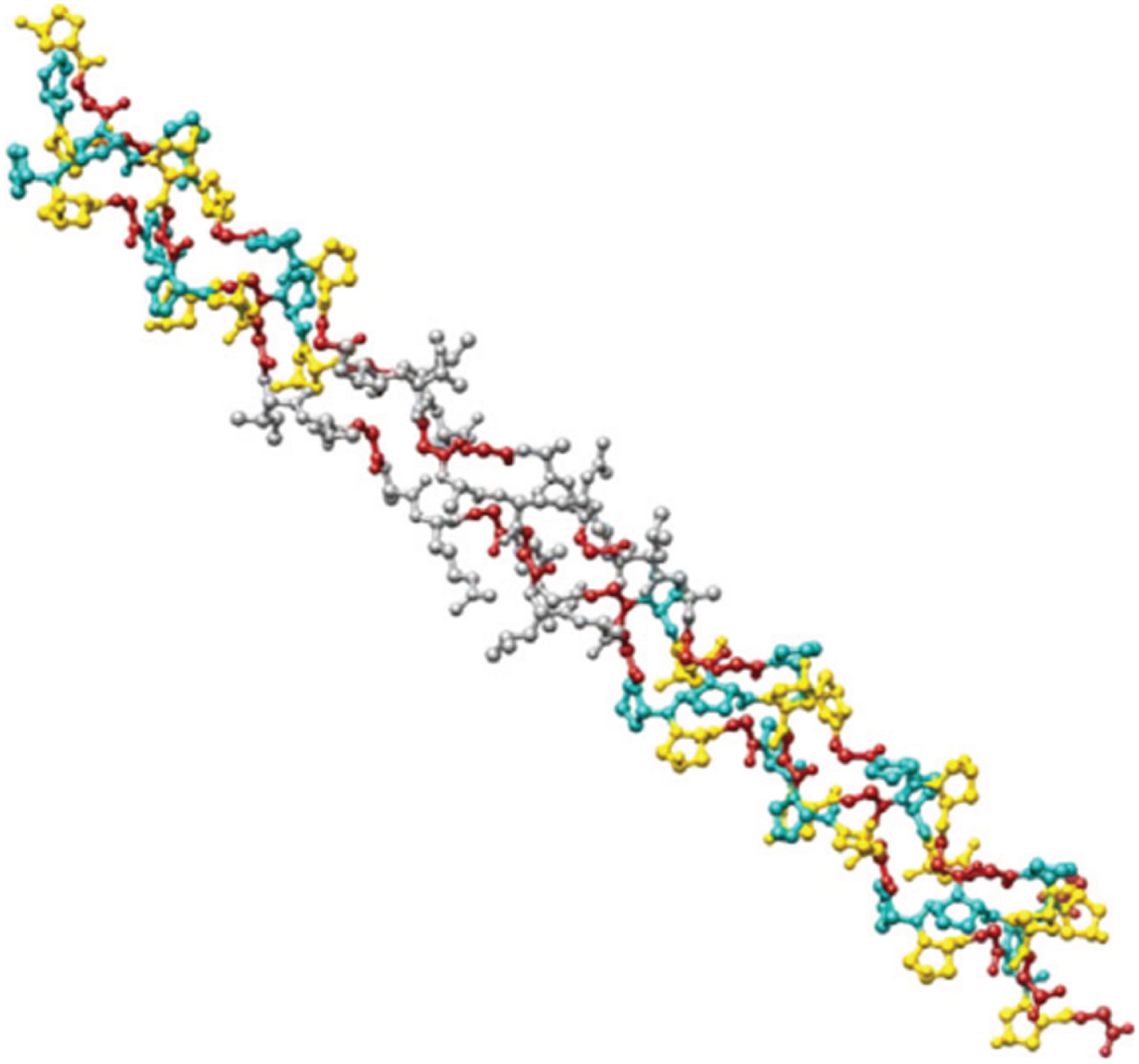
Collagen triple-helix structure [17].
The three polypeptidic fibrils can have a diameter of 10–500 nm [8], an approximate molecular weight of 285 kDa [9], with a length of 1400 amino acids that will characteristically have a glycine every three residues [10, 11], aspects that give its characteristic fibrillar helicoidal structure.
Collagen fibers are commonly white, opaque, and readily recognized in tissues. It is considered as a viscoelastic material that possesses high tensile strength and low extensibility. Its isoelectric point is around pH 5.8 [12]; and in terms of temperature, the shrinkage temperature (Ts) of most mammalian fibrils is between 62°C and 65°C, whereas fish fibrils Ts ranges from 38°C to 54°C. On the other hand, the denaturation temperature Tm is less by 25°C–30°C than Ts [13].
It is known that collagen is a molecule with low immunogenicity, diminishing the possibilities of not being accepted when ingested or injected to a foreign body. The only fractions capable of occasioning immune response are located in the helical region of the chains and in the telopeptide region [14].
Even though this molecule has low antigenicity, it can be modified to eliminate any immune response. An alternative can be carried out by the elimination of banded structure through heat or chemical treatment [15] degradation of nonhelical section by proteinases or cross-linking [16].
Collagen is produced from both natural and synthetic resources. Natural collagen can collect from animal and herbal sources [18]. The most common animal sources of collagen are bovine, porcine, human collagen, and marine organisms such as scale fish and fish skin. Other landed animal sources include chicken, kangaroo tail, rat tail tendons, duck feet, equine tendon, alligators’ bone/skin, bird’s feet, sheepskin, and frog skin. Although these sources are low cost and easy to collect after extended use can be allergenic and raise several diseases. Marine collagen is another possible natural source that seems not to have disease transmission [19].
Synthetic collagen sources are raised in order to prevent immune problems with natural collagen [20]. One example of these sources is a material commercially named KOD. It is a 36 amino acid synthetic protein that self-assembles into triple-helix nanofibers and hydrogels [21]. By the advantage of recombinant technology, another synthetic source for collagen has been established to provide high-quality and animal-derived contaminant-free collagens [22].
Classification of collagen types
According to Kielty and Grant [23], 25 different gene sequences have been discovered encoding for collagenous polypeptides giving rise to 13 distinct collagen types, which can be divided into three groups:
The first, most abundant group is the fibrous collagens. These are in the form of uninterrupted helices that are highly conservative and are mainly I, II, III, V, and XI. The second group is the high molecular weight collagen, comprising of numerous intervening non-helical sequences, in association with the basement membrane. Types IV and VII. The third group is a short-chain, nonhelical domain, and consists of types VI, VIII, IX, X, XII, and XIII [24–26].
Type I collagen
It is the major protein component of most connective tissues. The biosynthesis and fibrillogenesis of type I collagen within PDL could be determined by studying its posttranslational modifications. It comprises two identical α1 chains and a α2 chain which is low in hydroxylysine and glycosylated hydroxylysine. Collagen type II is a short-chain molecule that has only recently been located in the PDL (Romanos et al.) [24, 27].
Type III collagen
The periodontal ligament is rich in type III collagen (about 20%) which is covalently linked to type I collagen relatively high in hydroxyproline and cysteine whereas low in hydroxylysine. It is found in the periphery of Sharpey’s fiber attachments into the alveolar bone and around nerves and blood vessels, the function, however, is unknown.
Other types of collagen
Minute amounts of type IV, V, VI, and VII collagen have been found in the ligament. Type IV and VII collagen forms the major fraction of basal lamina protein of the blood vessels [27], the neurovascular bundles and epithelial rests of PDL. It does not form fibrils and helps maintain the structure and integrity of the PDL [28].
Type V is believed to be associated with the cell surface and coats the type III and type I fibrils. Type VI is a component of oxytalan fibers though not directly associated with the major fibrils. It may play a role in maintaining the integrity and elasticity of the ECM [29].
Type XII collagen helps organize the ECM architecture of dense connective tissues12 and occurs only when the ligament is fully functional [30, 31]. This type has an NC3 domain that carries glycosaminoglycan chains, and it interacts with matrix proteins such as decorin, cartilage oligomeric matrix protein, fibromodulin, and tenascin and could possibly be associated with the functional regeneration of the PDL [32].
Role of collagen in periodontium
Alveolar bone
Alveolar bone contains both organic and inorganic material. The dominant collagen is type I, although small amounts of type III collagen may be present, particularly in immature or healing bone. Most of this collagen can be regarded as intrinsic collagen secreted by osteoblasts. However, collagen inserted as Sharpey’s fibers can be considered as extrinsic collagen formed by adjacent fibroblasts. Mutation in the genes encoding the constituent peptides of the collagen type I triple helix may give rise to inherited conditions of Osteogenesis Imperfecta & Dentinogenesis Imperfecta [33]. Collagen of bone occurs as fibers arranged at an angle to each other so as to resist mechanical shear from any direction [34]. Woven bone is characterized by interwined collagen fibrils oriented in many directions, showing wide interfibrillar spaces. However, in case of lamellar bone, collagen fibrils are generally thicker and arranged in ordered sheets consisting of aligned and closely packed fibrils [26].
Periodontal ligament
The collagen of periodontal ligament is Type I (80%), type III (20%) with lesser amounts of Type IV, V, VI & XII also present. Type I collagen is the major protein component of most connective tissues including skin, gingiva and bone. It contains two identical α1 chains and a chemically different α2 chain. It is low in hydrolysine and glycosylated hydrolysine. It is the main collagen of the organic matrix of bone and cementum and is virtually insoluble due to crosslinks which provide the structural and mechanical stability for normal function. Type III collagen (20%) also consists of three α1 chains. It is high in hydroxyproline, low in hydroxylysine and contains cysteine. It is present in similar proportions to those found in embryonic tissues, and this probably reflects the high turnover rate within the ligament. Type III collagen is more fibrillar and extensible than type I and may be important in maintaining the integrity of the ligament during the small vertical and horizontal movements which occur during chewing. The principal fibers are composed mainly of collagen type I, whereas reticular fibers are composed of collagen type III. Collagen type III generally co-distributes with collagen type I to form mixed fibrils of infinitely varying proportions, a higher proportion of collagen type III is present in fetal tissue. Collagen type IV is a short chain molecule that has only recently been located in the periodontal ligament. It is found in the basal lamina. It is a microfibril forming collagen that ramifies the extracellular matrix, but it doesn’t directly associate with the major banded collagen fibrils. The molecule may be central in retaining the integrity & elasticity of the extracellular matrix. The molecular configuration of collagen fibers provides them with a tensile strength greater than that of steel. Thus, collagen imparts a unique combination of flexibility and strength to the tissues [35]. Radiographic studies with radiolucent thymidine, proline and glycine indicate a very high turnover rate of collagen in the periodontal ligament. The rate of collagen synthesis is twice as fast as that in gingiva and four times as fast in skin, as established in rat molar [36].
Cementum
Cementum is approximately 45 to 50% hydroxyappatite (inorganic) and 50% collagen and non-collagenous matrix proteins (organic). Collagen type I is the predominant collagen. It plays a key role in regulating periodontal tissues during development and regeneration. In addition, during early stages of cementogenesis, development and repair, type III collagen is present in high amounts but is decreased with maturation of this tissue. Also, type XII collagen may assist in maintaining periodontal ligament space versus continuous formation of cementum. Trace amounts of other collagens, including type V and type XIV are also found in extracts of mature cementum [37].
Gingiva
The connective tissue of the gingiva is known as lamina propria. Normal gingival tissue contains type I and type III collagens at a ratio of 5 : 1, which account for 99% of the collagen, type IV, which is associated with basal lamina accounts for remaining 1%. In granulation tissue, type III collagen predominates initially, and as it matures, decreases gradually to approximately 20% of the total collagen. The ratio of type V to type I collagen is increased at extraction sites in the early healing stages and gradually diminishes to usual levels, as does the ratio of type III to type I. the increase is probably related to angiogenesis, in which type V collagen may facilitate the migration of endothelial cells. The tensile strength of the wound augments as the content of type I collagen increases. Increasing age results in coarser and denser gingival connective tissue [38].
Biocompatibility
Nowadays various forms of collagen are being used successfully in the field of medicine and dentistry [39, 40]. Collagen is the material of choice in the management of severe burns, non-healing ulcers, traumatic and surgical wounds, vascular injuries after cardiac surgery or interventions and various cosmetic surgical procedures. Studies in dental research aim at the development of suitable biomaterials with unique functional properties. The wide use of collagen is associated to natural properties that include the low immune response and toxicity; achieve homeostasis; ability to promote cellular growth and attachment, etc. Collagen might activate platelets leading to adhesion (and possible thrombus formation) [41–43].
David Brett (2008) reviewed collagen based wound dressings and stated that they are uniquely suited to address the elevated levels of MMPs that act as a sacrificial substrate in the wound [44]. Doillon C J, Silver F H (1986) also revealed that collagen-based dressings produce a significant increase in the fibroblast production. It has a hydrophilic property that is important in encouraging fibroblast penetration, enhancing the deposition of organized and oriented collagen fibers by attracting fibroblasts and cause a directed migration of cells which aid in the uptake and bioavailability of fibronectin that help to preserve leukocytes, macrophages, fibroblasts and epithelial cells. These assist in the maintenance of the chemical and thermostatic microenvironment of the wound [45].
Applications of collagen in dentistry
Collagen is also used to activate platelets during platelet aggregation testing [48, 49].
Conclusion
Collagens are the major structural element of all connective tissues and are also found in the interstitial tissue of virtually all parenchymal organs, where they contribute to the stability of tissues and organs and maintain their structural integrity. The loss or defect of collagen can cause skin aging and other diseases. The collage treatments have demonstrated effective improvements in skin hydration, skin elasticity, medical and dental scaffold treatment in tissue engineering [49] and in many clinical studies. Collagen therapy can reach good improvement also does not cause any serious adverse reactions.
Conflict of interest
The authors have no conflict of interest to report.
Funding
None.
