Abstract
Background:
Both air pollution and dementia are current and growing global issues. There are plausible links between exposure to specific air pollutants and dementia.
Objective:
To systematically review the evidence base with respect to the relationship between air pollution and later cognitive decline and dementia.
Methods:
Medline, Embase, and PsychINFO® were searched from their inception to September 2018, for publications reporting on longitudinal studies of exposure to air pollution and incident dementia or cognitive decline in adults. Studies reporting on exposure to tobacco smoke including passive smoking or on occupational exposure to pollutants were excluded. Using standard Cochrane methodology, two readers identified relevant abstracts, read full text publications, and extracted data into structured tables from relevant papers, as defined by inclusion and exclusion criteria. Papers were also assessed for validity. CRD42018094299
Results:
From 3,720 records, 13 papers were found to be relevant, with studies from the USA, Canada, Taiwan, Sweden, and the UK. Study follow-up ranged from one to 15 years. Pollutants examined included particulate matter ≤2.5 μ (PM2.5), nitrogen dioxide (NO2), nitrous oxides (NOx), carbon monoxide (CO), and ozone. Studies varied in their methodology, population selection, assessment of exposure to pollution, and method of cognitive testing. Greater exposure to PM2.5, NO2/NOx, and CO were all associated with increased risk of dementia. The evidence for air pollutant exposure and cognitive decline was more equivocal.
Conclusion:
Evidence is emerging that greater exposure to airborne pollutants is associated with increased risk of dementia.
INTRODUCTION
Air pollution is a current and growing global problem [1]. It is a recognized causative factor in several non-communicable diseases (NCD) including heart disease, stroke, and cancer [1]. Dementia (a disabling, degenerative NCD) is also a growing global issue [1, 2]. There are plausible links between air pollution and increased risk of dementia [3–7]. Recent interest in this area has resulted in several publications examining the association between air pollution and subsequent dementia or cognitive decline [6, 8–11]. We provide a systematic overview of the current evidence base.
Air pollution
According to a recent Lancet commission on pollution and health, pollution is the largest environmental cause of disease and premature death in the world today, responsible for an estimated 16% of all deaths worldwide and associated with a much wider range of disease than was previously thought [1]. Air pollution in particular is at highest concentration in Low and Middle-Income Countries (LMIC) but can disperse globally and has a disproportionally greater effect on the vulnerable, children and older adults [1].
Dementia
The risk of dementia, and the cognitive decline that precedes it, rise with increasing age. The globally ageing population means that the absolute numbers of those living with dementia continue to increase with an estimated new case every three seconds [12]. The rise in dementia cases is global but due to differing patterns in risk factor exposure and healthcare access, the rise is greater in LMIC [12].
Air pollution and dementia
Exposure to air pollution, especially fine particulate matter, is thought to increase risk of hypertension, raised lipids, atherosclerosis, oxidative stress, insulin resistance, endothelial dysfunction, enhanced propensity toward coagulation, inflammation, and stroke, all of which also raise risk of cognitive decline and dementia [1–4, 13–17].
The 2017 Lancet commission on dementia prevention, intervention and care included air pollution in a list of potential risk factors for dementia [18]; the 2018 Lancet commission on pollution states that the evidence of causation is building, in particular for fine particulate matter and dementia in the elderly, and it calls for research to explore emerging causal links [1]. Given that air pollution is known to have a negative effect on human health, a clinical trial of the length needed to evaluate effect on cognitive function is unlikely and the best evidence to demonstrate a causal link will come from longitudinal observational studies. Recent interest in this area has led to the publication of several such studies examining air pollution exposure and incident cognitive decline or dementia [6, 11].
Our aim was to systematically review the evidence base with respect to the relationship between air pollution and incident cognitive decline and dementia in adult populations and to update our earlier review in this area [11]. The protocol for this review is registered with the International prospective register of systematic reviews (http://www.crd.york.ac.uk/prospero/) no. CRD42018094299 and is an update of an earlier review CRD42014007582 [12]
MATERIALS AND METHODS
Standard systematic review methodology was followed [19]. As this was an update of an earlier systematic review the same search terms were used [11] and the databases MEDLINE, Embase, and PsychINFO® were searched from inception to the 20 September 2018. Reference lists of all papers identified were screened for other published papers. Details of the search strategy are given in the Supplementary Material.
There were three independent analysts (RP, JP, NE). The lead analyst carried out the literature searches. All identified abstracts, or titles where abstracts were unavailable, were double read and a list of potentially relevant references compiled independently by at least two analysts. These lists were compared and differences were resolved by discussion. Once the list of possible references was agreed, full text articles were obtained, double read, and assessed for relevance independently by at least two analysts. Any differences in agreement were resolved by discussion. Inclusion was assessed in accordance with the inclusion and exclusion criteria below
Inclusion criteria
Longitudinal studies with evidence of some assessment of exposure to air pollution (aggregate assessment or constituent parts); Use of formal assessment of cognitive function; Report of incident cognitive decline or dementia outcomes; Data from adults (age ≥18); Minimum follow up 6 months.
Exclusion criteria
Studies reporting only occupational exposure to pollutants; Studies reporting exposure to other pollutants, e.g., organophosphates; Studies reporting only exposure to smoking (including passive smoking); Non-English publications (in the absence of resources available for translation).
The selection of longitudinal studies with assessment of exposure to air pollution, formal assessment of cognitive function and reports of cognitive decline (i.e., a change in cognitive function) or incident dementia were used to ensure the inclusion of the most robust data with regard to evaluation of causality. Data were extracted using standard extraction tables and information was collected on: the region where the study took place, the size and composition of the study population, the duration of follow up, the assessment of cognitive function or incident dementia, the measurement of exposure to air pollutants, types of pollutant, the analyses (principle summary measures include hazard ratios and odds ratios), results, and reported co-variates. In order to be as conservative as possible, results following adjustment for confounding were preferred for inclusion in the table.
Each included paper was also assessed for validity. Formal scoring was not used as existing instruments have poor discriminative ability when assessing quality. Instead each paper was assessed against key criteria based on the Critical Appraisal Skills Programme (CASP©) checklists [20]. Potential sources of bias in each study were tabulated.
RESULTS
There were 3,720 records identified by searches and where abstracts were double screened. Of those, 45 articles were assessed at full text stage and 13 were included [8, 21–31]. Two articles reported on the association between NOx and incident dementia in the same sample from the Swedish Betula study [31, 32]; the one that reported numerical results was selected for inclusion [31]. The remaining article had a focus on noise exposure and was excluded [32]. Further exclusion at full text stage was due to study design (lacking appropriate longitudinal data [10, 33–54]), where exposure measures were not clearly related to air pollution [5, 55–58], or where the article was a review only [59]. Several studies were ineligible for more than one reason. Figure 1 shows the flow chart for study inclusion.
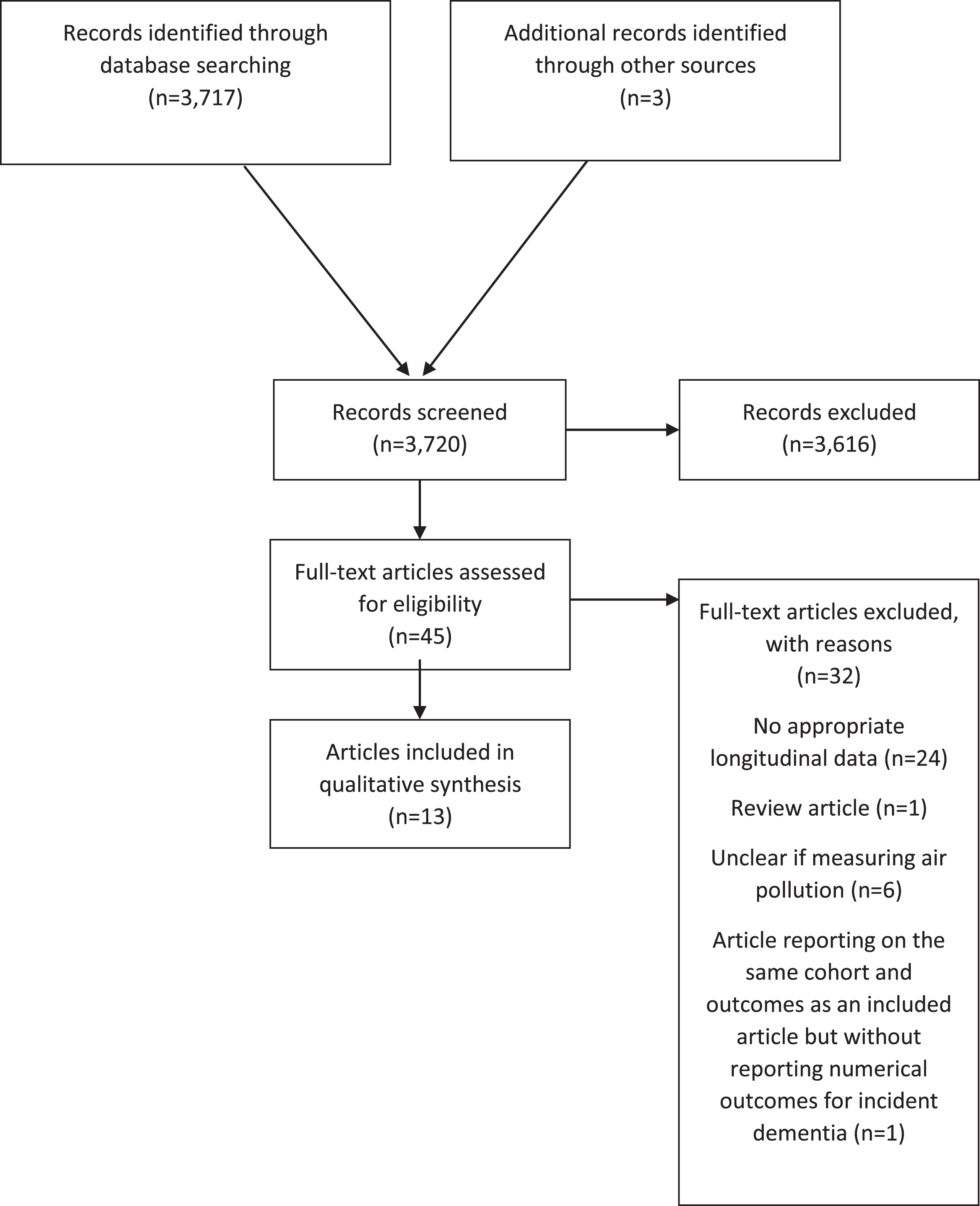
Flow chart.
Study characteristics
Four studies reported results from populations in the United States of America [21, 29], two from Canada [8, 9], two from Taiwan [27, 28], one from Sweden [26, 31], and two from the United Kingdom [23, 24] The samples from the UK both included populations from London but one reported on cognitive function [23] and the other on incident dementia [24]. The samples from Taiwan both selected participants from the National Health Insurance Research Database but selected differing subgroups of the population and presented results for different pollutants: for Jung et al. [27], particulate matter 2.5 (PM2.5); and for Chang et al. [28], nitrogen dioxide (NO2) and carbon monoxide (CO). The samples from Canada both selected residents of Ontario but also selected differing sub groups and reported on different measures of pollution; for Chen et al. [8], PM2.5; and for Chen et al. [9], residential proximity to a major roadway. There were three articles reporting on the Swedish Betula study, one on NOx and incident dementia [26], one on NOx and episodic memory [30], and one on PM2.5 and incident dementia [31]. Sample size ranged from 1,469 [30] to over two million [9], and two studies recruited only women (participants in the Nurses Health Study) [21] and the Women’s Health Initiative Memory Study (WHIMS) [29]. All studies were longitudinal but follow up was reported inconsistently. It varied from one year [22] to ∼5–10 years [23, 30] in studies with cognitive outcomes, and from ∼7 [8, 28] to ∼15 years [26] in studies with incident dementia outcomes. See Table 1 for study characteristics.
Study characteristics
AD, Alzheimer’s disease; ADC, Alzheimer’s Disease Centre; BL, baseline; FU, follow-up; LHID, Longitudinal Health Insurance Database; NACC, National Alzheimer’s Coordinating Centre; NHIRD, National Health Insurance Research Database; NHS, Nurses Health Study; ONPHEC, Ontario Population Health and Environment Cohort; REGARDS, Reasons for Geographic and Racial Differences in Stroke Study; T1, time-1; T1, time-2; WHIMS, Women’s Health Initiative Memory Study; y, year.
Exposure assessment
The most commonly examined pollutant was PM2.5, reported in nine articles [8, 31]. One study used distance to a major roadway as the main outcome with additional adjustment for PM2.5 and NO2 exposure in sensitivity analyses [9]. Four studies reported on NO2 [8, 28] and one on NOx [30]. See Supplementary Table 1.
The selected studies adopted a variety of modelling approaches, to obtain high resolution (to residential address level) exposure estimates for their populations. The methodologies varied from relatively simple interpolation approaches from selected monitoring sites within the study domain [28], to more refined approaches, exploiting Land Use Regression approaches and satellite data to improve predictions at locations remote from air pollution monitoring sites [8, 22]. Three studies employed an emissions approach with dispersion modelling, incorporating annual meteorology [23, 25], and atmospheric chemistry [25]. Two studies attempted to split the PM modelled estimates in those derived from vehicle tailpipes [23, 31] and PM derived from residential wood burning [31]. While most studies employed single models to estimate exposures to a range of pollutants, several studies employed different approaches for different pollutants, such as O3 and PM2.5 [8]. In most cases, studies presented some form of model evaluation or provided reference to an external source relating to model performance. Only one study employed road distance as their primary (proxy) measure for exposure to traffic related air pollutants [9], but this employed modelled pollutant estimates in their subsequent sensitivity analysis. For one study [28], the exposure measures used in the analyses were unclear. The period for evaluating associations between exposure to pollution and cognitive decline or incident dementia, ranged from days to weeks for the cognitive assessments to months to years for dementia. For dementia in particular, various lag or aggregated exposure periods were also used. It should be stated that there is no clear consensus as to what the most informative exposure period is to assess the neurological impacts of air pollution, but as modelling approaches look further back in time within the available cohorts the modelling uncertainty increases as the available measurement data become sparser. As with all modelling approaches, there is likely to be significant exposure misclassification, as modelling estimates at a point are unlikely to represent the true exposure of a mobile population. Here the view is that this degree of misclassification will be greater for pollutants with a high degree of spatial variation, such as NO2, and less marked with pollutants with a more uniform distribution such as PM2.5. These issues were reflected in the discussion of most of the papers cited, as was the difficulty in disaggregating the effect of independent pollutants that were highly correlated within the models.
Assessment of outcomes, dementia, and cognitive decline
Seven articles reported incident dementia cases [8, 31], one focused only on incident Alzheimer’s disease (AD) [27]. Six articles used varied measures of cognitive change [21–23, 30]. See Supplementary Table 1.
Association between air pollution exposure and cognitive outcomes
Overall, the evidence pointed to an association between greater pollution exposure and increased risk of dementia regardless of pollutant measure (see Fig. 2). The evidence relating to cognitive decline was equivocal. There was no clear pattern by region of recruitment or concentration of pollutant. Variation in statistical methods and the frequent use of quantiles for pollutant exposure prevented meta-analysis. See Table 2 for main results.

Number of studies investigating relationship between exposure to pollutants and cognitive function or dementia.
Key findings and results
AD, Alzheimer’s disease; VaD, vascular dementia; CDR-SB, Cognitive Dementia Rating Sum of Boxes; EEM; Episodic Memory Measure; MMSE, Mini-Mental Status Examination; CO, carbon monoxide NO2, nitrogen dioxide; O3, ozone; PM2.5 particulate matter ≤2.5 μm in diameter; PM10, particulate matter ≤10 μm in diameter; SO2, sulphur dioxide; ppb, parts per billion, y; year; *, statistically significant; (a, b), 95% confidence interval; HR, hazard ratio; HRIQR, hazard ratio per interquartile range increase; IQR, interquartile range; ns, non-significant; OR, Odds ratio. Q, quintile; SD, standard deviation; SES, socio-economic status.
For PM2.5, three studies [21, 29] reported an association between PM2.5 and decline in cognitive performance (i.e., higher exposure associated with higher risk), with the WHIMS study additionally reporting a dose dependent relationship between apolipoprotein E4 (APOE4) allele and PM2.5, such that the lowest decline was in those with lowest exposure and without an APOE4 allele [29]. In the Whitehall study, the association between PM2.5 and decline in cognitive performance was seen only for memory performance with a four-year time lag (average exposure over four years prior to second cognitive assessment) but not in other cognitive domains or with other time lag periods [23]. Two further studies found no relationship between PM2.5 and decline in cognitive performance [22, 25], although one reported a dose response relationship for the interaction between presence of APOE4, PM2.5, and cognitive decline [25] Greater exposure to PM2.5 was also associated with an increased risk of dementia [8, 31] and AD [24, 27], in UK, Canadian, Swedish, United States, and Taiwanese populations with the WHIMS study also reporting a dose dependent relationship for APOE4, PM2.5, and dementia risk [29]. For NO2/NOx, greater exposure was consistently associated with an increased risk of dementia [8, 28] and AD [24]. There was one analysis of NOx and cognitive decline that reported no relationship between NOx and decline in episodic memory [30]. Four studies also examined ozone as a pollutant [8, 27]. One found no relationship with incident dementia [8], one reported a decreased risk of dementia and AD [24], one found greater ozone exposure to be associated with increased risk of incident AD [27], and one reported only a dose dependent relationship between APOE4, ozone interaction, and cognitive decline [25], i.e., the lowest decline in those with lowest exposure and without an APOE4 allele [25]. A single study looked at carbon monoxide and found an association between greater exposure and increased risk of dementia [28].
Taking a different approach, Chen et al. and Carey et al. used a proxy measure of pollution exposure looking at the association between place of residence and distance to the nearest major roadway [9, 24]. This has been shown to have a cross sectional association with poorer cognitive scores in a population in Germany [47], but has not been examined with incident dementia. The results for Chen et al. showed a statistically significant dose response such that the closer the residence to a major roadway the greater the risk of incident dementia [9]. See Supplementary Table 2.
Study quality
Overall, all studies had reasonable clarity in their research questions, used adequate methodology and standard clinical assessments (although not always the gold standard) for cognitive outcomes, and employed a range of modelling approaches to estimate exposures that employed some form of statistical or dispersion modeling, with some form of prior evaluation. Further caution is required regarding interpreting the data relating to dementia risk and residential distance from a major roadway [9, 24] as this was not additionally adjusted for regional impact of wind conditions. Five studies had a greater potential for bias in measurement of outcome in the form of incident dementia, primarily due to the use of health records for the identification of cases [8, 28]. The use of health records rather than a rigorous assessment of all study participants is pragmatic for large sample sizes but may bring bias. Health records often rely on a level of self-referral for assessment and have the potential for missed cases, diagnoses made later in the disease course, and higher rates of case finding in those with comorbid conditions and are likely to have less systematic recording of potential confounders. Four studies used populations that restrict generalizability; the Nurses Health Study recruited only female nurses [21], the WHIMS included only women [29], the Whitehall study recruited predominantly male civil servants [23], and Cleary et al selected participants from an ongoing University of Washington National Alzheimer Coordinating Center [25]. All studies adjusted for a series of relevant confounders (see Supplementary Table 2). Overall, the majority of the studies were at low or low to moderate risk of bias (Supplementary Table 3).
DISCUSSION
Overall, the evidence from longitudinal cohort studies pointed towards an association between greater exposure to pollutants, in particular PM2.5, NO2/NOx and increased risk of dementia. The evidence for cognitive decline was more equivocal than that for the dementia outcomes. The pattern was mixed for O3 with studies reporting positive and negative associations with exposure and increased risk and one reporting no association. Results for CO, PM2.5–10, and PM10 were too few to allow strong conclusions. These results support a possible role for exposure to air pollution, especially pollutants PM2.5, NO2/NOx, and O3 and an increased risk of dementia and the decline in cognitive function that precedes it. Plausible pathways exist to support this. It is hypothesized that, when inhaled, the gas, particles, or material desorbed from the particle surface act to induce inflammatory responses, microglial activation, production of reactive oxygen species, and increased production and deposition of Aβ peptides [3, 60–65]. Furthermore, plausible mechanisms support the potential for inhaled PM2.5 or the even smaller UltraFine Particulate Matter <0.1 μm (UFPM) reaching the brain directly via the olfactory bulb with animal studies finding ultrafine particle penetration into the olfactory bulb, the frontal cortical, and subcortical areas of the brain [3, 66–70]. Although our review focused mainly on later life decline and incident dementia, exposure likely builds over the lifetime. Autopsy studies from children and young adults living in Mexico City have found associations between exposure to urban air pollution, particulate deposition and inflammation already present within the brain [71, 72], and population-based longitudinal studies are beginning to report associations between prior air pollution exposure and imaging outcomes; for example, the Atherosclerosis Risk In Communities study found higher long term PM exposure to be associated with smaller deep-grey matter volume [73].
Strengths and limitations
The systematic nature of our updated review and selected inclusion of only longitudinal studies with incident dementia or cognitive change provides the most rigorous filter with which to examine the evidence relating to the association between air pollution and incident cognitive decline or dementia. Furthermore, the risk of bias in the included studies was low to moderate. However, there are limitations. Studies were drawn from just five countries. The assessment of pollution, although geocoded, may not reflect the true local variation or exposure in a mobile population; for example, if, as shown, risk varies within 300 m of a major roadway, there is the potential for a huge variety of risk within even a small geographical area, potentially even more so when taking account of prevailing wind patterns [9]. This is further limited by the use of varied methods for the assessment of exposure to air pollution in the included articles and the data were too disparate to be combined in a meta-analysis. The use of incident dementia is robust but relies on health records where diagnostic rigor may be weaker and cases may be missed. Conversely, case finding bias may be prompted by other health concerns also stemming from exposure to air pollution. Furthermore, although this is in contrast to studies where specific assessment of cognitive function is required for all participants as part of the study procedures a measure of cognitive decline by itself does not necessarily indicate an ongoing degenerative process. As in all dementia risk factor evidence, there is also the question of adequate assessment of confounding, in particular where there may be an interaction with presence of APOE4. Furthermore, although many co-variates have been accounted for there remains, for air pollution in particular, the possibility of a role for both individual and parental socioeconomic status, living conditions, and pollution exposure through the life-course. This is particularly relevant considering that associations between air pollution and poorer cognitive performance have been shown in childhood [6, 7]. Finally, of course, there may be an emerging publication bias as this area expands and we could not assess this, we did not review the grey literature, nor could we combine the evidence we have in a useful meta-analysis.
Although the evidence base examining the association between air pollution and cognitive decline or dementia is smaller and less convincing than the equivalent evidence linking air pollution to increased risk of cardiovascular disease [1, 2], it is growing quickly. All of the articles that we identified had been published in the last five years, and 11 of the 13 we identified had been published since our last systematic review which searched until 1 November 2013 [11]. Our updated review, examining longitudinal evidence with incident decline, adds confirmatory evidence reducing uncertainty as to the likelihood of an association. Furthermore, the growing evidence base is reporting increasingly consistent results (at least for dementia outcomes), dose response relationships, and biological plausibility particularly for exposure to PM2.5. A detailed examination of the growing literature on potential mechanisms is beyond the scope of this review; however, for example, see Heusinkveld et al., Mumaw et al., Aragon et al., and Thompson [62–65] for more details.
Our review has drawn together and presented the existing evidence for exposure to air pollution and incident cognitive decline or dementia. Our goal now should be to strengthen the rigor and extent of the research in this area to allow specific recommendations to be made. This could be achieved by the use of an individual participant data meta-analysis but to do this, we need to examine a number of factors in more depth. These include: 1) the role of exposure duration; 2) the role of different pollutants and different combinations of pollutants using more sophisticated adjustment and modelling of exposure, e.g., including adjustment for presence of multiple pollutants, taking account of current and prior residential and other exposures such as school yards or workplaces; 3) the role of exposure in different populations in different geographical regions, such as low and middle income countries; 4) the role of modifying factors such as APOE4; 5) the potential variation in the association of air pollution with different cognitive domains; 6) the need to collect repeat imaging measures to allow insight into pathways and mechanisms; and 7) the potential for ameliorating the effects of exposure.
Conclusion
Air pollution, in common with the majority of established risk factors for dementia, does not influence cognition alone. Rather, it increases the risk of multiple non-communicable diseases, one of which is dementia. However, unlike the majority of the established dementia risk factors, the opportunity for personal control over exposure to risk from air pollution is low. Air pollution is pervasive, global, life-long, and bad for health. Further regulation and reduction of exposure has huge potential for health benefit and cost saving including potentially reducing dementia risk. At present, the evidence suggests that greater exposure to air pollution may increase risk of cognitive decline and dementia, and further research is needed to support robust recommendations.
Footnotes
ACKNOWLEDGMENTS
RP is funded by the Australian National Health and Medical Research Council Dementia Centre for Research Collaboration, NE is funded by the NHMRC Centre of Excellence in Cognitive Health APP1100579, KJA is funded by NHMRC Fellowship APP1102694. We acknowledge support from the UK National Institute for Health Research, and the ARC Centre of Research Excellence in Population Ageing Research CE170100005.
IM’s contribution was also part funded by the National Institute for Health Research Health Protection Research Unit (NIHR HPRU) in Health Impact of Environmental Hazards at King’s College London in partnership with Public Health England (PHE) and Imperial College London. The views expressed in this paper are those of the authors and not do not reflect the official policy or position of any of the following: the NHS, the NIHR, the Department of Health, Public Health England or the Medicines and Healthcare Products Regulatory Agency (MHRA).
