Abstract
BACKGROUND:
Occludin/ELL domain containing 1 (OCEL1) is a novel discovered protein with its molecular functions remaining unknown and its role in lung cancer has not been directly explored.
OBJECTIVES:
This study focused on the role of OCEL1 in the progression and prognosis of non-small cell lung cancer (NSCLC).
METHODS:
A public database and tissue samples (80 NSCLC tissue samples and paired normal lung samples) were used to compare differences in OCEL1 expression and investigate its relationship with clinical characteristics and prognosis.
RESULTS:
Compared to adjacent normal lung tissue samples, OCEL1 expression was significantly down-regulated in tumor tissues. In addition, there was a negative correlation between OCEL1 and Ki67 expression levels. Low OCEL1 expression was significantly associated with lymph node metastasis, higher TNM stage, and poor prognosis. Importantly, multivariate analysis identified OCEL1 expression as an independent predictor for unfavorable NSCLC prognosis.
CONCLUSIONS:
These results indicated that OCEL1 protein may serve as a novel prognostic biomarker in NSCLC.
Introduction
Lung cancer is the most common cause for cancer-related deaths worldwide [1]. In spite of the improvement in cancer screening and personalized therapy in recent years, five-year survival rates remain poor [2]. Lung cancer patients are usually asymptomatic in the early stages, with most patients diagnosed at advanced stages [3]. Therefore, continuous exploration of new molecular targets and improvement of targeted therapies are necessary for better clinical outcomes.
Occludin/ELL domain containing 1 (OCEL1) is a novel discovered protein that belongs to the ELL/ occludin family, including MARVELD2, OCEL1, occludin, ELL, ELL2, and ELL3. Previous research has demonstrated that OCEL1 is highly expressed in the eye, retina, and brain and may be a genetic cause of the Aicardi syndrome, which is a severe neurodevelopmental disorder [4]. In addition, OCEL1 is also overexpressed in the retina of intraocular hypertension mice [5]. However, the role of OCEL1 in cancer is not fully understood. One study based on global gene profiling analyses indicated that OCEL1 transcription was dependent on the P53 status in cancer [6]. Our previous work utilized bioinformatics analysis to demonstrate that OCEL1 could be a predictor marker of paclitaxel-based neoadjuvant therapy efficacy in HER2-negative breast cancer patients [7]. However, the role of OCEL1 in lung cancer has not been elucidated.
This study is the first to report on the aberrant expression and clinical significance of OCEL1 in NSCLC. Furthermore, OCEL1 expression was an independent factor for the unfavorable prognosis of NSCLC. Taken together, these findings indicated that OCEL1 played an important role in NSCLC and could be a potential diagnostic and prognostic biomarker in NSCLC patients.
Materials and methods
Bioinformatics analysis
The Cancer Genome Atlas (TCGA) datasets TCGA_ LUNG_exp_HiSeqV2-2015-02-24 and TCGA_LUAD _exp_HiSeqV2-2015-02-24 were downloaded from the UCSC cancer website (
Patients and tissue samples
In this study, 80 cases of tumorous tissue samples and paired adjacent normal lung tissues were enrolled. Clinical characteristics were obtained from medical records and pathological reports. This study was approved by The Human Ethics Review Committee of the First Hospital of China Medical University.
Immunohistochemistry (IHC) analysis
IHC staining was performed as described previously [10]. Anti-human OCEL1 rabbit antibody was used at a dilution of 1:100 (ab184839; Abcam, Cambridge, UK), with phosphate-buffered saline used as a negative control. Each section was evaluated and scored independently by two pathologists. A semi-quantitative scoring system was used in this assay. Intensity was scored as “0” (negative), “1” (weak), “2” (moderate), and “3” (strong) and the percentages of tumor cells within each category were calculated. Percentage scores were multiplied by staining intensity scores to generate IHC scores. The histoscores ranged from zero (minimum) to 300 (maximum). Immunostaining was considered positive when percentage scores
Statistical analysis
Statistical analyses were performed using SPSS 13.0 software (IBM, Armonk, NY, USA). Student’s
OCEL1 is significantly down-regulated in NSCLC and correlates with prognosis in public datasets. (A) Differences in OCEL1 expression between normal and lung cancer tissue samples from TCGA datasets (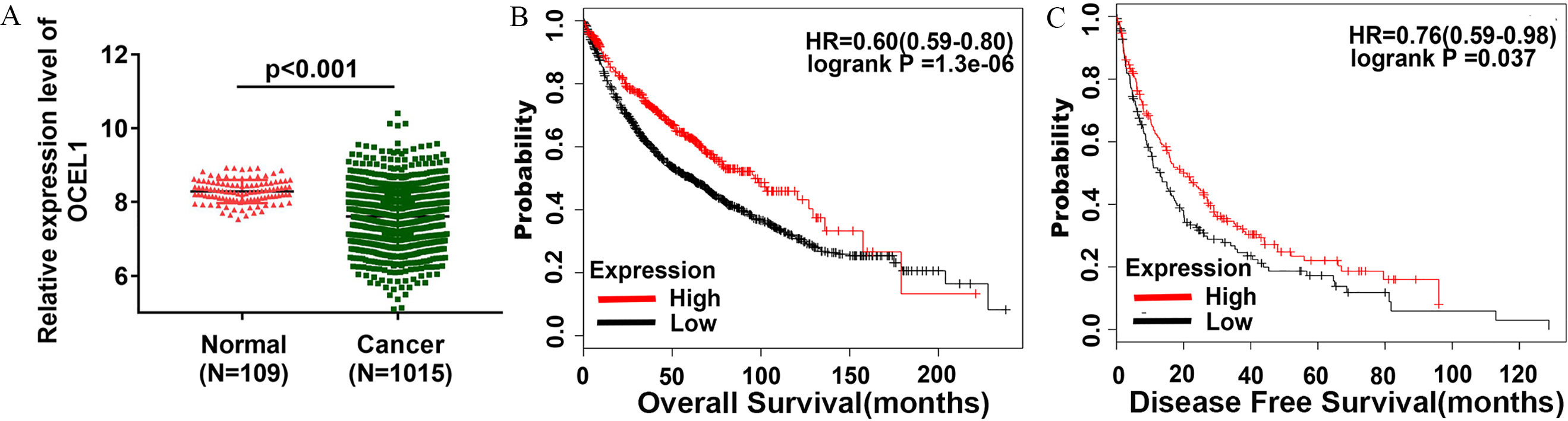
Decreased OCEL1 protein expression in NSCLC tissues. (A) Representative images of OCEL1 staining in human NSCLC and adjacent normal lung tissue samples; (B) IHC scores for OCEL1 were significantly reduced in cancer tissue samples compared to adjacent normal controls (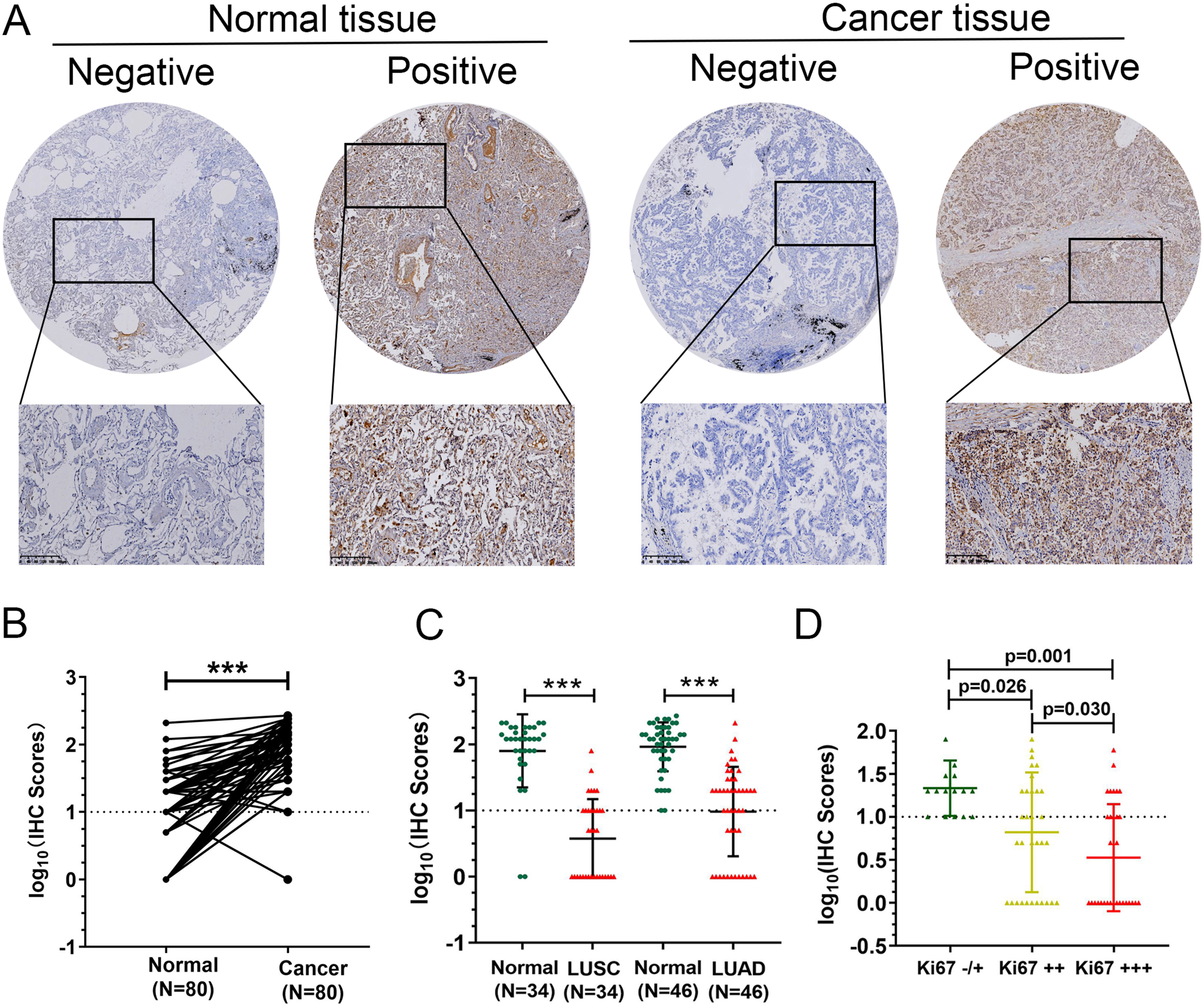
OCEL1 is significantly downregulated in NSCLC and correlates with prognosis in public datasets
To explore the clinical values of OCEL1 in NSCLC, 1016 cases of NSCLC samples and 109 cases of normal lung samples were obtained from the TCGA database. OCEL1 mRNA expression was significantly downregulated in NSCLC tissue compared to normal lung tissue (Fig. 1A). To further explore clinical significance of OCEL1, a Kaplan-Meier plotter software program (
Decreased OCEL1 protein expression in NSCLC tissues
To confirm the clinical significance of OCEL1 in NSCLC patients, 80 NSCLC tissue samples and paired normal lung tissue samples were collected in this study. IHC staining was used to analyze the expression of OCEL1 in tissues. Representative images of OCEL1 expression are shown in Fig. 2A. Based on the IHC staining results, it was found that OCEL1 was significantly downregulated in NSCLC tissues compared to lung tissue samples (Fig. 2B). In addition, OCEL1 was decreased in both lung adenocarcinoma (LUAD) and lung squamous carcinoma (LUSC, Fig. 2C). Further analysis revealed that OCEL1 IHC scores were significantly decreased along with expression of KI-67 (Fig. 2D).
Next, association between clinical characteristics and prognosis with the expression of OCEL1 was explored. A total of 80 NSCLC patients were divided into two groups: OCEL1-positive and OCEL1-negative, according to the IHC results. A chi-squared test indicated that low OCEL1 expression was significantly associated with lymph node metastasis (
Correlation between OCEL1 expression and clinical characteristics in NSCLC patients (
80)
Correlation between OCEL1 expression and clinical characteristics in NSCLC patients (
To further evaluate the diagnostic value of OCEL1 in NSCLC, ROC analysis was carried out. The larger the area under the ROC curve, the more accurate the experimental data and the more valuable its clinical applications. The results showed that OCEL1 level could distinguish NSCLC from normal tissues, with area under curve (AUC) of 0.922 (Fig. 3).
ROC analysis for OCEL1 diagnostic value in NSCLC.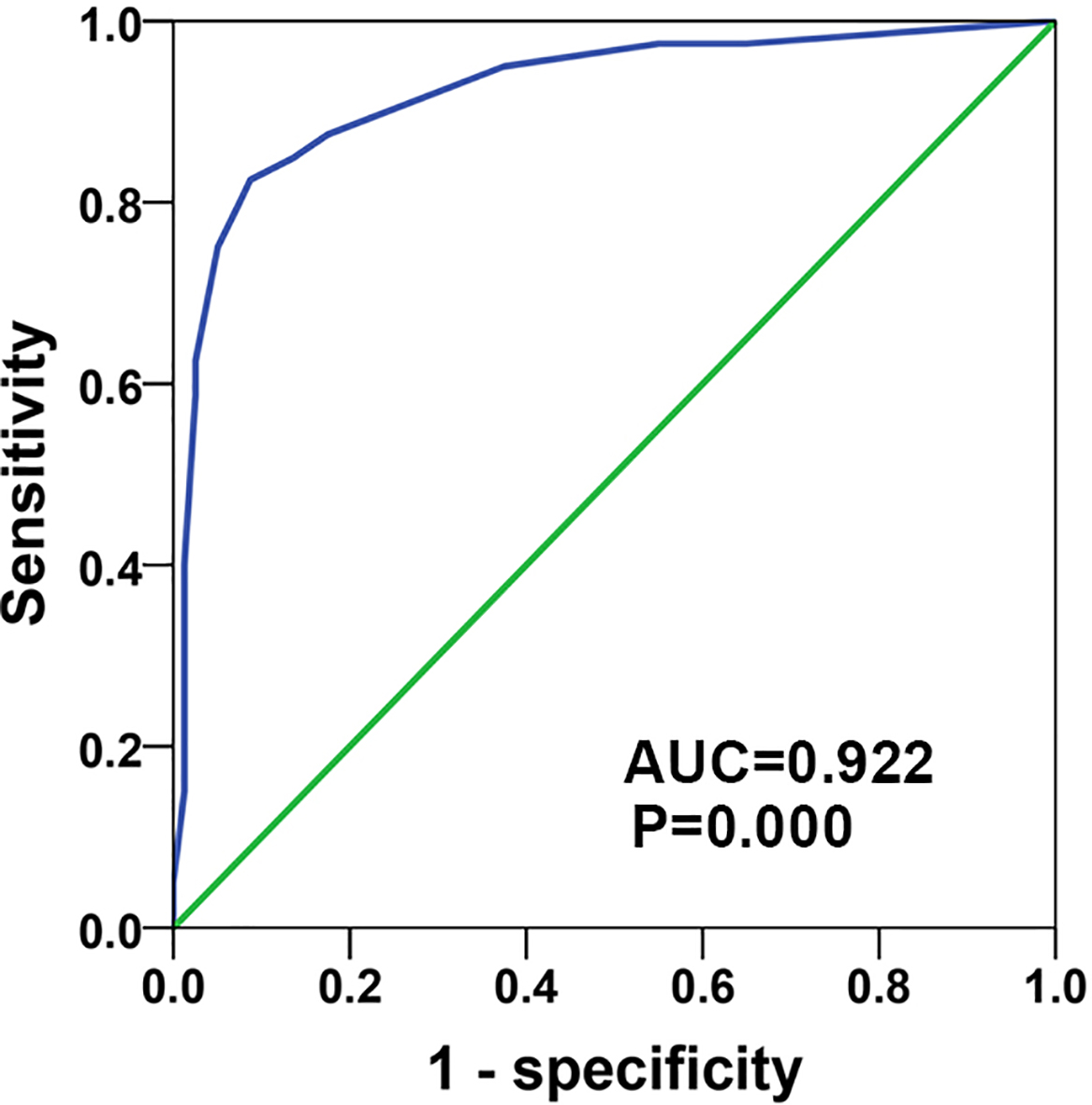
Kaplan-Meier analysis and log-rank test were performed to uncover the relationship between OCEL1 and overall survival in NSCLC patients. OCEL1-positive group had a longer survival time than OCEL1-negative group (
Cox regression analysis of overall survival in NSCLC patients
Cox regression analysis of overall survival in NSCLC patients
Features with
Kaplan-Meier curves for overall survival in 80 NSCLC patients. Correlation of OCEL1 expression (A), tumor sizes (B), and TNM stage (C) with overall survival.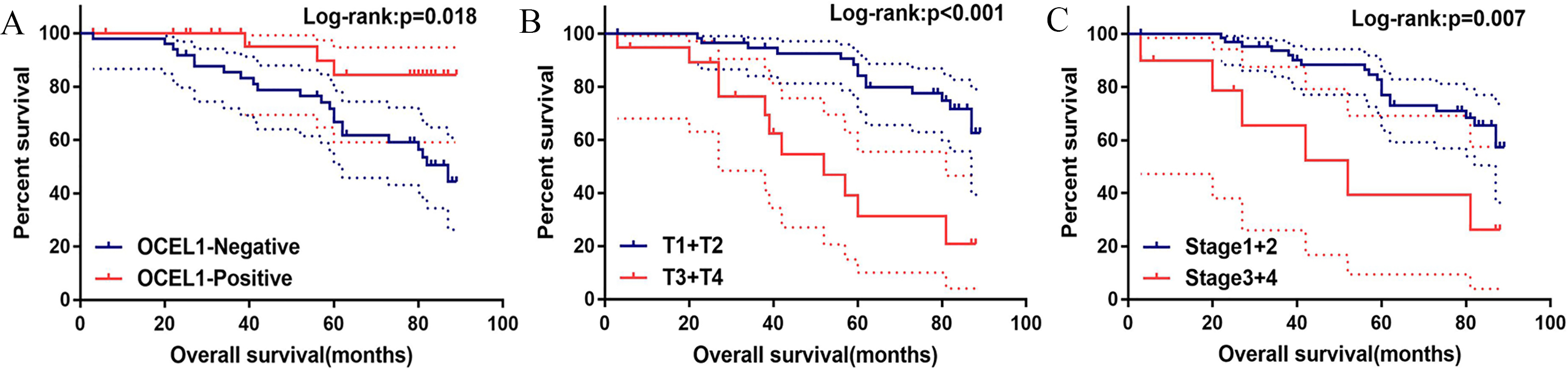
To analyze the influence of clinical and pathological features on the prognosis of patients, Cox proportional-hazards model was used. Univariate analysis showed that T stage (HR
Lung cancer is the main leading cause of cancer-related mortality. Because of the poor chemotherapy efficacy, the prognosis for patients remains unfavorable. Therefore, exploring prognostic markers is essential to improve clinical outcomes.
It is well-known that lung cancer is caused by a combination of environmental factors and genetic changes, including overexpression of oncogenes and inactivation of tumor suppressor genes [13, 14]. Extensive research has confirmed that abnormally expressed genes may cause malignant biological behavior in lung cancer cells [10, 15, 16]. OCEL1 is a novel protein with poorly understood molecular functions. One study has reported that OCEL1 may be the cause of the Aicardi syndrome [4]. It is known that embryonic development and tumorigenesis have similar molecular mechanisms. Therefore, it was suggested that OCEL1 may play an important role in tumorigenesis and tumor development.
Previous study has confirmed that OCEL1 is regulated by mutant P53. Mechanistically, mutant p53 uses p63 as a molecular chaperone to alter the transcription of OCEL1 [6]. In our previous study, OCEL1 was demonstrated to be associated with paclitaxel sensitivity in HER2-negative breast cancer patients. In addition, OCEL1 combined with DK8, FAM64A, and MARC2 as a predictor model enhanced the predictive effect of paclitaxel drug sensitivity [7]. However, its role in lung cancer has not been elucidated. In the present study, based on public datasets and our IHC results, we were the first to propose that OCEL1 is widely downregulated in NSCLC tissue samples and correlates with patient prognosis and clinicopathological features. Based on these results, we are the first to demonstrate the abnormal expression of OCEL1 in NSCLC tissues and its relationship with clinicopathological parameters. Furthermore, the ROC results showed that OCEL1 expression could accurately distinguish between cancerous and normal lung tissue, suggesting its potential value in the diagnosis of lung cancer. Subsequently, the prognostic value of OCEL1 was explored. Univariate and multivariate Cox regression analyses indicated that OCEL1 expression was an independent prognostic factor in LUAD patients. These results supported the hypothesis that OCEL1 was a potential tumor suppressor gene in NSCLC.
There are some limitations to this study. The study findings were based on public databases and NSCLC samples. The molecular mechanism of OCEL1 has not yet been elucidated. Thus, further comprehensive and in-depth analyses in vitro and in vivo are needed and will be addressed in future studies.
In conclusion, these results strongly suggested that OCEL1 played a significant role in NSCLC. Importantly, OCEL1 was downregulated in NSCLC tissues and could serve as a prognostic and diagnostic factor for NSCLC patients.
Footnotes
Acknowledgments
This work was supported by National Natural Science Foundation of China (No. 81972197, 81472193).
