Abstract
Neoadjuvant chemotherapy (NACT) followed by radical surgical hysterectomy and pelvic lymph node dissection is considered an effective method to treat patients with bulky stage IB–IIA cervical cancer, but not all patients benefit from NACT. Apoptotic proteins play important roles in the progression of chemotherapy, and second mitochondria-derived activator of caspase (Smac) may have a cooperative relationship with Omi/HtrA2, leading to carcinogenesis and chemotherapy resistance. Chemosensitivity is an important prognostic factor for cervical cancer patients. The aim of this study was to evaluate the significance of Smac, survivin, X-linked inhibitor-of-apoptosis protein (XIAP), and Omi/HtrA2 expression in predicting the response to neoadjuvant chemotherapy and the prognostic significance of te expression of these proteins in cervical cancer patients. Our findings showed that low expression levels of survivin and high expression levels of Omi/HtrA2 in chemotherapy-responsive cervical carcinoma patients significantly increased chemosensitivity.
Introduction
Cervical cancer is a serious concern to women in China, with related mortality ranked eighth among the most common cancers [1]. Recently, neoadjuvant chemotherapy (NACT) followed by radical surgical hysterectomy and pelvic lymph node dissection has become a valid alternative treatment because it reduces tumor volume and makes the mass resectable without increasing surgical complexity or complications. Despite these advances, the response to NACT remains poor, with a 5-year survival rate of only 50%–70% [2] and a NACT response rate of only 64% [3]. Therefore, to avoid potential therapy-related complications and inappropriate delays in surgical treatment, it would be advantageous to identify chemosensitive tumors before initiating NACT. Second mitochondria-derived activator of caspase (Smac) is a mitochondrial protein that interacts with inhibitor of apoptosis proteins (IAPs) and, upon stimulation of apoptosis, is released into the cytoplasm to inhibit the caspase-binding activity of IAPs. Recently, Smac has been confirmed to be chemosensitive in a variety of tumors, including breast, lung, and esophageal carcinomas [4, 5, 6]. These results suggest that the expression of Smac in tumor cells may predict a good response to chemotherapy. In addition to Smac, three additional proapoptotic proteins have been found to be associated with chemosensitivity. Therefore, in this study, we used immunohistochemistry to confirm the expression of the four proapoptotic proteins, Smac, survivin, Omi/HtrA2, and X-linked inhibitor-of-apoptosis protein (XIAP) in pre- and postchemotherapy tissues from chemotherapy-responsive and nonresponsive cervical cancer patients. We investigated the predictive significance of the expression of the four proapoptotic proteins in tumors from cervical cancer patients treated with platinum-based NACT and provided evidence of their potential role as predictive biomarkers.
Materials and methods
Patients and tissue specimens
From January 2004 to November 2013, patients diagnosed with cervical cancer and registered at Cancer Hospital of Chinese Academy of Medical Sciences, were considered for the study. We chose the chemotherapy-responsive patients and chemotherapy non-response patients by a statistical ratio of 2:1, 73 patients with bulky stage IB-IIA (primary tumor 4 cm in diameter) received a neoadjuvant platinum-based chemotherapy. 73 patients can provide biopsies that were taken pre-NACT following surgery and 70 patients can provide biopsies that were taken post-NACT following surgery to pathological and immunohistochemical analysis. The lesions in patients (pre- and post-NACT) were measured by physical examination, transvaginal ultrasound, and magnetic resonance imaging (MRI). All the patients had not undergone any previous treatment including radiation, chemotherapy, hormone drugs etc. All tissue specimens were obtained with the informed consent of all patients and approval of the local research ethical committee. The median follow-up of patients was 28 months (range 3–97 months).
NACT and therapeutic effect evaluation
All of the patients received one to three courses of platinum-based NACT, the regimens including: (i) TP: 175 mg/m
Clinicopathological findings for chemotherapy-responsive and nonresponsive patients
Clinicopathological findings for chemotherapy-responsive and nonresponsive patients
FIGO, International Federation of Gynecologists and Obstetricians; LVSI, lymphovascular space invasion; SCC squamous cell carcinoma antigen; UK: unknown.
Cancer tissues before and after NACT were obtained by cervical biopsy and surgery. Each pair of specimens was placed in formalin for histological confirmation and immunohistochemistry. Formalin-fixed paraffin sections of tumor tissues were subjected to immunohistochemical staining. The sections were cleared, treated with 0.3% H
Correlation between apoptosis protein expression and tumor response
Correlation between apoptosis protein expression and tumor response
CR, complete response; PR, partial response; PD, progressive disease; SD, stable disease, Smac, second mitochondria-derived activator of caspase, XIAP, X-linked inhibitor-of-apoptosis protein.
The SPSS version 21.0 software package was used for statistical analysis. Comparisons of quantitative data were analyzed with the chi-square test to compare the expression of apoptotic proteins between in pre- and post-chemotherapy tissues. Categorical data were analyzed with Wilcoxon test or Mann-Whitney U test in different groups, logistic regression analysis was used to identify significant multivariate predictors. A multivariate model was used to analyze all the variables that were significant in the univariate analysis. The correlation between different apoptotic proteins was evaluated by Spearman rank test. The survival time was calculated by Kaplan-Meier method and log-rank test. Multivariate survival analysis was performed according to the Cox proportional hazards model.
Results
Patient characteristics and clinical features
Based on the Response Evaluation Criteria in Solid Tumors guidelines, 52/73 patients were considered responsive (3 completely responsive (CR)
Apoptosis protein expression and tumor response
We analyzed Smac, Omi/HtrA2, and XIAP expression for their association with clinical responses (Table 2). Univariate logistic regression analysis revealed that survivin expression was significantly higher, while that of Omi/HtrA2 was significantly lower in the nonresponsive group compared with the responsive group (
Correlation between Smac, survivin, Omi/HtrA2, and XIAP expression in pretreatment biopsies and patient clinicopathological characteristics
Based on the intensity of staining and the level of expression, the 73 patients were divided into two groups: high staining level vs. low staining level and then assessed for clinicopathological characteristics. We found no correlation between the expression levels of Smac, survivin, and Omi/HtrA2 and the clinical factors, including age, pathological grade, and pathological type (
High expression level of Smac in prechemotherapy tissue (*200).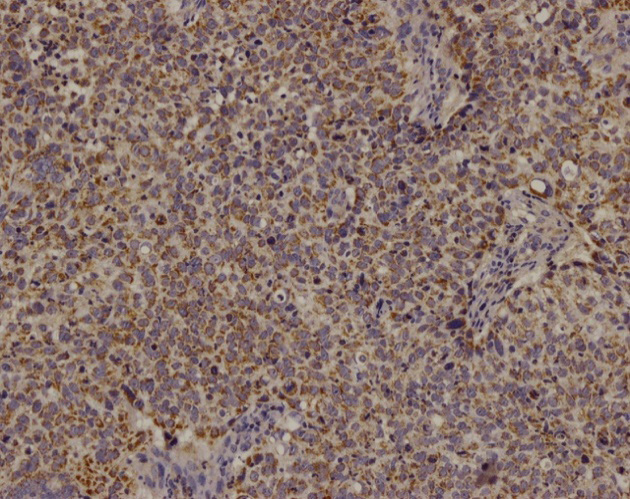
Low expression level of Smac in postchemotherapy tissue (*200).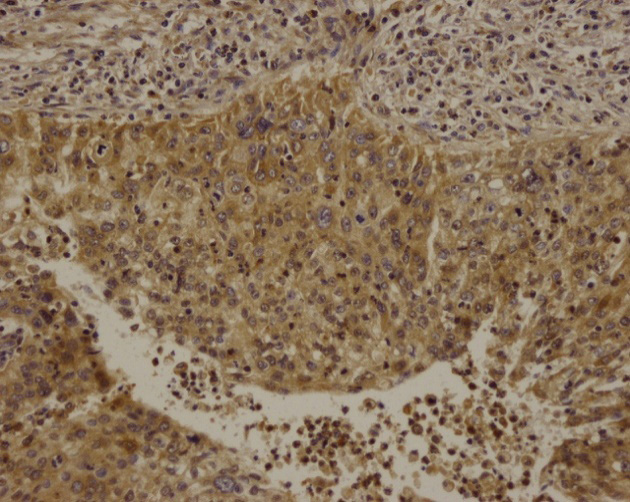
High expression level of Omi/HtrA2 in prechemotherapy tissue (*200).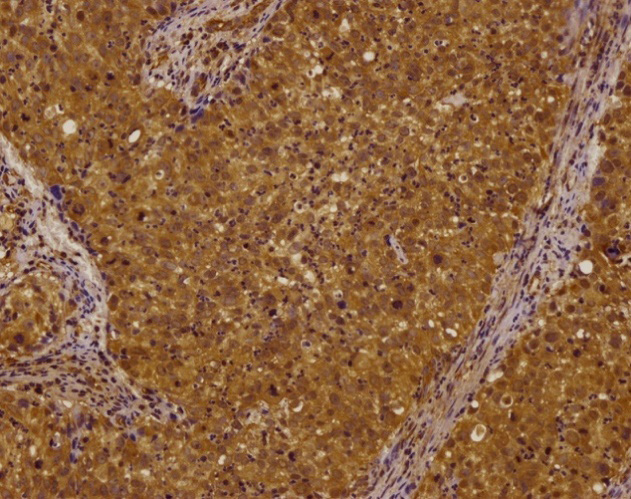
High expression level of Omi/HtrA2 in postchemotherapy tissue (*200).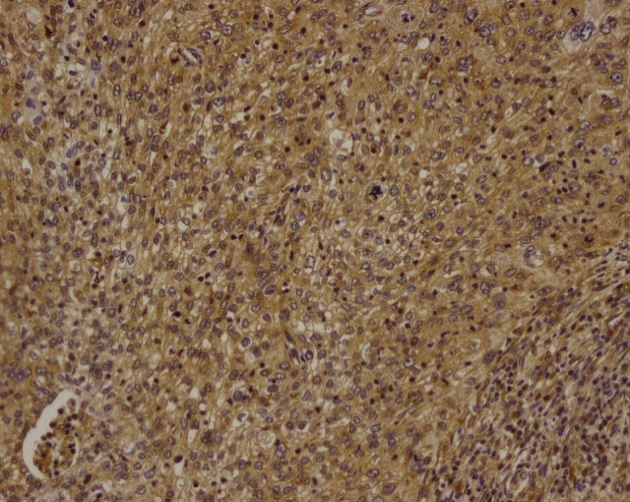
High expression level of survivin in prechemotherapy tissue (*400).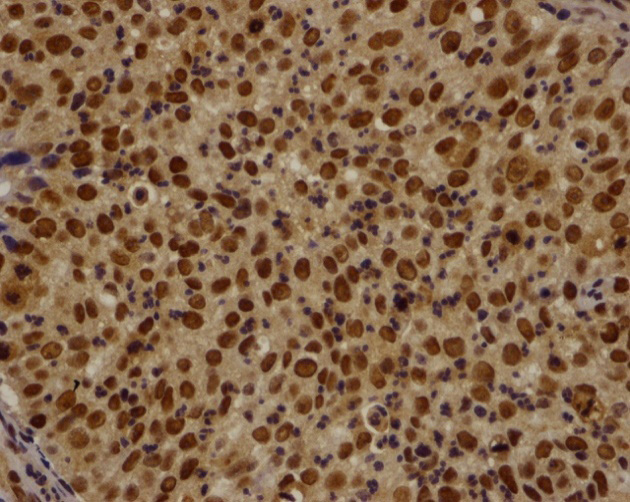
Low expression level of survivin in postchemotherapy tissue (*200).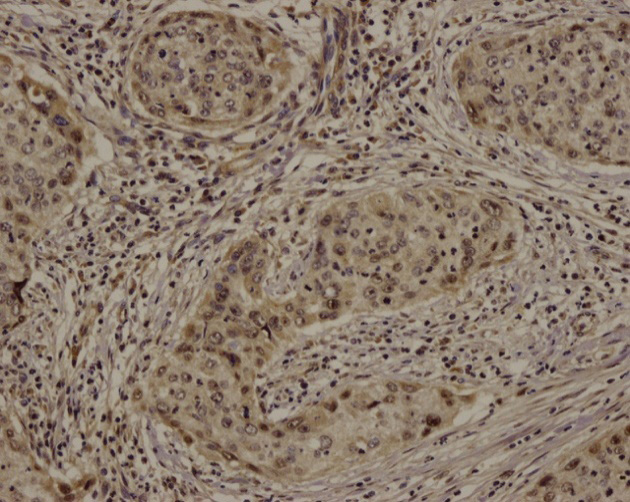
Smac, survivin, Omi/HtrA2, and XIAP expression in pre- and postchemotherapy cervical cancer tissues is shown in Figs 1–8. Smac, Omi/HtrA2, and XIAP were mainly expressed in the cytoplasm, while survivin was expressed in both the nucleus and cytoplasm. Table 3 shows Smac, survivin, Omi/HtrA2, and XIAP expression in pre- and postchemotherapy cervical cancer tissues. Using the Mann-Whitney U-test, we found no significant difference for any of the apoptosis proteins in pre- and postchemotherapy tissues (
High expression level of XIAP in prechemotherapy tissue (*200).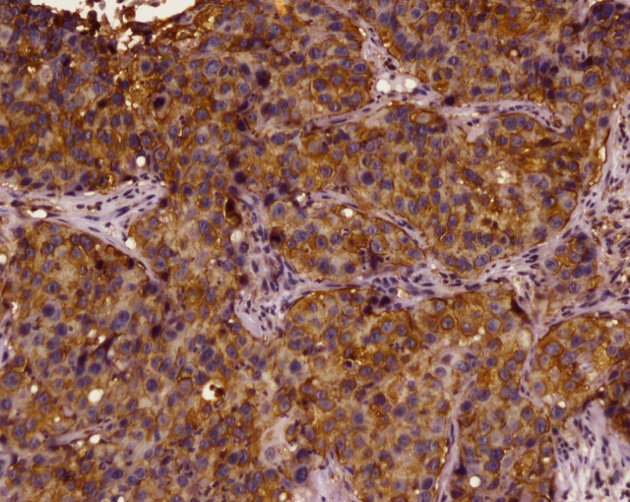
High expression level of XIAP in postchemotherapy tissue (*200).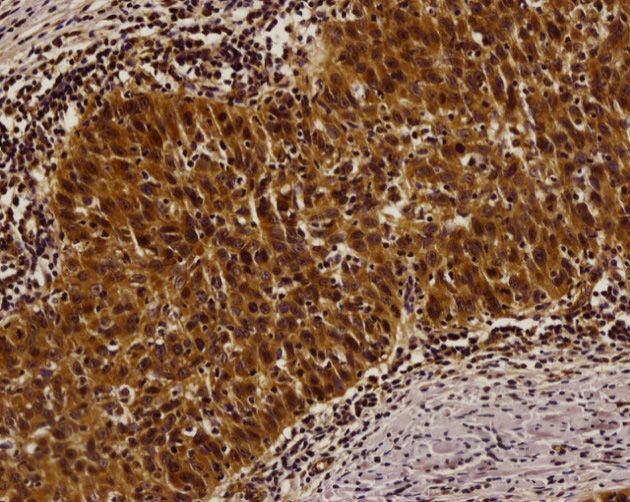
Apoptosis protein expression in pre- and postchemotherapy tissues
Apoptosis protein expression in pre- and postchemotherapy tissues in the CR/PR group
CR/PR, complete response/partial response; Smac, second mitochondria-derived activator of caspase; XIAP, X-linked inhibitor-of-apoptosis protein.
Apoptosis protein expression in pre- and postchemotherapy tissues in the PD/SD group
In pretreatment cervical carcinoma biopsies, Smac expression was correlated with Omi/HtrA2 expression (
Apoptosis protein expression and survival
The median patient follow-up time was 28 months (range 3–97 months), during which 31 cases developed recurrence and 26 died of cervical cancer. The median survival time was 65
Multivariate Cox-regression analysis for OS and PFS
Multivariate Cox-regression analysis for OS and PFS
Smac is a mitochondrial protein that interacts with inhibitor-of-apoptosis proteins (IAPs) and, upon stimulation of apoptosis, is released into the cytoplasm to inhibit the caspase-binding activity of IAPs, including XIAP, IAP1, IAP2, and survivin. IAP antagonists, such as the recently identified Omi/HtrA2, may also play an important tissue- or tumor-specific role. Previous reports have indicated that these apoptosis proteins are associated with sensitivity to chemotherapy or radiotherapy in many cancers, but few studies have focused on apoptosis proteins as potential predictive factors in the outcome of locally advanced cervical cancer patients treated with platinum-based NACT.
In this study, we explored the role of the apoptosis proteins Smac, survivin, Omi/HtrA2, and XIAP in the chemotherapeutic response to cervical cancer. Each protein is considered in turn in the following discussion.
Smac
Smac has been demonstrated to be a predictive factor in many cancers treated with chemotherapy [4, 5, 6]. Recently, some studies have demonstrated that Smac is highly expressed in cervical cancer [8, 9]. In a training set of 76 patients [8], a study showed that the expression level of Smac was significantly and positively associated with survival time in cervical carcinoma. In contrast, another study showed that Smac expression was unrelated to certain clinical characteristics, such as age, grade, and pathological type and that Smac expression plays no role in the development of cervical cancer [9]. In our study, we found that the
Previous studies based on Smac overexpression in other cancers have revealed Smac’s capacity to induce chemosensitivity. Xu et al. [4] indicated that Smac upregulation is a chemosensitization mechanism in esophageal squamous cell carcinoma and that Smac expression differs significantly between chemosensitive and chemoresistant tumors. “Smac-knockdown” was found to significantly suppress cisplatin-induced apoptosis, mitochondrial membrane potential collapse, caspase activation, and cytochrome-c release, leading to cisplatin resistance in vitro and in vivo. Similar findings have been shown for breast cancer [6] and rectal cancer [10]. Compared to chemotherapy, the relationship between Smac and radiotherapy in cervical cancer is clearer [11, 12]. Studies have shown that overexpression of the Smac gene in cervical cancer cell lines significantly enhances the activity of caspase-3 and ameliorates the apoptosis-inducing effects of irradiation on cancer cells [11]. In our study, Smac was expressed at higher levels in chemotherapy-responsive tissues than in nonresponsive tissues at rates of 34% and 23.8%, respectively. However, the difference was not statistically significant. The correlation between Smac and chemosensitivity in cervical carcinoma is currently unknown; further research is needed.
It is worth noting that Smac expression in postche-motherapy tissue was significantly higher than that in prechemotherapy tissue (
Omi/HtrA2
Omi/HtrA2, a newly identified apoptosis regulator, has been found to be overexpressed in renal cancer [13] and colon cancer [14]. Omi/HtrA2 is released from the mitochondria into the cytosol and has been found concurrently with Smac in several in vitro studies [15, 16, 17]. Omi/HtrA2 promotes apoptosis in a manner similar to that of Smac by preventing XIAP via direct binding in vitro [18]. This apoptosis protein was found to be overexpressed in several carcinomas. In a study of the role of Omi/HtrA2 in ovarian cancer, Yang et al. found that cisplatin decreased XIAP levels and increased cytosolic HtrA2/Omi levels in cisplatin-sensitive ovarian cancer cell lines, while cytosolic HtrA2/Omi levels increased and XIAP was downregulated in cisplatin-resistant ovarian cancer cells. The study concluded that cisplatin resistance may result from lower cytosolic Omi/HtrA2 levels in response to cisplatin treatment in human ovarian cancer cells; however, cytosolic Omi/HtrA2 levels are partially regulated by XIAP in ovarian cancer cells. In our study, we found that Omi/HtrA2 expression differed significantly according to the tumor response, demonstrating that Omi/HtrA2 may be involved in the chemotherapy response.
Survivin
Survivin is an apoptosis inhibitor and is involved in the complex network of mitosis regulation. Survivin has attracted attraction for its role in predicting chemosensitivity in tumor cells. In cervical cancer, some studies have reported that lower survivin levels are associated with higher local control and longer survival in women with cervical cancer treated with chemotherapy or radiotherapy. Lee et al. found that survivin overexpression was significantly related to local tumor bulk (
XIAP
XIAP is considered the strongest inhibition-of-apoptosis protein in the IAP family, blocking apoptosis by inhibiting caspase-3, -6, -7, and -9. XIAP is highly expressed in several malignancies, including cervical cancer, and plays an important role in regulating chemoresistance. XIAP expression in cervical cancer tissues is increased with reduced pathological differentiation, suggesting that XIAP may be an important predictor of cervical cancer prognosis. However, in our study, 31.8% of tumors were classified as low differentiation in the 22 XIAP-high tissues, while the rate was 47.1% in the 51 XIAP-low tissues. Unlike the previous study, we found that the lower the XIAP expression was, the poorer the differentiation.
Because of the powerful antiapoptotic ability of XIAP, studies targeting XIAP inhibitors have gained attention. Gagnon et al. found that downregulation of XIAP can enhance the sensitivity of cervical cancer cells to chemotherapy. The authors used small interfering RNA to inhibit the expression of XIAP in HeLa cells and MTT colorimetric analysis to detect the activity of cancer cell growth and found that XIAP RNA interference increased the cell-specific sensitivity to cisplatin and doxorubicin but not to Taxol. However, most studies have been performed in vitro, and to our knowledge, no studies have evaluated the role of XIAP in predicting the chemosensitivity of cervical cancer in vivo. Our study revealed that XIAP expression in the chemotherapy-responsive group was lower than that in the chemotherapy-nonresponsive group; however, the difference was not statistically significant (
A study of 41 cervical carcinoma cases found no association between XIAP expression and age, clinical stage, histology, or menopause but did find an association with disease relapse rates. The results showed that patients with low XIAP expression levels experienced longer survival; however, another study reached a different conclusion [8], finding that the expression level of XIAP was significantly and negatively associated with survival time in cervical carcinoma. Our study found no association between XIAP and prognosis. We believe that most of our patients were in the early cancer stage and this may have contributed to the results.
Given the complexity of the chemosensitization mechanism, we investigated whether each apoptosis protein acts independently or in combination with other proteins in predicting chemosensitization in carcinoma. In a study of breast cancer patients treated with anthracycline-based NACT, a significant negative correlation was found between survivin expression and Smac expression in the pretreatment of breast carcinoma [6]. Following NACT, tumor Smac expression was upregulated, and survivin expression was downregulated. This result is similar to the correlation between Omi/HtrA2 and XIAP in the development of chemoresistance in ovarian cancer, and in our study, we found that Smac expression also had an inverse correlation with Omi/HtrA2 expression. Our results also show that Smac expression correlates with Omi/HtrA2 expression, and in the chemotherapy-nonresponsive group, both Smac and Omi/HtrA2 expression increased after chemotherapy. Therefore, we hypothesized that there is synergy between Smac and Omi/HtrA2 in cervical carcinoma treated with platinum-based chemotherapy, and our results confirmed that the expression of these apoptosis proteins exists in a positive-feedback regulation system. This synergy may play an important role in the apoptosis pathway of human cervical carcinoma and in regulating chemosensitization or chemoresistance.
Many factors affect the prognosis of cervical cancer. Panici et al. evaluated 75 patients with locally advanced cervical cancer treated with neoadjuvant chemotherapy and found that the 3-year survival rate in the CR/PR group was significantly higher than that in the SD/PD group. Osman et al. [3] reported 5-year PFS and 5-year OS rates in NACT-responsive patients with cervical cancer of 61.9% and 72.8%, respectively, which was higher than that in the nonresponsive groups. In our study, the median survival time was 65 months, which is far lower than reported survival because nearly 1/3 of our group consisted of chemotherapy-nonresponsive patients. Additionally, the median survival time of chemotherapy-responsive patients was 83.5 months, and the median survival time of nonresponsive patients was 35.3 months. The prognosis in the chemotherapy-responsive group was significantly higher than that of the nonresponsive group (
Conclusion
Our results indicate that the low expression level of survivin and high expression level of Omi/HtrA2 in chemotherapy-responsive cervical carcinomas significantly increase chemosensitivity in cervical cancer. Antiapoptotic protein and proapoptotic proteins play important roles in the response to chemotherapy, and Smac may have a cooperative relationship with Omi/HtrA2, leading to carcinogenesis and chemotherapy resistance.
Footnotes
Acknowledgments
We thank Fang Liu, Kun Jia and other members from State Key Laboratory of Molecular Oncology, Cancer Institute & Hospital, Chinese Academy of Medical Sciences and Peking Union Medical College for reading of the manuscript and helpful discussion.
Conflict of interest
None.
