Abstract
OBJECTIVE:
Emerging studies show that microRNAs (miRNAs) play a essential role in tumorigenesis. Deregulation of miR-494 is frequently observed in various human cancers including non-small cell lung cancer (NSCLC). However, little is known about the clinical significance of serum miR-494. The aim of this study was to investigate the diagnostic and prognostic value of serum miR-494 for NSCLC.
METHODS:
We first compared miR-494 levels between NSCLC cell lines and lung bronchus epithelial cell line. A total of 90 NSCLC patients and 50 healthy controls were included in this study. MiR-494 levels were examined in serum samples by using real-time quantitative reverse transcription polymerase chain reactions. Association between serum miR-494 levels and the prognosis of NSCLC was further analyzed.
RESULTS:
Our results showed that miR-494 was elevated in NSCLC cell lines. Serum miR-494 levels were significantly increased in patients with NSCLC compared to healthy controls. Area under receiver operating characteristic (ROC) curve was 85.4%. In addition, serum miR-494 levels decreased remarkably when patients received effective therapy. High serummiR-494 levels were significantly associated with higher incidence of lymph node metastasis, advanced clinical stage and higher histological grade. Moreover, survival analysis demonstrated that patients in the high serum miR-494 group had a poorer 5 year overall survival and disease free survival compared with the patients in the low serum miR-494 group. Multivariate analysis showed that serum miR-494 was an independent risk factor.
CONCLUSIONS:
In conclusion, serum miR-494 was significantly elevated in NSCLC patients and closely correlated with poor clinical outcome, indicating that serum miR-494 might be a useful diagnostic and prognostic marker for NSCLC.
Introduction
Lung cancer is the leading cause of cancer-related mortality around the world and represents a significant public health issue [1]. Non-small cell lung cancer (NSCLC) is the major form and accounts for about 85% of of all cases of lung cancer [2]. Despite great progress has been achieved in diagnosis and therapeutic strategies, the prognosis of NSCLC remains abysmal, with less than 15% overall 5-year survival rate [3, 4]. Therefore great effort has been made to identify predictive biomarkers for diagnosis and prognosis of NSCLC.
MicroRNAs (miRNAs) are short, single stranded, highly conserved non-coding RNAs that have critical functions in gene regulation and affects various biological processes such as proliferation, differentiation, development and survival [5]. MiRNAs supress the synthesis of proteins by mRNA degradation or translational repression. A significant amount of evidence has demonstrated that dysregulation of miRNAs contributes to the growth and metastasis of NSCLC [6, 7]. The expression level of miR-152 was significantly downregulated in NSCLC specimens. In addition, miR-152 inhibition promoted the migration and invasion capacity of lung cancer cells and vice versa. Moreover, neuropilin-1 was identified as a downstream target of miR-152, indicating miR-152 acts as a tumor suppressor in NSCLC [8]. A serum miRNAs signature including miR-193b, miR-301, miR-141 and miR-200b could discriminate lung cancer patients from healthy controls with high accuracy, indicating serum miRNAs are promising biomarkers for NSCLC diagnosis [9].
MiR-494 is aberrantly expressed in various types of cancers such as breast cancer, glioma, prostate cancer and NSCLC [10, 11, 12, 13]. In addition, ovexpression of tissue miR-494 is associated with poor prognosis of NSCLC and thus miR-494 probably plays an oncogenic role in NSCLC [13]. However, tissue biopsy has limitations in monitoring cancer develepment as well as the therapeutic responses in real time. Liquid biopsy, which are noninvasive and can be easily repeated, has become an attractive method for screening diagnostic and prognostic biomarkers for NSCLC [14]. In this study, we investigated the expression level of serum miR-494 in patients with NSCLC as well as compared their expression with the clinicopathological parameters and prognosis of NSCLC.
Methods
Cell culture
NSCLC cell lines (A549, H520 and EPLC-32M1) and 16HBE normal lung bronchus epithelial cell line were obtained from the American Type Culture Collection (ATCC). All the cell lines were cultured in Dulbecco’s modified Eagle’s medium (Invitrogen, Carlsbad, CA, USA) supplemented with 10% fetal calf
The expression level of miR-494 in NSCLC cell lines.
Serum miR-494 was elevated in NSCLC and its diagnostic value.
All the procedures in this study were approved by the local Ethics Committees at the Third Affiliated Hospital of Anhui Medical University, and informed consents were obtained from each participant. Ninety serum samples of NSCLC patients as well as clinical and pathological data were obtained for the investigation. All of the NSCLC patients were pathologically confirmed and tumor node metastasis (TNM) staging classification was determined by UICC/AJCC 7th edition for the lung. Fifty serum samples from healthy volunteers were used as control.
Correlation between serum miR-494 levels and different clinicopathological variables in patients with NSCLC
Correlation between serum miR-494 levels and different clinicopathological variables in patients with NSCLC
The procedures for processing the blood samples are as follows: peripheral venous blood samples were withdrawn from NSCLC patients and healthy controls and were centrifuged at 2000 g for 10 min at room temperature to obtain serum. These serum samples were rapidly frozen and stored at
MiRNAs were extracted from 200
Serum miR-494 was significantly reduced in NSCLC patients following therapy.
The RNA concentration was determined using a NanoDrop ND-1000 spectrophotometer (NanoDrop ND-1000, Nanodrop technologie, DE, USA) and first-strand cDNA was synthesized using a TaqMan MicroRNA Reverse Transcription Kit (Applied Biosystems, Foster City, CA, USA). Amplifications were performed using a miScript SYBR Green PCR kit (Qiagen) and qRT-PCR was run on Applied Biosystems 7500 Real-Time PCR System (Applied Biosystems). Exogenous cel-miR-39 was used as an internal standard and expression level of serum miR-494 was quantitatively analyzed by the comparative threshold cycle (2
All statistical analyses were performed using the SigmaPlot v12.5 software (Systat Software Inc., San Jose, CA, USA) or GraphPad Prism 6.0 for Windows (GraphPad Software, La Jolla, CA, USA). The data didn’t follows a normal distribution. Mann-Whitney U test was used to compare the serum miR-494 levels between NSCLC patients and healthy controls. Continuous variables were analyzed with Student’s t-test/One way ANOVA and categorical variables were analyzed using the
Results
MiR-494 levels were upregulated in NSCLC cell lines
We compared the expression level of miR-494 between three NSCLC cell lines (A549, H520 and EPLC-32M1) and 16HBE normal lung bronchus epithelial cell line. Our results showed that miR-494 was significantly increased in NSCLC cell lines compared to the control (
The association between serum miR-494 levels and overall survival as well as disease free survival.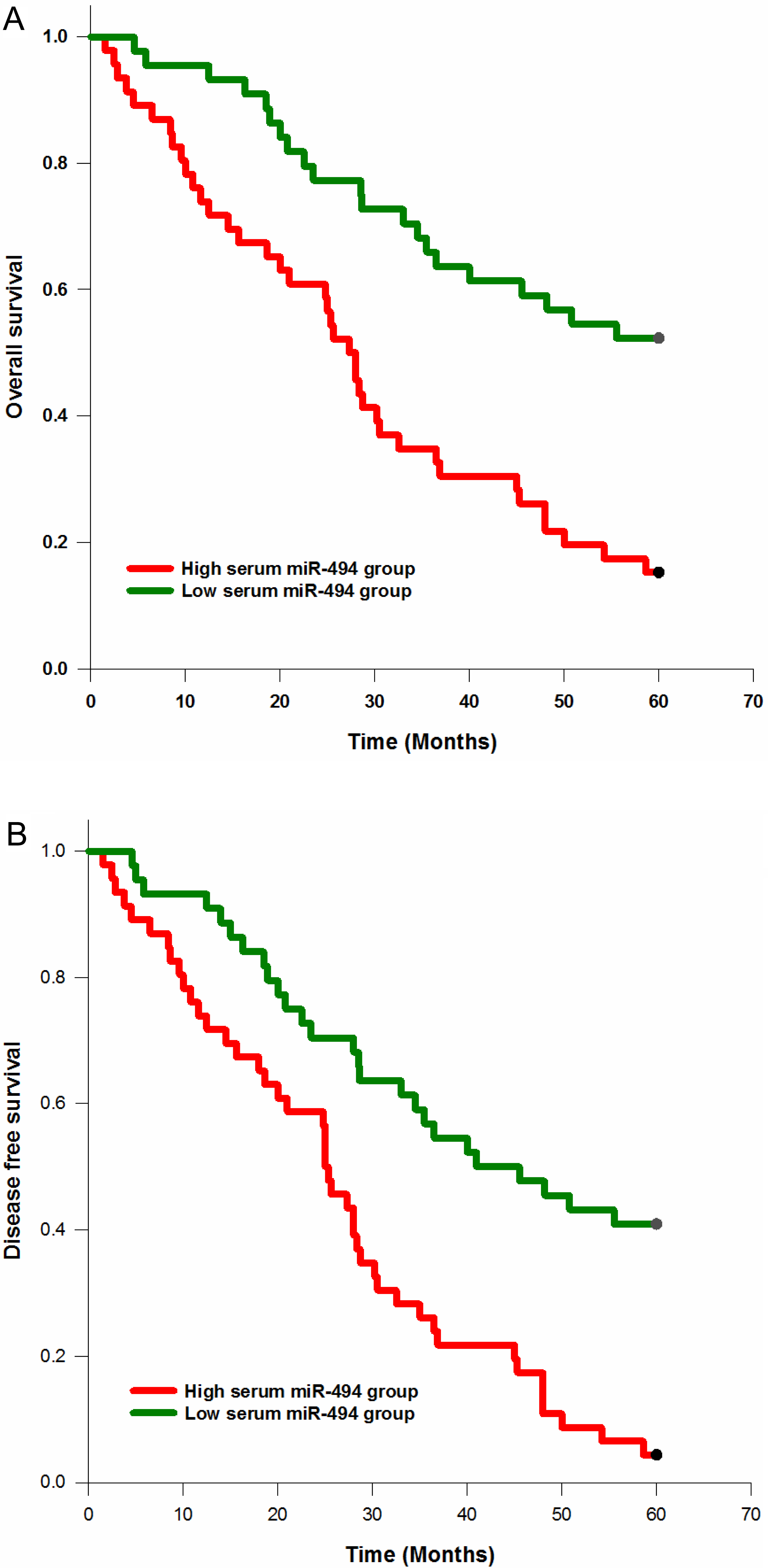
The median serum miR-494 levels in patients with NSCLC were remarkably upregulated compared with healthy individuals (
We then evaluated the changes of serum miR-494 levels in NSCLC patients after treatments. Our results showed that serum miR-494 levels was significantly reduced following therapy (
Serum miR-494 correlates with clinicopathological features of NSCLC
Chi-squared test was used to analyze the association between serum miR-494 levels and clinicopathological parameters of NSCLC. Our data showed that high serum miR-494 levels were strongly correlated with higher incidence of lymph node metastasis (
Serum miR-494 levels predicted survival in NSCLC
Kaplan-Meier method was used to explore the correlation between serum miR-494 levels and survival in patients with NSCLC. The results showed that the patients with high expression of serum miR-494 had a significantly lower 5 year overall survival compared to those with low expression of this small molecule (
As shown in Table 2, multivariate Cox regression analysis indicated that elevated serum miR-494 was also an independent risk factor in NSCLC (
Multivariate analysis of overall survival in patients with NSCLC
Multivariate analysis of overall survival in patients with NSCLC
In our present study, miR-494 was obviously up-regulated in NSCLC serum samples and cell lines compared with their respective controls. In addition, serum miR-494 had a good performance to discriminate NSCLC patients from healthy controls, and its levels were sensitive to effective treatment. Furthermore, high serum miR-494 levels were strongly associated with unfavorable clinicopathological variables and poor prognosis of NSCLC. These results suggest that miR-494 acts as an oncomiR in NSCLC and serum miR-494 might be a promising serum biomarker for diagnosis and prognosis of NSCLC.
Consistent with our results, miR-494-3p overexpression was associated with lung cancer progression in mice and with poorer survival in lung cancer patients. In addition, miR-494–3p promoted oncogenic activities of lung cancer cells by regulating NOTCH1 and PTEN/PI3K/AKT signaling [15]. MiR-494 was upregulated in lung cancer tissues and a negative correlation was observed between miR-494 expression and PTEN expression. Moreover, high miR-494 expression in lung cancer was correlated with worse clinical outcome [13]. Interestingly, a recent study showed that lung cancer cells could secret and deliver miR-494 into human vascular endothelial cells to promote angiogenesis by downregulating PTEN and activating Akt/eNOS pathway [16].
Similarly, miR-494 was significantly elevated in colorectal cancer tissues and cell lines. MiR-494 upregulation was associated with adverse clinical stage and distant metastasis as well as poorer survival rates. In addition, miR-494 increased the invasion and migration capability of cancer cells by inhibiting PTEN [17]. MiR-494 was increased in glioma cells subjected to ionizing radiation. MiR-494 promoted the migration and invasive capacity of cancer cells by regulating various components such as MMP2, EGFR, Akt and ERK [18].
However, miR-494 has also been reported to function as a tumor suppressor gene in many types of cancers. For instance, miR-494 levels were reduced in oral cancer and upregulation of miR-494 inhibited the proliferative capacity of oral cancer cells, indicatingmiR-494 played a tumor suppressive role in oral cancer. In addition, HOXA10 was identified as a downstream target of miR-494 [19]. Similarly, miR-494 was decreased in breast cancer tissues and cell lines. Ectopic expression of miR-494 inhibited the proliferation and metastasis of cancer cells both in vitro and in vivo by modulating PAK1 [20]. The concrete molecular function of a specific miRNA is closely correlated with the tissue microenviroment, which might account for the oncogenic and tumor suppressive role ofmiR-494 in different cancers.
A possible shortcoming of our study was that we only detected serum miR-494 levels in relatively small group. Large multicenter studies are required to validate our findings to minimize the potential bias. In addition, we did not compare the dignostic power of serum miR-494 with current available biomarkers such as cancer antigen-125, carcinoembryonic antigen and SCC antigen. Moreover, the underlying molecular mechanisms of miR-494 in NSCLC needs further investigation.
Taken together, our results showed that miR-494 levels were upregulated in NSCLC cell lines and patients. Moreover, high serum miR-494 levels were positively correlated with poor prognosis of NSCLC, suggesting that miR-494 may function as a tumor promoter gene in NSCLC. Serum miR-494 might not only serve as a diagnostic and prognostic biomaker for NSCLC, but aslo a potential novel therapeutic target.
Footnotes
Conflict of interest
We deny any conflict of interest.
