Abstract
BACKGROUND:
Despite the fact that weaning from mechanical ventilation (MV) is one of the main rehabilitation goals in patients with spinal cord injury (SCI), controversies are still open about the optimal rehabilitation approach.
OBJECTIVE:
This systematic review aimed at characterizing the rehabilitation interventions currently available to optimize weaning from MV in SCI patients.
METHODS:
On April 12
RESULTS:
Out of 413 records, 14 studies were included (2 randomized controlled trials, 7 observational studies, and 5 case reports). Most of the studies assessed a comprehensive rehabilitation approach, including high tidal volume ventilation, positioning, mechanical lung recruitment maneuvers, secretion management strategies, respiratory muscle training, and electrical stimulation.
CONCLUSION:
Our findings suggested that a comprehensive rehabilitation intervention might have a role in reducing MV duration in patients with SCI. Further studies are needed to better characterize the optimal rehabilitation strategies for enhancing functional recovery of patients with SCI.
Introduction
Spinal cord injury (SCI) is a detrimental neurological condition leading to impairment in motor, sensory, and visceral controls [1, 2, 3, 4]. It has been estimated that SCI prevalence ranges from 13.0 per million to 163.4 per million people with a high heterogeneity among countries [5, 6, 7]. In addition, approximately 75% of traumatic SCI involve young adults [5, 6, 7]. Therefore, health-care costs are extremely high, while personal and social costs are inestimable.
In this scenario, rehabilitation plays a pivotal role with growing evidence underlining the needing for a comprehensive rehabilitation approach targeting the multilevel physical and psychosocial disabilities of patients with SCI, reducing not only functional impairment and assistance costs but also improving health-related quality of life (HR-QoL) of patients with SCI [8, 9, 10, 11, 12, 13].
On the other hand, patients with cervical spinal cord lesions may suffer from a higher level of impairment in different body functions, including cough or breathing due to impaired control of abdominal and/or diaphragm muscles [14]. In particular, it has been reported that more than 90% of traumatic cervical SCIs require intubation, while more than 40% of those patients require chronic mechanical ventilation (MV) [15, 16]. Albeit MV is a life-saving intervention in patients with acute respiratory failure, several studies highlighted that prolonged MV crucially affects functional recovery and residual disability, with harmful consequences on length of stay and health-related quality of life (HR-QoL) [17, 18, 19, 20, 21]. Moreover, prolonged MV has been associated with a higher risk for infections, ventilator-associated pneumonia (VAP), and atelectasis [22]. As a result, prolonged MV might significantly affect clinical outcomes of patients with SCI, leading to a higher risk of death and lower survival [23, 24, 25].
Taken together, these findings highlighted the need for effective rehabilitation programs optimizing weaning from MV in patients with SCI not only to improve disability and promote functional recovery but also to reduce clinical complications and improve life expectancy [7, 26].
In recent years, growing evidence highlighted the benefits of respiratory rehabilitation interventions in weaning from MV. More in detail, the recent meta-analysis by Worraphan et al. [27] underlined the effectiveness of inspiratory muscle training (IMT) and early mobilization (EM) in facilitating weaning from MV. However, given the kinesiological differences in respiratory mechanics and the differences in respiratory tract innervation following SCI [28, 29], evidence in this specific population is needed to support the effectiveness of rehabilitation in the weaning process of patients with SCI.
Interestingly, the systematic review by Schreiber et al. [30] assessed the patient’s characteristics that might affect separation from MV in patients with SCI. However, the authors did not focus on rehabilitation approaches aiming at optimizing the weaning process.
Despite the effects of rehabilitative interventions in weaning from MV have been deeply studied [31, 32, 33], there is no clear evidence about specific rehabilitation strategies enhancing the weaning process in patients with SCI. Moreover, to the best of our knowledge, no previous systematic review assessed the effects of different rehabilitation approaches proposed to improve weaning from MV in SCI patients.
Therefore, the aim of this systematic review was to summarize the current evidence about the effects of rehabilitative interventions in reducing MV duration and enhancing the weaning process in patients with SCI.
Methods
Registration
This systematic review has been performed in accordance with the Preferred Reporting Items for Systematic Reviews and Meta-analyses (PRISMA) statement [34]. The international prospective register of systematic reviews (PROSPERO) was preliminary searched for similar review protocols in progress without showing similar reviews. The systematic review was submitted to PROSPERO and accepted on 13
Search strategy
Five databases (PubMed/Medline, Scopus, Web of Science, Cochrane Central Register of Controlled Trials (CENTRAL), and PEDro) were systematically searched simultaneously for studies published until April 12
Selection criteria
In accordance with the PICO model [35], we considered eligible clinical trials satisfying the following criteria:
P) Participants: mechanically ventilated patients with spinal cord injury, age I) Intervention: we considered all rehabilitation and/or physiotherapy interventions administered as exclusive or integrated interventions. C) Comparator: any comparator. O) Outcome: the primary outcomes were weaning duration (defined as time between first assessment and the absence of MV for 48 hours), MV duration (defined as time between start of MV and successful weaning), and weaning success rate (express as percentage of patients weaned per whole sample). The secondary outcomes were: i) Pulmonary function; ii) Extubation or decannulation time; iii) Length of stay; iv) Safety.
Only studies published in peer-reviewed International Journal were included. The exclusion criteria were: i) studies involving animals; ii) participants with pregnancy, clinical instability (defined as hemodynamic alterations, respiratory events, abnormal laboratory values, reduced level of consciousness or temperature alterations), or palliation; iii) Masters or doctorate theses, conference proceedings, and literature review; iv) language other than English. No publication date restriction was applied.
After duplication removal, the records were screened by two investigators that independently reviewed titles and abstracts. The articles meeting the enrolment criteria proceeded to the full-text review screening phase. Any disagreements were discussed with a third reviewer to reach consensus.
Lastly, relevant full-text records were assessed in by two independent reviewers; in case of disagreement, it was solved by asking a third reviewer.
All data were extracted by two independent reviewers through Excel. Any disagreement was solved by discussion between the two reviewers or by consulting a third reviewer.
The following data were extracted: 1) Authors; 2) Journal; 3) Publication year; 4) Nationality; 5) Population characteristics; 6) Intervention characteristics; 7) Comparator characteristics; 8) Outcomes; 9) Main findings.
A descriptive approach was used to synthesize both study characteristics and data extracted. The studies were grouped for the syntheses basing on the outcomes assessed. Moreover, subgroup analysis has been performed based on the type of intervention assessed.
Quality assessment and risk of bias
The quality assessment was performed through Joanna Briggs Institute Critical Appraisal Checklist for Randomized Controlled Trials, JBI Critical Appraisal Checklist for Cohort Studies, JBI Critical Appraisal Checklist for Case Series, or JBI Critical Appraisal Checklist for Case Reports basing on the study design [36]. Two independent reviewers performed independently the quality assessment. A third reviewer was involved in case of disagreement to achieve consensus.
Results
Study characteristics
A total of 407 records were identified from 5 databases assessed, while 6 records were identified from other sources. After duplication removal, 363 studies were assessed for eligibility and screened for title and abstract. As a result, 332 records were excluded, and 31 studies were subsequently screened in full text. Lastly, 14 studies [37, 38, 39, 40, 41, 42, 43, 44, 45, 46, 47, 48, 49, 50, 51, 52, 53] were included in the present systematic review. Figure 1 shows further details about the article selection process through the PRISMA flow diagram. Supplementary Table 2 shows the list of the 17 full-text studies assessed for eligibility and excluded, reporting the reasons for exclusion.
PRISMA 2020 flow diagram.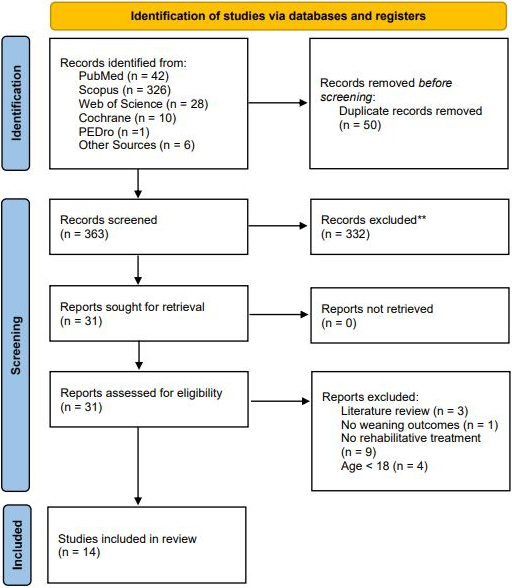
As a result, the following studies were included in the present systematic review: Atito-Narh et al. [37], Duarte et al. [38], Fenton et al. [39], Gundogdu et al. [40], Gutierrez et al. [41], Gutierrez et al. [42], Hatton et al. [43], Kim et al. [44], Korupolu et al. [45], McCaughey et al. [46], Peterson et al. [47], Toki et al. [50], Wong et al. [52], and Zhang et al. [53].
The studies included were published between 1999 [47] and 2021 [38, 43, 45] and were conducted in America (USA
The patients included were characterized by a mean age ranging between 27.24
All studies [37, 38, 39, 40, 41, 42, 43, 44, 45, 46, 47, 48, 49, 50, 51, 52, 53] included in this systematic review assessed patients with cervical SCI, while two studies [37, 45] included also patients with thoracic SCI. Interestingly, most of the studies included [37, 38, 40, 43, 44, 45, 46, 47, 48, 49, 50, 51, 52, 53] assessed acute SCI. In contrast, the RCT of Fenton et al. [39] assessed patients with sub-acute traumatic SCI, while the studies by Gutierrez et al. [41, 42] assessed patients with chronic SCI. Asia Impairment Scale (AIS) was used to characterize the functional impairment of SCI in eleven studies [37, 38, 39, 40, 42, 44, 45, 46, 50, 52, 53], while in three studies [41, 43, 47] the functional impairment was not reported. Table 1 summarizes in detail the sample characteristics of both intervention groups and comparator groups of each study included in the present review.
Rehabilitation interventions have been classified as changing in MV settings, mobilization/positioning techniques, respiratory muscle training, abdominal or diaphragmatic electrical stimulation, recruitment manoeuvrers (manual hyperinflation or intermitted positive-pressure breathing – IPPB), and secretion management (clearance of airway, swallowing therapy, tracheal suctioning).
Changing in MV settings: Five studies [39, 43, 45, 47, 52] assessed the effects of high Vt mechanical ventilation. More in detail, the RCT of Fenton et al. [39] assessed the effects of high Vt at 20 ml kg
Mobilization/positioning: Two studies [37, 42] assessed mobilization/positioning as a potential treatment for improving weaning of SCI patients. More in detail, the effects of Trendelenburg chest optimization positioning were assessed in the RCT by Gutierrez et al. [42]. Each positioning session was maintained for about 30 minutes. In contrast, Atito-Narh et al. [37] assessed the effects of different positioning strategies in their treatment protocol. More in detail, the positioning protocol Main characteristics of the studies included
Abbreviations: AIS
included physical turns from side to side and back 3–4 hourly and mobilise in wheelchair.
Respiratory muscles training: Three [40, 41, 53] studies assessed respiratory muscle training proposing different therapeutic strategies. In particular, the case series of Gutierrez et al. [41] assessed the effect of a resistance and endurance training protocol including 4 phases (pretraining optimization, inspiratory/expiratory resistance training, on-vent endurance training, and off-vent endurance training). On the other hand, Zhang et al. [53] assessed the effect of an inspiratory muscle training protocol. In particular, it was composed of passive activities (stretching of the intercostal muscles, bed tilting, passive movement of the scapula and the proximal end of the upper limbs), and strength and endurance training on the diaphragm. Lastly, Gundogdu et al. [40], assessed the effect of an inspiratory muscle training protocol with a threshold IMT device, administered in 10 repetitions, three times a day, five days per week until decannulation.
Abdominal or diaphragmatic electrical stimulation: Electrical stimulation was assessed in two studies [38, 46]. Duarte et al. [38] assessed the effects of transcutaneous electric diaphragmatic stimulation (TEDS) administrated for 20 minutes per session, twice a day, for 7 days a week. TEDS was administrated with a frequency of 30 hertz, pulse width of 1 ms, rise time of 0.7 ms, and current intensity of 60 milliamps. McCaughey et al. [46] assessed the effects of Abdominal Functional Electrical Stimulation (AFES), 20–40 minutes per session, five sessions per week on 4 alternate weeks, for 8 weeks.
Lung hyperinflation/recruitment maneuvers: Gutierrez et al. [41, 42] and Atito-Narh et al. [37] assessed lung hyperinflation maneuvers with ventilators or manual resuscitation bag.
Secretion management (including tracheal suctioning and swallowing rehabilitation): Four studies [37, 40, 44, 52] assessed the effects of secretion management, clearance of airway, swallowing therapy, or tracheal suctioning. In particular, Kim et al. [44] assessed the effects of mechanical insufflation-exsufflation (MI-E) or manually assisted cough (MAC) by abdominal thrust followed by suctioning or self-oral expectoration. Similarly, Wong et al. [52] assessed the effects of high-frequency percussive ventilation (HFPV) and mechanical insufflation-exsufflation (MI-E) for managing secretion, every 2–4 hours, for 30 to 45 minutes.
Interestingly, Atito-Narh et al. [37] included swallowing rehabilitation in their protocol, consisting of bedside assessment of swallow performance with deflated cuff before administering oral intake. Moreover, in the study by Gundogdu et al. [40] patients received daily care for oral hygiene, thermal (cold) and tactile stimulation, head and trunk positioning, dietary modification, swallowing maneuvers and oral motor exercises, including the lip, tongue and jaw movements according to the different patient characteristics for 60 min a day, 5 days a week for 3 to 6 weeks.
All rehabilitation programs assessed in the present systematic review have been summarized in detail in Table 1.
The intervention groups were compared with standard/low volume mechanical ventilation [39, 43, 45, 47], usual care/standard weaning protocol [38, 46], or positioning [42]. In particular, in the RCT performed by Gutierrez et al. [42], the intervention group, which performed Trendelenburg chest optimization (TCO), was compared with Supine Chest Optimization (SCO), setting the Vt on 20 mL/kg of ideal body weight for 30 min per session. All control protocols assessed in the present systematic review have been summarized in Table 1.
Primary Outcomes – Weaning duration, MV duration, and weaning success rate
Weaning duration has been assessed in eight trials [37, 38, 39, 40, 45, 46, 47, 52], two studies [38, 45] assessed MV duration, and four studies [41, 44, 45, 53] assessed weaning success rate. More in detail, the RCT performed by Fenton et al. [39] showed no significant differences in mean days to wean between high-Vt group and standard-Vt group (IG: 14.5 days, CG: 14 days;
In the case series by Atito-Narh et al. [37] assessing the effects of a comprehensive rehabilitation approach (ventilatory support, tracheal cuff deflation, mobilization of secretions with pressure monitored hyperinflation, routine bagging, positioning, swallowing and speech), the mean weaning duration was 56.1
Wong et al. [52] assessed the effects of high-Vt, MIE and HFPV, 13 (neurological levels C3-C4) were successfully weaned from MV, nine with level of injury at C1, C2, and C3 were not weaned, one patient with C4 AIS B needed night-time ventilation. Gutierrez et al. [41] reported that all tetraplegic patients with low neurological levels and completing the prescribed training underwent successful weaning from MV. Kim et al. [44] showed a weaning success rate of 24.2% in patients with cervical spinal cord injury. Lastly, Zhang et al. [53] reported successful weaning from MV in the patient that underwent to IMT program.
Secondary outcomes – pulmonary function
Pulmonary function was assessed in eight studies [37, 39, 40, 41, 42, 46, 50, 53]. In particular, in the RCT by Fenton et al. [39], no significant differences between groups were reported in terms of FVC values. However, significant within-group differences were reported in both groups (
Concurrently, the RCT by Gutierrez et al. [42] underlined that Spontaneous Breathing Trial (SBT) duration was significantly longer in TCO group compared to SCO group (IG: 87.67
In the cohort study by Gundogdu et al. [40], the means of the maximal inspiratory pressure (MIP), maximal expiratory pressure (MEP) and peak cough flow (PCF) values of MV-dependent patients after the weaning protocol significantly improved (MIP:
Secondary outcomes – extubation or decannulation
In the cohort study by Gundogdu et al. [40], the mean duration of decannulation was 31.7
Joanna Briggs Institute Critical Appraisal Checklist for the studies included
Joanna Briggs Institute Critical Appraisal Checklist for the studies included
The study by Duarte et al. [38] reported differences in length of stay in ICU between TEDS group and standard weaning protocol group (IG: 31
Secondary outcomes – ventilator dependence at discharge
Hatton et al. [43] showed that ventilator dependence at 30 hospital days or hospital discharge was significantly increased in high-Vt group (82% of patients) compared with standard-Vt group (38% of patients) (
Secondary outcomes – safety
The RCT by Fenton et al. [39] reported no significant differences in incidence of adverse pulmonary events (
Quality assessment
The quality assessment was performed following the Joanna Briggs Institute Critical Appraisal Checklist for Randomized Controlled Trials, JBI Critical Appraisal Checklist for Cohort Studies, JBI Critical Appraisal Checklist for Case Series, or JBI Critical Appraisal Checklist for Case Reports basing on the study design [36]. The studies included [39, 40, 42, 43, 44, 45, 46, 47, 52, 53] presented at least one serious risk of bias, which translated into an overall serious risk of bias for that study. The main quality concerns included the lack of data on baseline characteristics of study participants, nonrandom sampling approaches (convenience samples), missing data, and lack of a reliable tool to estimate and report outcomes. Further details about the quality assessment of each study included in this review are shown in Table 2.
Discussion
To date, rehabilitation could be considered as a milestone in the complex management of SCI patients [54, 55, 56], with several studies proposing different approaches to enhance the weaning process in mechanically ventilated SCI patients [37, 38, 39, 40, 41, 42, 43, 44, 45, 46, 47, 48, 49, 50, 51, 52, 53]. However, the optimal rehabilitation approach is still a challenge for physicians and researchers, considering that no clear indications are currently available for mechanically ventilated SCI patients.
Therefore, by this systematic review we aimed at providing a broad overview about the current rehabilitation strategies aiming at optimizing the weaning process of these patients, characterizing the specific rehabilitation approaches in order to reduce the weaning duration, improve functional outcomes and minimize MV related complications.
Interestingly, six main rehabilitative strategies have been identified in the scientific literature: i) high-Vt ventilation, ii) positioning, iii) mechanical lung recruitment maneuvers, iv) secretion management strategies, v) respiratory muscle training, and vi) electrical stimulation.
To date, high-VT ventilation in patients with SCI is commonly used in the clinical practice [57] and supported by specific guidelines [58]. In this context, SCI patients were frequently not affected by chronic pulmonary conditions, and “healthy lungs” should not be damaged by relatively high-volume ventilation. Moreover, a tidal volume of up to 1000 ml may represent approximately 30% of the normal inspiratory capacity of a healthy adult [29]. In addition, higher VTs stretch the airways smooth muscles, and promote the production of pulmonary surfactant, the alveolar surface tension with positive implications in the prevention of peripheral collapse of small airways [52]. Our results identified five studies [39, 43, 45, 47, 52] assessing the role of high-Vt compared to low-Vt, highlighting conflicting results. More in detail, two retrospective analyses [47, 52] supported higher VTs (more than 20 ml/kg IBW), suggesting positive implications for weaning process duration and complications rate. In addition, Wong et al. [52] suggested that higher VTs might optimize the respiratory status, vocalization, and participation in rehabilitation programs of patients with SCI, reducing MV duration. On the other hand, it should be noted that all patients underwent a comprehensive pulmonary rehabilitation program including HFPV, MIE and high-VT ventilation. Therefore, it is impossible to draw conclusions about each single rehabilitation intervention. On the contrary, the RCT by Fenton et al. [39] confirmed the safety of high-Vt ventilation (20 ml/kg vs 10 ml/kg IBW), without reporting difference in the weaning duration. Lastly, the more recent studies by Hatton et al. [43] and Korupolu et al. [45] raised doubt about the safety of this rehabilitation approach, since no advantages in weaning duration were found and a higher incidence of pneumonia and pulmonary adverse events were reported. Surprisingly, both studies did not report any interventions for the management of mucus encumbrance or other interventions aimed to prevent secretion stagnation and atelectasis [43, 45].
Altogether, these results underlined some concerns about the effectiveness of high-Vt ventilation. Despite these considerations, high-Vt ventilation should not be proposed alone, but included in a comprehensive rehabilitation intervention targeting the multilevel pulmonary impairment of patients with SCI.
In contrast, secretion management strategies were described in four studies [37, 40, 44, 52] reporting promising results in terms of weaning duration [37, 40, 52] or weaning success rate [44]. Despite the positive data, no study assessed the role of secretion management strategies without other interventions.
Although positioning techniques play a key role in the management of patients with SCI due to their widely documented role in secondary complications prevention [59], only two studies [37, 42] assessed mobilization/positioning as a potential treatment for improving weaning of SCI patients. Intriguingly, the RCT by Gutierrez et al. [42] reported significant differences in patients undergoing Trendelenburg positioning compared to supine chest optimization in terms of SBT duration. However, no significant results were reported in terms of weaning duration and weaning success rate, probably due to the small sample size. On the other hand, the case series from Atito-Nahr et al. [37] reported positive results of a specific positioning protocol included in a comprehensive rehabilitation approach. Further studies might clarify the role of different positioning in the complex rehabilitation program also improving pressure ulcer risk, joint contractures, swallowing optimization and several other disabling conditions that might benefit from positioning or repositioning techniques [60, 61, 62, 63, 64].
Interestingly, respiratory muscle training has been assessed by three studies [40, 41, 53]. In this scenario, a growing interest is rising in the current literature about the role of IMT in prolonged MV. In particular, the recent systematic review and meta-analysis by Vorona et al. [65] highlighted that IMT might be considered a key component of a comprehensive rehabilitation intervention aiming at optimizing weaning duration in difficult-to-wean patients [65]. However, neurological impairment characterizing SCI patients might drastically affect respiratory muscle recruitment and respiratory mechanics [28, 29, 66], with detrimental consequences on respiratory muscle’s response to training. Our results underlined that respiratory muscle training might improve weaning duration [40] or weaning success rate [41, 53]. Despite these considerations, a precise patient’s stratification is mandatory in a specific IMT that should be tailored to SCI level and SCI completeness, along with a precise inspiratory muscle weakness assessment.
To overcome the neurological deficit affecting respiratory muscle recruitment, two studies [38, 46] assessed the effects of electrical stimulations on the diaphragmatic muscle and abdominal muscles. On the other hand, it should be noted that several concerns are still open in the current literature about electrical stimulation in pulmonary rehabilitation and no strong evidence currently support this technique [31, 67]. However, electrical stimulations might be considered a suitable rehabilitation strategy in patients with low compliance levels or with high grade of neurological impairment to prevent muscle atrophy.
Taken together, our findings underlined that most of the studies included in the present review assessed different combinations of pulmonary rehabilitation strategies, integrated in a comprehensive rehabilitation intervention. In this scenario, it has been proposed that a multitarget approach might have a role in implementing the synergisms between different therapeutic interventions, with positive effects on functional outcomes of patients with a pulmonary function impairment [27, 68].
On the other hand, recent research is now focusing on a precise stratification based on patients’ characteristics. In particular, the review by Schreiber et al. [30] recently assessed the factors potentially related to successful weaning and weaning duration in patients with SCI. Interestingly, the authors underlined that It might be partly related to specific consequences on muscle recruitment and ventilation mechanics, which might be significantly influenced by patient’s SCI level and SCI completeness [30]. Moreover, presence of multiple spinal cord lesions and pulmonary comorbidities might be crucial factors that might affect weaning process [30]. In this scenario, a patient-tailored approach should consider these issues in order to better personalize the rehabilitative intervention of patients with SCI. Thus, we deeply characterized the participants of this study to provide a qualitative synthesis about the effectiveness of a precise intervention specific to the patient’s characteristics. To the best of our knowledge, this is the first systematic review that assessed the effects of a pulmonary rehabilitation approach in weaning from MV of patients with SCI, focusing on specific rehabilitation strategies to promote pulmonary function recovery and minimize complications.
Besides these considerations, we are aware that this review is not free from limitations. Firstly, the low number of the study included, and the heterogeneous study design did not allow to draw strong conclusions. However, it should be noted that these results reflect the currently available literature. More in detail, our findings underlined a large gap of knowledge in this field with current evidence still based on low-quality studies with controversial results. In addition, several questions are still open about the optimal rehabilitation approach since most of the rehabilitation strategies have been studied in a comprehensive approach. Moreover, the type of SCI lesion might severely influence the rehabilitation response and functional outcomes. On the other hand, the studies identified by the present review underlined a large heterogeneity of the study participants in terms of AIS classification which might severely limits the implications of the study’s results. In this context, a deeper patient stratification should be considered to address the needing for rehabilitative interventions tailored to patients’ characteristics.
Conclusions
Rehabilitation strategies with specific indications for patients with SCI are mandatory to prevent severe complications but also to enhance functional recovery and reduce assistance costs in patients with SCI. The results of the present systematic review supported the effects of a comprehensive rehabilitation approach that might include high-Vt ventilation, positioning, mechanical lung recruitment maneuvers, secretion management, respiratory muscle training and electrical stimulation. Despite the promising results, good-quality studies are mandatory to better characterize the effects of specific rehabilitation interventions reducing MV duration. Moreover, a better patients’ stratification is needed to optimize the weaning process and better address the clinical need for an evidence-based patient-tailored rehabilitation plan for these subjects.
Ethical approval
Not applicable.
Funding
The authors report no funding.
Informed Consent
Not applicable.
Author Contributions
Conceptualization, L.L., A.d.S., and M.I.; methodology, L.L., A.d.S., and M.I.; investigation, L.L., F.D.A., A.F., and A.T.; writing – original draft preparation, L.L. and F.D.A.; writing – review and editing, A.d.S and M.I.; visualization, A.F., A.T., C.C., and A.A.; supervision, A.d.S. and M.I. All authors have read and agreed to the published version of the manuscript.
Supplementary data
The supplementary files are available to download from http://dx.doi.org/10.3233/BMR-220201.
Footnotes
Acknowledgments
The authors want to thank Enrico Cavallo for his support to this work.
Conflict of interest
The authors declare that they have no conflict of interest.
