Abstract
BACKGROUND:
Various tools have been created to measure physical function during intensive care unit (ICU) stay and after ICU discharge, but those have not been validated in coronavirus 2019 (COVID-19) patients. There is a need for a reliable, valid and feasible tool to define the rehabilitation needs of post-ICU COVID-19 patients entering the acute wards and then rehabilitation clinics.
OBJECTIVE:
This study aims to investigate the validity, inter-rater reliability and feasibility of Chelsea Physical Assessment Tool (CPAx) in assessing the functional status of COVID-19 patients after discharge from the ICU.
METHODS:
Demographic and clinical characteristics of the patients were recorded. Patients were evaluated using the modified Medical Research Council (MRC) dyspnea scale, Functional Oral Intake Scale, Glasgow Coma Scale, CPAx, Barthel Index, Katz Index and MRC sum score, measurements of grip strength obtained by dynamometer, the 5 time sit-to-stand test and 30 seconds and sit-to-stand test. CPAx and the other functional assessment tools were administered to 16 patients within 48 hours following ICU discharge. For inter-rater reliability, another physiatrist independently re-assessed the patients. MRC sum score, Barthel and Katz indexes were used to assess construct validity of CPAx. The discriminative validity of CPAx was determined by its ability to differentiate between patients with and without ICU acquired muscle weakness based on MRC sum score. The intra-class correlation coefficients (ICC) were calculated to determine inter-rater reliability for total scores of the functional assessment tools. Cohen’s Kappa (
CONCLUSION:
CPAx is a valid, reliable, and feasible tool to assess the physical functional state in COVID-19 patients following discharge from the ICU.
Introduction
Patients with coronavirus 2019 (COVID-19) who survive after intensive care unit (ICU) support are at risk for several physical, mental, and psychosocial problems such as ICU acquired weakness, dysphagia, chronic inflammation, hypovitaminosis D, neuromyopathy, delirium, anxiety, and functional limitations, known as post intensive care syndrome [1, 2, 3, 4]. Post-acute COVID-19 patients are often transferred from the ICU to post-acute specialized COVID-19 rehabilitation units or other hospital wards. In this context, an adequate transfer of information regarding patients’ condition and functional status at the time of ICU discharge during handover is mandatory for both ICU and rehabilitation physicians [5]. After an increasing number of patients who display functional impairments after COVID-19 discharged from the ICU, there has been a surge in the literature regarding the evaluation of the functional status of COVID-19 patients, as well as rehabilitation interventions that can improve the functional status of COVID-19 patients after discharge from the ICU [6, 7]. As a result, practical, feasible, valid, and reliable tools for assessing the functional status of COVID-19 patients discharged from the hospital should be used to make a definite conclusion about the efficacy of rehabilitation interventions.
The present assessment tools to assess the functional status of patients following ICU discharge could be categorized as strength test, walk tests, functional tests, and health related quality of life (HRQOL) assessment [8]. Among manual muscle strength tests, Medical Research Council (MRC) sum score is the suggested tool to screen ICU acquired weakness. Walk tests such as six-minute walk test or timed up and go test could be difficult to carry out as the patients could not even sit due to severe impairments during the early period [8, 9]. Additionally, these tests require space to perform and may require the management of several drips, drains, and oxygen delivery systems, which complicates test execution while the patient is walking and turning. Because of the increase in patient admissions due to the unexpected pandemic, hospital rooms have become crowded. This made it difficult to perform walk tests like these due to limited space in patient rooms.
Physical functional assessments include evaluation of muscle strength, mobility, physical and functional activity [8]. Among functional tests, the Physical Function in ICU Test (PFIT), Functional Status Score for the ICU and the Chelsea Critical Care Physical Assessment Tool (CPAx) are specifically developed to assess function after ICU stay. Barthel and Katz indexes are general tools to assess functional daily activities in various diseases [8]. According to a systematic review of 26 different outcome measures, the CPAx and the PFIT demonstrated the strongest clinimetric properties with established reliability, validity, and responsiveness; however, the PFIT has a greater floor effect than CPAx [10, 11]. The PFIT and CPAx may be more suitable for the assessment of patients who may never reach the ability to perform submaximal exercise tests [12].
Among these functional assessment tools, CPAx is easy to use in the clinical setting which covers respiratory function, coughing capacity, moving within the bed, sitting, and standing balance, sit to stand, transferring from bed to chair, stepping, and grip strength. Duration of assessment time is short and relatively few equipment (hand dynamometer for grip strength) is required. Many numbers of patients who were delivering non-invasive ventilation (e.g. continuous positive airway pressure) had to be discharged from the ICU to other outpatient wards because ICU beds had to be reserved for COVID-19 patients requiring invasive ventilation [13]. Although there are several tools that were constructed to measure physical function during ICU stay and following ICU discharge [14, 15, 16], they had not been validated in patients with COVID-19. To define rehabilitation needs of post-ICU COVID-19 patients who had been stepping down to acute wards and onwards into rehabilitation there was a need for a reliable, valid and feasible tool. We aimed to investigate the validity and the inter-rater reliability of CPAx in the assessment of the functional status of COVID-19 patients discharged from the ICU. Our secondary aim was to investigate feasibility of commonly used assessment tools for assessing physical function after ICU in COVID patients discharged from the ICU.
Materials and methods
Study design and setting
This cross-sectional observational study was conducted between March 01 and May 30 2021 at Koç University Hospital and Gaziosmanpaşa Training and Research Hospital among COVID-19 survivors discharged from the ICU to the wards. The study was approved by the Research Ethical Board of the University of Health Sciences (approval number: 245/2021). The study was registered on clinicaltrials.gov.tr (NCT04762056) and conforms to the STROBE checklist.
Study participants
Patients who were discharged from the ICU with a diagnosis of COVID-19 pneumonia were enrolled in this study. Inclusion criteria were: a) age
Sample size calculation
MedCalc Statistical Software version 19.1 (MedCalc Software bv Ostend, Belgium) was used for sample size analysis. A sample size calculation was completed for a Pearson’s correlation with a two-sided test, alpha
Outcome measures
Demographic characteristics including age, gender, body mass index, comorbidities, sequential organ failure assessment score (SOFA score) and acute physiology and chronic health evaluation (APACHE II) on ICU admission, length of ICU stay, history and duration of invasive mechanical ventilation, history of extra corporeal membrane oxygenation (ECMO), and presence of tracheostomy were recorded. Modified MRC dyspnea scale was used to quantify disability associated with dyspnea and Functional Oral Intake Scalewas used to evaluate the swallowing function. Patients’ level of consciousness and responsiveness were evaluated with Glasgow Coma Scale.
Chelsea Critical Care Physical Assessment Tool, Barthel Index, Katz Index and MRC sum score, grip strength measurement via dynamometer, the 5 time sit-to-stand test and 30 seconds sit-to-stand test were used to assess the physical status of the patients within 48 hours following ICU discharge by a physiatrist. Another physiatrist independently re-assessed the patients for inter-rater reliability.
Validity
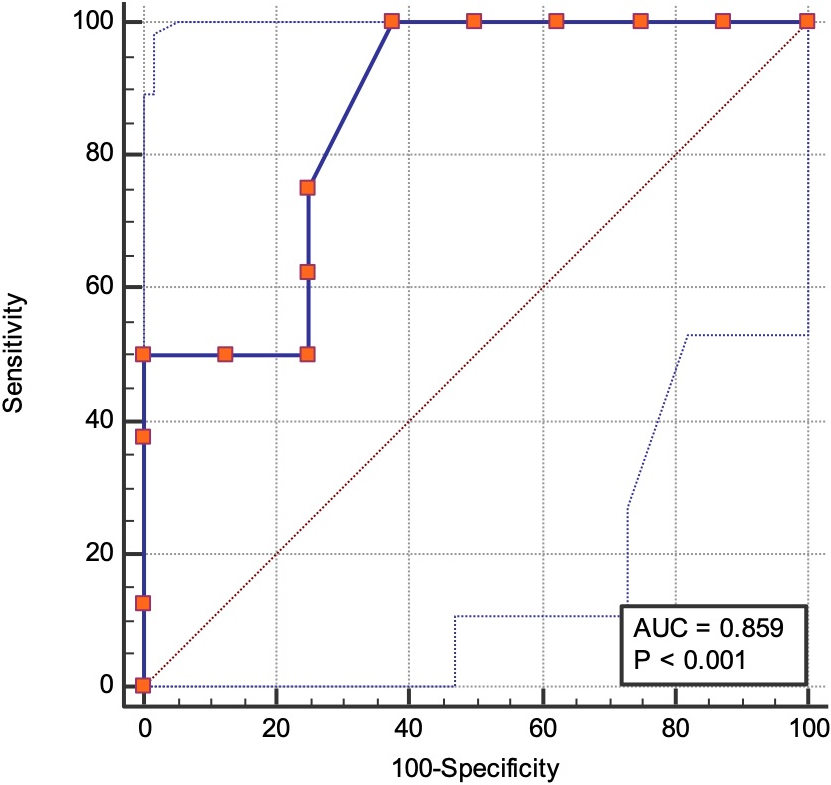
To assess construct validity MRC sum score, Barthel Index, Katz Index and modified MRC dyspnea scale were used. The discriminant validity of CPAx was determined by its ability to discriminate between patients with and without ICU acquired muscle weakness based on MRC sum score.
Inter-rater reliability
To assess inter-rater reliability another physiatrist completed the CPAx and other assessments including MRC sum score, Barthel and Katz indexes on the same day without communicating the first rater and was blinded to the first rater’s score.
Feasibility
To assess and compare the feasibility of existing tools for functional status assessment of COVID-19 patients discharged to rehabilitation wards, the number and the percentages of the patients who were able to complete each tool were recorded.
Sequential Organ Failure Assessment Score (SOFA score)
Sequential Organ Failure Assessment Score is used to describe the degree of organ dysfunction from 0 (normal) to 4 (most abnormal) for six vital organs [19].
Acute Physiology and Chronic Health Evaluation (APACHE II)
APACHE II is a classification system representing a general measure of severity of disease which is based on age, initial values of 12 physiologic measurements and previous health status. It is also used to compare the efficacy of intensive care over time. The score ranges between 0 and 71 and higher score is correlated to subsequent risk of hospital death [20].
Glasgow Coma Scale
The Glasgow Coma Scale is a structured method for assessment of the level of consciousness via evaluating motor, verbal and eye responses, that enable comparison of the changes over time. These three components are combined in a sum score between 3 (worst) and 15 (best) [21].
Functional Oral Intake Scale
The Functional Oral Intake Scale is a tool used to document change in the functional eating abilities of the patients. Swallowing abilities were assessed with the FOIS, which consists of seven choices to describe the quality of oral intake, ranging from 1 (worst) to 7 (normal) as below [22]:
Tube Dependent (levels 1–3)
No oral intake Tube dependent with minimal/inconsistent oral intake Tube supplements with consistent oral intake
Total Oral Intake (levels 4–7)
Total oral intake of a single consistency Total oral intake of multiple consistencies requiring special preparation Total oral intake with no special preparation, but must avoid specific foods or liquid items Total oral intake with no restrictions
Disability attributable to breathlessness was quantified using modified MRC dyspnea scale that stratifies severity of dyspnea in respiratory diseases, particularly COPD [14]. Dyspnea in daily living was evaluated by the modified MRC dyspnea scale which include five statements that describe almost the entire range of dyspnea from none (Grade 0) to almost complete incapacity (Grade 4) as follows [23]:
Grade 0: I only get breathless with strenuous exercise Grade 1: I get short of breath when hurrying on level ground or walking up a slight hill Grade 2: On level ground, I walk slower than people of the same age because of breathlessness, or I have to stop for breath when walking at my own pace on the level Grade 3: I stop for breath after walking about 100 yards or after a few minutes on level ground Grade 4: I am too breathless to leave the house or I am breathless when dressing
Manual muscle strength of six muscle groups (shoulder abduction, elbow flexion, wrist extension, hip flexion, knee extension, and ankle dorsiflexion) was evaluated on both sides using MRC scale. MRC sum score was calculated by summing the scores. This score, ranging from 0 to 60, reliably identifies significant weakness (
Hand grip strength measurement
Hand grip strength was measured using a handheld dynamometer (JAMAR Plus+ electronic dynamometer, part number: 563213, serial number: 2019070814, Sutton-in-Ashfield, Nottinghamshire, UK) in the standardized recommended position by American Society of Hand Therapy (with the patient as seated as possible, with the elbow as close as to 90
CPAx
The CPAx is a bedside assessment tool firstly reported to measure physical morbidity in critical care population in 2013 and recommended for use in post-acute COVID-19 patients [18, 25]. It consists of 10 items (respiratory function, cough, moving within the bed, supine to sitting on the edge of bed, dynamic sitting, standing balance, sit to stand, transferring from bed to chair, stepping, and grip strength) rated on a 6-point scale from complete dependency (level
Barthel Index
The Barthel Index is a measure of performance in activities of daily living (ADL). This ordinal scale includes 10 items of mobility and self-care ADL, assessing the degree of physical assistance required and time taken to perform each item. Scores range from 0 to 100. A higher score reflects greater ability to function independently (Scores 0–20: “total” dependency, 21–61: “severe” dependency, 62–90: “moderate” dependency, 91–99: “slight” dependency, 100: “full” independency) [26].
Katz Index
The Katz Index of Independence in Activities of Daily Living, commonly referred to as the Katz ADL, assesses the ability to perform activities of daily living independently, in the six functions of bathing, dressing, toileting, transferring, continence, and feeding. Each item is scored yes/no for independence. A score of 6 indicates full function, 4 indicates moderate impairment, and 2 or less indicates severe functional impairment [27].
The 5 time sit-to-stand test
The 5 repetition sit-to-stand test evaluates the exercise capacity and lower limb strength and assesses the changes in exercise capacity in COPD [28]. Normative values of the 5-repetition sit-to-stand test are reported as 11.4 sec (60 to 69 years), 12.6 sec (70 to 79 years), and 14.8 sec (80 to 89 years) in healthy individuals [29].
30 seconds sit-to-stand test
The 30 seconds sit-to-stand test evaluates the muscular endurance or strength endurance and the functional status of the patients those at risk for mobility. The score ranges from 0 (cannot complete even one stand) to 20 or more in highly fit individuals. Less than 10 times sit to stand indicates lower extremity strength and can be used as a measure of lower body strength in community-residing older adults [28].
Statistical analysis
Statistical analysis was performed using SPSS Statistics for Windows, version 27.0. (IBM Corp., Armonk, NY, USA). Histogram, normality plots and Shapiro-Wilk normality test were performed to assess the distribution of the data. Descriptive data were presented as median, interquartile range (IQR), minimum, maximum, frequency and percentage.
For construct validity, the Spearman Rho correlation coefficients were used to evaluate the correlation between CPAx and Barthel, Katz indexes (Spearman Rho coefficients were classified as follows:
The intra-class correlation coefficient (ICC, range 0.00–1.00) were calculated to determine inter-rater reliability for total scores. ICC values less than 0.5 were considered as poor reliability, values between 0.5 and 0.75 were considered as moderate reliability, values between 0.75 and 0.9 were considered as good reliability, and values greater than 0.90 were considered as excellent reliability [30]. Cohen’s Kappa (
Results
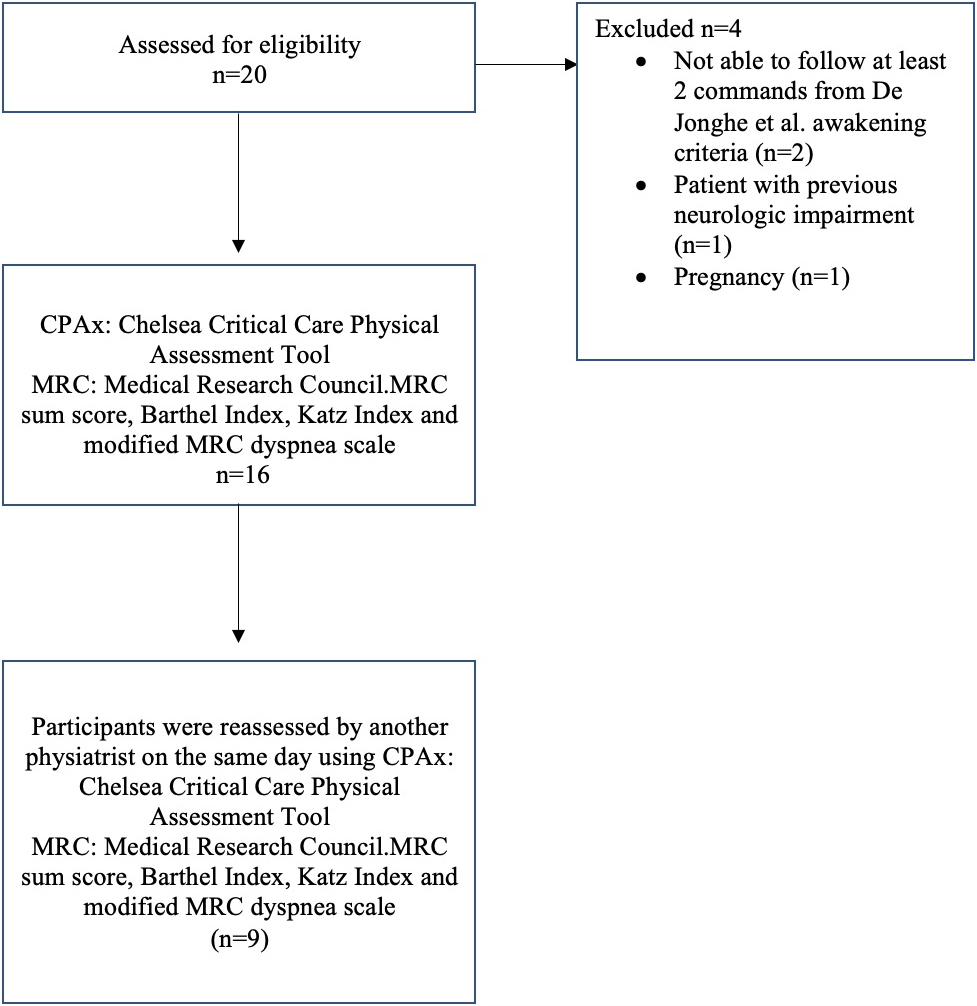
Demographic, clinical characteristics, and baseline data of 16 patients with COVID-19 transferred from the ICU to the ward are presented in Table 1. The flowchart of the study participants is depicted in Fig. 1.
Demographic, clinical characteristics and baseline data of the patients
Demographic, clinical characteristics and baseline data of the patients
Footnotes
Acknowledgments
None to report.
Conflict of interest
The authors have no competing interests to declare.