Abstract
OBJECTIVE:
To review and update the evidence for different forms of manual therapy (MT) and exercise for patients with different stages of non-specific neck pain (NP). Data sources: MEDLINE, Cochrane-Register-of-Controlled-Trials, PEDro, EMBASE.
METHOD:
A qualitative systematic review covering a period from January 2000 to December 2015 was conducted according to updated-guidelines. Specific inclusion criteria only on RCTs were used; including differentiation according to stages of NP (acute – subacute [ASNP] or chronic [CNP]), as well as sub-classification based on type of MT interventions: MT1 (HVLA manipulation); MT2 (mobilization and/or soft-tissue-techniques); MT3 (MT1
RESULTS:
Initially 121 studies were identified for potential inclusion. Based on qualitative and quantitative evaluation criteria, 23 RCTs were identified for review. Evidence for ASNP: MODERATE-evidence: In favour of (i) MT1 to the cervical spine (Cx) combined with exercises when compared to MT1 to the thoracic spine (Tx) combined with exercises; (ii) MT3 to the Cx and Tx combined with exercise compared to MT2 to the Cx with exercise or compared to usual medical care for pain and satisfaction with care from short to long-term. Evidence for CNP: STRONG-evidence: Of no difference of efficacy between MT2 at the symptomatic Cx level(s) in comparison to MT2 on asymptomatic Cx level(s) for pain and function. MODERATE to STRONG-evidence: In favour of MT1 and MT3 on Cx and Tx with exercise in comparison to exercise or MT alone for pain, function, satisfaction with care and general-health from short to moderate-terms. MODERATE-evidence: In favour (i) of MT1 as compared to MT2 and MT4, all applied to the Cx, for neck mobility, and pain in the very short term; (ii) of MT2 using sof-tissue-techniques to the Cx and Tx or MT3 to the Cx and Tx in comparison to no-treatment in the short-term for pain and disability.
CONCLUSION:
This systematic review updates the evidence for MT combined or not with exercise and/or usual medical care for different stages of NP and provides recommendations for future studies. Two majors points could be highlighted, the first one is that combining different forms of MT with exercise is better than MT or exercise alone, and the second one is that mobilization need not be applied at the symptomatic level(s) for improvements of NP patients. These both points may have clinical implications for reducing the risk involved with some MT techniques applied to the cervical spine.
Keywords
Introduction
Non-specific neck pain (NP) is defined as pain in the posterior and lateral aspect of the neck between the superior nuchal line and the spinous process of the first thoracic vertebra with no signs or symptoms of major structural pathology and no or minor to major interference with activities of daily life as well as with the absence of neurological signs and specific pathologies; such as: traumatic sprain and fracture, tumour, infectious or inflammatory cervical spondylolysis, etc. [72, 73, 74, 75, 76, 77, 78, 79, 80]. It accounts for around 25% of all outpatient visits to physiotherapy [72, 73, 74, 75] with a life-time incidence rate of 12 to 70% among the general population [73, 76, 77, 78, 79, 80], although men are less likely to be affected than women [79, 81, 82, 83, 84]. Most people with NP do not experience a complete resolution of symptoms with 50–85% reporting recurrence 1 to 5 years later [80]. Consequently, NP results in enormous health-costs in terms of treatment, lost wages and work absenteeism [78, 81, 84]. Despite its major prevalence and socioeconomic consequences, NP is the “poor cousin” to low back pain in terms of research investigation [77, 78]. In most cases a specific diagnosis cannot be made and NP is labelled non-specific, because of the multifactorial etiology [80, 81, 85, 86].
Within a “Bio-Psycho-Social” framework, a number of factors could be considered to contribute to NP. These include non-modifiable risk factors related to patho-anatomical features (e.g. history of trauma, age, gender and genetics) and adjustable risk factors, which are more related to psychosocial features (e.g. smoking, physical activity and sedentary life style, beliefs, coping style, expectations, and work satisfaction). These factors may also contribute to the transition from acute to chronic pain status [79, 80, 81, 82, 86, 87].
Conservative treatments used to help manage NP are numerous and include usual medical care (UMC: i.e. face to face interview, education, reassurance, medication, ergonomic and stay active advice), various forms of exercise, massage, and acupuncture among others, but there is a lack of evidence regarding their relative efficacy [76, 78, 80]. Manual therapy (MT) is also an increasingly popular treatment available to people with NP and many countries include MT in national guidelines for treating musculoskeletal disorders [79, 88, 89]. In general terms, these treatments are considered to be more useful than no intervention or placebo treatments [72, 76, 80, 81, 82, 85, 88]. MT includes both passive techniques (hands-on) and active techniques (hands-off) and should be used within a clinically reasoned and evidence-based-practice framework [89, 90, 91]. The aim of MT in the context of NP is to decrease pain, improve movement, motor control, and function and thereby reduce disability [79, 88, 89, 90, 91].
A recent systematic review (SR) from Hidalgo et al. [91] examined the efficacy of different common forms of MT for low back pain which had been reported in the literature or used in clinical practice. In that review, three categories of MT were identified and their efficacy examined according to specific inclusion criteria (both qualitative and quantitative). These categories were MT1 comprising high velocity low amplitude thrust manipulation (HVLA), MT2 comprising a range of spinal mobilization and/or soft-tissue-techniques, MT3 being MT2 combined with MT1. All categories could be combined or not with exercise (general or specific) and/or with UMC [91]. In addition to these forms of MT, mobilization-with-movement (MWM; i.e. MT4) is an increasingly popular form of treatment used clinically for a range of musculoskeletal disorders and receiving increasing research attention [92, 93].
PRISMA flowchart of inclusion.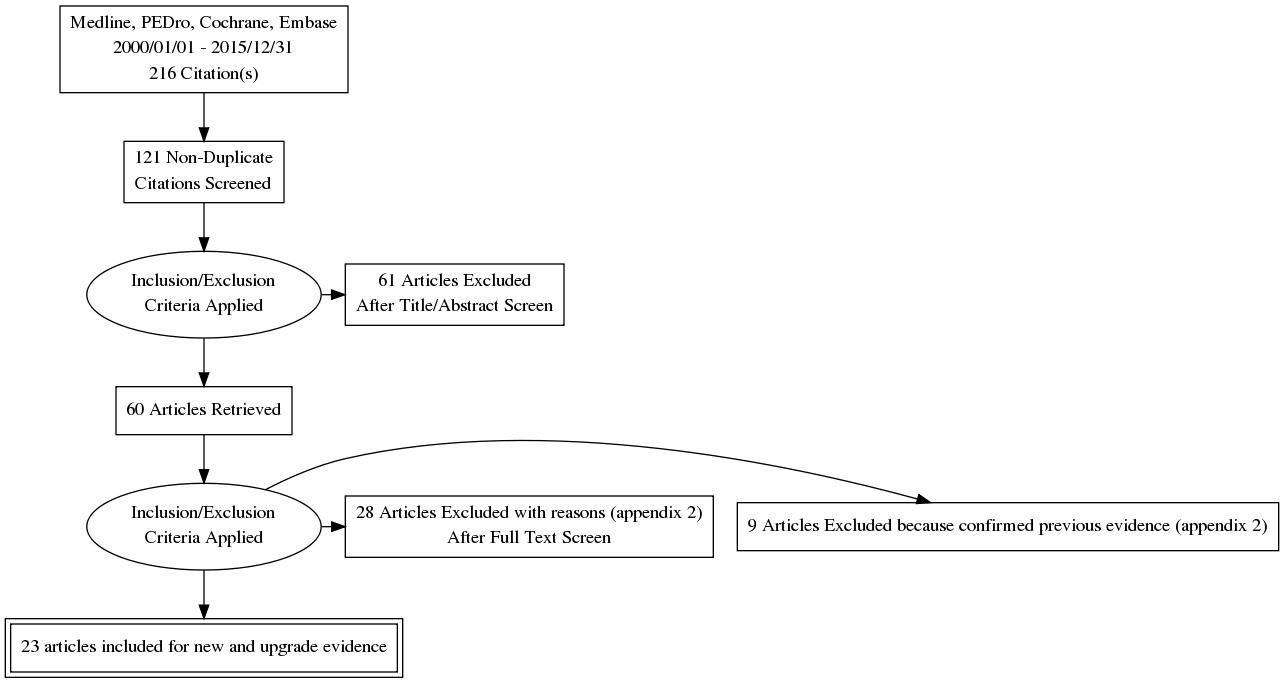
This type of rigorous systematic review of different forms of MT combined or not with exercise and compared with UMC has not yet been reported for NP. For example, previous reviews have reported that MT is more effective than a placebo treatment or no treatment at all for NP, but failed to establish levels of evidence for other forms of treatment such as UMC or exercise in comparison to MT. Moreover, these studies have not adequately investigated which MT approach when combined with UMC or exercise, is more effective for NP [75, 88, 94]. However, the number of studies investigating MT for NP has recently increased, possibly in part due to its popularity and use in clinical practice. Hence, there are a number of recently published trials that have not been considered in previous SRs of NP [75, 94, 96, 97, 98, 99, 100]. Further, the SRs published to date on NP, are not up to date, rarely focus on NP in isolation (more often including headache, radiculopathy, and whiplash) have not considered low risk of bias studies (methodological quality
This SR was conducted in accordance with the Co- chrane Collaboration Back Review Group (CCBRG) and PRISMA updated guidelines for SR [95, 101] and is based on the methodology and design of a previous qualitative-SR [91].
Search strategy
A literature search of randomized controlled trials (RCTs) published in English between 1
Inclusion criteria
Study design
RCTs were included only (i) if they presented a low-risk of bias, (ii) if subjects with NP were randomly allocated to receive either MT or a comparator group receiving “no-treatment”, a placebo procedure, or another usual conservative therapy for NP, (iii) if the randomization methods were appropriate and clearly reported, and (iv) if a single (assessors blinded) or double-blind design (assessors and patients blinded) was used.
Patients
NP was differentiated on the basis of duration of the pain episode, with acute pain
Studies were included if the patients were male or female aged between 18 and 60 years suffering from acute-subacute (0–12 weeks) or chronic (
With respect to severity, NP is also classified according to a 4-grade classification system of the Neck Pain Task Force [102], and for this SR, only RCTs with a population comprising NP grade I or II on this classification system were selected, i.e. no signs or symptoms of major structural pathology and no or minor (I) to major (II) interference with activities of daily life with the absence of neurological signs.
Interventions
As manual therapy (MT) interventions are broad by nature, we decided to use a clinical sub-classification system of MT in this SR with four major categories of MT techniques [91]. Moreover, this sub-classification was in accordance with a comprehensive evidence based search strategy and the MT treatment used and reported in the intervention group (IG) of included RCTs.
MT1 corresponds to spinal manipulation, where a HVLA thrust with “cavitation” is applied to the cervical spine (Cx) or thoracic spine (Tx) [103, 104, 105]. MT2 includes a range of mobilization techniques applied to the Cx or Tx which includes: low-velocity-mobilization such as physiological or accessory mobilization, articular muscle-energy-technique (MET, i.e. segmental analytic myotensive mobilization of Cx and Tx) and/or the soft-tissue techniques (STT) including “myofascial-release”, “trigger-points” “muscular-MET” (i.e. analytic myotensive techniques on specific muscles using “contract-relax” neurophysiological principles) of the neck region [82, 91, 103, 106]. MT3 comprises the combination of MT2 and MT1 [103, 105, 106]. MT4 corresponds to mobilization-with-movement (MWM) with cervical sustained-natural-apophyseal-glides (SNAGs) developed by Mulligan [107, 108].
Furthermore, as modern MT include hands off approach, sub-categorization of groups MT1-4 was based on the addition or not of exercise either specific (for example based on directional-preference, strengthening/ stabilization of specific deep-neck and scapular muscles, and motor control) or general (for example: range of motion exercises of the head and neck, sitting posture correction) or usual-medical-care (UMC; i.e. face to face interview, education, reassurance, medication, ergonomic and stay active advice) [91, 94, 104, 38, 39, 40, 41].
Summary of articles for patients with acute-subacute neck pain
Summary of articles for patients with acute-subacute neck pain
ANP: acute neck pain/SNP: subacute neck pain/ASNP: acute-subacute neck pain/VAS: Visual Analogue Scale/NDI: Neck Disability Index/CROM: Active Cervical Range of Motion/PPT: Pressure Pain Threshold/US: ultrasound/NPRS: Numeric Pain Rating Scale/FABQ: Fear-Avoidance-Belief-Questionnaire/SF-36: Short-form-health-survey/NPQ: Northwick Pain Questionnaire/UMC: Usual Medical Care/Cx: cervical/Th: thoracic/MOB: Mobilization/SNAGs: Sustained Natural Apophyseal Glides/HVLA: high velocity low amplitude thrust/IG: Intervention Group/CG: Control Group/IRT: Infrared Radiation Therapy/PAIVMS: Passive Accessory Intervertebral Movements/STT: Soft-Tissues-Techniques/SUS: Sham Ultrasound/Yes: significant difference with moderate to large clinical effect size/No: no significant difference with small clinical effect size on all timing outcome measures.
The control groups received: “no treatment”, a placebo, or another usual conservative treatment for NP (e.g. UMC, exercise, electrotherapy, physiotherapy, or rehabilitation) [95, 101, 41].
Outcome measures of effectiveness
The outcome measures were classified according to the CCBRG recommendations: pain, function, overall-health and quality of life (Appendix 1). Timing of the follow-up measurements was defined as very-short-term (end of treatment/discharge to 1 month), short-term (1–3 months), intermediate-term (3 months–1 year), or long-term (1 year or more).
Quality assessment
Two independent reviewers (JB and AD) assessed risk of bias, methodological quality, data extraction and clinical relevance of each trial.
Quantitative and qualitative criteria were assessed by applying the CCBRG criteria [95, 101]. Quantitative risk of bias was assessed, using an 11-point check-list (see Appendix 1).
Summary of articles for patients with chronic neck pain
Summary of articles for patients with chronic neck pain
CNP: chronic neck pain/VAS: Visual Analogue Scale/NDI: Neck Disability Index/CROM: Active Cervical Range Of Motion/PPT: Pressure Pain Threshold/US: ultrasound/NPRS: Numeric Pain Rating Scale/FABQ: Fear-Avoidance-Belief-Questionnaire/SF-36: Short-form-health-survey/NPQ: Northwick Pain Questionnaire/UMC: Usual Medical Care/Cx: cervical/Th: thoracic/MOB: Mobilisation/SNAGs: Sustained Natural Apophyseal Glides/HVLA: high velocity low amplitude thrust/IG: Intervention Group/CG: Control Group/IRT: Infrared Radiation Therapy/PAIVMS: Passive Accessory Intervertebral Movements/STT: Soft-Tissues-Techniques/SUS: Sham Ultrasound/Yes: significant difference between groups with moderate to large clinical effect size/No: no significant difference between groups with small clinical effect size on all timing outcome measures.
Qualitative assessments were made on the basis of the following criteria: a well determined distinction and separation between combined acute-subacute and chronic NP categories at baseline, a detailed description of MT intervention and the possibility that reviewers would be able to classify the MT techniques according to MT1-MT4 classification system, and a single-blind or double-blind RCT design.
Included studies were required to be low-risk of bias. We considered as “high-quality” those RCTs with single-blind (assessors blinded) or double-blind (patients and assessors blinded) designs that met at least 9/11 of CCBRG criteria indicated by an ‘A’. “Moderate quality” RCT status was assigned to studies of single-blind design with a minimum score of 7/11 indicated by a ‘B’ (Tables 1 and 2) [75, 91]. To reduce the number of words and the number of studies included in this SR, only RCTs that present new findings or update/upgrade previous evidence from SRs with our methodology are fully described in the results section and Tables 1–3. However, all studies from our search strategy, as well as reason of exclusion are presented in the Appendix 2.
Strength of evidence was determined by grouping similar “Patients Interventions Comparisons Outcomes Study Design” to provide an overall level of evidence (see Appendix 1 for the process of evidence) on the efficacy of the 4 categories of MT (MT1-MT4) combined or not with another intervention. Conclusions of evidence are summarized in Table 3.
The effect size was independently collected or calculated by two authors, and used to assess the clinical relevance of MT interventions in outcome measures. We reported the between groups means of difference (MD
Results
Two reviewers performed the selection of articles (Fig. 1). A qualitative SR was undertaken on the 23 low-risk of bias RCTs, based on the qualitative and quantitative criteria described above; 21 studies were classified as level A and 2 as level B quality (Tables 1 and 2). Summary findings are shown in Table 3, which includes a presentation of the level of evidence drawn from the selected RCTs.
Effects of interventions on acute-subacute NP
MT1 to the cervical spine with exercise versus MT1 to the thoracic spine with exercise
Puentedura et al. [42] evaluated the efficacy of MT1 to the upper Cx in comparison to MT1 on the Tx. Both interventions were combined with the same exercise (ROM exercises of the head and shoulder, and upper limb exercise against moderate resistance elastic band’s). The numbers of treatment sessions were similar in both groups (
MT1 with electro/thermal-therapy versus electro/thermal-therapy alone
Gonzalez-Iglesias et al. [72, 43] investigated in two studies the efficacy of MT1 (localized to the upper Tx) combined with electro/thermal-therapy as compared to electro/thermal-therapy alone for acute-subacute NP patients. The number of sessions was equivalent in both groups and both studies covered 5–6 sessions over 3 weeks. There were statistically significant improvements for pain (
Comparison of two MT2 interventions
Nagrale et al. [86] evaluated comprehensive MT2 (STT) that combined muscular-MET, trigger (ischemic compression) and tender-points (strain-counterstrain) techniques on the trapezius in comparison to simple MT2 (STT) that included only the muscular-MET on the trapezius for acute-subacute NP patients. At 2 and 4 weeks follow-up, the results showed significant improvements in both groups on pain reduction, function and side-bending. However, there was a significant clinically relevant difference between groups with large effect sizes for pain and function (SMD for CROM lateral flexion
MT2 versus sham-Ultrasound (SUS)
Blikstad and Gemmell [44] and Gemmell et al. [45] compared the effect of MT2 (STT) consisting of trigger point techniques to the trapezius muscle (ischemic compression and trigger point release) to SUS for acute-subacute NP. The results demonstrate that MT2 had an immediate effect on pain compared to SUS. However, in both studies, no statistically significant differences were apparent for any outcome measures between the groups.
MT3 versus usual-medical-care and home exercise
Bronfort et al. [46] studied the efficacy of MT3 (on hypomobile Cx and Tx segments and on STT) as compared to UMC (private consultation and education combined with medication (AINS, narcotic drugs and/or muscle relaxants, and advice to stay active) and to home exercise (2
MT3 with exercise versus MT2 with exercise
Masaracchio et al. [48] compared the effect of MT3 during two sessions (2
MT2 with exercise and MT4 with exercise versus exercise alone
Ganesh et al. [96] studied the effect of MT2 (accessory mobilization on the Cx for 10 sessions over 2 weeks) with exercise (flexibility and strengthening of cervical and scapular muscles, and cervical ROM exercises) in comparison to MT4 (SNAGs applied to the Cx in a sitting position) with exercise and exercise alone for patients with acute-subacute NP. All groups were instructed to continue the exercise at home for 4 weeks. The results demonstrated that all the groups improved overtime compared to baseline (
Effects of interventions on chronic NP
MT1 in comparison to MT2 and MT4
Izquierdo-Pérez et al. [49] compared three different treatments applied to the Cx. These were HVLA (MT1), accessory mobilization (MT2) and SNAGs (MT4). Each patient received 4 sessions within 2 weeks. All three groups showed similar improvements in pain, disability and ROM but there was no difference between interventions in any outcome measure apart from CROM in extension (
Lopez et al. [50] also studied the effect of the same three interventions applied to the Cx, i.e. HVLA (MT1), accessory mobilization (MT2) and SNAGs (MT4) and CROM. In comparison to Perez’ investigation [49], each patient received only one single therapy session. All of the treatments groups demonstrated similar efficacy for the management of pain (at rest, flexion/extension, rotation, side bending, pressure pain thresholds on C2), and CROM (multidirectional). However, only one significant difference (two way; treatment x time interaction,
Authors of both studies [49, 50] concluded by saying that all 3 techniques applied to the Cx were effective in the management of chronic NP with no differences between them. However, MT1 appears marginally better than other forms of MT based on improved CROM in extension only and pain at rest [49, 50].
MT1 to the cervical spine versus kinesio-Tape
Saavedra-Hernandez et al. [51] compared one group receiving MT1 (HVLA thrust to the mid-Cx and upper-Tx), to another group receiving only Kinesio-Tape applied to the neck for one week in patients with chronic NP. Both interventions demonstrated similar decreases in pain, disability and increases in CROM over the 1-week study period but the results showed that there were no statistically significant differences between both groups in all outcome measures except for the CROM in rotation at 7 days. Five patients reported minor adverse events with 3 (7.5%) in the manipulation group (minor increase in NP or fatigue) and two (5%) in the Kinesio-Tape group (cutaneous irritation related to the tape application). These minor post-treatment symptoms resolved within 24 hours. The authors concluded that the application of MT1 or Kinesio-Tape leads to similar reduction in pain and disability and increases in CROM, and that concerning CROM and disability, the changes were not clinically meaningful.
MT1 to the cervical spine versus MT1 to the thoracic spine
Martinez-Segura et al. [52] studied the relative efficacy of a single session of MT1 to the mid-Cx or to the upper-Tx for patients with chronic NP. All groups showed similar changes (
MT versus <<no-treatment>>
Sherman et al. [76] investigated the effectiveness of MT2 (STT to the Cx and Tx region, i.e. connective tissue massage, ischemic compression, myofascial release) in comparison to “no treatment” with a self-care booklet for patients with chronic NP. Differences between both groups were statistically significant for pain (
Schwerla et al. [82] compared MT3 to Cx and Tx combined with SUS to “no treatment” with SUS alone for chronic NP patients. The results showed clinical relevant differences in favour of the intervention group on pain reduction (
MT1 with infrared radiation therapy (IRT) and exercise versus IRT and exercise alone
Lau et al. [79] assessed the effectiveness of MT1 to the Tx combined with IRT (15 minutes over the painful site) and exercise (active neck mobilization, isometric neck muscle contraction for stabilization, and stretching of trapezius and scalene muscles) in comparison to a control group (IRT and exercise only) for chronic NP patients. This study showed that patients in the experimental group had clinically relevant improvements in NP (
MT2 on symptomatic spinal level(s) versus “sham” MT2 (random location)
Kanlayanaphotporn et al. [53] studied the immediate effects of MT2 (Cx accessory mobilization) on pain and active CROM. In the experimental group, the treatment details including the spinal level(s) to be treated, the grade of movement to be applied, and the most appropriate technique of mobilization were noted. In the control group, the patients received one of the following mobilization techniques that could be considered as a placebo procedure: a central PA, ipsilateral unilateral PA, or contralateral unilateral PA pressure. In both groups the MT2 intervention was applied for 1 minute repeated twice. Both group showed significant decrease in neck pain at rest and in pain at most painful movement. However, there were no statistically significant differences between the groups on pain and active CROM.
Aquino et al. [90] and Schomacher et al. [54] evaluated whether MT2, using the same techniques as described above for Aquino et al., and intermittent translatory traction in supine (accessory mobilization) between C2 and C7 for Schomacher et al., applied both to the symptomatic Cx level, was able to reduce pain compared to the same MT2 interventions but at an asymptomatic Cx level(s). Although all groups in both studies showed significant immediate pain relief, there was no significant difference between the groups.
These studies [90, 53, 54] demonstrate that identification of the symptomatic Cx segment is not important for the immediate effects of MT2 (accessory mobilization) on pain for chronic NP.
MT versus active rehabilitation
Bronfort et al. [78] compared MT3 alone (HVLA thrusts with STT) to the Cx and Tx for 20 sessions of 15–20 minutes), to MT3 with exercise (neck and upper body strengthening for 20 sessions of 1 hour), to MedX Exercise (high technology devices for strengthening of the neck and upper-body during 20 sessions of 1 hour). Although there was a tendency for greater improvement for the two exercise groups (MT3 with exercise and MedX exercise), the efficacy of these 3 interventions was not statistically different for pain, function and overall improvement during treatment. However, at 1-year follow-up, there were significant differences in favour of MT3 combined with exercise and MedX exercises groups as compared to MT3 alone on pain reduction (
Evans et al. [55] investigated the efficacy of MT1 (to the Cx and Tx for 20 sessions of 15–20 minutes) combined with high dose (20 sessions of 1-hour) supervised strengthening exercise (neck and upper body strengthening), to high dose supervised strengthening exercise alone, and low dose home exercise and advice for chronic NP patients. There were clinically relevant improvements at 12 weeks for both high dose exercise groups for pain and overall health improvement (
Akhter et al. [98] investigated the role of MT1 (HVLA on the stiff Cx segments for around 6 sessions over 3 weeks) combined with supervised exercise (flexibility, strengthening of the cervical and scapular muscles and CROM exercise) in comparison to supervised exercise regime alone for chronic NP patients. At the end of 3 weeks interventions both groups were instructed to do the same exercise for a period of 3 months on a daily basis. Both groups made significant improvement in pain and functional outcome measures (
The general trend of these three studies [78, 98, 55] was that combined MT1 and MT3 on the Cx and Tx with exercise demonstrated better results for pain, function, satisfaction with care and general health in comparison to exercise or MT alone for patients with chronic NP.
Discussion
The goal of this SR was to assess and update the best evidence by including only low-risk of bias RCTs reporting on the effectiveness of different MT approaches, classified into 4 categories (MT1-MT4), in the management of NP without associated disorders such as cervicogenic headache or radiculopathy. Efficacy for MT1-4 interventions was assessed in isolation or when combined with exercise or UMC.
MT: manual therapy; MT1: HVLA thrust; MT2: accessory an physiological mobilization and/or soft-tissue-techniques (STT) and/or muscle energy technique (MET); MT3: MT1
With respect to acute/sub-acute NP this review found moderate evidence in favour of (i) MT1 at the involved Cx level combined with exercise when compared to MT1 to the Tx combined with exercise [42]; (ii) MT3 (Tx HVLA
This review found moderate evidence of no difference in efficacy between MT2, comparing trigger point therapy to SUS [44, 45]. In addition there was limited evidence of no difference in efficacy between MT2 (Cx accessory mobilization) with exercise in comparison to MT4 (Cx SNAGs) combined with exercise in comparison to exercise alone on pain, disability and CROM [50].
With respect to chronic NP this review found strong evidence of no difference in efficacy for MT2 when comparing Cx accessory mobilization at the symptomatic level to the asymptomatic level for pain and function [90, 53, 54]. Moderate to strong evidence was found in favour of MT1 and MT3 at the Cx and Tx combined with exercise in comparison to exercise or MT alone for pain, function, satisfaction with care and general health at least in the short- to moderate-terms [78, 98, 55]. Moderate evidence was found in favour (i) of MT1 compared to MT2 (Cx accessory mobilization) and MT4 (Cx SNAGs), for CROM [49] and pain [50] in the very short-term; (ii) of MT2 (STT to the Cx and Tx) [76] and MT3 to the Cx and Tx [82] in comparison to no-treatment (self-care booklet or SUS), in the short-term for pain and disability [76]; (iii) of MT1 to the Tx with IRT and exercise as compared to IRT and exercises alone for pain, function, overall-health and CROM in the short to moderate-term [79]. Moderate evidence was found of no difference (i) between MT1 to the Cx and Cx-Tx in comparison to Kinésio-Tape applied to the neck region for pain, disability and CROM in the very short-term [51]; (ii) between MT1 to the Cx in comparison to MT1 to the Tx for pain, CROM and pressure pain threshold at the very short-term [52].
The evidence from this current SR is consistent with evidence provided from previous systematic reviews [75, 94, 56] reporting on the efficacy of MT for NP. However, the current review provides new evidence in this regard, as well as improves understanding of the levels of evidence for manual therapists. Due to the very large body of evidence regarding MT for NP, and the inability to present all this information in a single paper, we focused on RCT’s with low-risk of bias that would update and improve on previous reviews. This new evidence and confirmation of previous reviews can be seen in summary in Table 3.
This review provides manual therapists with information about treatment efficacy covering a wide range of commonly used MT in everyday clinical practice. Rather than combining all MT into a single comparison group we sub-categorized MT into 4 distinct groups combined or not with exercise. This enables the reader to better understand the evidence for different forms of MT and whether the addition of exercise improves treatment efficacy.
In addition to understanding the evidence for the efficacy of MT it is important to recognize any potential risks associated with MT intervention. This is particularly true for the cervical spine, which has a special vulnerability due to its unique anatomy and proximity to the brain. In the literature, MT to the cervical spine is often associated with adverse events particularly with regard to HVLA thrust techniques. Adverse events are important, not only from a morbidity/injury perspective, but also in terms of patient satisfaction and perception of improvement following treatment, which might be decreased in patients who experience adverse events [57]. In general however, there is a lack of consensus in reports of RCT’s regarding the classification and definition of adverse events following interventions. When adverse events have been reported we have described these adverse events for each included study in the result section. Future studies should follow more rigorous and standardized methods to allow more effective comparisons [58, 59, 60, 61, 62, 63, 64, 65].
Clearly, a way to prevent adverse events is not to perform cervical manipulation, and perhaps manipulate the thoracic spine instead. It is suggested that thoracic manipulation may have some efficacy in the treatment of neck pain [75]. However, there is moderate evidence favouring cervical over thoracic manipulation for acute NP [42]. Combining cervical mobilization with thoracic manipulation may be one way to bypass the risks involved with certain cervical techniques and also improve treatment efficacy [48]. In chronic NP, although moderate evidence was found in favour of cervical manipulation when compared to accessory mobilization or SNAGs to the cervical spine [49, 50], reported differences were marginal for Cx extension ROM only as well as pain at rest. Furthermore, there is moderate evidence of no difference between cervical and thoracic spinal manipulation at least in terms of immediate effects [52]. Hence, it is important to assess whether such small marginal improvements in outcome favouring Cx manipulation can be justified against the risks involved. Due to the rarity of serious adverse events following cervical MT techniques [66], it is virtually impossible to clearly identify the risk benefit analysis of Cx manipulation. Further investigation is required to compare a cervical and thoracic spine treatment approach against cervical manipulation alone, as well as the long-term effects. Meanwhile, we recommend the guidelines from a consensus of experts (
NP classification
To our knowledge, and in contrast to LBP, there are no recommended or validated classification systems to stratify NP and to target specific subgroups with OMT treatment formulated for each subgroup. Classification of patients with LBP into sub-groups and the application of specific OMT interventions for each matched sub-group has proved to be more effective than generic forms of treatment [67, 68, 69, 70, 71]. Consequently, stratified care for LBP is becoming a dominant topic in research and clinical practice [91, 68, 71].
Due to the lack of classification systems for NP, the treatment decision to apply a specific form of MT (MT1-4) and/or exercise is mainly based on clinical reasoning, which must include the subjective and physical examination. Firstly, the subjective examination should help to identify and exclude people with psychosocial issues (yellow flags) and serious spinal pathologies (red flags) [69]. Secondly, the dominant pain mechanism should be identified, and can be broadly divided into three categories. These categories are the “input mechanisms” corresponding to nociceptive pain and peripheral neuropathic pain; the “processing mechanism” defined as centrally maintained pain associated with central sensitization, and the cognitive-affective mechanisms of pain; the “output mechanisms” include the autonomic, motor, neuroendocrine and immune systems [69, 70, 71]. Thirdly, therapeutic goals and OMT treatment options can be determined from the integration of the subjective and physical examination [69, 70, 71].
Limitations
The results of our qualitative SR should be interpreted in the light of some limitations. First, although only low-risk of bias RCTs were include, there was much heterogeneity among trials; including the way the trial data was presented, the patients, comparison (control) groups (and co-interventions), outcomes measures, and studies’ design, as well as the report of adverse events. Secondly to identify which MT intervention should be evaluated, we used an original and comprehensive classification system in accordance with a comprehensive analysis of the literature as well as with clinical practice of MT. This classification system was used in a previous SR of MT for low back pain [91]. However, there is currently no ideal classification of MT techniques as MT is broad by nature. The MT2 category may be seen as the weakest category in this classification system, as it comprises a very wide range of mobilization techniques as well as articular MET and/or STT. For this reason we described throughout the text and tables the specific interventions used in RCT’s investigating MT2; attempting to improve understand of the efficacy of this MT approach for NP. Due to the heterogeneity among trials, a meta-analysis enabling pooled statistics of effect was not possible. Thirdly, some studies used adjuvant therapy in both intervention and comparison groups which create difficulties to evaluate objectively the intrinsic efficacy of MT. Finally, only studies published in English from 1
Conclusion
This SR has confirmed previous evidence and increased levels of confidence regarding efficacy of MT for NP. The clinical implications of this evidence can be broadly summarized to a number of points. Firstly, in general it can be seen that combining different forms of MT with exercise is better than MT or exercise alone. Secondly, there is moderate to strong evidence in favor of MT1 or MT3 combined with exercise for improvement in pain, function, and satisfaction with care for patients with NP when compared to UMC, exercise alone, MT alone or to no treatment. Thirdly, there is strong evidence that for chronic NP mobilization need not be applied at the symptomatic level for improvement in pain and function. This may have implications for reducing the risk involved with some MT techniques applied to the Cx as well as to choose the level(s) of Cx treatment in function of the irritability state of the patient. Fourthly, there is moderate evidence that in general MT1, MT2 and MT4 have similar effects on NP. Since intuitively Cx manipulation carries greater risk than mobilization or MWM these interventions could be seen as a viable option to manage NP together with exercise and in combination with Tx MT1. Future RCTs should be more rigorous in their investigation by not mixing categories of patients as well as intervention types.
Footnotes
Conflict of interest
None to report.
Appendix 1
Classification of outcome measures and Cochrane Collaboration Back Review Group (CCBRG) Levels of evidence for evaluating interventions [95, 101]
Outcome measures
Validated assessment tools
Pain
Visual analogue scale (VAS) and numerical-pain-rating-scale (NPRS) pressure pain thresholds (PPT)
Functional disabilities
Neck-Disability-Index (NDI), Fear-Avoidance-Belief-Questionnaire (FABQ), the Northwick-Neck-Pain-Questionnaire (NPQ), the cervical-Range-Of-Motion (CROM)
Overall-health improvement
Short-form-health-survey (SF-36)
Quality of life
Adverse events
Overall level of evidence
Conditions description
Strong
Consistent findings from multiple high quality trials (level A) (
3)
Moderate
Consistent findings among multiple moderate quality (level B) and/or one level A
Limited
One level B
Conflicting
Inconsistent findings among multiple trials
No evidence
No trials
Search strategy in MEDLINE
“Manual-Therapy” was used as a free-term in MeSH (MEDLINE). “Musculoskeletal-Manipulations” was the result of the MeSH heading terms, we added “Neck-Pain” to the MEDLINE search box as follows: “Musculoskeletal-Manipulation” [Mesh] and “Neck-Pain” [Mesh] and (“human” [MeSH-Terms] and (“male” [MeSH-Terms] or “female” [MeSH-Terms]) and Randomized-Controlled-Trial [ptyp] and English [lang] and “adult” [MeSH-Terms] and “2000/01/01” [PDat]: “2015/12/31”[PDat])
Risk of bias assessment
Appendix 2
Table 3) (1) and studies that have been excluded from the SR (2)
Studies that only confirmed previous evidence (not included in
(1) Authors, journals and quality score of included studies that confirmed previous evidences
Llamas-Ramos et al. 2014
Level B (7/11 cochrane-list)
Madson et al. 2012
Level B (8/11 cochrane-list)
Salom-Moreno et al. 2014
Level B (8/11 cochrane-list)
Leaver et al. 2010
Level B (8/11 cochrane-list)
Saavedra-Hernandez et al. 2013
Level A (9/11 cochrane-list)
Cleland et al. 2007
Level B (8/11 cochrane-list)
Suvarnnato et al. 2013
Level B (8/11 cochrane-list)
Dziedzic et al. 2005
Level A (9/11 cochrane-list)
Saayman et al. 2011
Level B (8/11 cochrane-list)
(2) Authors, journals and quantitative and/or qualitative criteria for reason of exclusion
Beltran-Alacreu et al. 2015
6/11 cochrane-list
Zaproudina et al. 2007
5/11 cochrane-list
Snodgrass et al. 2014
Mixed population
Ylinen et al. 2007
6/11 cochrane-list
Lluch et al. 2014
Mixed population
Martinez-Segura 2006
Mixed population
Vernon et al. 2013
Mixed population
Hoving et al. 2006
Mixed population
Dunning et al. 2012
Mixed population
Palmgren et al. 2006
5/11 cochrane-list
Martel et al. 2011
Mixed states
Cleland et al. 2005
Mixed population
Escortell-Mayor et al. 2011
Mixed population
McReynolds et al. 2005
6/11 cochrane-list
Boyles et al. 2010
Mixed population
Evans et al. 2003
Mixed states
Groeneweg et al. 2010
Mixed population
Hurwitz et al. 2002
Mixed population
Kanlayana- photporn et al. 2010
Mixed population
Hoving et al. 2002
Mixed population
Mansilla-Ferragut et al. 2009
5/11 cochrane-list
Wood et al. 2001
Mixed population
Strunk et al. 2009
Mixed population
Van Schalkwyk et al. 2000
Mixed population
Walker et al. 2008
Mixed population
Hanten et al. 2000
Mixed population
Häkkinen et al. 2007
Mixed population
Ali A et al. 2014
6/11 cochrane-list and mixed population
