Abstract
OBJECTIVES:
This study aims to evaluate and compare four breast cancer subtypes defined by immunohistochemistry expression of ER, PR, and HER-2 in correlation with Ki-67 and GATA-3 expression.
METHODS:
Slides from 89 paraffin blocks of invasive breast cancer patients with four molecular subtypes based on HER-2, ER, and PR expression were then stained with Ki-67 and GATA-3 antibodies to evaluate their expression in correlation with molecular subtype and metastases to lymph nodes.
RESULTS:
This study was a retrospective study of 89 invasive breast cancers. Luminal A; Luminal B; HER2+; and triple-negative types were 35 (39.3%), 10 (11.2%), 27 (30.3%), and 17 (19.1%) samples. Expression of Ki-67 was increased in triple-negative (TN) tumor compared to non-triple-negative (non-TN) tumor subtypes (p < 0.05). This Ki-67 expression was inversely correlated with the positivity of hormone receptor expression related to lymph-node metastases in TN-type tumors. Sixty-two (57%) samples were immunohistochemically positive for GATA-3. GATA-3 positive samples were significantly more likely to be ER and PR-positive, Ki-67 negative, and luminal A tumors.
CONCLUSIONS:
Subtype triple-negative breast cancer correlates with high expression of Ki-67 that contributes to poor prognosis of this subtype. The higher Ki-67 expression was correlated with the absence of hormone receptor expression compared with the negativity of Her-2 expression, downplay a role in nodal metastases in a triple-negative tumor. GATA-3 positive breast cancer showed luminal differentiation characterized by high ER expression and mainly was classified as luminal A type tumor with a better prognosis.
Introduction
Breast cancer is still the deadliest cancer in the world for women. Recent statistics in the United States reveal that it accounts for 232,340 total cancer cases and 39,620 cancer deaths each year. Several risk factors play an important role in female breast cancer. These include the age of menarche and menopause, hormones, genetics, parity, lactation, obesity, physical activity, diet, alcohol, smoking, and history of a previous biopsy or other mammary examination [1].
So far, the exact causes of breast cancer are still unknown. Approximately 50% of human cancers have mutations in their p53 gene, including in breast cancer. Germline mutation of BRCA1 may increase the risk of breast cancer by up to 80% by the age of 70, whereas in BRCA2 mutation, the risk may reach 50%.
HER2 (Human Epidermal Growth Factor Receptor 2) is a protein encoded by the ERBB2 gene. Amplification of this gene leads to the overexpression of HER2 protein, which results in increased proliferation and differentiation of cells [2]. Estrogen is a hormone that acts as a signal molecule in cells that express an estrogen receptor (ER), as in breast epithelial cells. Estrogen binding with ER will activate the estrogen-responsive genes to regulate cell growth and differentiation [3]. Like estrogen, progesterone will also affect the activity of breast cells that express progesterone receptors (PR), which then activate the various genes involved in cell proliferation.
Ki-67 is a protein encoded by the MKI-67 gene. This nuclear protein plays a role in cell proliferation and transcription of ribosomal RNA. The Ki-67 protein will be detected in the active phase of cell division (G1, S, G2, and M) and undetectable in phase G0.
GATA-3 is a GATA transcriptional factor family member that binds to the DNA consensus sequence (A/T)GATA(A/G). Its gene lies on chromosome 10p15 [4]. GATA-3 is expressed on the luminal cell nucleus [5]. This protein plays a role in the normal proliferation and differentiation of luminal epithelial cells of the mammary glands [6].
Materials and methods
Tissue samples
Eighty-nine formalin-fixed and paraffin-embedded specimens from patients diagnosed with invasive ductal carcinoma mammae were selected from histopathology files of the Department of Anatomical Pathology at Hasanuddin University in Indonesia.
Antibodies and immunohistochemistry
The specimens were cut in 5 μm sections and immunostained using primary antibodies against HER-2, ER, PR, Ki-67 (DAKO, Carpinteria, USA), and GATA-3 (Biocare, USA). Antibody dilutions and immunohistochemical procedures were performed by using streptavidin-biotin-peroxidase methods according to the manufacturing company’s standards and guidelines. Diaminobenzidine chromogen was used to visualize the protein expression.
Statistical analysis
The results were analyzed statistically using a one-way analysis of variance (ANOVA) with the unpaired t-test. Any value of p < 0.05 was considered statistically significant.
Results
Characteristics of 89 breast cancer samples in this study are listed in Table 1. The mean age of all samples was 47.5 years (SD = 9.68, range 37.8 to 57.1 years). Immunohistochemical staining using antibody HER-2, ER, PR, Ki-67, and GATA-3 were performed on these samples. Stained specimens were then grouped into molecular subtypes based on HER-2, ER, and PR expression. Samples of luminal A subtypes included ER+/PR+, HER-2-, ER−/PR+, HER-2-, ER+/PR−, and HER2-. Luminal B subtypes included ER+/PR+, HER-2+, ER−/PR+, HER-2+, and ER+/PR−, and HER−2+. Samples with ER−/PR− and HER2+ included HER2+ subtypes, and those with ER−/PR− and HER2- were triple-negative subtypes. Each subtype was compared with GATA-3 and Ki-67 expression and other variables.
Characteristics of samples
Characteristics of samples
In immunohistochemical studies in these slide samples, the expression of ER, PR, GATA-3, and Ki-67 proteins were expressed on the nucleus of tumor cells with varying percentages. In comparison, HER-2 proteins were expressed along the membrane of tumor cells with varying intensities that form a honeycomb appearance (Fig. 1).
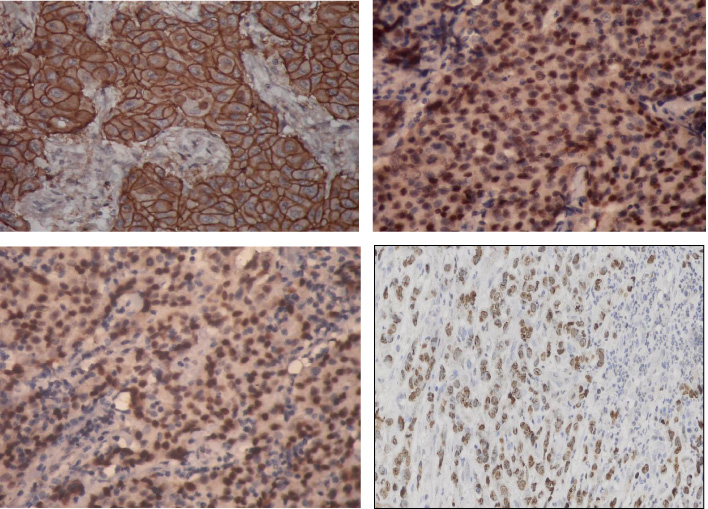
(A) HER-2 expression in breast cancer tissue (400×). (B) ER expression in breast cancer tissue (400×). (C) PR expression in breast cancer tissue (400×). (D) GATA-3 expression in breast cancer tissue (400×).
Out of 89 samples of breast cancer, 17 (19.2%) were triple-negative types (TN) and 72 (80.8%) were non-triple-negative (non-TN) types, which consist of 35 (39.3%) Luminal A, 10 (11.2%) Luminal B, and 27 (30.3%) HER-2 types. The expression of Ki-67 in the TN group (mean ± SE, 68.6% + 3.5%) was significantly higher than in the non-TN tumor group (35.2% + 2.3%, p < 0.0001; unpaired t-test).
In Table 2, tumor cells expressing Ki-67 in the Triple-negative (TN) group were significantly more than in the two groups of non-TN tumors (Luminal A and B). However, there is no significant difference between the other non-TN groups (HER2 type). There was only a significant difference in the Ki-67 expression among non-TN groups, i.e., between Luminal A and HER2 types. Although the percentage of Ki-67 expression was higher in the Luminal B than in the Luminal A group, the difference was not statistically significant.
The expression of ki-67 by subtypes tumor of breast cancer
The percentage of Ki-67 expression was presented in mean ± SE, #Luminal A versus Triple-negative; @ Luminal A versus HER-2; $Luminal B versus Triple negative, p < 0.05.
Ki-67 expression was compared with TN tumors and non-TN tumors with both positive metastases to lymph nodes to determine whether the cell proliferation affects metastasis of breast cancer to the lymph nodes. The Ki-67 expression was significantly higher in TN tumors with positive metastasis than in non-TN tumors (59.5% ± 4.3% versus 29.6% ± 3.1%, p < 0.001).
Out of 89 samples of breast cancer, 62 (57%) specimens expressed GATA-3 immunohistochemically. Samples with GATA-3 expressed were more significantly shown in well-differentiated grade (P < 0.001), associated with positive ER (P < 0.001), positive PR (P < 0.001), and negative Ki-67 expression (P = 0.017), and not related to the presence or absence of metastasis to the lymph nodes (Table 3). This study also found that the breast cancer specimens which expressed GATA-3 were more common in the Luminal A than other types (Table 4).
Expression of GATA-3 correlated with sample characteristics
aGATA-3 positive versus negative, p < 0.05.
Expression of GATA-3 in breast cancer subtypes
aGATA-3 positive in Luminal A versus other types.
Breast cancer is a tumor that has variations in the course of the disease and response to therapy. In addition to degrees and stages, breast cancer is also routinely examined for hormone receptor status (ER and PR) and HER-2 expression with immunostaining or in situ hybridization to determine the adjuvant therapy. Patients with ER-positive-primary tumors will be recommended to get adjuvant hormonal therapy, such as tamoxifen, for 5 years, while postmenopausal women will receive aromatase inhibitors. Patients with HER-2 over-expression will be advised to receive trastuzumab therapy targeted to HER-2/neu receptors. However, only 60% of patients benefited from endocrine therapy, and 30–40% of patients benefited from trastuzumab therapy.
The recent research was performed on several new biomarkers to predict responses based on molecular biology activities, but only a few were used in routine clinical practice. Previous research has classified breast cancer based on molecular and immunostaining results from hormone receptor and HER-2 expression. Besides being an indicator in determining adjuvant therapy, immunohistochemical expression of HER-2 and hormone receptors can be used as a predictor of the tumor characteristic.
In this study, it was shown that younger patients were found more in the triple-negative subtype (ER/PR-, HER2). The triple-negative subtype is a high-risk type of tumor because it does not benefit from targeted therapy aimed at these two receptor proteins. Since there is no specific therapy for this subtype, an understanding of its biological nature was needed, which will be the basis for developing effective treatment strategies.
The number of breast cancer samples expressing Her-2/neu in this study was lower than those expressing ER and PR. This has implications for the high number of Luminal A and triple-negative subtypes in this study. We cannot confirm whether there is a racial influence on HER-2/neu expression. A study conducted in Thailand has found a low number of breast cancers that express HER-2/neu. The definitive explanations cannot be made until there are results from various studies involving large numbers of patients who can support these results.
ER and PR expression in breast cancer was generally associated with a better prognosis. On the contrary, HER-2 expression renders a poor prognosis. Therefore, it is very important to determine the status of ER, PR, and HER-2 at the time of the initial diagnosis of surgical tissues.
In this study, it was shown that Ki-67 expression was higher in the TN tumor group compared to the non-TN tumor group. This represents that Ki-67 has a role in the poor prognosis of TN tumors. These results support many studies conducted on other tumor types, where tumors with poor prognosis have high Ki-67 expression and reveal high proliferative activity.
We also wanted to see whether the hormone receptor or Her-2 expression influences Ki-67 expression. In this study, the absence of hormone receptor expression was significantly related to the high number of Ki-67 expression but was not related to negative Her-2 expression. Hormone receptors have a significant effect on Ki-67 expression wherein tumors with receptor hormone (ER and or PR) are negative, Ki-67 expression is higher than tumors with positive hormone receptors. There is no influence from the presence of HER-2 expression on the expression of Ki-67.
In this study, we also found that Ki-67 expression in TN tumors with metastases to lymph nodes was higher than in non-TN tumors metastasized to lymph nodes. In previous studies, high Ki-67 expression affected the frequency of tumor metastasis to the lymph nodes [7]. Therefore, high Ki-67 expression, especially in TN tumors, contributes to the high risk of lymph node metastasis.
In human breast tissue, GATA-3 is expressed in luminal epithelial cells, and its expression is also seen in breast cancer [6,8]. GATA-3 expression is closely related to estrogen receptor (ER) in breast cancer [9]. This fact strongly indicates that GATA-3 plays an important role in the growth and differentiation of luminal epithelial cells that are consistent with the pattern of expression of GATA-3 in the type of luminal mammary carcinoma. GATA-3 is known to cause invasive breast cancer cells to undergo reversal epithelial-mesenchymal transition that will inhibit cancer spread and metastasis.
Immunohistochemical staining in this study showed that breast cancer samples expressing GATA-3 tended to express ER and PR, and most of them belonged to the luminal type A. This result follows the function of GATA-3, where this protein plays an important role in the process of differentiation of progenitor cells into luminal epithelial cells.
A previous study reported that low GATA-3 expression was associated with larger tumor size, metastases to lymph nodes, poorly differentiated, positive ER, and negative HER-2 [10]. In general, positive GATA-3 expression is a good marker of prognosis for breast cancer.
In conclusion, this study shows that the Luminal A subtype has a higher incidence than other breast cancer subtypes. TN-type breast cancer is associated with high Ki-67 expression, which can contribute to the poor prognosis of this type of tumor. The high Ki-67 expression is related to the absence of the hormone receptor, but not in the absence of HER-2 expression. High Ki-67 expression, especially in the triple-negative type, plays a role in the possibility of tumor cells metastasizing to the lymph nodes. Breast cancer that expresses GATA-3 is also seen to express ER and reflect the phenotype of Luminal A tumor. Like ER, GATA-3 is associated with a favorable prognosis.
Footnotes
Acknowledgements
The authors do not have acknowledgments.
Conflict of interest
None.
Funding
None.
