Abstract
Background:
Short cognitive screening instruments (CSI) are required to identify cognitive impairment in busy outpatient clinics. While the Six Item Cognitive Impairment Test (6CIT) is commonly used, its accuracy in those with mild cognitive impairment (MCI) and subjective cognitive decline (SCD) and against more widely-used CSIs is less well established.
Objective:
To examine the diagnostic accuracy of the 6CIT against the Montreal Cognitive Assessment (MoCA) and Quick Mild Cognitive Impairment (Q
Methods:
In total, 142 paired assessments were available (21 with SCD, 32 MCI, and 89 with dementia). Consecutive patients underwent a comprehensive assessment and were screened using the 6CIT, Q
Results:
The median age of patients was 76 (±11) years; 68% were female. The median 6CIT score was 10/28 (±14). The 6CIT was strongly, negatively, and statistically significantly correlated with the Q
Conclusion:
While the Q
Keywords
INTRODUCTION
The prevalence of cognitive impairment (CI) including dementia is expected to increase worldwide to over 150 million people by 2050 [1], generating additional workload in already busy primary and secondary care (outpatient) clinics, as systems work towards better and earlier diagnosis [2]. Guidelines and recommendations support the need to provide diagnostic services close to patients in the community, but several structural barriers exist aggravated by staff shortages and inadequate training [3]. Screening of symptomatic patients is further limited by a lack of suitably sensitive and specific instruments [4–6]. While a wide variety of performance-based instruments are available, they vary in their administration times, cognitive domains assessed and ability to differentiate between normal cognition, mild cognitive impairment (MCI), and dementia [7], though it is suggested that no single instrument will likely suit all situations [7]. These are also influenced by the well-documented time-accuracy trade off such that short screens tend to lower levels of diagnostic accuracy [8].
The Six-Item Cognitive Impairment Test (6CIT) [9], is a commonly-used short cognitive screening instrument (CSI) and is reported to have high diagnostic accuracy for dementia in an older hospital population (90% sensitivity and 96% specificity at a cut-off of ≥8/28 for dementia) [10]. There are, however, relatively few studies examining its performance in outpatient (secondary care) settings [11] and especially in persons with MCI, before the onset of functional decline and in those with subjective cognitive decline (SCD), where individuals are symptomatic but do not have evidence of cognitive impairment on testing. A recent validation in a memory clinic population showed a sensitivity of 88% for dementia and 66% for MCI [11] when compared to the Mini-Mental State Examination (MMSE). Further, few studies have compared the 6CIT to other short screens and none to those useful in identifying early cognitive decline [12]. A recent systematic review in 2018 suggests that additional robust validation studies are needed, comparing the 6CIT to a wide range of short cognitive assessments [12].
Given these points, this study aims to compare the diagnostic accuracy for cognitive impairment of the 6CIT against two other short CSIs, the Quick Mild Cognitive Impairment (Q
METHODS
Participants
This cross-sectional study was conducted parallel to a study evaluating the Q
Measures
Six-Item Cognitive Impairment Test
The 6CIT is a short (usually administration time between 2–3 minutes), CSI including seven questions covering three domains (orientation, episodic memory, and attention) [9]. The 6CIT is scored out of 28 points with higher scores suggesting cognitive impairment. Initially designed to detect dementia using a cut-off of ≥8/28, it is also validated in MCI [11] though sensitivity (66%) and specificity (70%) are low. A cut-off of ≥8/28 for dementia was used for the 6CIT [10] but more recently a cut-off of 9 or 10 is suggested based on more recent studies [12]. It does not have established cut-off scores for cognitive impairment.
Quick Mild Cognitive Impairment screen
The Q
Montreal Cognitive Assessment
The MoCA is a short CSI with seven subtests covering five cognitive domains including visuospatial, attention, processing speed, language, memory, and cognitive control scored out of 30 points with lower points indicating cognitive impairment. For screening in primary care, where high sensitivity is required, the established MoCA threshold of <26/30 is suggested [17]. Again, lower scores suggest more impaired cognition.
Data collection
Consecutive referrals underwent a comprehensive work-up for memory loss including history, physical examination, laboratory testing and neuroimaging. A short neuropsychological battery including the standardized MMSE (SMMSE) [24, 25] and two informant-rated assessments, the AD8 questionnaire [26] and IQCODE Short Form [27] were conducted by a consultant geriatrician, blind to the results of the CSIs, to inform the diagnosis. Cognitive screening was performed in a random counterbalanced order, approximately one hour before consultant review, by two independent trained raters, blind to each other and the final diagnosis. Alternate validated versions of verbal fluency (semantic for categories, e.g., animals) and logical memory (immediate verbal recall of a short story) were used for the Q
Analysis
Data were analyzed using R version 3.5.0 (2018-04-23) -“
RESULTS
In all, results for 142 patients with complete data were available and included in this analysis. The characteristics of participants according to each of the three diagnostic categories are presented in Table 1. The median age of these was 76 years, interquartile range (IQR)±11 (Q3–Q1 = 81–70), and the majority, 68%, were female. The median number of years in education was 12±4 years. Most (i.e., 63%,
Characteristics of symptomatic patients (
6CIT, Six-Item Cognitive Impairment Test; IQR, interquartile range; MoCA, Montreal Cognitive Assessment; Q, Quartile; Q
Correlations (
6CIT, Six-Item Cognitive Impairment Test; IQR, interquartile range; MoCA, Montreal Cognitive Assessment; Q
Table 3 provides the optimal cut-off scores according to Youden’s Index compared with previously published values along with the psychometric properties for each of the three CSIs for identifying cognitive impairment (MCI or dementia) at these points. In this sample, the optimal cut-off for the 6CIT was ≥7, which provided a sensitivity of 77% and specificity of 90% for cognitive impairment. At its established cut-off (9/10) [12], the 6CIT had lower and relatively poor sensitivity for cognitive impairment (68%), albeit with high specificity (95%). In this sample, the Q
Sensitivity, specificity, positive predictive value (PPV), negative predictive value (NPV), positive (PLR) and negative likelihood ratio (NLR) with 95% confidence intervals (CI), for the Six-Item Cognitive Impairment Test (6CIT), Quick Mild Cognitive Impairment (Q
*Recommended cut-off score; ∧Optimal cut-off based on Youden’s Index; †Weighted for Prevalence (unweighted likelihood ratios are presented in the Supplementary Material); NA, not available.
ROC curves showing the diagnostic accuracy of the CSIs for cognitive impairment are presented in Fig. 1, comparing the 6CIT to both the Q
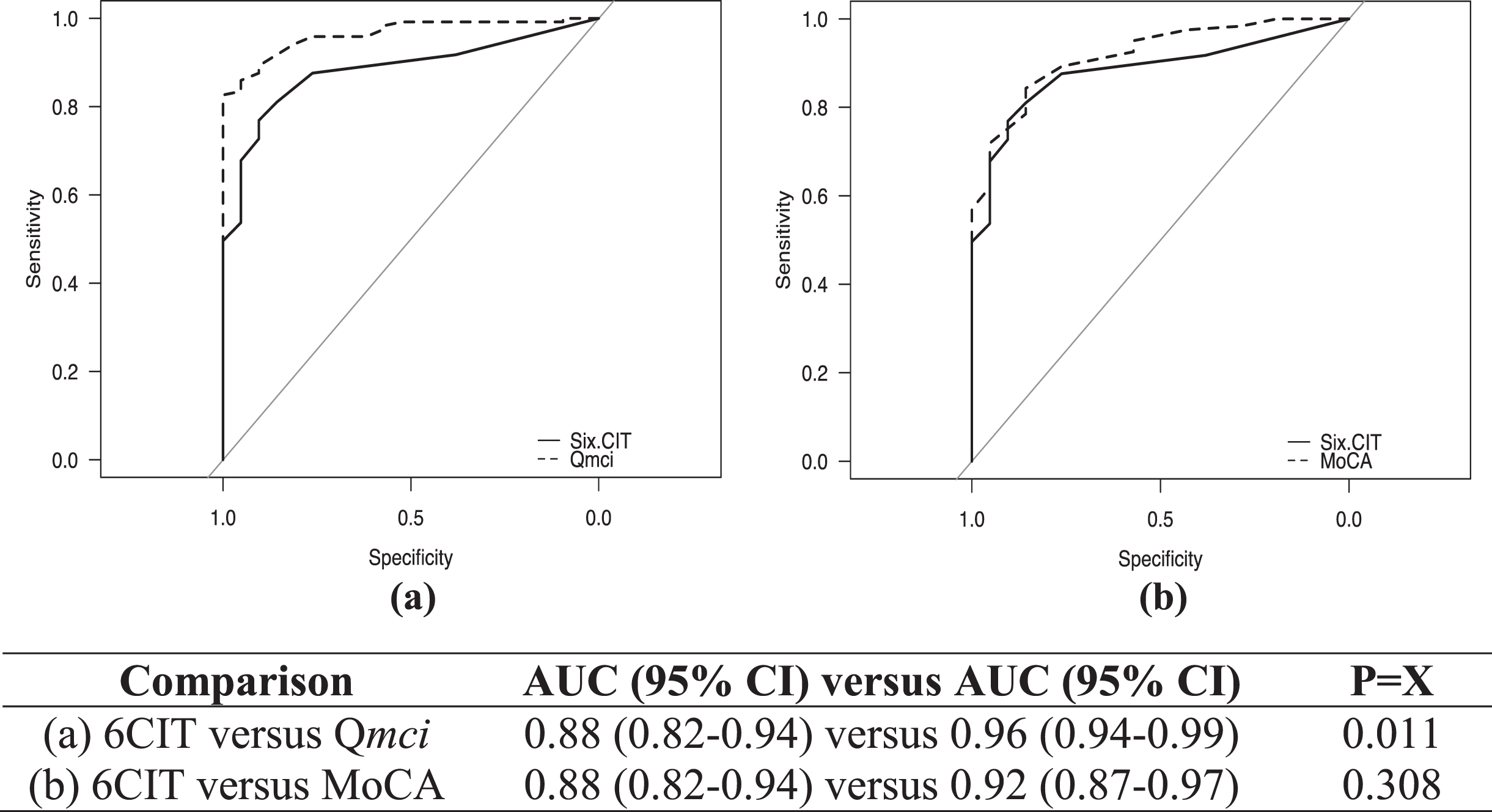
Receiver operating characteristic curves with area under the curve (AUC) scores with 95% confidence intervals (CI), showing the accuracy of the Six-Item Cognitive Impairment Test (6CIT) compared with the (a) Quick Mild Cognitive Impairment (
DISCUSSION
This study provides a psychometric evaluation of the 6CIT, validating it against two commonly-used short CSIs in a geriatric memory clinic population, where it showed strong and statistically significant correlation to two “MCI-specific” short CSI, the Q
The accuracy of all three instruments remained after adjustment for the effects of age and education. The difference in diagnostic accuracy between the Q
In this study, the optimal cut-off for the 6CIT was ≥7/28, yielding a good sensitivity of 77% and excellent specificity of 90% for cognitive impairment. This is lower than its more established cut-off of ≥8 [10] and the more recently-recommended cut-off of 9 or 10 out of 28 points [12]. The 6CIT, however, had low and relatively poor sensitivity for cognitive impairment at 9/10 (67–68%), albeit with high specificity (95%). In this sample, the MoCA and Q
This study has a number of limitations. The prevalence of cognitive impairment was high in this sample with only 21 patients with SCD and 32 with MCI being available for analysis, potentially resulting in in spectrum bias. Further, the sample size was small and likely underpowered the study to show superiority of one CSI over another. This study was conducted at a single center, with a homogenous population, potentially reducing the generalizability of the findings. While alternative versions of the MoCA can reduce learning effects, these may differ in their severity level, potentially influencing the accuracy of scores [34]. Further study with a larger sample size is now required to examine the diagnostic performance of the 6CIT in MCI and particularly in differentiating those with MCI and SCD.
In conclusion, while the 6CIT was statistically significantly less accurate for detecting cognitive impairment (either MCI or dementia) and in separating MCI from dementia and MCI from SCD, when compared with the Q
Footnotes
ACKNOWLEDGMENTS
The authors have no acknowledgments to report.
FUNDING
The authors have no funding to report.
CONFLICT OF INTEREST
Dr. Rónán O’Caoimh and Prof. D. William Molloy are co-copyright holders of the Quick Mild Cognitive Impairment screen.
The authors report no other conflict of interest.
