Abstract
A growing body of research has shown that many women, including those who are pregnant, have been victims of intimate partner violence (IPV), including physical and sexual assault [1]. In the last decade, research has examined and identified some of the direct and indirect health consequences of abuse, including physical, mental and reproductive health problems among women [2–5]. Studies have also suggested that children who are exposed to partner violence are at increased risk of developing short-term and long-term behavioural problems, as well as developmental delay, sleep disorders, school failure, depression, and other psychiatric disorders [6–9].
Most of the research examining relationships between IPV and women's mental health consider current violence [10–19]. Only a few studies have combined current and past violence and considered the influence of timing and continuous or repeated exposure [16–19]. In addition, previous studies have typically neglected psychological abuse even though it is the most frequently reported characteristic of violent relationships [20,21], and has been found to affect women's health as much as other types of abuse [22–24]. Most studies of violence and health come from Western cultures. Because it is not a foregone conclusion that Western research findings can be generalized to the vastly different cultures of the Pacific Islands, the present study involving Pacific parents is both theoretically and practically important.
The Pacific population is a demographically young and rapidly growing ethnic group in New Zealand, particularly in Auckland [25]. It represents 6.6% of the total New Zealand population [26]. Relative to the general population, Pacific people experience lower socioeconomic status, poorer health, and lower life expectancy [27].
Some researchers have contended that in Pacific societies the likelihood that family violence is considered normal or at the least acceptable may be higher than in non-Pacific cultures [28]. Within a Pacific context it is postulated that violence within the home may be attributable to the stress of living in New Zealand and related to factors such as unemployment and associated financial concerns [29].
Findings from the Pacific Islands Families (PIF) study, a prospective longitudinal study that follows a cohort of Pacific children and their families living in New Zealand, demonstrate that IPV prevalence rates were high for a general married or cohabiting female sample, with overall physical violence victimization rates of 22.9% [17]. This is much higher than the 5.3% of Auckland women found to have experienced physical violence by an intimate partner within the previous 12 months [10]. We have reported previously that mothers of Pacific children who were victims of any physical IPV in the previous 12 months were more than twice as likely as those who were not victims to report postnatal depressive symptoms at 6 weeks postpartum, after controlling for a range of other risk factors [30]. The aim of the present study was therefore to examine the effects of IPV measured at 6 weeks and 24 months postpartum on maternal mental health and lifestyle behaviour measured at 24 months postpartum. We hypothesized that women who were chronic or recurrent victims of IPV would have the poorest mental health and exhibit riskier lifestyle behaviour than those who were victims at one data point only; and that the latter group, in turn, would have poorer outcomes than those who were not victims at any data point.
Methods
Participants
Data were collected as part of the Pacific Islands Families: First Two Years of Life (PIF) study. This study follows a cohort of Pacific Island infants born at Middlemore Hospital in the year 2000. All potential participants were selected from births in which at least one parent identified as being of a Pacific Island ethnicity and a New Zealand permanent resident. Participants were identified through the Birthing Unit, in conjunction with the Pacific Islands Cultural Resource Unit. Information about the study was provided and consent was sought to make a home visit.
At 6 weeks and 24 months postpartum female interviewers of a Pacific ethnicity who were fluent in English and a Pacific language interviewed mothers within their home environment. Once informed consent was obtained, mothers participated in 1 h interviews concerning family functioning and the health and development of the child, conducted in the preferred language of the mother. Within the context of a wider interview, intimate partner violence and maternal health were measured. Detailed information about the PIF cohort and procedures is described elsewhere [31].
Measures
Intimate partner relationships
IPV was measured using Form R of the Conflict Tactics Scale (CTS), a psychometrically robust scale developed by Straus [32,33]. Participants were asked to enter their responses on an answer sheet while the interviewer read the questions aloud. Mothers reported on their partner's behaviour towards them. The CTS measure of Verbal Aggression includes six items; the Minor Physical Violence scale includes three items; and the scale of Severe Physical Violence includes six items. An individual was considered to be a victim of verbal aggression, minor physical violence, or severe physical violence if she reported that a partner had perpetrated any of the behaviours towards her during the past 12 months. Responses were included in these analyses if participants completed 17 of the 19 CTS items. Cronbach's alpha reliability was: Verbal Aggression, 0.77; Minor Violence, 0.84; and Severe Violence, 0.79 [21]. Physical violence was then defined as a dichotomous variable with two levels: ‘no violence’ or ‘any violence (minor and/or severe)’.
To incorporate the two data points, separate composite measures for verbal aggression and physical violence were formed, with the following categories: (i) not victims; (ii) victims at 6 weeks; (iii) victims at 24 months, and (iv) victims at both data points.
Psychological distress at 24 months postpartum
At 24 months postpartum, maternal mental health was assessed using the 12-item General Health Questionnaire (GHQ-12) [34], a self-report screening tool widely used to identify minor psychiatric disorder in adults. The GHQ-12 was scored to give a total of 12 using the binary method of scoring. A cut-off of 2/3 is recommended for screening psychological disorder. Mothers who scored above the cut-off were referred to as symptomatic, and mothers who scored below as non-symptomatic. The reliability coefficient of the GHQ in the PIF study was 0.87 [35].
Maternal lifestyle behaviour
As part of the 6 weeks and 24 months interviews, mothers were asked about their lifestyle behaviour. Mothers were classified as smokers if they smoked the day before the interview date, and as high-risk alcohol users if they drank six or more alcoholic drinks on at least one occasion in the last 12 months.
Sociodemographic characteristics
Mother's age, ethnicity, marital status, education level, household income, duration living in New Zealand, whether born in New Zealand, and cultural orientation, which were collected at the 6 weeks interview, were taken into account in this analysis.
Statistical analysis
χ2 tests were used to compare the distributions of sociodemographic characteristics between the current study cohort and the PIF mothers who were excluded from the current study. The dependencies between IPV measures at the two data points and the associations between IPV and health outcomes were explored using a χ2 test or Fisher's exact test where appropriate. McNemar's test was used to compare the change of IPV from 6 weeks to 24 months.
Three multivariable logistic regression models were run separately to explore the independent effects of verbal aggression and physical violence on maternal psychological distress (model 1), smoking (model 2), and high-risk alcohol use (model 3) at 24 months follow up. All the sociodemographic factors listed in Table 1 such as maternal age, educational level, ethnicity, duration living in New Zealand, marital status, household income, whether born in New Zealand, and cultural orientation were considered as candidate confounding factors in these analyses. The backward selection method was used to select significant effects from the candidate variables. The composite measures of verbal aggression and physical violence were forced to stay in these models; whereas sociodemographic factors were selected using a backward selection procedure.
All analyses were performed using SAS version 9.1 (SAS Institute, Cary, NC, USA), and a significance level of α = 0.05 was used to determine statistical significance for all calculations.
Subject characteristics
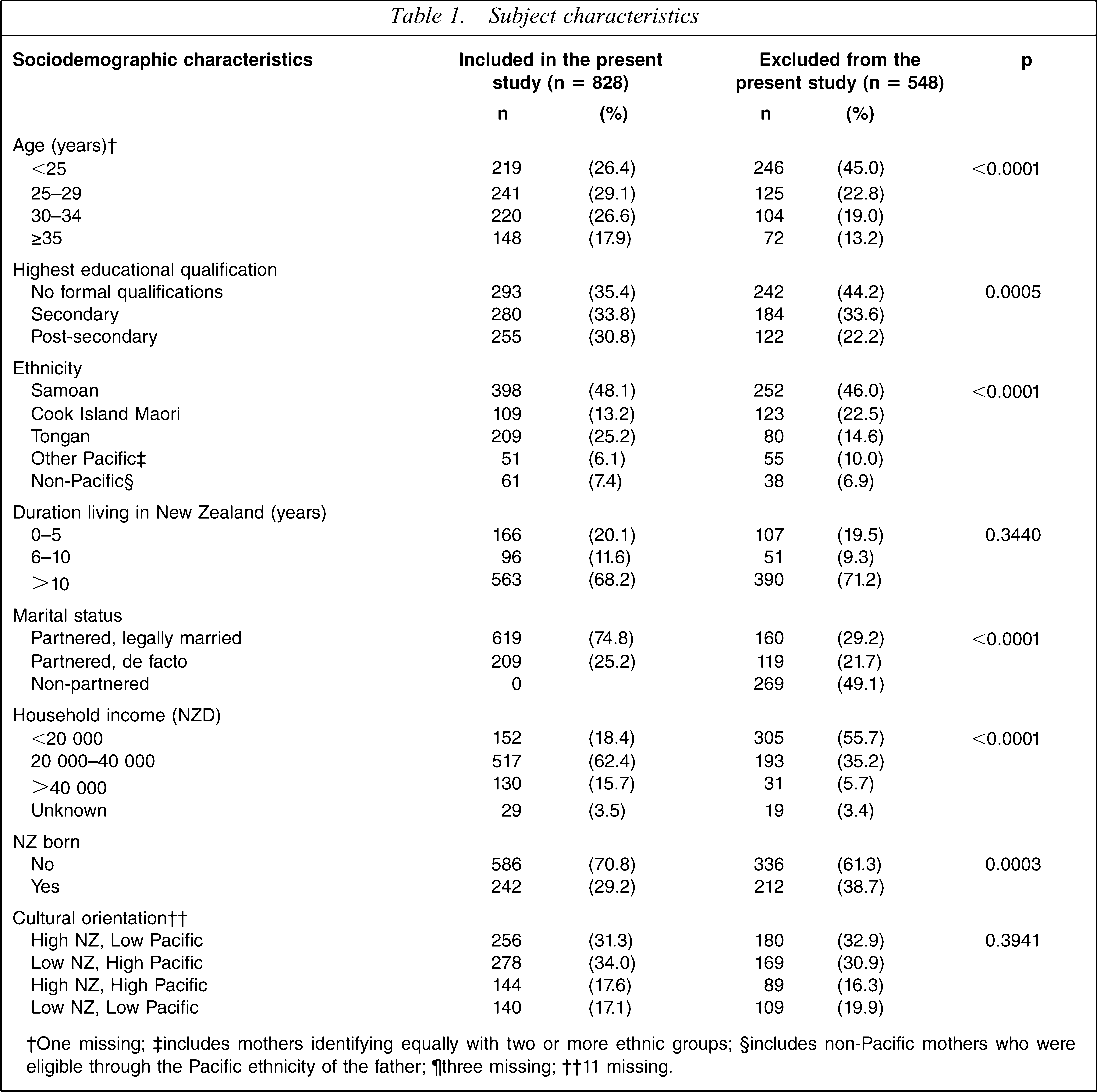
†One missing; ‡includes mothers identifying equally with two or more ethnic groups; §includes non-Pacific mothers who were eligible through the Pacific ethnicity of the father; ¶three missing; ††11 missing.
Change of intimate partner victimization over time

∗p < 0.0001, ∗∗p = 0.029 (McNemar test).
Results
Sample characteristics
Of the 1376 mothers who were interviewed at 6 weeks postpartum, 1144 (83.1%) were re-interviewed at 24 months. Among these mothers, 828 reported cohabiting in married or de facto partnerships at both data points and were included in the current study. The sociodemographic profile of this group differed from that of the 548 mothers who were excluded from the present study due to not being interviewed or being non-partnered at either data point. Compared with the latter group, the current cohort generally had higher educational qualifications, were more likely to be Tongan and less likely to be Cook Island Maori, were more likely to be cohabiting in married partnerships rather than in de facto partnerships, had higher household income, and were more likely to be born in New Zealand. There was no statistical difference, however, between these two groups in terms of duration living in New Zealand and cultural orientation. Details of comparisons of sociodemographic characteristics are presented in Table 1.
Prevalence of IPV
Of the cohort of 828 mothers, 76.2% (631) and 86.0% (712) reported being the victims of verbal aggression at 6 weeks and 24 months, respectively. The corresponding prevalences for physical violence were 22.9% and 27.2%, respectively. The association between IPV at 6 weeks and 24 months postpartum was significant both for verbal aggression and physical violence (both p < 0.0001), indicating that women who experienced IPV at 6 weeks were more likely to be victimized at 24 months. The percentages (frequencies) of the composite measures of verbal aggression were: 5.6% (46) non-victims; 8.4% (70) victims at 6 weeks; 18.2% (151) victims at 24 months; and 67.8% (561) victims at both data points. The corresponding values for physical violence were 59.3% (491), 13.5% (112), 17.8% (147), and 9.4% (78), respectively. McNemar's test indicated that there were more women who became new victims at 24 months than those who stopped being victims at 24 months (p < 0.0001 for verbal aggression and p = 0.0296 for physical violence).
Associations between IPV and maternal health indicators
Of 828 mothers, 825 completed the GHQ at 24 months. The prevalence (frequency) of maternal symptoms of psychological distress was 8.5% (70). Twenty-five per cent (204) of 821 reported smoking and 14.2% (117) of 826 were high-risk alcohol users at 24 months. The prevalence of psychological disorder, smoking and high-risk alcohol use at 24 months versus IPV at the two data points is presented in Table 3.
Rate of maternal psychological distress and lifestyle behaviours vs IPV
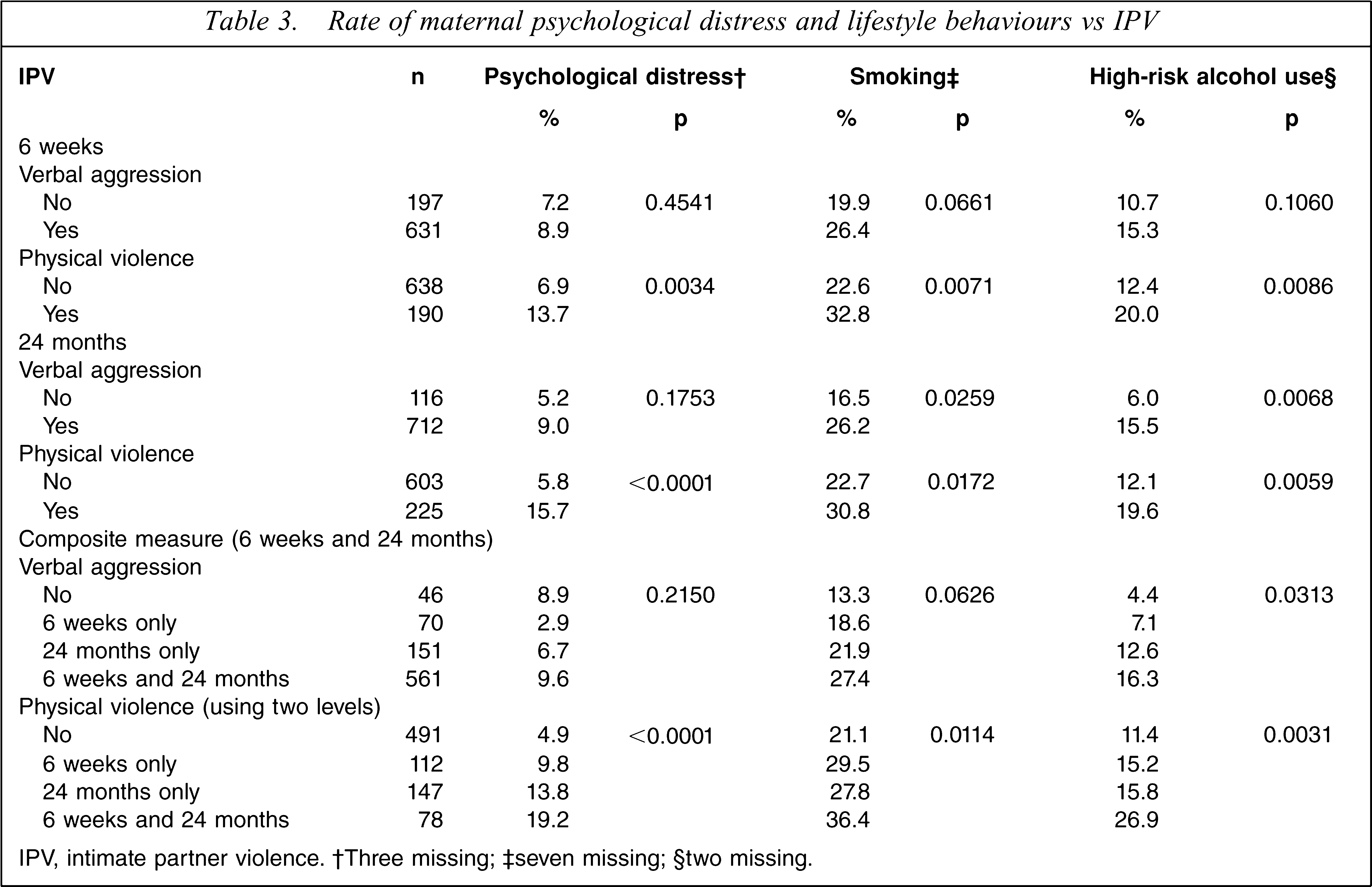
IPV, intimate partner violence. †Three missing; ‡seven missing; §two missing.
Intimate partner violence timing
Being a victim of verbal aggression at 6 weeks did not significantly change the prevalence of psychological disorder, smoking, or high-risk alcohol use compared to non-victims of verbal aggression. Victims of physical IPV at 6 weeks, however, were significantly more likely to be at risk of psychological disorder, high-risk alcohol use, and to be smokers.
The analyses of IPV at 24 months showed similar associations with maternal psychological distress compared with those at 6 weeks. The difference in smoking and high-risk alcohol use, however, became significant between the victims and non-victims of verbal aggression (p = 0.0259 and 0.0068, respectively).
Intimate partner violence duration
The duration of verbal aggression using the composite measure was not significantly associated with maternal psychological distress (p = 0.2150), but was significantly associated with high-risk alcohol use (p = 0.0313), and the association with smoking was marginally significant (p = 0.0626). Duration of physical violence was significantly associated with all three outcome measures (psychological disorder, smoking and high-risk alcohol use).
Multivariable logistic regression analyses
Table 4 shows the effects of IPV on maternal outcomes at 24 months post-partum following adjustment for maternal age, educational level, ethnicity, duration living in New Zealand, marital status, household income, whether born in New Zealand, and cultural orientation. Physical violence was significant in the model for predicting maternal psychological distress, while verbal aggression was not. Compared to women who did not experience physical violence at either data point, women who experienced physical violence at 6 weeks doubled the odds of reporting psychological distress. The odds increased to 3.47 (95% confidence interval (CI) = 1.75–6.86) for women experiencing physical violence at 24 months and 3.84 (95% CI = 1.78–8.30) for those experiencing physical violence at both data points.
Adjusted odds ratio with 95%CI from multivariable logistic regression analyses†
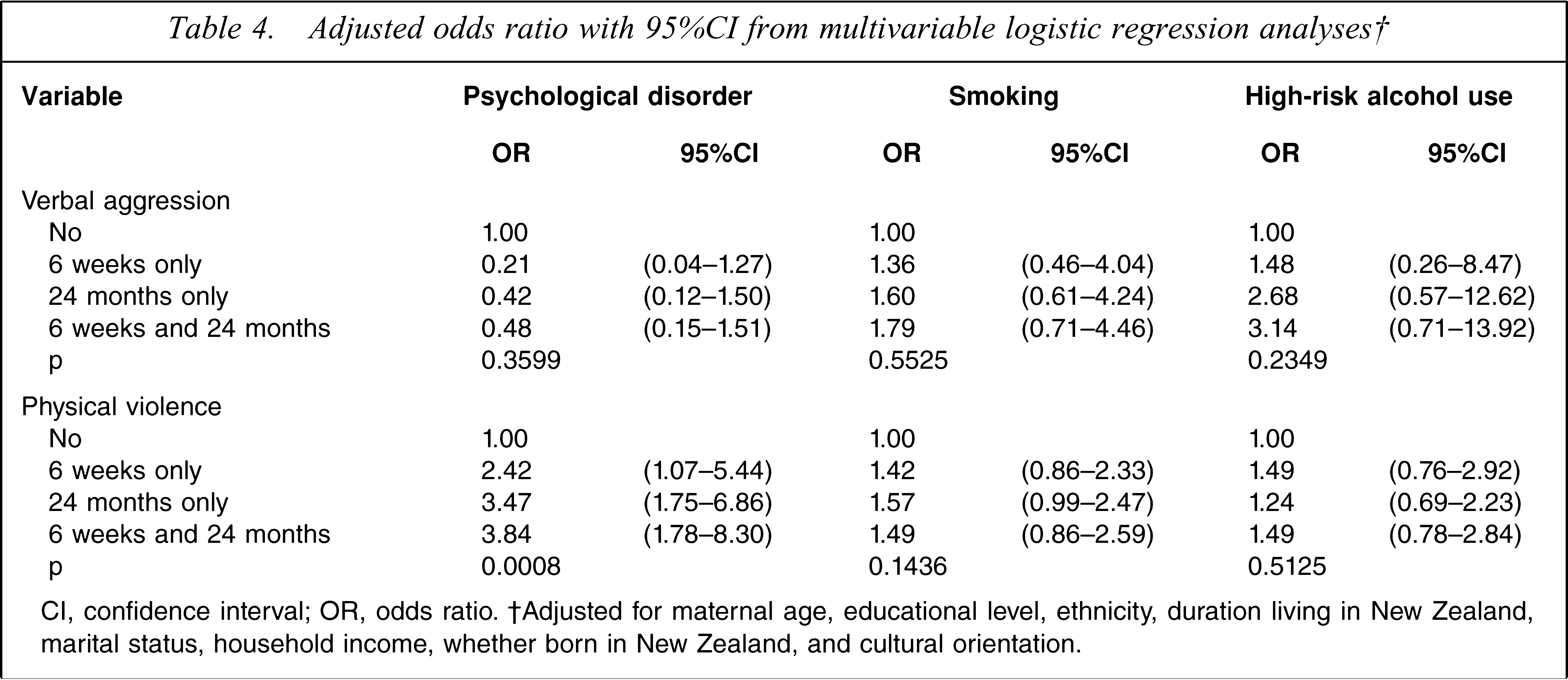
CI, confidence interval; OR, odds ratio. †Adjusted for maternal age, educational level, ethnicity, duration living in New Zealand, marital status, household income, whether born in New Zealand, and cultural orientation.
Neither verbal aggression nor physical violence was significantly associated with smoking or high-risk alcohol use at 24 months after adjusting for confounding factors. All p for these two factors was >0.05.
Additional analyses were undertaken among women who did not report physical violence to examine the independent effects of verbal aggression on mental health, smoking and high-risk drinking, and the results did not differ from the primary analysis results (results not shown).
Discussion
Main results
The aim of the present study was to examine the change in maternal IPV victimization from 6 weeks to 24 months postpartum and the impact of IPV on symptoms of psychological distress and lifestyle behaviour at 24 months postpartum. The findings suggest that mothers were more likely to experience IPV victimization at 24 months postpartum than at 6 weeks postpartum. Although both past and current exposure to physical IPV contributed to an increase in maternal psychological distress at 24 months postpartum, chronic or recurrent exposure contributed the most. Compared to women who did not experience such violence, the corresponding odds of reporting psychological distress was greater than twofold in the past victims group, threefold in the current victims group, and approximately fourfold in the continuous victims group. Although there was suggestion that physical violence and verbal aggression were both associated with lifestyle behaviour such as smoking and high-risk alcohol use, these associations diminished after controlling for other sociodemographic factors.
Research findings on IPV and pregnancy are inconsistent. Some suggest that violence may escalate with pregnancy [36] or during the postpartum period [37]. Others report that rates of abuse were lower during pregnancy than at other times [38, 39]. One study has also reported that while physical and sexual abuse decreased during pregnancy, emotional abuse increased during pregnancy [40]. Two studies that used prospective designs suggested that women were more likely to experience violent events during rather than after pregnancy [41], and that the prevalence of IPV was highest at 3 months post-partum and lowest at 24 months [42]. Although the present study showed an increase in IPV at 24 months postpartum compared to 6 weeks postpartum we did not collect data before pregnancy. Consequently, a complete picture cannot be drawn in terms of the change in IPV during and after pregnancy for Pacific women. More research is needed to further understand the pattern of violence characterizing the pregnancy–postpartum transition. This transition has special significance because it is a vulnerable time and any violent events could severely affect the health and well-being of the mother and infant [30,43].
The magnitude of physical IPV and the association with women's mental health found in the present study are comparable to findings from a number of other studies. Bogat et al. explored whether psychosocial indicators and severity of violence could be predicted from a woman's continuity and history of IPV and found that chronicity of violence (across partners and time) is related to worse psychosocial outcomes and greater severity of IPV [17]. Recency and continuity of IPV with one's current partner, however, affect psychosocial outcomes more negatively than more distal indicators of IPV. Studies conducted in Europe have also suggested that current abuse and past abuse are strongly associated with poor mental health [18, 19]. Synthesizing the findings from the current study with the extant ones suggests that although physical IPV has long-lasting effects on mental health, the impact is greater among women who experienced immediate or recent violence and greatest among those who experienced continuous or recurrent violence.
Although the prevalence of verbal aggression was much higher than physical violence in the present study (76% at 6 weeks and 86% at 24 months), the association with psychological distress was not significant before and after adjusting for confounding factors. In contrast, mothers who experienced verbal aggression or physical violence at both data points were more likely to report smoking or high-risk alcohol use at 24 months than those who did not, but these associations were not significant in the multivariable analyses after controlling for sociodemographic factors. Additional analyses to examine verbal aggression among women who did not report physical violence showed similar results. Contradictory to the present findings that neither physical violence nor verbal aggression was independently associated with either smoking or high-risk alcohol use, a US cross-sectional study reported that both psychological and physical IPV were independently associated with smoking and high-risk alcohol use [44]. Other studies have reported an association between battered women and alcohol use [45], and that IPV preceded both alcohol use and drug abuse in most cases involving presentations to accident and emergency departments [46]. A postulated explanation of substance use as an outcome of IPV is through post-traumatic stress disorder [47]. Women with post-traumatic stress disorder might use drugs or alcohol to calm or cope with the specific groups of symptoms associated with post-traumatic stress disorder: intrusion, avoidance, and hyper-arousal. The association of IPV with smoking has become a focus of research recently. Studies have found that women smokers are more than twice as likely to be victims of violence as women non-smokers [44, 48]. It is possible that differences in design, methodology, cultural norms, and prevalence of violence contribute to the different findings between the present study and others. The use of smoking as a dependent variable and IPV as the explanatory variable in the present study differs from the cited references [44, 48], in which prevalence of IPV was compared between smokers and non-smokers. Furthermore, the high prevalence of verbal aggression and low rates of smoking and high-risk alcohol use in women free of verbal aggression could affect the statistical power to detect the effect size. The far greater prevalence of verbal aggression could mean that it is more important at a population level than is physical violence. More studies are needed in Pacific and other populations to verify the validity of verbal aggression as a measure of psychological abuse and to further examine the impacts of both verbal aggression and physical violence on women's mental health and lifestyle behaviour. The continuity of the PIF cohort study will enable these issues to be revisited later in our longitudinal work.
Methodological considerations
The present longitudinal study has tracked the stability and change in IPV to establish the temporal sequence of events and identify the associations between IPV and maternal health beyond the early postpartum period. These design strengths, together with the size of the cohort and the cultural sensitivity of our methods and procedures demonstrate the robustness of the PIF study findings. The present study, however, is not exempt from limitations.
First, given that the data were based on maternal report, the possibility of bias from self-reporting is present. Second, selection biases as arising from the recruitment of the sample, attrition from the longitudinal sample or from the exclusion of women who move in and out of partner relationships, cannot be ruled out, which in turn will affect the generalizability of the findings. Third, there are considerable obstacles to implying a causal relationship. For example, IPV may (and often does) occur in the context of alcohol use by both partners, so violence may just as much be a consequence of alcohol use as a cause. Fourth, no diagnostic test of women's mental health was obtained to corroborate the self-reported outcome. Last, a few measurement limitations should be mentioned: Some plausible confounding factors were not adequately measured. For example, financial hardship was not directly measured (household income is a poor proxy for this), nor was stress from parenting, which could influence IPV. Further, the measure of high-risk drinking is not an indicator of high general consumption and does not take into account the functions and consequences of alcohol use (i.e. alcohol use may not be a method of coping with personal problems but to increase pleasure). Furthermore, we did not include other potentially relevant individual-difference variables (i.e. alcohol expectancies, generic predisposition and temperament) [49].
Despite these limitations the present study contributes to the scarce data available worldwide on IPV and maternal health and health-related behaviour from different ethnic groups. It is important to address and understand the complex relations between intimate partner violence, mental health, and behaviour to diagnose accurately and intervene in these problems. Reducing partner violence by Pacific peoples has been identified by Pacific communities and government agencies as a priority issue [50]. The present findings that partner violence increases during the postpartum period and the association between IPV and poorer maternal mental health reinforce the importance of early screening and intervention after birth because this is the critical period for both maternal and child care. Mothers who experience psychological distress after birth should be screened and monitored for intimate partner violence to enable early prevention and intervention of adverse health outcomes. Reducing and eliminating partner violence cannot be successful without the partner's involvement, and family and social support. From a disease prevention and health promotion point of view, violence intervention programmes, substance use treatment, and treatment of other forms of psychopathology should be integrated to better respond to multiple and concurrent adverse health outcomes.
Conclusions
Findings suggest that any form of intimate partner physical violence victimization (recent, past and repeated) may contribute to an increase in maternal psychological distress at 24 months postpartum. Health-related behaviours such as smoking and high-risk alcohol use at 24 months postpartum may to some degree be attributable to repeated victimization of physical violence and verbal aggression, but the relationships are not convincing and deserve further research in longitudinal studies.
Footnotes
Acknowledgements
The PIF Study is funded by grants awarded from the Foundation for Research, Science and Technology, the Health Research Council of New Zealand and the Maurice and Phyllis Paykel Trust. The authors gratefully acknowledge the families who participate in the study as well as other members of the research team. In addition we wish to express our thanks to the PIF Advisory Board for their guidance and support.
