Abstract
Historical and sociocultural factors have contributed to comparably poorer health and mental health for Indigenous Australians compared to non-Indigenous Australians. This situation is further complicated by differing definitions, manifestations, and conceptualizations of health and mental health among Indigenous Australians that are poorly understood by the wider community. As a result, health and mental health-care services for Indigenous people are often highly inappropriate and severely inadequate [1,2]. Although the inadequacy of mainstream service provision and assessment techniques for Indigenous Australians has been recognized for a number of years, little practical development has occurred [3].
This review will introduce the health and mental health status of Indigenous Australians while outlining some of the issues leading to inadequate mental health care for this population. ‘Indigenous Australians’ as used in this review refers to both Aboriginal and Torres Strait Islanders. The term ‘non-Indigenous Australians’ refers to members of the Australian population who are not Aboriginal or Torres Strait Islander and who typically align with the dominant Anglo-Saxon or Westernized culture of Australia. As used in this review, the term ‘mental health’ will refer to both psychological and cognitive functioning. ‘Psychological’ and ‘social and emotional well-being’ (SEWB) is used interchangeably and includes both psychiatric or psychological disorder and mental well-being. ‘Cognitive’ incorporates the range of brain or mental processes needed to conduct the activities of daily life. The review will also summarize the limitations of applying mainstream psychological and cognitive assessments to Indigenous Australians. Finally both the psychological and cognitive assessments that have been considered appropriate for use with Indigenous Australians will be reviewed and evaluated. This will lay a foundation for an appropriate evidence-based framework from which future developments can lead to improved mental health services for Indigenous Australians.
Health status of Indigenous Australians
Indigenous Australians' experience of poor mental and physical health has been well documented [1,2,4–7]. According to recent reports, the life expectancy of Indigenous Australians is reduced by around 17 years compared to non-Indigenous Australians and death rates are almost threefold higher [6]. Indigenous babies are twice as likely to be low birthweight (<2500g) and more likely to be hospitalized compared to non-Indigenous babies [6]. Low birthweight is associated with a greater risk of poor health, disability and death [6]. Indigenous Australians are also more likely to experience a chronic disease such as diabetes (threefold more likely), cardiovascular disease (1.3-fold more likely), respiratory disease (1.6-fold more likely to report asthma) or kidney disease (10-fold more likely) compared to non-Indigenous Australians (age-standardized) [4].
Physical ill health is strongly associated with mental ill health [1,8]. Cawte has described an ‘Aboriginal depression’ known as ‘ill-health depression’, which is depression arising from high levels of ill health and disease [9]. While comprehensive epidemio-logical data on mental illness in the Indigenous population are limited, recent reports suggest that 27% of Indigenous adults report high to very high levels of psychological distress; more than twice the rate for non-Indigenous Australians [4]. Indigenous Australians are hospitalized for self-harm at more than twice the rate of other Australians, and for Indigenous male patients it is almost threefold the national rate [8]. In a report on the burden of disease and injury for Indigenous Australians, mental health disorders were ranked second only to cardiovascular disease [10]. Anxiety and depression, alcohol dependence and harmful use, and schizophrenia contributed >75% to this total mental health burden [10]. Despite little investigation into cognitive problems in this population, rates are likely to be relatively high with widespread exposure to known risk factors including substance abuse, violence, head trauma, malnutrition, chronic illness and fetal alcohol syndrome [4,6,11,12]. The prevalence of dementia in Indigenous Australians aged >45 years from the Kimberley region has been reported at 12.4%; more than fivefold higher than the 2.4% reported among the same age group in the general Australian population [13].
Indigenous Australians and mental health
Sociocultural factors play an important role in the experience and expression of mental health and illness. Culturally, Indigenous Australians view life, including health, holistically, where well-being is understood in terms of the harmonized interrelations between spiritual, environmental, ideological, political, social, economic, mental and physical domains [1]. Such holistic notions of health have led to the recognition and establishment of a national Indigenous SEWB health framework [7,14]. For Indigenous Australians, a concept of self encompasses the individual, together with their family, the wider tribal group and the land, and involves a complex set of relational bonds and reciprocal obligations, loss or disintegration of which will lead to mental ill health [1,15]. Since colonization in Australia, these traditional connections have been severely disrupted by cultural genocide, dislocation, forced removal of children, destruction of culture as well as a devastating denial of basic human rights [2]. The consequence is an overwhelming sense of trauma, loss and grief for Indigenous Australians that is often not recognized or adequately addressed, and is perpetuated by their continued social, political and economic disadvantage [2].
Two dimensions of mental ill health have been described for Indigenous Australians. One is the ‘mental distress’ or ‘deep psychological malaise’ resulting from their collective experience as dispossessed and disadvantaged people [2,15]. The other incorporates the range of serious psychiatric or mental disorders that are also prevalent within the Indigenous population but which may manifest or be understood quite differently [2,15]. For Indigenous Australians, mind, body and spirit are inextricably linked and illness can be perceived as a normal reaction to spiritual forces or a curse [2]. Such concepts may be foreign to non-Indigenous people including health practitioners [16].
The differential meaning and experiences of mental health problems for Indigenous Australians compared to non-Indigenous Australians mean that distinct methods for their assessment and management are required. Despite the disproportionate levels of mental health problems in Indigenous populations, there remains a scarcity of culturally appropriate, objective and scientifically validated mental health assessment tools for use with Indigenous Australians [14]. Objective assessments enable valid measurement of psychological or cognitive changes and the detection of abnormalities with respect to healthy standards [17]. Without objective and scientific measures, clinical practice is dependent on the subjective skills and opinions of clinicians. The ability, however, of clinicians to accurately estimate mental functioning without the use of objective assessments can be poor [18]. Objective assessments can be used to detect abnormalities in settings in which psychological or cognitive impairments can affect an individual's ability to progress, learn, heal or rehabilitate such as in schools, employment, primary health care, prisons and drug rehabilitation programmes [17]. In these settings Indigenous Australians may be assessed by nonexperts, or non-Indigenous people who may have poor understanding of the unique psychological problems of Indigenous Australians. Consequently the nature and extent of mental health problems can remain unrecognized, undiagnosed and untreated [2]. Inability to appropriately measure psychological and cognitive function for Indigenous Australians is a fundamental hurdle that prevents any progress that may lead to the improvement of mental health services for this currently disadvantaged population. The development of appropriate assessment processes would allow valid routine screening and data collection to occur so that impairments can be recognized and quantified and appropriate treatment responses delivered promptly.
Limitations of traditional assessments in Indigenous populations
Cognitive and SEWB assessments can contribute to the misdiagnosis of impairment or mental illness if they are based on foreign concepts and/or symptomatology. Definitions of what constitutes normal (or abnormal) expressions of behaviour can vary considerably between cultures and even within cultures [19]. In non-Indigenous cultures it may be perfectly normal for a man to speak the name of a deceased relative or to talk to his mother in law, but in Indigenous Australian cultures such behaviours may be considered mad because they violate strict cultural rules and norms [11,20,21]. Psychiatric disorders may also be expressed through different symptomatology. For example, anger may represent a culturally specific symptom of depression for Indigenous Australians [22–24].
Context and experience dictates what is and what is not important or relevant for a particular culture and thus what abilities are valued and trained [19,25]. For non-Indigenous cultures, a small child might be considered intelligent if they can say a large number of words or count to 10, but an Indigenous child from a particular desert community might instead be expected to know directions, space and place or demonstrate independence to be considered intelligent [26,27]. Tests of verbal memory, such as list learning, may therefore be irrelevant to Indigenous people's lives and thus result in inferior performance when compared to non-Indigenous groups. However, on spatial memory tests or relevant verbal assessments that are based on skills nurtured by their specific culture, Indigenous people may demonstrate greater abilities than non-Indigenous people [28–32]. Despite these differences, psychological tests generally rely on questions and answers for which the standard response is obtained from the general population [2]. Test interpretation for Indigenous Australians may therefore be extremely problematic because current Indigenous norms are rarely available [33]. Traditional tests of mental functioning can rely heavily on the use of the English language, require written responses and resemble formal educational processes. Poor English literacy, a lack of formal education, as well as differing concepts of numbers, time and space can mean that Indigenous Australians may have limited experience with the knowledge base from which such tests are derived [11,27,34–38]. Administration of pencil-and-paper tests can be inappropriate for a culture that has no traditional written language and in which rates of English illiteracy can be high. Additionally, the common one-on-one approach used by many psychological tests can be both uncommon and objectionable to Indigenous Australians, who may reject direct approaches between strangers and can consider it rude to ask numerous questions [27,34]. Indigenous Australians might also find it inappropriate to talk to strangers about their innermost thoughts and feelings, which is a requirement of many mental health assessments [36]. An appropriate assessment must therefore meet two often conflicting prerequisites: it must be both scientifically and biomedically valid; and it must have relevance culturally for the target group.
Approaches for assessing mental health and cognition in Indigenous Australians
A literature search of key health science databases (including, but not limited to PsychINFO, PsychARTICLES, Medline, PubMed, Academic Search Premier (EBSCO), Science Direct, JSTOR, SpringerLink) was conducted using the following search terms in various combinations: Indigenous, Aboriginal, cognitive, assessment, mental health, social emotional well-being, psychological, Australian. Tests and techniques applied in assessing mental health for Indigenous Australians are summarized in Table 1 and discussed in the following sections.
Approaches to assessing cognitive function and mental health in Indigenous Australians
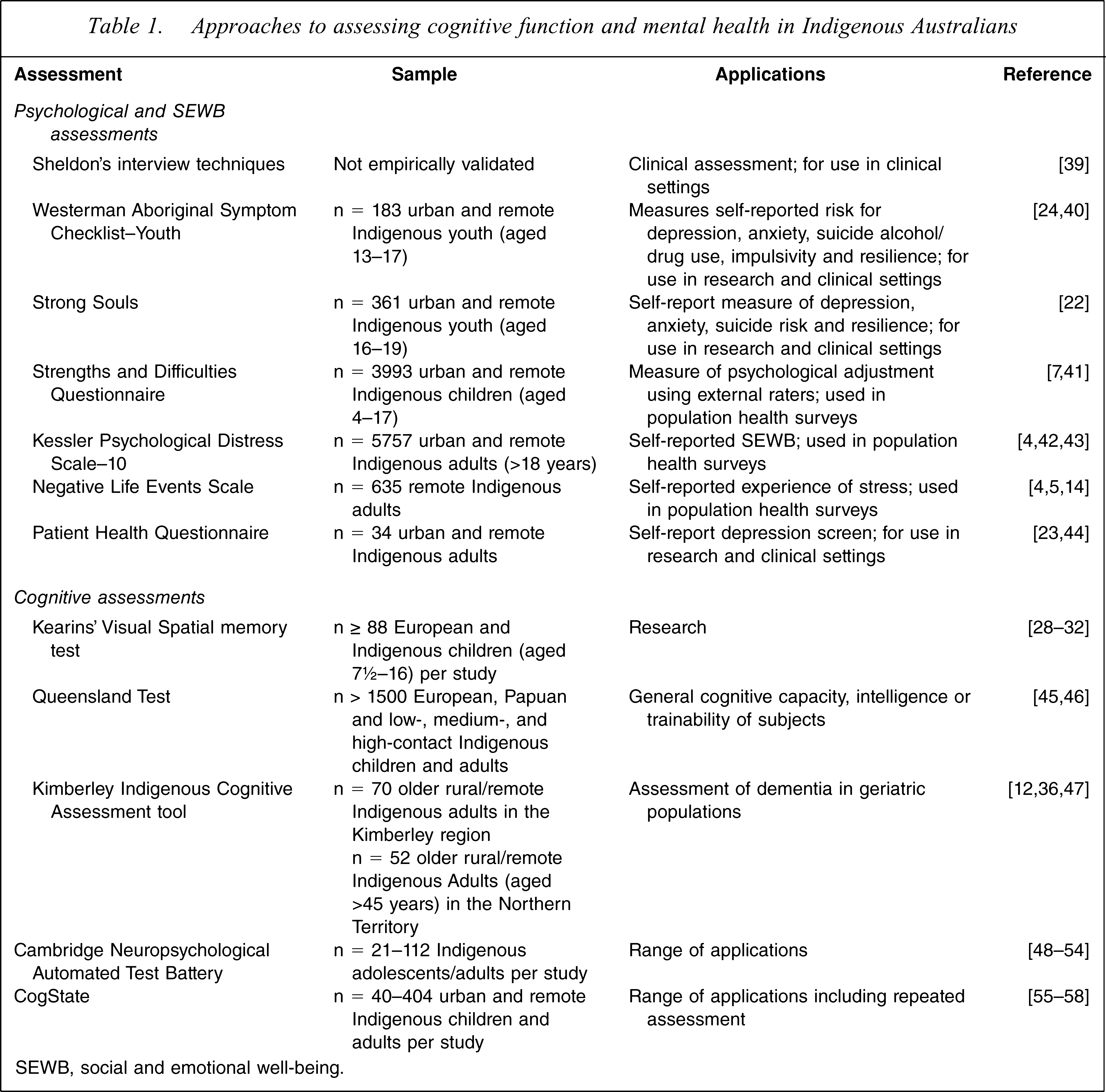
SEWB, social and emotional well-being.
Psychological and SEWB assessments
Clinical psychiatric assessment
While the clinical interview is currently considered the most appropriate way of assessing psychological problems among Indigenous Australians, it can be time-consuming and cultural and language factors may still hinder appropriate assessment [14]. Guidelines have been developed for the psychiatric assessment of Indigenous patients in remote settings [39]. These include a detailed description of how to act as a psychiatrist in remote communities, along with non-validated questions for assessing the mental health of Indigenous Australians [39]. Because the process of assessment can be as important as the content, these guidelines provide valuable guidance to assist mental health practitioners to adapt standard clinical interviews to assess Indigenous patients, including cultural protocols and communication strategies [39]. Although this approach is useful clinically, it does not represent a distinct tool that can be assessed for its validity and reliability and used to research or screen for psychological dysfunction in this population. This approach therefore requires further empirical evaluation to meet the requirements for evidence-based practice.
Youth psychological/SEWB assessments
A promising development has been the construction of an SEWB inventory that reflects Indigenous expressions of mental health problems [24,40]. The Westerman Aboriginal Symptom Checklist for Youth (WASC-Y) incorporates 53 self-report items measuring six constructs (depression, suicide, alcohol/drug use, impulsivity, anxiety, and cultural resilience) and includes a set of clinician guidelines for its application. The clinician guidelines include methods for culturally valid engagement of Indigenous youth, interpretation of youth symptoms within the culture, a model of cultural validation that assesses the role of culture in mental health symptoms and a model for the resolution of such culturally related mental health problems [40].
The reliability and validity of the WASC-Y were assessed in a sample of 183 Indigenous people aged 13–17 years from either the Perth metropolitan region or the northwest region of Western Australia including Port Hedland, Wickham, Karratha and Roebourne. Initial validation of the WASC-Y involved conducting separate exploratory factor analyses on each of the subscales individually rather than on all items collectively [24]. It is therefore unclear whether the items purporting to measure each of the constructs do actually cluster together. Nevertheless, each of the scales demonstrated good internal consistency (Cronbach a = 0.78, 0.88, 0.78, 0.67, 0.84, 0.75 for the Depression, Suicide, Alcohol/drug use, Impulsivity, Anxiety, and Cultural Resilience subscales, respectively). Further validation involved comparing the WASC-Y to clinical interview, resulting in kappas from 0.75 to 0.84, which represented good to excellent agreement between WASC-Y score and clinical interview for each of the scales [24]. Potential unintentional bias may have been introduced however, with the clinical interviews conducted by the main research who was not blind to outcomes generated by the WASC-Y. Further validation in a larger sample and in other regions of Australia is therefore warranted before its appropriateness for broader applications can be established [24,40]. Nevertheless, with its clinician guidelines, the WASC-Y provides a comprehensive assessment process for use with Indigenous Australians. The content is familiar and applicable to Indigenous expressions of psychological problems, and its adaptation for use with other Indigenous populations (e.g. Inuit people) has also been considered [59].
Strong Souls is a screening tool that was developed in the Northern Territory to assess SEWB in Indigenous youth enrolled since birth in an extensive life course study of chronic health outcomes (Aboriginal Birth Cohort; ABC study) [22,60]. Using plain English, Strong Souls consists of 25 items measuring four aspects of SEWB: anxiety, resilience, depression, and suicide risk. While Strong Souls measures similar constructs to the WASC-Y, it is shorter and has demonstrated better discriminative ability (with its four-item response scale) in combination with good face validity and strong reliability when pilot tested alongside WASC-Y and the abridged version of the Kessler Psychological Distress Scale (K6+) [22].
An initial validation study assessed the psychometric properties of Strong Souls in a sample of 361 Indigenous young people, aged 16–19 years, from >70 urban, rural and remote communities across the Northern Territory. The sample therefore represented significant cultural and linguistic diversity. Principal components and exploratory factor analyses were conducted using all items, and a four-factor solution was identified. This solution was consistent with the constructs of interest: anxiety (eigenvalue = 4.96; % variance = 17.5), resilience (eigenvalue = 2.67; % variance = 7.8), depression (eigenvalue = 1.96; % variance = 5.34) and suicide risk (eigenvalue = 1.49; % variance = 3.87). The tool demonstrated good internal consistency, with Cronbach alphas of 0.80, 0.71, 0.71 and 0.73 for the anxiety, resilience, depression and suicide risk subscales, respectively. Each of the subscales correlated with each other, demonstrating good convergent validity. Stable and consistent replication of identified factors was demonstrated when different extraction models were used in factor analyses. Construct validity was further demonstrated through the consistency of the derived factors with constructs identified as prevalent SEWB issues for Indigenous Australians [22].
The authors concluded that Strong Souls is valid, reliable, and appropriate for screening Indigenous young people in the Northern Territory, although replication of the findings in other regions and further clinical validation is warranted [22]. While the WASC-Y and Strong Souls may turn out to be important tools for cross-cultural evaluations of SEWB, both have been validated only for Indigenous youth. Other limitations include their design for pencil-and-paper administration and their high reliance on language. These limitations are, however, difficult to avoid in assessing mental and emotional status, and oral administration of both tools is possible.
National surveys have also recognized the relative lack of appropriate assessment tools for nationwide epidemiological data collection regarding the mental health of Indigenous Australians [4–7,14]. Some have therefore adapted mainstream tools for use with Indigenous populations. The Western Australian Aboriginal Child Health Survey (WAACHS) used an adapted version of the Strengths and Difficulties Questionnaire (SDQ) to assess the SEWB of 3993 Aboriginal Australian children aged 4–17 years, in addition to asking some other more general questions about the child's SEWB [7]. The SDQ uses external raters (parent, carer or teacher) to investigate whether the child has displayed any of 25 distinct behaviours indicative of five areas of psychological adjustment: emotional symptoms, conduct problems, hyperactivity, peer problems, and prosocial behaviour [41]. Pilot testing showed that modifications in both wording and the response scale were needed for it to be better understood by the Indigenous participants [41]. In clinical settings the SDQ can be used in conjunction with other techniques to identify and diagnose psychological problems because it specifies normal, borderline and abnormal ranges of scores. The WAACHS, however, did not involve comprehensive clinical assessments, so the SDQ was used to assess risk for clinically significant emotional or behavioural difficulties [41].
The adapted version of the SDQ was assessed for its validity and reliability. This process found that the reliability and consistency of the measure is of a high standard [61]. Four of the five subscales provided good reliabilities (reliability coefficients = 0.77–0.81) with the peer problems scale proving the least reliable (0.60). The overall scale reliability was exceptional (0.93) and the data showed adequate congruence with those reported by the creator of the scale. However, the internal reliability of the five subscales (and to a lesser degree the overall scale) declined slightly as level of relative isolation increased. This may reflect differences with interview procedures, because those living more remotely were more likely to require simultaneous translation to an Indigenous language during the interview. Alternatively, some concepts may have been less salient to remote cultural and living circumstances [61]. The adapted SDQ scale represents a promising measure for the assessment of mental health and well-being in Indigenous children and its use in future national surveys is advocated to enable appropriate comparisons between Indigenous and non-Indigenous data [62].
Adult psychological/SEWB assessments
Recognition of the lack of available data relating to adult mental health status for Indigenous Australians led to the addition of an SEWB module to the National Aboriginal and Torres Strait Islander Health Survey (NATSIHS; 2004-05) [4]. This module included five (slightly modified) questions from the Kessler Psychological Distress Scale (K-5) measuring non-specific psychological distress; along with additional questions relating to seven other domains: positive aspects of SEWB, the impact of psychological distress, feelings of anger, cultural identification, experience of discrimination, experience of life stressors, and removal from natural family [4].
The Australian Institute of Health and Welfare (AIHW) assessed the psychometric properties of the module to determine its suitability for understanding SEWB in Indigenous Australians. A workshop and report were provided to representatives from the National Advisory Group on Aboriginal and Torres Strait Islander Health Information and Data, the Office of Aboriginal and Torres Strait Islander Health, the Australian Bureau of Statistics and the National Aboriginal Community Controlled Health Organization [8,63]. They concluded that the module performed well and all eight domains (psychological distress (K-5), impact of psychological distress, positive well-being, anger, life stressors, discrimination, cultural identification, and removal from family) should be retained in future national surveys with some modification to five of the domains. The eight domains were well accepted, the data fitted with information gained from other data sets and each corresponded with the other SEWB domains and other measures of health as expected [8,63]. While the ‘don't know/not stated’ responses were at an acceptable level, most responses of ‘don't know/not stated’ were reportedly due to language and conceptual issues [63]. In addition, stakeholder consultation identified important SEWB factors such as resilience and self-efficacy that were not captured by the module. It was therefore recommended that the feasibility of including them in future surveys should be explored. Although not yet completely comprehensive, the utility of this module for epidemiological data collection and cross-cultural comparisons shows good potential.
Questions relating to the experience of life stressors that were used in the NATSIHS, were also used previously in the National Aboriginal and Torres Strait Islander Social Survey 2002. Recognising the potential value of the tool, and the apparent lack of published data (at the time), another study set out to evaluate what was termed the Negative Life Events Scale (NLES). The sample included 635 Indigenous householders and carers of young children from 11 remote communities across the Northern Territory [14]. The study's larger aim was to assess the impact of improved housing on the health of young children. Participants were required to indicate whether any of a list of negative life events had been a problem for them or their family or friends in the last 12 months [64]. Modifications to the scale were made based on the AIHW workshop recommendations and in consideration of the overall aims of the project. The word ‘problem’ was changed to ‘worry’ to reflect the Aboriginal English in use in the Northern Territory, and the phrase ‘you or anyone else living in this house’ was used instead of ‘you or your family or friends'. An item asking about vandalism or malicious damage was also added.
The results indicated that all except three items were appropriate for use in a wide range of Indigenous communities. These three items (‘divorce or separation’, ‘not able to get a job’ and ‘lost job’) were poorly endorsed, and showed poor discriminative ability and poor external reliability. This suggested that these items were not widely experienced by the sample and those who did endorse them were not among the most stressed respondents. Therefore, these items may not be measuring what they were intended to measure, or are not doing so in a reliable way [14]. Although the NLES was found appropriate for use in Indigenous populations, the effectiveness of the scale in comprehensively capturing Indigenous experiences of stress remains to be determined. Recommendations from the AIHW included broadening the range of stressors that are captured by the scale [8,63].
With a more clinical focus, Esler et al. have begun to assess the acceptability and validity of a tool for diagnosing depression: the Patient Health Questionnaire 9 (PHQ-9), for use with Indigenous Australian adults [23,44]. The unmodified PHQ-9 was considered unacceptable for use with Indigenous Australians due to its wording and rating scale. After consultation with Indigenous community members and health workers along with other health and mental health centre staff, a number of changes in wording and the addition of a question on the experience of anger were recommended, resulting in a 10-item scale. The consultation process led to recommendations that the screen be administered by an Aboriginal health worker and that family could be included in the assessment process. The adapted version of the tool was considered acceptable for use in the Darwin-based community-controlled Aboriginal health clinic where the study was conducted. Its appropriate use, however, was not generalizable for use in other situations without further evaluation.
A further validation study involved an Indigenous health worker administering the PHQ-9 to a sample of 34 Indigenous adults (mean age = 57.7 years) with ischaemic heart disease. They also underwent a semi-structured diagnostic clinical interview with a general practitioner to determine whether a diagnosis of minor or major depression was appropriate. Although the internal consistency of the tool was good (Cronbach a = 0.80) and the tool showed good concordance (73.6%) with the results of the diagnostic psychiatric interview, the results of the study may not be generalizable to the wider Indigenous population. As with many of these mental health tools, further validation in a larger sample of the general Indigenous population is therefore required.
Cognitive assessments
Identifying validated cognitive assessments appropriate for Indigenous Australians can prove equally as challenging. Cognitive assessment involves the measurement of specific behaviours as accepted surrogate markers of brain function [65]. Changes or abnormalities in brain function detected on cognitive assessments are typically interpreted with respect to healthy standards. For Indigenous populations, however, appropriate normative data are rarely available [33]. In research studies, cognitive assessment is used to improve knowledge about the factors that alter normal brain function and the nature of related changes. Such studies generally involve case–control study designs.
Research task
Following years of poor performance by Indigenous people on traditional forms of cognitive testing, in 1976 Kearins developed a memory task designed to reflect skills and strategies thought to be important for survival in the harsh desert environment of Central Australia [31]. Her research demonstrated that by providing tasks appropriate to Indigenous contexts, Indigenous children could perform the task at a level superior to their non-Indigenous counterparts. Other researchers, however, failed to replicate her results in different Indigenous groups [66–68]. Nevertheless, the performance of at least one other Indigenous sample, although not significantly superior, did equal the performance of non-Indigenous participants [67]. Although somewhat encouraging as an appropriate task for testing Indigenous memory ability, the task assesses merely one aspect of cognition and has never been transferred to a standardized assessment procedure with appropriate normative data. Its utility for clinical evaluations is therefore limited. Nevertheless, Kearins' research demonstrated the importance of designing and using ecologically valid tests for Indigenous Australians. This work was therefore pivotal in recognizing that poor performance by Indigenous Australians on tests that were designed for non-Indigenous populations may reflect the inadequacies of the assessment tools themselves for use in this population, rather than indicating organic brain dysfunctions. It also highlights the difficulties in comparing test scores between cultures on any assessment for which the design is based primarily on the cultural characteristics of one of the groups. Appropriate assessment of any cultural group must therefore involve the use of culturally fair assessment tools for which performance scores are interpreted with respect to normative data established from the same group.
Intelligence test
The Queensland Test was developed in the 1960s to assess general intelligence in Indigenous Australians, using five subtests [45,46]. These subtests are adapted versions of the Knox Cube Imitation Test, the Beads Test, Alexander's Passalong Test, the Form Assembly Test and the Pattern Matching Test [46]. Administered using pantomime alone, the test requires the solution of clear and unambiguous overt tasks using concrete, tangible materials [46]. Although the tasks incorporated in the Queensland test have been modified for use with Indigenous Australians, they are ‘still essentially Western in both origin and content' (p. 370) [69]. The extent of contact with mainstream non-Indigenous culture was found to impact on performance and this led to the establishment of three sets of norms for low, medium or high degrees of contact with mainstream non-Indigenous culture. Although originally designed as an intelligence test, the Queensland Test was later described as more useful for assessing the health or organic brain dysfunction of individuals within the culture [70]. Norms for the Queensland test are currently outdated [38] and no recent studies using this tool have been reported in the literature.
Dementia screen
A recent advance for assessing cognition in Indigenous Australians was the development of a dementia screen for older Indigenous people from the Kimberley region: The Kimberley Indigenous Cognitive Assessment (KICA) [36,47]. This screening tool assesses cognitive capacities associated with dementia including orientation, naming, registration, verbal comprehension, verbal fluency, free and cued recall, praxis and frontal executive function [47]. Although initially designed and validated for use with Indigenous people in the Kimberley region of Western Australia (n = 77), it has recently been validated among Indigenous populations in the Northern Territory (n = 52) [12,36,47]. These studies demonstrated that the KICA displays good internal consistency (Cronbach's α = 0.8–0.9), good sensitivity (≥82.3%) and good specificity (≥87.5%) for a cut-off score of 31–32/39 [12,36]. Limitations of the KICA include its question-and-answer format, with some questions requiring a pencil-and-paper response. Although cognitive screen data are supplemented by self and family reports regarding everyday behaviours and medical histories, making the KICA a comprehensive tool, these sections are also highly language based.
In addition, the test is designed to detect gross brain dysfunction at a single point in time and may have poor reliability for detecting the mild cognitive decline that may precede dementia. This is also a limitation of traditional pencil-and-paper neuropsychological tests used commonly in non-Indigenous populations, such as the Mini-Mental State Examination (MMSE). In the non-Indigenous population, more sensitive tests such as computerized cognitive screens are now used in at-risk patients to monitor cognitive change over time and detect mild cognitive decline early [71–73]. The KICA therefore shows promise in the same realm as the MMSE, to assess the overall severity of dementia, but it may have limited utility for monitoring change over time. The functions tested by the KICA specifically target those affected in patients with dementia, so tasks measuring attention, long-term memory, and visuospatial abilities that are likely to be affected by other causes of brain dysfunction have been excluded due to their inappropriateness during pilot testing [47]. These factors may be more suitably assessed using other styles of cognitive assessment.
Computerized cognitive assessments
The Cambridge Neuropsychological Test Automated Battery (CANTAB) is a computerized assessment tool utilizing non-verbal stimuli and requiring non-verbal responses on a touchscreen computer [73]. CANTAB has proven effective for cross-cultural assessments and for individuals with English as a second language [73,74]. The test has also been used successfully in a number of studies with Indigenous Australians [48–54]. In this population, these studies have demonstrated associations between specific aspects of cognitive performance and neurological disorders including Sydenham chorea [75] and Machado Joseph disorder [53], as well as substance abuse including petrol sniffing [48,50,52] and kava abuse [51,54]. These studies have used case–control designs. Therefore, the specific psychometric properties of the test for Indigenous Australians have not been documented. Advantages of computerized tests, however, can include standardized and quick administration, multiple alternate forms, automation of response recording, randomized presentation of stimuli, superior test–retest reliability, a lack of floor and ceiling effects, and the ability to assess a range of functions and record many responses in a short period [73,76–78]. Nevertheless CANTAB has limited utility for more widespread use in remote regions because it requires specialized technical equipment that can be expensive, cumbersome, and difficult to operate [65].
Cogstate (cogstate.com) is a more recently developed computerized, non-verbal assessment that can be downloaded from the Internet and administered on any computer, making it accessible and portable for a range of applications. Intended for the repeated assessment of cognitive function in diverse groups, Cogstate removes the chance aspect of card playing and modifies the rules of such games to generate valid tests of psychomotor function, attention, learning, memory and executive function [65]. Like many cultural groups internationally, Indigenous Australians in urban and remote regions have demonstrated enjoyment, familiarity and proficiency in the practice of card playing [65,79]. Recognizing the universality of playing cards, Cogstate was developed as a response to the need for appropriate cognitive assessments for Indigenous Australians. The test was initially applied more widely, and its scientific validity and clinical applications have been established in a number of non-Indigenous populations including children and adults, patients with Alzheimer's disease, attention-deficit–hyperactivity disorder, and sports-related head injury as well as in non-English-speaking populations [71,80–86].
Cogstate has also been used successfully with Indigenous Australians in research studies showing substance abuse-related cognitive impairments, and its psychometric properties in this population are in the process of being reported [55–58]. Using Cogstate, one study describes the performance of 237 healthy Indigenous adolescents living in remote regions and representing a diversity of cultural and language groups [55]. These results suggest that the tasks were performed appropriately, with response times and error rates increasing in association with task difficulty. For tasks that were presented over five rounds, participants' response duration and error rates decreased with each round, meeting task expectations and corresponding with performance patterns in non-Indigenous groups. The test–retest reliability of Cogstate has also been assessed in a sample of 40 Indigenous adolescents over repeated assessments [57]. The results of these analyses indicated no practice effects and good retest reliabilities (r = 0.29–0.82) for the simple card-based tests of psychomotor function, visual attention and working memory. Accuracy (but not speed measures) on the more complex learning and memory tasks also exhibited satisfactory reliabilities (r = 0.23–0.73) and no practice effects. Speeded measures exhibited some practice effects that may be ameliorated with the use of a dual baseline or practice test prior to the first assessment. These characteristics together with its sensitivity in detecting mild cognitive impairment make Cogstate a valuable tool for detecting cognitive decline or recovery of function with repeated assessments [72,57]. Other analyses have demonstrated the test's sensitivity to substance abuse-related impairments and have also indicated minimal impact of demographic factors such as gender and education on performance [55,56,58]. Age effects have been observed, however, in line with cognitive changes in other populations [55,58]. Thus the clinical utility of this (and other) tools is limited until appropriate normative data are established that accommodate factors (such as age) that are known to impact upon performance.
Conclusion
The assessments reviewed here are few and largely represent initial validations, indicating that this is indeed a novel and emerging field of research and clinical practice. Given the considerably high rates of poor health and particularly mental health experienced among Indigenous Australians, however, these studies are very important and further development in this field is a necessity to improve mental health outcomes for Indigenous Australians. Many of these assessments require further evaluation so it is clear that considerable development is required before a national protocol for assessing or screening for cognitive or mental health problems in Indigenous Australians is established. Until appropriate assessment tools and investigation methods are developed and utilized, the prevention, recognition and treatment of mental health problems for Indigenous Australians will remain severely inadequate.
Footnotes
Acknowledgements
