Abstract
Mental health problems are in the top 10 of all health conditions incurring health-related costs to employers [1–3]. The estimated 1 month prevalence of any mental disorder in Australian employees is 10.5% [4]. The symptoms of mental disorders such as fatigue, impaired attention, decreased concentration and poor memory affect the performance of employees [5,6]. Numerous reports consistently show that mental disorders lead to a reduction in employee productivity in terms of absenteeism and presenteeism (attending work while ill but not functioning at full capacity) [7–10]. Estimates indicate that mental disorders cost business and the economy m$ US51 billion in the USA (data collected in 2000) [11], $ CA2.16 billion in Canada (data collected 1996–1997) [12], and $ AU2.7 billion in Australia (data collected in 1997) [4].
Treatment of mental disorders (primarily using studies of depression) is accompanied by increased employee productivity [13–18]. Indications are, however, that employees who receive treatment for a mental disorder do not return to work productivity levels equivalent to that of employees without a mental disorder [19,20]. It is clear that treatment status and mental health symptoms interact with regards to employee productivity. Consequently, the effect of the interaction between treatment status and mental health symptoms on employee productivity requires further investigation. The authors are aware of only one large-scale national study that examined mental disorders and treatment-seeking interaction to quantify work loss days and work cutback days [4]. These surrogates of productivity are not monetized to provide an overall productivity estimate for Australia. The aim of the present study was to estimate employee work productivity by mental health symptoms while considering different treatment-seeking behaviours.
It has been shown that mental health symptom severity is related to functional disability, absenteeism, presenteeism and economic cost [6,21–25]. The Kessler 6 (K6) is a brief six-item questionnaire that assesses the level of psychological distress. The K6 was applied as a measure of symptoms in the present study. Previous work using the K6 indicated that high levels of psychological distress are associated with an estimated $ AU2.7 billion loss in productivity in Australia [24]. It has also been noted that presenteeism values estimated from K6 scores mirror those of results obtained by interviewer-administered surveys assessing mental disorders and work productivity [24]. Many prior studies, with some known exceptions [4,26–28], on the effect of mental health on productivity are limited by their methods of including only non-co-morbid psychiatric conditions (a problem identified by Kessler et al. [29]) or only specific comorbidities (e.g. depression and bipolar disorders) rather than all disorders. The K6 as a symptom measure overcomes this limitation by selecting cases by symptom severity and will therefore likely include psychiatric comorbid cases and more accurately reflect population characteristics. An additional limitation of most prior studies is that they include only employees who meet strict diagnostic criteria for a mental disorder. It is likely that employees with subclinical symptoms also contribute to productivity losses. Using the K6, individuals with symptoms, but who do not reach the diagnostic threshold, will be captured.
Methods
Sample
Employees of large Australian employers were presented with the World Health Organization Health and Work Performance Questionnaire (HPQ) as a component of a larger study, the Work Outcomes Research Cost-benefit (WORC) Project. Detailed information on the WORC project methodology is located at www.qcmhr.uq.edu.au/worc/methodology.htm. The University of Queensland Human Research Ethics Committee approved the study protocol.
Survey distribution
Detailed descriptions of the recruitment of employers and employees in the study have been previously published [30,31]. In brief, 58 large Australian companies agreed to participate in the study. HPQ surveys were circulated to employees of the participating organizations using either paper-based (n = 23 775 respondents) or Web-based (n = 36 781 respondents) methods depending on company-specific logistical considerations. Surveys were received between October 2004 and December 2005. Only employees over the age of 18 years were invited to participate.
Measures
The HPQ was designed to evaluate employee productivity for chronic and acute physical and mental disorders [1,32,33]. Further information on the HPQ is located at www.hcp.med.harvard.edu/hpq/.
Mental health
Embedded in the HPQ is the K6, a six-item scale of psychological distress that has excellent internal consistency, reliability and strongly discriminates between community mental health cases and non-cases [34–37]. In the present study we used published methods, in which a K6 score of 0–7 reflects low psychological distress, a score of 8–12 indicates moderate psychological distress and a score of 13–24 represents high psychological distress [35,36].
In addition to the K6, the HPQ contains questions relating to three types of mental disorders (depression, anxiety and other emotional problems). For each respondents are asked, ‘Do you have [CONDITION]?’ Response options are (i) no, I don't have this condition; (ii) yes, but I never received professional treatment; (iii) yes, I previously received (but I don't currently receive) professional treatment; or (iv) yes, and I currently receive professional treatment.
If a respondent answered option (iv) to any of the three mental disorder questions, they were classified as being ‘Yes, in current treatment’. If the response to all four mental health questions was option (i) the record was classified as ‘Don't have any conditions’. If the respondent did not fall into either of the two previous treatment categories, and answered option (iii), they were classified as ‘Yes, previously treated’. Those not categorized in the three previous treatment categories, and answering option (ii) were scored as ‘Yes, but never sought treatment’.
The 12 combinations of K6 severity category and treatment-seeking behaviours form the basis of productivity computations.
Employee productivity
The primary outcome measure is employee productivity, being a combination of absenteeism and presenteeism. To quantify absenteeism the HPQ probes employees about the hours they actually worked in the past 7 days and how many hours their employer expects them to work in a typical 7 day period. Similar to previously reported absenteeism ratio methods [24,38], absenteeism is calculated as the number of expected hours minus number of actual hours divided by the number of expected hours and represented as a percent.
To compute presenteeism the respondents were asked to rate the performance of an average person (Paverage ), working in a similar job to their own on a self-anchoring scale of performance of 0–10 (worst to best). Respondents also ranked their own performance (0–10 scale) over the past 28 days during the time they were at work (Pown ). The formula used to calculate presenteeism is
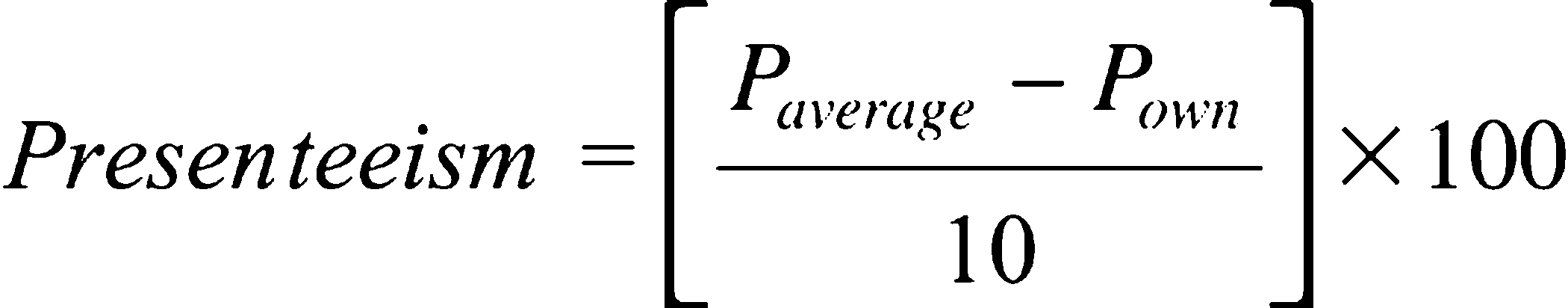
This presenteeism methodology is in line with previously published methods [18,24].
The total productivity (Tp) was calculated by the product of absenteeism with presenteeism using the formula:
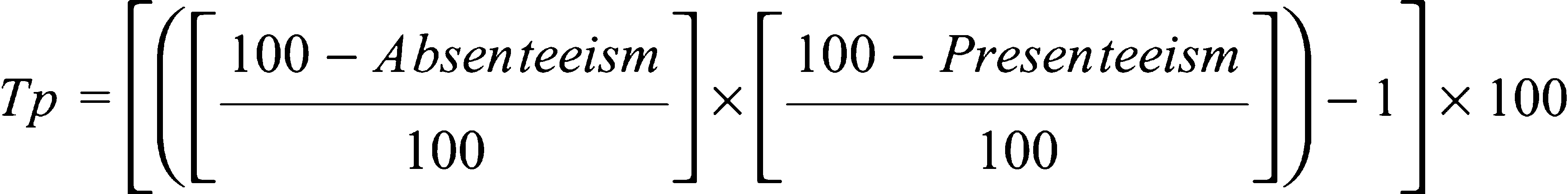
Positive productivity percentages indicate an increase in productivity; negative percentages represent decreased productivity.
Demographics
Demographic variables recorded by the HPQ included as covariates for subsequent ANOVA comparisons are gender, age (18–24, 25–34, 35–44, 45–54, 66–64, ≥65), marital status (married or cohabiting, separated, divorced, widowed and never married), number of children (0, 1, 2, 3, 4 or more) and education level (<year 10, year 10, year 12, some tertiary education, degree graduate, postgraduate degree). To control for physical comorbidity effects in the models, the total number of physical health conditions were coded into categories of 0, 1, 2, 3, 4, 5, ≥6, out of a possible 24 chronic physical conditions listed in the HPQ. Scoring comorbidities as the number of physical health comorbidities is a reasonable approach and has been used by previous researchers [6,16,24,33,39].
Statistics
Statistical significance of cross-tabulations was tested using the Pearson χ2 statistic. Mean productivity for the K6 was calculated for men and women separately using a univariate analysis of variance (ANOVA) with the dependent variable being percent productivity, the fixed factor being K6 category, and covariates being categorized age, marital status, education level attained, employee type and number of physical health conditions. Mean productivity for K6 by treatment-seeking behaviour was again estimated for men and women separately using an ANOVA model, with dependent variable being percent productivity, fixed factors being the K6 category and treatment-seeking behaviour, and the interaction of the two and the same covariates as listed for the first ANOVA.
Results
In total, there were 60 556 full-time respondents (25% response rate) to the HPQ. A total of 59 981 subjects had complete K6 and treatment-seeking behaviour responses. The demographic profile of respondents is described in Table 1. The prevalence of low, moderate and high psychological distress by gender is listed in Table 2. What can be noted about psychological distress is that between the sexes there is little meaningful difference in average K6 scores or prevalence of high psychological distress. In January 2009 the number of Australian full-time employees was estimated as 7.65 million (5.0 million men and 2.65 million women) [40]. Table 2 lists the number of employees by gender that occupies each K6 prevalence cell. Table 3 lists the mean productivity of each K6 category by sex while accounting for demographic variables. The productivity of high, moderate and low K6 were similar for men and women. Employees in the high psychological distress category had significantly lower productivity than both moderate and low psychological distress for men and women (p < 0.01 for all comparisons). Women had a low–high psychological distress productivity difference of 4.6% while men had a 10.9% difference. Thus it appears that high K6 affects male productivity more than it affects female productivity. The Australian Bureau of Statistics reported an average annualized salary of $ AU63 986 for full-time Australian employees (February 2009 data) [41], which approximates the average salary of $ AU65 201 recorded in the data presented. Men received a higher annual salary than women ($ AU69 061 and $ AU55 318, respectively). The approximate cost of high psychological distress in Australia for men and women is computed by multiplication of the productivity difference between low and high psychological distress by the number of employees with high psychological distress, by mean salary for each sex. This computation yields an overall cost of high psychological distress of $ AU1.93 billion, with $ AU1.62 billion attributable to men and $ AU0.31 billion for women. A similar calculation for moderate psychological distress yields a productivity loss of $ AU0.82 billion for men and $ AU0.06 billion for women (total of $ AU0.88 billion). Thus combined, moderate and high psychological distress results in a $ AU2.81 billion loss in employee productivity when treatment-seeking behaviour is not factored into the estimation.
Subject characteristics
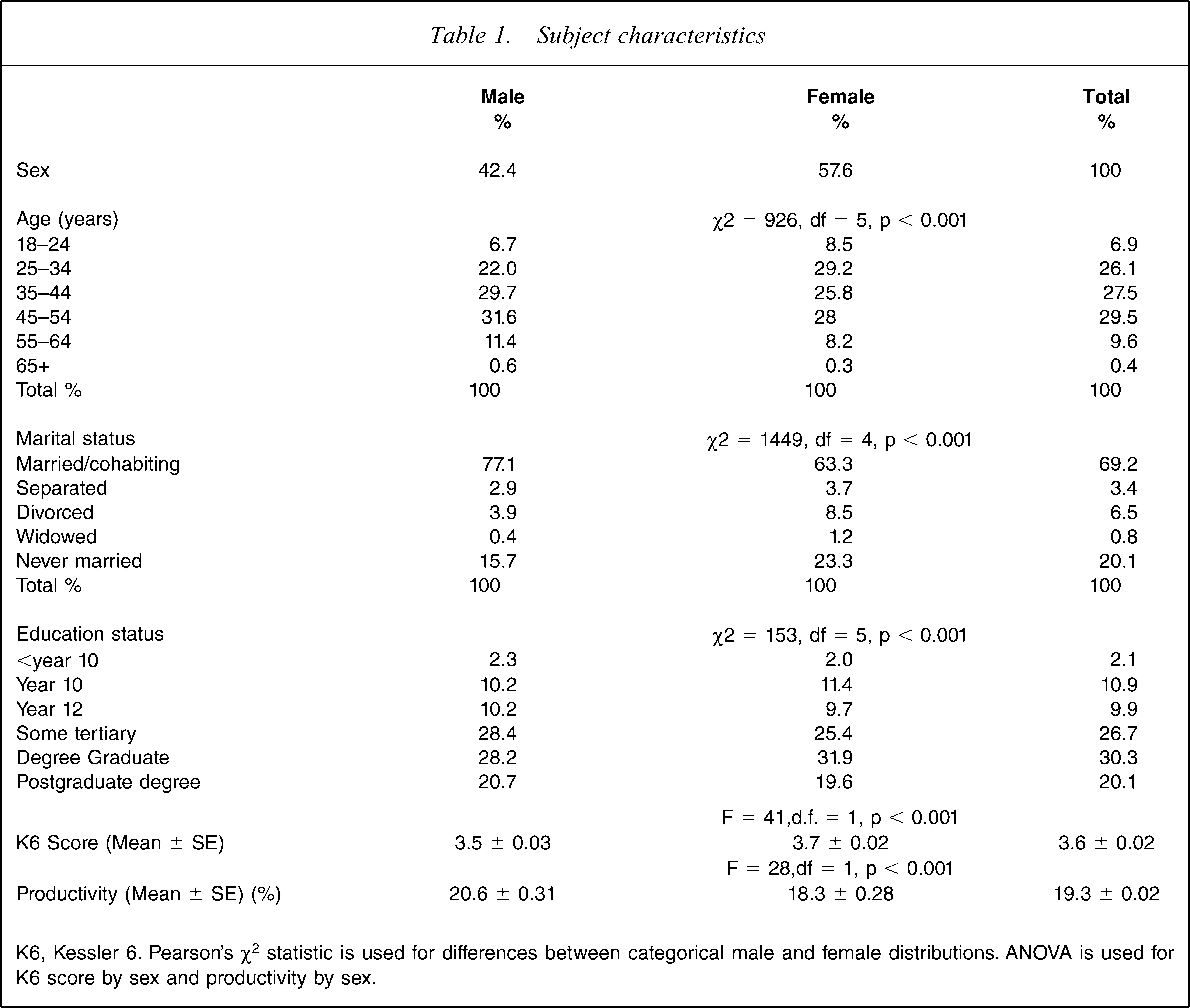
K6, Kessler 6. Pearson's χ2 statistic is used for differences between categorical male and female distributions. ANOVA is used for K6 score by sex and productivity by sex.
Prevalence of psychological distress (K6) vs gender
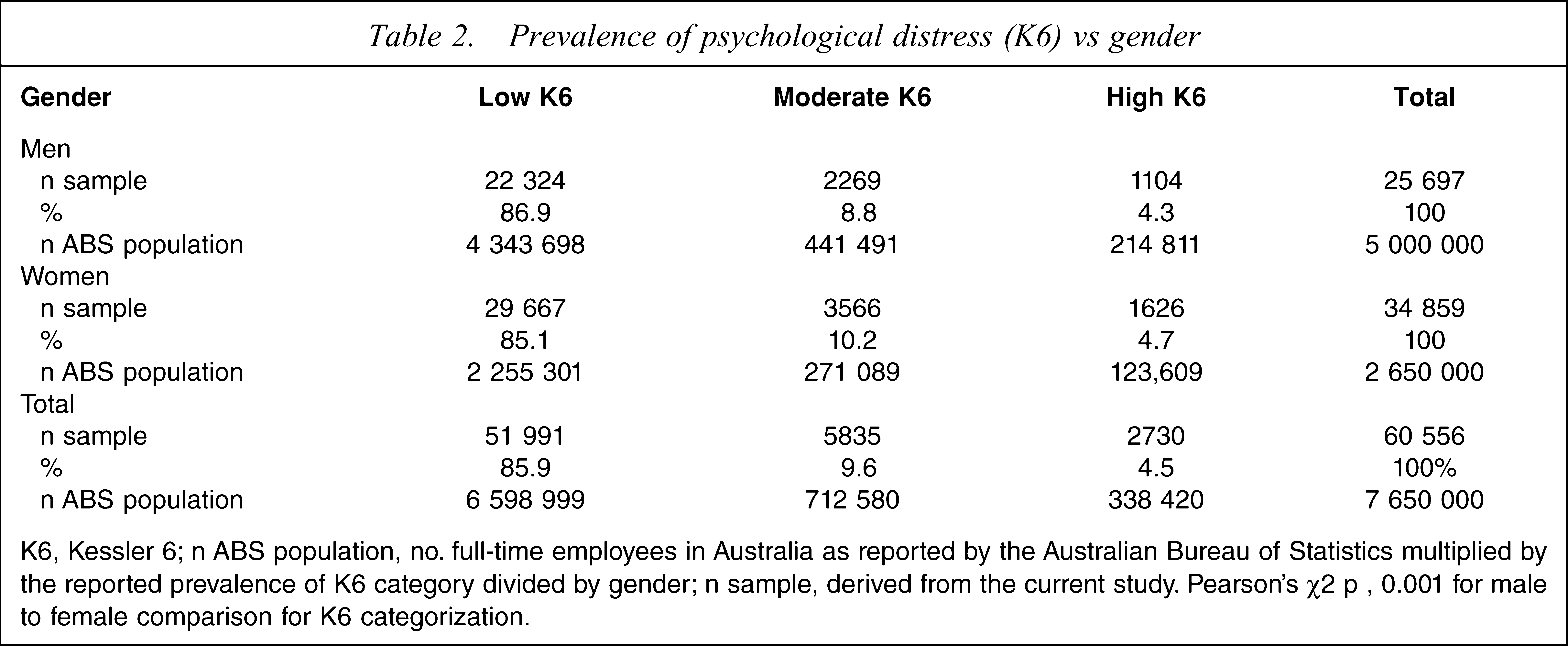
K6, Kessler 6; n ABS population, no. full-time employees in Australia as reported by the Australian Bureau of Statistics multiplied by the reported prevalence of K6 category divided by gender; n sample, derived from the current study. Pearson's χ2 p, 0.001 for male to female comparison for K6 categorization.
Productivity output of employees vs K6 diagnostic category and gender
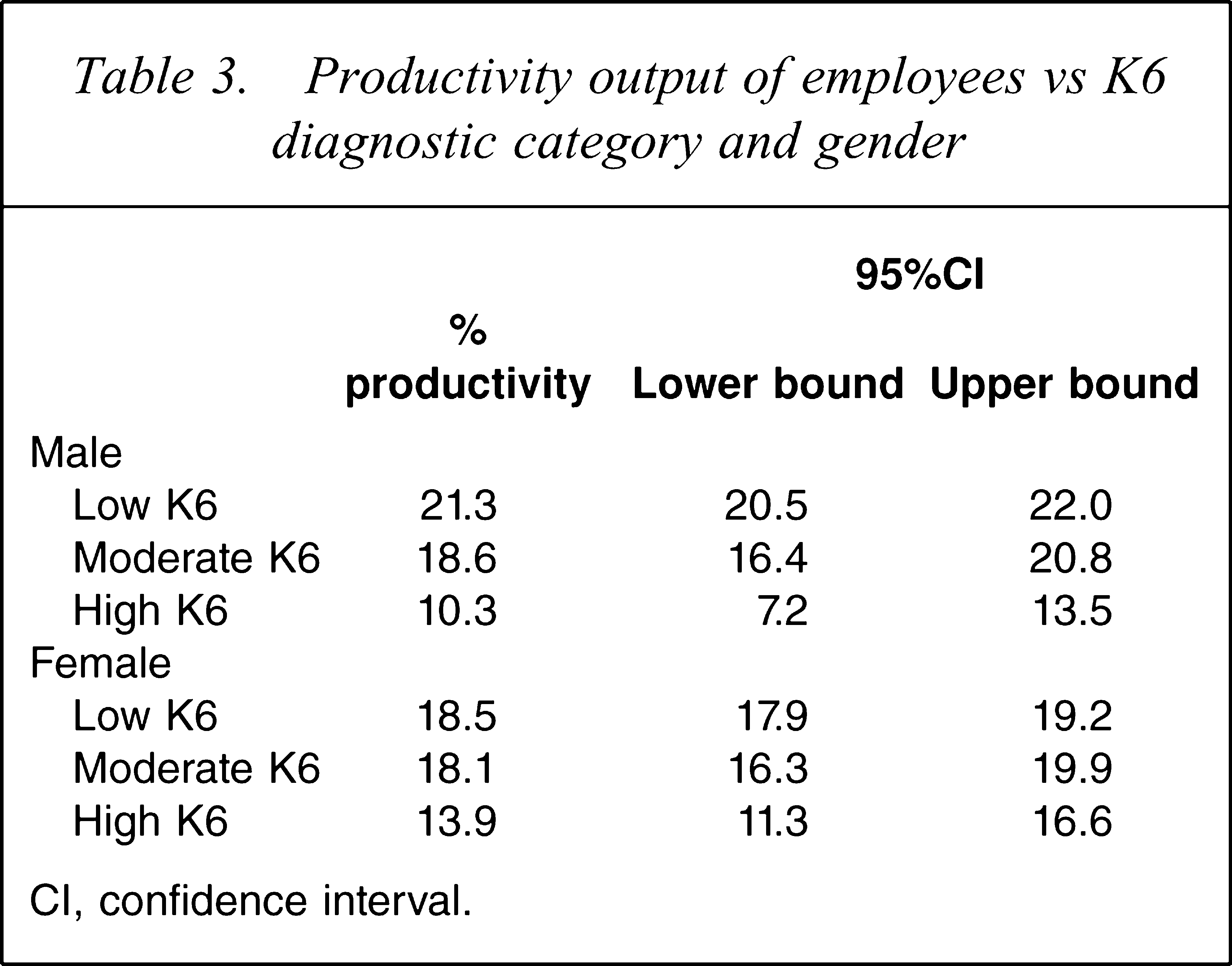
CI, confidence interval.
The percent of Australian employees in each treatment-seeking category versus K6 category versus gender are listed in Table 4. The percentages are multiplied by the estimated number of Australian employees [40], yielding the number of employees in each cell of the cross-tabulation.
Percentage of total of respondents in each K6 vs treatment vs sex
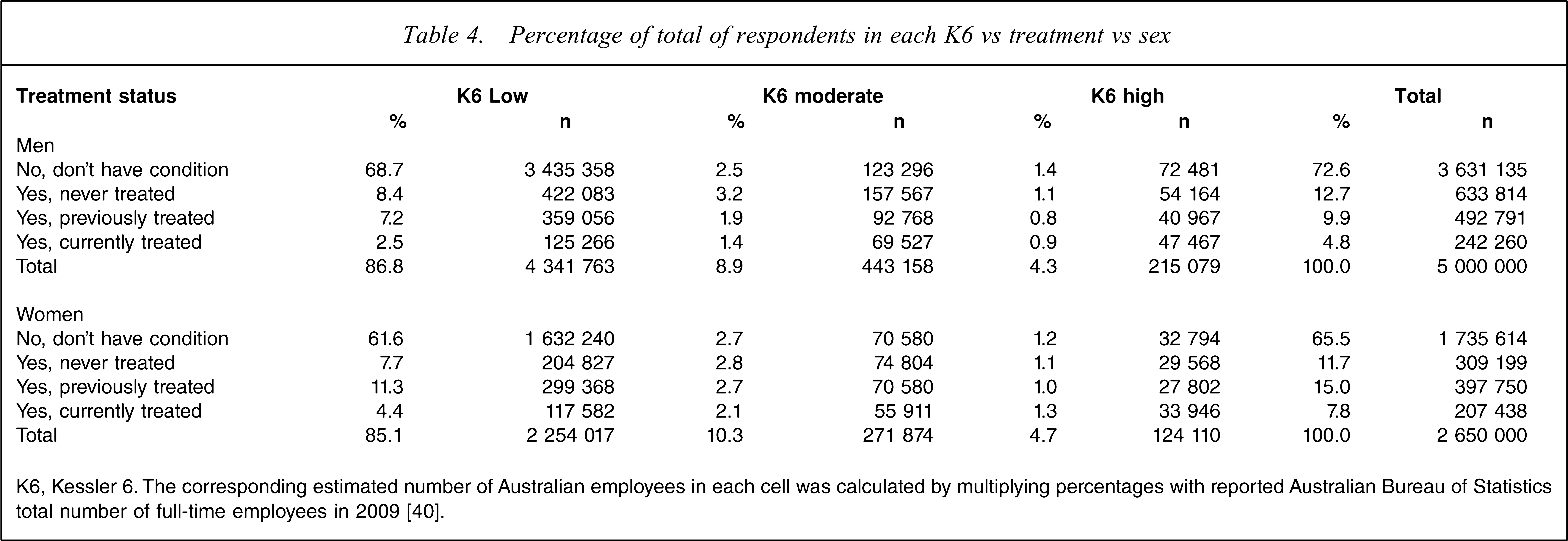
K6, Kessler 6. The corresponding estimated number of Australian employees in each cell was calculated by multiplying percentages with reported Australian Bureau of Statistics total number of full-time employees in 2009 [40].
Table 5 presents the productivity results of the ANOVA for the interaction of treatment-seeking behaviour with K6 for men and women. Employees without symptoms (low K6) who reported ‘No, I don't have condition’ are assumed to be the productivity reference group of employees with no current or past indications of a mental disorder. The employee productivity percent of all other combinations of treatment seeking and K6 category was subtracted from the reference category yielding mean productivity alterations. In Table 5 employee productivity differences are multiplied by average salary for men and women to yield a mean monetized productivity change for an individual employee in each category. Looking down the columns in Table 5 it is evident that in all three K6 categories those who rated themselves as in current treatment had the largest productivity decrements as compared to other treatment categories. With the exception of the ‘No, don't have condition’ treatment category, looking across the rows it is clear the increasing K6 is associated with decreasing productivity. By far the largest loss in productivity (28.7% for men and 16.6% for women) is the group of employees with high K6 and in current treatment.
Percentage change in employee productivity with low K6

K6, Kessler 6. Reference cell, ‘No, I don't have condition’. The percent productivity change is monetized by multiplication with the average 2008 salaries for men and women [41]. Thus productivity changes are the average for each employee occupying one of the cross-tabulated cells. Negative values are productivity losses, positive values are productivity gain. The actual productivity of the reference cell is 21.3% for men and 18.5% for women. Using these values the actual productivity of all other cells can be calculated.
Multiplication of the monetized productivity losses in Table 5 with the prevalence values for each cell in Table 4 yield the total monetized productivity losses per annum for Australian employers by sex (Table 6). In total, when treatment-seeking behaviour is taken into account, productivity losses to employers are estimated at $ AU5.9 billion. This figure is approximately double the $ AU2.8 billion productivity loss when K6 is evaluated without considering treatment-seeking behaviours. Of note is that the productivity loss, due to psychological distress when treatment-seeking behaviours are accounted for, is 2.6-fold higher in men than in women.
Total 12 month monetized employer productivity losses due to employee psychological distress (K6) and treatment-seeking behaviours
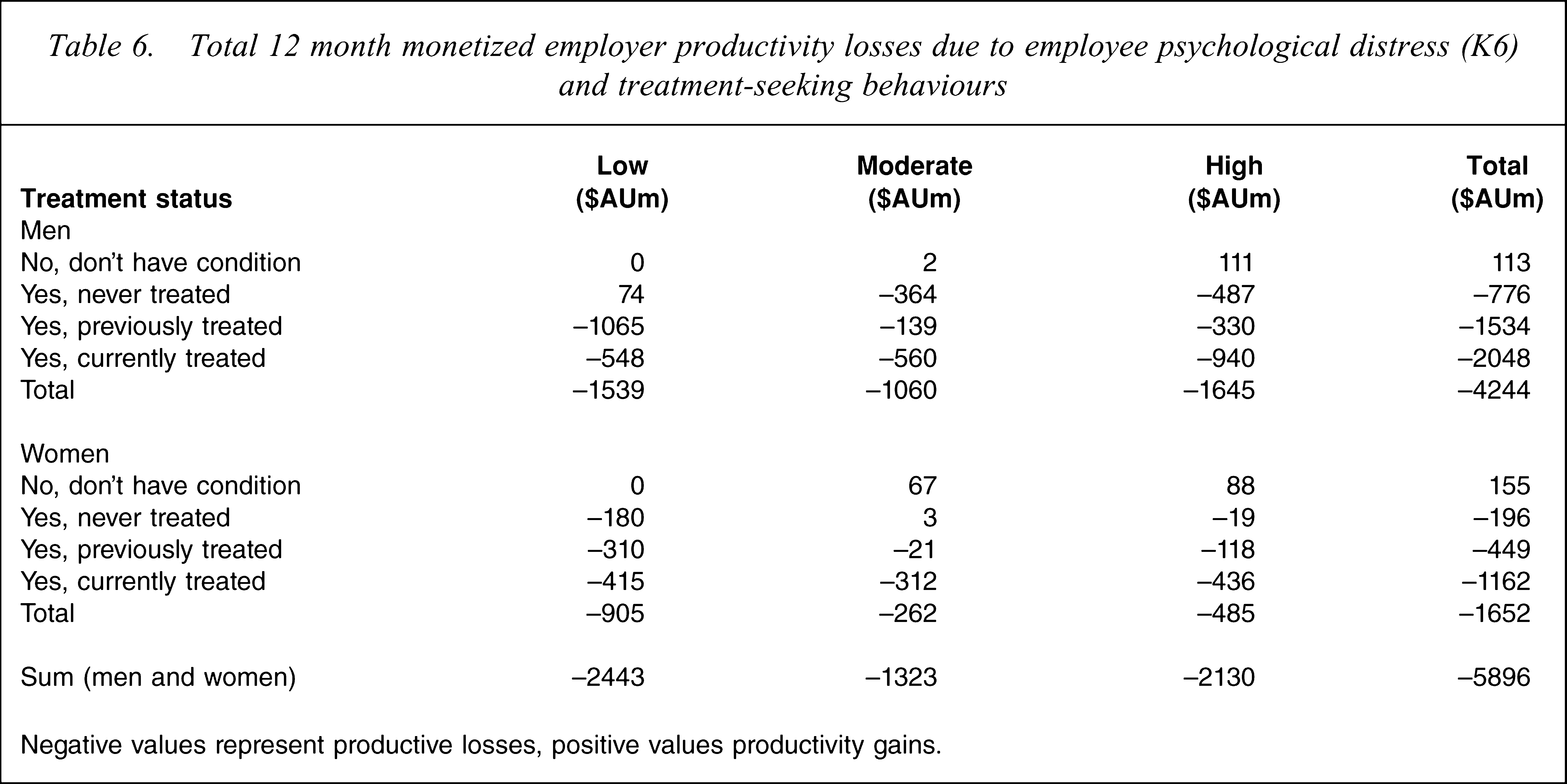
Negative values represent productive losses, positive values productivity gains.
Discussion
The present data exemplify the importance of including treatment status in the estimation of productivity losses due to psychological distress (mental health symptoms). When the prevalence of psychological distress and productivity losses is examined in isolation the estimated productivity impact on Australian employers was $ AU2.81 billion. When treatment-seeking behaviours were considered along with psychological distress prevalence data, the estimated productivity loss to Australian employers jumped to $ AU5.9 billion. This lost productivity equates to an annualized productivity loss of $ AU771 for the average Australian employee (not only those with psychological distress).
Employees who are in current treatment for a mental disorder could be considered a subpopulation for whom there would be little clinical intervention required because they are already engaged with a clinician. The productivity loss of employees in current treatment (Table 6) was the majority of overall productivity losses equating to $ AU3.2 billion. This economic loss may be viewed as set productivity losses that cannot be recouped. This is likely the case for low K6 subjects in current treatment but may not be the case for moderate and high K6 subjects in current treatment. It has been suggested that between 55% and 75% of people receive ineffective or substandard treatment for their mental disorder [42–46]. With this in mind, it stands to reason that a subsample of symptomatic employees (moderate or high K6) who are in current treatment may be under-treated. If this is the case then an effective intervention may be possible. Such an intervention may take the form of distribution of mental health awareness materials by employers addressing what to expect from treatment. Screening of employees for untreated depression followed by a telephone-based outreach programme including care management has been successful in the USA [18]. A similar programme that included the care management of those who remain symptomatic and are in treatment may be a natural extension of telephone outreach programmes. It should be noted that due to ethical considerations we recommend that the screening of employees be confidential and carried out by a third party mental health provider (e.g. Employee Assistance Programme) with no identifiable information shared with the employer. General practitioners (GPs) are the primary clinicians for most individuals with a mental disorder [47,48]. Continuing GP education of best practice treatments would also likely increase the number of employees in successful treatment.
Prior economic estimates suggest that treatment of depression that results in a reduction of symptoms is associated with increased employee productivity [13–18]. In these prior studies all subjects fell into the category of ‘in current treatment’. In the present study we also examined the productivity of those who are not in treatment. If one examines only those who are in current treatment (Table 5), those with lower symptoms (K6 score) have increased productivity, concordant with the impact of treatment. Another limitation of some prior estimates of the lost productivity due to mental disorders is that they used strict diagnostic criteria and did not include those with subthreshold symptoms. The use of the moderate psychological distress in the present study likely captures productivity loss from those employees who have subthreshold psychological symptoms. Furthermore, many studies of economic loss due to mental health symptoms examined non-comorbid mental disorders. The reality is that many individuals have comorbid disorders. Because the K6 total score does not discriminate between depression, anxiety or comorbid depression and anxiety, it is most likely that the use of the K6 in the present work would capture those employees with comorbidity.
A finding worthy of comment is that employees with a low K6 contributed $ AU2.4 billion of the total $ AU5.9 billion in lost productivity. This $ AU2.4 billion cannot be attributed to psychological distress per se because the employees had low psychological distress levels and therefore low-level symptoms. Rather, this is the effect of treatment status for a mental disorder. Employees with low psychological distress either currently treated or previously treated contribute $ AU2.3 billion of the $ AU2.4 billion lost productivity in the low-K6 group. These categories represent a group of successfully treated employees for a mental disorder. The data indicate that a proportion of these employees do not return to full productivity even with what appears to be effective treatment. These employees with a low K6 represent a group for whom further mental health intervention is unlikely to improve symptoms (although it may be maintaining remission). The lost productivity of this group, however, is a significant component of the estimates of productivity decrements due to mental disorders. The assumption is that employees who state that they are either in current or past treatment have had a mental disorder at some time. The total cost of mental disorders then, is $ AU5.2 billion of the total $ AU5.9 billion.
Men had a greater overall annualized productivity decrement than women ($ AU4.2 billion and $ AU1.7 billion, respectively). This was due to (i) men having a greater productivity percentage loss due to moderate and low psychological distress than women; (ii) substantially more men being in the workforce; and (iii) men having a higher salary than women. Thus it appears that psychological distress affects work performance in men more than it does in women. An alternate explanation may be that men and women rate work performance differently. A comparison of productivity estimates for men and women with a low K6 and having never been in treatment (the reference groups), however, shows that men rate their productivity as 21.9% and women rate their productivity at 19.3%. This small difference does not account for the larger productivity differences noted in those with psychological distress. From an employer's view this information suggests that interventions that target men with psychological distress may be appropriate.
Noteworthy is that employees with high psychological distress who were untreated had higher productivity than those with high psychological distress who were in current treatment. The expectation was that those with a high K6 would have similar productivity decrements regardless of treatment status. This is clearly not the case and highlights the importance of including treatment-seeking behaviour into productivity estimates. The finding that treatment is negatively associated with productivity is supported by other studies showing that receiving treatment for anxiety disorders and affective disorders is associated with more individuals not being in the labour force [49,50]. Lim et al. reported that treatment seeking for any mental disorder was associated with greater work loss and work cutback [4]. Employees in current treatment with a high K6 likely represent those who have just entered treatment, those with treatment-resistant symptoms or those who are inadequately treated. One conjecture is that these employees have been advised to take time off work or to cut back their workload by their treating clinician. An alternative explanation is that those with a high K6 who are not in treatment have a reduction in cognitive performance and compensate by working longer hours. This effect has been previously noted, especially in women [38]. A third explanation may be that employees who seek treatment, and subsequently receive a diagnosis, may have a more pessimistic view of their work performance than those without a diagnosis. A comparison, however, of externally reported work performance measures to self-reported performance measure in people with mental disorders noted a good concordance [51].
Limitations
There are two obvious criticisms of this paper: (i) non-random sampling; and (ii) low survey response rate. The first point to consider concerning both of these pertinent criticisms is that the WORC project was purposely designed to be a naturalistic study to promote ease of implementation by employers. In reality, workplaces self-select as to whether they engage in a mental health programme and employees self-select as to whether they answer a health survey in the workplace. Therefore, the current study methodology has ecological validity. The non-random sample of employees reported may not be entirely representative of the population of employees as a whole. For example, due to logistical considerations, we recruited companies with >1000 employees and therefore may not be able to extrapolate the results to employees of small- or medium-sized businesses. The response rate of 25% to the HPQ survey is low in epidemiological terms, but this is the typical response rate obtained when health questionnaires are sent to employees in multiple large companies [18,52–54]. Comparison of responders to non-responders, to a questionnaire containing mental health questions, showed no statistical difference on the Hamilton Depression Scale [55]. Previous studies indicate that a variation in the response rate is not related to prevalence of chronic conditions (including depression) or employee performance [53]. Additionally in the dataset we present here we have previously shown that response rates are not predictive of prevalence of psychological distress [31]. Although the sample is non-random, and has a response rate of 25%, it is one of the largest samples of employees collected. In the very least, the results are strongly indicative and will stimulate further research.
The HPQ measures of productivity (absenteeism and presenteeism) are self-reported and thus have the inherent limitations of any self-reported measure. Calibration studies show good concordance of the HPQ presenteeism metric with supervisor ratings and objective records [1,32,33]. One concern may be that, similar to depression [56], psychological distress may distort cognition, resulting in pessimistic or distorted ratings of performance. However, as previously noted, externally reported work performance has a good concordance with self-reported work performance measures in people with mental disorders [51]. Monetizing productivity is contentious at best. How an individual's perceived performance and their perceived performance of others translate into actual dollar changes is poorly researched. All the tools available to quantify presenteeism are crude surrogates, but they are currently the best available.
Costs did not include employee overheads (capital costs, fringe benefits etc.), replacement costs (employing temporary staff or payment of overtime), reduced customer satisfaction leading to loss of business, overrun of time-dependent projects, costs of suicide, employee attrition, early retirement, medical treatment for workplace accidents/incidents, effects on other employees (spill over effects) or workplace insurance claims and litigation.
The Australian labour force has seen a significant shift away from full-time employment, with the proportion of part-time workers increasing by 22% between 1991 and 2001 [57]. According to the existing literature, mental illness appears to be more prevalent in non-full-time employees, particularly for men [58,59]. A body of literature indicates that prior depression predicts future unemployment [60–62]. It is therefore reasonable to hypothesize that depressive symptoms may also predict increased risk of transitioning from full-time work, although there is little published evidence to support this. Given this information, the lost employee productivity estimates underestimate the overall productivity losses when part-time and casual employees are incorporated. Mental health problems can result in long-term sickness absence [63]; these absences would not have been captured to their full extent due to the employees not being present at work to answer the survey.
Conclusions
Psychological distress is prevalent, with 13.1% of male employees and 14.9% of female employees having either moderate or high levels of psychological distress. This equates to 0.66 million male employees and 0.39 million female employees (total 1.05 million employees) in Australia who have some degree of psychological distress. Treatment of mental disorders that reduces symptom levels to low K6 values returns employee productivity to near, but not the same as, the productivity of asymptomatic individuals with no prior history of a mental disorder (6.4% productivity difference between the groups). This highlights that workplace programmes addressing mental health have a real potential for substantial return on investment. Evaluation of the interaction between treatment-seeking behaviour and K6 symptom levels shows that the cost of psychological distress (mental health symptoms) to Australian employers is $ AU5.7 billion. Given the current global economic crisis with a downturn in overall productivity and output, an investment in the mental health of employees may play a role in increasing company productivity. In the current economic state many employees face job insecurity. Job insecurity is associated with worsening mental health [64,65], thus the need for mental health interventions may also be elevated.
Footnotes
Acknowledgements
The authors would like to acknowledge the contributions of Professor Ronald Kessler and Dr Philip Wang in the design of the study protocol and Catherine Cleary and Dr Judith Sheridan in the data collection. This work was financially supported by the Department of Health and Ageing, Mental Health Strategy Branch, Australian Government, Canberra, Australian Capital Territory; beyondblue: the national depression initiative, Melbourne, Victoria; and the Australian Rotary Health Research Fund, Parramatta, New South Wales, Australia.
