Abstract
The aim of the present study was to provide a critical review of prevalence estimates of combat-related post-traumatic stress disorder (PTSD) among military personnel and veterans, and of the relevant factors that may account for the variability of estimates within and across cohorts, including methodological and conceptual factors accounting for differences in prevalence rates across nations, conflicts/wars, and studies. MEDLINE and PsycINFO databases were examined for literature on combat-related PTSD. The following terms were used independently and in combinations in this search: PTSD, combat, veterans, military, epidemiology, prevalence. The point prevalence of combat-related PTSD in US military veterans since the Vietnam War ranged from approximately 2% to 17%. Studies of recent conflicts suggest that combat-related PTSD afflicts between 4% and 17% of US Iraq War veterans, but only 3–6% of returning UK Iraq War veterans. Thus, the prevalence range is narrower and tends to have a lower ceiling among combat veterans of non-US Western nations. Variability in prevalence is likely due to differences in sampling strategies; measurement strategies; inclusion and measurement of the DSM-IV clinically significant impairment criterion; timing and latency of assessment and potential for recall bias; and combat experiences. Prevalence rates are also likely affected by issues related to PTSD course, chronicity, and comorbidity; symptom overlap with other psychiatric disorders; and sociopolitical and cultural factors that may vary over time and by nation. The disorder represents a significant and costly illness to veterans, their families, and society as a whole. Further carefully conceptualized research, however, is needed to advance our understanding of disorder prevalence, as well as associated information on course, phenomenology, protective factors, treatment, and economic costs.
Despite a large body of literature on combat-related post-traumatic stress disorder (PTSD) there remains a lack of clarity regarding the prevalence of the disorder among military personnel and veterans. Even when there is consistency in issue or phenomenon, sufficient heterogeneity exists in the methodology of the studies that the conclusions drawn are often different, and data are available to support almost any position [1]. The 2007 debate in Science, and then later in the Journal of Traumatic Stress, following the Dohrenwend et al. re-evaluation of the prevalence of PTSD among Vietnam veterans documented by Kulka et al. in the National Vietnam Veterans Readjustment Survey (NVVRS) [2,3], demonstrates an interesting range of perspectives that experts in this field hold about the same study [4–15]. Data from this one study have been interpreted to indicate a 15.2% [3], 9.1% [2], and 5.4% [11,13] point prevalence of PTSD among Vietnam veterans when measured in the late 1980s – a potential overestimation of nearly 300%. A recent article by Dobbs in Scientific American and numerous media articles, radio and television stories, and blogs further reinforce that the issue of PTSD prevalence remains heatedly debated and continues to polarize the traumatology field and even politics in the US [16]. This is partly due to the fact that the stakes are huge: major decisions about Veterans Affairs (VA) funding, research allocations, disability payments, and even society's perspective on war itself hinge on these data.
Recent studies of returning Operation Iraqi Freedom (OIF) and Operation Enduring Freedom (OEF) veterans have generated numerous concerns regarding the long-term mental health consequences of combat exposure [17–23]. Historically, military conflicts have differed in duration, intensity, and public credibility of purpose [24], and the question regarding the similarity or difference of the psychological effects of combat across different combatant cohorts remains unanswered. The goal of the present study was to provide a critical review of prevalence estimates of combat-related PTSD among military personnel and veterans, and of the relevant factors that may account for the variability of estimates within and across cohorts, including methodological and conceptual factors accounting for differences in prevalence rates across nations, conflicts/wars, and studies. It was not the aim of this paper to identify a single point prevalence estimate. Indeed, it is difficult to narrow the range of point prevalence for combat-related PTSD due to the significant heterogeneity of methods and samples used across studies, even within the same conflict/war cohort. The direct comparison between US and other NATO military forces across the same conflicts offers a unique approach to demonstrating how these factors interact with sociopolitical and cultural factors and may manifest differently across different samples and studies. Because of factors unique to the peacekeeping experience compared to active combat, the issue of PTSD prevalence in peacekeepers will not be included in this review.
For the present review we examined MEDLINE and PsycINFO databases for literature on combat-related PTSD. The following terms were used independently and in combinations in this search: PTSD, combat, veterans, military, epidemiology, prevalence. This review is not intended to be exhaustive of all information pertaining to combat-related PTSD, a large and diverse body of literature.
Prevalence of combat-related PTSD in US samples
The point prevalence of combat-related PTSD reported across studies of US combat veterans ranges from approximately 2% to 17%; and lifetime prevalence approximately 6–31% [2,3,17–19,25–37]. Point prevalence rates from veterans of the Vietnam War range from 2.2% to 15.2% [2,3,25–28]. Among Persian Gulf War veterans, PTSD rates reported are between 1.9% and 13.2% [30–39] and from veterans of the current conflict in the Middle East, PTSD point prevalence is reported from 4% to 17.1% [17–19]. See Table 1 for a summary of studies.
Prevalence estimates of combat-related PTSD
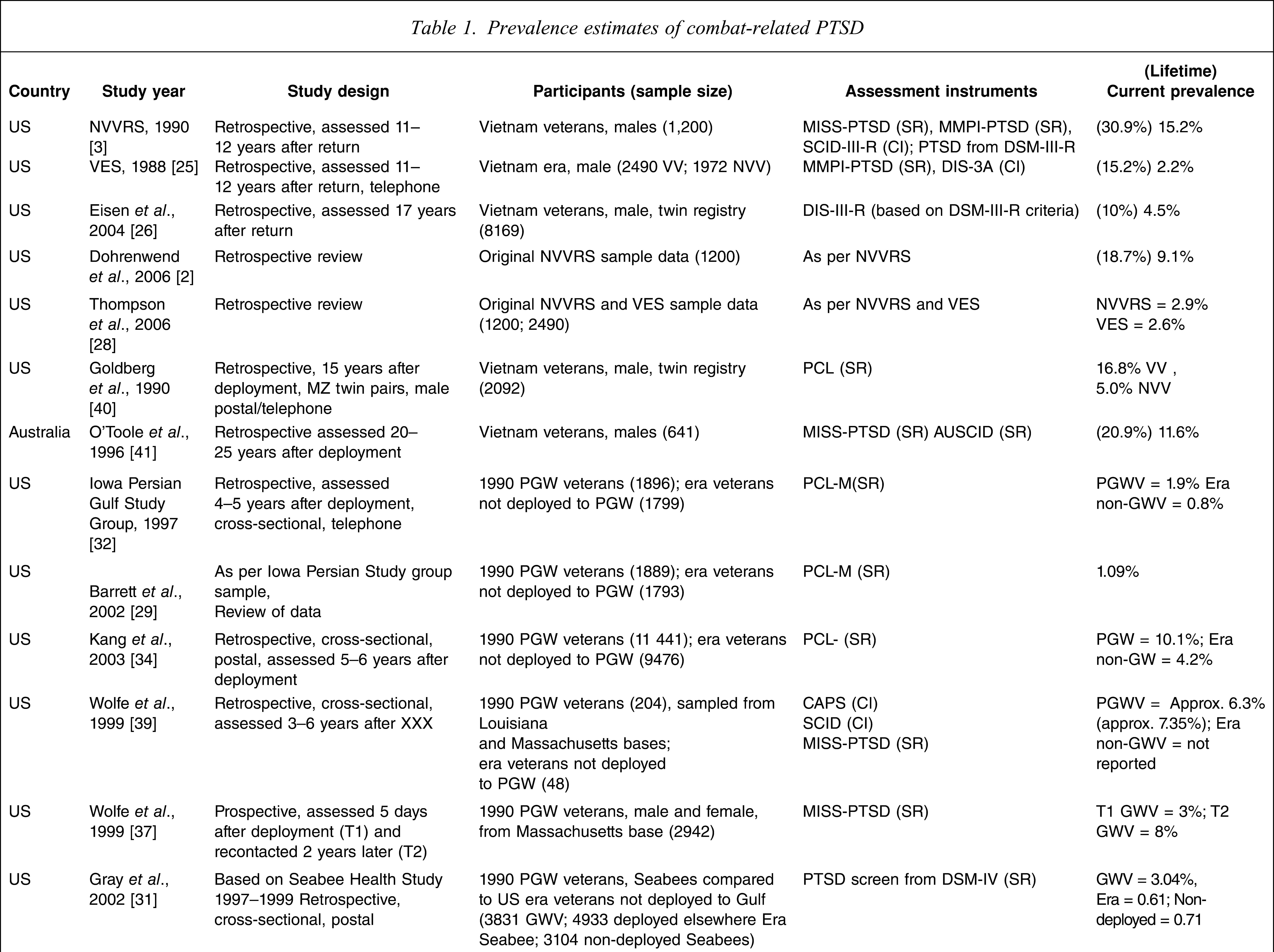
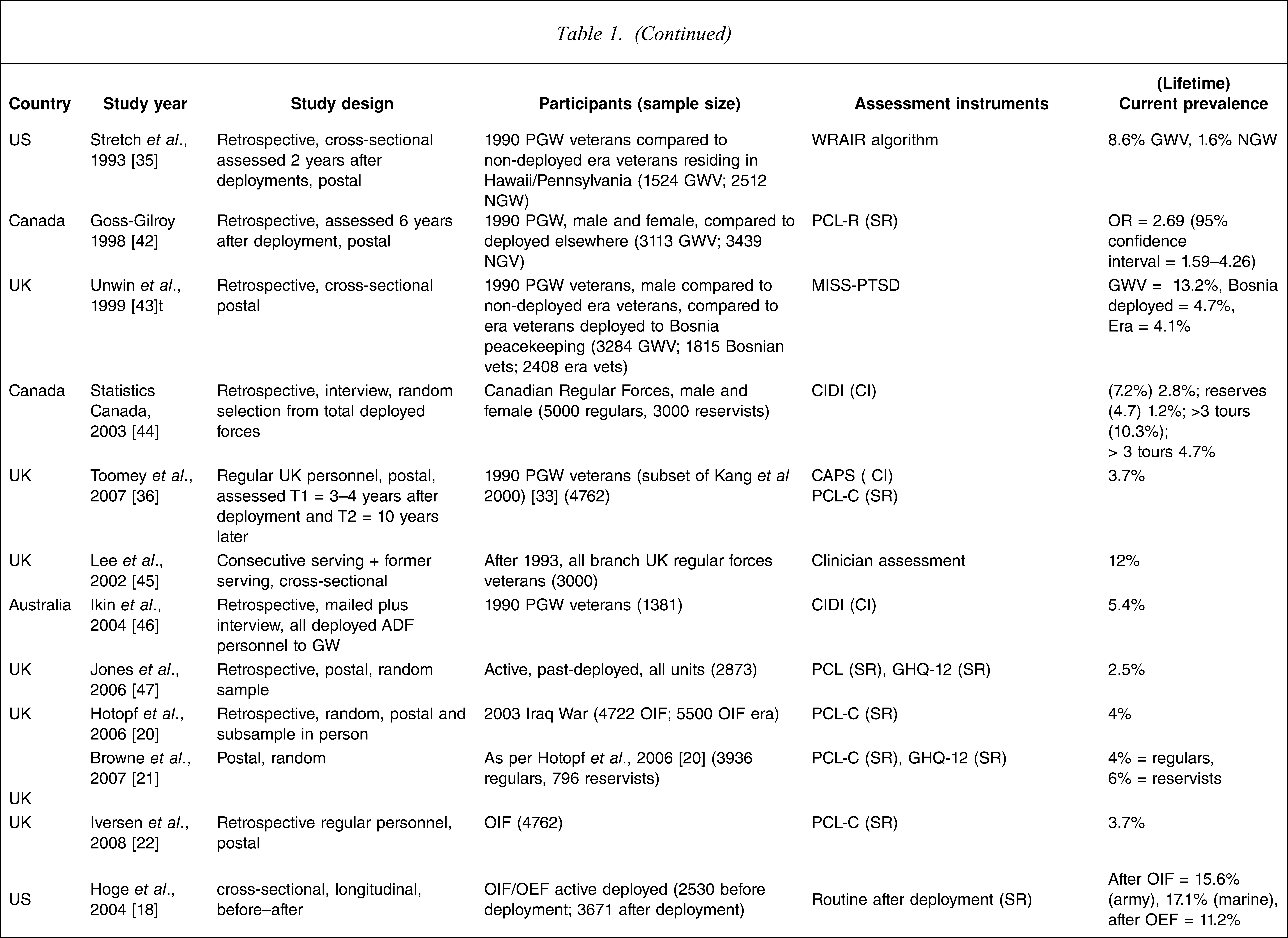

ADF, Australian Defence Force; AUSCID, Australian Version Structured Clinical Interview for DSM-IIIR; CAPS, Clinician-Administered PTSD Scale; CI, clinical interview; CIDI, Composite International Diagnostic Interview; DIS, Diagnostic Interview Schedule; GHQ-12, General Health Questionnaire-12; GW, Gulf War era veteran, did not serve in Gulf War; MISS-PTSD, Mississippi Scale for post-traumatic stress disorder; MMPI-PTSD, Minnesota Multiphasic Personality Inventory, PTSD subscale; MZ, monozygotic twins; NVV, Vietnam era veteran, did not serve in Vietnam; NVVRS, National Vietnam Veterans Readjustment Survey; OEF, Operation Enduring Freedom (Afghanistan); OIF, Operation Iraqi Freedom; PCL, PTSD Checklist; PCL-C, PTSD Checklist-Civilian; PGW, Persian Gulf War; SCID, Structured Clinical Interview for DSM; SR, self-report; VA, Department of Veterans Affairs; VES, Vietnam Experience Study; VV, Vietnam veteran; WRAIR, Walter Reed Army Institute of Research.
US Combat veterans demonstrate a two–fourfold increase in prevalence of PTSD compared to US civilians, depending on the subject cohort and research methodology used. Estimates of the point prevalence of PTSD among community samples of adults in the USA is 5–6% [49,50], with overall lifetime prevalence of the disorder estimated at 7.8%, [51]. Overall PTSD prevalence in VA primary care clinics is 11.5% [52]. The numbers of veterans seeking VA mental health care for PTSD has grown dramatically over the past 10 years [53]; a large proportion of which is due to newly diagnosed Vietnam veterans [16], with lowest rates among veterans of World War II [54]. Given that the VA serves a relatively small percentage of veterans nationally, and their patient population has a lower income and higher illness burden than the general population of veterans, one might expect that PTSD prevalence would be higher than among the entire population of veterans.
Vietnam War
The debate regarding the prevalence of combat related PTSD was fuelled to a large extent by the publication of contrasting findings of two major US studies of Vietnam veterans conducted in the late 1980s. The NVVRS used multiple self-report instruments in addition to the Structured Clinical Interview for DSM-III-R PTSD (SCID-PTSD) to estimate PTSD prevalence in a community sample of 1200 Vietnam veterans and Vietnam era non-serving veterans and civilians [3]. The NVVRS estimated that the prevalence of lifetime PTSD among male Vietnam theatre veterans was 30.9%, and point rates at 15.2%. Against the expectations of post-combat psychological burden at the time, the high rates of PTSD obtained in the NVVRS represented a significant and unanticipated mental health problem [2,12,55,56]. These elevated rates remain among the most frequently cited in the combat-related PTSD literature, although they have been criticized in relation to a number of theoretical and methodological factors [4,7,8,10–13,57]. Multiple revisions of the original NVVRS data on the basis of definitions of clinical severity have obtained lower prevalence rates [2,10].
Just prior to the release of the NVVRS findings, results from the Vietnam Experience Study (VES) were published [25]. Using a modified version of the Diagnostic Interview Schedule for PTSD (DIS-PTSD), that study compared rates of PTSD in a random sample of serving and non-serving Vietnam veterans (n = 4462) matched in terms of level of education, employment, income, marital status, and satisfaction with personal relationships. The VES reported that 14.7% of Vietnam veterans experienced combat-related PTSD at some time during or after military service, and 2.2% had the disorder during the month before the examination. This was dramatically lower than prevalence estimates of the NVVRS. According to the NVVRS researchers, the validity of the PTSD diagnoses made in the VES using the DIS-PTSD is unsupported in the literature [14]. Further discussion of the impact on prevalence estimates of different PTSD assessment instruments is included in the following section.
Also conducted in the late 1980s, the findings of the methodologically rigorous Vietnam Era Twin Registry studies [40], received relatively little attention. In that study (n = 6744 monozygotic and dizygotic pairs), monozygotic twins who were discordant for service in Vietnam were examined. Of the twins who had served in Vietnam, 16.8% had PTSD, in contrast to 5% of twins who had not served in Vietnam. The prevalence of PTSD in the twins exposed to high rates of combat exposure was ninefold higher than in their non-combat siblings. Subsequent analyses from that study have shown a significant influence of genetic heritability on symptom expression of PTSD [58,59]. That Twin study is now in the early stages of being replicated and extended almost 20 years later [Magruder KM: personal communication].
Operation Desert Storm (1991 Gulf War)
In later war cohorts the estimates of PTSD prevalence are also mixed. The 8 month, 1990 conflict in the Persian Gulf was unique in US Armed Forces history because 17% of the 694 000 personnel were from Reserve and National Guard Units. For the 40 days of air warfare and 5 days of ground combat, there were fewer than 200 battle deaths and relatively few casualties inflicted upon US military personnel. Unlike previous veterans, however, Gulf War veterans were subject to a variety of potentially harmful environmental exposures, both natural and man-made [33]. Researchers generally report lower rates of PTSD among Gulf War veterans than among military personnel from other wars [32,33,38,39,60].
To investigate mental health outcomes from the Gulf War, an epidemiological study (National Health Survey of Gulf War Era Veterans and Their Families) was conducted on a randomly chosen sample of 15 000 Gulf War and 15 000 non-war veterans selected from the total number of US troops who were deployed in the Persian Gulf area during the Gulf War [26,33,34,36]. In 1995, a total of 11 441 Gulf veterans (75%) and 9476 non-Gulf veterans (64%) selected for the first wave of evaluation, participated. At 5–7 years after deployment, 10.1% of deployed Gulf War troops (compared to 4.2% of non-deployed era veterans) were estimated to have PTSD during the month prior to completing the self-administered PTSD checklist (PCL), and general health symptom questionnaire [34]. Toomey et al. evaluated a subset (n = 2189) of the same Gulf veterans using retrospective self-report and face-to-face psychological examinations conducted approximately 10 years after deployment (i.e. 1998–2001) [36]. The war-onset prevalence of PTSD was estimated at 6.3% for deployed veterans and 1.1% in the non-Gulf deployed era veterans. Ten years after the end of the Gulf War, 1.8% of deployed veterans who had war-onset PTSD remained symptomatic. Within this cohort, the retrospective estimates of the prevalence of PTSD decreased over time. In contrast, Wolfe et al. reported a prospective PTSD prevalence of 3–7% among New England army veterans of the Persian Gulf War within 5 days of return from deployment, increasing at follow up 18–24 months later to 8–16% [39]; a phenomenon also noted by Gray et al. [61].
A curious outlier, the Iowa Persian Gulf Study Group reported PTSD prevalence estimates of 1.9% in a sub-sample of (n = 3969) of Gulf War veterans [30]. Such an anomalous result has been suggested to be the consequence of a study participation bias and response bias, which may have occurred given the contemporary media emphasis on reporting the less specific, somatically focused symptoms of ‘Gulf War syndrome’ at the time [60–62]. The variable course of the disorder, coupled with methodological, exposure and cohort differences, have influenced the heterogeneity of PTSD prevalence rates among Gulf War veterans, as they have done in Vietnam veterans.
Operation Iraqi Freedom and Operation Enduring Freedom
Using the self-report PCL, Hoge et al. evaluated the psychological sequelae of current US Army and Marine commitments to Iraq (OIF) and Afghanistan (OEF) [18]. In that study PTSD was present in 18.1–19.9% of returning OIF soldiers, 11.5% of returning OEF soldiers, and 9.4% of soldiers prior to deployment, but when stricter criterion measuring symptom severity was included these rates dropped to 12.2–12.9%, 6.2% and 5%, respectively. Unlike earlier studies, the Hoge et al. study estimated combat-related PTSD while fighting continued, and incorporated cross-sectional pre-deployment data [18]. Such contemporaneous data collection may reduce the potential impact of a wide range of influencing factors such as media contagion effects, social influence or peer contamination, recall bias, participation bias, and exaggeration or falsification due to compensation or litigation claims. In a later study of deployed US personnel (n = 303 950), the presence of PTSD was measured by scoring ≥2 on the four-item PTSD scale to obtain estimates of PTSD at 9.8% for OIF, 4.7% for OEF, and 2.1% for other locations [17]. In that study prior trauma exposure was not controlled for and false positives likely because such measures are designed to err in that direction.
In a population survey of 103 788 veterans active from 2001 to 2005 and newly registered with VA, 13% of the study population were diagnosed with PTSD [19]. Rates were highest in the veterans aged 18–24 years and lowest in veterans aged 40+ years. Another large scale study of 50 184 active military duty and Reserve/National Guard personnel reported an overall prevalence of new-onset PTSD based on the self-report PCL of 7.6–8.7% among those who were both deployed and reporting combat exposures, compared to 1.4–2.1% of deployers not reporting combat exposures and 2.3–3.0% of non-deployers [48]. Findings indicated higher rates of PTSD among personnel who were younger, less educated, enlisted, current smokers, and problem drinkers; with no effect found for race or service component (i.e. active duty versus Reserve/National Guard). Findings highlight the importance of specific combat exposures over mere war-zone deployment as contributing to new-onset PTSD.
Detracting from the value of these recent studies are concerns that results (i) are based entirely on self-report checklists, which have differential validity from structured psychiatric interviews [63]; (ii) may not incorporate information regarding functional impairment (required for DSM-IV diagnoses); and (iii) do not inquire about exposure to prior trauma. Failing to take such factors into account may result in overestimated rates of combat-related PTSD [2,10,64,65].
Prevalence of combat-related PTSD among samples from other Western nations
The prevalence estimates in studies of combat veterans of Western nations other than the USA have smaller ranges and lower ceilings (Table 1). The 2002 Canadian Forces Mental Health Survey of Regular Forces reported lifetime prevalence estimates of 7.2% and current estimates (i.e. within the last year) at 2.7% For those who have completed three or more operational tours, the figures rise to 10.3% in their lifetime, and 4.7% over the previous year [44].
In Australian samples, PTSD prevalence in Australian Defence Force (ADF) Vietnam veterans has been reported at around 21% for lifetime and 12% for current [41]. At 10–15 years after Gulf War deployment, 5.4% of 1871 ADF Gulf War Veterans have current PTSD [46]. Both estimates were obtained through structured clinical interviews. Estimates of PTSD in ground forces of the ADF serving in Iraq and Afghanistan are as yet unpublished, but Royal Australian Navy (RAN) estimates of PTSD in the 1739 sailors deployed to the Middle Eastern Area of Operations (MEAO) between 2001 and 2005 was 1.6% in total (corrected) as measured by scores >50 on the PCL [66]. From UK-based research, Lee et al. reported 12% prevalence of PTSD, based on a psychiatrists’ assessment among a consecutive sample of UK Gulf War veterans (n = 3000) attending Veterans Medical Service between 1993 and 2001 [45]. Jones et al. [47] mailed the PCL and General Health Questionnaire-12 to a random sample of UK veterans (n = 2873; including all branches) deployed after 1999. They reported that 53% of their sample had deployment experience and 2.5% of their total sample had PTSD in 2002. In the largest population-based study of UK combat veterans thus far, Hotopf et al. reported health outcomes in a random sample of UK armed forces personnel deployed to the 2003 War in Iraq (n = 4722) and personnel not deployed (n = 5550), who were demographically similar in all other ways [20]. Participants completed a 28-page questionnaire on various health concerns, general well-being and alcohol consumption as well as PTSD symptoms. Findings for current rates of PTSD were 4% of the sample. In a later study of the same sample, differences in prevalence rates between OIF-deployed regular UK army personnel and OIF-deployed UK army reservists was 4–6%, respectively [21]. Iversen et al. also reported a 3.7% prevalence PTSD among UK veterans (n = 4662) of Iraq [22].
The findings of PTSD prevalence in the 2.5–6% range are in contrast to the Hoge et al. finding of 17.1% among US veterans [18], when using an identical measure and case definition. In all UK-based studies, personnel from regular forces who had a combat role and/or contact with the enemy were more likely to have had PTSD symptoms than those deployed in other roles [20,22,23,47]. One possible reason for the disparity between US and UK samples lies with differences in the frequency, duration and intensity of combat exposure during deployment. Other UK-based research, however, argued that it is premature to conclude that significant deleterious effects are an inevitable outcome of going to war [20,67]. Differences between UK and US estimates may also be related to pre- and post-exposure factors including childhood vulnerability, sociopolitical variables and military training [21,68–70].
Methodological and conceptual factors
The 2–17% point prevalence for PTSD represents significant heterogeneity in numbers of affected veterans, even within the same war cohort. It has been suggested that the sources of variance are largely the results of methodological and conceptual factors that differ across studies, as is demonstrated in the progressive scaling down of estimates based on the NVVRS [71]. In the next section we address more generally a number of methodological and conceptual factors that differ across studies and may help to explain the wide range of combat-related PTSD prevalence across these studies.
Sampling strategies
Sample size
Over time the sample sizes on which prevalence has been determined have increased dramatically. Perhaps the most frequently cited point-prevalence of PTSD is from the NVVRS, which is based on only 1200 subjects compared with the Seal et al. sample of 103 788 OIF/ OEF veterans [19]. To what extent were the NVVRS 1200 (and then the smaller subsample overrepresented by high combat exposure and probable PTSD [26]) genuinely representative of the 2.7 million Vietnam veterans? Despite the complex statistical randomization procedures used, such figures may not logically appear representative or, even at face value, seem adequate to extrapolate to such a large population. In contrast, studies with very large samples rely on self-report measures over clinical interviews, and are thus methodologically less rigorous.
Selection/participation bias
Maximising response rates is important for survey research to be considered valid and reliable. Given that avoidance of trauma cues is a symptom of the disorder, those with PTSD may have avoided participation in epidemiological studies. The mass pre- and post-deployment psychiatric screening programmes seen in the recent US studies are likely to eliminate such issues from US studies, but other Western nations do not necessarily conduct mass-screening of their armed forces and this issue may remain of interpretive concern. Participants who are voluntarily assessed and remain anonymous may have fewer disincentives for candid self-appraisal, whereas those who are compulsorily screened may have more incentives to minimize distress including stigma from disclosure, avoidance of delays to post-deployment reunion, and the possibility of long-term consequences to future employment opportunities in and outside the military [17]. Alternatively, combat veterans who are ill may assign more salience to memories of combat, whereas those who are well may minimize combat exposure [60,62]. It is possible that veterans who most strongly associate their symptoms with their war experience may be prone to inflate the relationship between these variables [72]. Consequently, due to the demonstrated relationship between affective state and recall, perception and cognitive processing [43,72,73], the potential for sampling bias among those who do participate in research studies may increase. Thus far, research suggests that the influence of low participation rates [71] or non-responders [34,43,67,74] is unlikely to affect such studies’ larger outcomes.
Comparison groups
Appropriate comparison groups are difficult to identify in military research, because comparisons between military and civilian groups are often unsuitable. The military may attract high risk takers, exhibit a ‘healthy warrior bias’, and/or lack the representative racial and socioeconomic diversity of the general population [60,75], yet often age-matched civilian peers serve as comparison groups in military mental health research [47].
As a comparison group, reservists can also be distinct from regular military personnel. They may not maintain the same levels of fitness, have minimal deployment experience, be deployed to roles for which they are untrained, be assigned dangerous combat duties that they did not expect, and may face unique social and personal stressors when deploying or returning home [20,21,76]. In the past, soldiers who were physically or mentally ill were unlikely to be deployed [43,47,77]. Yet, armed forces are relying on larger numbers of reserve personnel whose pre-deployment health status may be less assured, and there may be a possible association between combat-related psychiatric disorders and reservist status [20,21,32,78,79]. Research has demonstrated that elite forces and officers, who are typically better trained and more cohesive, have better fitness and higher motivation, and frequently have lower levels of PTSD than lower ranks, general personnel and reservists [22,48,67]. Findings from research on Gulf War veterans demonstrate differences in levels of post-deployment mental health and psychosocial problems among National Guard and Reserve personnel involved in the 1990 Persian Gulf War compared to active duty troops [32,34,35]. In contrast, one large recent study found no PTSD prevalence differences between active duty personnel and reservists [48].
Exposure to combat risk has been one explanation for the differences in PTSD estimates observed between the USA and other nations’ combat forces. Personnel from different nations are deployed to different areas, which may differ in risk levels and combat intensity. It is unlikely, however, that non-US forces are not exposed to significant risk. In fact, several studies report that high risk and significant exposure occur for personnel from all nations deployed to war zones [22,43] and, as such, the differential exposure argument alone is insufficient to explain PTSD prevalence differences. Contrasting differences in prevalence results from US and UK force samples, Hotopf and Wessely reported that, unlike US combat forces deployed to the Persian Gulf War, in most cases even non-Gulf War-deployed veterans in UK studies had been deployed to other combat zones (e.g. Falkland Islands, Northern Ireland, Somalia, Kosovo), and therefore had been exposed to risk previously [60]. They and others have argued that because of differences in pre-, and post-military experiences, not combat exposure alone, it may be inappropriate to make too much of such comparisons [21,47,76,80].
Measurement strategies
Estimates of combat-related PTSD prevalence depend heavily on how symptoms and impairment are measured [81–83], the subsequent reliability and validity of the instruments themselves, and their lay versus expert administrators [2]. The VES study was criticized for using lay interviewers to administer a single abbreviated measure of PTSD (the abbreviated Diagnostic Interview Schedule; DIS-PTSD) to estimate prevalence, compared to the multicomponent assessment process administered by experienced clinicians, used in the NVVRS [2,84]. The DIS-PTSD measure has been argued to underestimate the rate of PTSD in civilian and military personnel [6,51]. The authors of the NVVRS, however, acknowledged that ‘when instrumentation and scoring procedures matched to those used by CDC were used with NVVRS data, the resulting estimates of current prevalence were statistically indistinguishable from those published from the CDC VES’ (p. 556) [84]. Clearly the type of measures used, their purpose for use as either screening or diagnostic tools, the anonymity or voluntary nature of their administration, in addition to the timing of administration, are all important mediating factors that contribute to the variability observed and the subsequent concern regarding the overarching definition of the PTSD construct [16,85].
Structured psychiatric interviews versus self-report instruments
Differences in PTSD prevalence have also been attributed to whether data were obtained via ‘self-report’ measures or ‘structured psychiatric interviews’, because there are good data that the former overestimate PTSD. This is, at least in part, because few self-report measures attempt to assess the extent of functional impairment. In a sample of war zone-deployed Dutch soldiers, PTSD prevalence from structured psychiatric interviews was 41% lower than estimates from self-report questionnaires [64]. Similar findings were noted in a post-9/11 sample of New York City adults, where it was found that 4.1% obtained a score indicative of ‘probable PTSD’ on a self-report instrument (the PCL) whereas less than half that (1.7%) met full symptom criteria on a structured psychiatric interview for PTSD [63]. The PCL is a commonly used self-report measurement tool to screen for PTSD and a clinical cut-off of ≥50 is typical [18,32]. Some studies, however, have demonstrated the overestimation of PTSD by the PCL with cut-off ≥50 [46,47]. Other studies have reported lower estimates of PTSD when assessed using structured clinical interviews (i.e. Clinician-Administered PTSD Scale) compared to rates obtained via self-report measures (i.e. PCL). They consider the former the gold standard for diagnosing mental disorders, and that the estimates obtained through structured interview are therefore more accurate [34]. Thus, studies based entirely on self-report measures that do not evaluate clinical impairment [17,18] may represent significant overestimates of PTSD prevalence.
DSM-IV clinically significant impairment criterion
The DSM-IV's introduction of the requirement that a trauma-exposed individual must appraise their exposure with horror, fear or helplessness, and that they must be significantly impaired as a consequence of their exposure for a diagnosis of PTSD to be made, has ultimately decreased the prevalence rate of PTSD and is a major explanatory factor for discordant prevalence estimates from studies using DSM-III-R criteria that did not require the ‘clinically significant impairment’ criterion for a diagnosis of PTSD. Studies have demonstrated that PTSD rates are reduced substantially when adjusted for PTSD symptoms that are unrelated to functional impairment [2,18,64]. Some assert that the Dohrenwend et al. GAF score of 7 as a cut-off for positive PTSD [2] is sufficiently conservative to capture genuine cases of impaired veterans [8,9], while others disagree [4,7,13]. McNally argued that the NVVRS PTSD prevalence drops from 9.1% to 5.4% (a 65% reduction of the original estimate) when a ‘clinically significant functional impairment’ criterion (e.g. score of 1–6 on a 10-point global assessment of functioning) is applied to the Dohrenwend et al. [2] reanalyses of the NVVRS data [11,13]. Data from a large community sample of civilians show that inclusion of the clinical significance criterion in DSM-IV reduces the conditional probability of PTSD, given exposure to trauma, by approximately 30% [83]. This particular issue, however, is much disputed due to its centrality to the debate surrounding the construct of PTSD as a whole [16,55,86], and further discussion is beyond the scope of this paper.
Timing and latency of assessment and potential for recall bias
The delay between combat exposure and the assessment of symptoms is a significant issue [20,87]. The validity and reliability of PTSD prevalence estimates may be compromised by (i) selection bias associated with normal military personnel attrition; (ii) poor recall; (iii) intervening influences of the media and popular opinion; (iv) systemic influences, such as VA disability incentives; (v) the influence of emotional and psychological state on memory and cognition; and (vi) other sociopolitical and cultural factors that may influence reporting.
In the epidemiological studies conducted with Vietnam veterans, data were not collected until 10–20 years after the war zone deployment and relied on retrospective self-reports of combat experiences and symptoms [56]. Concern regarding the reporting of combat exposure has been minimized in the NVVRS and largely mitigated for other community samples via the recent reanalyses by Dohrenwend et al. [2], which included a careful examination of archival records and supported the general reliability of self-reported combat exposures in a community sample of Vietnam veterans. Similarly, although Gulf War veterans’ health problems began surfacing in the early 1990s, the first large-scale research into the health consequence of participation in this war did not occur until 5 years after the war ended in both the USA [88] and the UK [60].
Recall biases are a direct threat to validity of war-related research. Typically, studies linking combat exposure to PTSD have relied upon retrospective self-reports of veterans [75,89]. Prevalence studies treat such accounts as reliable and accurate despite the presupposition that respondents’ clinical state was altered by the trauma [90]. In fact, research shows current clinical state, self-perceived health status, and salience of the memory all affect how traumatic experiences are recalled [39,62,72,73,91,92]. Because perception of illness can affect recall or interpretation of events leading to illness, veterans who feel unwell may be more likely to recall experiencing combat exposures during deployment [39,62,93]. Koenen et al. examined consistency in combat exposure reports and their relation to PTSD symptoms in Vietnam Veteran American Legionnaires (n = 1462) who responded to two mailed surveys, 14 years apart (1984,1998) [94]. Combat exposure reports were highly reliable (test–retest correlation = 0.87). Changes in exposure reporting, however, were related to changes in PTSD symptoms; specifically re-experiencing symptoms. Other research demonstrates that 88% of Gulf War veterans remembered traumatic events differently than how they had originally reported them 1 month after their war service and that increased reporting was positively associated with reports of PTSD symptoms [72].
Over time, the delay between exposure to combat and time of assessment has been reduced. Compared to the data collected on Vietnam veterans 10–20 years after the end of the war, Hoge et al. [17,18] and Seal et al. [19] reported the findings of combat exposure and symptom presentation immediately after deployment, while the fighting continued, and, increasingly, also have access to pre-deployment data [17–19]. Iversen et al. and Rona et al. also collected post-deployment data longitudinally and within 1 month after return [22,23]. Such approaches should result in stronger validity of conclusions. Timing of assessment, however, is a complex issue in that data indicate that prevalence of mental health problems may increase significantly at 120 days after deployment relative to immediate post-deployment assessments [16,84]. While a long delay between exposure and assessment is clearly undesirable, immediate assessment after deployment may also underreport the prevalence of PTSD due to the observation that soldiers may feel relief and optimism about their imminent return home, thereby masking immediate distress, or may purposefully minimize distress to avoid delaying their return and subsequent leave entitlements [87].
Finally, research demonstrates that attrition rates from the military after active duty for health and socioeconomic reasons are approximately 5% per year from UK armed forces, which translates to large numbers of veterans being lost from research sampling when post-deployment studies are delayed [60]. Hoge et al. reported that within 6 months after hospitalization, 47% of soldiers who were hospitalized for the first time in 1996 with a mental disorder as a primary diagnosis, left military service [95]. In comparison, only 12% of personnel hospitalized for non-psychiatric medical illnesses left the service in the same period. Therefore in cross-sectional studies such as those cited here, it is possible that the samples may reflect the self-selecting out of the unwell, the homeless, and the substance using; all factors that may be associated with psychiatric distress and disorder, thereby obscuring genuine prevalence rates.
Pre-, peri-, and post-deployment factors
Factors associated with combat are assumed to be critical mediators in the expression of PTSD, including deployment-specific factors such as intensity and duration of combat. Risk factors for PTSD also include features of personal vulnerability, other war zone experiences, and a wide range of sociocultural and situational factors. Pre-, peri-, and post-deployment factors interact to influence symptom development and adaptation, and significantly affect PTSD prevalence and course [22,23,76,96,97].
Pre-deployment factors
The expression of PTSD is partially mediated by genetic factors [58,94,98–101]. Other relevant pre-deployment factors include age and education at time of deployment, gender, race, early conduct problems, intelligence, childhood adversity, family history of psychiatric disorder, pre-deployment psychological and physical health, poor social support after a trauma, and personality pathology [23,102]. Our understanding of the relative contribution of each of these factors is still undeveloped.
Peri-deployment factors
Relevant peri-deployment factors include characteristics of the combat arena, intensity and duration of fighting, logistical/military support, and unit characteristics, and each combat deployment in the same cohort appears to have unique types of hazards [20,60], suggesting that deployment-specific stressors may contribute to the differences between groups.
A dose–response relationship between trauma intensity and PTSD severity has been hypothesized and has some empirical support [2,17,18,20,22,23,43]. For example, one study found that combat infantry units deployed to Iraq (n = 2530) reported significantly greater combat exposure than those deployed to Afghanistan (n = 3671), and accordingly the percentage who met screening criteria for major depression, generalized anxiety, or PTSD was significantly higher after duty in Iraq (15.6–17.1%) than after duty in Afghanistan (11.2%), or before deployment to Iraq (9.3%) [18]. Prevalence of PTSD was higher after deployment to Iraq (12.2–19.9%) than before (5.0–9.4%), and it increased in a linear manner as exposure to firefights increased (e.g. no firefights=4.5% PTSD prevalence; >5 firefights=19.3%). Similar findings have been replicated in a later US population-based study (n = 303 905) [17]. Iversen et al. also reported a strong association between time spent in a forward area and PTSD in UK soldiers deployed to Iraq [22]. Smith et al. also found that specific combat exposures, rather than mere war-zone deployment, were associated with PTSD in a population-based cohort of US military personnel (n = 50 184) [48].
The fact that most personnel exposed to combat do not develop PTSD, and that the dose–response relationship between combat and pathology is not always linear, obviously suggests that the development and course of PTSD is not solely determined by the features of the combat itself [20,22,65,67]. In fact, PTSD is highly dependent on cognitive appraisals of threat [103], and the risk of PTSD appears to be substantially reduced by high unit morale and good leadership in the war zone [22,23] and the perception of support and group cohesion among military personnel [23,67].
Post-deployment factors
Post-military factors also appear to contribute to course, presentation, and chronicity of PTSD [76]. These post-military factors have become central to the prevalence question, particularly in light of the latency between exposure and assessment seen in earlier research. Relevant post-military factors include individual symptoms, circumstances, stressors, and social support, as well as the post-deployment social and political environment.
Sociopolitical and cultural factors
Historical, contextual, and socioeconomic factors
The diagnosis of PTSD, first added to the DSM in 1980, was largely the result of attempts to account for the challenging impairment presented by Vietnam veterans at the time of homecoming [55,65]. In the immediate post-Vietnam era, compensation for significant functional impairment was difficult to obtain other than for observable physical injuries, and entrée to VA medical services was possible only via a ‘war-related’ disorder [56]. Thus, the development of the clinical conceptualization of PTSD has been heavily influenced by socioeconomic and political factors [55,104–106]. More recently there has been concern that health-care systems and disability policies encourage psychiatric illness. In fact, some argue that the US VA system has failed to benefit from the lessons of 20th century military psychiatry regarding social expectations and incentives [55,65,90,107–112]. Certainly recent administrative trends regarding PTSD disability claims are troubling. Among the relatively small subset of veterans seeking mental health treatment in VA clinics, most (up to 94%) also concurrently apply for PTSD disability benefits [113]. Further, the number of veterans receiving VA disability payments for PTSD increased 79.5% from 1999 to 2004, while all other disabilities increased only 12.2% during that same period [114]. Different compensation and support structures for veterans of non-US armed forces may partly explain different estimates of PTSD prevalence [16].
A particular concern is that veterans’ disability-seeking status may influence their clinical presentation in healthcare settings. Some veterans seeking evaluation in US VA medical centres may exaggerate, misrepresent or falsify their combat experiences [57,109,115], and some have created fictitious military service altogether [107,116–118]. Studies also show that veterans evaluated for PTSD in VA clinical settings may malinger or exaggerate psychiatric symptoms, especially when disability compensation is at stake [65,110,113,119–121]. Freeman et al. found that 53% of veterans in a PTSD treatment-seeking clinical sample appeared to have malingering psychopathology on a structured forensic psychiatric interview [120]. For a trenchant review of the effects of government disability pensions and benefits on veterans’ psychiatric functioning see Jones and Wessely [110].
The effect of disability-seeking for subjective ailments such as PTSD on the behaviour of claimants remains a significant issue in research and practice, and a matter of discussion among a number of US policy agencies [114,122]. Researchers conducting clinical trials have been encouraged to control for or exclude compensation-seeking veterans from clinical research [117,120,123]. The extent to which secondary gain may influence prevalence rates, however, is unclear and outcomes between clinical and community samples are not necessarily generalizable [1,13]. Although certain VA system policies or incentives may have an influence on treatment-seeking veterans (a small subset of all veterans), they may have relatively little impact on the larger veteran population represented in community samples. Thus, it is difficult to estimate how health care or other government policies might shape larger attitudes and reporting styles related to PTSD in community samples by influencing social attitudes and expectations.
Media and popular culture influences
Media stories and societal expectations influence symptom reporting and affect the validity of any retrospectively determined relationship between the trauma and psychiatric symptoms [46,62,89,92]. Research into significant historical events and memory recall has demonstrated that frequently repeated media-based narratives may reinforce inaccurate memories and beliefs about the event [60,92,124]. and the impact on help-seeking following a Hollywood glamorization of a psychologically tortured veteran can only be speculated upon [125]. Wessely and Jones cited the Vietnam War as an example where the public's changing opinion surrounding the war was likely to have influenced ‘a gradual “inflation” of traumatic memories to fit with the changing views’ (p. 12) [56]. See also Burkett and Whitley [107], Shephard [55], Jones and Wessely [110], McHugh and Triesman [126], and Satel and Frueh [105] for further discussion.
PTSD onset and course
The vast majority of combat veterans do not ever develop PTSD. Further, studies that estimate both lifetime and current prevalence of PTSD typically find that approximately half of the veterans who had PTSD at some point in the past do not meet diagnostic criteria for current PTSD [2,3,25,34,41,85]. In contrast, retrospective studies in samples of Holocaust survivors [127], Korean war veterans [128], Lebanon War veterans [129] and World War II veterans [130–132] indicate that the duration of ‘chronic PTSD’ can span an entire adult lifetime; up to 50 years after combat exposure [133]. The phenomenon of delayed-onset PTSD remains somewhat controversial. Although there is some empirical evidence to support the phenomenon [61], a recent review of delayed-onset PTSD found that the phenomenon in the absence of prior symptoms was rare [134]. In fact, one recent study found that delayed-onset PTSD was extremely rare among veterans more than 1 year after combat exposure, and there was no evidence of PTSD symptom onset ≥6 years after combat [135].
Symptom overlap with other psychiatric disorders
While Criterion A ‘the traumatic event’ [136], is a unique requirement for a DSM-IV PTSD diagnosis compared to other psychological disorders, PTSD is classified as an anxiety disorder and conceptually shares a significant overlap between symptoms of other mood and anxiety disorders. This overlap may partially account for the high comorbidity evident in PTSD [121]. High comorbidity of PTSD with psychiatric and medical diagnoses has been well documented, including high rates of comorbid substance abuse, anxiety, mood, and personality disorders [3,30,52,95,132,137–139]. The high degree of symptom overlap between PTSD and other Axis I psychiatric disorders has been suggested to indicate a problem with the conceptual foundation of the disorder, one of a number of challenges raised recently regarding the question of whether PTSD is actually a distinct and unique form of psychopathology [57,86,126,140,141].
Conclusions
The point prevalence of combat-related PTSD in studies of US military veterans ranges from approximately 2% to 17%, and the range tends to have a lower ceiling and is more narrow among veterans of other Western nations. There is considerable variability in rates of prevalence due to differences in sampling strategies; measurement strategies (e.g. use of structured psychiatric interviews versus self-report measures); inclusion and measurement of the DSM-IV clinically significant impairment criterion; latency of assessment and potential for recall bias; and the combat experience (including deployment factors, and pre-, peri-, and post-deployment factors). Prevalence rates are also likely affected by issues related to PTSD course, chronicity, and comorbidity; symptom overlap with other psychiatric disorders; and sociopolitical and cultural factors. Regardless of the true prevalence of combat-related PTSD, the disorder is associated with severe functional impairment (both occupational and social), high comorbidity with other psychiatric disorders, high medical comorbidity, and/or reduced quality of life for the veterans who suffer from it. Thus, it represents a significant and costly illness to veterans, their families, and society as a whole. Further methodologically rigorous research is needed to better elucidate our understanding of the prevalence, course, phenomenology, protective factors, and costs associated with combat-related PTSD.
Footnotes
Acknowledgements
This work was partially supported by Australian– American Fulbright Commission Postgraduate Award to Ms Richardson; Grant MH074468 from the National Institute of Mental Health to Dr Frueh; and awards from the McNair and Menninger Foundations to Dr Frueh. We thank Steve Herrera for his technical assistance. All views and opinions expressed herein are those of the authors and do not necessarily reflect those of our respective institutions or the US Department of Veterans Affairs.
