Abstract
From August 2016 to June 2018, a total of 7 patients underwent lateral ventriculo-superior sagittal shunt surgeries in our hospital. All cases were followed up for 3 months to 2 years after the surgeries. The results of their head CT scans or MRI scans indicated that the conition of hydrocephalus generally improved, and the symptoms of intracranial hypertension significantly improved or disappeared. The superior sagittal sinus shunt surgery for hydrocephalus is simple to operate and also safe and effective, and it's an important method of treatment for hydrocephalus. This article described the specific surgical procedure for lateral ventriculo-superior sagittal shunt surgery in detail so that this surgical procedure can be better promoted.
From August 2016 to June 2018, a total of 7 patients underwent lateral ventriculo-superior sagittal shunt surgeries in our hospital. All patients had undergone lateral ventriculo-peritoneal fluid shunt surgeries before, which all failed due to the occurrence of various post-surgical symptoms including abdominal infection, intracranial infection, and abdominal absorption disorder. For some patients, the hydrocephalus had not been cured after undergoing multiple shunt adjustment surgeries. Therefore, all the 7 patients underwent lateral ventriculo-superior sagittal shunt surgeries as well as follow-up diagnoses and examinations for the next 3 months to 2 years after the surgeries. The results of their head CT scans or MRI scans indicated that the condition of hydrocephalus generally improved, the symptoms of intracranial hypertension significantly improved or disappeared, and the shunts were unobstructed with no occurrence of serious complications including shunt obstruction, infection of shunt system and cerebral venous sinus thrombosis. The superior sagittal sinus shunt surgery for hydrocephalus is simple to operate and also safe and effective. It is an important method of treatment for hydrocephalus, and especially an effective remedy for the failure of lateral ventriculo-peritoneal fluid shunt surgery [1].
Hydrocephalus is one of the common diseases in the field of neurosurgery, and the most important method of treatment for hydrocephalus is endoscopic third ventriculostomy and fluid shunt surgeries [2], with ventriculo-peritoneal fluid shunt surgery being the most common type of fluid shunt surgery. In 1965, Sharkey first reported his success in performing superior sagittal sinus shunt surbery for the treatment of obstructive hydrocephalus [1]. This surgical procedure is in line with the effort to greatly shorten the drainage pathway, and introduces cerebrospinal fluid directly into the blood circulatory system from the ventricle, which is in line with the reasonable physiological processes [3], and to a large extent, avoids all the common complications caused by several other common fluid shunt surgeries and demonstrates its outstanding advantages. In recent years, there have been an increasing number of reports of lateral ventriculo-superior sagittal shunt surgeries for hydrocephalus, but the specific surgical procedures vary in various reports and are not described in detail. Through the previous surgical experience of our hospital combined with reports from other hospitals, we hope that this article will enable more neurosurgeons to understand more clearly the specific surgical procedure for lateral ventriculo-superior sagittal shunt surgery so that this surgical procedure can be better promoted.
Surgical method and procedure: We choose the Medtronic adjustable pressure shunt whose proximal end towards the sagittal sinus features an anti-reflux fissure umbrella, and this design can prevent the blood from flowing back into the shunt lumen, which is the main reason we choose the Medtronic shunt for our surgery. The shunt pump should be adjusted to the appropriate pressure based on the patient's preoperative intracranial pressure, and the intrinsic internal venous pressure of the superior sagittal sinus ranging from 5–10 cm H2O should also be taken into consideration when setting the pressure. The patients undergo general anesthesia and lie in the supine position, and two roughly 3 cm-long scalp incisions are made (see
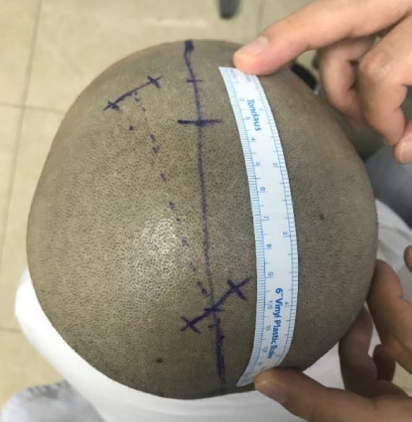
Design of surgical incisions.
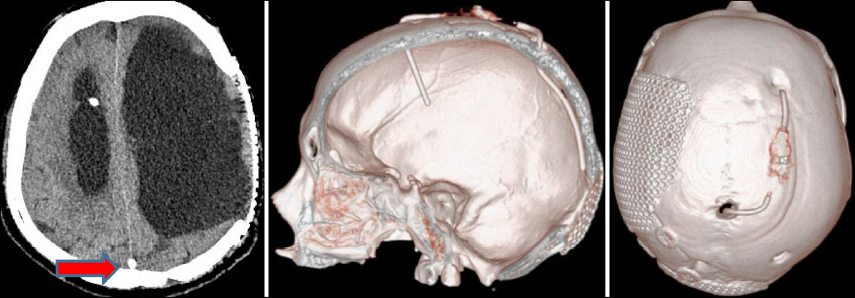
Image of post-surgical CT scan and 3D reconstruction of the sagittal sinus shunt (the arrow shows the proximal end of the fluid shunt towards the sagittal sinus).
Although the ventriculo-sagittal sinus shunt surgery has its outstanding advantages, it also has some disadvantages, especially the likelihood of occurrence of insufficient fluid shunting to patients with normal pressure cranial hydrocephalus and low pressure hydrocephalus after the intracranial pressure surgeries [4].
In recent years, there have been an gradually increasing number of reports of the ventriculosagittal sinus shunt surgeries, while the choice of the types of shunt pumps, as well as the position, direction and length of the placement of the proximal end of the fluid shunt towards the sagittal sinus all vary in different hospitals and demonstrate their own advantages and disadvantages [5,6]. This article only describes the detailed procedure and basic principles of the surgery in our hospital, and it still takes a longer time for the further follow-up observations to determine which method is better.
Footnotes
All contributing authors have no conflict of interests.
