Abstract
Various imaging modalities have been exploited and are successfully employed to investigate the anatomic or functional dissemination of tissues in the body. However, no single imaging modality allows overall structural, functional, and molecular information as each imaging modality has its own unique strengths and weaknesses. The combination of two popular imaging modalities that investigates the strengths of different methods might offer the prospect of improved diagnostic and therapeutic monitoring abilities. To date, only a few hybrid systems have become clinically adopted, but there are encouraging signs that the new generation of multimodality systems will be undergoing evaluation in the near future. On the other hand, significant progress has been made toward the creation of dual-modality imaging probes, which can be used as novel tools for future multimodality systems. The interdisciplinary research that couples molecular imaging science to nanotechnology has generated synergistically integrated novel dual-modality imaging probes. These all-in-one probes take full advantage of two different imaging modalities and could provide unique information that impacts preclinical and, eventually, clinical diagnostics. This review discusses the advantages and challenges in developing dual-modality imaging probes and summarizes the current state-of-the-art systems with respect to their unique design strategies and applications.
CURRENT IN VIVO IMAGING is one of the primary tools used to evaluate structure and function noninvasively in a living subject. Various imaging modalities, including optical bioluminescence/fluorescence, positron emission tomography (PET), single-photon emission computed tomography (SPECT), magnetic resonance imaging (MRI), magnetic resonance spectroscopy (MRS), computed tomography (CT), and ultrasonography (US), are all successfully employed to investigate the anatomic or functional dissemination of tissues in the body. In many cases, contrast in vivo imaging is generated by contrast agents, designed to provide or augment the imaging signal depending on the modality, for example, fluorophores for optical imaging, radioisotopes for PET and SPECT, paramagnetic agents for MRI, high-density molecules for CT, or acoustically active microbubbles for US.1 Using different types of contrast agents with various modalities, an enormous variety of parameters can be imaged, ranging from tissue density to specific molecular targets in vivo. These conventional probes show somewhat improved results in vivo, but they also tend to be nonspecific and unstable. More importantly, these materials are not sufficient to support the growing public demand for future diagnosis and therapy.
For these reasons, there has been considerable interest over the past 15 years in examining the possibility of more sophisticated imaging systems. Each imaging modality operates within defined parameters, such as detection sensitivity, tissue-penetrating depth, spatial resolution, temporal resolution, three-dimensional tomography, accuracy, and cost. For instance, PET has high target sensitivity but relatively poor spatial resolution, whereas MRI and CT can provide three-dimensional tomography but are limited by low target sensitivity. In contrast, optical imaging has relatively good sensitivity but suffers from low tissue penetration, whereas US has high spatial resolution but is limited by relatively low penetration and sensitivity. Because no single imaging modality can provide overall structural and functional information, an obvious approach is to combine two or more of these imaging methods together. A great effort has been made in the field of multi-modality systems; however, only a few hybrid instruments have become adopted. PET-CT and SPECT-CT2,3 have been successfully integrated and widely adopted in the clinic, and the PET-MRI system4,5 was recently introduced. Many others are under active development. There are only a few single multi-modality imaging instruments available that can be used for two different modalities. Until now, separate images acquired from two closely placed instruments have been integrated by software for further analysis. Although the development of multimodality imaging systems has been slow, significant progress has been made toward the creation of multimodality imaging probes. Recent advances in nanotechnology and imaging science have provided researchers with new tools for molecular imaging. Molecular imaging is now paving the way for powerful techniques aimed at extending existing or developing novel methods to characterize and measure specific molecular events in vivo, particularly those that play key roles in the disease process.6–8
Molecular imaging technology has enabled the development of a new generation of imaging probes. These sophisticated molecular imaging probes can visualize biologic processes or diagnose disease early in vivo. The progress of molecular imaging is becoming more and more dependent on the development of multifunctionalized novel imaging probes. The use of molecularly targeted imaging probes affords many advantages over conventional contrast agents. For instance, labeling of multiple targeting motifs, including peptides, proteins, or small molecules, provides enhanced binding affinity and specificity in vivo. The use of novel metals or biopolymers improves the physiochemical properties and delivery efficiency of conventional contrast agents. More importantly, combining various radioisotopes, fluorophores, and materials such as biopolymers, peptides, small molecules, and novel metals has significantly impacted the range of available imaging probes and profoundly improved the performance of existing imaging modalities (Figure 1).

Schematic diagram of dual-modality imaging probes. Radioactive isotopes, magnetic particles, fluorophores, and targeting motifs can be integrated into all-in-one systems in various combinations. NIR = near-infrared; NP = nanoparticle; QD = quantum dot.
Several review articles have discussed recent advances in and applications of single-modality molecular imaging probes for diverse imaging techniques.9,10 The present article summarizes the most recent reports on dual-modality molecular imaging probes that were designed based on dual-labeling techniques. The review focuses on molecular imaging probes that combine two or more modalities and does not discuss probes for single-modality or multimodality imaging systems combined via a hardware approach, which have been summarized elsewhere. 11 Instead of preparing two different imaging agents that are distributed differently in the body and complicating data fusion, dual-modality probes possess the signaling moieties for the two imaging systems into one molecule. Various combinations of dual labels for different imaging modalities can be designed in an all-in-one system, for PET-MRI, PET-optical imaging, PET-CT, PET-US, or MRI-optical imaging. These synergistically integrated dual-modality molecular imaging probes will be essential tools in multimodality in vivo imaging in the near future. Herein we discuss the unique concepts, characteristics, and applications of the various dual-modality molecular imaging probes available today.
Nuclear and MRI Combinations
Imaging modalities can be divided into two groups: those that provide structural information (ie, MRI, CT, and US) and those that provide functional or molecular information (ie, PET, SPECT, MRS, and optical imaging). Therefore, it is not surprising that much effort has been devoted toward combining one modality from each group, thus enabling function and structure to be examined at the same time. Radionuclide imaging such as PET has high target sensitivity but poor spatial resolution because of the absence of identifiable anatomic structures, particularly in the abdomen. 12 Although simultaneous PET-CT scanning used in clinical imaging aids in the accurate localization of regions of increased activity on PET, the combination of PET with MRI may also offer significant advantages. This combination of imaging modalities might find ways to take advantage of the high spatial resolution and excellent morphologic discrimination of MRI and the exquisite sensitivity of nuclear imaging in both preclinical and clinical settings. 13 Currently, spatial registration of independently acquired PET and magnetic resonance images is performed retrospectively and can partially analyze nonrigid tissue deformation, which can occur between the two images. 14 Several prototype PET-MRI systems have been successfully implemented for both small-animal and human imaging.4,5 Although clinical applications of such technology are still under debate, a few dual-modality imaging probes for PET-MRI systems have already been developed for future diagnostic applications.
The use of a 124I serum albumin (SA)-MnMEIO dual-imaging PET-MRI probe for imaging the sentinel lymph node is a good example. 15 The lymphatic system is a biologic defense system against infection and is also used as a passage in cancer metastasis. 16 Thus, accurate imaging of lymph nodes is critical for the diagnosis and treatment of cancer. Choi and colleagues developed a PET-MRI probe for lymph node imaging by combining radioactive iodide ions into the innate tyrosine residue of SA that were then coated onto the surface of MnMEIO magnetic nanoparticles (Figure 2A). 15 MnMEIO is a magnesium-engineered iron oxide nanoparticle that has a two- to threefold better magnetic resonance contrast effect compared with superparamagnetic iron oxide (SPIO) nanoparticles. 17 124I-SA-MnMEIO maintained equivalent contrast effects corresponding to the probe of each imaging modality without any interference between magnetic nanoparticles and radioactive iodide ions. When 124I-SA-MnMEIO nanoparticles were injected into the front paw of a mouse, brachial lymph nodes located deep inside the body were clearly imaged, as shown in Figure 2. PET visualized an intense red spot from the brachial lymph nodes without anatomic information (Figure 2B). In the MRIs, the anatomic upper body shape was clearly obtained in addition to a few dark spots identified as potential lymph nodes (Figure 2C). When these two images were overlaid, the accurate positioning of brachial lymph nodes in the context of the anatomic shape of a rat was clearly achieved (Figure 2D). However, this 124I-SA-MnMEIO nanoparticle system will need further in vivo studies after systemic administration prior to additional medical applications. A similar example, 64Cu-labeled dextran sulfate-coated SPIO, has been reported for atherosclerotic plaque imaging; however, noninvasive in vivo imaging has not yet been achieved. 18

A, Schematic diagrams of a 124I-SA-MnMEIO PET/MRI dual-modality probe. Chemically conjugated iodine ions serve for PET and MnMEIO for MRI, respectively. In vivo PET-MRI: 124I-SA-MnMEIO is injected into the forepaw of a rat for the lymph node imaging, (B) PET image, (C) MRI, and (D) PET-MRI fusion image. The white circle denotes the location of a brachial lymph node. Adapted with permission from Choi JS et al. 15 Copyright 2008, Wiley-Liss, Inc., a subsidiary of John Wiley & Sons, Inc.
A simple combination of radionuclide and magnetic nanoparticles shows the complementary nature of PET and MRI; however, the addition of tumor targeting motifs to hybrid dual-modality imaging probes could provide more specific cancer imaging. We recently created a novel bifunctional nanoprobe for dual PET-MRI of tumor integrin αvβ3 expression. 19 Integrin αvβ3, a cell adhesion molecule, is a viable target for noninvasive imaging of cancer and other angiogenesis-related diseases. Integrin αvβ3 plays an important role in tumor progression, angiogenesis, and metastasis.20,21 Integrin αvβ3 is overexpressed on both tumor vasculature and tumor cells but is not readily detectable in resting endothelial cells and most normal organs. 22 For these reasons, integrin αvβ3 has been widely used as an excellent target for imaging purposes. Integrin αvβ3 binds extracellular matrix molecules such as vitronectin, which contain the amino acid sequence arginine-glycine-aspartate (RGD). The RGD peptide strongly binds with an integrin αvβ3; thus, most imaging probes targeting integrin αvβ3 have been designed based on the RGD motif. 23 Indeed, we have reported various RGD-based probes with PET and near-infrared (NIR) fluorescence imaging by labeling of 18F, 24 NIR dyes, 25 and semiconductor quantum dots (QDs) 26 to cyclic RGD analogues, respectively. The RGD-based PET-MRI probe has a chelating moiety (1,4,7,10-tetraazacyclododecane-N, N′, N″, N‴-tetraacetic acid [DOTA]) on the surface of polyaspartic acid-coated iron oxide (PASP-IO) nanoparticles and is chemically conjugated with cyclic RGD peptide for integrin αvβ3 recognition (Figure 3A). The PASP-IO nanoparticles had a core size of 5 nm and a hydrodynamic diameter of about 45 nm. The particles were easily functionalized with DOTA for 64Cu chelation and RGD peptide for targeted delivery. DOTA-IO-RGD conjugates were found to bind specifically to an integrin αvβ3-positive U87MG cells on the basis of displacement competitive binding assays. When intravenously administered in U87MG tumor-bearing mice, both small-animal PET and T2-weighted MRI showed integrin-specific delivery of DOTA-IO-RGD nanoparticles (Figure 3, B-D). The success of this approach may allow for early clinical tumor diagnosis with a high degree of sensitivity while providing anatomic and molecular information specific to the tumor of interest.

A, Schematic diagram of an integrin αvβ3 targeting 64Cu-DOTA-IO-RGD PET/MRI dual-modality probe. B, A two-dimensional projection micro-PET image of a mouse bearing an integrin αvβ3-positive U87MG tumor at 4 hours postinjection of the probe. T2-weighted MRIs of mice (C) before and (D) 4 hours after intravenous injection of the probe. The arrow indicates the tumor. Adapted with permission from Lee HY et al. 19 Copyright 2008, by the Society of Nuclear Medicine, Inc.
Despite the ability of a PET-MRI dual-modality probe to provide complementary imaging information obtained from the two detection systems, there are concerns about the practical use of the probes. Ideally, a PET-MRI dual-modality probe would have optimal characteristics for both instruments. However, PET is a highly sensitive imaging modality that requires the introduction of only a trace amount of probes, whereas MRI is relatively insensitive and needs high doses of the same dual-modality probe to be injected. Therefore, the detection sensitivities for the different imaging modalities should be further considered and optimized. Integrated PET-MRI imaging systems are still at early stages of development.27,28 With the development of newer MRI systems with much improved sensitivity and the improvement in PET-MRI fusion, rationally designed PET-MRI dual-modality imaging probes will likely have more applications.
Nuclear and Optical Combinations
Research is under way to couple PET or SPECT and optical imaging to allow multimodal functional and molecular imaging.29,30 The development of a nuclear-optical imaging system is valuable because of the opportunity to obtain complementary data from two similar contrast mechanisms within the same device. 29 With the use of nuclear-optical imaging probes, we can take full advantage of the unique high detection sensitivity of both nuclear and optical systems instead of preparing different imaging probes. Because optical imaging can provide micron-level spatial resolution and can be used to cross-validate nuclear images, several applications can be adopted in clinical practice. For instance, nuclear imaging can provide a whole-body image and localize disease tissue, whereas the fluorescence component can validate biopsied tissues or serve as a visual guide during surgery. Although a combined nuclear-optical imaging system is in its infancy, several peptide-, small molecule-, and antibody-based dual-modality imaging probes for multimodality systems have already been reported.
Small peptide ligands represent a class of potential targeting unit candidates for imaging because they have a well-defined chemical structure, can be easily synthesized by solid-phase peptide chemistry, and possess relatively short clearance when employed as imaging agents in vivo. 31 An example of a peptide-based dual-modality imaging probe that allows both nuclear and optical imaging has been reported by Li and colleagues. 32 They synthesized 111In-DTPA-Lys(IRDye800)-c(KRGDf), composed of both an 111In chelator, diethylenetriaminepentaacetic acid (DTPA), for nuclear imaging and a NIR fluorescent dye, IRDye800, for optical imaging. The dual-labeled probe inhibited the adhesion of melanoma M21 cells to the vitronectin-coated surface while maintaining the moderate biologic activity of the RGD motif. In addition, the probe showed higher uptakes in an integrin αvβ3-positive M21 melanoma than in an integrin αvβ3-negative M21-L melanoma after intravenous injection. Both optical imaging and gamma scintigraphy enabled noninvasive detection of the bound probe to integrin αvβ3-positive tumors. Similar strategies have been adopted and designed for targeting interleukin-11 receptor α chain (IL-11Rα). 33 Interleukin 11 (IL-11) is a multifunctional cytokine that belongs to a family of pleiotropic and redundant cytokines that use the glycoprotein 130 transducing subunit in their high-affinity receptors. It has been shown that IL-11 and its receptor, IL-11Rα, are related to breast cancer development and progression and may play an important role in the bone metastasis of human breast cancer.34,35 Moreover, IL-11 is reported to be a predictor of poor prognosis of breast cancer. 36 Thus, IL-11Rα can be used for in vivo targeting for cancer diagnostics. Wang and colleagues developed DLIA-IL-11Rα as a dual-imaging probe targeting IL-11Rα. DLIA-IL-11Rα consists of the cyclic peptide cyclic(Cys-Gly-Arg-Arg-Ala-Gly-Gly-Ser-Cys), which is known to target IL-11Rα, 37 111In-DTPA as the radiotracer moiety, and IR-783 as a NIR fluorescent dye for optical imaging. DLIA-IL-11Rα continued to possess the targeting capability to IL-1Ra-positive breast cancer cell lines, MDA-MB-231 and MDA-MB-231-1833, respectively. In a human breast cancer xenograft model, DLIA-IL-11Rα showed specific binding in the tumor region, and images acquired by optical and radionuclear methods were consistent. 37
Small molecules have also been applied to develop dual probes for breast cancer microcalcification imaging based on bisphosphonates (BPs). BPs bind to the hydroxyapatite (HA) bone mineral surface, 38 and BP-based radiotracers are used to image osteoblastic bone lesions and to treat the bone metastasis associated with breast cancer. 39 Bhushan and colleagues reported a BP-based dual-imaging probe that used SPECT-CT and optical imaging. 40 The Pam-Tc/Re-800 probe possesses a bifunctional BP as a targeting ligand, a 99mTc chelating agent, and an IRDye800 for SPECT and optical imaging, respectively (Figure 4A). Pam-Tc/Re-800 showed eightfold increased specificity for HA over other calcium salts found in the body and permits SPECT-CT and NIR fluorescence detection of HA with high sensitivity. In vivo imaging capability was investigated in the syngeneic rat model of breast cancer microcalcification based on ectopic expression of adenovirus-expressed bone morphogenetic protein 2.

A, Chemical structure of a Pam-Tc/Re-800 SPECT/MRI dual-modality probe. Bisphosphonate (BP) binds avidly to hydroxyapatite (HA), a marker of breast cancer microcalcification. In vivo imaging of rat breast cancer microcalcification 4 h after intravenous injection of the probe in a breast cancer microcalcification model. Intraoperative near-infrared (NIR) fluorescence optical imaging (B) and SPECT-CT (C). Arrows indicate the location of breast cancer microcalcification. Adapted with permission from Bhushan KR et al. 40 Copyright 2008, American Chemical Society.
Simultaneous imaging of breast cancer microcalcifications was performed by both SPECT-CT and a custom intraoperative optical imaging system 4 h post injection. As shown in Figure 4, B and C, breast cancer microcalcifications were observed with high signal to background ratios in optical and SPECT images, respectively, and Pam-Tc/Re-800 acted as a bone-seeking dual probe with higher uptake in skeleton and microcalcified tumors than in other organs and tissues. Although direct peptide- and small molecule-based dual-labeled probes showed promising results in vitro and in vivo, these probes tend to be unstable and rapidly cleared. More importantly, biologically active peptides generally lack sites permitted for chemical modification without significantly affecting their biologic activities.
Modern inorganic and polymer chemistry and imaging science have yielded new strategies for designing nanomaterial-based imaging probes that efficiently detect target molecules or diagnose diseases.9,41,42 Such probes have large surface areas, which are ideal for efficient surface modification with a wide range of imaging moieties, improved stability, and enhanced targeting. Our group developed QD-based dual-modality probes for both PET and optical imaging. 43 QDs are inorganic fluorescent semiconductor nanoparticles with superior properties for optical imaging compared with those of conventional organic fluorophores, such as high quantum yields, strong resistance to photobleaching and degradation, and large surface areas for chemical modifications. 44 QD surface modification with enriched RGD peptides allowed for strong integrin αvβ3 targeting, and DOTA conjugation enabled PET imaging after 64Cu labeling. It was found that the majority of the probe in the tumor was within the vasculature, as evidenced by the strong overlay of the QD fluorescence signal and vasculature integrin αvβ3 staining. 26 This dual-modality probe showed sufficient tumor contrast in an integrin αvβ3-positive U87MG tumor-bearing mice with a tumor to muscle ratio of 4. There was an excellent linear correlation between the results measured by in vivo PET and those measured by ex vivo optical imaging and tissue homogenate fluorescence. Furthermore, PET allowed us to use the probe at a concentration much lower than that required for in vivo optical imaging; this dual-modality probe has significantly reduced the potential toxicity of QDs.
Dual-labeled antibody has been used to image breast cancer in vivo. The human epidermal growth factor receptor (HER) is a member of the epidermal growth factor family of extracellular protein ligands. 45 The HER consists of transmembrane receptor tyrosine kinases that regulate complex intracellular signaling networks to control normal and pathologic cellular growth, differentiation, and survival. 46 Among various HER families, overexpression of HER2 is an important prognostic factor associated with an aggressive tumor progression and poor prognosis in breast cancer. Trastuzumab (Herceptin, Genentech, San Francisco, CA) is a humanized anti-HER2 antibody that acts on the HER2 signaling and is approved clinically as an anticancer therapy in breast cancer whose tumors overexpress HER2.47,48 Given that the presence of HER2 on the plasma membrane of cells has also made it a potential target for cancer diagnostics, several investigators have developed various imaging probes by labeling intact and fragments of trastuzumab with different contrast agents to image HER2-overexpressing tumors. 49 Sampath and colleagues developed a dual-labeled antibody (Figure 5A), (111In-DTPA)n-trastuzumab-(IRDye800)m, and demonstrated imaging specificity for HER2 in vitro and HER2-overexpressing tumors in vivo. 50 The binding of (111In-DTPA)n-trastuzumab-(IRDye800)m to SKBr3 cells that overexpress HER2 indicated that local expression of HER2 is present only along the outer rim of the cell (see Figure 5A). In vivo, this dual-imaging probe successfully identified HER2-overexpressing tumors by both planar NIR fluorescence imaging and SPECT from SKBr3 tumor-bearing mice after intravenous administration (Figure 5, B and C).
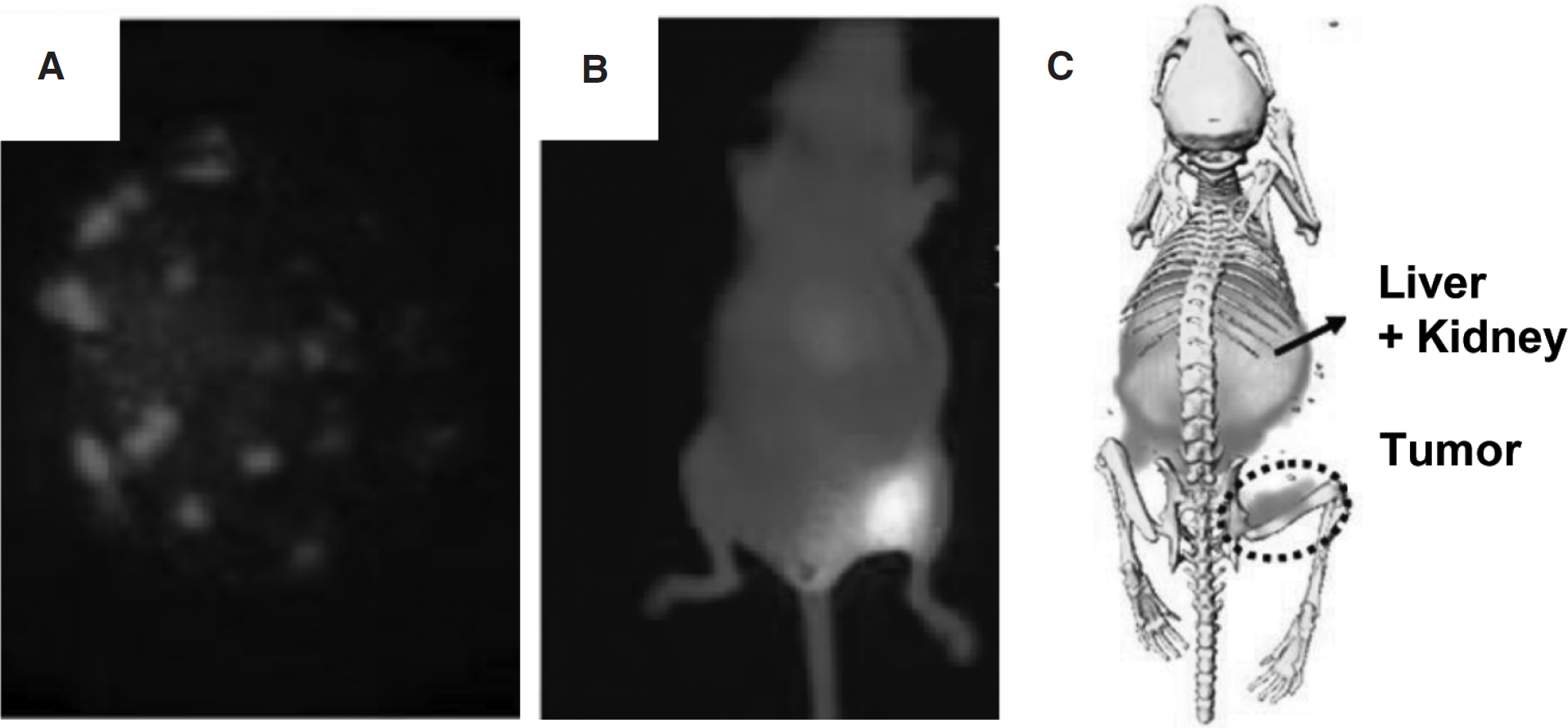
A, Fluorescence microscopy imaging shows significant binding of (111In-DTPA)n-trastuzumab-(IRDye800)m in HER2-overexpressing SKBr3 cells. In vivo imaging of SKBr3-Luc tumor-bearing mice 48 h after intravenous injection of the probe, (B) near-infrared fluorescence optical imaging and (C) three-dimensional SPECT integrated for 20 minutes. Adapted with permission from Sampath L et al. 50 Copyright 2007, by the Society of Nuclear Medicine, Inc.
The dual-modality tumor-targeting imaging probes described herein allow cross-validation and direct comparison between radionuclide and fluorescence optical imaging. Even though radionuclide imaging and optical imaging have comparable sensitivity, dual-modality nuclear and optical imaging studies have been predominantly done with small animals, presumably owing to the limited penetration depth of fluorophores. Combining nuclear imaging for high sensitivity at deep tissue detection and optical imaging for enhanced resolution could allow comprehensive visualization of the probe distribution and provide a rapid and efficient imaging method for basic research and potential clinical applications.
MRI and Optical Imaging Combinations
MRI employs nonionizing radiation and has become an integral tool in clinical radiology and in experimental settings. Different relaxation times of tissue results in endogenous contrast and exogenous contrast agents can further enhance images by selectively shortening either the longitudinal (T1) or transverse (T2) relaxation time. 51 MRI provides three-dimensional tomographic images and a submillimeter level of higher spatial resolution. Magnetic resonance contrast agents act predominantly by shortening either T1 or T2. T1-shortening agents (paramagnetic or positive contrast agents) increase the signal intensity of T1-weighted imaging parameters, whereas T2-shortening agents (superparamagnetic or negative contrast agents) decrease the signal intensity of T2-weighted imaging parameters. Currently, various positive and negative magnetic resonance contrast agents have been reported, such as paramagnetic gadolinium-containing liposomes, SPIO nanoparticles, and MnMEIO nanoparticles.17,52 A significant limitation of MRI is the inherent low sensitivity of the probes that makes validation of in vivo imaging by more than one approach essential. To take advantage of MRI combined with the benefits of other imaging modalities, growing attention has focused on the development of dual-imaging probes. Besides PET-MRI as described, MRI-optical imaging also provides a powerful way to validate in vivo molecular targets. MRI-optical imaging combines the high spatial- temporal resolution and deep tissue penetration of MRI with the high sensitivity of the optical methods.
Among the numerous multimodality imaging probes, nanoparticles for MRI and optical imaging are probably the most frequently studied. Magnetic resonance-detectable and fluorescent liposomes carrying RGD peptides 53 and cross-linked iron oxide (CLIO) nanoparticles have been loaded with Cy5.5 NIR fluorescent dyes either via an enzyme-cleavable linker 54 or with additional targeting ligands, such as antivascular cell adhesion molecule antibodies, 55 E-selectin binding peptides, 56 or annexin V. 57 They have been extensively reviewed elsewhere. 51 These dual-imaging probes showed promising proof of concept; however, most of the studies could not be carried out simultaneously with both MRI and optical imaging, likely owing to the low sensitivity of MRI or limited tissue penetration of light even in the NIR region. Lee and colleagues reported thermally cross-linked superparamagnetic iron oxide (TCL-SPIO) nanoparticles and their application to the dual imaging of cancer in vivo. 58 Unlike dextran chemically CLIO nanoparticles, TCL-SPIO nanoparticles are fabricated by a thermal cross-linking method using a Si-OH-containing polyethylene glycol (PEG)-grafted copolymer (Figure 6A). The polymer employed in the study was composed of a surface-reactive function (−Si(OH)3) for further customized modification and a protein-repelling function (PEG). When Cy5.5 TCL-SPIO nanoparticles were intravenously administered to Lewis lung carcinoma tumor-bearing mice, the tumor was unambiguously detected in T2-weighted MRIs and in optical images within 4 hours (Figure 6, B and C). Interestingly, TCL-SPIO nanoparticles do not possess any tumor-targeting ligands on its surface; its efficiency in detecting tumors in vivo may be due to the enhanced permeability and retention (EPR) effect achieved by the antibiofouling and stable polymer coating layers. 59

A, Schematic diagram of thermally cross-linked iron oxide nanoparticles, Cy5.5 TCL-SPIO MRI-optical imaging dual-modality probe. In vivo imaging of LLC tumor-bearing mice 3.5 h after intravenous injection of the probe, (B) T2-weighted fast spin-echo image and (C) near-infrared (NIR) fluorescence optical imaging. The red arrows indicate the tumor. Adapted with permission from Lee H et al. 58 Copyright 2008, American Chemical Society. PEG = polyethylene glycol.
The nanoparticle structures of most negative MRI contrast agents generally allow simple surface modification by embedding them in functionalized polymers or by grafting fluorescent dyes or targeting moieties. On the other hand, the development of dual-modality-positive MRI probes seems impeded because they were mainly based on the chelates of metal ions with a large number of unpaired electrons, such as Gd3+, and their molecular structures. Furthermore, the nonspecificity of metal complexes and their short rotational correlation time limit the proton relaxivity. 60 Various strategies were introduced aimed at the preparation of Gd3+-based agents with improved stability and functionality by using biocompatible polymers, 61 nanoparticles, 62 or QDs. 63 As a consequence of their diverse structures, contrast agents were simply functionalized by targeting groups or fluorescent dyes. Besides the multiple chemical conjugations of metal chelating groups, Bridot and colleagues developed novel hybrid gadolinium oxide nanoparticles (5–10 nm) for MRI-optical imaging. 64 It has been reported that crystalline gadolinium oxide nanoparticles exhibit higher relaxivities than the gadolinium chelates. 65 These hybrid nanoparticles were synthesized by encapsulation of paramagnetic Gd2O3 cores within a polysiloxane shell, which carries fluorescent dyes for optical imaging and PEGs for improved in vivo stability and reduced undesirable organ accumulation. The gadolinium oxide core induces an enhancement of the positive contrast of MRIs compared with widely used positive MRI agents such as Gd-DTPA followed by fluorescence imaging. Consequently, dual-imaging probes were suited for MRI-optical imaging and freely circulate in the blood vessels without undesirable accumulation in the lung and liver. Although the probe has not been tested in tumor models, it can be expected that these particles could show enhanced tumor accumulation by the EPR effect. As described in the previous section, an optimization process of combined characteristics for both MRI and optical imaging is needed. A relatively high amount of contrast agent needed for MRI in the current systems limits the unique sensitivity of the optical imaging modality.
Other Multimodality Imaging Combinations
CT is widely used for diagnosis because radiography can go across the human body and the internal anatomic structures can be externally visualized. 66 Generally, iodinated molecules are applied as contrast agents for CT owing to the high x-ray absorption coefficient of iodine. 67 Current CT contrast agents such as iodine-based compounds have several limitations, including short imaging times owing to rapid renal clearance, renal toxicity, and vascular permeation. Recently, the use of dense nanoparticles as contrast agents for CT was proposed. For instance, a polymer-coated Bi2S3 nanoparticle was reported as an injectable CT contrast agent with a fivefold increase in x-ray absorption compared with iodine and improved circulation times in vivo. 68 Gold nanoparticles were also efficiently applied in vivo as CT contrast agents. 69 PEG-coated gold nanoparticles showed x-ray absorption comparable to that of iodine molecules and successfully accumulated in hepatoma-bearing rats after intravenous administration. 70 Despite the ubiquitous nature of CT in the clinical setting, the development of novel dual-modality imaging probes for CT receives little attention owing to the lack of efficient contrast molecules. Gold nanoparticles might be attractive candidates for dual-modality probes for CT because it is easier to control the size, shape, and surface modification. Alric and colleagues reported gadolinium chelate-coated gold nanoparticles as dual-imaging probes for CT-MRI. 71 They synthesized these particles by encapsulating gold nanoparticles within a multilayered DTPA shell, which is composed of gadolinium chelates bound to each other through disulfide bonds. The Au@DTDTPA-Gd nanoparticles showed dose-dependent x-ray absorption properties and relaxivities. The particles freely circulated in the blood pool without undesirable accumulation in the lung, liver, and spleen followed by either radiography or MRI. Given that surface modification of gold nanoparticles can be achieved by covalent grafting of targeting moieties, targeted Au@DTDTPA-Gd dual-imaging probes can be developed.
US is the most commonly used clinical imaging modality because of its safety, low cost, ease of use, and wide availability. 72 US contrast agents are generally in the form of small, acoustically active microbubbles ranging from several hundred nanometers to a few micrometers in diameter. 73 Targeted microbubbles are rapidly emerging as a quantitative molecular imaging method by taking advantages of its high spatial resolution and lack of ionizing radiation. Targeting is accomplished either through modifying the chemical structures of the microbubble shell or through conjugation of targeting ligands to the surface. 74 As these microbubbles typically have large sizes, they stay predominantly within the vascular system after administration; thus, molecular targets are exclusively vasculature related. Tumor angiogenesis imaging with contrast-enhanced US has been explored with microbubbles targeted to integrin αvβ3, 75 endoglin, 76 and vascular endothelial growth factor receptor 2 (VEGFR2). 77 US has relatively high spatial resolution but limited use owing to the relatively poor depth penetration and sensitivity. For this reason, the biodistributions and pharmacokinetics of targeted microbubbles cannot be accurately determined. Willmann and colleagues reported 18F-labeled microbubbles targeted to the tumor angiogenesis-related receptor VEGFR2 by using US-PET. 78 The authors evaluated the biodistribution of targeted microbubbles in angiosarcoma tumor-bearing mice. PET revealed that targeted microbubbles were rapidly cleared from the blood circulation in several minutes and accumulated in the liver and spleen by Kupffer cells and splenic macrophages, respectively. Furthermore, uptake of targeted microbubbles in tumor was confirmed by ex vivo gamma counting. The results provided insights into the whole-body biodistribution of targeted microbubbles in vivo. These might have practical implications, such as pharmacokinetics and biodistribution, for performing molecular imaging by using targeted microbubbles for contrast-enhanced US.
Photoacoustic computed tomography (PCT) shows promise as an in vivo multimodality imaging tool. PCT combines optical excitation of tissue using a laser or radiowaves, which are differentially absorbed in tissue, with ultrasound detection of the photoacoustic waves produced by radiation-induced thermoelastic expansion. PCT provides optical contrast with improved spatial resolution and tissue penetration compared with pure optical imaging techniques. Consequently, both structural and functional in vivo imaging can be accomplished with an improved contrast and a reduced noise by PCT compared with conventional optical imaging or US. Recently, several novel metals, such as gold nanorods, 79 gold nanocages, 80 and QDs, 81 as well as trastuzumab-labeled NIR dyes, 82 have been applied for PCT. The combination of PCT with US was designed, and in vivo validation of tumor-targeted PCT-US was reported by de la Zerda and colleagues. 83 In this study, cyclic RGD-PEG conjugated single-walled carbon nanotubes (SWNT-RGD) have been used as the imaging probe. We previously reported that SWNT-RGD is stable in serum and can be specifically accumulated in tumors 84 ; tumor accumulation and biodistribution of SWNT-RGD were evaluated by 64Cu-labeled SWNT-RGD and further analyzed in tissues by Raman microscopy. 85 The photoacoustic signal produced by SWNT was observed to be dose dependent. For PCT-US, SWNT-RGD was intravenously injected in U87MG tumor-bearing mice. As shown in Figure 7, three-dimensional PCT-US images of the tumor and its surroundings were acquired before and after 4 h injection. The subtraction of PCT images before and after injection demonstrated eight times higher photoacoustic signals in the tumor compared with mice injected with plain SWNT (see Figure 7A). PCT images were also verified using Raman microscopy on excised tumor tissues (see Figure 7B). Given that existing NIR fluorophores or novel metals can be considered PCT probes, those agents can be simply applied to multimodality systems, such as PCT-US-optical imaging or PCT-US-CT. The low cost and flexible contrast mechanisms of PCT may facilitate its integration into existing imaging systems, thereby accelerating the use of the combined strengths of both modalities.
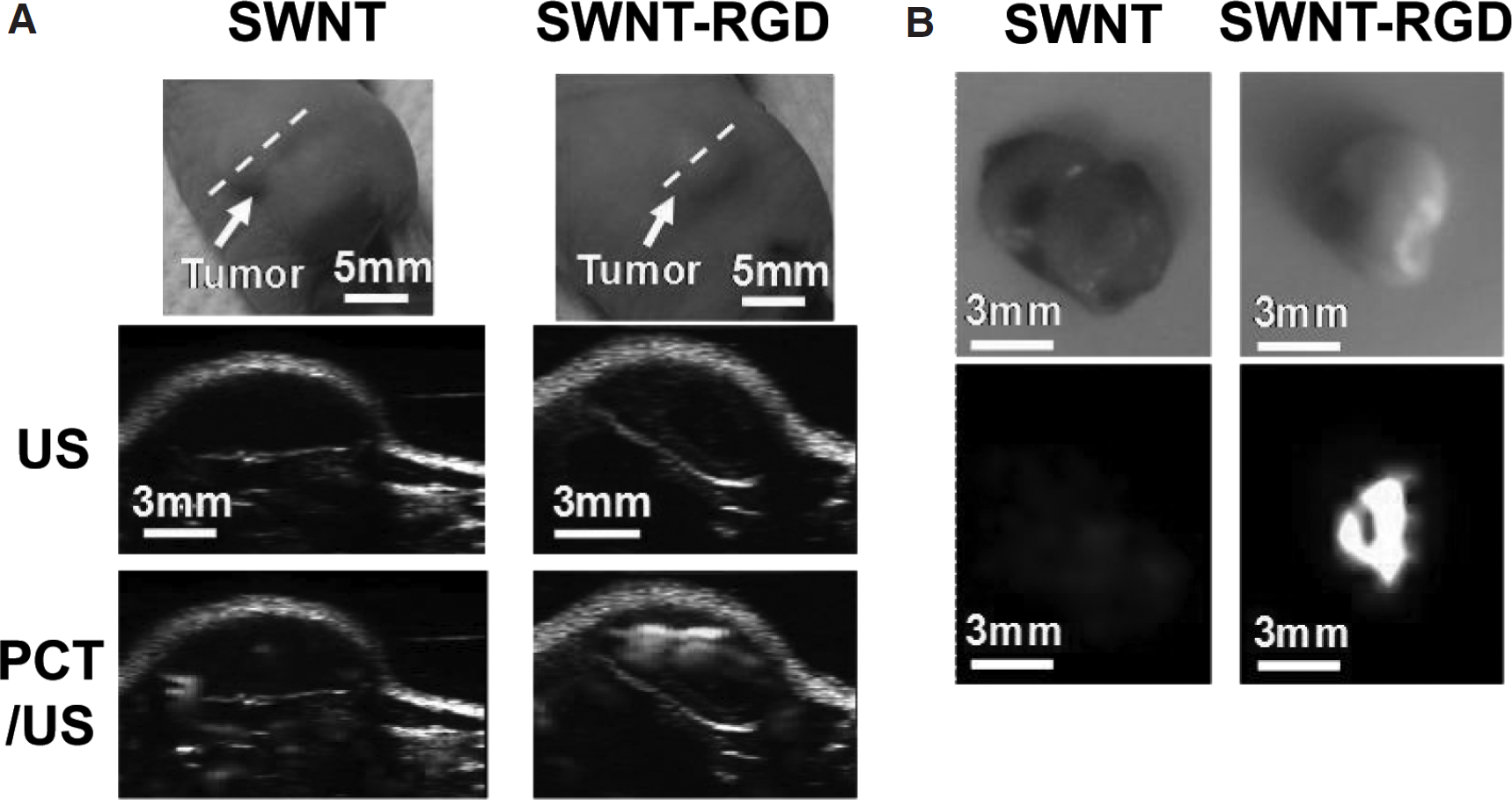
PCT-US shows that SWNT-RGD targets tumor in U87MG tumor-bearing mice 4 h after intravenous injection. A, Ultrasound (gray) and photoacoustic (green) images of one vertical slice through the tumor. The high photoacoustic signal in the tumor was monitored after injection of SWNT-RGD. B, Validation of the in vivo photoacoustic images by Raman ex vivo microscopy. Adapted with permission from de la Zerda A et al. 83 Copyright 2008, Macmillan Publishers Limited.
Future Directions
The clinical perspectives of multimodality imaging are tremendous. These powerful approaches will offer the unprecedented and paradigm-shifting opportunity to study the components and dynamics of biologic processes at the molecular level. It is also expected to improve our understanding of the distribution of molecules, therapeutic drugs, transplanted cells, and genes in vivo with enhanced spatial resolution, temporal resolution, and sensitivity. At the end of the spectrum, multimodality imaging will play an essential role in supporting advanced patient-specific treatment, in diagnosing disease, in predicting which therapy to use, in planning therapy, and in monitoring therapeutic treatment. To make dreams become reality, a lot of emphasis is needed not only on imaging system design but also, more importantly, on imaging probe design. The emergence of molecular imaging technologies and interdisciplinary research at the interface of the imaging science and nanotechnology has generated novel multimodality imaging probes that can be used as novel tools for future imaging modalities. Many of these probes reportedly show promising results on the proof of concept for multimodality imaging. However, the application of a multimodality imaging probe is in its infancy, and much work remains to be done, which includes characterization of the accuracy and reproducibility of different techniques, standardization of methods, and improvements in imaging analysis. Furthermore, cross-validation of the detection sensitivities for the different imaging devices should be considered. For instance, the high detection sensitivity can be shared by nuclear and optical combinations; however, careful correlations must be taken into consideration for nuclear imaging-MRI or optical imaging-MRI combinations.
In this article, we introduced various emerging approaches enveloped by the term dual-modality probes with respect to their design strategies and applications. Most of the design platforms are flexible and tunable for a wide array of new application in nanomedicine. For instance, dual-modality imaging probes can be simply developed for diagnosis and therapy, theragnostics, by combining therapeutic drugs and molecular imaging. Such theragnostics hold great promise in personalized medicine.86,87 Overall, the dual-modality image is believed to be greater than the sum of its parts.
Footnotes
Acknowledgment
Financial disclosure of authors and reviewers: None reported.
