Abstract
The health risks and economic costs of obesity are a growing public health concern [1]. Currently, more than one-third of adults are obese (defined as BMI ≥30 kg/m2) [2]. Among women, obesity is most prevalent among those older than 60 years of age [2] and in minorities [3].
The high prevalence of obesity in women may be, in part, a function of pregnancy, as pregnancy is a time during which a woman's weight increases considerably. Childbirth is associated with weight increases beyond the term of the pregnancy [4–6]. However, the amount of weight retained after pregnancy is highly variable [7]. Most research examining the impact of pregnancy on postpartum weight has focused on changes in weight in the first year after childbirth. Research on long-term postpartum weight retention is limited [8].
We recently reported that obesity was significantly more prevalent 5–10 years after cesarean than after vaginal birth [9]. This observation led us to question whether long-term changes in weight may differ by route of first delivery. The present study was, therefore, undertaken to investigate whether changes in weight after childbirth differs by route of delivery and to identify factors that influence long-term changes in weight after childbirth.
Materials & methods
This is an analysis of data from the MOAD study, a longitudinal cohort study of maternal health outcomes after cesarean versus vaginal delivery. The study methods have previously been reported [9]. Briefly, MOAD participants were recruited from the obstetrical population at a large community hospital in suburban Maryland (MD, USA). Women were enrolled in the study 5–10 years after their first delivery. Participants were recruited based on the mode of delivery of their first child (cesarean vs vaginal). The recruitment of women in the cesarean and vaginal birth groups was frequency matched to ensure that age at the time of first delivery and years since that delivery were similar between the two groups. Exclusion criteria (applied to the index birth) included: maternal age of <15 or >50 years, delivery at <37 weeks gestation, placenta previa, multiple gestation, known fetal congenital anomaly, stillbirth, prior myomectomy and abruption. Women who experienced these events during subsequent pregnancies were not excluded. This research was approved by the Institutional Review Board and all participants provided written informed consent.
At study enrollment, weight was measured by research staff on a balance scale. Height was also measured and BMI was calculated (weight/height2 in kg/m2). Due to the retrospective design of this analysis, weight and other characteristics assessed at the MOAD study enrollment are referred to as occurring at follow-up.
Maternal weight at the conclusion of the first pregnancy was obtained from each participant's obstetrical chart. While maternal weight at hospital admission is recorded by nursing staff, the value recorded is typically self-reported by the patient at the time of admission. Nevertheless, because obstetrical patients are weighed every week in the last month of pregnancy, the recorded weights are presumed to be timely and accurate.
A list of maternal characteristics hypothesized to be associated with long-term maternal weight change was identified a priori. The independent variable of primary interest was mode of delivery for each woman's first birth (e.g., cesarean vs vaginal birth). This, and all other obstetrical variables, were abstracted from the hospital record by members of our research team who are also obstetricians. The obstetrical variables of interest included maternal age at first delivery, history of diabetes prior to the first delivery (including gestational diabetes) and the baby's birth weight (kg).
Data collected at enrollment included: self-reported primary race (black race vs all other races), smoking history (current, former or never), educational attainment (less than college degree, college degree or graduate degree), parity and gravidity. In addition, for each delivery reported, the participant was asked whether she breastfed and if so, the duration of breastfeeding for each delivery (months). The average number of months of lactation per delivery was calculated as the total months of breastfeeding divided by the number of deliveries for each participant.
The first outcome considered was obesity at follow-up, defined as a BMI >30 kg/m2. Demographic and obstetrical history characteristics were summarized using median and interquartile range (IQR) for continuous variables, and percentage and frequency for categorical variables. Differences between obese and nonobese women were tested using Wilcoxon rank-sum tests for continuous variables and χ2-tests of independence for categorical variables.
The relationship between each participant's weight at follow-up and her weight at first delivery (e.g., 5–10 years prior to enrollment) was explored graphically using scatter plot and least-squares linear regression. For each participant, the difference between follow-up weight and weight at first delivery was calculated. Most women lost weight over the 5–10 years from their first delivery. Thus, most values for change in weight had negative values.
Univariate linear regression was used to identify factors associated with change in weight. The characteristics significantly associated with change in weight were further investigated in multivariate analysis. Where necessary, piecewise linear models were developed to address nonlinear relationships. Final multivariate linear regression models were determined using Akaike Information Criterion [10]. Because our primary goal for this analysis was to explore the possible effect of cesarean versus vaginal delivery on maternal weight change, a variable reflecting the mode of first delivery was retained in all models.
All analysis was performed using SAS 9.2© statistical software (SAS Institute Inc., NC, USA, 2002–2008). Graphical figures were created using S-Plus 8.0© statistical software (Insightful Corp., WA, USA, 2007). Statistical significance was defined at the α = 0.05 level.
Results
At the time of analysis, the MOAD study included 1011 participants. Of these, 52 women (5%) were excluded from the analysis because maternal weight at first delivery was not available. An additional 11 women were excluded as outliers because they either lost more than 40 kg (n = 8) or gained more than 20 kg (n = 3). Finally, 43 women who had delivered their last child within 12 months of enrollment were excluded. Thus, 905 women were included in this analysis. Among these women, median weight at follow-up was 73 kg (IQR: 60–81) and 24% of participants were obese at follow-up. The median age at follow-up was 40 years (IQR: 36–43) and the median duration of time between first childbirth and follow-up was 7.4 years (IQR: 6.4–9.0).
Demographic and obstetrical history characteristics of the 905 women, overall and by obesity status at follow-up, are shown in
Demographic and obstetrical characteristics† of the study population, overall and by obesity status at follow-up (n = 905).
Median (interquartile range) or percentage (frequency).
Wilcoxon rank-sum test for continuous variables; χ2-tests for categorical variables.
Former smoker defined as having smoked >100 cigarettes in a lifetime, but not currently a smoker.
Among women who reported breastfeeding with at least one child (n = 693).
Women who were missing average duration of lactation (n = 27).
The strong association between weight at first delivery and follow-up weight is illustrated in
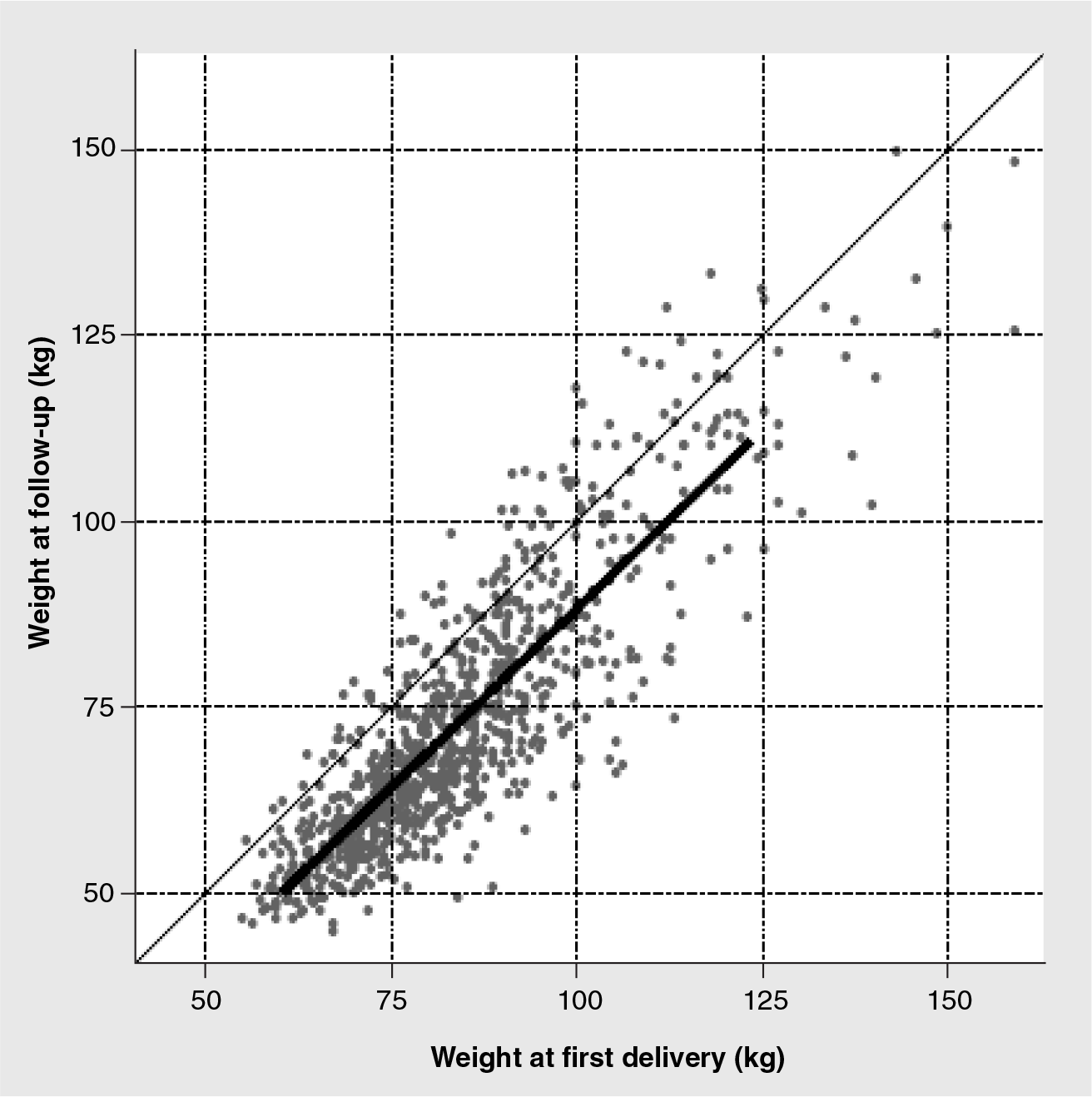
Univariate linear regression was used to investigate characteristics associated with change in weight between first delivery and follow-up (
Change in maternal weight (from first delivery to study enrollment) as a function of demographic, obstetric and reproductive risk factors (n = 905).
Restricted to women who reported successfully initiating breastfeeding with at least one child (n = 693).
Women who were missing average duration of lactation (n = 27).
Not applicable.

These variables were candidates for the multivariate analysis and the most parsimonious adjusted model is shown in
Discussion
The primary objective of this study was to investigate whether the very strong association observed between cesarean and obesity later in life could be attributed to route of delivery (e.g., whether that association was independent of the possible difference between women who deliver by cesarean). Although women who delivered by cesarean were more likely to be obese 5–10 years from delivery, this association was not significant after accounting for other differences, most notably weight at the time of first childbirth. Obesity during pregnancy is known to be associated with cesarean birth [11] and our results suggest that mode of delivery has no effect on long-term changes in maternal weight. Maternal weight at the time of a first delivery is a strong predictor of weight 5–10 years later and the long-term weight trajectory is similar for women who deliver by cesarean and vaginal birth.
An important finding from this research is the substantial impact of race on changes in maternal weight. This finding is consistent with prior research, but extends such research by controlling for the confounding effects of diabetes, maternal weight during pregnancy, breastfeeding practices and maternal education [4,6,12–14]. Furthermore, prior studies of race and weight retention have been limited by the use of self-reported, retrospectively recalled weights, limited follow-up time, or other population constraints [12–14]. For example, a 10-year prospective cohort study found that black women had a much greater chance of becoming overweight after childbirth, but utilized retrospectively recalled pregravid weights [15]. Findings by Gunderson and colleagues suggested that the increased odds of becoming overweight for black mothers was explained by differences in parity and pregravid obesity [5]. However, these findings suggest that racial differences persist after adjustment. Gunderson has suggested that weight gain among black women may reflect differences in social, cultural and behavioral factors. Given the high prevalence of obesity in black women, it is important to better understand the causes that may contribute to greater postpartum weight in this population [1,3].
Another striking finding from the present study was the impact of diabetes. After controlling for maternal weight at first delivery and the weight of the neonate, the participants with gestational diabetes or pregestational diabetes retained significantly more weight than those who were not exposed to diabetes before delivery. This effect persisted after controlling for the confounding effect of weight at the time of delivery. Unfortunately, we did not have a sufficient sample to investigate possible differences between gestational and pregestational diabetes on long-term weight change. The extra weight retained by mothers with a history of gestational diabetes may indicate continued insulin resistance, which may exacerbate the risk for Type 2 diabetes if not controlled [16].
In this cohort, additional deliveries (after the first) contributed marginally to long-term maternal weight. Specifically, multiparous women lost more weight than primiparous women (although this association was marginally significant in a multivariate model). Prior studies have demonstrated inconsistent results regarding the impact of multiparity on maternal weight, with some suggesting no association between parity and weight [4,5,17] and others suggesting an association between increasing maternal weight with additional pregnancies [18,19].
No association between breastfeeding and changes in maternal weight was found. This is somewhat surprising because breastfeeding has been associated with short-term weight loss after childbirth [20]. In fact, women are often advised to breastfeed as a strategy to promote weight loss after delivery. However, the literature is conflicting and inconsistent regarding the benefits of breastfeeding on long-term maternal weight [15,16,21,22]. Some research has suggested that the recommended dietary caloric allowance for lactating women is too high and that greater caloric intake coupled with a more sedentary lifestyle may explain why weight loss with lactation is highly variable [4].
The finding in this study that weight increases with length of follow-up supports current literature [17]. However, this association is unlikely related to childbirth, since weight tends to increase with age [17].
While this study had a strong focus on reproductive factors, it was limited by data regarding lifestyle, including exercise and dietary practices, which could have important influence on weight. Also, an inherent limitation of this study is the lack of data regarding prepregnancy weight and gestational weight gain. Many prior studies of long-term changes in weight after pregnancy have focused on the impact of gestational weight gain, but the impact of gestational weight gain in this population cannot be commented on [15–18,21]. In addition, the impact of unmeasured differences between women who delivered vaginally and those who delivered by cesarean cannot be excluded. Last, a limitation of this research is that the population in this study was highly educated and was somewhat older at first delivery than would be typical for US women. These characteristics may limit the generalizability of the results, especially with respect to teenage mothers and less affluent populations.
A strength of this study is the relatively large population size. With a sample size of almost 1000 women, this cohort facilitated an examination of a variety of potential risk factors related to long-term weight. Also, the focus on reproductive factors allowed for an assessment of parity, breastfeeding and mode of delivery while controlling for obesity at delivery. Another strength of this analysis is that maternal weight at first delivery was recorded prospectively and is, therefore, not subject to potential recall bias. Also, the use of obstetrical records for reproductive data (including baby birth weights) is more likely to provide valid exposure data than maternal recall.
Conclusion
This study provided a unique opportunity to examine long-term changes in maternal weight 5–10 years after pregnancy. The findings of this research have important implications for the clinical care of obstetrical patients. Specifically, our results suggest that efforts to prevent obesity should be targeted at black women and women with diabetes. Women with these characteristics may be appropriate targets for educational, behavioral and nutritional interventions that promote the return to a long-term healthy weight after pregnancy.
Future perspective
With increasing obesity worldwide, efforts to help adults maintain a healthy weight become more critical. Given the limited effectiveness of most weight-loss interventions, prevention of obesity is critical. Our research suggests that black women and women with gestational diabetes may be ideal populations to target for obesity prevention trials.
Executive summary
Maternal weight at the time of first delivery is a strong predictor of weight 5–10 years later, with an average change in weight of −11 kg.
Over 5–10 years from the time of first delivery, black women and women with diabetes lost less weight compared with women without these characteristics.
After a first delivery, long-term changes in maternal weight were not influenced by cesarean versus vaginal birth (although women who deliver by cesarean are more likely to be heavier at the time of birth and 5–10 years later). Breastfeeding did not influence long-term change in maternal weight.
Footnotes
Support was provided by the Eunice Kennedy Shriver National Institute of Child Health and Human Development (R01HD056275). The authors have no other relevant affiliations or financial involvement with any organization or entity with a financial interest in or financial conflict with the subject matter or materials discussed in the manuscript apart from those disclosed.
No writing assistance was utilized in the production of this manuscript.
The authors state that they have obtained appropriate institutional review board approval or have followed the principles outlined in the Declaration of Helsinki for all human or animal experimental investigations. In addition, for investigations involving human subjects, informed consent has been obtained from the participants involved.
