Abstract
Polycystic ovary syndrome (PCOS) is a common condition in women of reproductive age, and has reproductive, metabolic and psychological implications. Weight gain and obesity worsen the features of PCOS, while weight loss improves the features of PCOS. While there are potential barriers to successful weight management in young women who do not suffer from PCOS, women with PCOS may experience additional barriers. Weight management strategies in younger women with or without PCOS should encompass both the prevention of excess weight gain and achieving and maintaining a reduced weight through multidisciplinary lifestyle management, comprising dietary, exercise and behavioral therapy, as well as attention to psychosocial stress and practical and physiological barriers to weight management. Further research is warranted in the examination of specific barriers to weight management in women with PCOS, as well as in the determination of optimal components of lifestyle weight management interventions in young women in order to facilitate long-term compliance.
Obesity and excess weight are major chronic diseases in Western countries. In many developed and developing countries, the past decade has seen a dramatic increase in the prevalence of adults and children who are overweight or obese [201]. Consequently, there has been an increase in the incidence of obesity-related illnesses, such as Type 2 diabetes mellitus (DM2) and cardiovascular disease (CVD). Obesity also significantly impairs fertility [1] and increases pregnancy complications, both independently and by exacerbating the common condition of polycystic ovary syndrome (PCOS). Given that obesity is associated with higher risks of chronic illness, it is therefore responsible for a significant increase in healthcare. At a macro level, it has been estimated that healthcare costs attributed to obesity account for approximately 5–7% of the total health spending in the USA and 2–3% of the total health spending in Canada, Australia and New Zealand [202]. While some governments in the Western world are beginning to be confronted by the financial and social burden posed by obesity to the economy, attention is being increasingly focused on how best to intervene in order to mitigate this burden through policies and programs [2,3]. Determining priority target groups at greatest risk for obesity demonstrates that women aged 25–45 years represent a high-risk group for weight gain [203] and that those with children are at an increased risk because of weight gain associated with pregnancy and subsequent lifestyle change. Whilst the trajectory to chronic disease may be decades in the future, there are compelling physiological and social reasons as to why focusing lifestyle programs on young women are likely to yield important benefits.
The increasing rate of obesity in women of childbearing age presents a concern for two reasons. First, there is an increased likelihood that women entering pregnancy with a high BMI will gain and retain more weight in subsequent pregnancies. Second, there is emerging evidence that maternal obesity may potentially have a deleterious effect on the fetus and increase the propensity of the child towards becoming obese [4,5]. Exposure to overnutrition in fetal life results in a series of central and peripheral neuroendocrine responses that, in turn, program the development of fat cells and of the central appetite regulatory system [6]. Thus, the physiological responses to relative overnutrition in early life may directly contribute to an intergenerational cycle of obesity, although as yet there are still multiple confounding factors present when considering the consequences of the fetal origins of disease. Under these circumstances, optimal nutritional management of women of childbearing age before conception, as well as during and after pregnancy, may provide opportunities to improve health outcomes for the mother and her child.
Polycystic ovary syndrome
Polycystic ovary syndrome is the most common endocrinopathy affecting reproductive-aged women, with a prevalence of approximately 11% of Australian women and 21% of Australian indigenous women [7–9]. PCOS diagnosis is based on reproductive features, including ovulatory disturbance and hyperandrogenism. Women with PCOS present with a range of clinical reproductive features, including hyperandrogenism, hirsutism, anovulation, menstrual irregularity, infertility and the potential for increased pregnancy complications [10,11]. Women with PCOS also present with metabolic features, such as elevated risk factors for DM2 and CVD with increased metabolic syndrome, impaired glucose tolerance and DM2 and the potential for increased risk for CVD [12–15]. There is emerging evidence that PCOS is also associated with psychological features, including worsened quality of life and increased anxiety and depression [16]. The etiology of PCOS is underpinned by insulin resistance [7,17,18]. In PCOS, hyperinsulinemia augments hyperandrogenism, both through increasing ovarian androgen production in isolation [19] and synergistically with luteinizing hormone [20], as well as through decreasing hepatic production of the androgen-binding protein, sex hormone-binding globulin [21]. This worsens the clinical reproductive manifestations of PCOS, including hyperandrogenism, infertility and ovarian dysfunction.
Obesity & polycystic ovary syndrome
Polycystic ovary syndrome is also a condition that has a strong relationship with obesity. It is proposed that women with PCOS are affected by both PCOS-specific inherent insulin resistance with additional obesity and lifestyle-related extrinsic insulin resistance [22]. Obesity, specifically abdominal obesity, further increases insulin resistance [23,24]. Insulin resistance is strongly associated with an increased risk for DM2 and CVD in the general population [25–27] and in women with PCOS [28]. Obesity or insulin resistance exacerbate the reproductive, metabolic and psychological features of PCOS [13,29–31]. Women with PCOS may also display elevated rates of overweight, obesity and abdominal obesity. However, the prevalence of obesity in women with PCOS varies greatly from country to country, although population-based data are lacking, making comparisons between countries difficult [32]. In a recent study comparing women with PCOS (n = 401) and age-matched controls from the National Health and Nutrition Examination Survey I (NHANES I) study (n = 2586), a lower proportion of women with PCOS had a BMI of less than 25 and higher proportion of women with PCOS had a BMI of more than 30 [33].
To date, whether the association between obesity and PCOS is related to obesity worsening the presentation of PCOS or PCOS conferring a predisposition to obesity is unknown. In keeping with the increase in insulin resistance with obesity and the role of insulin resistance in exacerbating the clinical features of PCOS, the prevalence of PCOS is also reported to be higher in overweight populations. Alvarez-Blasco et al. reported an increased prevalence of PCOS in overweight and obese women (28.3%) in Spain [34], a marked increase from the previously described prevalence of 4–8% in a number of studies [8,35]. A large Danish study also reported a greater number of clinical features of PCOS with increased BMI [36]. However, a recent US study reported no significant increase in the prevalence of PCOS between underweight, normal weight, overweight and obese women (8.2–12.4%), and a similar increase in BMI for women with or without PCOS compared with population changes [37]. However, this latter study was based on a small number of women with PCOS, was potentially underpowered and PCOS diagnosis was not directly established. Therefore, it is probable that PCOS will increase in prevalence as weight increases among young women. However, further population-based studies assessing cross-sectional and longitudinal incidence and PCOS prevalence in relation to BMI and obesity are warranted.
In women, obesity manifests with a range of reproductive conditions, including early menarche, subfertility, PCOS and pregnancy complications, including gestational diabetes, which usually precede typical obesity-related metabolic comorbidities (Figure 1). Women who are obese, especially those with reproductive complications including PCOS, are identified as specific high-risk subgroups for further progression through to metabolic complications, including prediabetes, DM2 and CVD. Hence, practicing clinicians have a unique opportunity to identify female patients at greatest risk of obesity-related metabolic complications early in life through the recognition of women with ‘reproductive insulin-resistant conditions’. These patients can then be targeted for early screening, the prevention of further weight gain and the prevention of progression to prediabetes, DM2 and CVD later in life.

The continuum of potential lifestyle-related reproductive and metabolic implications across the lifespan.
Polycystic ovary syndrome & lifestyle modification
Given the strong association between obesity, abdominal obesity, insulin resistance and the features of PCOS, weight loss or prevention of excess weight gain is a logical initial treatment aim. The Androgen Excess PCOS Society (AEPCOS) statement on lifestyle modification in women with PCOS proposes lifestyle modification as the primary therapy in overweight and obese women with PCOS [32]. Lifestyle intervention has been advocated as part of a targeted approach to the treatment of the clinical, reproductive and metabolic features of PCOS, to be used prior to or in combination with medical therapies (Figure 2). A number of short-to medium-term studies demonstrate that modest weight loss (5–10% of initial body weight) improves metabolic, reproductive and psychological features of PCOS, including hyperandrogenism, insulin resistance, dyslipidemia, glucose tolerance, menstrual function, ovulation, pregnancy, conception and quality of life [32,38–40]. A multidisciplinary approach is being increasingly advocated and the benefits of exercise and behavioral interventions in PCOS have been demonstrated, both in combination with [38–40] and independent of structured energy restriction [41,42]. Despite these documented benefits, achieving and maintaining weight loss is an issue of increasing concern both for the general population and for women with PCOS [43]. The AEPCOS position statement notes the issue of maximizing program compliance, retention and weight maintenance as crucial clinical and research questions [32]. With regard to the comparative efficacy of dietary, exercise or combined integrated interventions, nonsignificant lower drop-out rates were reported for a combined diet and exercise intervention (40.6%) versus diet alone (53%) in women with PCOS [38]. Similarly, nonsignificant higher drop-out rates were reported for a diet alone intervention (35%) compared with a structured exercise training program (15%) in women with PCOS [41], with similar levels of adherence to the diet or exercise programs. However, there are limited data examining these concepts. To date, the optimal intervention in order to maximize compliance and reduce attrition in young women with PCOS is unknown and requires further research.
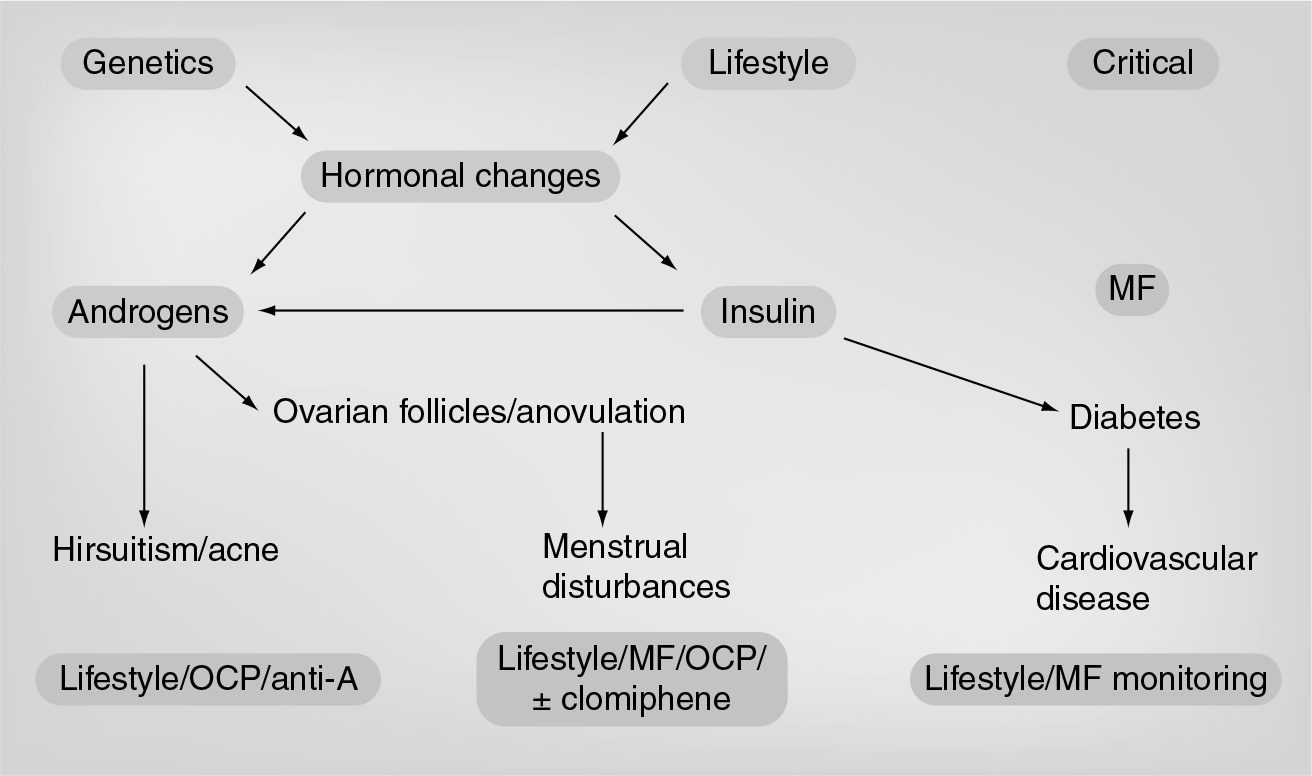
Summary of a targeted approach to lifestyle and medical therapy in polycystic ovary syndrome.
Polycystic ovary syndrome & potential mechanisms of barriers to weight management
Anecdotally, women with PCOS are considered to be a population with specific barriers to weight management. Mechanistically, these may work either through increasing susceptibility to weight gain or resistance to weight loss. Weight loss studies in women with PCOS typically show high drop-out rates (e.g., 26–38% over 1–4 months for women with PCOS [44,45] compared with 8–9% over 4 months in women without PCOS [46–48]). There are a number of physiological reasons for these potential difficulties in weight management. Insulin resistance and hyperinsulinemia may predispose women with PCOS to gain weight, supported by a study demonstrating insulin-therapy induced weight gain [49] through the anabolic effects of insulin and changes in energy expenditure, glycosuria and food intake [50–55]. However, a range of studies have demonstrated that elevated insulin secretion, hyperinsulinemia or insulin resistance (using surrogate fasting or postprandial/clamp measures of insulin resistance) is either associated with greater, similar or lesser weight gain in free-living observational studies [56].
In addition, androgen excess may favor abdominal fat deposition [57] that could contribute to insulin resistance in women with PCOS. Increases in carbohydrate craving are also reported for women with elevated androgen levels who do not suffer from PCOS [58], indicating the potential for increased food intake in women with PCOS. In support of this, one study reported that women with PCOS consumed higher amounts of high glycemic index (GI) foods (e.g., white bread and fried potatoes) compared with women without PCOS [59], and lean women with PCOS consumed less total energy than weight-matched women without PCOS, suggesting that women with PCOS may need to follow more stringent dietary restrictions in order to maintain a suitable weight [60]. Both resting energy expenditure and the thermic effect of food have been reported to be either reduced [61,62] or not to differ [63,64] between women with PCOS and weight-matched controls. Appetite regulation has also been reported to be impaired in women with PCOS, with increased postprandial hunger and abnormal regulation of some appetite hormones, including ghrelin and cholecystokinin [65,66], although this finding has not been consistently reported [67]. At present, it is not clear if women with PCOS are a population with specific barriers to weight management, thus further research is required in this area.
Polycystic ovary syndrome & dietary treatment
If women with PCOS are a population with specific barriers to weight management, it is possible that specific dietary and lifestyle advice is warranted. A number of dietary compositions have been investigated in women with PCOS (Table 1), with specific diets proposed to be more optimal than others for weight management or for inducing more favorable hormonal or metabolic effects. Two small studies examined the effect of very low carbohydrate diets and reported reductions in weight, fasting insulin and free testosterone over 24 weeks in overweight women with PCOS [68,69], and an audit of reduced glycemic load diets (low GI foods, 40– 45% carbohydrate and 30% protein) in lean and overweight women with PCOS reported reductions in BMI and waist circumference [70], although these studies lacked a control group. Two studies comparing high and low protein isocaloric diets (30% protein and 40% carbohydrate, compared with 15% protein and 55% carbohydrate) reported equivalent reductions in weight, fasting insulin, reproductive hormones and reproductive parameters [44,45], and modest improvements for the higher protein intake, with a greater reduction in postprandial glucose, no decrease in high-density lipoprotein cholesterol in weight loss and sustained reduction in free androgen index in weight loss [44]. One recent study reported greater reductions in weight, fat mass and total cholesterol, high-density lipoprotein cholesterol and ApoB for a high compared with a low protein diet; this was achieved through the addition of a high or low protein supplement to a standard energy reduced diet [71]. Meal replacements and moderate reductions in fat or carbohydrate through fat or carbohydrate counting, in conjunction with low GI foods, were all equivalently effective in reducing weight and improving reproductive and metabolic parameters [72]. At present, there is no evidence for one dietary strategy being optimal in achieving and maintaining weight loss and reproductive and metabolic improvement long-term.
Trials of modification of dietary macronutrient composition in lifestyle programs and its impact on key features in overweight/obese women with polycystic ovary syndrome.

C: Carbohydrate; ER: Energy restriction; F: Fat; FAI: Free adrogen index; GL: Glycemic load; HBA1c: Glycosylated hemoglobin; HC: High carbohydrate;
HDL-C: High-density lipoprotein cholesterol; HOM: Homeostasis assessment of insulin resistance; HP: High protein; hsCRP: Highly sensitive C reactive protein;
IR: Insulin resistance; LDL-C: Low-density lipoprotein cholesterol; NS: Nonsignificant; P: Protein; RCT: Randomized controlled trial; SHBG: Sex hormone-binding globulin; T: Testosterone; TC: Total cholesterol; TG: Triglyceride; WM: Weight maintenance; WMD: Weight maintenance diet.
Adapted with permission from [32].
It is difficult to determine whether the presentation of weight gain/obesity in women with PCOS is essentially different to the rest of the population owing to the general increase in obesity rates in developed nations. Improved monitoring is required in order to assess this issue further. In addition, it is not yet known whether proposed difficulties in weight management in PCOS are due to the population group of younger women being studied or whether they are due to PCOS-specific physiology. Interestingly, poorer study retention rates have been documented in weight loss interventions both for females and for subjects of a younger age [73–75], suggesting specific barriers to weight management in this group. Furthermore, several longitudinal population studies report an increased weight gain in young women. According to the Women's Health Australia (WHA) study, young women (18-23 years of age) gained more weight (6.32 kg) over longitudinal follow-up (8-10 years) than midaged (weight gain: 3.43 kg) or older women (weight loss of 1.69 kg) [203]. These results are supported by the NHANES study, which reported that women aged 25–44 years experienced the greatest average weight gain [76]. There are currently no similar longitudinal studies in women with PCOS for comparison. Therefore, younger women are an important target for weight management.
Barriers to obesity management in younger women
Many diverse factors give rise to disturbed energy balance, with the interaction between these factors, rather than the influence of any single factor, affecting individual and population weight. Lifestyle factors, such as physical activity and dietary intake, are core determinants but are influenced by factors including age, gender, life-stages, socioeconomic status and psychological factors.
There are a number of critical life-stages or events that put women at risk for excess weight gain and younger women are at an increased risk. Physical inactivity is prevalent among women, particularly in the age groups of 18–24 and 25–34 years, with approximately 30–33% of women reporting no exercise in the previous 2 weeks [204]. Rates of leisure time and physical activity decline in women following significant life-events, such as having children [77], with reasons for lower participation rates including lack of motivation, childcare, time and support [78]. Commencing paid work is also reported as a barrier to participation in physical activity. In the WHA cohort, almost 40% of young women changed activity patterns, with reasons for change including marriage, having children or commencing paid work [203]. These results are supported by other longitudinal studies of Australian women that found that younger women (35-44 years of age) with children gained more weight than older women [79,80]. The Nurses' Health Study reported that 30% of new cases of obesity and 43% of new cases of DM2 could be prevented by adopting a moderately active lifestyle, that each 2-h increment in television watching was associated with a 23% increase in obesity and a 14% increase in DM2 and each 1 h of walking was associated with a 24% reduction in obesity and a 34% reduction in DM2 [81]. Therefore, these perceived barriers are likely to significantly affect weight management-related behaviors.
Pregnancy and childbirth often result in the retention of weight after delivery, particularly with early cessation of breastfeeding. It is generally recognized that more women now entering pregnancy are overweight or obese, and weight gain during pregnancy is greater than that recommended, with Polley et al. reporting the mean postpartum weight retention as 3.7 ± 5.9 kg [82]. This is supported by data demonstrating that young women who gave birth during the 10-year WHA study period gained 2–3 kg in addition to the almost 4-kg gain experienced by women who had not had children [203]. Furthermore, women may suffer additional barriers to weight management with aging. While an increase in body fat and obesity prevalence occurs with aging in industrialized societies, menopausal women are particularly prone to rapid weight gain. The mechanistic reasons for this are not yet clear, but may include factors such as increased visceral abdominal fat in postmenopausal women, potentially related to decreased estrogen levels [83]. As women in midlife are at an increased risk for developing obesity and related chronic diseases, such as CVD, osteoporosis, DM2 and hypertension [203], the years prior to menopause are critical for interventions that may prevent or slow down weight gain and associated health changes. In addition, there appears to be a significant influence of psychological factors on weight management behaviors in women. As women with PCOS are at an increased risk for depression and anxiety, and demonstrate worsened quality of life [84], this indicates mood may potentially exacerbate obesity in this group. Women are more likely to eat in response to mood compared with men [85], and food is often used by women as a means to cope with stress and to escape from reality [86], with Chang et al. reporting that US low-income overweight and obese mothers (18-35 years of age) take large portions of energydense comfort food, such as chocolate and icecream, in order to cope with daily stress [87]. Stress-driven eating is significantly associated with obesity in women (odds ratio: 3.24; 95% CI: 2.19-4.79) but not in men [88]. Furthermore, young women cited lack of time and motivation as the most important barriers to physical activity and healthy eating [89], and more women than men felt that they were chronically time-pressured [90]. Support from family and friends is also crucial for weight management in young women. Young women were more likely to perceive social situations as barriers to healthy eating or being physically active [91], and support or sabotage by friends and family predicted the success of weight maintenance [92].
Weight management strategies in younger women
Young women both with and without PCOS may experience unique barriers to weight management, supporting the claim that they are a population in which both weight loss and prevention of weight gain is a crucial goal. However, this raises the question of what the best means for achieving and maintaining weight loss is in young women in general, irrespective of PCOS status. The concept of obesity prevention addresses excess weight gain in normal-weight individuals, the progression from overweight to obesity in those who are already overweight and preventing weight gain in those who have previously lost weight.
There are few studies specifically addressing the issue of prevention of weight gain in young women. A recent systematic review reported only nine randomized controlled trials in the past 10 years, assessing in total 375 men and 1595 women aged 18–50 years, with a 2–5% difference in weight between intervention and control groups [93]. Only two of these studies were in young women alone. While all interventions were comprehensive and multifactorial, with exercise, dietary and behavioral components, the nature of these components, the length of interventions and the intensity varied greatly.
These included more general messages to prescriptive interventions with dietary and physical activity targets, and intervention durations ranging from moderate-(13 weeks) to long-term (5 years) interventions. One successful randomized controlled trial to prevent weight gain in 250 community-based young women with children was based on self-management skills [94]. Simple, clear diet and physical activity messages were used with self-monitoring, problem-solving, goal-setting and relapse-prevention discussions, supported with ongoing mobile phone text messages for 1 year. Self-monitoring appeared to be particularly helpful in weight management for this group [95]. This study also supports the concept that prevention of weight gain requires a less intensive intervention compared with treatment of obesity, which is important when targeting large numbers of the population. However, some personal contact may be important, since correspondence-only courses have not been successful in weight-gain prevention [96]. This makes both direct comparisons of interventions and practical advice on successful intervention components difficult to determine.
With regard to weight-loss studies in young women, the bulk of the literature specifically assessing this population has been accomplished in young women with PCOS, as previously described. With regard to lifestyle interventions incorporating physical activity and behavioral interventions, while women are generally advised to increase physical activity to assist their efforts in weight loss, the actual effects of physical activity is often misunderstood. Increasing levels of evidence suggest that physical activity has minimal effects on weight loss per se [97]. Studies in overweight and obese young women found that exercise-only interventions did not result in weight loss [98,99]. Similarly, the addition of physical activity to dietary interventions did not enhance weight loss [38,100,101], although it provides benefits in improving body composition during weight loss. There is conflicting evidence regarding whether physical activity improves metabolic health. Some studies in women with or without PCOS report that physical activity is associated with greater decreases in fat mass and better retention of fat-free mass during energy restriction [38,100], improved insulin sensitivity [102,103] and reduced homocysteine levels [99], while other studies report no improvements in insulin sensitivity or lipid profiles [38,98]. Gender-specific effects have been found in exercise-only interventions, with the program resulting in weight loss in men but not in women [98,104]. Studies to date suggest that exercise should be a part of weight management in younger women in order to promote fat loss and prevent muscle loss during energy restriction.
Multicomponent interventions incorporating diet, physical activity advice and support with psychological techniques have the potential to be most effective in facilitating long-term behavior change, which is essential for weight management. A review examining the additive effect of combining interventions for exercise-behavior therapy or weight-loss medication with dietary advice found that each was associated with similar weight changes [105]. In addition, a systematic review of psychological interventions for overweight and obesity suggests that behavioral and cognitive-behavioral strategies are effective weight-loss therapies, at least in the short-term [106].
Behavioral support plays an important role in facilitating behavioral change in weight management. Specific skills, such as self-monitoring, countering negative thoughts, managing environmental cues and others, contribute to the success of lifestyle modification. Very few interventions in young women employed a combined therapy utilizing diet, exercise and behavioral support. The Health Hunters program from Sweden is the only combined lifestyle program specifically developed for this group [107]. This 1- year program was developed to prevent weight gain in lean and overweight young women aged 18–28 years who have at least one obese parent. Analysis of those who comlpeted the program found that the intervention group demonstrated significantly greater improvement in BMI, waist circumference and waist:hip ratio compared with the control group. However, the small magnitude of weight reduction achieved (<5%) may be of limited clinical significance. To date, developing strategies that are either effective in preventing excess weight gain or both are efficacious in producing clinically significant weight loss and effective in facilitating long-term adherence among free-living young women, remains a challenge.
Practical implications for weight management in younger women
In overweight and obese women with PCOS, weight loss has been demonstrated to improve a range of reproductive, metabolic and psychological features [32]. The AEPCOS society position statement recommends lifestyle management, and energy restriction where required as key treatments in PCOS, as long as the dietary regime is safe and sustainable (Box 1) [32]. With regard to specific dietary advice for PCOS, the evidence for one diet composition being optimal in the management of PCOS is currently limited. However, a range of potential dietary approaches have demonstrated positive effects on reproductive and metabolic parameters in women with PCOS, including modifying GI and glycemic load, carbohydrate or protein amount, use of meal replacements, modifying fatty acid intake or fat or carbohydrate counting. Further research is required into optimal macronutrient compositions in weight loss and maintenance in PCOS and optimal dietary strategies for weight management. Where potential barriers to weight management exist in women with PCOS, further assessment of both optimal satiating dietary compositions and optimal strategies for the treatment of the unique barriers to weight management in PCOS is warranted.
Lifestyle modification principles suggested for obesity management in polycystic ovary syndrome.
Weight management through lifestyle modification combining behavioral, dietary and exercise management can be effective in improving reproductive function, as well as metabolic and psychological parameters.
Reduced-energy diets (500-1000 kcal/day reduction) are effective options for weight loss and can reduce body weight by 7–10% over a period of 6–12 months.
Dietary pattern should be nutritionally complete and appropriate for each life stage. A variety of approaches, including high carbohydrate diets, high dietary protein diets, low glycemic index or load diets, as well as meal replacements, may be successful for achieving and sustaining a reduced weight.
The structure and support within a weight management program is crucial and may be more important than the dietary composition. Goal setting, weight monitoring and individualization of the program, intensive follow-up and monitoring by a physician and support from a physician, family, spouse or support from peers, may assist in improving successful outcomes.
Lifestyle programs need to address issues such as self-esteem, managing stress, emotional eating and time constraints.
Structured exercise is an important component of a weight loss regime.
Adapted from [112].
Weight loss is achievable and has been demonstrated in women with PCOS through intensive structured interventions [40,44,72]. Similarly, in the general population, intensive interventions in women can result in weight loss, supported by the Women's Healthy Lifestyle Project, where dietary fat was reduced to 25% and energy and physical activity increased to between 1000 and 1500 kcals per day, with positive results for weight, total cholesterol, triglyceride, blood pressure and glucose [108]. However, the issue of program adherence and long-term weight maintenance remains a concern for both the general population and women with PCOS. In a study examining the barriers to program participation experienced by families attending a prevention of weight gain program, the authors suggested that programs should reduce practical barriers, provide transportation, childcare, refreshments and financial compensation [109]. Flexible sessions and close attention to motivation and expectations may lead to improved participation. Effective strategies should also seek to address the barriers to a healthy lifestyle in young women. Studies to date suggest that lack of time is a significant barrier to a healthy diet and physical activity in young women [89,110]. Currently, most recommendations for weight loss place a high demand on the participants' time, whether in food preparation or in the engagement of a specific physical activity routine. Simple strategies that could fit around the busy schedules of working women, women with young children or working mothers need to be developed.
Increasing levels of evidence demonstrate that stress could be a cause of unhealthy lifestyles in women [86,87]. Emotional eating also appeared to be a significant factor in influencing energy intake in women. Thus, strategies that involve stress management could be explored in weight loss interventions for women. Since stress is often associated with time-pressure, strategies on time management could also be investigated within the context of weight management in women. By contrast, the recommended weight-loss strategies should not add to the burden of coping with daily lives, otherwise the intervention itself will become an additional source of stress. The support of family members and other significant individuals in the lives of women is an important determinant of the success in lifestyle modification [87,89]. Interventions targeting the social environment of young women, such as family, peer groups or workplace, could be investigated. Interventions targeting individuals could also include strategies that empower young women to elicit support from their social environment.
Investing in research into effective approaches for diet and lifestyle modification in order to assist women of childbearing age to lose weight or limit weight gain should be a critical focus in managing the obesity epidemic. The optimum time for such preventative care should be before pregnancy in ‘at-risk’ young women, such as those with PCOS, although this would be more difficult, given that many pregnancies are not planned. Such approaches need to be tailored to the nutritional and psychological needs of women during their reproductive years, recognizing that each moment of contact between healthcare provider and patient is not an isolated event, but rather an important part of a continuum of care. Short- and long-term multidisciplinary studies on program content, delivery and cost–effectiveness in relevant groups of young women are warranted.
Conclusion
Lifestyle management of PCOS is advised as an initial treatment strategy, and weight loss improves reproductive and metabolic parameters in overweight women with PCOS. Prevention of excess weight gain in normal-weight women, reduction of weight in overweight and obese women and long-term maintenance of weight loss are all crucial approaches for weight management in young women. While national data from several countries suggest that younger women are at a high risk of weight gain, limited research has been performed regarding weight management in this group, and even less specifically in women with PCOS. In young women, regardless of PCOS status, stress and lack of time are significant barriers to weight loss. However, most interventions developed for the general population are likely to be time-consuming and stress-inducing for its participants. This may explain the high rates of attrition among young women in weight loss interventions that involved strategies developed for the general population. There is an urgent need for further research in order to develop appropriate strategies that would be feasible and sustainable for young women in general, and specifically in PCOS. Furthermore, if unique barriers to weight management exist in PCOS, further research is warranted in order to assess optimal dietary composition and strategies.
Future perspective
We anticipate that there will be comprehensive systematic reviews evaluating the state of research into the effect of weight loss on PCOS, optimal dietary compositions and lifestyle management strategies for weight loss and weight maintenance in women with PCOS. This will inform the development of evidence-based guidelines to guide the clinical management of PCOS. The potential mechanisms involved in energy metabolism in PCOS will be elucidated and any abnormalities that could confer difficulties in weight management will also be identified. Potential treatment strategies for these abnormalities identified. Lifestyle management of overweight and obesity in young women in general and in women with PCOS specifically will incorporate a multidisciplinary approach including a structured focus on behavioral management. Prevention of weight gain will be seen as an important approach to combating obesity.
Executive summary
Polycystic ovary syndrome (PCOS) is a common condition in women of reproductive age and has important reproductive, metabolic and psychological consequences.
Obesity worsens the features of PCOS, while weight loss improves the features of PCOS.
The optimal means of achieving and sustaining weight loss in women with PCOS is not yet known, but a range of dietary strategies exist.
Potential barriers to weight management exist for women with PCOS, but further research is required.
Young women represent a key population that has an increased risk for weight gain in adulthood and unique social and psychological barriers to weight management.
Obesity prevention should address excess weight gain in normal-weight individuals, the progression from overweight to obesity in those women who are already overweight and preventing weight gain in those women who have previously lost weight.
Weight management strategies in young women should focus on a multifaceted lifestyle management approach with the inclusion of dietary, exercise and behavioral advice, and addressing issues such as nutritional requirements in reproductive years, time management and psychosocial stressors.
Footnotes
The authors have no relevant affiliations or financial involvement with any organization or entity with a financial interest in or financial conflict with the subject matter or materials discussed in the manuscript. This includes employment, consultancies, honoraria, stock ownership or options, expert testimony, grants or patents received or pending, or royalties.
No writing assistance was utilized in the production of this manuscript.
