Abstract
Introduction
The effect of natural background radiation on Cancer is still challenging. The investigation of association between external gamma rays and Cancer was the main goal of study.
Materials & Methods
External Gamma rays were measured using a radiation survey meter in 184 urban and rural health centers to estimate the exposure to the population in residential areas of Babol. The dose distribution map was compared to the 5 years radiation induced cancer incidence data from cancer registry center in north part of Iran.
Results
Results showed that although the external gamma ray level in Babol is nearly equal to the average natural background radiation in the world, there is a relatively weak inverse association between local external gamma ray and incidence of Cancer [Correlation coefficient = −0.43, (p<0.01)].
Conclusion
This finding might be due to the inhibition of cancer induction following exposure to the low doses of ionizing radiation and probably can be a confirmation of radiation hormesis. However, due to some uncertainties, the conclusion should be interpreted with caution. Further national and international studies are suggested.
INTRODUCTION
Large populations all over the world continue to be exposed to natural background radiation. The risk of exposure of large populations to small doses of radiation is estimated by extrapolation of deterministic effects at medium to high doses (UNSCEAR, 1958). According to this extrapolation, people believe that ionizing radiation at low doses, produces harmful effects similar to those effects produced by radiation at high doses like nuclear accidents or A-bombs. So, linear non threshold theory (LNT) is the basis of collective dose estimation of the number of deaths following exposure to small doses of natural or artificial radiation (NCRP, 1995). However, the results of many investigations do not support the LNT theory (Jaworowski 1997; Tschaeche 1998). Among various kinds of stochastic effects of radiation, cancer is supposed to be the major cause of radiation induced mortality. Nowadays, the public's awareness about radiation and cancer is growing. However, the mechanisms of radiation carcinogenesis remain unknown. Carcinogenesis is the result of many factors. No single factor induces cancer (Trosko 1996). Radiation mutagenesis as well as non targeted radiation effects are considered to result radiogenic malignancies (Goldberg and Lehnert 2002; Wright 2005). The relationship between radiation and carcinogenesis has been investigated by many researchers (Noguchi et al 1987; Wise 2003) and various kinds of results have been reported. Some of these reports have indicated that cancer rates show a significant increase with low doses of radiation (Cardis et al 2005; Körblein and Hoffmann 2006). Some others have shown no association between low dose radiation and cancer mortality (Allwright et al 1983). There are also some reports indicating inverse relationship between radiation and cancer incidence (Nambi and Soman 1987; Tao et al 2000). This study is an effort to investigate a possible relationship between reported cancer incidence and external terrestrial radiation dose level in residential areas of Babol which are located in Mazandaran province in the north part of Iran.
MATERIALS & METHODS
Environmental terrestrial external gamma radiation dose rates were measured throughout Babol, Iran, over a period of 1 year, with the objective of determining the background radiation level and estimating the exposure to population in residential areas. We used local health centers as dosimetry places because 97% of the population is covered by these health centers. The geographical distribution of population in most of rural areas of Babol is concentrated around the local health centers. So, it seems that the measured doses in health centers can provide a good estimation of population dose. We also made a random rapid dose survey inside some of the people's homes to confirm dose values. No significant changes were seen in dosimetry data compared to local health centers. Radon plays an important role in internal exposure. However, we didn't measure the radon level indoor or outdoor because the main goal of the study was to determine a possible relation between the external gamma rays and cancer. A distribution map of terrestrial external gamma dose rate was also overlaid on geographical map of area under study, using the Photoshop software. This was based on data collected using a Geiger survey meter (Graetz X5CPlus – Germany) calibrated by Iranian Atomic Energy Organization (IAEO). The measurements were taken at 184 (43 Urban and 141 rural) areas. Each measurement was repeated 3 times and the average was recorded as mean dose rate (R mean) for corresponding area. The incidence of cancer for each area was derived from the cancer registry data in each local health center during 5 years (2001 – 2005) and checked by the data from ministry of health and medical education cancer registry organization. The 5 years incidence (5 yr. Inc.) of cancer for each area was calculated by dividing the total number of registered cancer during 5 years to the average number of population (P ave.) of each area for study duration. The descriptive analysis and correlation between 5 years cancer incidence and the average dose rate was done using SPSS-16 software.
Absolute and relative frequency of local health centers and the corresponding number of registered cancers.

RESULTS
The total population in the areas under study and the total numbers of registered cancers during 5 years was 448209 and 832 respectively. The yearly incidence of cancer was calculated as 37 cases in 100000 persons. Leukemia, breast, and GI cancer were the most frequent types of cancer in our study. However, due to lack of reliable pathology diagnosis in some health centers records, we considered crude five years cancer incidence regardless of their types. Table-1 shows the relative and absolute frequency of local health centers and the corresponding number of registered cancers. The minimum and maximum measured dose rate were 31.33 and 95.67 nSv/h respectively (average dose rate = 60.62 ± 12.96 nSv/h or 0.53 mSv/yr). Figures 1 and 2 show the geographical location and dose distribution map of area under study respectively.

The geographical location and map of area under study.
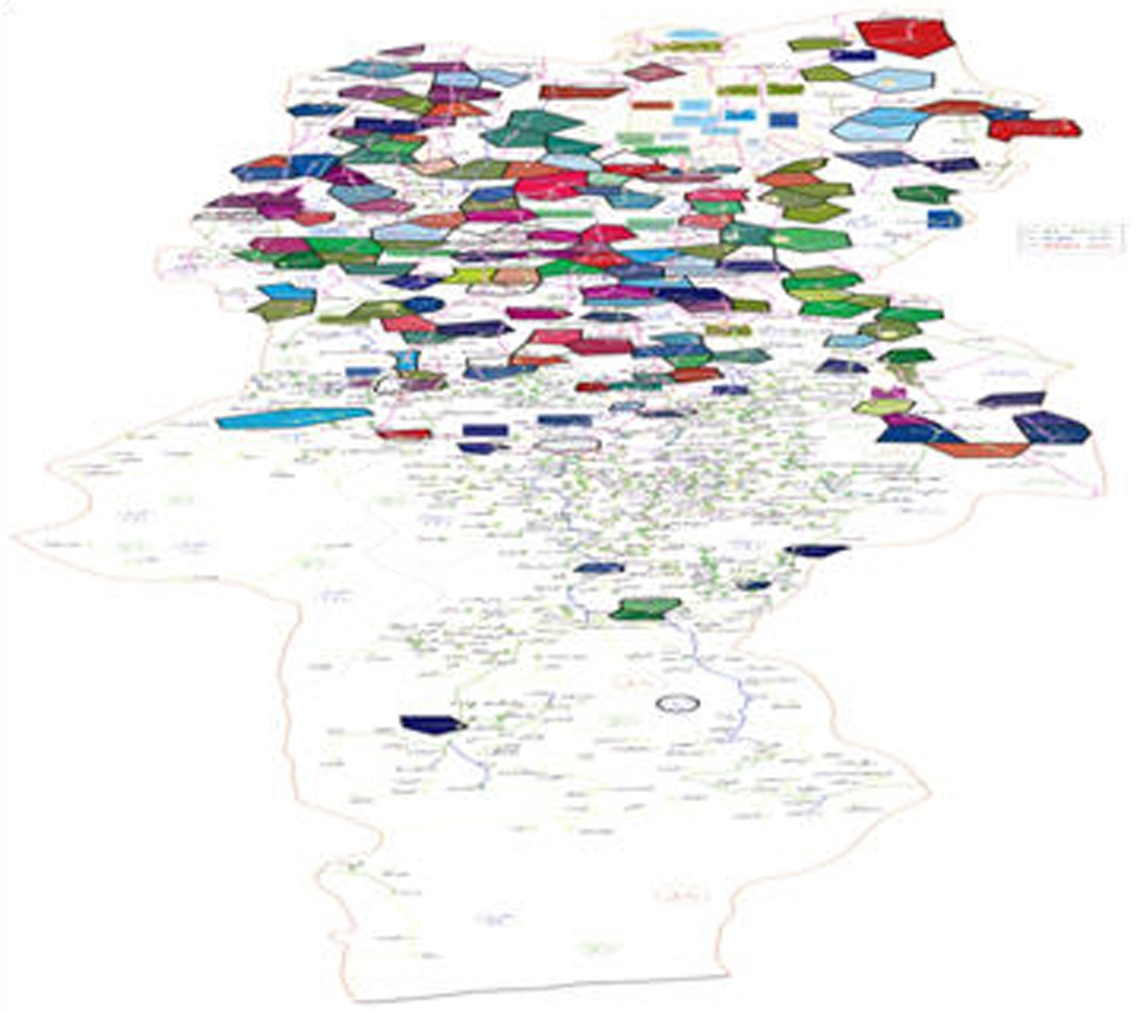
The local external gamma ray dose distribution map of Babol-Iran. The green, blue and red areas show the area with radiation dose range between 31.3 – 53.3, 53.6 – 67 and 67.3 – 95.6 nSv/h respectively.
The correlation coefficient between mean dose rate of each area and 5 years cancer incidence was found to be −0.43 (p<0.01). Figure 3 shows the curve estimation provided by regression analysis. It was also found that the best curve is fitted by cubic model. As figure shows, there was a non-linear weak inverse relationship between cancer incidence and the mean radiation dose. A regression equation that best describe the reported cancer incidence and the mean radiation dose was developed.

The curve estimation between 5 years cancer incidence and mean dose rate. The curve shows the best curve fit provided by regression analysis.
DISCUSSION
Results show that the average dose rate in the area under study is about 60 nSv/h or 0.53 mSv/yr which is about one half of world wide average of 1.1 mSv/yr. The natural background radiation dose/dose rate has been investigated by many researchers in various parts of the world and a wide range of results were reported. The average radiation dose rate in some parts of Nigeria is reported by Ajayi et al (2008) as 60 nGy/h which is similar to the results of the present study. Harb et al (2008) in Egypt and Lu and Zhang (2008) in China have reported the natural background radiation levels about 10 times lower than the value reported in the present study. The terrestrial gamma radiation dose rate in north-west areas and Punjab province of Pakistan (0.34 and 0.28 mSv/y respectively) which were investigated by Rahman et al (2008) and Fatima et al (2008) are about one-half of the mean dose rate of Babol in the present study. Also El-Taher et al (2007) from Egypt, Osmanlioglu et al (2007) from Turkey and Oyedele (2006) from Namibia have measured the dose rate from environmental radioactivity about 45 nGy/h, 0.06 and 0.07 mSv/y respectively which are much lower than the 0.53 mSv/y in the present study especially in two latter cases. Zunic et al (2001) have measured the level of natural radiation exposure to the rural population of Yugoslavia to be as high as 430 nGy/h, which is much higher than the measured values in the present study. It seems that the values of terrestrial external gamma radiation dose rate vary over different soil types, depending the geological characteristics present in the various study areas. Although the mean radiation dose rate in the present study is comparable with some reports and is higher than some others, it is still lower than the yearly dose of less than 1 mSv recommended by ICRP (1991) to prevent the possible radiation effects like cancer and genetic disease.
Results of the present study also show a non-linear inverse relationship between cancer incidence and the mean radiation dose. There are a lot of studies on carcinogenesis of low doses of ionizing radiation from natural sources in the world with various kinds of results. It has shown that radiation induced cancer cases due to soil radioactivity and lung cancer risk from in-door radon may be low (Puskin and Pawel 2005; Farai et al 2006). Another study in Nigeria estimated that for the entire population of 98.5 million, about 1.6 E-4 % annually are at risk of incurring cancer due to exposure to terrestrial gamma radiation induced cancers (Jibiri 2001). Nambi and Soman (1987) have reported an inverse relationship between environmental radiation levels and cancer incidence in India. Tao et al (2000) have indicated that the mortality of all cancers in high background radiation areas (HBRA) in China have been lower than that in the ordinary background radiation area (OBRA), but these differences in incidences are not statistically significant. Sun et al (2000) reported an excess of relative risk (−0.11) of solid cancer mortality after prolonged exposure to natural high background radiation for the same geographical area and time period as the Tao et al (2000) study. Chen and Wei (1991) have reported that although the frequencies of chromosome aberrations in HBRA inhabitants compared with OBRA residents are higher, the differences in the cancer mortality rates for the HBRA and OBRA are not significant. A preliminary study on the population exposed to high level natural radiation in Kerala, India, showed that, there is no evidence that cancer incidence is consistently higher because of the terrestrial gamma-radiation exposure (Nair et al 1999). The 36 years cancer mortality records for inhabitants of the high radon background, and an adjacent control area in Japan revealed that the relative risk of lung cancer death in the high radon background area was lower than in the control area, although the difference was not statistically significant (Mifune et al 1992). A study on lung cancer among population of high background radiation area in Italy showed that the area with high background radioactivity levels has higher lung cancer mortality rates in both sexes but the results are not statistically significant (Forastiere et al 1985). Monfared et al (2006) showed that no significant changes were seen between the health status and cancer incidence of high and ordinary background radiation areas inhabitants in Ramsar, Iran. Körblein and Hoffmann (2006) have indicated that crude cancer rates showed a highly increase with background radiation in a study performed in Bavaria. However, they recommend that the results should be interpreted with caution. We found that the area under study of Babol can be considered as ordinary background radiation area and no hot spots were found in Babol area. Thus lack of increase in cancer incidence could be a predictable finding. However Yalow (1994) has reported that “no reproducible evidence shows harmful effects associated with increases in background radiation of 3 to 10 times the usual levels”. As Figure 3 shows, the cancer incidence decreases with doses between 65–80 nSv/h and doses below 60 n Sv/h induces more cancer incidence. Although we did not measure doses beyond 96 nSv/h, it seems that the cancer incidence trends to increase with the doses over this value. The maximum recorded level of external gamma rays in the present study is about 0.84 mSv/yr which is still lower than worldwide average. So, the study of positive health effects of increased background radiation was not possible. According to Figure 3, both very low and high doses of radiation lead to increased cancer frequency and this is in concordance of radiation hormesis concept of both high and low amounts of a radiation are harmful for health. These findings, expected on the basis of evidence supporting the radiation hormesis phenomenon, indicate that while high levels of exposure to ionizing radiation are indeed harmful, ecologically realistic low levels can be stimulatory and largely beneficial (Hickey et al 1983). This is consistent with data both from animal studies and human epidemiological observations on low-dose induced cancer. It is shown that “the average production rate of endogenous DNA double strand breaks (DSB) per cell per day in the body is about 103 times higher than that of radiogenic DSB from background irradiation” (Pollycove and Feinendegen 2003). According to hormesis theory, low doses of radiation causes DNA damage prevention and repair and immune stimulation. The probable involved mechanisms are damage prevention, damage enzymatic repair (Otsuka et al 2006), damage removal by apoptosis, changes in gene expression (Ikushima 1992) and stimulation of immune response (Liu 1992). In fact low doses of radiation could be proposed as a possible treatment modality in cancer patients (Balaram and Mani 1994). Liu (2003) has supported radiation hormesis in immunity with low-dose radiation. However, despite the increasing number of studies on the radiation hormesis, many gaps in our knowledge still remain. Considering these gaps, it is too soon to state that radiation affects humans in a hormetic manner. Some reports indicate that a low-dose of ionizing radiation induces adaptive protection against radiogenic damage, the net cancer risk can be estimated from the difference between cancer induction and cancer prevention and “it may be lower than predicted by the LNT theory or even negative with more benefit than damage” (Feinendegen 2003). The main uncertainties of our study are that, the other confounding factors which affect cancer incidence are not considered and cohorts are more suitable than cross sectional studies, like the present study, for revealing the correlation between a risk factor and corresponding disease. Due to lack of exactly similar works, it is difficult to conclude that low and very low dose of ionizing radiation may prevent against cancer. So this study just can express the association between radiation and cancer. However, Zou et al (2000) have reported that there is no relation between the exposure to high background radiation in HBRA of Yangjiang in China and the risk of nasopharyngeal carcinoma with or without the adjustment for other confounding factors of cancer. The main aim of the present study was to investigate the association between external gamma rays and cancer incidence. Obviously, this type of study can't provide a cause & effect conclusion. To conclude this matter, we needed a matched control population which in the present study wasn't available. The correlation coefficient between mean dose rate of each area and 5 years cancer incidence is not enough strong [–0.43 (p<0.01)]. So, we can just state that there is a weak inverse association between external gamma rays and cancer incidence. The determination of harmful effects of low doses of radiation is difficult indeed because of methodological problems and difficulty in measuring reliable dose (Borja-Aburto et al 1990). So, further personal dosimetry studies including radon dosimetry are needed along with biological studies. Further cohort analyses are ongoing.
Footnotes
ACKNOWLEDGMENT
This work is financially supported by Babol University of Medical Sciences, research affairs. Authors would like to thank Dr. Hasan Ashrafian for his kindly assistance in providing cancer data. We also appreciate Ms. Tarane Shabestani Monfared for preparing figures and maps.
