Abstract
Objective
A 3-bowl system is used for washing-up eating utensils on many expeditions when running water is not available. The utensils are washed in the first bowl until they are visibly clean, rinsed in the second bowl, and disinfected in the third bowl. The objective of this study was to evaluate the efficacy of this system in reducing bacterial loads on contaminated utensils and to compare it with alternative washing-up methods.
Methods
Different washing-up systems were tested with a simulated dish washing of 5 contaminated mess tins followed by 5 uncontaminated mess tins. Porridge was used to simulate food residue and was mixed with Escherichia coli to produce bacterial contamination. Reduction of bacterial load on the mess tins was measured, as were subjective observations regarding the various systems.
Results
Bacterial load on contaminated tins is reduced when the 3-bowl system is used. Uncontaminated tins become contaminated in bowl 1, but this is then reduced in subsequent bowls. Disinfectant use, especially bleach, produced a marked reduction in bacterial load on contaminated and uncontaminated tins when used in bowl 2. Detergent is needed to remove grease, and a final rinse removes the smell of disinfectant.
Conclusions
Overall, the most effective washing-up system in the laboratory was removal of most food residue with detergent in bowl 1, finish washing with bleach until visibly clean in bowl 2, and a final rinse in drinkable water in bowl 3. This system has advantages over the established 3-bowl system by getting mess tins clean more easily, killing potentially harmful bacteria, and removing the smell and taste of disinfectant.
Introduction
When on expedition or traveling in remote places, there are often limited facilities available for routine hygiene. Water is usually collected from rivers, and toilets tend to be holes in the ground. 1 –3 Diarrhea is a common illness of wilderness travelers, occurring in about one third of expedition participants4,5 and participants on wilderness recreation courses. 6 The incidence of diarrhea may be as high as 74% on adventure trips. 7 There was a 45% occurrence of diarrhea among Appalachian Trail hikers reporting consistent use of water disinfection, implying that wilderness diarrhea is not caused solely by waterborne pathogens, and that poor hygiene, with fecal-oral transmission, is also a contributing factor. 8 Some authors suggest that hand hygiene and cleaning of cooking utensils is more important than treating water, especially to prevent giardiasis. 9 A meta-analysis of water, sanitation, and hygiene interventions to reduce diarrhea in less developed countries found that though water supply and quality are important, hygiene, especially hand washing, is probably more significant. 10 There has been no research into the best systems for hand washing or dish washing in such situations. Unpublished personal observations suggest that 66% of UK-based expedition and adventure travel companies use disinfectant in their washing-up system, and half of these use systems B or C of this study (see the “Methods” section). These systems use 3 washing-up bowls (Figure 1). The utensils are generally washed in the first bowl until visibly clean, rinsed in the second bowl, and disinfected in the third bowl. 1
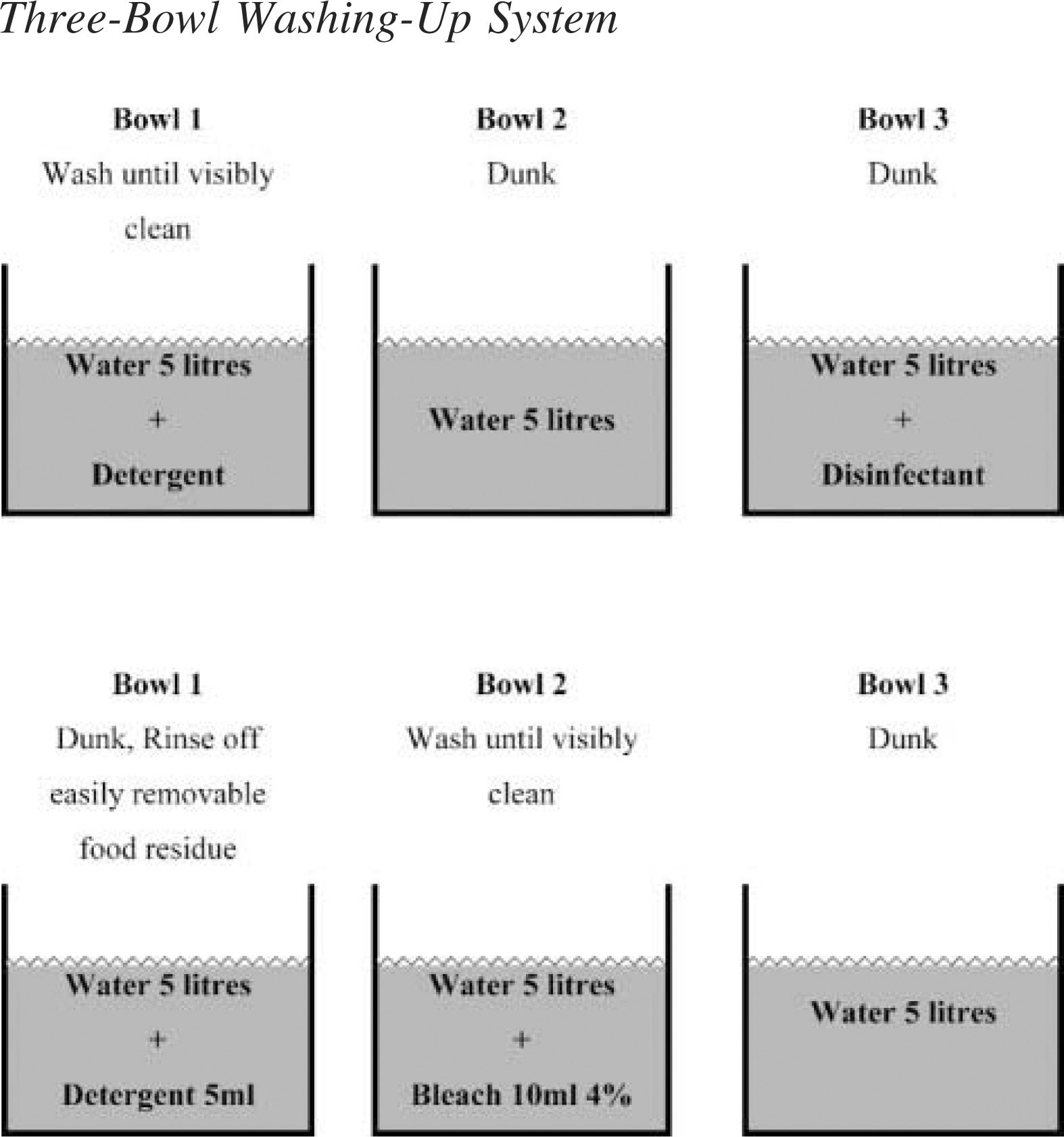
(top) The established 3-bowl washing-up system (system B or C). (bottom) The proposed improved alternative 3-bowl washing-up system (system G).
The aims of any washing-up system are to clean utensils, remove food waste, and kill potential pathogens, thereby preventing illness. Problems with these systems may include objectionable taste of disinfectant remaining on utensils, skin reactions possibly caused or worsened by disinfectant, noncompliance by persons who think such a system is unnecessarily complex, and shortages of water. When thinking about a washing-up system for use in basic camps, one should consider the fact that hand hygiene is difficult; therefore, dirty hands will be washed during the washing-up process, risking disease by fecal-oral transmission of pathogens from hands to eating utensils. Such remote basic camps tend to be in environmentally sensitive areas, which should be protected. Thus, disposal of washing-up water, food residue, and chemicals needs to be considered. Another consideration is the quality of the water used, which may be contaminated from its source.
The objective of this study was to determine the best field washing-up system to clean utensils, reduce bacterial load, and reduce unwanted disinfectant residues.
Methods
Washing-up Systems
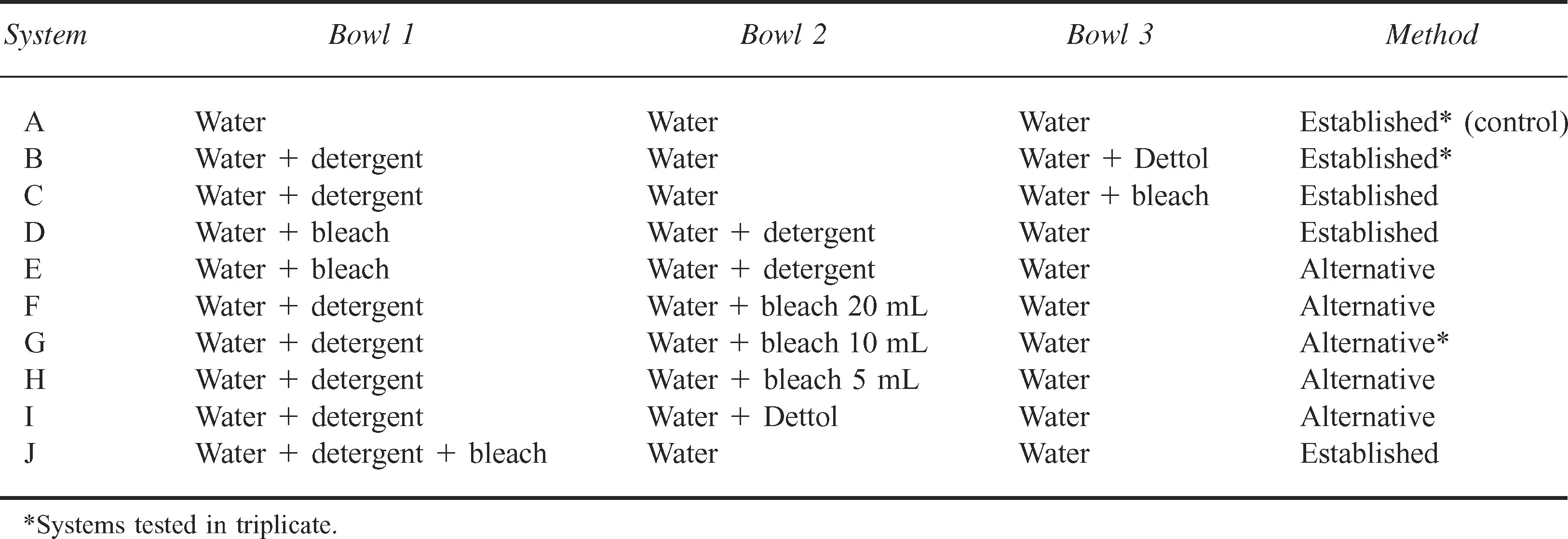
Eighteen 3-bowl systems were initially tested. The results of only 10 of these systems (systems A–J) will be discussed because the others were found to be wholly inadequate. Three of these 10 systems were tested in triplicate to show reproducibility and allow statistical analysis. The other 7 systems were tested only once. The systems varied by the method of washing-up, which was 1 of 2 methods (established or alternative), and by the contents of the 3 bowls. With the established 3-bowl method, tins were washed in bowl 1 until visibly clean, then dunked in bowl 2, and then dunked in bowl 3. With the alternative method, easily removable food residue was washed off in bowl 1, and then the tins were washed until visibly clean in bowl 2 and dunked in bowl 3. When a mess tin was dunked, it was submersed in the water and agitated for a few seconds. Visibly clean washing-up bowls were initially wiped with alcohol Azo-wipes (Vernon Carus Ltd, Preston, UK) and allowed to dry in a drying cabinet before being filled. Each bowl was filled with 5 L of sterile distilled water at room temperature. Most systems had a bowl with added detergent, which was 5 mL of Sainsbury's original washing-up liquid (Sainsbury's Supermarkets Ltd, London, UK) (not claiming to be antibacterial). Most systems also had a bowl with added disinfectant, which was either Dettol (4.8% wt/vol chloroxylenol; Reckitt Benckiser Healthcare UK Ltd, Hull, UK) or bleach (4% sodium hypochlorite). Unless otherwise stated, 20 mL of each disinfectant was used. Table 1 shows the systems that were fully studied. System A did not use detergent or disinfectant, rather, just 3 bowls of water to act as a control.
Variations of the 3-bowl washing-up system that were tested
How the Systems were Tested
The different washing-up systems were tested with a simulated dish wash of 10 porridge-coated mess tins. The first 5 tins to be washed (tins 1–5) were coated with porridge contaminated with Escherichia coli, whereas the second 5 tins (tins 6–10) were uncontaminated. To remove the method of manual cleaning as a variable in this study, the tins were washed without a sponge, dishcloth, or scourer. A 4-cm2 sample area on the mess tins was marked with a sterile cardboard template. This area was swabbed, and the collection was suspended in 10 mL of sterile saline. The suspension was then diluted by factors of 10, if needed, to give readable counts. One milliliter of this sample was then mixed with Columbia Blood Agar Base (Oxoid, Basingstoke, Hampshire, UK) agar in a pour plate. Mess tins 1, 5, 6, and 10 were sampled before washing-up, after being in bowl 1, after being in bowl 2, and after being in bowl 3. After setting, the pour plates were incubated overnight at 37°C in air. The colony forming units (CFUs) were then counted, and the data were adjusted according to the dilutions made. By this method the threshold of detection was 2.5 CFUs per square centimeter of mess tin. The author made subjective, unblinded observations regarding the ease of use and the smell of disinfectant remaining on the mess tins.
How the Porridge was Contaminated
Twenty milliliters of Iso Sensitest Broth (Oxoid) was inoculated with ATCC 25922 E coli and incubated overnight at 37°C to produce a 109 CFUs·mL−1 concentration. The concentration was checked for each broth by diluting by 1000 and 1 000 000 and plating out with a Spiral Plater (Don Whitley, Shipley, West Yorkshire, UK). The E coli broths used were all of very similar inocula (from 4 × 108 CFUs·mL−1 to 2.5 × 109 CFUs·mL−1). Porridge soil was made daily by boiling 300 mL of tap water in a glass beaker over a Bunsen burner. Porridge oats (37.5 g) were then added. This mixture was simmered and occasionally stirred until creamy. To simulate greasy expedition food, 10 mL of sunflower oil was mixed in before the porridge was allowed to cool on the bench. The porridge was divided into 10 portions of 20 g. Five of these portions had 2 mL of the 109 CFUs·mL−1 E coli broth added. This was mixed in a vortex machine to give a concentration of 108 CFUs E coli per 1 g of porridge. Ten metal mess tins were autoclaved. Tins 1 to 5 were spread with 20 g of porridge with the added E coli. Tins 6 to 10 were spread with 20 g of uncontaminated porridge. After porridge application, the tins were left for approximately 1 hour before they were washed-up.
Statistical Methods
The computer program Instat2 (GraphPad Software Inc, San Diego, CA) was used for statistical analysis. Comparison of the log10 bacterial count reductions from the triplicate laboratory testing was analyzed with 1-way analysis of variance and the Student's t test.
Results
Table 2 shows the bacterial load as CFUs per square centimeter on the mess tins at the start and after each bowl washing for systems A through J.
Bacterial load for tins 1 and 5 at the start and after each bowl for systems A through J
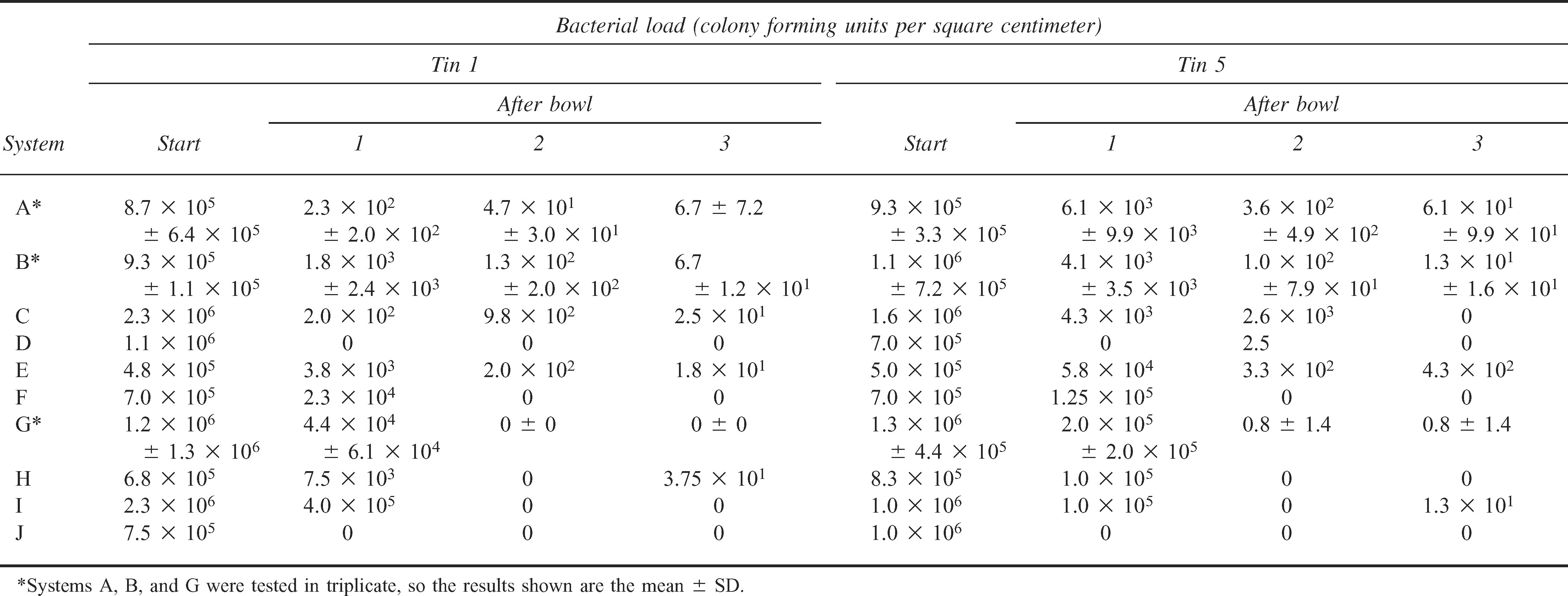
Bacterial load for tins ± and 10 at the start and after each bowl for systems A through J
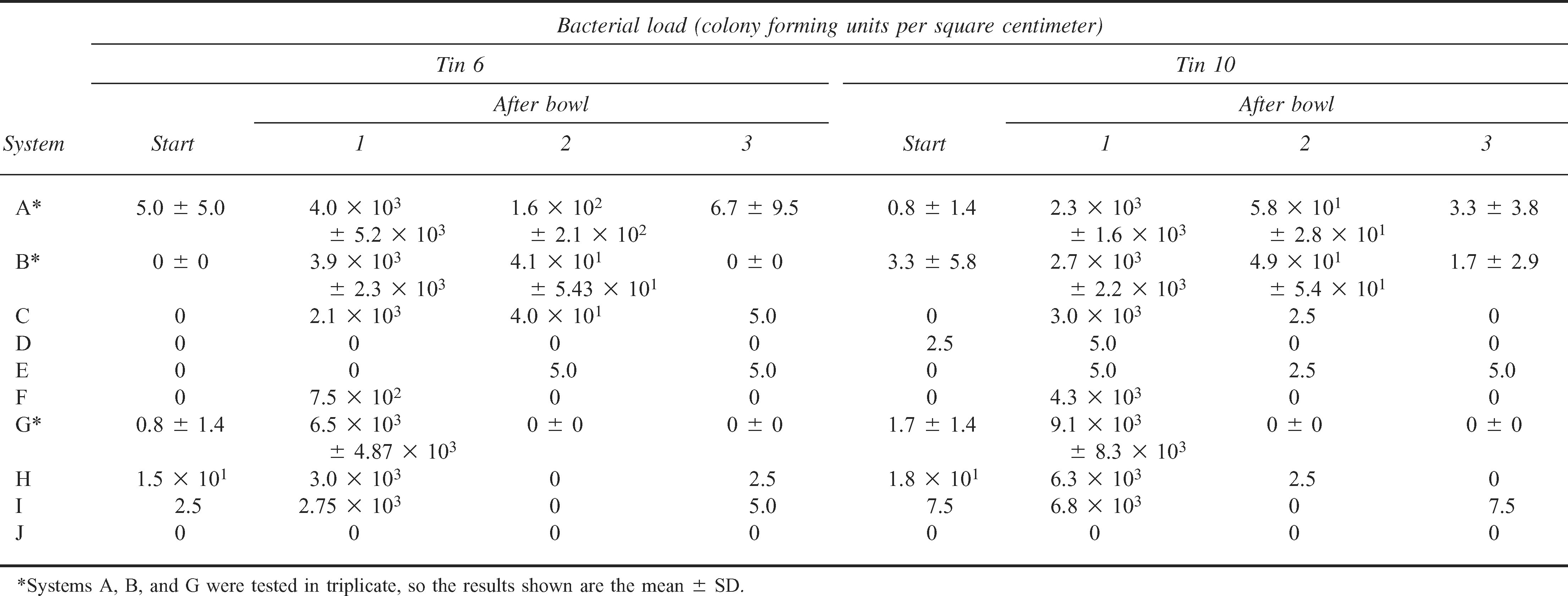
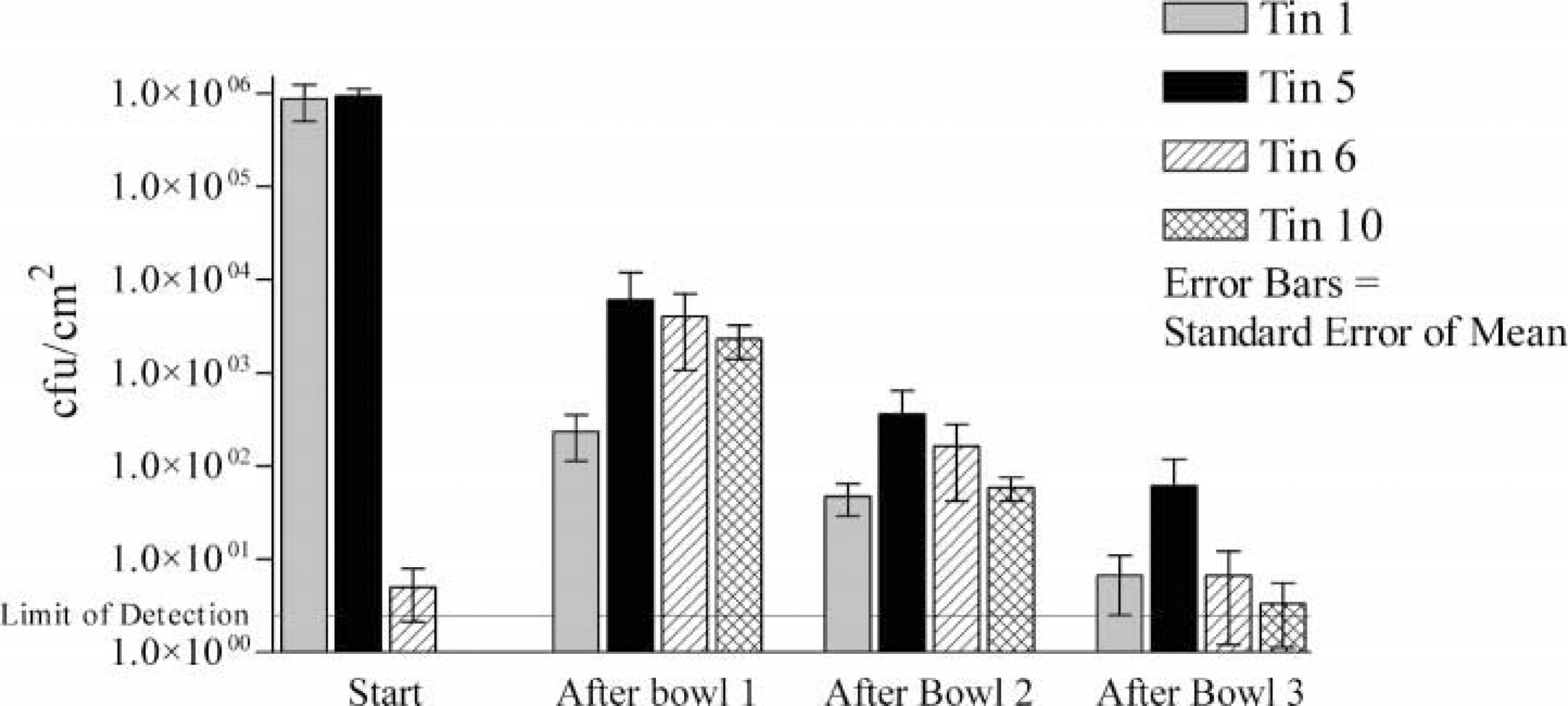
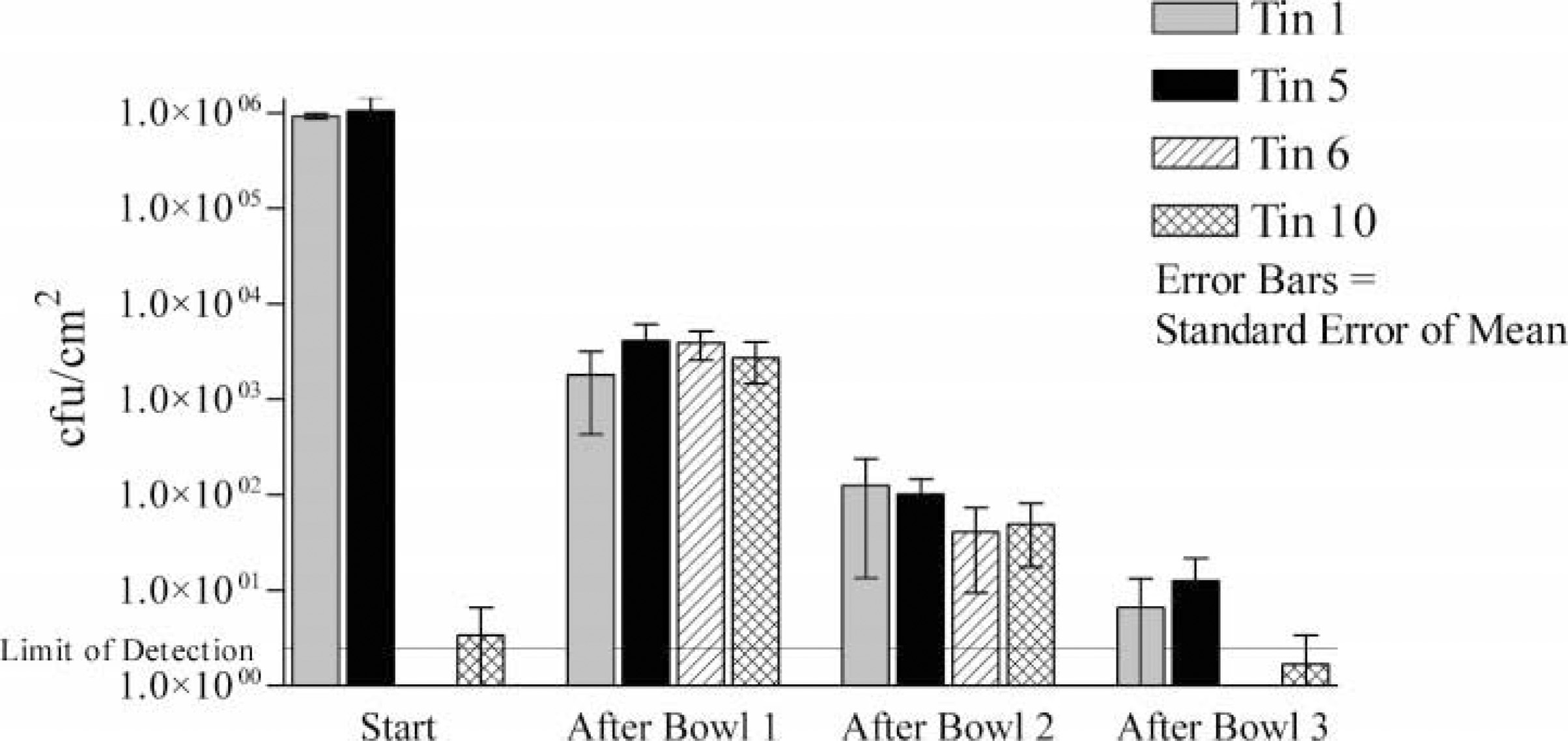
For system A (Figure 2), the bacterial load on contaminated tins 1 and 5 was reduced by dilution. The bacterial load on uncontaminated tins 6 and 10 dramatically increased before the dilution effect. The mess tins were still greasy at the end of the systems. For system B (Figure 3), again the bacterial load on contaminated tins was reduced, but the bacterial load on uncontaminated tins dramatically increased before being reduced in bowls 2 and 3. The mess tins were clean but smelled of Dettol at the end of the system. System C gave very similar results to system B. System D removed most bacteria from tins 1 and 5 in bowl 1 and prevented tins 6 and 10 from becoming significantly contaminated. The mess tins were clean and did not smell of bleach at the end of the system. The disadvantage was that it was very difficult to remove all the food residue in bowl 1, and in the field there would therefore be a tendency to wash some food residue off in bowl 2. System E had the same combination of bowls as system D but with the alternative method to simulate the extra cleaning that would invariably happen in bowl 2 as bowl 1 became dirty. Tins 1 and 5 were not satisfactorily decontaminated, and tins 6 and 10 were more contaminated than in system D. For system F, swapping the detergent and bleach bowls and still using the alternative method reduced bacterial load below detectable levels by bowl 2. This system was easy to use, and at the end of the system the mess tins were clean and did not smell of bleach. For system G (Figure 4), halving the bleach concentration still meant the bacterial load fell below detectable levels by bowl 2 and reduced the bleach exposure to the user. For system H, reducing the bleach by half again resulted in some breakthough contamination by bowl 3. For system I, using Dettol in bowl 2 with the alternative method was easy but was not as effective at reducing contamination as was bleach. For system J, combining the detergent and bleach was effective at reducing bacterial load to below detectable levels but produced noxious fumes and left the mess tins smelling strongly of bleach.
Mean bacterial counts on mess tins at the start and after each bowl for system A (established method with water + water + water, ie, control system). CFUs indicates colony forming units.
Mean bacterial counts on mess tins at the start and after each bowl for system B (established method with detergent + water + Dettol). CFUs indicates colony forming units.
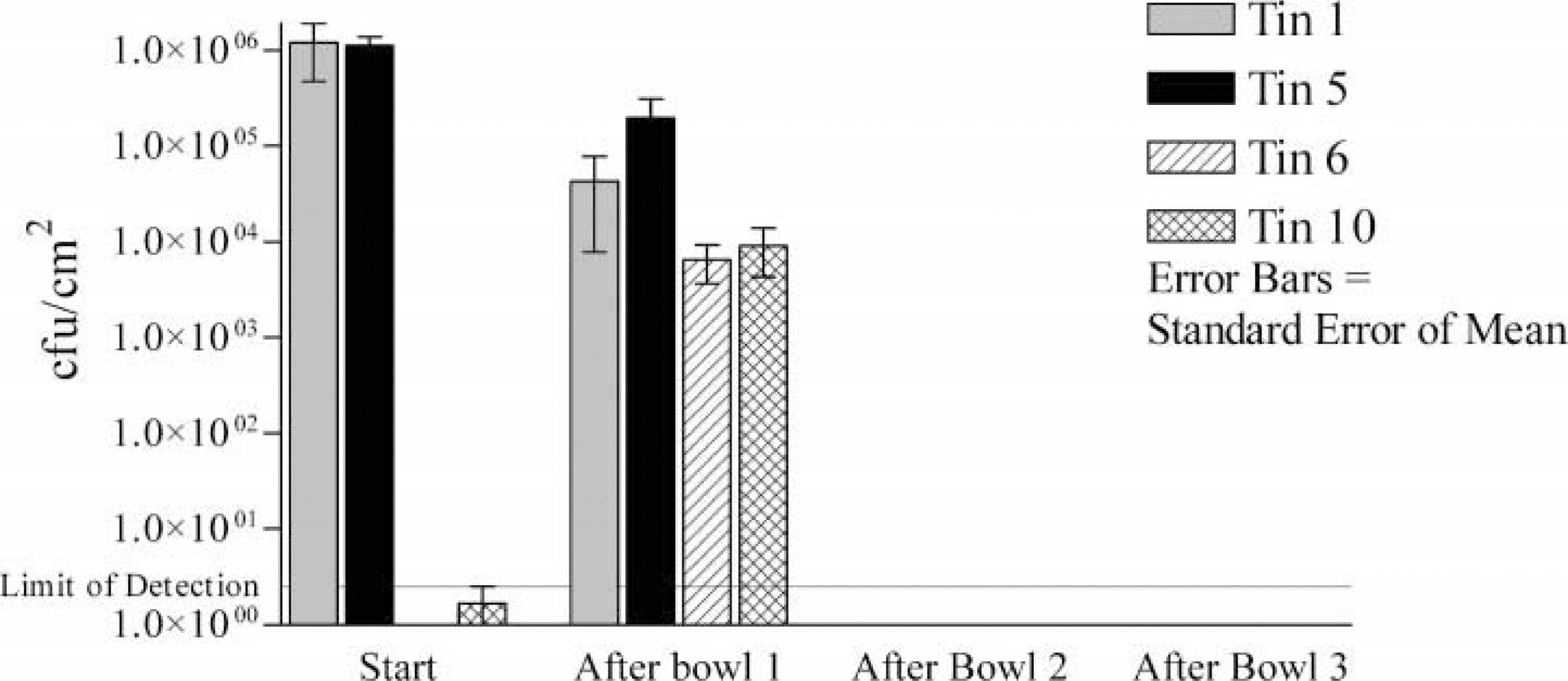
Mean bacterial counts on mess tins at the start and after each bowl for system G (alternative method with detergent dunk + bleach 10 mL wash + water). CFUs indicates colony forming units.
Subjective Observations
Grease was removed from mess tins only after they had been in a bowl containing detergent. By using the established 3-bowl method, the water in bowl 1 became filthy, thus making it increasingly difficult to get mess tins visibly clean. It was easier to use the alternative method where most food residue was removed in the first bowl and then the mess tin was made visibly clean in the second bowl.
Statistics
To compare reduction in bacterial load, it is usual to consider the log10 reduction in CFUs. By using 1-way analysis of variance, there was no significant statistical difference among the three 3-bowl systems tested in triplicate (systems A, B, and G) for any of the tins. If only the first 2 bowls of each of these systems are considered by using the Student's t test system, system G was significantly better than system A for tin 1 (P = .0268), tin 5 (P = .0160), tin 6 (P = .0090), and tin 10 (P = .0115) and significantly better than system B for tin 5 (P = .0100) and tin 10 (P = .0540). This is important for situations when water availability is reduced and only 2 bowls are used.
Discussion
All systems except system A worked well to clean utensils. The systems using the alternative method of washing-up (systems E–I) were easier to use, because removing the final bits of food residue was easier in a fairly clean bowl 2 than in a dirty bowl 1. Systems D, F, G, and J were the best for reducing bacterial load because they all involved washing (as opposed to just dunking) the mess tins in bleach. Systems A and D through I left the mess tins free from a smell of disinfectant. The only 2 systems that were included in all these “best” categories were systems F and G. Because system G uses less bleach, this system should be considered the best overall.
The best system, system G, provided very good bacterial load reduction and left the mess tins clean, not greasy, and not smelling of bleach. Also, the system was easy to use as tested. Systems B and C are the most commonly used systems at the moment, but they do not have very good bacterial load reduction, they leave the mess tins smelling of disinfectant, and they are not as easy to use because of the build up of food residue in bowl 1. System D left mess tins clean and not smelling of bleach and had good bacterial load reduction; however, as with systems B and C, because of the build up of food residue in bowl 1 with the established method, it was not easy to use as tested. On expedition, persons would likely start moving to bowl 2 to finish removing food residue once bowl 1 became dirty. System E is an example of how a good system (system D) will fail if the user starts washing more in bowl 2 than in bowl 1. A good system must still be good when users opt for the easy option. System G fulfils this criterion, but system D does not.
Compared with variations (systems B and C) where only a quick dunk in disinfectant occurred, getting the mess tins visibly clean in disinfectant (systems D, F, G, and J and, to a lesser extent, H and I) worked well because of the increased contact time between the utensils and disinfectant while washing.
A useable system must also minimize potential problems such as objectionable taste of disinfectant remaining on utensils, skin reactions possibly caused or worsened by disinfectant, noncompliance by persons who think such a system is unnecessarily complex, and shortages of water. A final rinse bowl should remove the smell and taste of disinfectant from mess tins and allow rinsing of hands, thereby possibly reducing the risk of skin reactions. Disinfectant used in bowl 3 leaves a residual smell. In unpublished research, 13 of 20 expedition team members using such a system could taste the disinfectant at the next meal. Only 5 of 20 could taste disinfectant when system G was used. Whether residual disinfectant on mess tins is beneficial in preventing contamination between meals has not been tested. A final rinse in water that may be contaminated from its source, the washing-up bowl, or incorrect use could cause problems. To avoid these situations, the washing-up bowl should be cleaned and disinfected and preferably stored dry and away from potential contamination, the water used should be treated to the same standard as drinking water, and the group should be educated that bowls must be used in the correct order and only for washing-up. If these standards cannot be met, a final rinse may not be a safe option.
All 3 bowls may not always be feasible if, for example, water is very scarce, carrying 3 bowls is difficult, or a final rinse bowl is not safe. Systems D, F, and G and perhaps H and I are good with only the first 2 bowls, with the disadvantage of a disinfectant smell. If only the first 2 bowls of systems A, B, C, and E are used, there is too much bacterial contamination remaining on mess tins. System J may be useable with only 1 bowl if water is very scarce and users are willing to tolerate the smell and fumes.
Comments
The washing-up systems’ ability to reduce bacterial load was tested with E coli in the porridge. This was chosen to model enterotoxigenic E coli, which causes 50% of travelers’ diarrhea. 11 Other gram-negative bacteria such as Campylobacter, Shigella, and Salmonella are likely to respond in a similar way. Gram-positive bacteria, such as Staphylococcus aureus, and parasites may or may not respond in the same way. The porridge was contaminated to simulate bacterial contamination that could occur from a variety of sources. On expeditions, contamination is unlikely to be in the food but to come from utensils not washed up promptly, washers’ hands, washing-up bowls, and any scourers used. In this study, only tins 1 to 5 were initially contaminated. This showed the effect of washing contaminated tins and also contaminated the water to show what happens when uncontaminated tins (tins 6–10) are washed in contaminated water.
Additional suggestions regarding washing-up derived from a review of the literature include using hot water, if available,12,13 probably in bowl 1; using a scourer, if needed, in bowl 2 with the disinfectant to prevent contamination of the scourer12,14; allowing utensils to air dry after washing 15 –17; and cleaning the washing-up bowls and allowing them to dry. 14 –16 If the bowls are wet before use, they may harbor potentially harmful bacteria and should be suitably cleaned with disinfectant. 14 If there is an outbreak of diarrhea and vomiting during the expedition, the concentration of bleach should probably be increased up to 100 mL in 5 L of water, which is similar to the concentrations used for cleaning in hospitals during viral gastroenteritis outbreaks. 18 All other aspects of camp hygiene, especially hand washing, should be maintained at a high level as well.
Limitations
Only 3 systems were tested in triplicate because of time constraints. More testing of these systems and of the others would allow better statistical analysis. The results were useful, however, to determine their potential usefulness and which systems should be tested in triplicate.
None of the disinfectants were inactivated at the time of sampling. This may mean the results show higher bacterial count reductions than would occur in real life, as contact time would have been longer. However, the concentration of bacteria is unlikely to be as high in real life as those used here. Very high inoculums were used in this study to stress the systems; thus, this may be considered a limitation.
The use of a sponge or scourer was not included in these experiments to keep the study focused on the effects of various wash solutions and their order. Because these cleaning implements are likely to be used on expedition, their effect on reducing contamination should be evaluated in future studies.
Bacterial count reduction in the laboratory may not be the same with variable users in a basic campsite and may not equate to reduced gastroenteritis on expeditions and adventure travels.
The qualitative results, regarding ease of use and smell, are limited because they were assessed by the unblinded author. Questionnaire studies have been carried out on participants in the field comparing qualitative aspects of systems B and G, and the results are being analyzed for future publication.
Other areas of personal hygiene, such as hand washing, were not investigated and probably play a large role in wilderness and expedition illness rates. 8 –10,19
The effect of the proposed new washing-up system on other potentially pathogenic organisms (eg, S aureus, Salmonella, Shigella, and parasites) should be tested.
Work should also be performed to evaluate the best way to protect the environment when disposing of detergents and disinfectants on wilderness expeditions.
Recommendations
The popular 3-bowl washing-up system (systems B or C) should be replaced with an alternative system (system G), that is, remove most food residue and grease with detergent in bowl 1 and then wash with bleach until visibly clean in bowl 2. Then, if safe water can be used in a suitably cleaned bowl 3, the utensils can be rinsed to remove disinfectant residue. If there is a shortage of water or a rinse bowl cannot be achieved safely, then the first 2 bowls of this system can be used alone to provide good bacterial killing and mess tin cleansing with the disadvantage of some disinfectant residues.
Footnotes
Acknowledgments
I would like to thank the following for their help in this research: Prof Alasdair MacGowan, Dr Robin Howe, Dr Christopher Redman, and Wing Commander Andy Green for their advice; Dr Karen Bowker and the laboratory staff for all their help; and Dr Rosy Reynolds for advice on statistical analysis.
*
Presented at the 9th Conference of the International Society of Travel Medicine, Lisbon, Portugal, May 1–5, 2005.
