Abstract
This article reports for the first time the medical significance of the Levantine viper (Macrovipera lebetina) in India. This snake is found in India in the mountainous regions of Jammu and Kashmir and is capable of causing necrosis and hemostatic manifestations, as seen in the case reported here. It is thus a class II snake of medical significance, as defined by the World Health Organization grading scale. This finding reinforces the recent decision by the Indian Government to abandon the term “Big Four” to describe important venomous species in India. Levantine viper venom is not included in the manufacture of Indian polyvalent anti–snake venom; thus, there is no current antidote for this species. Recommendations are to manage confirmed bites from this species without Indian anti-snake venom. In areas where this snake is found to be a significant contributor to envenomations, alternative anti-snake venoms can be sourced from outside India for use in high-risk groups. Continuing attention to preserving dead snakes brought with the victim for reliable identification remains a high priority.
Keywords
Until recently, the entirely unhelpful title of the “Big Four” snakes of medical significance has predominated in India. This definition has been largely propagated by “herpetologists” with little understanding or experience of the medical significance of venomous species. 1 Recent papers have shown that the term “Big Four” is misleading and counterproductive, as there are many more than 4 medically significant species in India.2,3 The majority of these are not countered with an effective anti–snake venom (ASV) due to the belief that only 4 species need be covered in the current polyvalent ASV mix. 2 In October 2007, the Indian Government's Department of Health and Family Welfare rejected the notion of the “Big Four” and instead adopted the concept of snakes of medical significance, as outlined in a World Health Organization (WHO) paper. 4 This model divides medically important snakes into 2 main classes: class I, those commonly causing death or serious disability, and class II, those that uncommonly cause bites but are recorded to cause death or local necrosis. 4
As a result of government initiatives, many more hospitals are now preserving dead snakes brought with patients in an attempt to definitively identify all snakes of medical significance in India. This case study reports the discovery of a further snake of medical significance in India, the Levantine viper (Macrovipera lebetina). The species is not well reported in the literature and is found in a number of neighboring countries, with a range extending to North Africa.5,6
Case report
On July 7, 2007, a 33-year-old male soldier, who had been on sentry duty at an altitude of 7800 feet, retired to bed in an army bunker, on a sturdy cot, in the state of Jammu and Kashmir. At 2345 hours, he was awakened by a sharp pain in the little finger of the left hand. On wakening, he saw a large snake in the room, and it was killed by his colleagues.
The snake was 94.5 cm in length and was initially thought by the soldiers to be a northern saw-scaled viper (Echis sochureki). The snake was preserved and subsequently examined using standard morphologic features—supranasal shield shape, head shape and size, and scale keeling 5 —by an experienced herpetologist (IDS) and was identified as a Levantine viper (M lebetina).
The victim complained of severe pain at the bite site, and a tourniquet was applied above the wrist and on the upper arm just above the elbow with 2 handkerchiefs. This tourniquet did not occlude arterial flow, as evidenced by the presence of intact distal pulses when evaluated at the first point of medical contact. A number of superficial incisions were made around the bite site in an attempt to remove venom.
On presentation to local medical staff, the victim's pulse rate (PR) was 88 beats/min and the respiratory rate (RR) was 20 breaths/min. Measured clotting time was 3 minutes (normal range < 10 minutes). 7 There was swelling and discoloration at the bite site. The patient was given tetanus toxoid and antibiotics.
The victim was transported to a nearby military hospital by a vehicle and arrived at 0245 hours on July 8, 2007. On arrival, the patient had edema extending to the hand, with bluish discoloration and necrosis around the bite site. By 0345 hours, the swelling had progressed to the elbow. The patient's PR was 76 beats/min, blood pressure was 100/60 mm Hg, and RR was 20 breaths/min. His pupils were reactive to light, and there were no other symptoms and no signs of neurologic impairment.
A blood sample was taken at 0330 hours and revealed a total white blood cell count of 15.5 × 109/L, with 81% polymorphonuclear leukocytes, hemoglobin (Hb) 13.3 gm/dL, packed cell volume (PCV) 41%, and platelet count 156 × 109/L. The patient's bleeding time (Ivy method 7 ) and clotting time (Lee and White method 7 ) were within the normal range. Blood urea nitrogen (BUN), serum creatinine, serum glutamic oxaloacetic transaminase (SGOT), and serum glutamic pyruvic transaminase (SGPT) were normal, as was a urinalysis.
At 0400 hours, the swelling had markedly increased and rapidly crossed the wrist joint. Given this degree of progression, 5 vials of Serum Institute of India polyvalent ASV reconstituted in 500 mL normal saline were administered over 1 hour. No skin sensitivity test was performed at the hospital (in line with the local protocol). A prophylactic regimen to prevent ASV reactions was in place and the patient received 25 mg promethazine and 100 mg hydrocortisone intravenously as premedication 5–10 minutes before commencement of ASV. The patient was closely monitored for any signs of ASV reaction during the infusion of ASV over 1 hour. No such reaction occurred.
A blood sample was taken at 0600 hours and sent for analysis. The results revealed Hb 11.8 gm/dL, PCV 37%, and platelets normal. Bleeding and clotting times, BUN, creatinine, and serum enzymes SGOT and SGPT remained normal. Urine showed no signs of abnormality. The patient's PR was 74 beats/min, blood pressure was 116/54 mm Hg, and RR was 22 breaths/min.
Routine clotting tests were carried out every 2 hours for the first 24 hours and then daily after that period, which was in line with local practice. All clotting tests were normal, and there were no signs of coagulation disturbance or thrombocytopenia. The patient's urine output remained normal, and there were no laboratory findings of renal impairment.
In line with the local protocol, 2 vials of polyvalent ASV were given in 100 mL of normal saline by intravenous infusion over 1 hour at 2-hour intervals until the pain ceased. In the local protocol, pain is regarded as a clinical endpoint for ASV administration. The victim received 14 vials over the next 14 hours, with no adverse reactions. In total, 19 vials of ASV were administered.
By 1545 hours on July 8, 2007, 15 hours after the bite, the swelling had extended to the left pectoral region. In addition, the patient had ecchymoses on the upper arm, deltoid, and pectoral region.
On July 10, 2007, 48 hours after the bite, the patient had continuing severe swelling of the left hand and arm. The patient complained of severe pain in the hand, pain on passive stretching of the fingers and wrist joint, and the skin of the hand was tight and shiny. In the absence of equipment to objectively measure intracompartmental pressure, clinical signs and symptoms were used to determine that a fasciotomy was required to prevent ischemic damage to the hand as a result of the swelling. A fasciotomy over the palmer aspect of the hand was carried out by linear incisions and drainage.
The necrosis of the left little finger at the bite site continued to increase until the whole finger was involved (Figure), and on July 20, 2007, 12 days after the bite, the digit was amputated at the level of the proximal inter-phalangeal joint. Post operative care was administered until the patient was discharged on August 10, 2007 for 6 weeks of convalescent leave.
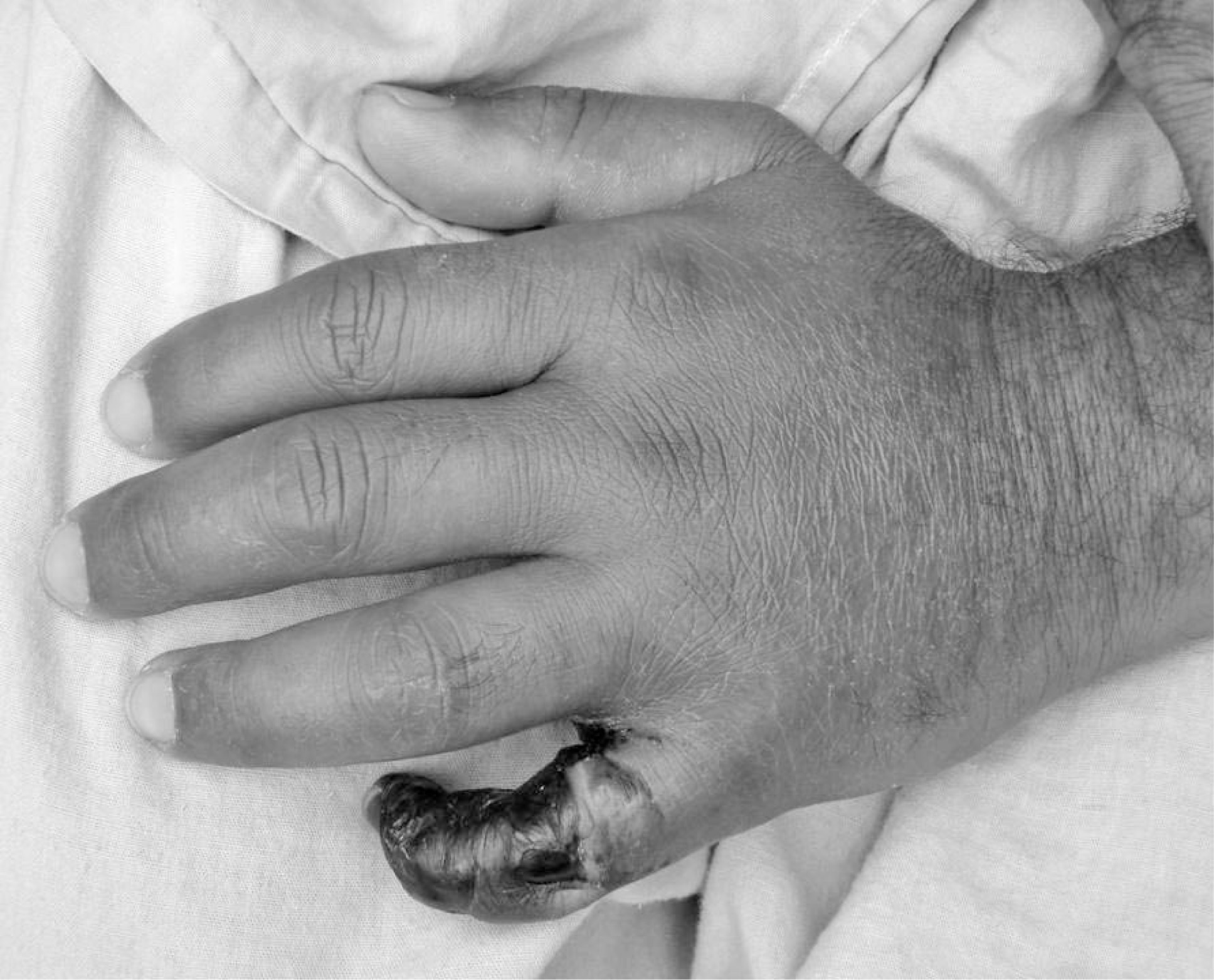
Necrosis of the patient's finger at day 4.
Discussion
The Levantine viper (M lebetina) is a true viper that reaches a length of up to 1.6 m. Its range includes Jammu and Kashmir in India, the Northwest Frontier, and the Balochistan provinces of Pakistan, through the Middle East, Israel, Syria, Lebanon, and into North Africa, Tunisia, and Libya. Its preferred environment is mountains and rocky environments, and it is frequently found beneath rocks.5,8 It is slow moving, which has led to the historic view that this species is deaf (even before the recognition that all snakes are in fact deaf to airborne sounds). The Deaf Adder mentioned in the Bible has been presumed to be this species. 9 It is also, as in this case, found at high altitudes, including it amongst the small group of high-altitude medically significant species. 10
Reported bites in the literature are rare, the most significant being Corkill's classic paper on snakebites in Iraq. 9 In Corkill's review, only 2 confirmed Levantine viper bites are reported; 13 others are identified as resulting from this species on the basis of symptoms or locality and are thus unreliable. Although reports of 50% mortality rates from this species are made, based on Corkill's paper, this is misleading as the series was so small. 11
Corkill reported symptoms of severe swelling, necrosis, and bleeding with hematuria, epistaxis, and melena. The severe swelling, pain, necrosis, and ecchymoses seen in our case mirrored these symptoms. In the second of Corkill's reported cases, the victim underwent sloughing of the tissue on the bitten finger.
Venom analysis has demonstrated that Levantine viper venom contains enzymes that activate both factor X and factor V, in addition to metalloproteinases.12,13 Clinically, no effect on coagulation was evidenced in this case, although there was a small drop in Hb and PCV.
The current Indian ASV does not contain antibodies raised against the Levantine viper and is, therefore, likely to be ineffective. We have been unable to find any studies referring to crossprotection from other ASVs not raised against this species. There is a polyvalent ASV produced by the Institute of Immunology, Zagreb, Croatia, that could be sourced by institutions such as the armed forces who have personnel operating in environments where this species is found. There may, of course, be problems related to the regional variation of the venom used to produce the European Levantine viper ASV, but in the absence of a locally produced equivalent, it is probably worth trying in a significantly envenomed victim.
This case provides further evidence of the lack of applicability of the notion of the “Big Four” snakes in India. 2 Both the Levantine and Russell's viper (Daboia russelii) are large brown true vipers and inhabit the same area. In the absence of dead snakes to verify the species responsible for a bite, even the number of bites resulting from a key species such as Russell's viper cannot be accurately assessed.
India has 4 species of cobra (Naja naja, N kaouthia, N oxiana, and N sagittifera), 6 species of krait (Bungaus caeruleus, B fasciatus, B sindanus sindanus, B sindanus walli, B niger, and B andamanensis), the Russell's viper (D russelii), 2 species of saw-scaled vipers (Echis carinatus and E sochureki), the king cobra (Ophiophagus hannah), and at least 1 deadly pitviper (Hypnale hypnale).3,5,14 With the Levantine viper, this would place the current number of snakes of medical significance at 16! The remaining pitvipers and coral snakes are of unknown medical significance. The current Indian polyvalent ASV is prepared using venom from just 4 of these species.
In order to establish whether further ASVs are required, it is essential to assess the number of bites from species not included within the current ASV configuration. As in this case, the initiatives to encourage the preservation of dead species brought with the victim and to ensure that they are correctly identified will enable such an assessment to be carried out. 15 Interestingly, this was a key recommendation of Corkill's paper in 1932. 9 The hospital concerned in this case study will continue to preserve and analyze species responsible for bites in the geographic area and to develop a more detailed study of the offending species.
In the absence of an effective ASV, confirmed bites from this species should be managed conservatively, as in other cases of species not covered by the current polyvalent ASV. 3 Attention should be paid to the high likelihood of necrosis, and bleeding parameters should be carefully assessed. Any clinical assessment of compartment syndrome should be accompanied by objective measurement of the compartment pressure. No polyvalent ASV should be administered to confirmed bites from this species.
A further interesting feature of this case is that the victim was bitten while sleeping on a cot. It is a frequent tenet of snakebite literature that sleeping on a cot, rather than on the ground, will prevent snakebite. 1 It has also been suggested that this practice is responsible for higher numbers of bites among Hindus, who sleep on the floor, rather than Muslims, who mainly sleep on cots. 16 However, in areas such as the Tharparker District of Pakistan, with a predominantly Muslim population, bites while sleeping are still common. Sleeping on a cot may provide some protection against snakebite, but it is not certain. In our case, the victim was bitten in a military bunker, while sleeping on a cot, demonstrating the lack of effectiveness of snakebite prevention by physical means.
