Abstract
Objective
To evaluate animal-caused fatalities in New Mexico using data collected during medicolegal death investigations, including toxicology, survival interval, and circumstances.
Methods
A retrospective review of the computerized database and hard copies of files from a centralized, statewide medical examiner's office, excluding deaths due to zoonotic diseases and motor vehicle collisions involving animals.
Results
Between 1993 and 2004, 63 deaths caused by animals were reported in New Mexico. The majority of decedents were male (46/63, 73%) and non-Hispanic white (33/63, 52%). Horses were the most commonly implicated animals, with 43 (68%) deaths due to a person being thrown from, crushed, dragged, or kicked by a horse. Cattle caused 9 deaths (14%), dogs caused 3 (5%), and venomous animals caused 3, whereas a bear was responsible for 1 death. Ten decedents (16%) had alcohol present at the time of death, and 8 would have been over the legal blood alcohol concentration for driving (0.08%). Ten deaths (16%) were work-related and included deaths of jockeys and ranch workers. The majority of deaths (42/63, 67%) occurred in remote locations, potentially delaying access to treatment. Survival intervals ranged from 1 day to 33 years.
Conclusions
Whereas both human and animal behavior can be difficult to predict, a review of animal-caused fatalities investigated by a medical examiner revealed that in many cases, deaths could have been prevented by either the use of protective gear or alterations in human behavior.
Introduction
Interactions between humans and animals, whether recreational or occupational, are usually rewarding and enjoyable. Unfortunately, given the unpredictability of both human and animal nature, encounters between animals and humans sometimes result in tragic consequences. Previous studies have focused on the damage and deaths caused by dog bites, 1 –4 national trends as reported by CDC Wonder,5,6 and occupational farm-related animal injuries. 7 –10 Given the largely rural nature of New Mexico and the ample opportunities for human interactions with both wild and domestic animals, I wanted to investigate animal-caused fatalities in this state. By using data from a medical examiner's office, I collected information on the specific animal involved, how the incident occurred, how long a person survived after the initial injury, and whether drugs or alcohol were present in the decedent at the time of death. Understanding the populations most at risk for these types of fatalities and the circumstances under which they occur will, hopefully, help in targeting education and prevention measures most effectively to reduce the occurrence of animal-caused fatalities.
Methods
In New Mexico, deaths that are sudden, violent, untimely, unexpected, or unattended by a physician are investigated by a statewide, centralized medical examiner's office called the Office of the Medical Investigator (OMI). Each year the OMI investigates approximately one third of the deaths in the state, and although the OMI does not have jurisdiction on federal lands (American Indian reservations and military installations), the agency is often contracted to investigate unnatural deaths (homicides, suicides, and accidents) on these lands. Autopsies are performed at the OMI's facility on the University of New Mexico campus in Albuquerque, using a system of transporters to bring bodies in from around the state. Eight board-certified forensic pathologists work with a team of field investigators to determine cause and manner of death for approximately 5000 deaths each year.
The OMI has been computerized since the 1970s, providing researchers with an electronic database of more than 30 years of medicolegal death investigation data. Cause and manner of death are coded for each case using an in-house alphanumeric system that enables queries of the database for specific types of deaths. For this study I identified all animal-caused fatalities from 1993 through 2004, excluding zoonotic disease deaths and motor vehicle collisions involving animals to be consistent with previously published studies.5,6 I abstracted demographic information on the decedents, as well as circumstantial information such as animal involved, whether the death occurred in an occupational setting, rural vs urban location, injuries involved, survival period after the injury, manner of death, and any toxicological findings. Data were entered into an Excel spreadsheet and analyzed with SAS version 9.1, using χ2 and Fisher exact tests to analyze categorical variables and Wilcoxon's rank sum test to compare continuous variables. P ≤ .05 was considered significant.
Results
Reviewing the OMI's records from 1993 to 2004 revealed 63 animal-related deaths exclusive of zoonotic infections and animal-motor vehicle collisions, yielding an annual age-adjusted mortality rate of 0.3 per 100 000 population, with 4 to 7 animal-caused deaths each year. Men were more frequently involved than women, with 46 male decedents (73% of the total) identified compared to 17 female decedents. Ages ranged from 2 to 93 years, with a median age of 48 years (Figure). Comparing the age distribution to that published for the national total, I found that in New Mexico, as in the rest of the United States, the highest percentages of animal-caused deaths occurred in 20 to 64 year olds (66.7% of the total in New Mexico, 53.4% of the total nationally). 6 As with the national trend, the elderly (65 years and older) made up the second most commonly affected group, with 22.2% of the total compared to 29.5% nationally. 6 White non-Hispanics were the most commonly involved racial/ ethnic group, with 52% of the animal-caused fatalities, compared to 29% white Hispanic and 19% American Indian. During this time period, New Mexico's population comprised 44% white non-Hispanic residents, 42% white Hispanic, 10% American Indian, 2% African American, 1% Asian Pacific Islander, and 1% other, indicating an overrepresentation of white non-Hispanics and American Indians among this category of cause of death. There were no significant differences in age by either gender or by racial/ethnic classification.
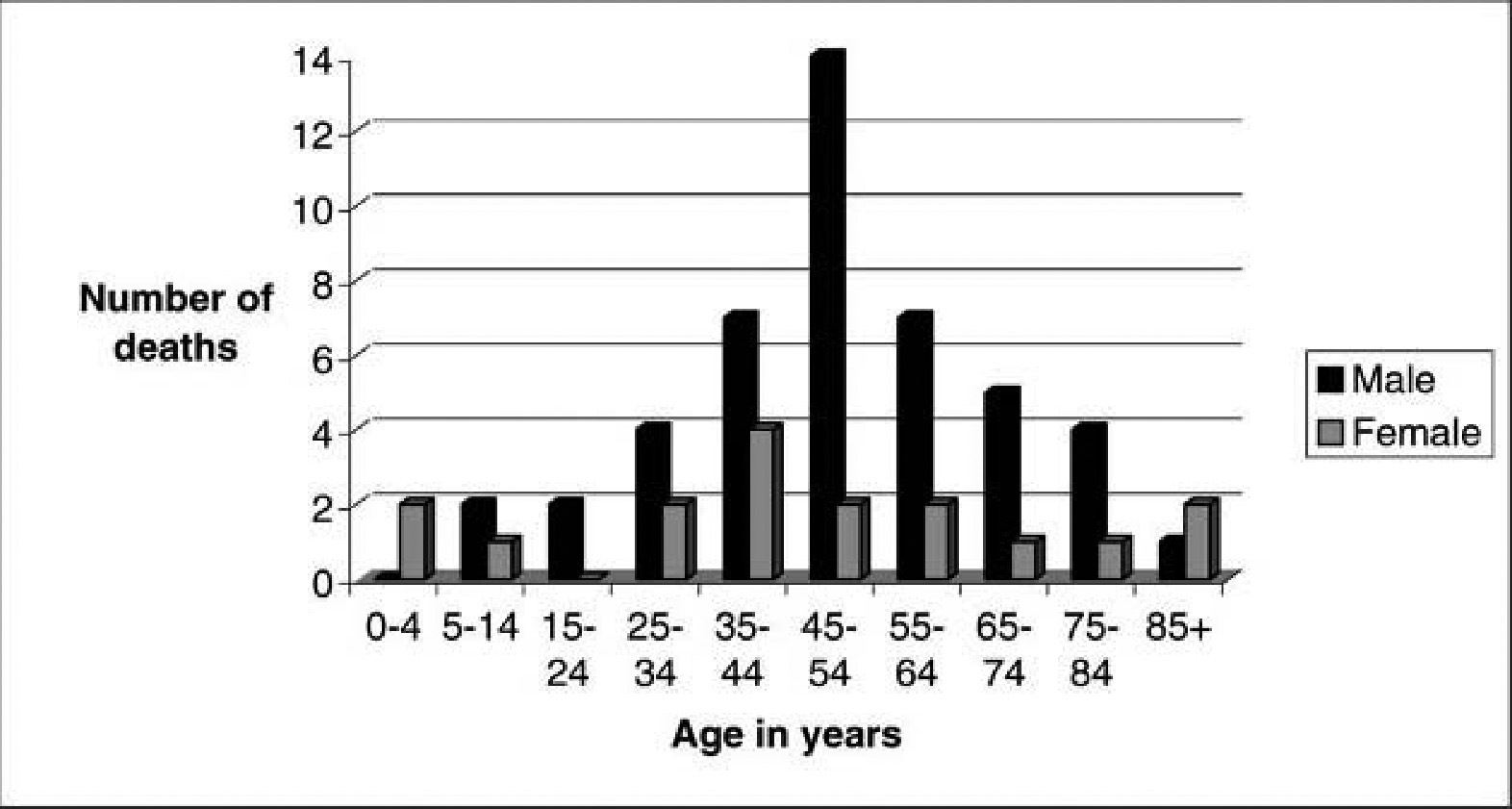
Age distribution by gender of animal-caused fatalities in New Mexico occurring between 1993 and 2004.
Temporally, the highest numbers of animal-caused fatalities occurred in late spring and summer (April, May, June with 9, 7, and 10 deaths, respectively), with 54% of the incidents occurring between May and August. The fewest deaths occurred in November and December, with 2 deaths each. All deaths were ruled to be accidental (vs homicide, suicide, natural, or undetermined), and the most common causes of death were multiple injuries (41%) and head and neck injuries (33%).
The majority of deaths (58/63, 92%) were due to nonvenomous animals. The Table shows that horses were the animals most commonly involved with fatalities, with a total of 43/63 deaths (68%) due to a person falling from, being thrown from, crushed, dragged, or kicked by a horse. The majority (29/43, 67%) of horse-related deaths occurred in rural settings. In the horse-caused fatalities, 15 decedents fell from a horse, 8 were thrown, and in 2 cases the incident was not witnessed. In these 2 cases, the decedents were last seen alive riding a horse, then found dead in a pasture with injuries consistent with a fall from a horse. Eight people died after being kicked by a horse, 5 were crushed by a falling horse, 3 were dragged to their deaths, and 2 people died after being struck in the chest by a horse's head. One person died after being thrown during a parade, 1 was killed by a kick from a horse at a horse show, 1 died while on a hunting trip, 1 was fatally injured in a feedlot, 2 received fatal injuries at race tracks, and the rest (37/43, 86%) were injured while riding or working with horses on privately owned land. None of the decedents killed in horse-related accidents was reported to be wearing a helmet at the time of injury, and the cause of death was head injury in 31/43 (72%) of these deaths. In the remaining 12 deaths the fatal injury was to the chest (2), abdomen (4), or chest and abdomen (6).
Numbers of human deaths caused by specific animals in New Mexico, 1993–2004
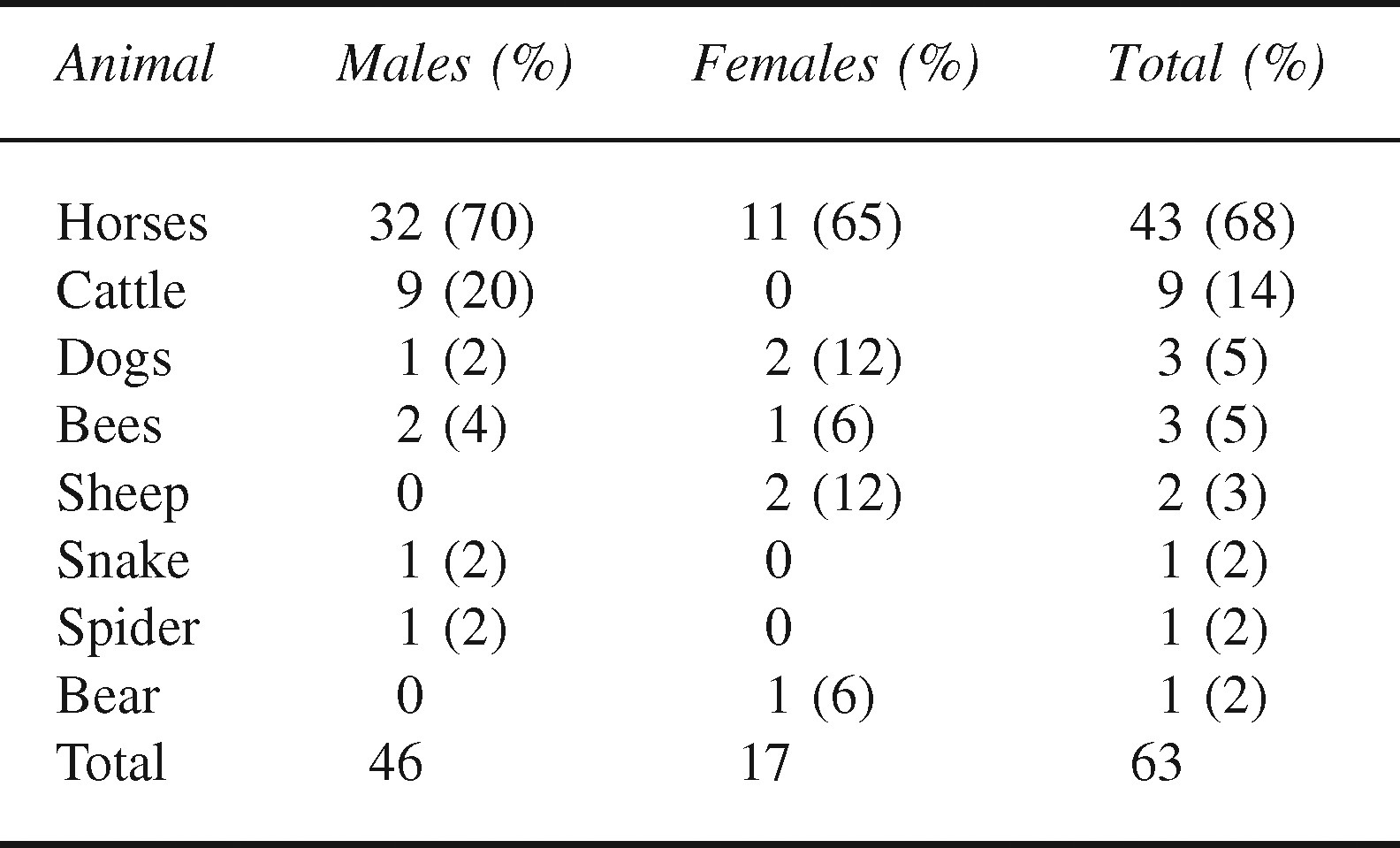

Cattle were the second most commonly involved animals, with 9 deaths (14%) during this time period, all in males. As with horse-related deaths, the majority (6/9, 67%) of these deaths occurred in rural locations. Bulls were implicated in 8 of the 9 deaths: 4 by trampling, 2 by being thrown off a bull during a rodeo, 1 by goring, and 1 by kicking. All but one of these deaths resulted from blunt force injuries to the chest and abdomen, with 1 resulting from head trauma. A ninth decedent died after being struck in the head by a cow. Two deaths occurred after rams attacked elderly women who were attempting to move sheep from one pasture to another, with the rams “butting” the women hard enough to knock them to the ground and cause fatal blunt trauma to the head, neck, and extremities. In 2 of the 3 cases of anaphylaxis after a hymenoptera (bees and wasps) sting, the decedents were known to be allergic but did not have epinephrine with them at the time of the sting. An unusual occurrence, death by bear mauling, took place when a bear entered a home in a mountainous area looking for food after a dry summer and attacked the elderly homeowner in the kitchen. The bear was later destroyed and found to have evidence of the attack present upon necropsy.
The majority of people in this study (38/63, 60%) died either immediately after the incident or within an hour of its occurrence. Twenty-five people survived 24 hours or more after injury, with a range of 1 day to 33 years, a median survival time of 13 days, and a mean survival time of 5 years. Three decedents lived from 13 to 33 years with paralysis caused by horseback-riding accidents, and 4 survived from 15 to 19 years with seizure disorders caused by horseback riding accidents. All 7 ultimately died from complications from either the paralysis or seizure disorders, leading to their inclusion in this study. The majority of the injuries (42/63, 67%) occurred in a rural location. There was no statistically significant difference in the proportion of people surviving more than 1 day between fatalities occurring in a rural location (15/42, 36%) vs those occurring in an urban location (10/21, 48%) where access to medical care would be expected to be more expeditious. However, time from injury to receipt of medical care was not recorded, precluding comparison of such times in rural and urban locations.
Six deaths (9.5%) occurred in children under the age of 18, ranging in age from 2 years to 15 years and comprising 3 girls and 3 boys. As with adults, horses were the most commonly implicated animals, involved in 5 of the 6 childhood deaths. One child was attacked and killed by a dog. Parents were nearby in all but one of the cases.
Ten of the deaths (16%) were determined to be occupational, and all occurred among males. Bulls caused 3 occupational deaths and horses caused 7. Those killed while working with animals included jockeys, rodeo competitors, a farrier, and farm/ranch workers. Ages ranged from 18 to 77 years, with half the decedents being white non-Hispanic and the other half white Hispanic. Seven of the deaths occurred in remote locations classified as rural, and only 1 decedent survived more than 2 days after the original injury.
Alcohol was found in blood samples drawn at autopsy in 10 decedents. If they had been driving rather than working around animals, 8 of the 10 could have been charged with driving while intoxicated, given that their blood alcohol concentrations were over the legal limit of 0.08%. Blood alcohol concentrations ranged from 0.031% to 0.32%, with a mean blood alcohol concentrations of 0.183%. One person was also found to have cocaine present at the time of death. In 25 decedents, a survival interval of more than 24 hours precluded obtaining a blood sample for alcohol and drug testing at the time of injury.
Discussion
As with previous studies, I found that white males were most at risk for animal-caused fatalities. 6 –8,10 Males are theorized to be more at risk for animal-related deaths because of their increased likelihood to participate in outdoor activities, including hunting, fishing, ranching, and farming. 6 American Indians were also overrepresented compared to the demographic composition of New Mexico, perhaps because of differences in lifestyles and residence. Most American Indians in New Mexico reside on reservations, and the majority of American Indian reservations in New Mexico are located in rural areas. 11 All ages of people were affected, and deaths occurred in both recreational and occupational settings. The increased occurrence in late spring and summer is not surprising, as people are more likely to be outdoors working or interacting with animals when the weather becomes more pleasant. The annual age-adjusted rate of animal-caused deaths for New Mexico (0.3 per 100 000 population per year) is higher than the national age-adjusted rate of 0.1 per 100 000. 12 New Mexico's annual rate is, however, comparable to other primarily rural and sparsely populated western states, including Wyoming, South Dakota, Idaho, and Montana. 12 The age distribution of animal-caused fatalities was similar to that found by analyzing data from CDC Wonder, with adults 20 to 64 years of age most at risk followed by the elderly. 6 As with previous studies, nonvenomous animals were the most commonly implicated in these nonzoonotic animal-caused deaths, with horses the most commonly involved.6,7 Similar to other studies, people were most likely to be injured by falling from or being thrown from a horse, with head injuries the most common cause of death in horse-related fatalities.13,14 No mention of helmet use was found in any of the reports of death in this study, and nationally reported helmet use among horseback riders, particularly those who ride Western style, is low, with riders complaining that helmets were uncomfortable. 15
The percentage of deaths caused by venomous animals in New Mexico during the study period (8%) was markedly lower than that reported in a previous review of national trends (39%). 6 Possible theories for this include increased physician awareness in a state where venomous animals are prevalent, leading to rapid diagnosis and treatment of envenomations, and heightened caution on the part of hikers and outdoor enthusiasts regarding venomous animals. A lower number of bee and wasp stings in this arid southwestern state is most likely because of a lack of nectaring sources, flowering plants sensitive to the frequent droughts experienced in New Mexico. Additionally, a mite infestation in the late 1990s destroyed New Mexico's wild honeybee colonies, leaving only paper wasps, domestic honeybees, and hornets as the more aggressive stinging hymenoptera found in the state (David Richman, PhD, oral communication, 2007).
Dog bites tend to receive the most attention of animal-related injuries. In response to several high profile dog maulings, New Mexico passed the Dangerous Dog Act in 2005, requiring owners of dangerous dogs to ensure they are securely restrained. 16 Previously published studies found that most dog bites requiring medical attention affect children under the age of 15, and that children are bitten 2 to 3 times more frequently than one would expect, given the proportion of children in the population. 1 Three deaths due to dog maulings were investigated by the OMI from 1993 to 2004, but only one was in a child under 15 years of age. Looking at a published report of nonfatal dog bites in New Mexico between 1998 and 2003, 291 dog-bite-related hospital discharges were identified, and among this group children ages 0 to 14 years had the highest rate of dog-bite hospitalizations. 16 Evidence indicates dog bites are a problem in New Mexico, but the OMI data reveal that these bites are usually not fatal.
Using medical examiner data offers some potential benefits for epidemiologic researchers. The information resulting from medicolegal death investigations exceeds that available on a 1-page death certificate and may include medical records, scene investigation results, toxicological test results, microbiological assay results, notes from interviews with witnesses and family members, police reports, and autopsy results. This information can be particularly useful for studying deaths such as animal-caused fatalities, where the circumstances may be enlightening for possible prevention efforts. National databases, such as CDC Wonder, often do not include information on activity at the time of injury or location of death,5,6 information that can often be obtained from the medical examiner or coroner records. There are limitations, however, including the OMI's lack of jurisdiction on federal lands, which could lead to an underreporting of animal-related deaths, and the fact that OMI does not currently use International Classification of Disease codes, but rather relies on an in-house coding system. The OMI is currently working with New Mexico's Bureau of Vital Records and Health Statistics to link autopsy records with International Classification of Disease codes assigned by the Bureau of Vital Records and Health Statistics when issuing death certificates, so that OMI data can be compared to other data sources using International Classification of Disease codes.
Although both animal and human behavior can be difficult to predict, a review of animal-caused fatalities in New Mexico revealed that in many cases deaths could have been prevented by either the use of protective gear or alterations in human behavior. Given the preponderance of horse-related deaths in this and other studies, most due to head injuries, and the documented effectiveness of helmets in preventing these types of head injury, measures should be taken to increase awareness of the need for both caution and helmets when riding. 13 –15 Riding clubs, pony club meetings, and 4-H clubs offer excellent educational opportunities to teach young riders about safe riding and handling tips when working with horses. Considering that most cattle-related fatalities were due to injuries to the chest and abdomen, rodeo competitors riding bulls should wear chest protectors. While this may not be feasible for people routinely handling cattle, injuries could be reduced by ensuring that handling facilities for livestock are sturdy and in good repair, as several of the cattle-related fatalities occurred when cattle left a chute or were loose in a corral rather than being properly restrained. Poor judgment also played a role in several deaths, with people entering enclosures with bulls known to be mean or picking up a venomous snake. Supervisors of employees working with animals need to make safety a priority. Alcohol consumption should be avoided when working with animals, just as it should be when driving or operating machinery. People with known bee/wasp allergies should always carry their epinephrine and an oral antihistamine, even (or especially) when vacationing. A medical alert bracelet could also serve to inform emergency personnel of their allergies. Children should always be closely supervised when interacting with animals, even animals that are thought to be “good” with kids. As with so many public health challenges, a few moments of caution can prevent heartbreaking consequences.
Footnotes
*
This information was presented as a 10-minute oral presentation at the 2006 American Public Health Association Annual Conference in Boston, MA, November 4–8, 2006.
