Abstract
This study aimed to determine whether the number of nucleated red blood cells (NRBCs) in maternal circulation during the first trimester of pregnancy could identify pregnancies that will have an anomalous Doppler in the second trimester. A total of 85 blood samples were obtained at 11–14 weeks of gestation with mean uterine arterial perfusion index >1.6, as noted by Doppler ultrasonography. NRBCs were enriched by magnetic automated cell sorting using anti-CD71 and were stained with May/Grunwald/Giemsa. A total of 4.8 NRBCs (range 1–75) were identified in 68 cases. Follow-up scans at 22–24 weeks were available in 46 cases. In 39 women, blood flow in the uterine arteries normalized, whereas in seven, high resistance was noted. One woman in the high-resistance group developed preeclampsia (PET; four NRBCs) and another delivered an intrauterine growth restriction (IUGR) baby (75 NRBCs). The number of NRBCs in women whose Doppler indices later normalized and in those who continued to have increased impedance was similar. The study indicates that NRBC number in maternal circulation during the first trimester cannot be used to screen pregnancies at high risk for developing preeclampsia (PET)/IUGR. High-impedance blood flow in the uterine arteries in the first trimester may be due to an unfinished process of trophoblastic invasion, most likely to be completed successfully by 22–24 weeks.
Keywords
P
Doppler ultrasound studies have shown that impaired placental perfusion at 22–24 weeks of gestation is associated with high impedance to flow in the uterine arteries, which is characterized by the presence of an early diastolic notch in the waveform of these vessels (Harrington et al. 1996; Frusca et al. 1997). Therefore, Doppler ultrasound examination of the uterine arteries can be used to identify a group of pregnancies at high risk for subsequent development of PET/IUGR.
Recently, it has been demonstrated that fetal cells, as well as fetal DNA, in maternal circulation in weeks 22 and 23 of gestation precede the onset of PET, suggesting that impaired placental perfusion is associated with an increase in fetomaternal trafficking (Holzgreve et al. 1998,2000; Lo et al 1999; Al-Mufti et al. 2000a,b; Zhong et al. 2002).
Because PET is a major cause of fetal and maternal morbidity and mortality, it is important to develop a predictive screening test early in pregnancy so that we can anticipate pregnancies at high risk for this complication.
This is a preliminary study aimed at determining whether the number of nucleated red blood cells (NRBCs) in maternal circulation during the first trimester of pregnancy could identify pregnancies that will have an anomalous Doppler finding during the second trimester.
Materials and Methods
Materials
Twenty milliliters of peripheral blood was obtained from 85 pregnant women in the first trimester of pregnancy with increased impedance to both uterine arteries (mean uterine arterial perfusion index >1.6) as defined by color ultrasound examination. Ten women with normal flow velocity waveforms were used as controls. All pregnancies were singleton. Women were healthy, normotensive on no medication, and carried fetuses with no obvious defects and normal growth. All women gave consent to participate in the study.
Follow-up scans in weeks 22 and 23 of pregnancy were obtained for 46 of the 85 originally tested cases. Details of the pregnancy outcomes were available from the patients' files. PET was diagnosed as maternal blood pressure >140/90 mmHg with positive protein on reagent strip urinalysis of urine protein collection >300 mg/24 hr.
The diagnosis of IUGR was made if the birth weight was below the fifth percentile of the normal range of gestation.
Methods
Mononuclear cells were isolated by density gradient centrifugation with Histopaque 1083, magnetically labeled with CD71 antibody to the transferrin receptor, and positively selected using magnetic automated cell sorting. Isolated cells were next stained with May/Grunwald/Giemsa and NRBCs were identified and enumerated by morphology under a light microscope.
Results
NRBCs were identified in the blood samples of all cases tested (Figure 1). Of 85 women with abnormal first-trimester Doppler ultrasound, 39 were not available for reevaluation. In another 39, ultrasound findings normalized during the second trimester and seven women continued to have abnormal Doppler ultrasound findings during the second trimester. Of the latter, one woman later developed PET, one delivered an IUGR baby, and five had uncomplicated pregnancies and proceeded to deliver normal babies.
Table 1 shows the number of NRBCs isolated from maternal circulation during the first trimester of pregnancy. In the control group, an average of four cells (range 1–7) were identified, and in women with abnormal Doppler ultrasound waves, the mean NRBC number was 4.8 (range 1–75). Among women who continued to have an abnormal Doppler in the second trimester, the cell number was 4.9 (range 1–75). Four NRBCs were identified in the pregnant woman who subsequently developed PET, and 75 such cells were isolated from the blood of the woman with the IUGR baby.
NRBC isolated from maternal peripheral blood stained with May/Grunwald/Giemsa.
Discussion
Early recognition of patients at risk for development of PET/IUGR might allow a reduction of the worldwide mortality and morbidity associated with this complication of pregnancy. The availability of screening tests for early detection of this problem will help to identify patients in need of more careful monitoring and preventive treatment, to evaluate the progress of the disorder, and to improve pregnancy outcome.
Previous studies demonstrated a correlation between the number of NRBCs and abnormal uterine artery Doppler ultrasound in women who develop PET/IUGR during the second trimester of pregnancy (Holzgreve et al. 1998,2000; Al-Mufti et al. 2000a,b). The present report, which must be considered preliminary because only seven of the 46 women tested continued to have high-impedance blood flow during the second trimester and only two of the seven developed PET or IUGR, indicates that the number of NRBCs in the maternal circulation during the first trimester cannot be used as a second-line screening to identify pregnancies at high risk for PET/IUGR. There was one case with high NRBC number and subsequent delivery of an IUGR baby, but this finding is not sufficient to establish a possible correlation and more pregnancies complicated by PET/IUGR must be tested to confirm this finding.
Number of NRBCs isolated from maternal blood in the first trimester from pregnancies with abnormal Doppler and from controls
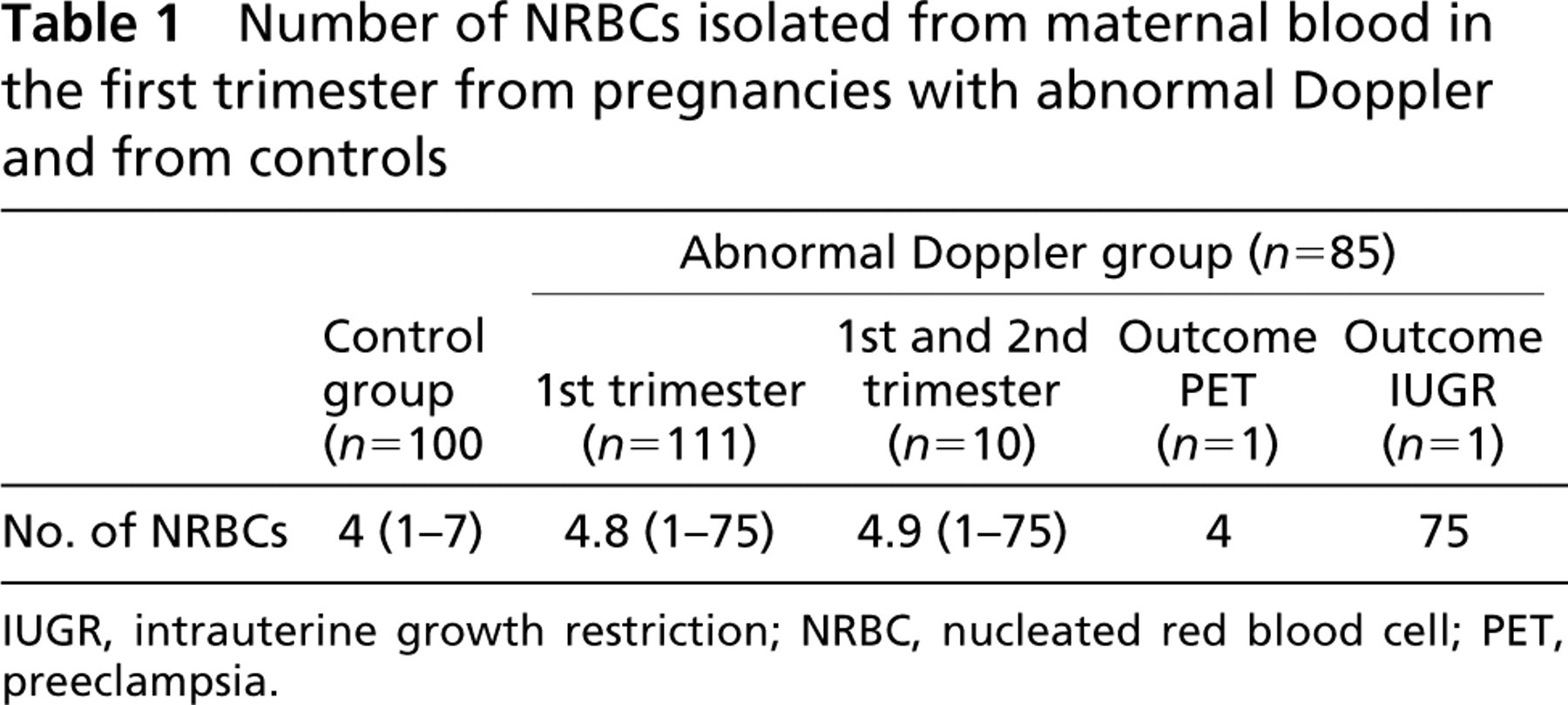
IUGR, intrauterine growth restriction; NRBC, nucleated red blood cell; PET, preeclampsia.
The NRBCs detected in our study must be both fetal and maternal, but we did not attempt to identify their origin because of the low cell numbers. However, it has been postulated that the increase in the number of fetal NRBCs during pregnancy precedes the increase in the number of maternal NRBCs (Al-Mufti et al. 2000a). In addition, female carriers of the β-thalassemia trait were excluded from the study because we had previously demonstrated that under the stress of pregnancy, carriers of the β-thalassemia trait produce and release into the circulation a significant number of NRBCs (Mavrou et al. 2003).
High-impedance blood flow in the uterine arteries in the first trimester may be due to an unfinished process of trophoblastic invasion, most likely to be completed successfully by 22–24 weeks. This may explain why the Doppler findings normalized during the second trimester.
