Abstract
The identity and functions of surface proteins on human leptomeningeal and meningioma cells are incompletely characterized. Some structural and functional similarities between the leptomeninges and pleura suggest that proteins important to pleural function and tumorigenesis might also be relevant to leptomeningeal disease. Mesothelin is a recently described, 40-kDa membrane protein expressed in pleura. Its functions in this tissue are under investigation. Sections of 20 normal adult brains with leptomeninges and 49 World Health Organization (WHO) grade I, 21 grade II, and 2 grade III meningiomas were analyzed using an extensively characterized monoclonal antibody to mesothelin and streptavidin-biotin complex immunohistochemistry. Five meningiomas were also evaluated by Western blot. Mesothelin immunoreactivity was detected in the arachnoid in 6 of 20 cases and in 23 of 49 WHO grade I meningiomas. It was also detected in 7 of 21 WHO II tumors and 1 of the 2 anaplastic meningiomas. By Western blot, all five meningiomas exhibited mesothelin precursor protein, including one where notable immunoreactivity was not identified in a formalin-fixed tissue section. These findings suggest that mesothelin is expressed in at least some arachnoid and meningioma cells. Future studies may clarify its role in the development of meningiomas, meningeal seeding of gliomas, and metastases to the leptomeninges.
T
Mesothelin is a cell surface differentiation protein. The functions of mesothelin are not established but may include a role in cell adhesion (Chang and Pastan 1996). However, the importance of this role is uncertain because mice deficient in mesothelin develop normally, reproduce, and display no overt histologic abnormalities in a number of tissues (Bera and Pastan 2000).
The expression of mesothelin in the human leptomeninges and meningiomas has not been studied. Nonetheless, some similarities in the structure and functions of the pleura and leptomeninges suggest that mesothelin might be expressed in leptomeningeal cells or meningiomas and important to meningeal function. In this study, we analyzed leptomeninges in adults and World Health Organization (WHO) grade I–III meningiomas.
Materials and Methods
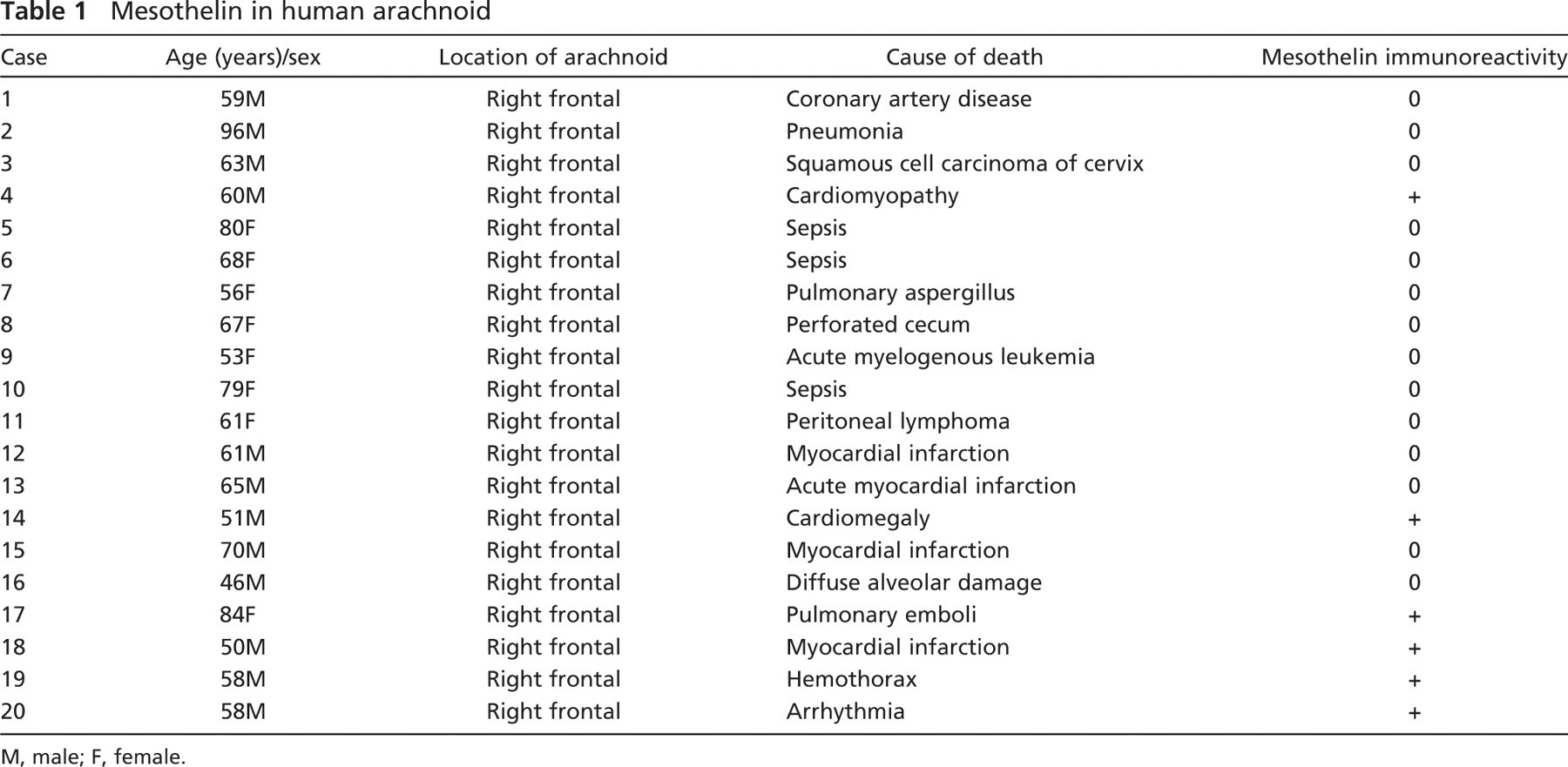
Leptomeninges from autopsy samples of 20 adult patients who died without neurologic disease or central nervous system lesions and 72 meningiomas were analyzed. The latter group included 49 WHO grade I, 21 WHO grade II, and 2 WHO grade III meningiomas (Perry et al. 2007) collected between 2000 and 2007 from the University of Rochester or from the consultation service. Patient characteristics for the leptomeningeal samples and tumor characteristics are listed in Tables 1 and 2, respectively.
Immunohistochemistry
Each case was analyzed with a monoclonal antibody to human mesothelin made against a 100 amino acid sequence present in the membrane-bound form of mesothelin (Chang and Pastan 1996) (used at 1:200 dilution, clone 5B2; Novo Castra, Newcastle upon Tyne, UK), which has been characterized previously (Ordonez 2003), and streptavidin-biotin immunohistochemistry. Sections of mesothelioma were used as a positive control. For antigen retrieval, tissue sections were incubated in a thermoresistant chamber with 10× Reveal Decloaker (Biocare Medical; Concord, CA) at 120–123C and pressure of 20–24 psi for 45 min. Immunoreactivity in the membrane and cytoplasm was assessed and graded as 0 or + in leptomeninges, and in meningiomas as 0 if no distinct immunoreactivity was found, 1 if 1–10% of cells were immunoreactive, 2 if 11–25% of cells were positive, 3 if 25% but <50% of cells were immunoreactive, and 4 when >50% of cells away from section edges were immunoreactive. Differences in groups were analyzed by one-way ANOVA using In Stat (Sigma; St. Louis, MO).
Mesothelin in human arachnoid
Western Blots
Protein from five WHO grade I meningiomas was obtained by mechanical homogenization in RIPA Lysis Buffer (Upstate Biotechnology; Waltham, MA) with 1:100 Protease Inhibitor Cocktail (Sigma) and frozen at −85C. The tissue slurries were thawed on ice and vortexed vigorously. Solids were removed by centrifugation. Protein concentrations were quantified using a Bradford assay (BioRad Protein Assay reagent), and 35 μg protein from each was loaded on 7.5% acrylamide gels and transferred to 0.45-μm nitrocellulose membrane. The membrane was blocked overnight at 4C in 5% milk in Tris-Cl buffer with Tween 20 and reacted with an affinity purified goat anti-mesothelin 69-kDa precursor primary antibody (sc-27714; Santa Cruz Biotechnology, Santa Cruz, CA) at 1:200 for 2 hr at room temperature. This was followed by horseradish peroxidase–conjugated secondary antibody treatment. Detection was achieved with Western Lightening (PerkinElmer; Boston, MA) on Xomat film (Kodak; Rochester, NY).
Results
Immunohistochemical findings are summarized in Tables 1 and 2. Mesothelin immunoreactivity was not detected in normal pia but was found in the cytoplasm of arachnoid cells in six cases with leptomeninges (Figure 1A). In meningiomas, mesothelin immunoreactivity was detected in the cytoplasm and was variably distinct in the cell membrane in 23 of 49 (47%) WHO grade I meningiomas (Figure 1B), including 10 of 14 (71%) meningothelial, 9 of 18 (59%) transitional, and 1 of 11 (9%) fibrous tumors. The percentage expression in the meningothelial and transitional subtypes was significantly different than that in the fibroblastic group (
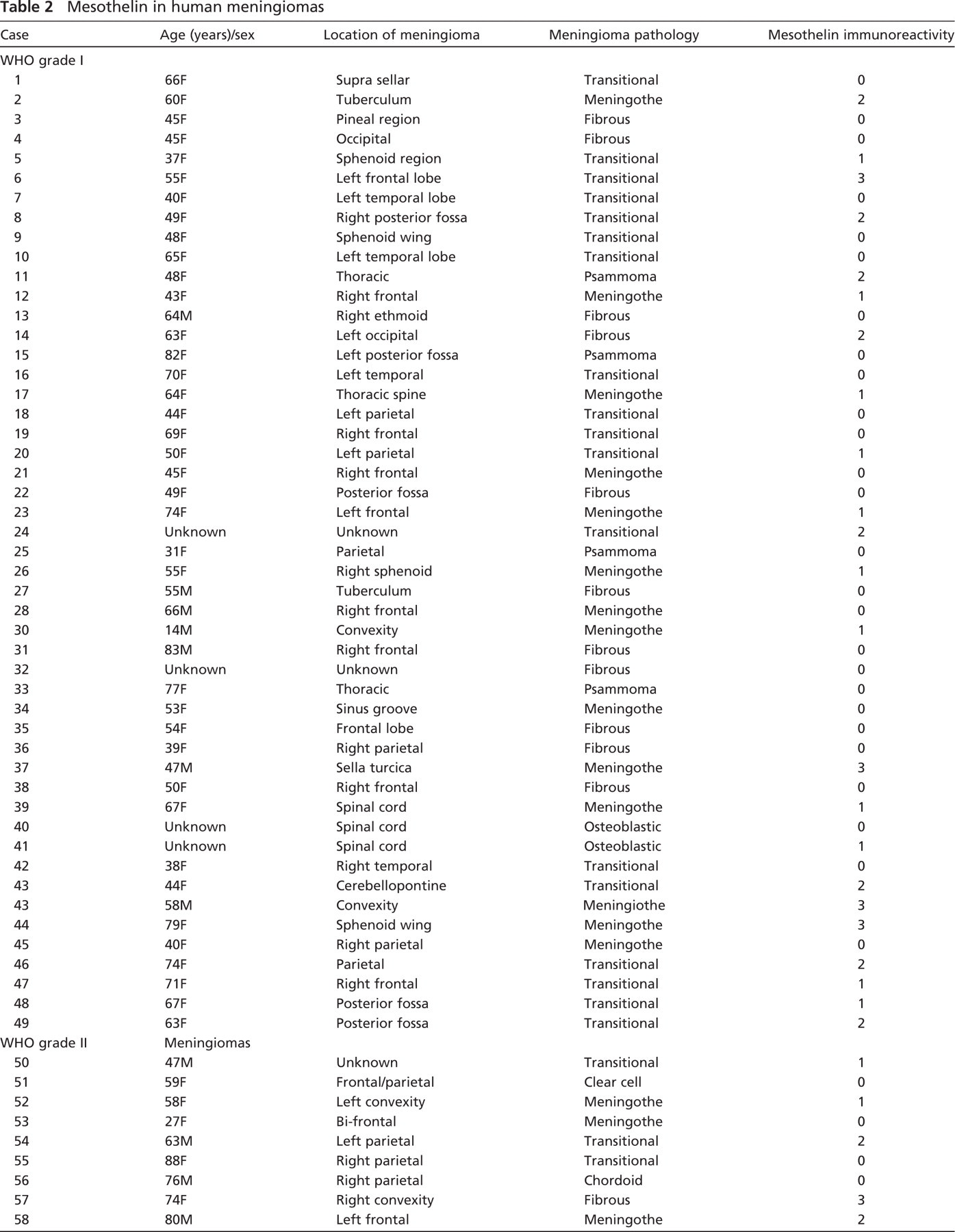
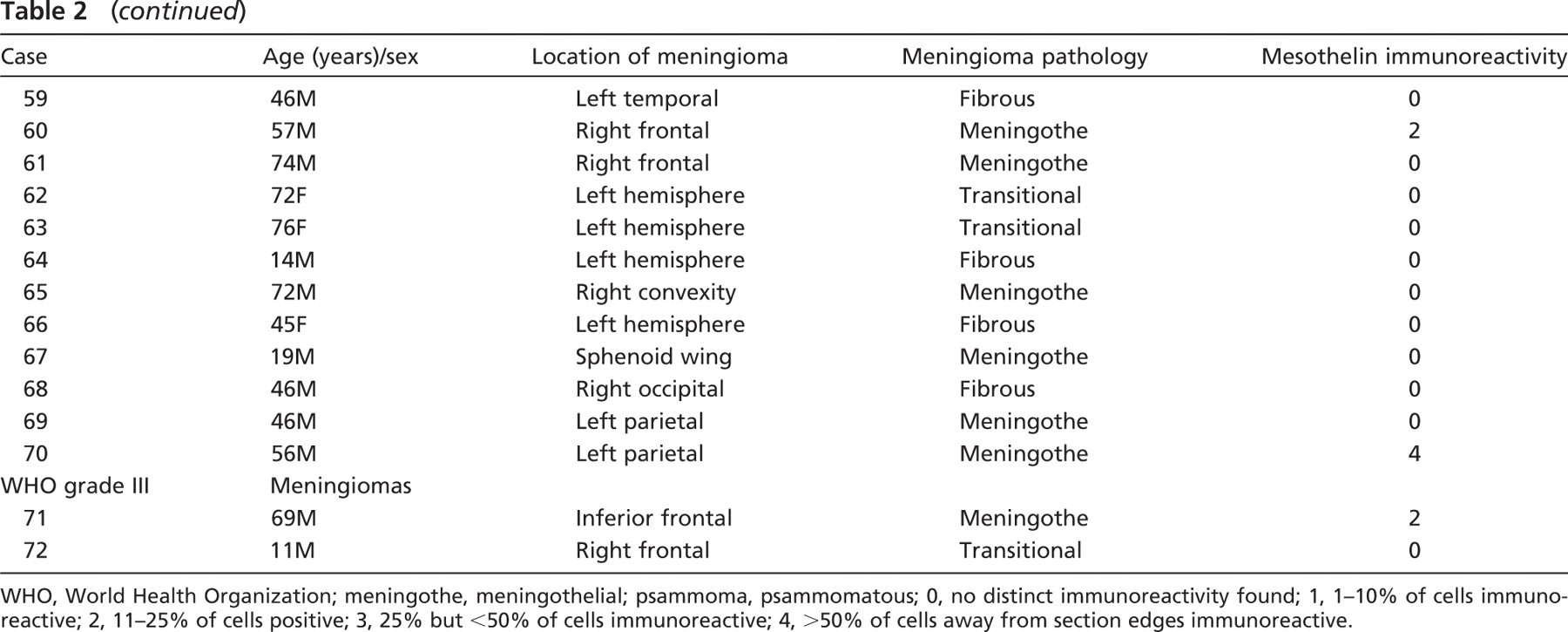
Mesothelin in human meningiomas
The Western blot of lysates from five WHO grade I meningiomas (Cases 43, 45, and 47–49) all showed the 69-kDa mesothelin precursor protein, including Case 45, in which distinct mesothelin immunostaining was not shown in the formalin-fixed, paraffin-embedded section (Figure 2).
Discussion
Mesothelin was detected in the arachnoid and in meningiomas of all grades, and the precursor protein was also detected in meningiomas. To our knowledge, this is the first identification of mesothelin in these tissues. By immunohistochemistry, mesothelin was found in nearly one half of the WHO grade I meningiomas and in one third of atypical, WHO grade II meningiomas. Using Western blot, the mesothelin precursor was shown in each of the meningiomas analyzed. These findings suggest that mesothelin is expressed in meningiomas. Moreover, in view of the overfixation of the autopsy material and in some meningiomas, it is possible that the 40-kDa mesothelin is expressed in a greater percentage of leptomeningeal cells and meningiomas than was detected here.
In our study, immunoreactivity was seen in the cytoplasm with a variable membrane distribution similar to the cytoplasmic, with or without membranous, immunostaining as seen in many tumors including mucinous carcinomas of the ovary, adenomatoid tumors, adenocarcinoma of the endometrium, and pancreatic adenocarcinomas (Ordonez 2003; Jhala et al. 2006). In our mesothelioma controls, using the monoclonal antibody titered to a greater dilution than used in cited studies, nests of mesothelioma cells showed membrane, but also showed cytoplasmic staining. Because meningiomas are solid, often syncytial tumors that, by definition, have interdigitating membranes, processes, and desmosomes, the distinction may be more difficult than in papillary structures such as the majority of gland and lumenbearing adenocarcinomas studied previously, and it is felt that membrane localization occurs.
In this initial study, mesothelin was detected more commonly in meningothelial and transitional than fibrous meningiomas but was not restricted to a specific histological subtype. Several studies have suggested that sporadic WHO grade I and II meningiomas might be divided into meningothelial and non-meningothelial subtypes based on the relative expression of the neuro-fibromatosis type 2 tumor suppressor gene (
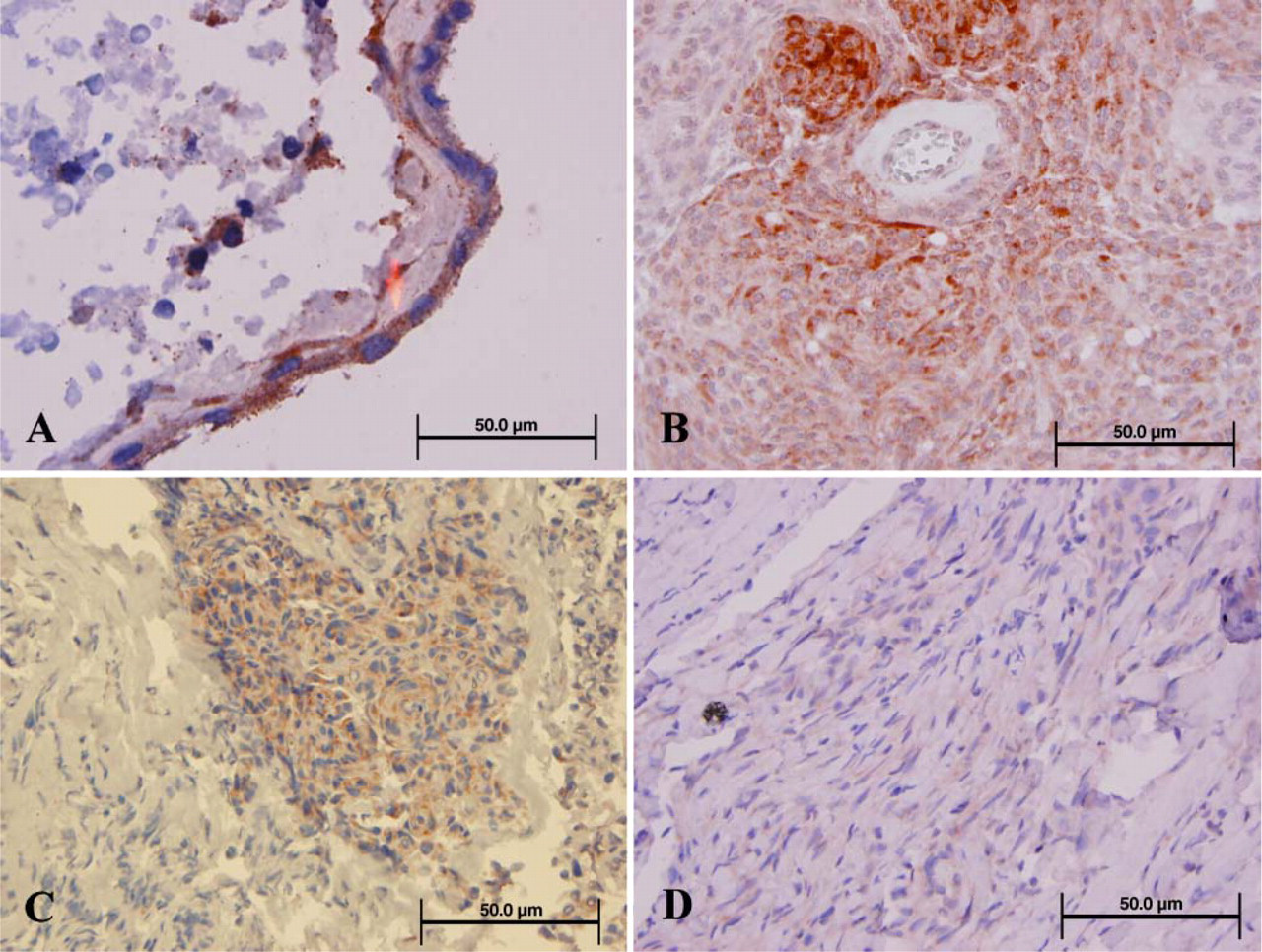
Mesothelin immunohistochemistry. (
The functions of mesothelin in the normal leptomeninges and meningiomas have yet to be studied. Moreover, they have not been established in mesothelium, mesotheliomas, or other carcinomas (Ho et al. 2007). Mice deficient in mesothelin develop normally and have tissues reported to be histologically normal, although the brain was not extensively analyzed (Bera and Pastan 2000). Nonetheless, in bronchial, ovarian, pancreatic, and gastrointestinal carcinomas, the 4- to 10-fold overexpression of mesothelin suggests it plays an important role in the oncogenesis of many tumors (Chang and Pastan 1992, 1996; Scholler et al. 1999; Ordonez 2003; Hucl et al. 2007).
In some pathologic conditions, mesothelin may facilitate binding of neoplastic cells to peritoneum or pleura. For example, mesothelin has been shown to bind MUC16, a mucin glycoprotein with high affinity (Rump et al. 2004; Gubbels et al. 2006). This seems to facilitate binding of ovarian carcinomas to peritoneum and may facilitate seeding (Rump et al. 2004; Gubbels et al. 2006). Although this interaction alone does not seem sufficient to secure this anchoring, it may represent an initial step in a cascade of events resulting in cell adhesion analogous to leukocyte adherence to damaged endothelium mediated by a number of selectins (Rump et al. 2004; Gubbels et al. 2006). Thus, mesothelin expression by peritoneal cells seems to bind MUC16 and facilitate ovarian carcinomatous peritonitis. Because a number of adenocarcinomas express MUC16, and adenocarcinomas represent one of the most common carcinomas metastasizing to the leptomeninges, it is conceivable that this interaction with mesothelin facilitates establishment of metastases there and development of meningeal carcinomatosis.
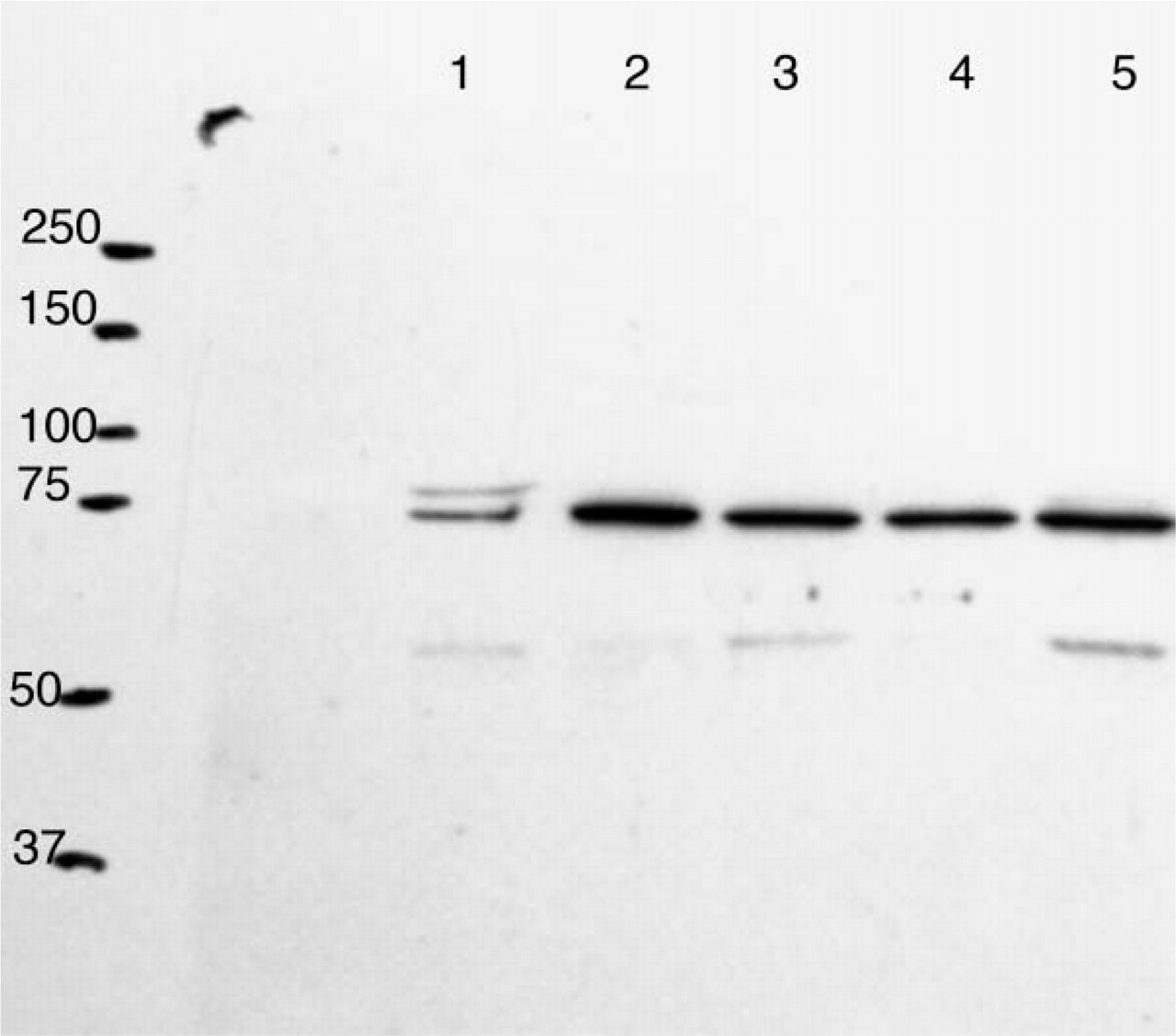
Mesothelin Western blot. Mesothelin precursor protein (69 kDa) is detected in all five WHO grade I meningiomas (Cases 43, 45, and 47–49).
Screening for soluble mesothelin-related peptides (SMRPs) or the cleavage product megakaryocyte potentiation factor (MPF) in serum has been proposed as a diagnostic tool to screen for occult mesotheliomas and some carcinomas in peripheral tissues (Onda et al. 2005, 2006; Scherpereel et al. 2006; Creaney et al. 2007; Ho et al. 2007). One study found significantly higher SMRPs in pleural fluid of patients with mesothelioma than in patients with other lung tumors or pleuritis, with a specificity of 98% and sensitivity of 67% (Creaney et al. 2007). Nonetheless, levels of SMRPs did not correlate with tumor volume (Hassan et al. 2006). Because meningiomas reside outside the blood–brain barrier, a study in progress is evaluating whether increased SMRPs or MPF may be detected in the serum of patients with meningiomas and might identify early recurrence.
The expression of mesothelin in the brain has not been extensively studied. In our evaluation of sections of normal cortex, mesothelin appeared confined to the arachnoid and was not widely detected. The relatively restricted expression of mesothelin in human tissues suggests that therapies targeting mesothelin in tumors might not produce extensive damage to many normal tissues. In recognition of this, monoclonal antibodies against mesothelin are being developed as a possible therapy for carcinomas widely expressing mesothelin (Hassan et al. 2004; Onda et al. 2005). Demonstration of mesothelin in the leptomeninges and meningiomas, which are outside the blood–brain barrier, raises the possibility that such immunotherapies might also be useful for treating meningiomas. Such antibodies might also be useful in blocking or limiting the adhesion of metastasis, particularly of mucin-16–expressing carcinomas to the leptomeninges. Studies underway are evaluating these possibilities.
Footnotes
Acknowledgements
We thank Dr. Jay Reeder for helpful comments on the project.
